Abstract
SIV infection in macaques is a relevant animal model for HIV pathogenesis and vaccine study in humans. To design a safe and effective vaccine against HIV, we evaluated the suitability of naturally-occurring avirulent Newcastle disease virus (NDV) strains and several modified versions of NDV as vectors for the expression and immunogenicity of SIV envelope protein gp160. All the NDV vectors expressed gp160 protein in infected cells. The gp160 expressed by these vectors formed oligomers and was incorporated into the NDV envelope. All the NDV vectors expressing gp160 were attenuated in chickens. Intranasal immunization of guinea pigs with modified NDV vectors such as rNDV-APMV-2CS/gp160 and rNDV-APMV-8CS/gp160 (NDV strain LaSota containing the cleavage site sequences of F protein of avian paramyxovirus (APMV) serotype 2 and 8, respectively), and rNDV-BC-F-HN/gp160 (NDV strain BC containing LaSota F cleavage site and LaSota F and HN genes) elicited improved SIV-specific humoral and mucosal immune responses compared to other NDV vectors. These modified vectors were also efficient in inducing neutralizing antibody responses to tier 1 A SIVmac251.6 and tier 1B SIVmac251/M766 strains. This study suggests that our novel modified NDV vectors are safe and immunogenic and can be used as vaccine vector to control HIV.
Similar content being viewed by others
Introduction
Human immunodeficiency virus-1 (HIV-1) infection can cause acquired immunodeficiency syndrome (AIDS) in humans1. According to the Joint United Nations Programme on HIV/AIDS, currently more than 36 million people are infected with HIV globally2. Vaccination remains the most efficient approach to control HIV infection in humans. However, a safe and effective vaccine against HIV infection is unavailable. One of the obstacles to develop an effective vaccine against HIV is the lack of a good animal model to test vaccine candidates. Rhesus macaques have been identified as the relevant animal model to evaluate HIV vaccine candidates due to their high degree of genetic relatedness with humans and the similarity between HIV-1 infection in humans and simian immunodeficiency virus (SIV) infection in macaques. Several experimental HIV vaccines have been evaluated in macaques using SIV or simian-human immunodeficiency virus (SHIV) challenge models3,4,5,6. These include recombinant proteins, peptides, inactivated viruses, DNA and live viral vectored vaccines either alone or in different prime-boost combinations. In parallel, there have been six HIV vaccine efficacy trials in humans that have tested four different vaccine strategies but only RV144 trial showed a modest level of efficacy7,8,9. The data from this trial or from a macaque challenge study10 indicated the importance of HIV envelope (Env) protein expressed by recombinant viral vectors and further emphasized the role of antibodies in inducing protective immune responses against HIV.
In the last 30 years, many experimental vaccines have been evaluated for HIV. Among these vaccines, live viral vectored vaccines have shown promising results. To-date, majority of viral vector vaccine studies have been based on viruses such as fowl pox virus, vaccinia virus, adenovirus, vesicular stomatitis virus (VSV) and measles virus11,12. However, pre-existing immunity and safety concerns of systemic spread and potential neurovirulence are some of the demerits of these viral vectors12,13,14. Therefore, additional viral vectors that are safe and free from pre-existing immunity in the human population need to be evaluated.
Newcastle disease virus (NDV), an avian virus, belongs to the genus Avulavirus in the family Paramyxoviridae. NDV is a non-segmented, negative-sense RNA virus, containing six genes, which encode eight proteins. Based on pathogenicity in chickens, NDV strains are classified into three pathotypes: avirulent (lentogenic), moderately virulent (mesogenic) and highly virulent (velogenic)15. Natural lentogenic strains LaSota and B1 are used as live vaccines all over the world. NDV has several advantages for use as a vaccine vector for humans16. There is no pre-existing immunity to NDV in the human population. It is highly safe in humans. It infects via intranasal route and induces robust local and systemic immune responses16,17. Lentogenic NDV strain LaSota has already been evaluated as a vaccine vector in several animal models17,18,19,20. In addition, mesogenic NDV strain Beaudette C (BC) has been tested as vector in rhesus macaques and it has been shown to replicate to a higher titer, did not cause any disease and induced superior antibody responses compared to the NDV strain LaSota21. But mesogenic strain BC is moderately virulent to chickens; therefore, a concern to poultry industry. Currently, both mesogenic and velogenic NDV strains are designated as select agents and hence cannot be used as vaccine vectors. Therefore, we modified the recombinant BC to make it avirulent so that it can be used as a vaccine vector for SIV antigens. This was accomplished either by exchanging complete or part of the genes coding for F and HN proteins with the corresponding genes of the avirulent strain LaSota or by mutating the polybasic residues at F protein cleavage site to either mono or dibasic residues. All the modified BC vectors were found to be avirulent for chickens and met the requirements for exclusion from Select Agent Regulations15.
In this study, our goal was to identify the NDV vector that expresses SIV Env gene at the highest level and induces the best immune response. We chose the SIV Env protein for evaluation because it has been shown by several studies that, similar to HIV Env protein, the SIV Env protein is the major antigen against which neutralizing antibodies are produced22,23. A series of recombinant (r) NDV vectors expressing gp160 of SIV mac239 strain were used to immunize guinea pigs. The levels of immune response to SIV Env protein expressed by different NDV vectors were evaluated. Our results identified several rNDV/SIV viruses that were highly immunogenic and elicited antibodies that neutralized the SIV mac251.6 strain in vitro.
