Abstract
Various home blood-pressure (HBP) measurement schedules were compared to determine the optimal schedule of HBP measurement for the diagnosis of hypertension. Out of 319 individuals who were suspected of having hypertension based on office BP measurements and who did not take antihypertensive drugs, 157 individuals who completed 42 HBP measurements over 7 days and who had a valid 24-h ambulatory blood pressure (ABP) measurement were included in this analysis. We evaluated five HBP measurement schedules to determine the optimal HBP measurement schedule for the diagnosis of hypertension. The cumulatively averaged HBP from 5 to 6 measurement days showed a Pearson correlation coefficient of >0.990 compared to HBP averaged for 6 or 7 days depending on the method. The intraclass correlation coefficient of the cumulatively averaged HBP measurements compared with the 24-h ABP measurement was excellent (≥0.75) from the average of three measurement days and increased steadily with increasing averaged days of HBP measurements. Compared with a diagnosis using a 24-h ABP measurement, the diagnostic sensitivity, specificity, and positive and negative predictive values of HBP measurements were not different among the five methods. The diagnostic agreement of cumulatively averaged HBP measurements was nearly perfect (kappa ≥ 0.9) from the average of five measurement days compared with a diagnosis based on HBP measurements averaged for 6 or 7 days and diagnosis based on averaged HBP measurements of previous days. We suggest obtaining HBP measurements over 5 days or more, in the morning and evening, taking two or more measurements per occasion, and averaging all of the readings as the optimal schedule of HBP measurement for the diagnosis of hypertension.
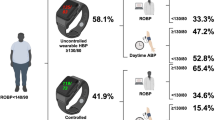
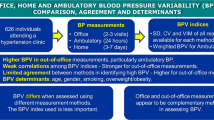
Similar content being viewed by others
Introduction
The diagnosis of hypertension using an appropriate method of blood pressure (BP) measurement is important in preventing cardiovascular diseases caused by hypertension. Office BP (OBP) measurement has been used in the diagnosis and treatment of hypertension. However, OBP measurement has disadvantages, such as difficulty in frequent measurement and the white coat effect [1, 2].
Home BP (HBP) measurement can minimize the white coat effect. It can be performed frequently without visiting a clinic and is more related to the prognosis of cardiovascular disease compared with OBP measurements [2, 3]. It also has the additional advantages of ease of measurements and measurements at a lower cost compared with the 24-h ambulatory BP (ABP) measurement [3, 4].
Many guidelines currently recommend HBP measurements in the diagnosis and treatment of hypertension [1, 2, 5,6,7]. Recommendations related to the timing, number of days, and number of measurements for HBP measurement remain inconsistent [1, 2, 5, 6]. Several studies have suggested an optimal schedule [8,9,10,11,12,13], but it is difficult to apply uniformly, because the daily lifestyle of Asians is different from that of Westerners.
In this study, we aimed to analyze and compare various schedules of HBP measurements in the diagnosis of hypertension and suggest an appropriate schedule for Asians.
Methods
Study population
The study population and protocol were described previously. Briefly, individuals whose OBP measured by a physician was ≥140/90 mmHg were included. Individuals with secondary hypertension, hypertensive emergencies or urgencies, New York Heart Association functional class III or VI heart failure, clinically significant arrhythmia, serum creatinine ≥1.7 mg/dl, or previous drug or alcohol abuse within the last 6 months were excluded. Pregnant women and individuals who were working at night, were currently participating in other intervention trials, had taken other clinical study drugs within the last month, and were taking medications that affect BP were also excluded. The study protocol was approved by the Institutional Review Board of each participating hospital (Dongguk University Ilsan Hospital, Inje University Ilsan Paik Hospital, Myongji Hospital, and Seoul Medical Center). All participants provided written informed consent before entry into the study.
