Abstract
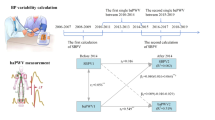
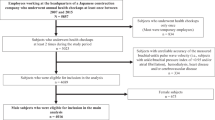
Some studies have shown that a higher ideal cardiovascular health score (CVHS) predicts a lower incidence of arterial stiffness. Few studies have used multiple measurements of CVHS to examine the impact of CVHS on arterial stiffness. The current study aimed to identify the long-term patterns in CVHS trajectory and to explore the association between CVHS trajectory and arterial stiffness. The study cohort consisted of 18,854 participants from the Kailuan Study who were followed up for five physical examinations over 8.10 years. Five discrete CVHS trajectories were identified among the participants: low-stable (8.10%), low-moderate (6.84%), moderate-low (23.46%), moderate-stable (39.83%), and elevated-stable (21.77%). After adjustment for confounding factors, generalized linear model analysis showed that CVHS trajectory group correlated negatively with brachial–ankle pulse wave velocity (baPWV). Compared with the low-stable group, the low-moderate group, moderate-low group, moderate-stable group, and elevated-stable group had B values of −41.81, −24.11, −86.79, and −169.54, respectively. We also used logistic regression to calculate odds ratios (ORs) and 95% confidence intervals (CIs) for CVHS trajectory groups and arterial stiffness. In fully adjusted models, ORs were 0.76 (95% CI: 0.62–0.94) for the low-moderate group, 0.80 (95% CI: 0.67–0.97) for the moderate-low group, 0.51 (95% CI: 0.42–0.62) for the moderate-stable group, and 0.23 (95% CI: 0.18–0.29) for the elevated-stable group compared with the low-stable group. The results were consistent across a number of sensitivity analyses. In conclusion, the higher long-term attainment and the improvement of CVHS were negatively associated with baPWV and could reduce the risk of arterial stiffness. Our study emphasizes the importance of optimizing CVH throughout life to prevent the incidence of arterial stiffness.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
GBD 2016 Causes of Death Collaborators. Global, regional, and national age-sex specific mortality for 264 causes of death, 1980-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1151–210.
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, et al. INTERHEART study investigators. effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study):case-control study. Lancet. 2004;364:937–52.
Khanji MY, van Waardhuizen CN, Bicalho VVS, Ferket BS, Hunink MGM, Petersen SE. Lifestyle advice and interventions for cardiovascular risk reduction: a systematic review of guidelines. Int J Cardiol. 2018;263:142–51.
Lloyd-Jones DM, Hong Y, Labarthe D, Mozaffarian D, Appel LJ, Van Horn L. American Heart Association Strategic Planning Task Force and Statistics Committee et al. Defining and setting national goals for cardiovascular health promotion and disease reduction: the American Heart Association’s strategic Impact Goal through 2020 and beyond. Circulation. 2010;121:586–613.
Huffman MD, Capewell S, Ning H, Shay CM, Ford ES, Lloyd-Jones DM. Cardiovascular health behavior and health factor changes (1988-2008) and projections to 2020:results from the National Health and Nutrition Examination Surveys. Circulation. 2012;125:2595–602.
Wilsgaard T, Loehr LR, Mathiesen EB, Løchen ML, Bønaa KH, Njølstad l, et al. Cardiovascular health and the modifiable burden of incident myocardial infarction: the Tromsø Study. BMC Public Health. 2015;15:221.
Xanthakis V, Enserro DM, Murabito JM, Polak JF, Wollert KC, Januzzi JL, et al. Ideal cardiovascular health: associations with biomarkers and subclinical disease and impact on incidence of cardiovascular disease in the Framingham Offspring Study. Circulation. 2014;130:1676–83.
Bonet J, Vicente A. Arterial stiffness, organic subclinical damage and cardiovascular risk factor. Med Clin. 2009;133:137–8.
Laurent S, Cockcroft J, Van Bortel L, Boutouyrie P, Giannattasio C, Hayoz D, et al. European network for non-invasive investigation of large arteries. expert consensus document on arterial stiffness: methodological issues and clinical applications. Eur Heart J. 2006;27:2588–605.