Methods
Cells and Viruses
Chicken embryo fibroblast cell line (DF-1), human embryonic kidney cells (HEK 293) and a human epidermoid carcinoma cell line (HEp-2) were obtained from the American Type Culture Collection (ATCC, Manassas, VA). The modified vaccinia virus strain Ankara (MVA) expressing T7 RNA polymerase was kindly provided by Dr. Bernard Moss (NIH, Bethesda, MD). The NDV strains LaSota and the modified rNDVs were propagated in 9-day-old chicken eggs.
Construction of modified versions of NDV vectors
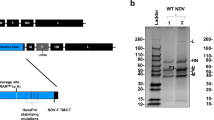
We used plasmid pNDV carrying the antigenome cDNA of NDV strain LaSota24 and modified plasmid pBC of strain Beaudette C (BC) containing some regions of the F gene of NDV strain AKO-1825 and plasmid pNDV containing a mutation Y527A in the cytoplasmic tail of F protein26, as described previously. In addition, we also made a few modified versions of recombinant pBC containing the F and HN protein of strain LaSota. All the BC recombinants had the avirulent cleavage site as that of strain LaSota (GRQGR↓L) and hence the experiments were carried out in BSL-2. Two modified pNDV- rLaSota vectors containing the avian paramyxovirus serotype-2 (APMV-2) fusion protein cleavage site (KPASR↓F) and avian paramyxovirus serotype-8 (APMV-8) fusion protein cleavage site (YPQTR↓L) were also constructed. They were abbreviated by different names as shown in Fig. 1.
Construction of the modified recombinant NDVs expressing SIV gp160 gene. The SIV gp160 ORF of SIV mac 239 was inserted between P and M genes in the rNDV vectors. Genes derived from rBC or AKO-18 are shown as black or gray rectangles, respectively. F gene segments derived from the NDV strain LaSota strain are shown as white bars. All the viruses contain the avirulent F protein cleavage site sequence of strain LaSota, or APMV-2 or APMV-8.
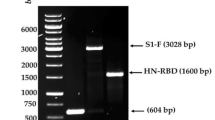
Construction of rNDV and modified rNDV vectors expressing the SIV envelope glycoprotein (gp160)
The plasmid containing codon optimized envelope gp160 gene of SIV mac239 strain was modified by PCR to contain transcriptional signals of NDV and restriction site for PmeI. (Forward: 5′AGCTTTGTTTAAACTTAGAAAAAATACGGGTAGAAGGCCACCATGGGCT130 GCCTGGGCAAC3′, Reverse: 5′GTTTAAACTCACAGCAGGGTCAGTTCC3′). The amplified fragment was cloned into TOPO-TA, sequence confirmed and inserted between the P and M genes of the antigenomic cDNA of strain LaSota (pNDV) and the modified rNDV vectors (Fig. 1). The recombinant viruses were recovered by reverse genetics17 and propagated in 9-day-old chicken eggs. To determine the stability of gp160 genes in different rNDV vectors, the recombinant viruses were passaged ten times in chicken eggs and sequence verified.
Expression of SIV gp160 in cells infected with rNDV and modified rNDVs
To detect expression of SIV gp160, DF-1 cells in 6-well plates were infected with 0.1 MOI of rNDVs containing SIV gp160 and the parental rLaSota virus for 24 h. The cell lysates were analyzed for expression of gp160 by Western blot using a 1:100 dilution of SIV gp120-specific mAb (VM-18S) obtained through the NIH AIDS Reagent Program, Division of AIDS, NIAID, NIH. In order to investigate the incorporation of SIV Env into the NDV virion, allantoic fluid from infected chicken eggs was obtained at 3-day post infection (dpi) and centrifuged at 3,000 rpm for 10 min. The viruses were purified by ultracentrifugation through a 30% sucrose gradient and the pellet containing the viruses was collected and analyzed by Western blot using SIV gp120-specific mAb.
Analysis of SIV gp160 protein oligomers formation
The formation of oligomers of SIV gp160 expressed by recombinant NDV vectors was determined by protein cross-linking of protein, followed by Western blot analysis27. Briefly, monolayers of DF-1 cells were infected with 0.1 MOI of different rNDVs expressing SIV gp160 and rLaSota. After 24 h, cells were harvested and washed twice in PBS. The proteins were cross-linked using 1 mM dithiobis (succinimidyl propionate) (DSP; Pierce), a thiol-cleavable, amine-reactive, and membrane-permeative cross-linker and analyzed under reducing conditions and non-reducing conditions by SDS-PAGE and immunoblotting with gp120-specific mAbs.
Growth kinetics of rNDVs expressing SIV gp160 in DF-1 cells
The multistep growth kinetics of all the rNDVs were analyzed in DF-1 cells. Cells grown in 6-well plates were infected in duplicate with each rNDVs expressing SIV gp160 at an MOI of 0.001. Supernatant (200 μl) was collected at 8 h intervals until 64 h post infection (hpi). Virus titers in the supernatants were quantified in DF-1 cells by limiting dilution and expressed as 50% tissue culture infective dose per milliliter (TCID50/ml)28.
