Abstract
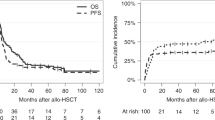
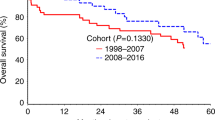
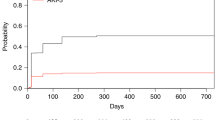
Myeloablative conditioning regimens with significant extramedullary toxicity result in high rates of renal dysfunction including acute kidney injury (AKI). Here we examine the incidence and impact of a reduced creatinine clearance (below 60 ml/min) before day 90 (early renal dysfunction, ERD) in patients receiving the reduced toxicity fludarabine/i.v. busulfan (FluBu4) regimen prior to allogeneic transplant. Of 91 patients receiving FluBu4, 62 (68%) developed ERD. ERD resulted in worse overall survival (OS, 2.2 years versus median not reached, p = 0.04) and progression-free survival (PFS, 1.6 years versus median not reached, p = 0.02). This was due to a higher relapse rate (34% versus 14%, p = 0.03) in the ERD group. In time-dependent Cox proportional hazards models adjusted for age, ERD was associated with worse OS (hazard ratio [HR] 2.67, 95% confidence interval [CI] 1.06–4.21, p = 0.043) and PFS (HR 2.52, 95% CI 1.17–4.28, p = 0.030). Patients with ERD surviving 1 year had an increased risk of chronic kidney disease (CKD, OR 10; 95% CI 1.4–112.6, p = 0.0181), which was associated with worse survival (3.2 years versus median not reached, p = 0.002). ERD after FluBu4 is therefore a poor prognostic sign resulting in increased relapse, worse OS, and high risk of CKD at 1 year.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Hingorani S. Renal complications of hematopoietic-cell transplantation. N Engl J Med. 2016;374:2256–67. https://doi.org/10.1056/NEJMra1404711.
Hingorani SR, Guthrie K, Batchelder A, Schoch G, Aboulhosn N, Manchion J, et al. Acute renal failure after myeloablative hematopoietic cell transplant: incidence and risk factors. Kidney Int. 2005;67:272–7. https://doi.org/10.1111/j.1523-1755.2005.00078.x.
Schrier RW, Parikh CR. Comparison of renal injury in myeloablative autologous, myeloablative allogeneic and non-myeloablative allogeneic haematopoietic cell transplantation. Nephrol Dial Transplant. 2005;20:678–83. https://doi.org/10.1093/ndt/gfh720.
Hahn T, Rondeau C, Shaukat A, Jupudy V, Miller A, Alam AR, et al. Acute renal failure requiring dialysis after allogeneic blood and marrow transplantation identifies very poor prognosis patients. Bone Marrow Transplant. 2003;32:405–10. https://doi.org/10.1038/sj.bmt.1704144.
Pinana JL, Valcarcel D, Martino R, Barba P, Moreno E, Sureda A, et al. Study of kidney function impairment after reduced-intensity conditioning allogeneic hematopoietic stem cell transplantation. A single-center experience. Biol Blood Marrow Transplant. 2009;15:21–9. https://doi.org/10.1016/j.bbmt.2008.10.011.
Liu H, Li YF, Liu BC, Ding JH, Chen BA, Xu WL, et al. A multicenter, retrospective study of acute kidney injury in adult patients with nonmyeloablative hematopoietic SCT. Bone Marrow Transplant. 2010;45:153–8. https://doi.org/10.1038/bmt.2009.99.
Kersting S, Koomans HA, Hene RJ, Verdonck LF. Acute renal failure after allogeneic myeloablative stem cell transplantation: retrospective analysis of incidence, risk factors and survival. Bone Marrow Transplant. 2007;39:359–65. https://doi.org/10.1038/sj.bmt.1705599.
Tokgoz B, Kocyigit I, Polat G, Eser B, Unal A, Kaynar L, et al. Acute renal failure after myeloablative allogeneic hematopoietic stem cell transplantation: incidence, risk factors, and relationship with the quantity of transplanted cells. Ren Fail. 2010;32:547–54. https://doi.org/10.3109/08860221003728721.
Abboud I, Porcher R, Robin M, de Latour RP, Glotz D, Socie G, et al. Chronic kidney dysfunction in patients alive without relapse 2 years after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2009;15:1251–7. https://doi.org/10.1016/j.bbmt.2009.05.016.
Shimoi T, Ando M, Munakata W, Kobayashi T, Kakihana K, Ohashi K, et al. The significant impact of acute kidney injury on CKD in patients who survived over 10 years after myeloablative allogeneic SCT. Bone Marrow Transplant. 2013;48:80–4. https://doi.org/10.1038/bmt.2012.85.
Parikh CR, Schrier RW, Storer B, Diaconescu R, Sorror ML, Maris MB, et al. Comparison of ARF after myeloablative and nonmyeloablative hematopoietic cell transplantation. Am J Kidney Dis. 2005;45:502–9. https://doi.org/10.1053/j.ajkd.2004.11.013.
Pinana JL, Perez-Pitarch A, Garcia-Cadenas I, Barba P, Hernandez-Boluda JC, Esquirol A, et al. A time-to-event model for acute kidney injury after reduced-intensity conditioning stem cell transplantation using a tacrolimus- and sirolimus-based graft-versus-host disease prophylaxis. Biol Blood Marrow Transplant. 2017;23:1177–85. https://doi.org/10.1016/j.bbmt.2017.03.035.
