Abstract
Chronic rhinosinusitis with nasal polyps (CRSwNP) is characterized by type 2 inflammation with accumulation of activated group 2 innate lymphoid cells (ILC2s) and elevation of thymic stromal lymphopoietin (TSLP). A member of the TNF superfamily (TNFSF), TNFSF15, is known to induce the production of type 2 cytokines in ILC2s. Although ILC2s have been implicated in CRSwNP, the presence and role of TNFSFs in ILC2-mediated type 2 inflammation in CRSwNP has not been elucidated. Here, we investigate the involvement of TNFSFs in ILC2-mediated type 2 inflammation in CRSwNP. We found that receptor activator of NF-κB (RANK) ligand (RANK-L (TNFSF11)) was significantly elevated in nasal polyps (NPs), and that the receptor of RANK-L, RANK, was expressed on ILC2s in human peripheral blood and NPs. An agonistic antibody against RANK induced production of type 2 cytokines in human ILC2s, and TSLP significantly enhanced this reaction. The membrane-bound RANK-L was detected mainly on CD45 + immune cells, including TH2 cells in NPs. The co-culture of NP-derived ILC2s and TH2 cells significantly enhanced production of type 2 cytokines, and anti-RANK-L monoclonal antibody suppressed this enhancement. In conclusion, RANK-L, together with TSLP, may play an inductive role in the ILC2-mediated type 2 inflammation in CRSwNP.
Similar content being viewed by others
Introduction
Chronic rhinosinusitis with nasal polyps (CRSwNP) is a common chronic inflammatory disease in the human upper airways and sinuses that affects ~0.5–4% of the general population in Europe, Asia, and the USA.1,2 Immunologically, CRSwNP is characterized by type 2 inflammation with eosinophilia and high levels of type 2 cytokines, including IL-5 and IL-13.1,3,4,5 It has been reported that TH2 cells,6 mast cells7, and group 2 innate lymphoid cells (ILC2s),3,8,9,10 which are able to produce type 2 cytokines, are accumulated in nasal polyps (NPs).9,10 Among these cells, ILC2s are considered to be a key initiator and amplifier for type 2 inflammation due to the ability of these cells to produce type 2 cytokines via innate immune stimulation.10 We recently found that ILC2s were not only elevated but also activated and releasing type 2 cytokines in NPs.9 Thus far, the mechanisms controlling activation of ILC2s in NPs are still not understood. Epithelial cell-derived cytokines, IL-25, IL-33 and thymic stromal lymphopoietin (TSLP) are well known to control ILC2-mediated production of type 2 cytokines.3,11 We recently characterized the presence of these epithelial-derived cytokines in NPs from CRSwNP patients in Chicago, Illinois, and reviewed published studies for these cytokines in NPs.12 Interestingly, TSLP was certainly elevated in CRSwNP in most studies.12,13 In contrast, IL-25 and IL-33 were not always elevated in NPs; there were mixed results in other parts of the world and thus, the relative importance of IL-25 and IL-33 in CRSwNP remains uncertain.12 Since TSLP alone does not induce the production of type 2 cytokines in ILC2s, and IL-25 and IL-33 are not elevated in NPs,8,14 other factors, in addition to TSLP, may play important but unrecognized roles in ILC2-mediated type 2 inflammation in CRSwNP.
Recently, two separate groups have reported that death receptor 3 (DR3, TNF receptor superfamily 25 [TNFRSF25]) was expressed on human blood ILC2s, and that a ligand TNF-like cytokine 1A (TL1A, TNF superfamily 15 [TNFSF15]) induced the production of IL-5 and IL-13 in human ILC2s.15,16 They also found that TL1A synergistically enhanced IL-25- and IL-33-mediated production of IL-5 and IL-13 in human ILC2s.15 Furthermore, several groups also found that TNF receptor II (TNFRII [TNFRSF1B]) and glucocorticoid-induced TNFR-related protein (GITR [TNFRSF18]) were expressed on ILC2s, and their ligands, TNF, and GITR ligand induced type 2 cytokine production in ILC2s.10,17,18 Most members of the TNF receptor superfamily (TNFRSFs), including DR3, TNFRII, and GITR, share a nuclear factor-kappa B (NF-κB) signal transduction pathway and play an important role in immunity and inflammation.10 However, the presence of TL1A, TNF, GITR ligand, and other TNF ligand superfamilies (TNFSFs) and their role in ILC2-mediated type 2 inflammation in NPs has not been well elucidated.
For this study, we hypothesized that members of TNFSF are closely involved in the ILC2-mediated type 2 inflammation in NPs, and that the elevation of TSLP enhances the role of TNFSFs in CRSwNP. We therefore set out to define the presence of TNFSFs, their function in human ILC2s, and their contribution to type 2 inflammation in CRSwNP.
Results
The elevation of RANK-L in NPs
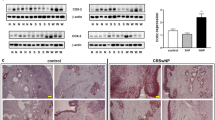
To clarify the expression of TNFSFs in NPs, we analyzed our published microarray data in NPs compared with normal control uncinate tissue (UT)19 (GEO series GSE36830) and found that mRNAs for lymphotoxin beta (TNFSF3), receptor activator of NF-κB ligand (RANK-L, TNFSF11), and B-cell activating factor of the TNF family (BAFF, TNFSF13B) were significantly elevated in NPs (not shown). Since we previously reported the elevation of BAFF in NPs,20 we performed qPCR for lymphotoxin beta and RANK-L and confirmed that they were both significantly elevated in NPs (n = 39) compared with control UT (n = 21) (Fig. 1a, and not shown). We next examined the presence of receptors for these ligands on ILC2s by flow cytometry. The gating strategy used to identify ILC2s is shown in Supplementary Fig. 1. We found that the receptor for RANK-L, RANK (receptor activator of NF-κB, TNFRSF11A), but not the receptors for lymphotoxin beta or BAFF, were expressed on both blood and NP ILC2s (n = 6) (Fig. 1b, and not shown). Interestingly, cell-surface expression of RANK was significantly higher on NP ILC2s than blood ILC2s (Fig. 1b, c). Based on the initial screen results and the presence of the receptor on human ILC2s, we decided to focus further studies on the RANK-L cascade in NPs. We next confirmed the presence of RANK-L protein in tissue homogenates and found that RANK-L protein was significantly elevated in NPs from patients with both nonsteroidal anti-inflammatory drug (NSAID) tolerant (n = 69) and sensitive (n = 12) CRSwNP compared with control UT (n = 13) (Fig. 1d). Since the endogenous decoy receptor of RANK-L, osteoprotegerin (OPG), may be present in NPs and it may affect RANK-L-mediated reactions, we also measured OPG mRNA by qPCR. Interestingly, we found that OPG was significantly reduced in NPs compared with control UT (Fig. 1e, left). Consequently, the RANK-L/OPG ratio was significantly elevated in NPs compared with control UT (Fig. 1e, right).
