Abstract
Aim of this study was to evaluate the effect of cervical spondylosis surgery on cervical lordosis and to identify factors affecting the change by latest follow-up. Literature search was carried out in electronic databases and study selection followed a priori eligibility criteria. Random effects meta-analyses were performed to estimate effect size/s of change in lordosis after surgery (at latest follow-up) and metaregression analyses were performed to identify factors affecting this change. Nineteen studies (1845 patients; age 55.18 [95% CI: 54.78, 55.57] years; 60.99 [60.63, 61.36] % males; follow-up 25.59 [25.20, 25.99] months) were included. Whereas, corpectomy (4.06 [2.65, 5.46] degree; p < 0.00001) and discectomy (4.59 [2.07, 7.11] degree; p < 0.00001) were associated with increase, laminectomy (−1.87 [−8.40, 4.66] degree; p = 0.57) and laminoplasty (0.25 [−1.07, 1.56] degree; p = 0.711) were not associated with significant change in lordosis at latest follow-up. Change in Japanese Orthopedic Association (JOA)/modified JOA (mJOA) score at latest follow-up was also significantly (p = 0.0005) higher in anterior than in posterior surgery group. Change in lordosis at latest follow-up had significant positive relationship with follow-up duration but had significant inverse associations with age, male gender, and preoperative JOA/mJOA score, independently. In posterior surgery subjects, after adjusting for age and gender, preoperative JOA/mJOA score was significantly inversely related to change in lordosis.
Similar content being viewed by others
Introduction
Cervical spondylosis is the osteoarthritic degeneration of cervical spine components such as uncovertebral and facet joints and intervertebral discs causing several motor and sensory dysfunctions. Pathophysiology is multi-factorial that may include the formation of osteophyte and/or chondro-osseous spurs, disc herniation, and hypertrophy of facet joints and/or ligaments which affect canal diameter and sagittal mobility1,2,3.
Cervical spondylosis manifests as myelopathy, radiculopathy or radiculomyelopathy which requires radiological diagnosis4,5,6. Symptoms may include weakness, gait instability, decreased dexterity, gut and urinary problems, spasticity, axial pain in the neck and arm regions, headache, blurred vision, tinnitus, palpitations, hypomnesia, and facial flushing and sweating7, 8.
Conservative management is usually restricted to cases with mild and moderate symptoms9, 10 and more serious cases require surgery involving either anterior, posterior, or circumferential decompression11, 12 depending on number of diseased segments, sagittal alignment, stenosis morphology, history of prior surgery, and bone quality1. Early surgical intervention has potential for the prevention of significant morbidity and mortality in patients with progressive instability and neurologic deficit13.
A large number of studies have reported the outcomes of various surgical interventions in cervical spondylotic myelopathy and/or radiculopathy patients with follow-up of up to 15 years. Although, many of these studies have also reported outcomes with regards to the change in cervical lordosis but variability in the effect size provides impetus for a systematic review to refine the evidence. There is no previous systematic review of studies which examined the change in lordosis after surgical intervention. Therefore, aim of the present study was to carry out a systematic review of relevant studies and to perform a meta-analysis of the of the change in lordosis and neurological outcomes at the latest follow-up reported in individual studies and to identify the factors affecting the change in cervical lordosis.
Method
This study was performed by following the Cochrane Collaboration’s guidelines14 and is reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) statement15.
Eligibility, meta-analysis endpoint and metaregression analysis variables
Eligible studies of this meta-analysis were those reporting the outcomes of surgical intervention/s in cervical spondylosis patients with a follow-up duration of at least one year and measured change in lordosis preoperatively, after surgery and at latest follow-up.
Meta-analysis endpoints (outcome measures) were: a) the change in lordosis from baseline through the latest follow-up, and b) the change in Japanese Orthopedic Association (JOA)/ modified JOA (mJOA) score from baseline through the latest follow-up. For metaregression analyses, change in lordosis at the latest follow-up (dependent variable) was tested to evaluate the relationships with several explanatory variables including the number of subjects in a study, follow-up duration, age of subjects at the time of surgery, gender (percentage of males), disease duration, percent smokers, percent patients with myelopathy, or radiculopathy, or radiculomyelopathy, percentage of 1, 2, 3, or >3 levels involved, duration of surgery, blood loss during surgery, hospital stay duration, percent incidence of surgical complications, preoperative JOA/mJOA score, preoperative NDI score, preoperative lordosis, preoperative range of motion (ROM), and preoperative neck/arm visual analogue scale (VAS) score.
