Abstract
Regulatory T (Treg) cells play a major role in the development of an immunosuppressive tumor microenvironment. The origin of intratumoral Treg cells and their relationship with peripheral blood Treg cells remain unclear. Treg cells consist of at least three functionally distinct subpopulations. Here we show that peripheral blood CD45RA−FOXP3hi Treg cells (Treg II cells) are phenotypically closest to intratumoral Treg cells, including in their expression of CCR8. Analyses of T cell antigen receptor repertoires further support the hypothesis that intratumoral Treg cells may originate primarily from peripheral blood Treg II cells. Moreover, the signaling responsiveness of peripheral blood Treg II cells to immunosuppressive, T helper type 1 (TH1) and T helper type 2 (TH2) cytokines reflects intratumoral immunosuppressive potential, and predicts future relapse in two independent cohorts of patients with breast cancer. Together, our findings give important insights into the relationship between peripheral blood Treg cells and intratumoral Treg cells, and highlight cytokine signaling responsiveness as a key determinant of intratumoral immunosuppressive potential and clinical outcome.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Josefowicz, S. Z., Lu, L. F. & Rudensky, A. Y. Regulatory T cells: mechanisms of differentiation and function. Annu. Rev. Immunol. 30, 531–564 (2012).
Lu, L., Barbi, J. & Pan, F. The regulation of immune tolerance by FOXP3. Nat. Rev. Immunol. 17, 703–717 (2017).
Sakaguchi, S., Miyara, M., Costantino, C. M. & Hafler, D. A. FOXP3+ regulatory T cells in the human immune system. Nat. Rev. Immunol. 10, 490–500 (2010).
Kumar, V. Adenosine as an endogenous immunoregulator in cancer pathogenesis: where to go? Purinergic Signal. 9, 145–165 (2013).
Vignali, D. A., Collison, L. W. & Workman, C. J. How regulatory T cells work. Nat. Rev. Immunol. 8, 523–532 (2008).
Tanaka, A. & Sakaguchi, S. Regulatory T cells in cancer immunotherapy. Cell Res. 27, 109–118 (2017).
Chaudhary, B. & Elkord, E. Regulatory T cells in the tumor microenvironment and cancer progression: role and therapeutic targeting. Vaccines 4, 28 (2016).
Bates, G. J. et al. Quantification of regulatory T cells enables the identification of high-risk breast cancer patients and those at risk of late relapse. J. Clin. Oncol. 24, 5373–5380 (2006).
Shang, B., Liu, Y., Jiang, S. J. & Liu, Y. Prognostic value of tumor-infiltrating FoxP3+ regulatory T cells in cancers: a systematic review and meta-analysis. Sci. Rep. 5, 15179 (2015).
Rech, A. J. et al. CD25 blockade depletes and selectively reprograms regulatory T cells in concert with immunotherapy in cancer patients. Sci. Transl. Med. 4, 134ra162 (2012).
Liakou, C. I. et al. CTLA-4 blockade increases IFNγ-producing CD4+ICOShi cells to shift the ratio of effector to regulatory T cells in cancer patients. Proc. Natl Acad. Sci. USA 105, 14987–14992 (2008).
Ladoire, S. et al. Pathologic complete response to neoadjuvant chemotherapy of breast carcinoma is associated with the disappearance of tumor-infiltrating FoxP3+ regulatory T cells. Clin. Cancer Res. 14, 2413–2420 (2008).
Sugiyama, D. et al. Anti-CCR4 mAb selectively depletes effector-type FoxP3+CD4+ regulatory T cells, evoking antitumor immune responses in humans. Proc. Natl Acad. Sci. USA 110, 17945–17950 (2013).
Miyara, M. et al. Functional delineation and differentiation dynamics of human CD4+ T cells expressing the FoxP3 transcription factor. Immunity 30, 899–911 (2009).
Liyanage, U. K. et al. Prevalence of regulatory T cells is increased in peripheral blood and tumor microenvironment of patients with pancreas or breast adenocarcinoma. J. Immunol. 169, 2756–2761 (2002).
Martens, A. et al. Baseline peripheral blood biomarkers associated with clinical outcome of advanced melanoma patients treated with ipilimumab. Clin. Cancer Res. 22, 2908–2918 (2016).