Elevation of RANK-L in NPs and expression of RANK on human ILC2s. a, e The total RNA was extracted from whole control UT (Con, n = 21) and NP tissue (n = 39) from patients with CRSwNP. Expression of mRNAs for RANK-L and OPG was analyzed using qPCR. Gene expression was normalized to a housekeeping gene, β-glucuronidase (GUSB), and expression levels were shown as % expression of GUSB. b Representative histograms of flow-cytometric plots for RANK on ILC2s in blood and NPs (n = 6) are shown. Levels of cell surface expression of RANK on ILC2s are shown by geometric mean fluorescence intensity (gMFI). c A comparison of the gMFI ratio of RANK to isotype IgG1 between blood ILC2s and NP ILC2s is shown. d Protein extracts were generated from control UT (Con, n = 13), NPs from CRSwNP patients who did not have NSAID sensitivity (n = 69) and who did have NSAID sensitivity (n = 12). Expression of RANK-L protein in tissue homogenates was determined by Luminex. RANK-L protein concentrations were normalized to the concentration of total protein. *p < 0.05, **p < 0.01, and ***p < 0.001 were calculated by Mann–Whitney test (a, e), one-way ANOVA Kruskal–Wallis test (d), paired t test (b), and Wilcoxon test (c)
RANK-L induced production of type 2 cytokines in human ILC2s
Since we found elevation of ligand, RANK-L, in NPs and expression of receptor, RANK, on human ILC2s, we investigated the effect of the RANK-L to RANK cascade on human ILC2s sorted from peripheral blood and NP tissue. We found that an agonistic anti-RANK antibody but not goat control IgG significantly induced IL-5 and IL-13 on both blood and NP ILC2s (Fig. 2a, b, not shown). Although it was not potent as agonistic antibody, recombinant RANK-L also significantly induced the production of IL-13 in both blood and NP ILC2s (Supplementary Fig. 2a).
RANK-mediated production of type 2 cytokines in ILC2s. a Sorted blood ILC2s (n = 14) and b NP ILC2s (n = 8) were cultured in the presence or absence of 10 µg/ml agonistic anti-RANK antibody (a-RANK) for 4 days. c–e Sorted blood ILC2s were cultured with 10 ng/ml TSLP, 10 µg/ml a-RANK and their combination (c, n = 12) in the presence or absence of 0.001% dimethyl sulfoxide (DMSO) (vehicle control), 100 nM dexamethasone (Dex) (d, n = 7), and 10 µM IMD0354 (IMD) (e, n = 3) for 4 days. The concentrations of IL-5 and IL-13 were measured by Luminex assay. Not significant (NS), *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001 were calculated by Wilcoxon test (a, b) and one-way ANOVA Kruskal–Wallis test (c–e)
TSLP is known to act in synergy with IL-25 and IL-33,14,21,22 and is significantly elevated in NPs (Supplementary Fig. 3a).12,13 We therefore examined whether RANK-L can act in synergy with TSLP on blood ILC2s. We found that TSLP significantly and synergistically enhanced RANK-L and anti-RANK antibody-mediated production of type 2 cytokines in blood ILC2s (Fig. 2c; Supplementary Fig. 2b).
The binding of ligand, RANK-L, to receptor, RANK, mainly activates the NF-κB signaling pathway.23 We stimulated blood ILC2s with an agonistic anti-RANK antibody and TSLP, and examined the effect of glucocorticoid (dexamethasone, an inhibitor of the NF-κB pathway) and IMD0354, an inhibitor of IκB kinase-β1, on the production of IL-5 and IL-13. We found that dexamethasone and IMD0354 significantly suppressed RANK-mediated production of IL-5 and IL-13 in blood ILC2s (Fig. 2d, e). We previously reported that dexamethasone, IL-10, and transforming growth factor beta (TGF-β) inhibited IL-33-mediated production of type 2 cytokines in human ILC2s.22 We therefore investigated the inhibitory effects of IL-10 and TGF-β and found that IL-10 but not TGF-β1 significantly suppressed RANK-mediated production of type 2 cytokines in blood ILC2s (Supplementary Fig. 2c, d). These results suggest that NF-κB may be a key shared transcription factor controlling RANK-L- and IL-33-mediated induction of type 2 cytokines in human ILC2s.
The source of RANK-L in NPs
RANK-L is a homotrimeric membrane-bound protein that can be released from the cell surface by cleavage.24 Both the soluble and membrane-bound forms of RANK-L are known to activate the receptor, RANK.24,25 To examine the source of RANK-L in nasal mucosa, we used immunohistochemistry and flow cytometry. Immunohistochemical analysis showed that RANK-L was mainly detected on submucosal inflammatory cells, and RANK-L-positive cells were significantly elevated in NPs compared with control UT (Fig. 3a–e). Flow-cytometric analysis showed that the frequency of RANK-L + cells (median, range) in NPs was significantly higher in CD45 + cells (88.9%, 68.8–100%) compared with CD45− cells (11.1%, 0–31.3%) (n = 12) (Fig. 3f). These results suggest that the main source of RANK-L in NPs is CD45 + immune cells and therefore we focused further studies on immune cells.