Veerasamy M, Ford GA, Neely D, Bagnall A, MacGowan G, Das R, et al. Association of aging, arterial stiffness, and cardiovascular disease: a review. Cardiol Rev. 2014;22:223–32.
Rosenberg AJ, Lane-Cordova AD, Wee SO, White DW, Hilgenkamp TIM, Fernhall B, et al. Healthy aging and carotid performance: strain measures and β-stiffness index. Hypertens Res. 2018;41:748–55.
Cecelja M, Chowienczyk P. Dissociation of aortic pulse wave velocity with risk factors for cardiovascular disease other than hypertension a systematic review. Hypertesion. 2009;54:1328–36.
Aatola H, Hutri-Kähönen N, Juonala M, Viikari JS, Hulkkonen J, Laitinen T, et al. Lifetime risk factors and arterial pulse wave velocity in adulthood: the cardiovascular risk in young Finns Study. Hypertension. 2010;55:806–11.
Im JA, Lee JW, Shim JY, Lee HR, Lee DC. Association between brachial-ankle pulse wave velocity and cardiovascular risk factors in healthy adolescents. J Pediatr. 2007;150:247–51.
Loehr LR, Meyer ML, Poon AK, Selvin E, Palta P, Tanaka H, et al. Prediabetes and diabetes are associated with arterial stiffness in older adults: The ARIC Study. Am J Hypertens. 2016;29:1038–45.
Recio-Rodríguez JI, Rodriguez-Sanchez E, Martin-Cantera C, Martinez-Vizcaino V, Arietaleanizbeaskoa MS, Gonzalez-Viejo N. EVIDENT Investigators group et al. Combined use of a healthy lifestyle smartphone application and usual primary care counseling to improve arterial stiffness, blood pressure and wave reflections: a randomized controlled trial (EVIDENT II Study). Hypertens Res. 2019;42:852–62.
Aatola H, Hutri-Kahonen N, Juonala M, Laitinen TT, Pahkala K, Mikkilä V, et al. Prospective relationship of change in ideal cardiovascular health status and arterial stiffness: the cardiovascular risk in young finns study. J Am Heart Assoc. 2014;3:e000532.
Spring B, Moller AC, Colangelo LA, Siddique J, Roehrig M, Daviglus ML, et al. Healthy lifestyle change and subclinical atherosclerosis in young adults: coronary artery risk development in young adults (cardia) study. Circulation. 2014;130:10–7.
Shah AM, Claggett B, Folsom AR, Lutsey PL, Ballantyne CM, Heiss G, et al. Ideal cardiovascular health during adult life and cardiovascular structure and function among the elderly. Circulation. 2015;132:1979–89.
Niyonkuru C, Wagner AK, Ozawa H, Amin K, Goyal A, Fabio A. Group-based trajectory analysis applications for prognostic biomarker model development in severe TBI: a practical example. J Neurotramua. 2013;30:938–45.
Nagin DS. Analyzing developmental trajectories: a semiparametric, group based approach. Psychol Methods. 1999;4:139–57.
Zhang Q, Zhou Y, Gao X, Wang C, Zhang S, Wang A, et al. Ideal cardiovascular health metrics and the risks of ischemic and intracerebral hemorrhagic stroke. Stroke. 2013;44:2451–6.
Brown IJ, Tzoulaki I, Candeias V, Elliott P. Salt intakes around the world: implications for public health. Int J Epidemiol. 2009;38:791–813.
Wu SL, Huang ZR, Yang XC, Zhou Y, Wang AX, Chen L, et al. Prevalence of ideal cardiovascular health and Its relationship with the 4-year cardiovascular events in a northern chinese industrial city. Circ Cardiovasc Qual Outcomes. 2012;5:487–93.
Tanaka H, Munakata M, Kawano Y, Ohishi M, Shoji T, Sugawara J, et al. Comparison between carotid-femoral and brachial-ankle pulse wave velocity as measures of arterial stiffness. J Hyoertens. 2009;27:2022–7.