Data acquisition
For the acquisition of required data, literature search was undertaken in electronic databases including Embase, Google Scholar, Ovid SP, and PubMed/Medline. For primary search, ‘cervical-spondylosis-surgery’, ‘cervical-spondylotic-myelopathy-surgery’, ‘cervical-spondylotic-radiculopathy-surgery’ and ‘cervical-spondylotic radiculomyelopathy-surgery’ combinations were used. For secondary searches, each of the primary combination was used with several MeSH and keywords including cervical lordosis, cervical curvature, arthroplasty, corpectomy, discectomy, laminectomy, and laminoplasty. Search encompassed original research articles published before October 2015. Additional searches included the bibliographies of retrieved research articles and software suggestions based on retrieved articles.
Data and analyses
Relevant data including the patients’ demographic/clinical/orthopedic characteristics, surgery type/technique, study population and follow-up characteristics, study design and analyses, outcome assessment and outcomes, and perioperative data were obtained from the retrieved research articles and organized in specialized datasheets.
For the estimation of effect size of the change in lordosis by the latest follow-up, data were either extracted raw from the respective research articles, if provided, or calculated by using baseline and final values given in the study reports. Inverse variance weighted effect sizes of overall (all surgical interventions) and subgroups (surgery type-wise) were obtained under random effects meta-analyses which were carried out in Stata software (version 12; Stata Corporation, College Station, Texas).
Metaregression analyses were also carried out with Stata software by using restricted maximum likelihood (ReML) method. A p value of less than 0.05 was considered to show a significant relationship. Between-study variance was tested with tau2 index and the percentage of between-study heterogeneity (outcome inconsistency) was assessed with I2 index. Publication bias assessment was carried out with Begg’s funnel plot asymmetry test of meta-analysis of the change of lordosis at the latest follow-up and trim and fill method was used to estimate the number of possible missing studies.
Results
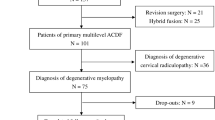
Nineteen studies (1845 patients) were selected for data acquisition16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34 by following the eligibility criteria (Fig. 1). Majority of the included studies had more than one arms and thence the number of datasets attained was 35. There was no significant publication bias (Begg’s Test: adjusted Kendall’s Score (P-Q) = −79 ± 70.42; p = 0.268). Trim and fill method also did not find a significant number of missing studies (Fig. 2).
Important characteristics of the included studies are presented in Table S1 (Supporting information file. Average follow-up duration was 25.59 [95% CI: 25.20, 25.99] (range 12 to 102) months. Average age of the subjects at the time of surgery was 55.18 [54.78, 55.57] years and 60.99 [60.63, 61.36] % of these subjects were male. Average disease duration in these subjects was 27.14 [25.46, 28.83] months. Percentage of subjects with 1, 2, 3, 4 or more than 4 cervical levels involved in surgery were 28 ± 37%, 23 ± 32%, 36 ± 42%, 11 ± 16% and 2 ± 10%, respectively.
Overall, duration of surgery, blood loss during surgery, and hospital stay duration were 133.65 [132.17, 135.14] minutes, 78.86 [75.37, 82.35] milliliter, and 4.41 [4.17, 4.66] days, respectively. There was a significant correlation between the duration of surgery and blood loss (r = 0.657; p < 0.0028), but not between duration of surgery and hospital stay (r = 0.306; p = 0.216), or between blood loss and hospital stay (r = 0.355; p = 0.17).
Change in lordosis and JOA/mJOA score after cervical spondylosis surgery
Overall, there was a significant difference between anterior and posterior approaches to surgical interventions in changing postoperative lordosis at the latest follow-up (p < 0.00001). Whereas, corpectomy and discectomy were associated with an increase of 4.06 [95% confidence interval: 2.65, 5.46] (p < 0.00001) and 4.59 [2.07, 7.11] degrees (p < 0.00001) respectively, laminectomy (−1.87 [−8.40, 4.66]; p = 0.57) and laminoplasty (0.25 [−1.07, 1.56]; p = 0.711) were not associated with significantly changed lordosis angle at the latest follow-up (Fig. 3).