Pathogenicity of rNDVs expressing SIV gp160 in chicks
The pathogenicity of the different rNDVs expressing SIV gp160 was determined by the intracerebral pathogenicity index (ICPI) test in 1-day-old SPF chicks29. In the ICPI test, 0.05 ml of a 1: 10 dilutions of fresh egg-grown virus was injected into group of ten 1-day-old SPF chicks by the intracerebral route. At each 12 h observation, birds were scored 0 if normal, 1 if sick, and 2 if dead. The ICPI is the mean score per bird over 8-day observation period.
Immunization of guinea pigs
Groups of 5-week-old female guinea pigs (3 animals/group) were immunized with either the parental vector (rLaSota/gp160) or modified rNDVs expressing SIV gp160 (100 μl each of 1 × 105 TCID50) via intranasal route after xylazine and ketamine anesthesia. The control group was inoculated with rLaSota without any SIV gene. All the animals received one booster dose of immunization after 3-weeks. Blood was collected at different time intervals (days 0, 14, 21, 28, 35, 42, 49, 56 and 63). Vaginal wash samples were also collected and processed as described previously27.
Serum and mucosal antibody responses
The SIV gp160 specific antibody responses were analyzed using enzyme-linked immunosorbent assays (ELISAs). ELISA plates (96 well), were coated overnight with a purified recombinant gp130 protein of SIV mac239 (received from NIH AIDS Reagent Program, Division of AIDS, NIAID, NIH)30 at a concentration of 1 μg/ml in 100 μl volume/well, in sodium carbonate-bicarbonate buffer (pH 9.8). The plates were then blocked with 3% skim milk and 2% sucrose27. Serum samples or vaginal wash samples were diluted in dilution buffer (Zoetis Inc, Kalamazoo, MI) and added to the plates. The plates were incubated for 1 h with a 1:1000 dilution of an isotype-specific secondary antibody, horseradish peroxidase (HRP)-conjugated goat anti-guinea pig IgG (Seracare, Millford, MA), goat anti-guinea pig IgG1, goat anti-guinea pig IgG2a (Novus Biologicals, Littleton, CO), or sheep anti-guinea pig IgA (Immunology Consultants Laboratory, Newberg, OR). After washing, the plates were developed with ABTS (2,2′-azinobis [3-ethylbenzothiazoline-6-sulfonic acid]-diammonium salt) peroxidase substrate solution (Zoetis Inc, Kalamazoo, MI). The plates were analyzed at 405 nm using an ELISA plate reader.
Virus neutralization assay
Neutralizing antibody levels were measured using a pseudovirus based assay in TZM-bl cells31. Envelope pseudotyped viruses of tier 1 A SIVmac251.6, tier 1B SIVmac251/M766 strains and tier 2 SIVmac239CS.23 were made by transfecting the appropriate plasmids in 293 T/17 cells31. Two-fold serial dilutions of heat inactivated serum samples were made in culture media and added to 96-well plates (10 μl/well). Then 200 TCID50 of pseudovirus in 40 μl volume was added to each well. After incubation for 1 h at 37 °C, TZM-bl cells were added to each well (1.5 × 104/well in 150 μl volume of culture media containing 10% heat-inactivated FBS and DEAE-dextran). Assay controls included TZM-bl cells alone (cell control) and TZM-bl cells with virus and no antibody (virus control). After 48 h incubation at 37 °C, the medium was removed from each well and replaced with 50 μl of RPMI 1640 medium (Invitrogen) and 50 μl of BriteLite plus Reagent (Perkin Elmer). The cells were lysed for 2 min and 100 μl of cell lysate was transferred to a 96-well black microtiter plate, and luminescence was measured. The 50% inhibitory dose (ID50) titer was measured.
Ethics Statement
All the animal experiments were conducted in our Bio Safety Level-2 + facility according to the protocols approved by Institutional Animal Care and Use Committee of the University of Maryland.
Results
Generation of rNDVs expressing SIV gp160
The transcription cassette containing the ORF of SIV mac239 gp160 gene was inserted between the P and M genes as an additional gene-cassette into the antigenomic cDNA of lentogenic NDV strain LaSota and other modified NDV vectors (Fig. 1). All the rNDVs were recovered by standard reverse genetic technique24. The designation of each rNDV carrying SIV mac239 gp160 gene is described in Fig. 1. The recovered viruses were passaged 10 times in 9-day-old chicken eggs and the presence of the foreign gene was confirmed by sequence analysis.
Expression of SIV gp160 protein by rLaSota and modified rNDVs
To detect expression of the SIV gp160, DF-1 cell monolayers were infected with rLaSota and modified rNDVs containing SIV gp160 gene. DF-1 cell lysates were analyzed by Western blot using gp120 specific mAb. All the rNDVs expressed the cleaved gp160 Env protein of 120 kDa in size (Fig. 2). The densitometric analysis (data not shown) revealed that the level of gp160 expressed by different rNDVs varied slightly, with modified-rNDV-LaSota-527/gp160 showing highest level of expression followed by modified-rNDV-AKO-331-390/gp160. To determine the incorporation of SIV gp160 into NDV particle, the allantoic fluid harvested from eggs infected with rNDVs was ultracentrifuged through a 30% sucrose cushion and the purified virus was analyzed by Western blot using gp120-specific mAb (Fig. 3). Western blot analysis showed that SIV gp160 was incorporated into NDV particle. The insertion of SIV gp160 gene into the rNDV genome did not alter the expression of HN protein present on NDV envelope, as shown by similar levels of HN protein expression by all rNDVs.