Yao, X. et al. Levels of peripheral CD4+FoxP3+ regulatory T cells are negatively associated with clinical response to adoptive immunotherapy of human cancer. Blood 119, 5688–5696 (2012).
Chinen, T. et al. An essential role for the IL-2 receptor in Treg cell function. Nat. Immunol. 17, 1322–1333 (2016).
Fontenot, J. D., Rasmussen, J. P., Gavin, M. A. & Rudensky, A. Y. A function for interleukin 2 in Foxp3-expressing regulatory T cells. Nat. Immunol. 6, 1142–1151 (2005).
Antonioli, L., Pacher, P., Vizi, E. S. & Hasko, G. CD39 and CD73 in immunity and inflammation. Trends Mol. Med. 19, 355–367 (2013).
Plitas, G. et al. Regulatory T cells exhibit distinct features in human breast cancer. Immunity 45, 1122–1134 (2016).
De Simone, M. et al. Transcriptional landscape of human tissue lymphocytes unveils uniqueness of tumor-infiltrating T regulatory cells. Immunity 45, 1135–1147 (2016).
Campbell, D. J. & Koch, M. A. Phenotypical and functional specialization of FOXP3+ regulatory T cells. Nat. Rev. Immunol. 11, 119–130 (2011).
Vu, M. D. et al. OX40 costimulation turns off Foxp3+ Tregs. Blood 110, 2501–2510 (2007).
Carstens, J. L. et al. Spatial computation of intratumoral T cells correlates with survival of patients with pancreatic cancer. Nat. Commun. 8, 15095 (2017).
Baras, A. S. et al. The ratio of CD8 to Treg tumor-infiltrating lymphocytes is associated with response to cisplatin-based neoadjuvant chemotherapy in patients with muscle invasive urothelial carcinoma of the bladder. Oncoimmunology 5, e1134412 (2016).
Hendry, S. et al. Assessing tumor-infiltrating lymphocytes in solid tumors: a practical review for pathologists and proposal for a standardized method from the International Immunooncology Biomarkers Working Group: part 1: assessing the host immune response, TILs in invasive breast carcinoma and ductal carcinoma in situ, metastatic tumor deposits and areas for further research. Adv. Anat. Pathol. 24, 235–251 (2017).
Barsheshet, Y. et al. CCR8+FOXp3+ Treg cells as master drivers of immune regulation. Proc. Natl Acad. Sci. USA 114, 6086–6091 (2017).
Loyher, P. L. et al. CCR2 influences T regulatory cell migration to tumors and serves as a biomarker of cyclophosphamide sensitivity. Cancer Res. 76, 6483–6494 (2016).
Curiel, T. J. et al. Specific recruitment of regulatory T cells in ovarian carcinoma fosters immune privilege and predicts reduced survival. Nat. Med. 10, 942–949 (2004).
Facciabene, A. et al. Tumour hypoxia promotes tolerance and angiogenesis via CCL28 and Treg cells. Nature 475, 226–230 (2011).
Redjimi, N. et al. CXCR3+ T regulatory cells selectively accumulate in human ovarian carcinomas to limit type I immunity. Cancer Res. 72, 4351–4360 (2012).
Tan, M. C. et al. Disruption of CCR5-dependent homing of regulatory T cells inhibits tumor growth in a murine model of pancreatic cancer. J. Immunol. 182, 1746–1755 (2009).
Adeegbe, D. O. & Nishikawa, H. Natural and induced T regulatory cells in cancer. Front. Immunol. 4, 190 (2013).
Su, S. et al. Blocking the recruitment of naive CD4+ T cells reverses immunosuppression in breast cancer. Cell Res. 27, 461–482 (2017).
Walker, M. R., Carson, B. D., Nepom, G. T., Ziegler, S. F. & Buckner, J. H. De novo generation of antigen-specific CD4+CD25+ regulatory T cells from human CD4+CD25− cells. Proc. Natl Acad. Sci. USA 102, 4103–4108 (2005).
Tran, D. Q., Ramsey, H. & Shevach, E. M. Induction of FOXP3 expression in naive human CD4+FOXP3− T cells by T-cell receptor stimulation is transforming growth factor-β-dependent but does not confer a regulatory phenotype. Blood 110, 2983–2990 (2007).
