Abstract
Data sources An electronic search was conducted using EMBASE, LILACS, PubMed, SciELO, Scopus, Web of Science, and two grey literature data sources. All issues of nine dentistry journals and relevant chapters in four endodontic textbooks were manually searched.
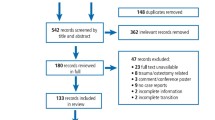
Study selection Abstracts of all the studies that were identified during the electronic and manual searches were obtained and screened independently by two reviewers in order to select clinical studies, case series, or case reports describing subcutaneous emphysema that occurred in adult patients during or immediately after root canal treatment.
Data extraction and synthesis Predetermined data were extracted from each study independently by two reviewers and organised into data tables. All disagreements were resolved through discussion with a third reviewer. The data obtained were combined through a narrative synthesis.
Results Following full-text evaluation according to the inclusion criteria, 51 articles that described 65 cases of subcutaneous emphysema were included. There were 36 case reports and 15 case series. The condition was mainly reported in female patients and maxillary teeth. While the age of the patients ranged from 18 to 63 years, this demographic information was missing from a few studies. Details on the involved tooth and diagnosis were also missing from several articles. In most of the cases, subcutaneous emphysema developed during initial root canal treatment. The diagnosis was mainly based on intraoral, plain facial, neck, or chest radiographs, while computed tomography (CT) scans were obtained in fewer cases. The majority of the patients were referred to a different practice, a hospital or university clinic for the management of the condition by more specialised healthcare practitioners. In addition to drying root canals using air pressure, irrigation with hydrogen peroxide, and the air-water spray produced by handpieces, it was reported that laser-produced spray and ozone gas infiltration may also be the culprits of subcutaneous emphysema. The signs and symptoms resolve within 17 days. Its management mostly remains empirical and involves the use of antibiotics, analgesics, local application of cold or hot compresses, or administration of oxygen and hospitalisation, among other methods.
Conclusions The systematic review showed that subcutaneous emphysema can occur during both surgical and nonsurgical endodontic treatment. Air streams or air-water sprays should not be directed toward the root canals or areas with mucosal discontinuity. None of the management approaches were clearly associated with a faster recovery. The review asked for developing guidelines in order to avoid unnecessary or potentially harmful interventions.
Similar content being viewed by others
A Commentary on
Fasoulas A, Boutsioukis C, Lambrianidis T.
Subcutaneous emphysema in patients undergoing root canal treatment: a systematic review of the factors affecting its development and management. Int Endod J 2019: DOI: 10.1111/iej.13,183. [Epub ahead of print].

GRADE rating
Commentary
Evidence-based dentistry integrates the patient's needs and preferences, the dental practitioner's clinical expertise, and the most current scientific evidence. Champions of this approach share their knowledge and skills to promote evidence-based dentistry in practice, guiding colleagues, patients, and policy makers in the application of critical thinking skills and evidence-based decision-making.1 Although subcutaneous emphysema is seen as an unfortunate event that is less frequently encountered during the endodontic treatment, dental practitioners should have good knowledge of this topic and be aware that this condition can contribute to serious health consequences. The commentary serves as an extension of the facts mentioned in the systematic review, while seeking to further discuss this subject. Fasoulas et al.2 presented evidence on the factors that may affect the development of subcutaneous emphysema during root canal treatment and on the management of this condition. The systematic review described the quality requirements during the critical appraisal of eligible studies (that is, selection bias, patient information and history, diagnosis, details of the endodontic treatment and management) and provided the predetermined data items extracted from individual studies (that is, patient information and history, diagnosis, information on the endodontic treatment and management) along with a list of excluded studies. The reviewed cases more often involved female patients and maxillary teeth. In addition to drying root canals using air pressure, irrigation with hydrogen peroxide and the air-water spray produced by handpieces, it was reported that laser-produced spray and ozone gas infiltration may also be to blame for subcutaneous emphysema. While the signs and symptoms resolve within approximately two weeks, its management mostly remains empirical and ranges from the use of antibiotics, analgesics and local application of ice packs, to administration of oxygen and hospitalisation. It appears that these approaches do not necessarily lead to a faster recovery. Perhaps of particular concern is the fact that in one of the reviewed studies3 endodontic treatment was carried out prior to there being a clear diagnosis. Rubber dam isolation was rarely used in the reviewed cases. Since many of the included articles have been published over 20 years ago, clinical techniques, materials, and equipment may differ from those used today in clinical practice. Also, it is quite interesting that many of the cases have been reported by physicians without a background in dentistry. For instance, according to Sujeet & Shankar,4 a radiograph of the neck showed emphysema with prevertebral air in the cervical soft tissues, likely caused by means of a 'high-speed dental drill' that introduced air through the soft tissue adjacent to the roots of the mandibular molars. Using CT imaging may help with identifying areas affected and associated risks, while cone beam computed tomography (CBCT) in particular may be used to confirm the clinical diagnosis and establish the tissue planes involved (Graham et al. 2018).5 Dental practitioners should be aware of the factors leading to subcutaneous emphysema and regularly consult the literature to improve their knowledge on this topic. Moreover, treatment guidelines should be followed to prevent undesired clinical outcomes, especially at university clinics. Future articles must thoroughly document certain information about study participants (for example, gender, age), diagnosis, and clinical interventions, so that dental practitioners can use the best available evidence in their clinical decision-making.
References
Clarkson J E, Bonetti D. Why be an evidence-based dentistry champion? J Evid Based Dent Pract 2009; 9: 145-150.
Fasoulas A, Boutsioukis C, Lambrianidis T. Subcutaneous emphysema in patients undergoing root canal treatment: a systematic review of the factors affecting its development and management. Int Endod J 2019. DOI: 10.1111/iej.13183.
Marmolejo A T, Molano-Valencia P E. Enfisema orofacial. Rev ADM 2011; 68: 136-139.
Sujeet K, Shankar S. Images in clinical medicine. Prevertebral emphysema after a dental procedure. N Engl J Med 2007; 356: 173.
Graham C, Chung M, Feinberg L, O'Neill F, Balmer C. Child's play - an unforeseen complication of surgical emphysema. Oral Surg 2018; 11: 318-322.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pais, E. The causes of subcutaneous emphysema of relevance to dental practitioners?. Evid Based Dent 20, 111–112 (2019). https://doi.org/10.1038/s41432-019-0065-y
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41432-019-0065-y