Measurements of OBP, HBP, and 24-h ABP
The BP measurement schedule is shown previously [14]. Conventional OBP was measured with a validated oscillometric device (WatchBP Home; Microlife, Taiwan) after the participants had rested for at least 5 min in a sitting position. Measurement was performed three consecutive times at 1-min intervals. HBP was measured with the same devices used for the measurement of OBP.
HBP measurements started on the evening of the first visit day and continued for seven consecutive days, ending on the morning of the eighth day. HBP was measured three times at 1-min intervals, in the morning (between 07:00 or waking and 09:00) after micturition and before breakfast, and in the evening (between 21:00 and 23:00 or bedtime) in a quiet place after 5 min of rest in a seated position.
On the eighth day, participants started their 24-h ABP measurements on the non-dominant arm using an automated and non-invasive oscillometric device (Mobil-O-Graph, I.E.M. GmbH, Germany) with a measurement interval of 30 min. Participants were instructed to continue with their normal daily activities during the study period. A valid measurement of 24-h ABP was defined as valid readings for more than 70% of the total measurement attempts and at least 14 measurements during the daytime (10:00 to 20:00 h) and at least seven measurements during the nighttime (00:00 to 06:00 h) [15].
Definition of hypertension
Hypertension based on ABP measurements was defined as a 24-h average systolic BP (SBP) ≥ 130 mmHg and/or a 24-h average diastolic BP (DBP) ≥ 80 mmHg. Hypertension based on HBP measurements was defined as averaged SBP ≥ 135 mmHg and/or averaged DBP ≥ 85 mmHg [1, 2, 5].
Statistical analysis
Five methods of averaging HBP measurements were evaluated and compared (Fig. 1).
-
(1)
Method 1: The HBP measured on the first evening (HBP measured on the evening of the first day) was excluded. The mean HBP of the first day was the average of the HBP measured on the first morning (HBP measured on the morning of the second day) and on the second evening (HBP measured on the evening of the second day).
-
(2)
Method 2: The HBP measured on the first evening and on the first morning were excluded. The mean HBP of the first day was the average of the HBP measured on the second evening and on the second morning (HBP measured on the morning of the third day).
-
(3)
Method 3: The HBP measured on the first evening and on the first morning were excluded. The mean HBP of the first day was the average of the HBP measured on the second evening and on the second morning. The mean BP of each session was the average of the first and second readings (the third reading was excluded).
-
(4)
Method 4: The HBP measured on the first evening and on the first morning were excluded. The mean HBP of the first day was the average of the HBP measured on the second evening and on the second morning. The mean BP of each session was the average of the second and third readings (the first reading was excluded).
-
(5)
Method 5: All HBP measurements were included. The mean HBP of the first day was the average of the HBP measured on the first evening and on the first morning.
The reliability of HBP averaging methods was evaluated as follows. The first, second, and third readings of each morning and evening HBP measurement were compared using ANOVA. The mean of each morning and evening HBP reading (mean of three readings, mean of first two readings, and mean of second and third readings) was compared over 7 days using ANOVA. The cumulatively averaged SBP and DBP of HBP measurements were compared with the average 24-h SBP and DBP using an intraclass correlation coefficient (ICC). The similarity between cumulatively averaged SBP and DBP of HBP measurement of successive days and all of the measurement days (excluding the first measurement day for methods 1, 2, 3, and 4, and including the first measurement day for method 5) was assessed using the Pearson correlation coefficient. The limits of agreement and bias between cumulatively averaged SBP and DBP of HBP measurements from successive days and all the measurement days were calculated using a Bland–Altman plot.
The diagnostic accuracy of the five methods of averaging HBP measurements was evaluated as follows. The diagnostic sensitivity, specificity, positive predictive value, and negative predictive value of each HBP measurement method according to the cumulatively averaged days were calculated using the 24-h ABP measurement as the reference standard method. The diagnostic agreement of a diagnosis based on the cumulatively averaged HBP of successive days with a diagnosis based on the average of all measurement days, previous averaged days, and 24-h ABP was assessed with kappa statistics (κ). Statistical analyses were performed using MedCalc version 15.8 (MedCalc Software bvba; Ostend, Belgium) and SigmaPlot version 13.0 (Systat Software, LaJolla, CA, USA). A p-value <0.05 was considered statistically significant.