Improvement in JOA/mJOA score at the latest follow-up was also significantly (p = 0.0005) higher in anterior surgery (4.08 [3.49, 4.66]; p < 0.00001) than in posterior surgery (2.75 [2.03, 3.48]; p < 0.00001; Fig. 4). Change is JOA/mJOA score at latest follow-up was significantly correlated with the change in lordosis at the latest follow-up (r = 0.575; p = 0.002).
Both the preoperative lordosis and preoperative JOA/mJOA score were not significantly different between anterior and posterior surgery subjects.
None of the included studies reported SF-36 related patient outcomes; one study used Core Outcome Measures Index (COMI) and four studies used Odom grading for the assessment of patient rating of the surgical outcomes. Overall percentage of patients rating the outcomes as excellent or good was 82.05 [78.05, 86.06] % for anterior surgery (Fig. 5). No data were available with regards to patient-related outcomes for posterior surgery interventions.
Forest graph showing the overall effect size of patients reported outcomes of the surgery with anterior approaches. ACCF, anterior cervical corpectomy and fusion; ACDF, anterior cervical decompression and fusion; COMI, Core Outcome Measures Index; Odom, Odom grading system; PEEK, polyetheretherketone cage; TIT, titanium cage.
Prognostic factors of change in postoperative lordosis at the latest follow-up
Change in lordosis had a significant positive relationship with the follow-up duration in both anterior (coefficient: 0.058; p = 0.047) and posterior (coefficient: 0.191; p = 0.040) surgical approaches as well in overall surgical interventions (coefficient: 0.085; p = 0.004).
Age was inversely associated with the change in lordosis in overall cervical surgical interventions (coefficient: −0.338; p = 0.005) but not in either anterior surgery (coefficient: −0.204; p = 0.235) or in posterior surgery (coefficient: −0.114; p = 0.595) subgroups. In the overall surgical interventions, percentage of males was inversely associated with the change in lordosis (coefficient: −0.117; p = 0.022) as well as in posterior surgery (coefficient: −0.182; p = 0.057) group. But gender was not significantly associated with the change in lordosis in anterior surgery (coefficient: 0.0009; p = 0.990).
Preoperative JOA/mJOA score was inversely associated with the change in lordosis in the overall surgical interventions (coefficient: −1.301; p = 0.017) as well as in posterior surgery (coefficient: −1.371; p = 0.006) group. However, preoperative JOA/mJOA score was not significantly associated with the change in lordosis in anterior surgery (coefficient: −0.505; p = 0.441).
Change in lordosis at the latest follow-up did not have significant relationship with the preoperative lordosis neither in anterior (coefficient: 0.067; p = 0.696) nor in posterior (coefficient: −0.228; p = 0.389) surgery groups or in overall surgical interventions (coefficient: −0.119; p = 0.445). Neither the percentage of patients with myelopathy, nor radiculopathy or radiculomyelopathy had significant relationships with the change in lordosis at latest follow-up.
In multivariate analyses, none of the independent variables (age, gender or preoperative JOA/mJOA score) was significantly associated with the change in lordosis at the latest follow-up in overall surgical interventions as well as in anterior surgery group. However, in posterior surgery group, preoperative JOA/mJOA score (coefficient: −1.162; p = 0.037) was significantly inversely related to the change in lordosis in multivariate analyses with covariates of age, gender and preoperative JOA/mJOA score.
All outcomes of metaregression analyses are presented in Tables S2–S4.
Discussion
Anterior surgical approaches are found to be associated with significant increase in lordosis, whereas there was no significant change in lordosis after posterior surgical approaches. Both the surgical approaches were associated with significantly improved JOA/mJOA scores but improvement in JOA/mJOA score was significantly higher in anterior surgery group at latest follow-up. Independently, the change in lordosis had a positive relationship with follow-up duration but had independent inverse relationship with age, percentage of males, and preoperative JOA/mJOA score. However, neither age or gender nor preoperative JOA/mJOA scores were significantly associated with change in lordosis in anterior surgery group. In posterior surgery group, whereas, male gender and preoperative JOA/mJOA score had significantly inverse independent relationships with the change in lordosis but after adjusting for age and gender, only preoperative JOA/mJOA score was inversely associated with the change in lordosis at latest follow-up.