The main source of RANK-L was immune cells in NPs. The presence of RANK-L-positive cells was assessed by immunohistochemistry. a Negative control antibody staining in NP is shown. b, c Representative immunostaining for RANK-L in NP (b) and control UT (c) are shown. d High-magnification image of (b) is shown. e The number of RANK-L-positive cells in control UT (n = 8) and NPs (n = 11) was counted. f (left) Representative-flow cytometric plots for RANK-L + cells in NPs are shown. We gated on single, live, RANK-L-positive (RANK-L + ) cells compared with isotype control IgG2b. f (right) RANK-L + cells were further separated into CD45 + and CD45− populations, and the frequency of RANK-L + cells in the two populations was calculated (n = 12). *p < 0.05 and ****p < 0.0001 were calculated by Mann–Whitney test (e) and pair t test (f)
As RANK-L is known to be expressed on activated T cells, B cells, and basophils in humans,26,27,28,29 we first determined the frequency of RANK-L + cells in CD3 + T cells, CD19 + B cells, granulocytes (side scatter [SSC] high cells), and CD3−CD19− non-granulocytes (CD3−CD19mid-low cells) (Supplementary Fig. 4a). We found that RANK-L was mainly detected on CD3−CD19− cells (median, range; 77.3%, 59.8–96.1%) and CD3 + T cells (12.5%, 2.6–24.8%) compared with CD19 + B cells (6.4%, 1.1–11.2%) and granulocytes (1.66%, 0–3.9%) within the population of CD45 + cells (n = 7) (Fig. 4a). The percentage of RANK-L + cells in each cell type is shown in Supplementary Fig. 4b, d. We first focused on CD3 + T cells and found that RANK-L was highly expressed on CRTH2 + CD4 + TH2 cells compared with CRTH2− CD4 + T cells and CD4− T cells in NPs (Fig. 4d, e; Supplementary Fig. 5a and not shown). We further analyzed CD3−CD19− cells and found that RANK-L + cells were mainly CD11c + cells, but not basophils (CD117− FcεRIa+), plasmacytoid dendritic cells (DCs) (BDCA4 +), macrophages (CD68 +), or mast cells (CD117 + FcεRIa +) (Fig. 4b; Supplementary Fig. 4c and not shown). Bando et al. have reported expression of both RANK-L and RANK on mouse group 3 ILCs (ILC3s).30 We also investigated whether RANK-L is expressed on ILC subsets and found that RANK-L was weakly detected on ILC2s and CRTH2− ILCs, which were a mixture of group 1 ILCs (ILC1s) and ILC3s (n = 5, Supplementary Fig. 6a). However, the expression of RANK-L on NP ILCs was similar to CRTH2−CD4 + T cells (Supplementary Fig. 6b). We therefore ruled out the importance of RANK-L in NP ILCs.
Identification of RANK-L expressing cells in NPs. a The frequency of granulocytes (Gran; SSChigh and CD45 + cells), CD19 + B cells (CD45 + CD19 + CD3− cells), CD3 + T cells (CD45 + CD3 + cells), and CD3− CD19−cells (SSC mid-low, CD45 + CD3− CD19mid-low cells) in RANK-L + CD45 + cells in NPs was calculated (n = 7). b The frequency of CD11c− cells and CD11c + cells in RANK-L + CD45 + cells is shown (n = 7). c The frequency of mDC1 (CD1chigh CD141− CD11c + cells), mDC2 (CD141 + CD1c− CD11c + cells), and CD11c + non-mDCs (CD1cmid-lowCD141− cells) in RANK-L + CD45 + cells in NPs is shown (n = 3). d, f Representative histograms of flow-cytometric plots and bar graphs for RANK-L on TH2 cells, CRTH2− CD4 + T cells (n = 9), CXCL16− HLA-DR + CD11c + cells, and CXCL16 + HLA-DR + CD11c + cells (n = 6), in NPs are shown. e, g Comparisons of the gMFI ratio of RANK-L to isotype IgG2b between TH2 cells and CRTH2−CD4 + T cells and between CXCL16 + cells, CXCL16− cells, and ILC2s are shown. Not significant (NS), *p < 0.05, **p < 0.01, and ****p < 0.0001 were calculated by one-way ANOVA Kruskal–Wallis test (a, g), Holm–Sidak’s multiple comparisons test (c), paired t test (d, f), and Wilcoxon test (b, e)
Since we found that a larger subset of RANK-L + CD11c + cells expressed human leukocyte antigen-D related (HLA-DR) (Supplementary Fig. 4d), we initially hypothesized that RANK-L + CD11c + cells were myeloid DCs (mDCs). However, the majority of these cells were not classical mDC1s (CD1c + ) or mDC2s (CD141 + ) in NPs (n = 3) (Fig. 4c; Supplementary Fig. 4e). It has been reported that a subset of intestinal DCs express a membrane-bound chemokine, CXCL16 on the cell surface and that these unique DCs interact with ILC3s via a CXCL16 receptor, a CXCR6-dependent manner in mice.31 Interestingly, we found that the expression of RANK-L was significantly higher on CXCL16 + HLA-DR + CD11c + cells (called CXCL16 + cells) rather than on CXCL16− HLA-DR + CD11c + cells (Fig. 4f, g; Supplementary Fig. 5b). These results suggest that RANK-L is mainly expressed on TH2 cells and CXCL16 + antigen presenting cells in NPs.
Chemokines may play a role on the interaction of RANK-L expressing cells and ILC2s in NPs
We hypothesized that chemokines might play a role in the co-localization of ILC2s with RANK-L + CXCL16 + cells, and TH2 cells in NPs. We first found that a CXCL16 receptor, CXCR6, was expressed on ILC2s in NPs (Fig. 5a). This suggests that RANK-L + CXCL16 + cells may be able to interact with ILC2s in a CXCL16-CXCR6-dependent manner in NPs. We next found a high level of CCR4 on both TH2 cells and ILC2s in NPs (Fig. 5b), which confirmed previous observations.21 We also found that mRNAs of the ligands for CCR4, CCL17, and CCL22 were significantly elevated in NP tissue compared with control UT (Fig. 5c). These results suggest that the accumulation of CCR4 ligands may play a role in recruiting ILC2s and TH2 cells to the same area within NPs.