Results
Characteristics of study population
Of the 319 individuals referred to the study, 157 participants who completed the study protocol without missing even one HBP measurement for 7 days and had a valid 24-h ABP measurement were included in the final analysis. The reasons for exclusion were as follows: 22 withdrew their consent, 1 took antihypertensive medication, 9 refused the 24-h ABP measurement, 3 refused the HBP measurement, 21 had invalid data for the ABP measurement, and 106 had invalid HBP measurements (one or more missing measurements, i.e., <42 measurements).
The clinical characteristics of the patients are summarized in Table 1. Among the 157 participants, hypertension was diagnosed in 125 (79.6%) by 24-h ABP measurement. The proportion of male sex, current smoking status, and diabetes in the hypertensive subjects was significantly higher than that in the normotensive subjects.
Reliability of HBP according to the average HBP
As shown in Fig. 2, the first reading of the morning SBP measurements was higher than the second and third readings on the first and fourth day and the third reading on the third and seventh day. The first reading of evening SBP measurements was higher than the third reading on the first and fourth day. No difference was found between the DBP of morning and evening measurements.
Triplicate morning and evening home blood pressure reading for 7 days. a Morning systolic blood pressure, b morning diastolic blood pressure, c evening systolic blood pressure, and d evening diastolic blood pressure. Data are expressed as the mean ± standard deviation. *p < 0.05 vs. second and third readings. †p < 0.05 vs. third reading
The average of the triplicate readings of the evening SBP on day 1 was higher than the evening SBP on days 6 and 7 (Figure S1a). The average of the first and second reading of the evening SBP on day 1 was higher than that of evening SBP on days 4–7 (Figure S1b). The average of the second and third readings of the evening SBP on day 1 was higher than the evening SBP on days 6 and 7 (Figure S1c). Morning SBP and morning and evening DBP did not differ between the days according to the BP averaging method.
Among the three averaging methods, the average of the first and second readings was the highest, followed by the average of the three readings as the second highest, and the lowest was the average of the second and third readings (Table 2). The difference was significant but small.
Reliability of average HBP according to the cumulative measurement days
In the analysis comparing the average HBP according to the cumulative measurement days to the HBP averaged for 6 or 7 days, depending on the method (Fig. 3, Table S1), the Pearson correlation coefficient of SBP was >0.990 from the average of five measurement days in methods 1, 2, and 3 and from the average of six measurement days in methods 4 and 5. The correlation of DBP was >0.990 from the average of five measurement days in methods 1, 2, 3, and 5 and from the average of six measurement days in method 4.
The Bland–Altman plot analysis between the average BP of all measurement days according to each method and the cumulatively averaged BP revealed a continuous reduction of bias and limits of agreement with increasing numbers of averaged days (Figures S2–6).
Reliability of HBP compared with ABP as a reference
From the average of three measurement days, the ICC of HBP compared with the 24-h ABP showed an excellent correlation (≥0.75) [16] that increased steadily with increasing averaged days of HBP measurement (Fig. 4, Table S2). The ICC of SBP and DBP was higher than 0.770 from the average of five measurement days in methods 1 and 2, and from the average of three measurement days in method 5. The ICC of method 4 was more than 0.770 from the average of six measurement days for SBP and seven measurement days for DBP.
Diagnostic accuracy of HBP measurements according to the averaging method
The diagnostic power of each method was compared with the diagnosis of hypertension using the 24-h ABP measurement (Table 3). The sensitivity, specificity, positive predictive value, and negative predictive value of HBP measurements in the diagnosis of hypertension did not change with an increasing cumulative number of averaged days of HBP. Compared with the diagnosis by 24-h ABP, diagnosis by cumulatively averaged HBP showed fair to good agreement (kappa statistics) [16]. The areas under the receiver operating characteristic curve (AUCROC) of each method (excluding first measurement days for methods 1–4) were 0.739–0.759 when five measurement days were averaged, 0.731–0.747 when six measurement days were averaged, and 0.743–0.755 when seven measurement days were averaged. No difference in AUCROC was found between methods.