Incorporation of the SIV gp160 into rNDV particles. The allantoic fluid containing each virus was harvested from eggs and passed through 30% sucrose cushion. The sedimented virus was suspended in PBS and used for Western blot analysis. Monoclonal antibodies specific to SIV gp160 and NDV HN were used to detect these proteins. Molecular weight of the detected virus proteins (in kDa) are shown.
Oligomer formation of SIV gp160 expressed by rNDV
The envelope protein of SIV assembles to form noncovalent associated oligomers. The oligomeric complex plays an important role in virus entry and is the major target of the neutralizing antibodies23. Hence, we determined the oligomerization of the gp160 expressed by different modified NDV vectors in infected DF-1 cells. Cell lysates from NDV-infected DF-1 cells were cross-linked with DSP followed by SDS-PAGE analysis in reducing and non-reducing conditions followed by Western blotting with gp120-specific antibodies. The presence of oligomers of higher molecular weight (>220 kDa) under nonreducing conditions and monomers (120 kDa) under reducing conditions is shown in Fig. 4. These results suggest that rLaSota and modified rNDVs support the expression of SIV gp160 as one predominant oligomer of size greater than 220 kDa.
Oligomer formation of of SIV-1 gp160. Lysates of DF-1 cells infected with modified rNDVs expressing SIV gp160 were cross-linked with DSP and analyzed by SDS-PAGE under reducing (−) or non-reducing (+) conditions. Monomeric gp120 and oligomeric gp160 (shown on right margin) expressed by different rNDV vectors were detected after immunblotting with SIV gp120-specific monoclonal antibodies. Two gels were run so as to include all the 18 lysates of infected DF1 cells.
Biological characterization of rNDV expressing gp160
The growth kinetics of the rLaSota and modified rNDVs expressing SIVgp160 were compared in DF-1 cells (Fig. 5). Compared to parental rLaSota without any insert, the replication of rLaSota and modified rNDVs containing SIVgp160 gene was reduced. Although there were differences in the growth kinetics of modified rNDVs, all the viruses containing the SIVgp160 gene insert reached to similar titers at 64 h post infection. The pathogenicities of modified NDVs expressing SIVgp160 and the parental rLaSota virus was evaluated by the ICPI test in 1-day-old chicks. The ICPI values of all rNDVs and modified rNDVs were 0.00 suggesting that wild-type rNDV and modified rNDVs expressing SIVgp160 are avirulent and the insertion of foreign gene had no major effect on virus growth and pathogenicity.
In Vitro growth kinetics of rLaSota and modified rNDV vectors expressing SIV gp160 in DF-1 cells. DF-1 Cells were infected with their respective viruses at 0.001 MOI, in the presence of 10% fresh chicken egg allantoic fluid and 2% FBS. Cell culture supernatant samples were harvested every 8 h intervals until 64 h post infection and titrated by TCID50 assay in DF-1 cells. The graph shows the geometric mean ± standard error of the mean (SEM) of TCID50 values.
Evaluation of humoral immune responses in guinea pigs
Nine groups of female Hartley guinea pigs (n = 3) were immunized on days 0 and 21 with rLaSota and modified rNDVs expressing SIV gp160 via intra nasal route. The animals in all the groups remained healthy without any clinical signs. The induction of SIV Env-specific total IgG, IgG1 and IgG2a in serum was measured in all groups on days 14, 21, 28, 35, 42, 49, 56, and 63 by ELISA (Fig. 6). Barring rNDV-LaSota control group, Env-specific antibody responses were detected on day 14 in all the groups. The total IgG, IgG1 and IgG2a antibody responses increased between days 28 and 42 in all groups. Total IgG response peaked on day 56 before decreasing on day 63. The IgG1 responses decreased on day 49 in all groups except in rNDV-LaSota-gp160 and in modified-527-AKO271-330/gp160 groups and peaked on day 56 before decreasing on day 63. Similarly, IgG2a responses decreased on day 49 and increased on day 56 except the wild type rNDV group. The gp160-specific IgG response observed with the modified-rNDV-APMV2-CS/gp160, modified-rNDV-BC-F-HN/gp160 and modified rNDV-APMV8-CS/gp160 groups were significantly higher than rNDV-LaSota gp160 group. The highest IgG titer was observed in modified-rNDV-APMV2-CS/gp160 group. The antibody titers in other groups were slightly higher than the rLaSota group. These results indicated that SIV Env-specific IgG responses could be enhanced by using Modified-rNDV-APMV-2-CS/160, Modified-rNDV-APMV-8-CS/160 and Modified-rNDV-BC-F-HN/160 vectors.
Serum antibody responses against SIV gp160 in guinea pigs. Serum samples (1:1000), collected from immunized guinea pigs at the indicated time point, were analyzed for anti-SIV gp120 antibodies using ELISA. Arrows indicate times of rNDV immunizations on days 0 and 21. The geometric mean ± standard error of the mean (SEM) for 3 animals/group are shown in each graph.