The expression of CXCR6 and CCR4 on ILC2s and the elevation of CCL17 and CCL22 in NPs. a, b Representative histograms of flow-cytometric plots and bar graphs for CXCR6 (a, n = 6) in NP ILC2s and CCR4 (b, n = 5) in NP ILC2s and NP TH2 cells are shown. The total RNA was extracted from whole control UT tissue (Con, n = 21) and whole NP tissue (n = 39). c Expression of mRNAs for CCL17 and CCL22 was analyzed using qPCR. *p < 0.05, **p < 0.01, and ****p < 0.0001 were calculated by paired t test (a, b) and Mann–Whitney test (c)
TH2 cells and CXCL16 + cells enhanced type 2 cytokine production in ILC2s
Finally, we examined whether RANK-L + cells are able to enhance ILC2-mediated production of type 2 cytokines. We performed a (1:1) co-culture using ILC2s with TH2 cells, CRTH2− CD4 + T cells, or CXCL16 + cells sorted from NP tissue, and compared production of type 2 cytokines from co-culture and individual culture (Fig. 6a). We first found that NP ILC2s and TH2 cells (n = 12), but neither CXCL16 + cells (n = 4) nor CRTH2− CD4 + T cells (n = 10) released type 2 cytokines without stimulation (Supplementary Fig. 7). We then found that the co-culture of ILC2s with TH2 cells significantly enhanced the production of IL-5 and IL-13 (5.0-fold and 4.2-fold, respectively, n = 12), compared with the sum of individual cultures (Fig. 6c, d). In contrast, the co-culture of ILC2s with CRTH2− CD4 + T cells did not enhance the production of type 2 cytokines (Fig. 6b). Similarly, we found that the co-culture of ILC2s with CXCL16 + cells significantly enhanced the production of IL-5 and IL-13 (5.3-fold and 2.2-fold, respectively, n = 4, Fig. 6e, f). Finally, we found that a neutralizing anti-RANK-L antibody, denosumab, significantly suppressed the enhancement of type 2 cytokine production in the ILC2-Th2 cell co-culture (Fig. 6g). These results suggest that TH2 cells and CXCL16 + cells enhance production of type 2 cytokines in ILC2s via a RANK-L-mediated pathway, and that interaction between ILC2s and RANK-L + cells may play an important role in the amplification of type 2 inflammation in NPs.
Co-culture of ILC2s with RANK-L expressing cells enhanced the production of type 2 cytokines. a The schema of our co-culture study is shown. b, c, e We performed a (1:1) cell number co-culture using sorted NP ILC2s with NP CRTH2−CD4 + T cells (n = 10, b), NP ILC2s with NP TH2 cells (n = 12, c), and NP ILC2s with NP CXCL16 + cells (n = 4, e) for 4 days. We also cultured equal numbers of NP ILC2s, NP CRTH2− CD4 + T cells, NP TH2, and NP CXCL16 + cells separately (Individual culture) for 4 days. d, f The ratio of IL-5 and IL-13 production in the co-culture of NP ILC2s with TH2 cells or ILC2s with CXCL16 + cells to the sum of individual culture is shown (d, n = 12, f, n = 4). g NP ILC2s were co-cultured with NP TH2 cells in the presence or absence of 10 µg/ml denosumab and isotype human control IgG2 (n = 8) for 4 days. The concentrations of IL-5 and IL-13 were measured by Luminex assay. Cytokine amounts were shown in pg from 10,000 ILC2s plus 10,000 T cells or 10,000 CXCL16 + cells. Not significant (NS), *p < 0.05, **p < 0.01, and ***p < 0.001 were calculated by Wilcoxon test (b, c), ratio paired t test (e), and Friedman test (g)
Discussion
RANK-L, RANK, and RANK-L decoy receptor, OPG, play an essential role in osteogenesis, organization of lymphoid tissue, and DC survival.24,25 The dysregulation of RANK-L is involved in numerous diseases, including osteoporosis, osteopetrosis, rheumatoid arthritis (RA), Paget’s bone disease, and periodontal disease.32 Denosumab, which is a fully human RANK-L monoclonal antibody, has been approved for treatment of diseases caused by overexpression of RANK-L.32 RANK-L was originally discovered as a co-stimulator in initiation of the acquired immune response, and RANK-L on activated T cells induces the survival signal or maturation of DCs via RANK.26,33,34 Herein, we report a novel role for RANK-L with findings suggesting that RANK-L is able to activate ILC2-mediated type 2 immunity.
We clearly showed that RANK-L and agonistic anti-RANK antibody-induced production of type 2 cytokines in human ILC2s (Fig. 2; Supplementary Fig. 2) and that the levels of RANK-L in sinus tissue positively correlated with markers for type 2 inflammation, including IL-13, eosinophil cationic protein (ECP), Charcot–Leyden crystal (CLC), and TSLP (Supplementary Fig. 3b, c). This suggests that RANK-L may be involved in controlling the type 2 inflammation in CRSwNP. However, the degree of cytokine production induced by RANK-L in ILC2s was not profound (Fig. 2a; Supplementary Fig. 2a). It is well known that overexpression of RANK-L is associated with type 3 (TH17) inflammation, but not with type 2 inflammation.35 This suggests that upregulation of RANK-L alone may not be sufficient to induce type 2 inflammation. Importantly, we also found that TSLP potently enhanced RANK/RANK-L-mediated production of type 2 cytokines in human ILC2s (Fig. 2c; Supplementary Fig. 2b). This suggests that RANK-L acts as an inducer and TSLP as an enhancer, that ILC2s are a target cell population to control initiation and amplification of type 2 immunity,10 and that the elevation of all three factors; inducer, enhancer, and target cells, may be necessary to induce RANK-L-mediated type 2 inflammation. In the case of osteoporosis, RA and other type 3 inflammatory diseases, TSLP, or ILC2s are probably neither present nor elevated, and therefore overexpression of RANK-L may not induce type 2 inflammation in these diseases. In contrast, in CRSwNP, our studies indicate that the unique environment within NP tissue is characterized by accumulation of all three factors, RANK-L, TSLP, and ILC2s, therefore enabling RANK-L to trigger type 2 inflammation, and explaining the positive correlation of RANK-L with type 2 inflammation in CRSwNP.9 It is well known that TSLP and ILC2s are highly elevated in many other type 2 inflammatory diseases, in addition to CRSwNP, including allergic asthma and atopic dermatitis.14,21,36 There may be value in future studies testing whether RANK-L is also elevated in other type 2 inflammatory diseases.
In an ancillary study, we found that RANK is also expressed on CRTH2− ILCs (Supplementary Fig. 8a, b). This suggests that overexpression of RANK-L may influence ILC1 and/or ILC3-mediated inflammation in NPs. However, in view of the low frequency of ILC1/3 in CRSwNP compared with ILC2s,9 we think they may play only a minor role in NPs.