The diagnostic agreement of the cumulatively averaged HBP measurements, compared with a diagnosis by averaged HBP for 6 or 7 days (depending on the method) as a reference, and diagnosis by averaged HBP of previous days was nearly perfect (kappa ≥ 0.9) from the average of five measurement days (Fig. 5, Table S3).
Discussion
The major findings of the present study are as follows. First, although a significant difference was found between the average of three readings and two readings (average of the first and second readings and average of the second and third readings), no difference in both the diagnostic accuracy and reliability was noted between methods. Second, discarding the HBP measurement of the first day did not improve the diagnostic accuracy. Third, the reliability and diagnostic accuracy of HBP increased steadily with increasing averaged days of HBP measurement and reached a plateau on day 5 in each method. Finally, the diagnostic accuracy of HBP measurements, which was evaluated using sensitivity, specificity, positive and negative predictive values, kappa statistics, and areas under the receiver operating characteristic curve, was not different between the methods.
In general, many practice guidelines recommend HBP measurements in the morning and evening [1, 2, 7, 17]. However, a controversy exists about averaging HBP readings. The European Society of Hypertension and the Japanese Society of Hypertension recommend taking two measurements per occasion and averaging these readings [1, 2]. The American Heart Association recommends at least two measurements per occasion [7], and the Korean Society of Hypertension guidelines proposes taking one to three measurements per occasion and averaging the three readings [6]. In the present study, the first reading of BP per occasion was higher than the second and/or third readings, which was consistent with the results of previous studies [9, 11, 18]. The average of the first and second readings was the highest, followed by the average of all three readings, and the average of the second and third readings was the lowest. However, differences in sensitivity, specificity, positive and negative predictive values, and kappa statistics were not found. Moreover, the reliability of HBP was not different when HBP was measured for 5 or more days in comparison with the average of the 24-h ABP or the 7 days HBP (or 6 days discarding the first measurement day). Therefore, averaging three or two readings (average of the first and second readings and average of the second and third readings) did not affect the diagnostic accuracy of HBP measurement.
The European Society of Hypertension and the Canadian Hypertension Education Program (CHEP) have recommended discarding the BP reading of the first monitoring day [1, 5]. However, the evidence for excluding the first monitoring day is very weak as is noted in the CHEP (Grade D) [5], and only few studies have shown evidence supporting that the accuracy of the diagnosis of hypertension is improved when BP measured on the first monitoring day is excluded [19]. In the study of Nunan et al. [19], the inclusion of readings taken on the first monitoring day had no clinical impact on diagnostic accuracy. However, they included cases with a minimum number of eight readings (1 a.m. and 1 p.m. daily readings on ≥4 days) during the first week, which was less than that of our study (42 readings for 7 days). In the present study, when average HBP was compared with the average 24-h ABP or 7 days HBP (or 6 days HBP discarding the first measurement day), the correlation of the average HBP excluding the first measurement day reached a plateau from the average of four measurement days. The correlation of the averaged HBP including the first monitoring day reached a plateau from the average of five measurement days. This result indicates that a monitoring period of five or more days is adequate, which was also suggested by Stergiou et al. [20].
The present study has potential limitations that should be noted. First, we used a 24-h ABP measurement as the reference for the diagnosis of hypertension. Attempts to define the best schedule for HBP measurement should also take into account cardiovascular outcomes. In the analysis of an international database that included three populations (Ohasama study, Finn-Home study, and Tsurugaya study) [8], the optimal number of days needed for the diagnosis and prediction of cardiovascular events was inconsistent. Similar to the observation from the HONEST study [21], even a single HBP measurement was a potent predictor of cardiovascular events. However, 7 days of measurement were needed to diagnose hypertension reliably. In addition to these inconsistent results, the international database included studies with different HBP measurement schedules (once in the morning and evening for up to 1 month, once in the morning for up to 1 month, and twice in the morning and evening for 7 consecutive days) and different methods in the assessment of cardiovascular events. Therefore, a larger population-based cardiovascular outcome study in a controlled condition is needed to assess the optimal schedule for HBP measurement. Second, our study population was comprised entirely of Asians and, therefore, the findings may not be generalizable to other ethnic groups.
