Abstract
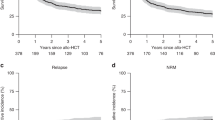
Relapsed/refractory Peripheral T-cell Lymphomas are characterized by a poor prognosis, especially for patients who are not candidates for allogeneic hematopoietic stem-cell transplantation. We conducted a retrospective analysis on 73 consecutive patients affected by relapsed/refractory T-Cell lymphomas who were considered eligible for allogeneic transplant. All patients were referred at our center from 2001 to 2017. With a median follow-up of 40 months (range 9–192 months), 4-year second-line failure-free survival and overall survival were 14% (CI95%:7–24) and 34% (CI95%:22–46). Extranodal disease at relapse (HR 2.25, CI95%: 1.11–4.56, p = 0.02) and first-line failure-free survival < 12 months (HR 3.37, CI95%: 1.67–6.88, p < 0.01) had a negative prognostic impact on survival. Only 45 out of 73 patients (62%) received allogeneic transplant. For the 28 (38%) patients who did not proceed to transplant, disease progression was the main reason for ineligibility. Median survival from time of transplant was 31 months (range 4–185 months). A first-line failure-free survival < 12 months had a negative prognostic impact also for allografted patients (2-year survival 45% vs 73%, p = 0.03) identifying a very high-risk population which requires novel treatments pre and post-transplant to obtain a long-term disease control.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Weisenburger DD, Savage KJ, Harris NL, Gascoyne RD, Jaffe ES, MacLennan KA. et al.Peripheral T-cell lymphoma, not otherwise specified: A report of 340 cases from the International Peripheral T-cell Lymphoma Project.Blood. 2011;117:3402–8.
Swerdlow SH, Campo E, Pileri SA, Harris NL, Stein Harald, Siebert R. et al.The 2016 revision to the World Health Organization (WHO) classification of lymphoid neoplasms.Blood. 2016;127:2375–90.
d’Amore F, Gaulard P, Trümper L, Corradini P, Kim WS, Specht L, et al. Peripheral T-cell lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 2015. Sep;26 Suppl 5:v108-15. https://doi.org/10.1093/annonc/mdv201.
Schmitz N, Trümper L, Ziepert M, Nickelsen M, Ho AD, Metzner B. et al.Treatment and prognosis of mature T-cell and NK-cell lymphoma: an analysis of patients with T-cell lymphoma treated in studies of the German High-Grade Non-Hodgkin Lymphoma Study Group.Blood. 2010;116:3418–25.
Mak V, Hamm J, Chhanabhai M, Shenkier T, Klasa R, Sehn LH. et al. Survival of patients with peripheral T-cell lymphoma after first relapse or progression: Spectrum of disease and rare long-term survivors. J Clin Oncol. 2013;31:1970–6.
Kharfan-Dabaja MA, Kumar A, Ayala E, Hamadani M, Reimer P, Gisselbrecht C, et al. Clinical practice recommendations on indication and timing of hematopoietic cell transplantation in mature T cell and NK/T cell lymphomas: an international collaborative effort on behalf of the Guidelines Committee of the American Society for Blood and Marrow Transplantation. Biol Blood Marrow Transplant. 2017;23:1826–38. https://linkinghub.elsevier.com/retrieve/pii/S1083879117306237.
Corradini P, Dodero A, Zallio F, Caracciolo D, Casini M, Bregni M. et al.Graft-versus-lymphoma effect in relapsed peripheral T-cell non-Hodgkin’s lymphomas after reduced-intensity conditioning followed by allogeneic transplantation of hematopoietic cells. J Clin Oncol. 2004;22:2172–6.
Dodero A, Spina F, Narni F, Patriarca F, Cavattoni I, Benedetti F, et al. Allogeneic transplantation following a reduced-intensity conditioning regimen in relapsed/refractory peripheral T-cell lymphomas: long-term remissions and response to donor lymphocyte infusions support the role of a graft-versus-lymphoma effect. Leukemia. 2012;26:520–6. http://www.nature.com/articles/leu2011240.
Shustov AR, Gooley TA, Sandmaier BM, Shizuru J, Sorror ML, Sahebi F. et al. Allogeneic haematopoietic cell transplantation after nonmyeloablative conditioning in patients with T-cell and natural killer-cell lymphomas. Br J Haematol. 2010;150:170–8.
Smith SM, Burns LJ, van Besien K, LeRademacher J, He W, Fenske TS, et al. Hematopoietic cell transplantation for systemic mature T-cell non-Hodgkin lymphoma. J Clin Oncol. 2013;31:3100–9. https://doi.org/10.1200/JCO.2012.46.0188.
Harris NL, Jaffe ES, Stein H, Banks PM, Chan JK, Cleary ML, et al. A revised European-American classification of lymphoid neoplasms: a proposal from the International Lymphoma Study Group. Blood. 1994;84:1361–92. http://www.ncbi.nlm.nih.gov/pubmed/8068936.