We found that the effect of agonistic anti-RANK antibody on the induction of type 2 cytokines in ILC2s was stronger than recombinant RANK-L protein (Fig. 2; Supplementary Fig. 2). Both RANK-L and RANK have a homotrimeric structure, and only trimeric RANK-L fully activates RANK on cells.37,38,39 However, recombinant RANK-L protein (amino acid: 64–245) may not form a complete trimeric structure because it is lacking several β-sheet structures, which are required to form the native trimeric RANK-L.39 In contrast, anti-RANK antibody can stimulate a homotrimeric RANK.39 This trimeric signaling may explain why anti-RANK antibody was more effective than recombinant RANK-L in activating ILC2s.
Although RANK is the only functional receptor for RANK-L, RANK-L decoy receptor, OPG, is secreted as a soluble form and competes with RANK–RANK-L binding.24,25 It has been reported that soluble RANK-L complexed with OPG is a predominant form compared with free soluble RANK-L due to the high-affinity interaction between RANK-L and OPG.40 In this study, we found not only elevation of RANK-L but also downregulation of OPG in NPs (Fig. 1a, e). This dual effect implies that OPG-free active RANK-L may be highly abundant in NPs compared with control nasal mucosa. We and others have previously reported that ILC2s are highly elevated in NPs.9,10 We also found elevation of RANK expression on ILC2s in NPs (Fig. 1b, c). When combined with the finding that RANK-L is expressed on CXCL16 + DCs, and that a CXCL16 receptor, CXCR6, is found on ILC2s, these results suggest that within NP tissue, there is a favorable environment for the interaction of OPG-free RANK-L on DCs and RANK on ILC2s; this interaction may well contribute to the initiation or perpetuation of type 2 inflammation in NPs. We also found that the co-culture of NP ILC2s with CXCL16 + cells enhanced ILC2-mediated production of type 2 cytokines (Fig. 6e, f). The results suggest that CXCL16 + cells may be involved in ILC2-mediated type 2 inflammation in CRSwNP at least in part via a RANK-L-dependent manner. Since characterization of CXCL16 + cells in NPs is not well understood, advanced studies will be required to clarify the role of CXCL16 + cells in NPs.
We also demonstrated that RANK-L was highly expressed on TH2 cells in NPs (Fig. 4d, e). We then investigated how TH2 cells might co-localize with ILC2s and found that the chemokine receptor CCR4 was expressed on both TH2 cells and ILC2s in NPs, and that CCR4 ligands were elevated in NPs (Fig. 5b, c). Of further relevance to this question, others have found that PGD2 can recruit both TH2 cells and ILC2s via a CRTH2-dependent manner and that PGD2 is highly elevated in NPs, especially in patients who have NSAID sensitivity.41,42,43,44 These results suggest that CCR4 ligands and PGD2 may play important roles in both the accumulation and co-localization of ILC2s and TH2 cells to the same area within NPs. In this study, we further analyzed a direct interaction between ILC2s and TH2 cells in NPs. We found that freshly isolated NP-derived TH2 cells but not CRTH2− CD4 + T cells released type 2 cytokines without additional stimulation (Supplementary Fig. 7), and that NP TH2 cells were able to enhance the production of type 2 cytokines in NP ILC2s in a co-culture (Fig. 6c, d). These results suggest that TH2 cells not only actively release type 2 cytokines but also enhance ILC2-mediated type 2 inflammation in NPs in vivo. Recent studies suggest that T cells are able to directly interact with ILC2s through the ligation of OX40/OX40-ligand, inducible T-cell costimulatory (ICOS)/ICOS ligand, and programmed cell death 1 (PD-1)/PD-1 ligand 1.45,46,47,48 The role of these interactions on ILC2-mediated type 2 inflammation in NPs is still unclear. In support of the functional activation of a direct mechanism, we found that denosumab almost completely abolished the enhanced active production of type 2 cytokines in a NP TH2-ILC2 co-culture (Fig. 6g). Unexpectedly, we also found that RANK was expressed on TH2 cells (Supplementary Fig. 8c), and this observation indicates a potential RANK–RANK-L interaction within TH2 cells. However, we also found that agonistic anti-RANK antibody induced significantly less amounts of IL-5 and IL-13 in TH2 cells compared with ILC2s (4.2-fold and 89-fold, respectively; Supplementary Fig. 8d, e). In the terms of interaction, we were not able to detect soluble RANK-L in supernatants of NP TH2 cells (not shown). Taken together, these results suggests that the direct interaction of ILC2 and TH2 cell enhances type 2 cytokine responses and that the enhancement activity is mainly controlled by a RANK-L-dependent activation of ILC2s. Clearly, future studies will be required to validate the mechanisms and quantify the importance of interaction between ILC2s and TH2 cells in controlling the production of type 2 cytokines in NPs.
In conclusion, we provide evidence that RANK-L, a member of the TNF superfamily, plays an inductive role in ILC2-mediated type 2 inflammation in NPs. TSLP clearly enhances the RANK-L-mediated production of type 2 cytokines from ILC2s in CRSwNP. Inhibition of the RANK-L/RANK axis and/or TSLP offers potentially effective strategies for suppression of ILC2-mediated type 2 inflammation in CRSwNP.
Methods
Patients and tissue collection
All control patients and patients with CRSwNP were recruited from the Otolaryngology clinic and the Northwestern Sinus Center of Northwestern Medicine. All CRS patients met the criteria for CRSwNP as defined by the International Consensus Statement on Allergy and Rhinology: Rhinosinusitis.49 Patients with an established immunodeficiency, pregnancy, coagulation disorder, or diagnosis of eosinophilic granulomatosis with polyangiitis or cystic fibrosis were excluded from the study. Control patients were undergoing surgery for non-CRS indicated procedures such as septoplasty. All NP tissues were collected during endoscopic sinus surgery. Detailed characteristics of subjects in this study are shown in Supplementary Tables 1 and 2. All subjects signed informed consent, and the study was approved by the Institutional Review Board of Northwestern University Feinberg School of Medicine (IRB project number: STU00080917). Human peripheral blood leuko paks (STEMCELL Technologies, Vancouver, British Columbia, Canada) were obtained from healthy subjects for isolation of blood ILC2s and T cells.
