Abstract
This case report describes conservative management of an uncomplicated enamel dentine crown fracture with tooth fragment reattachment. This time efficient technique allowed for achievement of an optimal aesthetic result with simultaneous patient and clinician satisfaction. The outright disadvantages of extensive restorative material usage are therefore largely avoided. The use of a minimal preparation and fracture line embracing technique using composite resin proved successful in this case.
Similar content being viewed by others
Key points
-
Reviews tooth fragment reattachment techniques as a treatment option for a fractured incisor.
-
Highlights consideration to factors that may influence the long-term prognosis of the bonded fragment.
-
Emphasises the importance of long-term monitoring for a technique with unknown longevity.
Case report
An 18-year-old male presented as an emergency patient to general practice with a fractured upper central incisor. He gave a history of a traumatic blow to the upper jaw during a footballing incident one day previous. Upon parental advice, the fragment was stored in a container of milk since the incident. He was not experiencing any pain and therefore the patient's sole complaint was the aesthetic concern of the fractured incisor. Medically, the patient was fit and well with no known drug allergies. He reported no prior history of trauma to the dentition. The patient is a keen football player with regular training sessions four times per week. He was seen one week prior for a recall examination with a sole diagnosis of generalised dental plaque biofilm induced gingivitis on an intact periodontium.1
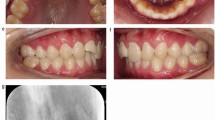
Extra oral examination was unremarkable with no evidence of any contusions, lacerations or bony fractures. Intra oral soft tissues highlighted no abnormalities. Special investigations of the fractured upper right central incisor were performed. The tooth had normal mobility for an upper central incisor and a negative result to percussion testing. Sensibility testing proved positive with Endo-Frost and electronic pulp testing (Fig. 1).
Radiographic Investigations
Radiographically, a long cone periapical of the upper right central incisor was taken for tooth displacement and root fracture assessment. There were no indications for radiographs of the lips or cheeks as the full-sized fragment was available (Fig. 2).
Radiographic report (Fig. 3): Grade 1 periapical upper right one. Enamel and dentine loss visible. Wide root canal with no coronal pulpal exposure. Complete root formation and closed apex with no evidence of periapical radiolucencies. No signs of tooth displacement or root fracture.
Diagnosis
Following history taking, examination and special tests the following diagnoses were devised:
Generalised dental plaque biofilm-induced gingivitis on an intact periodontium1
Uncomplicated enamel dentine crown fracture of upper right one with no pulpal exposure
Full sized fractured fragment available with minimal loss of tooth tissue.
Treatment options
The risks and benefits of each treatment option were discussed in detail with the associated prognosis of each treatment choice.
Smoothen sharp edges of remaining tooth (risk of sensitivity/pulpal death/reduced aesthetics)
Reattachment of broken tooth fragment (risk of de-bond/colour changes/unknown longevity)
Direct restoration with resin-based composite (risk of de-bond/aesthetic considerations)
Indirect restoration with a full coverage crown (destructive/risk of pulpal death)
Extraction and implant placement (risk of biological/mechanical failures).
The best outcome can be expected when the crown fragment is in a single piece and can be reapproximated with its source (remaining tooth) with minimal loss of tooth structure.2
Treatment
Following assessment of the tooth fragment, minimal loss of tooth structure was evident. There had been sufficient hydration of the fragment while stored in milk with no marked colour changes. The patient opted for tooth fragment reattachment with a double chamfer and composite resin technique.2 Detailed assessment of the occlusion was required to ensure removal of any potential interferences in guidance movements. Fabrication of an athletic mouth guard was planned; this was to be worn during contact/sporting activities. The patient was encouraged to maintain good oral hygiene practice and avoid incising into hard items to reduce the risk of fragment debond.