The strengths of this study are as follows. First, we enrolled patients who were suspected of having hypertension and excluded those who were taking antihypertensive agents to determine the optimal schedule of HBP measurement in the diagnosis of hypertension. Thus, we could eliminate the effects of antihypertensive drugs. Second, many studies measure HBP from 6:00 p.m. to 9:00 p.m. in accordance with the Western lifestyle. However, in Asia, including Korea, measuring BP at home between 6:00 p.m. and 9:00 p.m. is difficult, because many people eat dinner out. Although the Japanese guidelines recommended that measurements be taken before bedtime, no controlled studies have been conducted to evaluate the optimal schedule of HBP measurement. Therefore, in this study, evening HBP was measured between 9:00 and 11:00 p.m. to minimize interference with daily life. Third, previous studies have included participants who had lost some measurements during the study period. However, to obtain the most accurate results, the present study included only participants who completed 42 HBP measurements over 7 days and who had a valid 24-h ABP measurement. Finally, we used an HBP measurement device with a built-in memory to prevent patients from reporting errors or inaccurate recordings.
In conclusion, we suggest performing HBP measurements for 5 days or more, including morning and evening measurements, taking two or more measurements per occasion, and averaging all of the readings as the optimal schedule for HBP measurement in the diagnosis of hypertension.
References
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Bohm M, Christiaens T, Cifkova R, De Backer G, Dominiczak A, Galderisi M,Grobbee DE, Jaarsma T, Kirchhof P, Kjeldsen SE, Laurent S, Manolis AJ, Nilsson PM, Ruilope LM, Schmieder RE, Sirnes PA, Sleight P,Viigimaa M, Waeber B, Zannad F,TaskForce Members. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens. 2013;31:1281–357.
Shimamoto K, Ando K, Fujita T, Hasebe N, Higaki J, Horiuchi M, Imai Y, Imaizumi T, Ishimitsu T, Ito M, Ito S, Itoh H, Iwao H, Kai H, Kario K, Kashihara N, Kawano Y, Kim-Mitsuyama S, Kimura G, Kohara K, Komuro I, Kumagai H, Matsuura H, Miura K, Morishita R, Naruse M, Node K, Ohya Y, Rakugi H, Saito I, Saitoh S, Shimada K, Shimosawa T, Suzuki H, Tamura K, Tanahashi N, Tsuchihashi T, Uchiyama M, Ueda S, Umemura S, Japanese Society of Hypertension Committee for Guidelines for the Management of Hypertension. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2014). Hypertens Res. 2014;37:253–390.
Shimbo D, Abdalla M, Falzon L, Townsend RR, Muntner P. Role of ambulatory and home blood pressure monitoring in clinical practice: a narrative review. Ann Intern Med. 2015;163:691–700.
Yarows SA, Staessen JA. How to use home blood pressure monitors in clinical practice. Am J Hypertens. 2002;15:93–6.