Marie, J. C., Letterio, J. J., Gavin, M. & Rudensky, A. Y. TGF-β1 maintains suppressor function and Foxp3 expression in CD4+CD25+ regulatory T cells. J. Exp. Med. 201, 1061–1067 (2005).
Schlenner, S. M., Weigmann, B., Ruan, Q., Chen, Y. & von Boehmer, H. Smad3 binding to the foxp3 enhancer is dispensable for the development of regulatory T cells with the exception of the gut. J. Exp. Med. 209, 1529–1535 (2012).
Ouyang, W., Beckett, O., Ma, Q. & Li, M. O. Transforming growth factor-β signaling curbs thymic negative selection promoting regulatory T cell development. Immunity 32, 642–653 (2010).
Konkel, J. E. et al. Transforming growth factor-β signaling in regulatory T cells controls T helper-17 cells and tissue-specific immune responses. Immunity 46, 660–674 (2017).
Murai, M. et al. Interleukin 10 acts on regulatory T cells to maintain expression of the transcription factor Foxp3 and suppressive function in mice with colitis. Nat. Immunol. 10, 1178–1184 (2009).
Chaudhry, A. et al. Interleukin-10 signaling in regulatory T cells is required for suppression of Th17 cell-mediated inflammation. Immunity 34, 566–578 (2011).
Wei, J. et al. Antagonistic nature of T helper 1/2 developmental programs in opposing peripheral induction of Foxp3+ regulatory T cells. Proc. Natl Acad. Sci. USA 104, 18169–18174 (2007).
Caretto, D., Katzman, S. D., Villarino, A. V., Gallo, E. & Abbas, A. K. Cutting edge: the Th1 response inhibits the generation of peripheral regulatory T cells. J. Immunol. 184, 30–34 (2010).
Overacre-Delgoffe, A. E. et al. Interferon-γ drives Treg fragility to promote anti-tumor immunity. Cell 169, 1130–1141 (2017).
Sun, W. et al. A positive-feedback loop between tumour infiltrating activated Treg cells and type 2-skewed macrophages is essential for progression of laryngeal squamous cell carcinoma. Br. J. Cancer 117, 1631–1643 (2017).
Tiemessen, M. M. et al. CD4+CD25+Foxp3+ regulatory T cells induce alternative activation of human monocytes/macrophages. Proc. Natl Acad. Sci. USA 104, 19446–19451 (2007).
Acknowledgements
We would like to thank M. Kirschenbaum for obtaining consent from patients and acquiring samples at City of Hope Comprehensive Cancer Center. We would like to thank D. Dunkley for organizing the collection of blood samples from age-matched healthy controls. This work was supported by the Department of Defense Breast Cancer Research Program, Stand Up to Cancer, the Breast Cancer Research Foundation and the V Foundation. Research reported in this publication included work performed in the Analytical Cytometry Core and Pathology Research Services Core supported by the National Cancer Institute of the National Institutes of Health under award number P30CA33572. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
L.W. and P.P.L. designed experiments; L.W., D.L.S., T.Y.T., S.S., R.W., D.S., A.R. and C.A. conducted experiments; L.W. and X.L. analyzed experimental data; J.Y. and J.W. identified and recruited patients into this study; L.W. and P.P.L. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information: Zoltan Fehervari was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
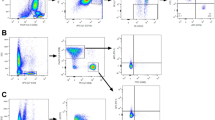
Supplementary Figure 1 Treg cell gating strategy for flow and phosflow cytomery.
(a) Representative flow plots for peripheral and intratumoral Treg cells. (b-c) Representative flow plots showing the percentages of IL-2Rβ+ (b) and IL-2Rγ+ (c) in peripheral blood Tconv, Treg I, II and III cells. (d) Representative flow plots for peripheral blood Treg cells in phosflow cytometry.
Supplementary Figure 2 Expressions of immune-regulating proteins in peripheral blood Treg cell subpopulations and intratumoral Treg cells.