Cervical lordotic curvature can be observed as early as 10 weeks of fetal development arising by the posterior wedging of the cervical disks35, 36. In asymptomatic individuals, average cervical lordosis is reported variably; 21.337, 22.338 and 3439 degrees, depending on the method used to measure the curvature. No significant sex differences are noted but increase in lordosis with age is evident37, 40. Cervical lordotic curvature distributes the compressive load differently from rest of the spine; 36% of compressive load is transmitted through the anterior column and 64% through the posterior facet joints41, 42.
Configuration of the sagittal cervical curve has important clinical implications43,44,45. Attainment of the depth of cervical lordosis is reported to be an important factor in achieving better surgical outcomes in patients with neurologic deficits46,47,48,49,50, and therefore, rehabilitation of cervical lordosis is considered as an important part of treatment as the compression of nervous tissue can be injurious otherwise51.
McAviney et al.52 have found increase in the number of cervical complaints below 31 and above 40 degree of cervical lordosis. They have also noticed that patients with straight and/or kyphotic cervical curves were 18 times more likely to report symptoms. A statistically significant association has also been found between cervical lordosis of less than 20 degree and cervical pain52. Harrison et al.53 have reported that chronic pain was associated with lowest lordotic curves in 70 patients with chronic neck pain. Studies have also found an association between depth of cervical lordosis and chronic headache54, 55. Several researchers have reported that neurologic improvement is associated with posterior shift of the spinal cord and for this to happen, lordotic alignment of the cervical spine is essential to allow the spinal cord to shift dorsally46, 56, 57.
In the present study, we have found that improvement in JOA/mJOA score at the latest follow-up was significantly higher in patients who underwent discectomy and corpectomy in comparison with posterior surgery subjects which was associated with significantly higher change in lordosis in the anterior surgery subjects. In a previous meta-analysis comparing anterior decompression and fusion with laminoplasty in the treatment of multilevel cervical ossification of posterior longitudinal ligament, laminoplasty group was found to have significantly reduced postoperative cervical lordosis which was also associated with late deterioration of neurological function58, 59.
In the present study, higher changes in surgical outcomes are seen in individuals with more severe disease conditions preoperatively e.g. change in JOA score at latest follow-up was strongly inversely associated with the preoperative JOA/mJOA score (coefficient: −0.74; p = 0.00001). There was also a significant positive correlation between the change in JOA/mJOA score and change in lordosis (r = 0.575; p = 0.002) at the latest follow-up. Similarly, there was significant inverse correlation between the change in lordosis and change in neck VAS score (r = −0.591; p = 0.0158) at the latest follow-up. This may suggest that surgery is better equally for patients with moderate or severe conditions. Whether patients with less or moderate conditions may be advised to seek non-surgical treatments first should depend on the availability and suitability of non-surgical treatment options and risks involved.
Success of cervical laminectomy as well as laminoplasty is determined by the presence of lordosis angle of at least 10 degrees and the preservation of at least 50% facet joints60, 61. Laminoplasty involves two distinct effects; a direct effect of posterior decompression and an indirect effect of anterior decompression due to posterior shift of the spinal cord from anterior compressive lesions62 and therefore, is considered as a useful alternative. However, laminoplasty is associated with poor clinical outcomes in the presence of kyphotic or S-shaped cervical spine malalignment owing to the prevention of posterior shift of the spinal cord63. Although, in the present study, change in lordosis at the latest follow-up had no significant association with the degree of preoperative cervical curvature; neither in anterior nor in posterior surgery groups, data were relatively lesser for studying this effect in posterior surgery group. Moreover, it is reported that cervical lordosis does not significantly differ between asymptomatic and symptomatic individuals and there is considerable inter-individual variation in the lordotic degree of the spinal spine55, 64.
In the present study, it was not possible to examine the effect of surgical interventions on the cervical range of motion owing to the unavailability of adequate data. However, in a separate meta-analysis of 36 studies, we have found that not only the cervical ROM decrease significantly after spondylosis surgery but also there was a significant positive relationship between decrease in ROM and follow-up duration (unpublished data). Other studies have also reported decrease in ROM after cervical spondylosis surgery65, 66.
In the present study, only a few studies reported adjacent segmental complications a synthesis of which revealed approximately 4.1 ± 2.7% incidence. Among other notable surgery-related adverse events included implant dislodgement (5.7 ± 5.1%), dysphagia (11.2 ± 8.4%), dysphonia (7 ± 4.4%), hematoma (2.2 ± 1.4%), CSF leakage (3.4 ± 5.7%), nerve palsy (5.12 ± 4.6%), and neurological complications (5 ± 3.6%). Previously, it is reported that the majority of complications with cervical spondylosis surgery are well-manageable and have no long-term impact67. However, an increased risk of complications has been found to be associated with later age, higher operative time, and combined anterior-posterior procedures67.