Quantitative polymerase chain reaction (qPCR)
The total RNAs were isolated from whole-tissue extracts, and cDNA was prepared, as previously described.5,12,20 Real-time RT-qPCR was performed with the TaqMan method using a StepOnePlus Real-Time PCR System (Applied Biosystems, Foster City, CA) in 20 μL reactions (10 μL 2x TaqMan Fast Advanced Master Mix [Applied Biosystems], 1 μL 20x primer and probe mixture for target gene, 1 μL 20x primer and probe mixture for β-glucuronidase (GUSB) plus cDNA equivalent to 10 ng of the total RNA). Primer and probe sets were purchased from Applied Biosystems or Integrated DNA Technologies (Coralville, Iowa), and are shown in Supplementary Table 3. The mRNA expression levels were normalized to the percentage of expression of a housekeeping gene, GUSB.
Tissue homogenates and measurement of protein
Freshly obtained tissue specimens were prepared as previously described.5 The concentration of ECP, RANK-L, IL-5, and IL-13 in cell-free supernatants was measured by ELISA kit (MBL, Woburn, Mass), and Luminex multiplex assay (MILLIPLEX MAP Human RANK-L Magnetic Bead and MILLIPLEX MAP Human Cytokine/Chemokine Panel from EMD Millipore, Burlington, MA). The minimal detection limits for ECP, RANK-L, IL-5, and IL-13 are 0.125 ng/ml, 5.0 pg/ml, 3.2 pg/ml, and 3.2 pg/ml, respectively. The concentration of RANK-L, IL-13, and ECP in tissue homogenates was normalized to the concentration of the total protein as detected by BCA protein assay kit (Thermo Fisher Scientific Inc., Waltham, MA).
Cell isolation and cell sorting from human blood and NP tissue
Human leukocytes were isolated from a human peripheral blood leuko pak (STEMCELL Technologies) by centrifugation at 500 g for 10 min with equal volume of dPBS with 2% fetal bovine serum (FBS) at room temperature. After aspiration of the supernatants, red blood cells were lysed by ammonium chloride solution (STEMCELL Technologies), and supernatants were removed after centrifugation at 300 g for 5 min. To remove platelets, cells were resuspended in dPBS + 2% FBS, and centrifuged at 200 g for 10 min at room temperature. After removing the supernatants, ILC2s were enriched by EasySep™ Human ILC2 Enrichment Cocktail kit (STEMCELL Technologies) according to the manufacturer’s instructions. After enrichment, cells were blocked by Fc Block reagent and then incubated with FITC anti-Lineage Cocktail (CD3, CD14, CD16, CD19, CD20, CD56), FITC anti-FcεRIa, FITC anti-CD11c, FITC anti-CD303, BUV395 anti-CD4, PE anti-CD5, Brilliant Violet 421 anti-CD45, Alexa Fluor 647 anti-CRTH2, PE/Cy7 anti-CD127, and APC/Cy7 anti-CD161. We then sorted blood ILC2s as CD45 + , Lin (CD3, CD11c, CD14, CD16, CD19, CD20, CD56, CD303, FcεRIa)−, CD4−, CD5−, CD127 + , CRTH2 + , CD161 + cells with a BD FACSAria SORP cell sorter (BD Biosciences) at the Robert H Lurie Comprehensive Cancer Center at Northwestern University. All antibodies are listed in Supplementary Table 4.
We also sorted ILC2s, TH2 cells, CRTH2− CD4 + T cells, and CXCL16 + cells from NPs from patients with CRSwNP. Tissue samples were fragmented and incubated with 30 µg/ml DNase I and 1 mg/ml type I collagenase containing media at 4 °C overnight. Following this, tissues were minced using a gentleMACS dissociator (Miltenyi Biotec, Auburn, CA), and the cells were filtered through 70 -µm nylon mesh (BD Biosciences, San Jose, CA). Cells were then treated with red blood cell lysis solution (Miltenyi Biotec) before counting and staining for cell sorting. After the isolation, cells were first treated with Aqua LIVE/DEAD fixable dead cell staining reagent (Invitrogen, Carlsbad, CA) at room temperature in the dark. Cells were then blocked by Fc Block reagent and incubated with FITC anti-human Lineage Cocktail, FITC or PerCP/Cy5.5 anti-CD11c, FITC anti-CD303, PE anti-CXCL16, PE/Cy7 anti-FcεRIa or anti-HLA-DR, BUV395 anti-CD4, PE/Dazzle 594 anti-CD5, Alexa Fluor 700 anti-CD45, Alexa Fluor 647 anti-CRTH2, BV421 anti-CD127, and APC/Cy7 anti-CD161 at 4 °C in the dark. We sorted ILC2s (Aqua−, CD45 + , Lin (CD3, CD11c, CD14, CD16, CD19, CD20, CD56, CD303)−, CD4−, CD5−, FcεRIa−, CD127 + , CRTH2 + , and CD161 + cells) CRTH2− CD4 + T cells (Aqua−, CD45 + , Lin + , FcεRIa−, CD5 + , CD4 + , CRTH2−), TH2 cells (Aqua−, CD45 + , Lin + , FcεRIa−, CD5 + , CD4 + , CRTH2 + ), and CXCL16 + cells (Aqua−, CD45 + , CD11c + , HLA-DR +, and CXCL16 + cells) with a BD FACSAria SORP cell sorter. The purity of blood and NP ILC2s was >98% (not shown).
Cell culture
Sorted blood and NP ILC2s, TH2 cells, CRTH2− CD4 + cells, and CXCL16 + cells (10,000 cells/ml) were suspended in the RPMI 1640 medium supplemented with 25 IU/ml IL-2 (Prometheus, San Diego, CA), 10% FBS, 100 U/ml penicillin, and 100 μg/ml streptomycin, as previously described.22 ILC2s were stimulated with 10 ng/ml TSLP (R&D Systems, Minneapolis, MN), 50 ng/ml RANK-L (R&D Systems), 10 μg/ml goat control IgG (R&D Systems), and 10 μg/ml agonistic anti-RANK antibody (R&D Systems) in the presence or absence of 10 ng/ml IL-10 (R&D Systems), 20 ng/ml TGF-β1 (R&D Systems), 0.01% or 0.001% DMSO (Sigma-Aldrich, St. Louis, MO), 100 nM dexamethasone (Sigma-Aldrich), and 10 nM IκB inhibitor IMD0354 (Selleckchem, Houston, TX) for 4 days. We did dose-dependent experiments using 10–50 ng/ml RANK-L and 1–10 µg/ml anti-RANK antibody (n = 2, not shown) and then selected optimal concentrations for this study.