Chunduri S, Dobogai LC, Peace D, Saunthararajah Y, Chen HY, Mahmud N, et al. Comparable kinetics of myeloablation between fludarabine/full-dose busulfan and fludarabine/melphalan conditioning regimens in allogeneic peripheral blood stem cell transplantation. Bone Marrow Transplant. 2006;38:477–82. https://doi.org/10.1038/sj.bmt.1705480.
Beri R, Chunduri S, Sweiss K, Peace DJ, Mactal-Haaf C, Dobogai LC, et al. Reliability of a pretransplant i.v. BU test dose performed 2 weeks before myeloablative FluBu conditioning regimen. Bone Marrow Transplant. 2010;45:249–53. https://doi.org/10.1038/bmt.2009.133.
Chunduri S, Dobogai LC, Peace D, Saunthararajah Y, Quigley J, Chen YH, et al. Fludarabine/i.v. BU conditioning regimen: myeloablative, reduced intensity or both? Bone Marrow Transplant. 2008;41:935–40. https://doi.org/10.1038/bmt.2008.13.
Fein JA, Shimoni A, Labopin M, Shem-Tov N, Yerushalmi R, Magen H, et al. The impact of individual comorbidities on non-relapse mortality following allogeneic hematopoietic stem cell transplantation. Leukemia. 2018;32:1787–94. https://doi.org/10.1038/s41375-018-0185-y.
Shouval R, de Jong CN, Fein J, Broers AEC, Danylesko I, Shimoni A, et al. Baseline renal function and albumin are powerful predictors for allogeneic transplantation-related mortality. Biol Blood Marrow Transplant. 2018. https://doi.org/10.1016/j.bbmt.2018.05.005.
Jagasia MH, Greinix HT, Arora M, Williams KM, Wolff D, Cowen EW, et al. National Institutes of Health Consensus Development Project on Criteria for Clinical Trials in Chronic Graft-versus-Host Disease: I. The 2014 Diagnosis and Staging Working Group report. Biol Blood Marrow Transplant. 2015;21:389–401.e1. https://doi.org/10.1016/j.bbmt.2014.12.001.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J, et al. 1994 Consensus Conference on Acute GVHD Grading. Bone Marrow Transplant. 1995;15:825–8.
Thomas ME, Blaine C, Dawnay A, Devonald MA, Ftouh S, Laing C, et al. The definition of acute kidney injury and its use in practice. Kidney Int. 2015;87:62–73. https://doi.org/10.1038/ki.2014.328.
Kersting S, Dorp SV, Theobald M, Verdonck LF. Acute renal failure after nonmyeloablative stem cell transplantation in adults. Biol Blood Marrow Transplant. 2008;14:125–31. https://doi.org/10.1016/j.bbmt.2007.09.016.
Parikh CR, Sandmaier BM, Storb RF, Blume KG, Sahebi F, Maloney DG, et al. Acute renal failure after nonmyeloablative hematopoietic cell transplantation. J Am Soc Nephrol. 2004;15:1868–76.
Andersson BS, de Lima M, Thall PF, Wang X, Couriel D, Korbling M, et al. Once daily i.v. busulfan and fludarabine (i.v. Bu-Flu) compares favorably with i.v. busulfan and cyclophosphamide (i.v. BuCy2) as pretransplant conditioning therapy in AML/MDS. Biol Blood Marrow Transplant. 2008;14:672–84. https://doi.org/10.1016/j.bbmt.2008.03.009.
Jo T, Arai Y, Kondo T, Kitano T, Hishizawa M, Yamashita K, et al. Chronic kidney disease in long-term survivors after allogeneic hematopoietic stem cell transplantation: retrospective analysis at a single institute. Biol Blood Marrow Transplant. 2017;23:2159–65. https://doi.org/10.1016/j.bbmt.2017.08.016.
Ando M, Ohashi K, Akiyama H, Sakamaki H, Morito T, Tsuchiya K, et al. Chronic kidney disease in long-term survivors of myeloablative allogeneic haematopoietic cell transplantation: prevalence and risk factors. Nephrol Dial Transplant. 2010;25:278–82. https://doi.org/10.1093/ndt/gfp485.
Bellomo R, Ronco C, Kellum JA, Mehta RL, Palevsky P. Acute Dialysis Quality Initiative w. Acute renal failure—definition, outcome measures, animal models, fluid therapy and information technology needs: the Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group. Crit Care. 2004;8:R204–12. https://doi.org/10.1186/cc2872.
Mehta RL, Kellum JA, Shah SV, Molitoris BA, Ronco C, Warnock DG, et al. Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care. 2007;11:R31 https://doi.org/10.1186/cc5713.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
PRP receives honoraria and consulting fees from Celgene, Amgen, and Janssen.
Rights and permissions
About this article
Cite this article
Sweiss, K., Calip, G.S., Oh, A.L. et al. Renal dysfunction within 90 days of FluBu4 predicts early and late mortality. Bone Marrow Transplant 54, 980–986 (2019). https://doi.org/10.1038/s41409-018-0361-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-018-0361-8