Among the limitations of the present study, one constraint was that relatively lesser data regarding the quality of life after surgery and at follow-ups were available. None of the studies measured SF36 PCS/MCS scores. There can also be some impact of the lordosis measurement method as it is found that Cobb method slightly underestimates cervical lordosis than posterior tangent method53. In the individual studies of the present meta-analysis, all investigators measured lordosis by using Cobb method. Use of the random effects model for the meta-analyses may also affect the precision of effect sizes. However, it was necessary to choose because of the inclusion of more heterogenous populations with majority of the studies were retrospective in design. Because, among the included studies, 2 were randomized controlled, 2 were prospective non-randomized and rest were retrospective in design, the present study was also hampered by the avoidance of the quality assessment with a single tool.
Conclusion
Cervical spondylosis surgery is found to be associated with significant increase in lordosis as well as JOA/mJOA score in surgeries with anterior approaches but not with posterior surgical approaches. Improvement in lordosis angle was significantly positively associated with follow-up duration and age and inversely associated with the change in lordosis. Independently, gender and preoperative JOA/mJOA score had no significant associations with lordosis change in anterior surgery group, but had significantly inverse relationships with the change in lordosis at the latest follow-up in posterior surgery subjects. In posterior surgery group, after the adjustment of age and gender, only preoperative JOA/mJOA score had significantly inverse relationship with the change in lordosis at the latest follow-up.
References
Lebl, D. R., Hughes, A., Cammisa, F. P. Jr. & O’Leary, P. F. Cervical spondylotic myelopathy: pathophysiology, clinical presentation, and treatment. HSS J. 7, 170–78 (2011).
Yarbrough, C. K., Murphy, R. K., Ray, W. Z. & Stewart, T. J. The natural history and clinical presentation of cervical spondylotic myelopathy. Adv Orthop. 2012, 480643, doi:10.1155/2012/480643 (2012).
Karadimas, S. K., Erwin, W. M., Ely, C. G., Dettori, J. R. & Fehlings, M. G. Pathophysiology and natural history of cervical spondylotic myelopathy. Spine (Phila Pa 1976) 38, S21–36 (2013).
Young, W. F. Cervical spondylotic myelopathy: a common cause of spinal cord dysfunction in older persons. Am Family Physician. 62, 1064–70 (2000).
Singh, A., Crockard, H. A., Platts, A. & Stevens, J. Clinical and radiological correlates of severity and surgery-related outcome in cervical spondylosis. J Neurosurg. 94, 189–98 (2001).
Kalsi-Ryan, S., Karadimas, S. K. & Fehlings, M. G. Cervical spondylotic myelopathy: the clinical phenomenon and the current pathobiology of an increasingly prevalent and devastating disorder. Neuroscientist. 19, 409–21 (2013).
Matz, P. G. et al. The natural history of cervical spondylotic myelopathy. J Neurosurg Spine. 11, 104–11 (2009).
Muheremu, A. & Sun, Y. Atypical symptoms in patients with cervical spondylosis might be the result of stimulation on the dura mater and spinal cord. Med Hypotheses. 91, 44–6 (2016).
Emery, S. E. Cervical spondylotic myelopathy: diagnosis and treatment. J Am Acad Orthop Surg. 9, 376–88 (2001).
Rhee, J. M. et al. Nonoperative management of cervical myelopathy: a systematic review. Spine (Phila Pa 1976) 38, S55–67 (2013).
Yalamanchili, P. K., Vives, M. J. & Chaudhary, S. B. Cervical spondylotic myelopathy: factors in choosing the surgical approach. Adv Orthop. 2012, 783762, doi:10.1155/2012/783762 (2012).
Galbraith, J. G., Butler, J. S., Dolan, A. M. & O’Byrne, J. M. Operative outcomes for cervical myelopathy and radiculopathy. Adv Orthop. 2012, 919153, doi:10.1155/2012/919153 (2012).
McDonnell, M. & Lucas, P. Cervical spondylosis, stenosis, and rheumatoid arthritis. Med Health R I. 95, 105–9 (2012).