The percentages of CD73+ (n=40) (a), PD1+ (n=40), ****p<0.0001 (b), Tim3+ (n=40), ****p<0.0001 (c), LAG3+ (n=40), ****p<0.0001; ***p=0.0002 (d), GITR+ (n=20), ****p<0.0001; **p=0.007 (e) or HLA-DR+ (n=40), ****p<0.0001; ***p=0.0003 (f) in peripheral Tconv, Treg I, II and III cells from newly diagnosed patients with BC were determined by flow cytometry. Friedman test. Shown are mean ± s.e.m. Representative flow plots showing the percentages of LAG3+ (d), GITR+ (e), or HLA-DR+ (f) in intratumor Treg cells from untreated primary breast tumors (n=8). Data from intratumoral Treg cells were highlighted with purple box.
Supplementary Figure 3 Flow sort gating strategy of peripheral blood Tconv and Treg cell subpopulations.
Peripheral Treg I (CD45RA+CD25lo), II (CD45RA−CD25hi), III (CD45RA−CD25lo) and Tconv (CD45RA−CD25−) cells were sorted from PBMCs of newly diagnosed patients with BC.
Supplementary Figure 4 Chemokine receptors CCR2, CCR10 and CXCR3 not differentially expressed in intratumoral Treg cells.
The percentages and representative flow plots of CCR2+, ***p=0.0003; *p=0.03 (a), CCR10+, ****p<0.0001; **p=0.009 (b), CXCR3+, ****p<0.0001; *p=0.025 (c) in peripheral Tconv, Treg I, II and III cells from newly diagnosed patients with BC (n=20) and in intratumor Treg cells from untreated primary breast tumors (n=8). Friedman test. Shown are mean ± s.e.m. Data from intratumoral Treg cells were highlighted with purple box.
Supplementary Figure 5 Intratumoral Treg cells have higher TCR clonal overlap with peripheral Treg II cells.
(a) TCRβ CDR3 regions of flow sorted intratumor Treg cells (CD4+CD25+CD127−) and paired peripheral Treg I, II or III cells from patients with BC (n=3) were sequenced. Pair-wise scatter plots showing the overlapping TCR clones between intratumor Treg cells and peripheral Treg cell subpopulations. (b) The percentages of unique TCR nucleotide clonal overlap between peripheral blood Treg I, II or III cells. Shown are mean ± s.e.m.
Supplementary Figure 6 Representative flow plots showing TGFβ-induced signaling in peripheral blood Treg II cell subpopulation.
TGFβ (25ng/ml for 30 mins)-induced Smad2/3 phosphorylation in peripheral blood Treg II cells from newly diagnosed patients with BC (n=40) was determined by phosphoflow cytometry with anti-p-Smad2 (pS465/pS467)/p-Smad3 (pS423/pS425) antibody. Plots from relapsed patients with BC were highlighted with red box.
Supplementary Figure 7 Representative flow plots showing IL-10-induced signaling in peripheral blood Treg II cell subpopulation.
IL-10 (100ng/ml for 15 mins)-induced STAT1 phosphorylation in peripheral blood Treg II cells from newly diagnosed patients with BC (n=40) was determined by phosphoflow cytometry with anti-p-STAT1 (pY701) antibody. Plots from relapsed patients with BC were highlighted with red box.
Supplementary Figure 8 Representative flow plots showing IL-4-induced signaling in peripheral blood Treg II cell subpopulation.
IL-4 (50ng/ml for 15 mins)-induced STAT6 phosphorylation in peripheral blood Treg II cells from newly diagnosed patients with BC (n=40) was determined by phosphoflow cytometry with anti-p-STAT6 (pY641) antibody. Plots from relapsed patients with BC were highlighted with red box.
Supplementary Figure 9 Representative flow plots showing IFNγ-induced signaling in peripheral blood Treg II cell subpopulation.
IFNγ (50ng/ml for 15 mins)-induced STAT1 phosphorylation in peripheral blood Treg II cells from newly diagnosed patients with BC (n=40) was determined by phosphoflow cytometry with anti-p-STAT1 (pY701) antibody. Plots from relapsed patients with BC were highlighted with red box.
Supplementary Figure 10 Cytokine signaling index of Tconv, Treg I or Treg III cells not correlated with clinical outcome.
Relapse-free survival (RFS) was compared between patients with BC (n=40) with above median CSI and below median CSI in peripheral Tconv (p=0.22) (a), Treg I (p=0.68) (b) or Treg III cells (p=0.07) (c) using Kaplan-Meier estimate and log rank test. All blood were collected from patients with BC at diagnosis before surgery or any therapy who had been clinically followed for at least 36 months. NS, not significant.