A shade was taken by positioning the patient at a 45-degree angle using natural daylight. The chroma, hue and value of the fractured incisor were analysed adjacent to the classical A1-D4 shade guide and an appropriate shade match undertaken. The chasm between the tooth and fragment was gently prepared to a double chamfer. The tooth fragment was reattached using an iBond etch 35 gel (etch and rinse) and iBond total etch system. The chasm was filled with Unodent dentine shade B2 and enamel shade A2 to achieve an undetectable transition. Curing of the composite resin was completed using a Bluephase LED unit with a light intensity of 1200 mW/cm2. The final restoration was polished with a combination of white stone-finishing burs and abrasive discs to achieve a high gloss and smooth surface. This ensured improved wear resistance, discouragement of biofilm retention and reduction of marginal staining.3
Over contour technique (using composite resin to 'embrace' the fracture line after rebonding) recovered 97% of a tooth's natural strength2 (Figs 4-8).
Follow up
6-8 weeks: Clinical and radiographic examination
1 year: Clinical and radiographic examination.4
Long term management
See Figures 9 to 11.
One week review
See Figures 12 to 13.
Six week review
See Figures 14 to 15.
At the six-week clinical and radiographic review according to the IADT guidelines4 the upper right central incisor remained vital and demonstrated normal mobility. There had been minimal discolouration of the bonded tooth fragment and the patient was pleased with the outcome. There was a negative result to percussion testing and radiographically (Fig. 15) there appears to be no signs of any abnormal changes. All aspects of the clinical and radiographic examination appear consistent with the hydrated fragment successfully bonded to a vital tooth.
Outcome
The patient remains asymptomatic six months following reattachment and is under monitor. The athletic mouthguard is worn four times per week during sporting/contact activities. The patient is extremely grateful and pleased with the outcome.
Discussion
The long-term prognosis of a tooth with an uncomplicated enamel-dentine crown fracture is dictated by the pulpal response to the sustained injury. The aim for the clinician is to minimise pulpal inflammation by achieving an effective dentine seal. This limits bacterial ingress and improves the long-term prognosis.5
No material can identically reproduce the natural aesthetics and contours of tooth structure. Conventional use of resin-based composites often requires extensive bevelling and overlaying of the restorative material to improve aesthetics. This subjects the restoration to risk of marginal discolouration and breakdown, compromising retention of the restoration.6
There are many advantages to tooth fragment reattachment. An aesthetically pleasing result can be achieved due to a perfect shade and translucency match. The incisal edge of the fragment will wear naturally at a similar rate to the adjacent teeth. This technique produces a positive emotional response for the patient and good clinician satisfaction as the natural tooth contour and contacts are reproduced. In addition, tooth fragment reattachment is an economical technique and less time consuming for the clinician.7,8,9
Various techniques have been proposed for tooth fragment reattachment: pins, posts, undercut preparations within the pulpal chamber, circumferential external bevel of the enamel and V shaped notches within the enamel. Reports suggest no consistencies in a particular technique having a higher success rate than another.9
Disadvantages of tooth fragment reattachment are also important to consider. Aesthetics can be compromised if the fragment is allowed to dehydrate following fracture, with potential for the bonded tooth fragment to discolour over time following reattachment. The fractured tooth will require continuous monitoring and there is unknown longevity of the bonded restoration. It has been shown there is 'predicted' eventual separation of the repaired tooth fragment due to the bonded junction progressively breaking down.10
Consideration should be given to the storage condition of the fractured segments and the influence on the long-term prognosis. Collapse and dehydration of the fractured segment can be avoided by storage within sterile saline at 37 degrees Celsius. This prevents dimensional change of the fragment.7,9 Rinsing of the tooth fragment in 0.12% chlorhexidine solution can be considered as a step to disinfection.6,7 Other suitable storage mediums include: milk, water and saline.7,11 In this particular case, the fragment was retained in milk until reattachment. This may have contributed to the success of the restoration.
Another key consideration for tooth fragment reattachment is the choice of adhesive material. In vitro studies3,7 comparing unfilled bonding resins have highlighted fracture strengths similar to that of an intact tooth. Retention of the fractured segment with a total etch technique proved to be greater than with enamel etching alone.2 A study by Singhal12 compared the use of composite resin, compomer, resin modified glass ionomer and resin cements as the adhesive choice for incisor fragment reattachment. The highest fracture strength was seen with use of composite resin. Pusman8 studied the use of bonding resin with or without use of composite resin to reattach tooth fragments. The outcomes revealed composite resin increased the fracture resistance when no preparation was carried out.