Higgins, J. P. T., Green, S. Cochrane Handbook for Systematic Reviews of Interventions. Version 5.1.3. Available at http://handbook.cochrane.org/ (2011).
Moher, D., Liberati, A., Tetzlaff, J. & Altman, D. G. PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg. 8, 336–41 (2010).
Burkhardt, J. K. et al. A comparative effectiveness study of patient-rated and radiographic outcome after 2 types of decompression with fusion for spondylotic myelopathy: anterior cervical discectomy versus corpectomy. Neurosurg Focus. 35, E4, doi:10.3171/2013.3.FOCUS1396 (2013).
Cabraja, M., Abbushi, A., Koeppen, D., Kroppenstedt, S. & Woiciechowsky, C. Comparison between anterior and posterior decompression with instrumentation for cervical spondylotic myelopathy: sagittal alignment and clinical outcome. Neurosurg Focus. 28, E15, doi:10.3171/2010.1.FOCUS09253 (2010).
Chen, Y. et al. Surgical strategy for multilevel severe ossification of posterior longitudinal ligament in the cervical spine. J Spinal Disord Tech. 24, 24–30 (2011).
Dai, L. Y. & Jiang, L. S. Anterior cervical fusion with interbody cage containing beta-tricalcium phosphate augmented with plate fixation: a prospective randomized study with 2-year follow-up. Eur Spine J. 17, 698–705 (2008).
Edwards, C. C. 2nd, Heller, J. G. & Murakami, H. Corpectomy versus laminoplasty for multilevel cervical myelopathy: an independent matched-cohort analysis. Spine (Phila Pa 1976). 27, 1168–75 (2002).
Gao, R. et al. Long term results of anterior corpectomy and fusion for cervical spondylotic myelopathy. PLoS One. 7, e34811, doi:10.1371/journal.pone.0034811 (2012).
Kawakami, M. et al. Preoperative instability does not influence the clinical outcome in patients with cervical spondylotic myelopathy treated with expansive laminoplasty. J Spinal Disord Tech. 15, 277–83 (2002).
Kimura, S. et al. Boomerang deformity of cervical spinal cord migrating between split laminae after laminoplasty. Eur Spine J. 9, 144–51 (2000).
Lee, C. H., Jahng, T. A., Hyun, S. J., Kim, K. J. & Kim, H. J. Expansive Laminoplasty versus laminectomy alone versus laminectomy and fusion for cervical ossification of the posterior longitudinal ligament: is there a difference in the clinical outcome and sagittal alignment? Clin Spine Surg. 29, E9–5 (2016).
Lian, X. F. et al. Noncontiguous anterior decompression and fusion for multilevel cervical spondylotic myelopathy: a prospective randomized control clinical study. Eur Spine J. 19, 713–9 (2010).
Liao, J. C., Niu, C. C., Chen, W. J. & Chen, L. H. Polyetheretherketone (PEEK) cage filled with cancellous allograft in anterior cervical discectomy and fusion. Int Orthop. 32, 643–8 (2008).
Lin, Q. et al. A comparison of anterior cervical discectomy and corpectomy in patients with multilevel cervical spondylotic myelopathy. Eur Spine J. 21, 474–81 (2012).
Liu, J. et al. Anterior cervical discectomy and fusion versus corpectomy and fusion in treating two-level adjacent cervical spondylotic myelopathy: a minimum 5-year follow-up study. Arch Orthop Trauma Surg. 135, 149–53 (2015).
Liu, Y. et al. Comparison of 3 reconstructive techniques in the surgical management of multilevel cervical spondylotic myelopathy. Spine (Phila Pa 1976) 37, E1450–8 (2012).
Machino, M. et al. Impact of diabetes on the outcomes of cervical laminoplasty: a prospective cohort study of more than 500 patients with cervical spondylotic myelopathy. Spine (Phila Pa 1976) 39, 220–7 (2014).
Niu, C. C., Liao, J. C., Chen, W. J. & Chen, L. H. Outcomes of interbody fusion cages used in 1- and 2-levels anterior cervical discectomy and fusion: titanium cages versus polyetheretherketone (PEEK) cages. J Spinal Disord Tech. 23, 310–6 (2010).
Oh, M. C., Zhang, H. Y., Park, J. Y. & Kim, K. S. Two-level anterior cervical discectomy versus one-level corpectomy in cervical spondylotic myelopathy. Spine (Phila Pa 1976) 34, 692–6 (2009).