In the co-culture study, we performed a (1:1) co-culture using sorted ILC2s with CRTH2− CD4 + T cells, TH2 cells, or CXCL16 + cells for 4 days. In some experiments, we performed co-culture of ILC2s with TH2 cells in the presence or absence of 10 µg/ml denosumab (Amgen inc., Thousand Oak, CA) and 10 µg/ml isotype control human IgG2 (BioLegend, San Diego, CA). In individual condition wells, we plated equal volumes of ILC2s (10,000 cells/ml), T cells (10,000 cells/ml), or CXCL16 + cells (10,000 cells/ml), and cytokine amounts were shown as pg from 10,000 ILC2s + 10,000 T cells or 10,000 DCs.
Flow-cytometric analysis
Cells were first treated with Aqua dead cell staining reagent as a live/dead discriminator. Cells were then incubated with an Fc Block reagent (Miltenyi Biotec) for 10 min at 4 °C in the dark. All antibodies are listed in Supplementary Table 4. Cells were stained for 30 min at 4 °C in the dark, and washed with MACS buffer (Miltenyi Biotech). After washing, cells were fixed with a BD Cytofix/Cytoperm Kit (BD Biosciences), resuspended in MACS buffer, and stored at 4 °C in the dark before analysis on a CytoFLEX flow cytometer (Beckman Coulter, Indianapolis, IN). All analysis was performed with FlowJo software, version 10.1 (TreeStar, Ashland, OR), and the experimental method was established and verified with the proper single-stained control beads (BD Biosciences and eBiosciences) and fluorescence minus one (FMO) negative controls (not shown).
Immunohistochemistry
Immunohistochemistry was performed as described previously.20,50 For antigen retrieval, sections were placed in boiling 10 mM citrate buffer for 15 min, and cooled slowly and rinsed. Sections were blocked for endogenous peroxidase activity with 3% hydrogen peroxide/methanol. After rinsing, tissue sections were blocked for nonspecific binding with 5% goat serum/0.3% Tween-20/PBS. After avidin/biotin blocking (Vector Laboratories, Burlingame, Calif), tissue sections were incubated with 0.25 μg/ml rabbit anti-human RANK-L polyclonal antibody (HPA045142, Sigma-Aldrich) or 0.25 μg/ml rabbit control IgG antibody (Thermo Fisher Scientific Inc.) overnight at 4 °C. Sections were incubated in the biotinylated secondary goat anti-rabbit IgG antibody (Vector Laboratories) at a 1:200 dilution for 1 h at room temperature. After another rinse, sections were incubated in ABC reagent (avidin–biotin–horseradish peroxidase complex; Vector Laboratories) for 1 h at room temperature. Sections were incubated with ImmPACT™ NovaRED™ reagent (Vector Laboratories) for 5 min at room temperature. Then they were rinsed in deionized H2O, counterstained with hematoxylin, dehydrated, cleaned, mounted, and coverslipped using Cytoseal 60 (Richard-Allan Scientific, Kalamazoo, MI) in preparation for microscopic analysis. Slides were blinded, and five pictures were randomly taken from each slide using Olympus IX71 and cellSens Entry software (Olympus, Tokyo, Japan). The number of RANK-L-positive cells in the nasal tissue was counted by two independent observers.
Statistics
All data were reported as the mean ± SEM. Normality tests were performed with Shapiro–Wilk normality test (two groups) and Brown–Forsythe test (multiple groups). Comparisons of two groups were performed using Mann–Whitney test or Wilcoxon test if the data were nonparametric or using paired t test or ratio paired t test if the data were parametric. Multiple groups were compared using one-way ANOVA Kruskal–Wallis test or Friedman test followed by a Dunns’s post test if the data were nonparametric or using one-way ANOVA following by a Holm–Sidak’s post test if the data were parametric. A p-value of <0.05 was considered significant. Correlations were assessed by Spearman correlation.
References
Fokkens, W. J. et al. European position paper on rhinosinusitis and nasal polyps 2012. Rhinol. Suppl. 23, 1–298 (2012).
Stevens, W. W., Schleimer, R. P. & Kern, R. C. Chronic rhinosinusitis with nasal polyps. J. Allergy Clin. Immunol. Pr. 4, 565–572 (2016).
Kato, A. Immunopathology of chronic rhinosinusitis. Allergol. Int 64, 121–130 (2015).
Schleimer, R. P. Immunopathogenesis of chronic rhinosinusitis and nasal polyposis. Annu Rev. Pathol. 12, 331–357 (2017).
Tan, B. K. et al. Heterogeneous inflammatory patterns in chronic rhinosinusitis without nasal polyps in Chicago, Illinois. J. Allergy Clin. Immunol. 139, 699–703 (2017).
Lam, E. P. et al. IL-25/IL-33-responsive TH2 cells characterize nasal polyps with a default TH17 signature in nasal mucosa. J. Allergy Clin. Immunol. 137, 1514–1524 (2016).
Takabayashi, T. et al. Glandular mast cells with distinct phenotype are highly elevated in chronic rhinosinusitis with nasal polyps. J. Allergy Clin. Immunol. 130, 410–420 (2012).
Mjosberg, J. M. et al. Human IL-25- and IL-33-responsive type 2 innate lymphoid cells are defined by expression of CRTH2 and CD161. Nat. Immunol. 12, 1055–1062 (2011).
Poposki, J. A. et al. Group 2 innate lymphoid cells are elevated and activated in chronic rhinosinusitis with nasal polyps. Immun. Inflamm. Dis. 5, 233–243 (2017).
Kato, A. Group 2 innate lymphoid cells in airway diseases. Chest 156, 141–149 (2019).
Mjosberg, J. & Spits, H. Human innate lymphoid cells. J. Allergy Clin. Immunol. 138, 1265–1276 (2016).