Evaluation of mucosal immune responses in guinea pigs
Vaginal wash samples were evaluated for antibody responses by ELISA using SIV gp130-coated plates (Fig. 7). Very low total IgG, IgG1 and IgG2a antibody titers were detected on day 21, but the antibody responses increased significantly in all groups after the boost except in the rNDV-LaSota control group. The titer of total IgG, IgG1 and IgG2a were highest between days 28 and 63. Similar to IgG responses in serum, the response was highest in the modified-rNDV-APMV2-CS/gp160 group.
Mucosal antibody responses against SIV gp160 in guinea pigs. Vaginal wash samples collected from guinea pigs at indicated time points were diluted in PBS (1:10) and analyzed by ELISA for SIV gp120-specific antibodies. Arrows indicate times of rNDV immunizations on days 0 and 21. The geometric mean ± standard error of the mean (SEM) for 3 animals/group are shown in each graph.
Evaluation of neutralizing antibody responses in guinea pigs
Serum samples were evaluated for neutralization titer against tier 1 A SIVmac251.6, tier 1B SIVmac251/M766 and tier 2 SIVmac239CS.23 HIV strains on days 35, 49, and 63 by TZM.bl assay (Fig. 8). Neutralizing antibody (nAb) titer (expressed as ID50) was detected against SIVmac251.6 in all groups with the highest ID50 values in modified-rNDV-APMV2-CS/160 group on days 35, 49 and 63 followed by modified-rNDV-BC-F-HN/gp160 group on days 35 and 49 and modified rNDV-APMV8-CS/160 group on day 63. The nAb response in the modified-rNDV-APMV2-CS/160 group peaked on day 35. The nAb activity detected against SIVmac251/M766 was higher in the rNDV-APMV8-CS/160 group followed by modified-rNDV-APMV2-CS/160 and modified-rNDV-BC-F-HN/gp160. A very low response to tier 2 SIVmac239CS.23 was detected, consistent with the highly neutralization-resistant phenotype of this virus32. The nAb response to SIVmac251.6 was significantly higher than the response to SIVmac251/M766 in all the guinea pig groups.
Neutralizing antibody activity represented as ID50 (50%-inhibitory-dilution) against heterologous tier 1 A SIV mac251.6, tier 1B SIV mac 251/M766 and homologous tier 2 strain SIV mac239cs.23. Serum samples from immunized guinea pigs were obtained on days 35, 49 and 63 and tested for neutralization of pseudoviruses by the TZM-bl assay. Serum obtained from negative control group (rNDV-LaSota-Control) was used as as an indicator of background signal. The dashed lines denote background titers of <20. The Statistical significance between different groups were compared to serum samples from modified-rNDV-APMV2-CS/gp160, which showed highest neutralizing antibody titers, with Tukey’s multiple comparison test. The geometric mean ± standard error of the mean (SEM) for the 3 animals/group are shown in each graph. *P value < 0.05; **P value < 0.005; ***P value < 0.001 are indicated on each graph.
Discussion
We have previously shown that lentogenic NDV strain LaSota expressing HIV-1 Env protein gp160 induces strong mucosal and serum antibody responses in guinea pigs27. In another study we used the NDV strain LaSota to compare the biochemical immunological characteristics of Env proteins gp160, gp140 and gp12033. We found that similar to gp160, gp140 and gp120 formed oligomers which were recognized by conformation-sensitive monoclonal antibodies. Our results showed that NDV strain LaSota expressing gp140 induced higher antibody responses compared to the other recombinants in guinea pigs. We have also shown that immunization of guinea pigs with NDV strain LaSota co-expressing Env and Gag proteins elicited potent immune responses to HIV17. All the above studies showed that lentogenic strain LaSota is a promising vaccine vector for HIV. However, these results need to be confirmed in a relevant animal model in which challenge studies can be performed. Therefore, in this study we have expressed SIV Env protein using several NDV vectors and compared their immune responses in guinea pigs. We have identified a modified NDV vector that induces higher antibody responses in guinea pigs. This vector needs to be evaluated in macaques by SIV challenge.
In this study, we have used rNDV as a vaccine vector for SIV Env protein because of several reasons16. NDV is antigenically distinct from human pathogens. Most humans are not exposed to NDV and hence there is no pre-existing immunity. NDV grows in Vero cell line which is certified for vaccine production. Vaccines derived from NDV vectors can be given nasally and can induce effective humoral and mucosal immune responses. NDV has an intrinsic immune-modulatory property for the induction of efficient immune responses. Compared to lentogenic strains, mesogenic strains of NDV have been found to mount an effective immune response in non-human primates21. However, mesogenic strains are Select Agents and must be handled in BSL-3 facility which makes development and testing of mesogenic NDV vectors challenging. Therefore, in this study, the polybasic F cleavage site of mesogenic strain BC was modified to the dibasic F cleavage site of lentogenic strain LaSota. The change in F cleavage site reduced the virulence of mesogenic strain BC suggesting that it has the potential to be used as a vaccine vector. Changing the F protein cleavage site of lentogenic strain LaSota to those of APMV-2, 7 and 8 also eliminated the need for exogenous protease supplementation, while still containing avirulent F protein cleavage site. These modifications were done to improve the replication ability of strain LaSota and hence enhance its usage as a vaccine vector. The modified viruses were avirulent by ICPI test and induced higher levels of immune responses against SIV Env protein in guinea pigs.