Leung AA, Nerenberg K, Daskalopoulou SS, McBrien K, Zarnke KB, Dasgupta K,Cloutier L, Gelfer M, Lamarre-Cliche M, Milot A, Bolli P, Tremblay G, McLean D, Tobe SW,Ruzicka M, Burns KD, Vallee M, Prasad GV, Lebel M, Feldman RD, Selby P, Pipe A,Schiffrin EL, McFarlane PA, Oh P, Hegele RA, Khara M, Wilson TW, Penner SB, Burgess E, Herman RJ, Bacon SL, Rabkin SW, Gilbert RE, Campbell TS, Grover S, Honos G, Lindsay P, Hill MD, Coutts SB, Gubitz G, Campbell NR, Moe GW, Howlett JG, Boulanger JM, Prebtani A,Larochelle P, Leiter LA, Jones C, Ogilvie RI, Woo V, Kaczorowski J, Trudeau L, Petrella RJ,Hiremath S, Drouin D, Lavoie KL, Hamet P, Fodor G, Gregoire JC, Lewanczuk R, Dresser GK, Sharma M, Reid D, Lear SA, Moullec G, Gupta M, Magee LA, Logan AG, Harris KC,Dionne J, Fournier A, Benoit G, Feber J, Poirier L, Padwal RS, Rabi DM, CHEP Guidelines Task Force. Hypertension Canada’s 2016 Canadian Hypertension Education Program Guidelines for blood pressure measurement, diagnosis, assessment of risk, prevention, and treatment of hypertension. Can J Cardiol. 2016;32:569–88.
Shin J, Park JB, Kim KI, Kim JH, Yang DH, Pyun WB, Kim YG, Kim GH, Chae SC, Guideline Committee of the Korean Society of Hypertension 2013 Korean Society of Hypertension guidelines for the management of hypertension: Part I—Epidemiology and diagnosis of hypertension. Clin Hypertens. 2015;21:1.
Whelton PK, Carey RM, Aronow WS, Casey DE, Jr., Collins KJ, Dennison Himmelfarb C, DePalma SM, Gidding S, Jamerson KA, Jones DW, MacLaughlin EJ, Muntner P, Ovbiagele B, Smith Jr SC, Spencer CC, Stafford RS, Taler SJ, Thomas RJ, Williams Sr KA, Williamson JD, Wright Jr JT. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension 2017 2018;71:1269–1324.
Niiranen TJ, Asayama K, Thijs L, Johansson JK, Hara A, Hozawa A, Tsuji I, Ohkubo T, Jula AM, Imai Y, Staessen JA, IDHOCO Investigators. Optimal number of days for home blood pressure measurement. Am J Hypertens. 2015;28:595–603.
Verberk WJ, Kroon AA, Kessels AG, Lenders JW, Thien T, van Montfrans GA, Smit AJ, de Leeuw PW. The optimal scheme of self blood pressure measurement as determined from ambulatory blood pressure recordings. J Hypertens. 2006;24:1541–8.
Stergiou GS, Nasothimiou EG, Kalogeropoulos PG, Pantazis N, Baibas NM. The optimal home blood pressure monitoring schedule based on the Didima outcome study. J Hum Hypertens. 2010;24:158–64.
Stergiou GS, Skeva II, Zourbaki AS, Mountokalakis TD. Self-monitoring of blood pressure at home: how many measurements are needed? J Hypertens. 1998;16:725–31.
Johansson JK, Niiranen TJ, Puukka PJ, Jula AM. Optimal schedule for home blood pressure monitoring based on a clinical approach. J Hypertens. 2010;28:259–64.
Almeida AE, Stein R, Gus M, Nascimento JA, Arevalo JR, Fuchs FD, Ribeiro JP. Improved diagnostic accuracy of a 3-day protocol of home blood pressure monitoring for the diagnosis of arterial hypertension. Blood Press Monit. 2013;18:119–26.
Park JS, Rhee MY, Namgung J, Lee SY, Cho DK, Choi TY, Kim SY, Kim JY, Park SM, Choi JH, Lee JH, Kim HY. Comparison of optimal diagnostic thresholds of hypertension with home blood pressure monitoring and 24-hour ambulatory blood pressure monitoring. Am J Hypertens. 2017;30:1170–6.
O’Brien E, Asmar R, Beilin L, Imai Y, Mallion JM, Mancia G, Mengden T, Myers M, Padfield P, Palatini P, Parati G, Pickering T, Redon J, Staessen J, Stergiou G, Verdecchia P, European Society of Hypertension Working Group on Blood Pressure Monotoring. European Society of Hypertension recommendations for conventional, ambulatory and home blood pressure measurement. J Hypertens. 2003;21:821–48.