A systematic review concluded tooth fragment reattachment without further preparation; attached using an adhesive system, associated with an intermediate composite was the indicated technique. This technique ensures adequate recovery of some of the strength lost.13 Another systematic review described simple reattachment as the ideal technique when complete fragment adaptation is possible.14 In those cases where complete fragment adaptation is not achievable and a minimal gap or fracture line is visible, consideration should be paid to patients rising aesthetic demands. A study analysing in vitro tooth fragment reattachment techniques stated the optimal technique is dependent upon the nature of the fracture and the adaptation between the fractured aspects of the tooth.13 Over contouring with composite resin is sometimes necessary to meet the rising high aesthetic demands of patients to ensure an indiscernible fracture line. Each case should be treated individually and the optimal technique applied dependent on the clinical situation and patient's expectations.
Conclusion
Tooth fragment reattachment is a conservative, time efficient method of meeting a patient's aesthetic demands and minimising long term complications. Considerations should be paid to the various factors which may influence the long-term prognosis of a fractured tooth. Although fragment reattachment techniques have an unknown longevity, this can be a simple alternative to more extensive use of restorative materials with their associated pitfalls.
References
Papapanou P N, Sanz M, Buduneli N et al. Periodontitis: Consensus report of Workgroup 2 of the 2017. World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Clin Periodontol 2018; 45(Suppl 20): S162-S170.
Macedo GV, Ritter A V. Essentials of rebonding tooth fragments for the best functional and esthetic outcomes. Pediatr Dent 2009; 31: 110-116.
Ahmad I. Minimum intervention, maximum satisfaction: reconstruction guided by a fragment. J Cosmetic Dent 2012; 28(1): spring.
International Association of Dental Traumatology. Dental Trauma Guidelines. Revised 2012. Available at: https://www.iadt-dentaltrauma.org/1-9%20%20iadt%20guidelines%20combined%20-%20lr%20-%2011-5-2013.pdf (accessed 18 December 2018).
Olsburgh S, Jacoby T, Krejci I. Crown fractures in the permanent dentition: pulpal and restorative considerations. Dent Traumatol 2002; 18: 103-115.
Terry D A. Adhesive reattachment of a tooth fragment: the biological restoration. Pract Proced Aesthet Dent 2003; 15: 403-409.
Sapna C, Renjith Kumar M, Rakesh R, Rajan P R. Uncomplicated crown fracture: A biological management option. Int J Applied Dent Sci 2014; 1: 15-17. Available at: http://www.oraljournal.com/vol1issue1/pdf/23.1.pdf (accessed August 2019).
Pusman E, Cehreli Z C, Altay N, Unver B, Saracbasi O, Ozgun G. Fracture resistance of tooth fragment reattachment: effects if different preparation techniques and adhesive materials. Dent Traumatol 2010; 26: 9-15.
Chu F C S, Yim T M, Wei S H Y. Clinical considerations for reattachment of tooth fragments. Quintessence Int 2000; 31: 385-391.
Maitin N, Maitin S N, Rastogi K, Bhushan R. Fracture tooth fragment reattachment. BMJ Case Rep 2013; doi: 10.1136/bcr2013009183.
Shirani F, Malekipour M R, Tahririan D, Manesh V S. Effect of storage environment on the bond strength of reattachment of crown fragments to fractured teeth. J Conserv Dent 2011; 14: 269-272.
Singhal R, Pathak A. Comparison of the fracture resistance of reattached incisor tooth fragments using 4 different materials. J Indian Soc Pedod Prev Dent 2012; 30: 310-316.
de Sousa A P B R, França K, de Lucas, Rezende LV M et al. In vitro tooth reattachment techniques: A systematic review. Dent Traumatol 2018; 34: 297-310.
Garcia F C P, Poubel D L N, Almeida J C F et al. Tooth fragment reattachment techniques - A systematic review. Dent Traumatol 2018; 34: 135-143.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Panchal, D. A case report of uncomplicated crown fracture: tooth fragment reattachment. Br Dent J 227, 259–263 (2019). https://doi.org/10.1038/s41415-019-0630-y
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41415-019-0630-y
This article is cited by
-
Long term attachment
British Dental Journal (2019)