Several reports have shown that an effective neutralizing antibody response conferred protection against HIV in different animal models. However, non-neutralizing antibodies also played a significant role in decrease of incidence of HIV-1 infection in phase III RV144 vaccination trial7,8. In this study, we have developed several modified rNDV vectors and have used these vectors to express SIVgp160 mac239 envelope protein. The expression of SIV gp160 in DF-1 cells was higher in modified-rNDV-LaSota-527/gp160 followed by the modified-NDV-rBC vectors. Studies have shown that foreign envelope proteins expressed by rNDV gets incorporated into NDV envelopes17. In this study. We found that SIV gp160 also got inserted into the envelope of NDV particle. An important advantage of the SIV envelope protein incorporation into NDV particles is that they can effectively mount potent immune responses.
SIVmac239CS.23 and its closely related derivatives SIVmac251.6 and SIV mac251/M788 vary widely in their ability to neutralization with the same antisera34. rNDV vectors expressing SIVmac239 gp160 induces neutralizing antibodies to strain SIVmac251.6 and SIVmac251/M788 whereas the same antibodies rarely neutralize infectivity of SIVmac239CS.23. This might be due to a subset of antibodies that bound with an affinity too low to neutralize the SIVmac239CS.23. The current notion is that, more easily neutralized viruses have a more open conformation Env glycoprotein, while the Env glycoprotein of more neutralization-resistant viruses exist primarily in a more closed conformation35. The variations in the neutralization titer might be also due to the antigenic heterogeneity among different SIV strains. SIV infects diverse hosts and it is possible that the virus evolves having its own neutralizing determinants32. SIVmac239CS.23 was remarkably resistant to neutralization even with homologous anti-sera induced by our rNDV vectors. It could be due distinct molecular determinants of neutralization of this virus strain compared to SIVmac251.6 and SIV mac251/M788 virus strains36. The serum antibody levels were increasing from day 28–56 as evident by ELISA results, but the nAb titers were decreasing over time. The reduction in nAb titer over time might be due to lack of persistent infection, which is essential for the clonal selection of high-affinity antibodies. We measured levels of antibodies present in vaginal secretions, because mucosal antibodies play an important role in prevention of sexual transmission of HIV and SIV. Immunization with rNDV vectors expressing SIVgp160 elicited gp120-specific IgG in the vaginal wash samples of all of the animals. In addition, the NDV vectored SIV vaccines used in this study elicited nAbs against SIV strains different from vaccinated strain.
The major drawback of most viral vectors for vaccination is the interference of their replication after homologous virus boosting37,38. Usage of pox virus, vaccinia virus and adenovirus as viral vectors are limited by this drawback. It can be overcome by use of either heterologous viral vector or use of homologous viral vector with modifications. Therefore, we modified NDV vector in this study to test immunogenicity against SIV Env protein. Some of these modified vectors have shown improved immunogenicity and protective efficacy in prime-boost vaccination in our previous studies25,39,40. Although we have not tested these modified NDV vectors for prime-boost vaccination in this study, we expect these vectors to produce better immune responses against SIV or HIV proteins in future prime-boost vaccination studies.
In summary, we compared different modified rNDV vectors expressing SIVgp160 by prime and boost strategy for induction of serological and mucosal antibody responses to tier 1 A SIVmac251.6, tier 1B SIVmac251/M766 and tier 2 SIVmac239CS.23 strains. These rNDV vectors induced higher levels of nAbs in guinea pigs, without causing any clinical signs. Modified-rNDV-APMV2-CS/gp160 stimulated nAb response to SIVmac251/M766 at a higher magnitude than other modified vectors in guinea pigs. Previous studies have shown that SIVmac239CS is highly neutralization resistant which explains the low neutralizing titers by all the rNDV vectors32. We have identified three rNDV vectors that induced higher levels of humoral immune responses against SIV. The potential of these vectors needs to be tested in other animal models such as macaques.
References
Gallo, R. C. & Montagnier, L. The discovery of HIV as the cause of AIDS. The New England journal of medicine 349, 2283–2285, https://doi.org/10.1056/NEJMp038194 (2003).
UNAIDS. Global AIDS report, UN Joint Programme on HIV/AIDS http://www.unaids.org/sites/default/files/media_asset/global-AIDS-update-2016_en.pdf (2016).
Shedlock, D. J., Silvestri, G. & Weiner, D. B. Monkeying around with HIV vaccines: using rhesus macaques to define ‘gatekeepers’ for clinical trials. Nature reviews. Immunology 9, 717–728, https://doi.org/10.1038/nri2636 (2009).
Eugene, H. S., Pierce-Paul, B. R., Cragio, J. K. & Ross, T. M. Rhesus macaques vaccinated with consensus envelopes elicit partially protective immune responses against SHIV SF162p4 challenge. Virology journal 10, 102, https://doi.org/10.1186/1743-422X-10-102 (2013).
Pal, R. et al. Immunization of rhesus macaques with a polyvalent DNA prime/protein boost human immunodeficiency virus type 1 vaccine elicits protective antibody response against simian human immunodeficiency virus of R5 phenotype. Virology 348, 341–353, https://doi.org/10.1016/j.virol.2005.12.029 (2006).
Chea, L. S. & Amara, R. R. Immunogenicity and efficacy of DNA/MVA HIV vaccines in rhesus macaque models. Expert review of vaccines 16, 973–985, https://doi.org/10.1080/14760584.2017.1371594 (2017).