Ohashi, M., Yamazaki, A., Watanabe, K., Katsumi, K. & Shoji, H. Two-year clinical and radiological outcomes of open-door cervical laminoplasty with prophylactic bilateral C4–C5 foraminotomy in a prospective study. Spine (Phila Pa 1976). 39, 721–7 (2014).
Song, K. J., Lee, K. B. & Song, J. H. Efficacy of multilevel anterior cervical discectomy and fusion versus corpectomy and fusion for multilevel cervical spondylotic myelopathy: a minimum 5-year follow-up study. Eur Spine J. 21, 1551–7 (2012).
Bagnall, K. M., Harris, P. F. & Jones, P. R. A radiographic study of the human fetal spine. I. The development of the secondary cervical curvature. J Anat. 123, 777–82 (1977).
Broberg, K. B. On the mechanical behavior of the intervertebral disc. Spine. 8, 151–65 (1983).
Gore, D., Sepic, S. & Gardner, G. Roentgenographic findings of the cervical spine in asymptomatic people. Spine. 11, 521–4 (1986).
Owens, E. & Hoiris, K. Cervical curvature assessment using digitized radiographic analysis. Chiropr Res J. 4, 47–62 (1990).
Harrison, D., Janik, T., Troyanovich, S. & Holland, B. Comparisons of lordotic cervical spine curvatures to a theoretical model of the sagittal cervical spine. Spine. 21, 667–75 (1996).
Kim, H. J. et al. Cervical lordosis actually increases with aging and progressive degeneration in spinal deformity patients. Spine Deformity. 2, 410–414 (2014).
Albert, T. J. & Vacarro, A. Postlaminectomy kyphosis. Spine (Phila Pa 1976) 23, 2738–45 (1998).
Deutsch, H., Haid, R. W., Rodts, G. E. & Mummaneni, P. V. Postlaminectomy cervical deformity. Neurosurg Focus. 15, E5–9 (2003).
Katsuura, A., Kukuda, S., Imanaka, T., Miyamoto, K. & Kanemoto, M. Anterior cervical plate used in degenerative disease can maintain cervical lordosis. J Spinal Disord. 9, 470–6 (1996).
Kawakami, M. et al. Axial symptoms and cervical alignments after cervical anterior spinal fusion for patients with cervical myelopathy. J Spinal Disord. 12, 50–6 (1999).
Nightingale, R. W., McElhaney, J. H., Richardson, W. J., Best, T. M. & Myers, B. S. Experimental impact injury to the cervical spine: relating motion of the head and the mechanism of injury. J Bone Joint Surg Am. 78, 412–21 (1996).
Baba, H. et al. Lordotic alignment and posterior migration of the spinal cord following en bloc open-door laminoplasty for cervical myelopathy: a magnetic resonance imaging study. J Neurol. 85, 626–32 (1996).
Batzdorf, U. & Flannigan, B. D. Surgical decompressive procedures for cervical spondylotic myelopathy. A study using magnetic resonance imaging. Spine. 16, 123–7 (1991).
Swank, M. L., Sutterlin, C. E., Bossons, C. R. & Dials, B. E. Rigid internal fixation with lateral mass plates in multilevel anterior and posterior reconstruction of the cervical spine. Spine. 22, 274–82 (1997).
Stein, J. Failure of magnetic resonance imaging to reveal the cause of a progressive cervical myelopathy related to postoperative spinal deformity: a case report. Am J Phys Med Rehabil. 76, 73–5 (1997).
Naderi, S., Ozgen, S., Pamir, M. N., Ozek, M. M. & Erzen, C. Cervical spondylotic myelopathy: surgical results and factors affecting prognosis. Neurosurg. 43, 43–9 (1998).
Harrison, D. E., Cailliet, R., Harrison, D. D., Janik, T. J. & Holland, B. A new 3-point bending traction method for restoring cervical lordosis and cervical manipulation: a nonrandomized clinical controlled trial. Arch Phys Med Rehabil. 83, 447–53 (2002).
McAviney, J., Schulz, D., Bock, R., Harrison, D. E. & Holland, B. Determining the relationship between cervical lordosis and neck complaints. J Manipulative Physiol Ther. 28, 187–93 (2005).