Ben-Shlomo Y, Spears M, Boustred C, May M, Anderson SG, Benjamin EJ, et al. Aortic pulse wave velocity improves cardiovascular event prediction: an individual participant meta-analysis of prospective observational data from 17,635 subjects. J Am Coll Cardiol. 2014;63:636–46.
Munakata M, Nunokawa T, Tayama J, Yoshinaga K, Toyota T. Brachial-ankle pulse wave velocity as a novel measure of arterial stiffness: present evidences and perspectives. Curr Hypertens Rev. 2005;1:223–34.
Kawai T, Ohishi M, Onishi M, Ito N, Takeya Y, Maekawa Y, et al. Cut-off value of brachial-ankle pulse wave velocity to predict cardiovascular disease in hypertensive patients: a cohort study. J Atheroscler Thromb. 2013;20:391–400.
Zheng X, Zhang R, Liu X, Zhao H, Liu H, Gao J, et al. Association between cumulative exposure to ideal cardiovascular health and arterial stiffness. Atherosclerosis. 2017;260:56–62.
Yamashina A, Tomiyama H, Arai T, Hirose K, Koji Y, Hieayama Y, et al. Brachial-ankle pulse wave velocity as a marker of atherosclerotic vascular damage and cardiovascular risk. Hypertens Res. 2003;26:615–22.
Crichton GE, Elias MF, Robbins MA. Cardiovascular health and arterial stiffness: the Maine-Syracuse Longitudinal Study. J Hum Hypertens. 2014;28:444–9.
Ohkuma T, Ninomiya T, Tomiyama H, Kario K, Hoshide S, Kita Y. Collaborative Group for J-BAVEL(Japan Brachial-Ankle Pulsewave Velocity Individual Participant Data Meta-Analysis of Prospective Studies) et al. Brachial-ankle pulse wave velocity and the risk prediction of cardiovascular disease: an individual participant data meta-analysis. Hypertension. 2017;69:1045–52.
Vlachopoulos C, Aznaouridis K, Stefanadis C. Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol. 2010;55:1318–27.
Yan N, Zhou Y, Wang Y, Wang A, Yang X, Russell A, et al. Association of ideal cardiovascular health and brachial-ankle pulse wave velocity: a cross-sectional study in Northern China. J Stroke Cerebrovasc Dis. 2016;25:41–8.
García-Hermoso A, Martínez-Vizcaíno V, Gomez-Marcos MÁ, Cavero-Redondo I, Recio-Rodriguez JI, García-Ortiz L. Ideal cardiovascular health and arterial stiffness is spanish adults-The EVIDENT Study. J Stroke Cerebrovasc Dis. 2018;27:1386–94.
Acknowledgements
We thank the staff and participants of the Kailuan study for their important contributions.
Funding
The work for this article was supported by the national natural science foundation of China (81873896) to YY.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Zhang, R., Xie, J., Yang, R. et al. Association between ideal cardiovascular health score trajectories and arterial stiffness: the Kailuan Study. Hypertens Res 43, 140–147 (2020). https://doi.org/10.1038/s41440-019-0341-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-019-0341-4
Keywords
This article is cited by
-
Association between the trajectory of ideal cardiovascular health metrics and incident chronic kidney disease among 27,635 older adults in northern China–a prospective cohort study
BMC Geriatrics (2024)
-
Exposure to organochlorine pesticides and polychlorinated biphenyls, adherence to an ideal cardiovascular health, and arterial stiffness among Chinese adults
Environmental Geochemistry and Health (2024)
-
Association of cardiovascular health score trajectory and risk of subsequent cardiovascular disease in non-diabetic population: a cohort study
BMC Public Health (2023)
-
Time spent in a better cardiovascular health and risk of cardiovascular diseases and mortality: a prospective cohort study
Journal of Translational Medicine (2023)
-
Temporal relationship between arterial stiffness and blood pressure variability and joint effect on cardiovascular disease
Hypertension Research (2023)