Supplementary Figure 11 Cytokine plasma levels in patients with BC at diagnosis do not correlate with clinical outcome.
(a) Plasma levels of TGFβ, IL-10, IL-4 and IFNγ were determined by ELISA and compared between relapse-free (n=25) and relapsed (n=15) BC patients. Shown are mean ± s.e.m. (b) The association between plasma level of TGFβ (p=0.08), IL-10 (p=0.79), IL-4 (p=0.36) or IFNγ (p=0.58) and signaling response in Treg II cells, respectively. Spearman correlation coefficient test. NS, not significant.
Supplementary Figure 12 Treg II CSI in healthy donors were lower than in relapsed patients with BC.
(a-b) PBMCs from age-matched healthy donors (HD) (n=10) were stimulated with TGFβ (25ng/ml, 30 mins), IL-10 (100ng/ml, 15 mins), IL-4 (50ng/ml, 15 mins) or IFNγ (50ng/ml, 15 mins). TGFβ-induced p-Smad2/3 and IL-10-induced p-STAT1, ***p<0.001 (a), IFNγ-induced p-STAT1 and IL-4-induced p-STAT6 **p=0.008; *p=0.028 (b) in peripheral Treg II cells were determined by phosphoflow cytometry and were compared between healthy donors (n=10) and relapsed patients with BC (n=15). (c) Treg II CSI was compared between HD (n=10) and relapsed patients with BC (n=15), ****p<0.001, two-tailed, Mann-Whitney test. Shown are mean ± s.e.m.
Supplementary Figure 13 Cytokine signaling index (CSI) of peripheral Treg I or III cells not associated with immunosuppressive potential of intratumoral Treg cells.
Untreated breast primary tumor tissue sections were stained for FoxP3, CD8, CD68, CD123, CK, and DAPI. (a) The density of Treg cells within primary tumors (FoxP3+ cell number per mm2) from patients with BC who later relapsed (n=9) and from patients who remained relapse-free (n=11), p=0.07, two-tailed, Mann-Whitney test, Shown are mean ± s.e.m. (b) The association between Treg cell density and the percentage of Treg cells within 20μm from TAMs (n=20) (p=0.14). (c-d) The association between Treg I CSI (p=0.52) (C) or Treg III CSI (p=0.15) (d) and the percentage of Treg cells within 20μm from TAMs (n=20). Spearman correlation coefficient test. NS, not significant.
Supplementary Figure 14 Consistent cytokine signaling responses in reference PBMCs between discovery and validation runs.
Different vials of reference PBMC from the same healthy donors (n=5) were thawed and run together with samples from patient with BC in the discovery and validation cohorts to determine consistency between runs. (a) TGF-induced Smad2/3 phosphorylation, (b) IL-10-induced STAT1 phosphorylation, (c) IL-4-induced STAT6 phosphorylation, or (d) IFNγ-induced STAT1 phosphorylation in Treg II cells.
Supplementary information
Supplementary Information
Supplementary Figures 1–14 and Supplementary Tables 1 and 2
Rights and permissions
About this article
Cite this article
Wang, L., Simons, D.L., Lu, X. et al. Connecting blood and intratumoral Treg cell activity in predicting future relapse in breast cancer. Nat Immunol 20, 1220–1230 (2019). https://doi.org/10.1038/s41590-019-0429-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41590-019-0429-7
This article is cited by
-
How chemokines organize the tumour microenvironment
Nature Reviews Cancer (2024)
-
Development of a cellular model to study CCR8 signaling in tumor-infiltrating regulatory T cells
Cancer Immunology, Immunotherapy (2024)
-
A distinct “repair” role of regulatory T cells in fracture healing
Frontiers of Medicine (2024)
-
Genetic, DNA methylation, and immune profile discrepancies between early-stage single primary lung cancer and synchronous multiple primary lung cancer
Clinical Epigenetics (2023)
-
Phosphoflow cytometry to assess cytokine signaling pathways in peripheral immune cells: potential for inferring immune cell function and treatment response in patients with solid tumors
Journal of Experimental & Clinical Cancer Research (2023)