Harrison, D. D. et al. Modeling of the sagittal cervical spine as a method to discriminate hypolordosis: results of elliptical and circular modeling in 72 asymptomatic subjects, 52 acute neck pain subjects, and 70 chronic neck pain subjects. Spine (Phila Pa 1976) 29, 2485–92 (2004).
Vernon, H., Steiman, I. & Hagino, C. Cervicogenic dysfunction in muscle contraction headache and migraine: a descriptive study. J Manipulative Physiol Ther. 15, 418–29 (1992).
Nagasawa, A., Sakakibara, T. & Takahashi, A. Roentgenographic findings of the cervical spine in tension-type headache. Headache. 33, 90–95 (1993).
Sodeyama, T., Goto, S., Mochizuki, M., Takahashi, J. & Moriya, H. Effect of decompression enlargement laminoplasty for posterior shifting of the spinal cord. Spine. 24, 1527–31 (1999).
Yamazaki, A., Homma, T., Uchiyama, S., Katsumi, Y. & Okumura, H. Morphologic limitations of posterior decompression by midsagittal splitting method for myelopathy caused by ossification of the posterior longitudinal ligament in the cervical spine. Spine. 24, 32–4 (1999).
Liu, W. et al. Comparison of anterior decompression and fusion versus laminoplasty in the treatment of multilevel cervical ossification of the posterior longitudinal ligament: a systematic review and meta-analysis. Ther Clin Risk Manage. 12, 675–685 (2016).
McAllister, B. D., Rebholz, B. J. & Wang, J. C. Is posterior fusion necessary with laminectomy in the cervical spine? Surg Neurol Int. 3, S225–31 (2012).
Epstein, N. E. Laminectomy for cervical myelopathy. Spinal Cord. 41, 317–327 (2003).
Kimura, I., Shingu, H. & Nasu, Y. Long-term follow-up of cervical spondylotic myelopathy treated by canal-expansive laminoplasty. J Bone Joint Surg Br. 77, 956–61 (1995).
Suda, K. et al. Local kyphosis reduces surgical outcomes of expansive open-door laminoplasty for cervical spondylotic myelopathy. Spine (Phila Pa 1976) 28, 1258–62 (2003).
Kelly, M. P., Mok, J. M., Frisch, R. F. & Tay, B. K. Adjacent segment motion after anterior cervical discectomy and fusion versus Prodisc-c cervical total disk arthroplasty: analysis from a randomized, controlled trial. Spine (Phila Pa 1976) 36, 1171–79 (2011).
Kai, Y. et al. Neurogenic thoracic outlet syndrome in whiplash injury. J Spinal Disord. 14, 487–93 (2001).
Lee, S. E., Chung, C. K. & Jahng, T. A. Early development and progression of heterotopic ossification in cervical total disc replacement. J Neurosurg Spine. 16, 31–36 (2012).
Turel, M. K. et al. Reduction in range of cervical motion on serial long-term follow-up in patients undergoing oblique corpectomy for cervical spondylotic myelopathy. Eur Spine J. 22, 1509–16 (2013).
Fehlings, M. G. et al. Perioperative and delayed complications associated with the surgical treatment of cervical spondylotic myelopathy based on 302 patients from the AOSpine North America Cervical Spondylotic Myelopathy Study. J Neurosurg Spine. 16, 425–32 (2012).
Acknowledgements
This work was supported by the National Natural Science Foundation of China (Grant No. 31300137). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Conceived and designed the study: R.Z.H. Performed literature search and extracted data: Z.D.M., W.J. and L.H.Y. Analyzed the data: C.L., X.L., R.Z.H., J.Y. and W.J. Drafted the manuscript: Z.D.M.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Meng, Z., Yu, J., Luo, C. et al. Anterior Cervical Spondylosis Surgical Interventions are Associated with Improved Lordosis and Neurological Outcomes at Latest Follow up: A Meta-analysis. Sci Rep 7, 4407 (2017). https://doi.org/10.1038/s41598-017-04311-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-04311-6
This article is cited by
-
Full endoscopic laminotomy decompression versus anterior cervical discectomy and fusion for the treatment of single-segment cervical spinal stenosis: a retrospective, propensity score-matched study
Journal of Orthopaedic Surgery and Research (2024)
-
Effectiveness of hyper and hypothermic application revulsively on range of motion, symptom score and quality of life in patients with cervical spondylosis: a randomized controlled trial
Advances in Traditional Medicine (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.