Jaffe ES, Harris, NS WHO Classification Tumors of Hematopoietic and Lymphoid Tissues. (Eds.) Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H. Lyon Thiele J, France; IARC Publication 2001.
International Non-Hodgkin's Lymphoma Prognostic Factors Project. A predictive model for aggressive non-Hodgkin’s lymphoma. N Engl J Med. 1993;329:987–94.
Gallamini A. Peripheral T-cell lymphoma unspecified (PTCL-U): a new prognostic model from a retrospective multicentric clinical study. Blood. 2004;103:2474–9. https://doi.org/10.1182/blood-2003-09-3080.
Cheson BD, Horning SJ, Coiffier B, Shipp MA, Fisher RI, Connors JM, et al. Report of an international workshop to standardize response criteria for non-Hodgkin’s lymphomas. J Clin Oncol. 1999;17:1244–1244. https://doi.org/10.1200/JCO.1999.17.4.1244.
Cheson BD, Pfistner B, Juweid ME, Gascoyne RD, Specht L, Horning SJ, et al. Revised response criteria for malignant lymphoma. J Clin Oncol. 2007;25:579–86. https://doi.org/10.1200/JCO.2006.09.2403.
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, et al. Defining the intensity of conditioning regimens: working definitions. Biol Blood Marrow Transplant. 2009;15:1628–33. http://linkinghub.elsevier.com/retrieve/pii/S1083879109003231
Sorror ML. Hematopoietic cell transplantation (HCT)-specific comorbidity index: a new tool for risk assessment before allogeneic HCT. Blood. 2005;106:2912–9. https://doi.org/10.1182/blood-2005-05-2004.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J. et al. 1994 consensus conference on acute GVHD grading. Bone Marrow Transplant. 1995;15:825–8.
Shulman HM, Sullivan KM, Weiden PL, McDonald GB, Striker GE, Sale GE, et al. Chronic graft-versus-host syndrome in man. A long-term clinicopathologic study of 20 Seattle patients. Am J Med. 1980;69:204–17. http://www.ncbi.nlm.nih.gov/pubmed/6996481.
Chihara D, Fanale MA, Miranda RN, Noorani M, Westin JR, Nastoupil LJ, et al. The survival outcome of patients with relapsed/refractory peripheral T-cell lymphoma-not otherwise specified and angioimmunoblastic T-cell lymphoma. Br J Haematol. 2017;176:750–8. https://doi.org/10.1111/bjh.14477.
Iacobelli S. Suggestions on the use of statistical methodologies in studies of the European Group for Blood and Marrow Transplantation. Bone Marrow Transplant. 2013;48(S1):S1–37. http://www.nature.com/articles/bmt2012282.
StataCorp. Stata Statistical Software: Release 13. College Station, TX: StataCorp LP; 2013.
R Development Core Team. R: A language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2013. ISBN 3-900051-07-0 U http://www. R org/.
Dodero A, Carniti C, Raganato A, Vendramin A, Farina L, Spina F, et al. Haploidentical stem cell transplantation after a reduced-intensity conditioning regimen for the treatment of advanced hematologic malignancies: posttransplantation CD8-depleted donor lymphocyte infusions contribute to improve T-cell recovery. Blood. 2009;113:4771–9. https://doi.org/10.1182/blood-2008-10-183723.
Dodero A, Carrabba M, Milani R, Rizzo E, Raganato A, Montefusco V. et al. Reduced-intensity conditioning containing low-dose alemtuzumab before allogeneic peripheral blood stem cell transplantation: graft-versus-host disease is decreased but T-cell reconstitution is delayed. Exp Hematol. 2005;33:920–7.
Le Gouill S, Milpied N, Buzyn A, Peffault De Latour R, Vernant J-P, Mohty M, et al. Graft-versus-lymphoma effect for aggressive T-cell lymphomas in adults: a study by the Société Française de Greffe de Moëlle et de Thérapie Cellulaire. J Clin Oncol. 2008;26:2264–71. https://doi.org/10.1200/JCO.2007.14.1366.
Kyriakou C, Canals C, Finke J, Kobbe G, Harousseau J-L, Kolb H-J, et al. Allogeneic stem cell transplantation is able to induce long-term remissions in angioimmunoblastic T-cell lymphoma: a retrospective study from the Lymphoma Working Party of the European Group for Blood and Marrow Transplantation. J Clin Oncol. 2009;27:3951–8. https://doi.org/10.1200/JCO.2008.20.4628.
Hsu Y-T, Tsai H-J, Chang JS, Li S-S, Tang J-L, Yeh S-P, et al. Stem cell transplantation for T-cell lymphomas in Taiwan. Bone Marrow Transplant. 2018;53:993–1000. http://www.nature.com/articles/s41409-018-0116-6.
