Abstract
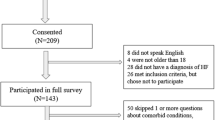
Despite various Peyronie’s disease (PD) treatment options, the literature is sparse regarding patient preference for available therapies. Our data explore resource and treatment choices made by PD men following diagnosis. A survey was mailed to 719 randomly selected PD men evaluated at our institution from 1990–2012. Questions included evaluation of treatments and preferred information resources. Results were summarized as a descriptive report with statistical analyses performed as indicated. A total of 162 men (median age 65) responded with median PD duration of 9.2 years. Information sources included medical websites (38.9%), physician (35.8%), and books (<1%). Overall, patients felt 72.5% (SD = 40) of physicians had a good understanding of PD. About 53.1% of men had tried at least one therapy with 37.2% trying two or more. In comparing therapies, most surgical patients reported improvement at 82.8%. Among a cohort of PD men responding to a mailed survey, medical websites were the most widely used source of information. Almost half of the patients chose not to pursue any form of therapy, while the remaining majority elected for non-operative intervention. These results suggest a need for greater patient and provider education on PD management.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Nehra A, Alterowitz R, Culkin DJ, Faraday MM, Hakim LS, Heidelbaugh JJ, et al. Peyronie’s Disease: AUA Guideline. J Urol. 2015;194:745–53.
Stuntz M, Perlaky A, des Vignes F, Kyriakides T, Glass D. The prevalence of Peyronie’s Disease in the United States: a population-based study. PLoS ONE. 2016;11:e0150157.
Gelbard MK, Dorey F, James K. The natural history of Peyronie’s disease. J Urol. 1990;144:1376–9.
Garaffa G, Kuehhas FE, De Luca F, Ralph DJ. Long-term results of reconstructive surgery for Peyronie’s disease. Sex Med Rev. 2015;3:113–21.
Brant WO, Reed-Maldonado A, Lue TF. Injection therapy for Peyronie’s disease: pearls of wisdom. Transl Androl Urol. 2015;4:474–7.
Alizadeh M, Karimi F, Fallah MR. Evaluation of verapamil efficacy in Peyronie’s disease comparing with pentoxifylline. Glob J Health Sci. 2014;6:23–30.
Kendirci M, Usta MF, Matern RV, Nowfar S, Sikka SC, Hellstrom WJ. The impact of intralesional interferon alpha-2b injection therapy on penile hemodynamics in men with Peyronie’s disease. J Sex Med. 2005;2:709–15.
Paulis G, Barletta D, Turchi P, Vitarelli A, Dachille G, Fabiani A, et al. Efficacy and safety evaluation of pentoxifylline associated with other antioxidants in medical treatment of Peyronie’s disease: a case-control study. Res Rep Urol. 2016;8:1–10.
Paulis G, Brancato T, D’Ascenzo R, De Giorgio G, Nupieri P, Orsolini G, et al. Efficacy of vitamin E in the conservative treatment of Peyronie’s disease: legend or reality? A controlled study of 70 cases. Andrology. 2013;1:120–8.
Trost LW, Gur S, Hellstrom WJ. Pharmacological management of Peyronie’s disease. Drugs. 2007;67:527–45.
Raheem AA, Garaffa G, Raheem TA, Dixon M, Kayes A, Christopher N, et al. The role of vacuum pump therapy to mechanically straighten the penis in Peyronie’s disease. BJU Int. 2010;106:1178–80.
Martinez-Salamanca JI, Egui A, Moncada I, Minaya J, Ballesteros CM, Del Portillo L, et al. Acute phase Peyronie’s disease management with traction device: a nonrandomized prospective controlled trial with ultrasound correlation. J Sex Med. 2014;11:506–15.
Levine LA, Newell M, Taylor FL. Penile traction therapy for treatment of Peyronie’s disease: a single-center pilot study. J Sex Med. 2008;5:1468–73.
Sullivan J, Moskovic D, Nelson C, Levine L, Mulhall J. Peyronie’s disease: urologist’s knowledge base and practice patterns. Andrology. 2015;3:260–4.
LaRochelle JC, Levine LA. A survey of primary-care physicians and urologists regarding Peyronie’s disease. J Sex Med. 2007;4(4 Pt 2):1167–73.
Smith JF, Walsh TJ, Conti SL, Turek P, Lue T. Risk factors for emotional and relationship problems in Peyronie’s disease. J Sex Med. 2008;5:2179–84.
Nelson CJ, Diblasio C, Kendirci M, Hellstrom W, Guhring P, Mulhall JP. The chronology of depression and distress in men with Peyronie’s disease. J Sex Med. 2008;5:1985–90.
Davis S, Ferrar S, Sadikaj G, Binik Y, Carrier S. Shame, catastrophizing, and negative partner responses are associated with lower sexual and relationship satisfaction and more negative affect in men with Peyronie’s disease. J Sex Marital Ther. 2017;43:264–76.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors listed on this manuscript certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Bole, R., Ziegelmann, M., Avant, R. et al. Patient’s choice of health information and treatment modality for Peyronie’s disease: a long-term assessment. Int J Impot Res 30, 243–248 (2018). https://doi.org/10.1038/s41443-018-0028-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-018-0028-4
This article is cited by
-
Consulting “Dr Google” for sexual dysfunction: a contemporary worldwide trend analysis
International Journal of Impotence Research (2020)