Fleiss JL, Levin B, Paik MC. Statistical methods for rates and proportions. Hoboken. 3rd edn. New Jersey, USA: John Wiley & Sons; 2003. p. 598–626.
Daskalopoulou SS, Rabi DM, Zarnke KB, Dasgupta K, Nerenberg K, Cloutier L, Gelfer M, Lamarre-Cliche M, Milot A, Bolli P, McKay DW, Tremblay G, McLean D, Tobe SW, Ruzicka M, Burns KD, Vallee M, Ramesh Prasad GV, Lebel M, Feldman RD, Selby P, Pipe A, Schiffrin EL, McFarlane PA, Oh P, Hegele RA, Khara M, Wilson TW, Brian Penner S, Burgess E, Herman RJ, Bacon SL, Rabkin SW, Gilbert RE, Campbell TS, Grover S, Honos G, Lindsay P, Hill MD, Coutts SB, Gubitz G, Campbell NR, Moe GW, Howlett JG, Boulanger JM, Prebtani A, Larochelle P, Leiter LA, Jones C, Ogilvie RI, Woo V, Kaczorowski J, Trudeau L, Petrella RJ, Hiremath S, Stone JA, Drouin D, Lavoie KL, Hamet P, Fodor G, Gregoire JC, Fournier A, Lewanczuk R, Dresser GK, Sharma M, Reid D, Benoit G, Feber J, Harris KC, Poirier L, Padwal RS. The 2015 Canadian Hypertension Education Program recommendations for blood pressure measurement, diagnosis, assessment of risk, prevention, and treatment of hypertension. Can J Cardiol. 2015;31:549–68.
Kawabe H, Saito I. Correlation of repeated measurements of home blood pressure on one occasion and diagnosis of hypertension: study by measurement over seven consecutive days. Clin Exp Hypertens. 2008;30:79–85.
Nunan D, Thompson M, Heneghan CJ, Perera R, McManus RJ, Ward A. Accuracy of self-monitored blood pressure for diagnosing hypertension in primary care. J Hypertens. 2015;33:755–62.
Stergiou GS, Ntineri A. The optimal schedule for self-home blood pressure monitoring. J Hypertens. 2015;33:693–7.
Saito I, Kario K, Kushiro T, Teramukai S, Yaginuma M, Mori Y, Okuda Y, Shimada K. Home blood pressure and cardiovascular risk in treated hypertensive patients: the prognostic value of the first and second measurements and the difference between them in the HONEST study. Hypertens Res. 2016;39:857–62.
Acknowledgements
This study was supported by a grand from Dong-A ST Co. Ltd., Seoul, Korea. The sponsor was not involved in study design, study conduction, data interpretation, or the writing of the manuscript. This study was supported by a grand from Dong-A ST Co. Ltd., Seoul, Korea.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M-YR has received lecture honoraria from Pfizer Inc., LG Life Sciences Ltd, Bayer Korea Ltd, Hanmi Pharm. Co., Ltd, Yuhan Co., Ltd, Boryung Pharmaceutical Co. Ltd, and a research grant from Boryung Pharmaceutical Co., Ltd and Dong-A Pharmaceutical Co., Ltd.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Rhee, MY., Kim, J.Y., Kim, JH. et al. Optimal schedule of home blood-pressure measurements for the diagnosis of hypertension. Hypertens Res 41, 738–747 (2018). https://doi.org/10.1038/s41440-018-0069-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-018-0069-6
This article is cited by
-
Diagnostic performance of clinic and home blood pressure measurements compared with ambulatory blood pressure: a systematic review and meta-analysis
BMC Cardiovascular Disorders (2020)
-
Validation of an automated home blood pressure measurement device in oldest-old populations
Hypertension Research (2020)