Bellei M, Foss FM, Shustov AR, Horwitz SM, Marcheselli L, Kim WS, et al. The outcome of peripheral T-cell lymphoma patients failing first-line therapy: a report from the prospective, International T-Cell Project. Haematol. 2018;103:1191–7. https://doi.org/10.3324/haematol.2017.186577.
Rohlfing S, Dietrich S, Witzens-Harig M, Hegenbart U, Schönland S, Luft T. et al. The impact of stem cell transplantation on the natural course of peripheral T-cell lymphoma: a real-world experience. Ann Hematol. 2018;97:1241–50.
Pro B, Advani R, Brice P, Bartlett NL, Rosenblatt JD, Illidge T, et al. Brentuximab Vedotin (SGN-35) in patients with relapsed or refractory systemic anaplastic large-cell lymphoma: results of a phase II study. J Clin Oncol. 2012;30:2190–6. https://doi.org/10.1200/JCO.2011.38.0402.
Gambacorti Passerini C, Farina F, Stasia A, Redaelli S, Ceccon M, Mologni L, et al. Crizotinib in advanced, chemoresistant anaplastic lymphoma kinase–positive lymphoma patients. J Natl Cancer Inst. 2014;106. https://doi.org/10.1093/jnci/djt378
Gutierrez-Garcia G, Garcia-Herrera A, Cardesa T, Martinez A, Villamor N, Ghita G, et al. Comparison of four prognostic scores in peripheral T-cell lymphoma. Ann Oncol. 2011;22:397–404. https://doi.org/10.1093/annonc/mdq359.
Maurer MJ, Ellin F, Srour L, Jerkeman M, Bennani NN, Connors JM, et al. International assessment of event-free survival at 24 months and subsequent survival in peripheral T-cell lymphoma. J Clin Oncol. 2017;35:4019–26. https://doi.org/10.1200/JCO.2017.73.8195.
Maurer MJ, Ghesquières H, Jais J-P, Witzig TE, Haioun C, Thompson CA, et al. Event-free survival at 24 months is a robust end point for disease-related outcome in diffuse large B-cell lymphoma treated with immunochemotherapy. J Clin Oncol. 2014;32:1066–73. https://doi.org/10.1200/JCO.2013.51.5866.
Hallek M, Fischer K, Fingerle-Rowson G, Fink A, Busch R, Mayer J, et al. Addition of rituximab to fludarabine and cyclophosphamide in patients with chronic lymphocytic leukaemia: a randomised, open-label, phase 3 trial. Lancet. 2010;376:1164–74. http://linkinghub.elsevier.com/retrieve/pii/S0140673610613815
Casulo C, Byrtek M, Dawson KL, Zhou X, Farber CM, Flowers CR, et al. Early relapse of follicular lymphoma after rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone defines patients at high risk for death: an analysis from the National LymphoCare Study. J Clin Oncol. 2015;33:2516–22. https://doi.org/10.1200/JCO.2014.59.7534.
Hapgood G, Zheng Y, Sehn LH, Villa D, Klasa R, Gerrie AS, et al. Evaluation of the risk of relapse in classical hodgkin lymphoma at event-free survival time points and survival comparison with the general population in British Columbia. J Clin Oncol. 2016;34:2493–500. https://doi.org/10.1200/JCO.2015.65.4194. Available from
Majithia N, Rajkumar SV, Lacy MQ, Buadi FK, Dispenzieri A, Gertz MA, et al. Early relapse following initial therapy for multiple myeloma predicts poor outcomes in the era of novel agents. Leukemia. 2016;30:2208–13. http://www.nature.com/articles/leu2016147.
Loirat M, Chevallier P, Leux C, Moreau A, Bossard C, Guillaume T, et al. Upfront allogeneic stem-cell transplantation for patients with nonlocalized untreated peripheral T-cell lymphoma: an intention-to-treat analysis from a single center. Ann Oncol. 2015;26:386–92. https://academic.oup.com/annonc/article/26/2/386/2800589.
Acknowledgements
The authors would like to thank all patients and their families. Supported in part by Associazione Italiana contro le Leucemia-Linfomi e Mielomi (AIL) and Associazione Italiana Ricerca sul Cancro (AIRC).
Author information
Authors and Affiliations
Contributions
Conception and design: A.M., N.C., P.C.. Collection and assembly of data: N.C., N.M.. Data analysis: A.M., N,M.. Interpretation: All authors. Manuscript writing: First draft prepared by A.M. and N.M. All authors helped in revising the manuscript. Final approval of manuscript: All authors
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Mussetti, A., Martinetti, N., Cieri, N. et al. Real-life feasibility of salvage allogeneic transplantation in peripheral T-cell lymphomas. Bone Marrow Transplant 54, 1237–1244 (2019). https://doi.org/10.1038/s41409-018-0417-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-018-0417-9