Kim, J. H., Excler, J. L. & Michael, N. L. Lessons from the RV144 Thai phase III HIV-1 vaccine trial and the search for correlates of protection. Annual review of medicine 66, 423–437, https://doi.org/10.1146/annurev-med-052912-123749 (2015).
Rerks-Ngarm, S. et al. Vaccination with ALVAC and AIDSVAX to Prevent HIV-1 Infection in Thailand. New Engl J Med 361, 2209–2220, https://doi.org/10.1056/Nejmoa0908492 (2009).
Pollara, J., Easterhoff, D. & Fouda, G. G. Lessons learned from human HIV vaccine trials. Current opinion in HIV and AIDS 12, 216–221, https://doi.org/10.1097/COH.0000000000000362 (2017).
Pal, R. et al. ALVAC-SIV-gag-pol-env-based vaccination and macaque major histocompatibility complex class I (A*01) delay simian immunodeficiency virus SIVmac-induced immunodeficiency. Journal of virology 76, 292–302 (2002).
Ura, T., Okuda, K. & Shimada, M. Developments in Viral Vector-Based Vaccines. Vaccines 2, 624–641, https://doi.org/10.3390/vaccines2030624 (2014).
Robert-Guroff, M. Replicating and non-replicating viral vectors for vaccine development. Current opinion in biotechnology 18, 546–556, https://doi.org/10.1016/j.copbio.2007.10.010 (2007).
Cooper, D. et al. Attenuation of recombinant vesicular stomatitis virus-human immunodeficiency virus type 1 vaccine vectors by gene translocations and g gene truncation reduces neurovirulence and enhances immunogenicity in mice. Journal of virology 82, 207–219, https://doi.org/10.1128/JVI.01515-07 (2008).
Johnson, J. E. et al. Neurovirulence properties of recombinant vesicular stomatitis virus vectors in non-human primates. Virology 360, 36–49, https://doi.org/10.1016/j.virol.2006.10.026 (2007).
Samal, S. K. in The Biology of Paramyxoviruses. (ed S. K. Samal) 69-114 (Caister Academic Press, Norfolk, UK., 2011).
Kim, S. H. & Samal, S. K. Newcastle Disease Virus as a Vaccine Vector for Development of Human and Veterinary Vaccines. Viruses 8, https://doi.org/10.3390/v8070183 (2016).
Khattar, S. K. et al. Mucosal Immunization with Newcastle Disease Virus Vector Coexpressing HIV-1 Env and Gag Proteins Elicits Potent Serum, Mucosal, and Cellular Immune Responses That Protect against Vaccinia Virus Env and Gag Challenges. mBio 6, ARTN e01005-1510.1128/mBio.01005-15 (2015).
Khattar, S. K. et al. Enhanced Immune Responses to HIV-1 Envelope Elicited by a Vaccine Regimen Consisting of Priming with Newcastle Disease Virus Expressing HIV gp160 and Boosting with gp120 and SOSIP gp140 Proteins. Journal of virology 90, 1682–1686, https://doi.org/10.1128/Jvi.02847-15 (2016).
Kong, D. et al. Newcastle disease virus-vectored Nipah encephalitis vaccines induce B and T cell responses in mice and long-lasting neutralizing antibodies in pigs. Virology 432, 327–335, https://doi.org/10.1016/j.virol.2012.06.001 (2012).
Khattar, S. K., Collins, P. L. & Samal, S. K. Immunization of cattle with recombinant Newcastle disease virus expressing bovine herpesvirus-1 (BHV-1) glycoprotein D induces mucosal and serum antibody responses and provides partial protection against BHV-1. Vaccine 28, 3159–3170, https://doi.org/10.1016/j.vaccine.2010.02.051 (2010).
DiNapoli, J. M. et al. Newcastle disease virus-vectored vaccines expressing the hemagglutinin or neuraminidase protein of H5N1 highly pathogenic avian influenza virus protect against virus challenge in monkeys. Journal of virology 84, 1489–1503, https://doi.org/10.1128/JVI.01946-09 (2010).
Patterson, L. J. et al. Potent, persistent induction and modulation of cellular immune responses in rhesus macaques primed with Ad5hr-simian immunodeficiency virus (SIV) env/rev, gag, and/or nef vaccines and boosted with SIV gp120. Journal of virology 77, 8607–8620 (2003).
Luke, W. et al. Simian immunodeficiency virus (SIV) gp130 oligomers protect rhesus macaques (Macaca mulatta) against the infection with SIVmac32H grown on T-cells or derived ex vivo. Virology 216, 444–450, https://doi.org/10.1006/viro.1996.0082 (1996).
Huang, Z. H., Krishnamurthy, S., Panda, A. & Samal, S. K. High-level expression of a foreign gene from the most 3′-proximal locus of a recombinant Newcastle disease virus. Journal of General Virology 82, 1729–1736 (2001).
Kim, S. H., Paldurai, A., Xiao, S., Collins, P. L. & Samal, S. K. Modified Newcastle disease virus vectors expressing the H5 hemagglutinin induce enhanced protection against highly pathogenic H5N1 avian influenza virus in chickens. Vaccine 32, 4428–4435, https://doi.org/10.1016/j.vaccine.2014.06.061 (2014).
Manoharan, V. K., Khattar, S. K., Paldurai, A., Kim, S. H. & Samal, S. K. A Y527A mutation in the fusion protein of Newcastle disease virus strain LaSota leads to a hyperfusogenic virus with increased replication and immunogenicity. The Journal of general virology 97, 287–292, https://doi.org/10.1099/jgv.0.000350 (2016).
Khattar, S. K., Samal, S., DeVico, A. L., Collins, P. L. & Samal, S. K. Newcastle Disease Virus Expressing Human Immunodeficiency Virus Type 1 Envelope Glycoprotein Induces Strong Mucosal and Serum Antibody Responses in Guinea Pigs. Journal of virology 85, 10529–10541, https://doi.org/10.1128/Jvi.05050-11 (2011).
Reed L, J., Muench. H. A simple method of estimating fifty per cent endpoints. The american journal of hygiene, 493–497 (1938).
Alexander, D. J. in A laboratory manual for the isolation and identification of avian pathogens (ed L. H. ARP H. G. Purchase, C. H. Domermuth & J. E. Pearson) 114–120. (American Association for Avian Pathologists, Inc., Kennett Square, PA., 1989).
Hill, C. M. et al. Envelope glycoproteins from human immunodeficiency virus types 1 and 2 and simian immunodeficiency virus can use human CCR5 as a coreceptor for viral entry and make direct CD4-dependent interactions with this chemokine receptor. Journal of virology 71, 6296–6304 (1997).
Montefiori, D. C. Evaluating neutralizing antibodies against HIV, SIV, and SHIV in luciferase reporter gene assays. Curr Protoc Immunol Chapter 12, Unit12 11, https://doi.org/10.1002/0471142735.im1211s64 (2005).
Jia, B. et al. Immunization with Single-Cycle SIV Significantly Reduces Viral Loads After an Intravenous Challenge with SIV(mac)239. Plos Pathog 5, 1000272, https://doi.org/10.1371/journal.ppat (2009).
Khattar, S. K. et al. Comparative Immunogenicity of HIV-1gp160, gp140 and gp120 Expressed by Live Attenuated Newcastle Disease Virus Vector. PloS one 8, 0078521, https://doi.org/10.1371/journal.pone (2013).
Wu, Z., Qian, G., Zhen, Q. L., Narayan, O. & Stephens, E. B. Neutralization of SIVmac239/17E in lymphocyte cultures involves virus strain-specific linear and conformational epitopes encoded by different regions of the env gene including the “V3” domain. Virology 222, 184–192 (1996).
Guttman, M. et al. Antibody potency relates to the ability to recognize the closed, pre-fusion form of HIV Env. Nature communications 6, 6144, https://doi.org/10.1038/ncomms7144 (2015).
Moore, J. P. et al. Primary isolates of human immunodeficiency virus type 1 are relatively resistant to neutralization by monoclonal antibodies togp120, and their neutralization is not predicted by studies with monomeric gp120. Journal of virology 69, 101–109 (1995).
Cooney, E. L. et al. Safety of and immunological response to a recombinant vaccinia virus vaccine expressing HIV envelope glycoprotein. Lancet 337, 567–572 (1991).
Papp, Z., Babiuk, L. A. & Baca-Estrada, M. E. The effect of pre-existing adenovirus-specific immunity on immune responses induced by recombinant adenovirus expressing glycoprotein D of bovine herpesvirus type 1. Vaccine 17, 933–943 (1999).
Kim, S. H., Paldurai, A. & Samal, S. K. A novel chimeric Newcastle disease virus vectored vaccine against highly pathogenic avian influenza virus. Virology 503, 31–36, https://doi.org/10.1016/j.virol.2017.01.006 (2017).
Kim, S. H. & Samal, S. K. Heterologous prime-boost immunization of Newcastle disease virus vectored vaccines protected broiler chickens against highly pathogenic avian influenza and Newcastle disease viruses. Vaccine 35, 4133–4139, https://doi.org/10.1016/j.vaccine.2017.06.055 (2017).
Acknowledgements
We thank Laura Sanglas Crespi and other laboratory members for their technical assistance and help. We thank Girmay Gebreluul and Yonas Araya for their help with handling of guinea pigs.
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: Vinoth K. Manoharan, Sunil K. Khattar and Siba K. Samal. Performed the experiments: Vinoth K. Manoharan and Sunil K. Khattar. Serum neutralization assay: Celia C. LaBranche, David C. Montefiori Analyzed the data: Vinoth Manoharan. Contributed reagents/materials/analysis tools: Siba Samal. Wrote the paper: Vinoth Manoharan, Sunil Khattar and Siba Samal.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Manoharan, V.K., Khattar, S.K., LaBranche, C.C. et al. Modified Newcastle Disease virus as an improved vaccine vector against Simian Immunodeficiency virus. Sci Rep 8, 8952 (2018). https://doi.org/10.1038/s41598-018-27433-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-27433-x
This article is cited by
-
The phosphatase and tensin homolog gene inserted between NP and P gene of recombinant Newcastle disease virus oncolytic effect test to glioblastoma cell and xenograft mouse model
Virology Journal (2022)
-
Viruses as tools in gene therapy, vaccine development, and cancer treatment
Archives of Virology (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.