Ogasawara, N. et al. Epithelial activators of type 2 inflammation: elevation of thymic stromal lymphopoietin, but not IL-25 or IL-33, in chronic rhinosinusitis with nasal polyps in Chicago, Illinois. Allergy 73, 2251–2254 (2018).
Nagarkar, D. R. et al. Thymic stromal lymphopoietin activity is increased in nasal polyps of patients with chronic rhinosinusitis. J. Allergy Clin. Immunol. 132, 593–600 (2013).
Bartemes, K. R., Kephart, G. M., Fox, S. J. & Kita, H. Enhanced innate type 2 immune response in peripheral blood from patients with asthma. J. Allergy Clin. Immunol. 134, 671–678 (2014).
Yu, X. et al. TNF superfamily member TL1A elicits type 2 innate lymphoid cells at mucosal barriers. Mucosal Immunol. 7, 730–740 (2014).
Meylan, F. et al. The TNF-family cytokine TL1A promotes allergic immunopathology through group 2 innate lymphoid cells. Mucosal Immunol. 7, 958–968 (2014).
Nagashima, H. et al. GITR cosignal in ILC2s controls allergic lung inflammation. J. Allergy Clin. Immunol. 141, 1939–1943 e1938 (2018).
Ogasawara, N. P. J. et al. TNF induces the production of type 2 cytokines in human group 2 innate lymphoid cells. J. Allergy Clin. Immunol. pii: S0091-6749(19)31184-4 (2019). https://doi.org/10.1016/j.jaci.2019.09.001. [Epub ahead of print].
Seshadri, S. et al. Reduced expression of antimicrobial PLUNC proteins in nasal polyp tissues of patients with chronic rhinosinusitis. Allergy 67, 920–928 (2012).
Kato, A. et al. Evidence of a role for B cell-activating factor of the TNF family in the pathogenesis of chronic rhinosinusitis with nasal polyps. J. Allergy Clin. Immunol. 121, 1385–1392 (2008).
Salimi, M. et al. A role for IL-25 and IL-33-driven type-2 innate lymphoid cells in atopic dermatitis. J. Exp. Med. 210, 2939–2950 (2013).
Ogasawara, N. et al. IL-10, TGF-beta, and glucocorticoid prevent the production of type 2 cytokines in human group 2 innate lymphoid cells. J. Allergy Clin. Immunol. 141, 1147–1151 (2018).
Paranjape, A. et al. Dexamethasone rapidly suppresses IL-33-stimulated mast cell function by blocking transcription factor activity. J. Leukoc. Biol. 100, 1395–1404 (2016).
Walsh, M. C. & Choi, Y. Biology of the RANKL-RANK-OPG system in immunity, bone, and beyond. Front. Immunol. 5, 511 (2014).
Hanada, R., Hanada, T., Sigl, V., Schramek, D. & Penninger, J. M. RANKL/RANK-beyond bones. J. Mol. Med. 89, 647–656 (2011).
Wong, B. R. et al. TRANCE (tumor necrosis factor [TNF]-related activation-induced cytokine), a new TNF family member predominantly expressed in T cells, is a dendritic cell-specific survival factor. J. Exp. Med. 186, 2075–2080 (1997).
Yeo, L. et al. Cytokine mRNA profiling identifies B cells as a major source of RANKL in rheumatoid arthritis. Ann. Rheum. Dis. 70, 2022–2028 (2011).
Meednu, N. et al. Production of RANKL by memory B cells: a link between B cells and bone erosion in rheumatoid arthritis. Arthritis Rheumatol. 68, 805–816 (2016).
Huber, C., Odermatt, A., Hagmann, B., Dahinden, C. A. & Fux, M. In human basophils, IL-3 selectively induces RANKL expression that is modulated by IgER-dependent and IgER-independent stimuli. Allergy 69, 1498–1505 (2014).
Bando, J. K. et al. The tumor necrosis factor superfamily member RANKL suppresses effector cytokine production in group 3 innate lymphoid cells. Immunity 48, 1208–1219 (2018).
Satoh-Takayama, N. et al. The chemokine receptor CXCR6 controls the functional topography of interleukin-22 producing intestinal innate lymphoid cells. Immunity 41, 776–788 (2014).
Lacey, D. L. et al. Bench to bedside: elucidation of the OPG-RANK-RANKL pathway and the development of denosumab. Nat. Rev. Drug Disco. 11, 401–419 (2012).
Wong, B. R. et al. TRANCE is a novel ligand of the tumor necrosis factor receptor family that activates c-Jun N-terminal kinase in T cells. J. Biol. Chem. 272, 25190–25194 (1997).
Bachmann, M. F. et al. TRANCE, a tumor necrosis factor family member critical for CD40 ligand-independent T helper cell activation. J. Exp. Med. 189, 1025–1031 (1999).
Roberts, C. A., Dickinson, A. K. & Taams, L. S. The interplay between monocytes/macrophages and CD4( + ) T cell subsets in rheumatoid arthritis. Front. Immunol. 6, 571 (2015).
Kim, B. S. et al. TSLP elicits IL-33-independent innate lymphoid cell responses to promote skin inflammation. Sci. Transl. Med. 5, 170ra116 (2013).
Lam, J., Nelson, C. A., Ross, F. P., Teitelbaum, S. L. & Fremont, D. H. Crystal structure of the TRANCE/RANKL cytokine reveals determinants of receptor-ligand specificity. J. Clin. Invest. 108, 971–979 (2001).
Crockett, J. C., Mellis, D. J., Scott, D. I. & Helfrich, M. H. New knowledge on critical osteoclast formation and activation pathways from study of rare genetic diseases of osteoclasts: focus on the RANK/RANKL axis. Osteoporos. Int. 22, 1–20 (2011).
Das, S., Sepahi, I., Duthie, A., Clark, S. & Crockett, J. C. RANK receptor oligomerisation in the regulation of NFkappaB signalling. J. Mol. Endocrinol. 53, 81–91 (2014).
Nelson, C. A., Warren, J. T., Wang, M. W., Teitelbaum, S. L. & Fremont, D. H. RANKL employs distinct binding modes to engage RANK and the osteoprotegerin decoy receptor. Structure 20, 1971–1982 (2012).
Eastman, J. J. et al. Group 2 innate lymphoid cells are recruited to the nasal mucosa in patients with aspirin-exacerbated respiratory disease. J. Allergy Clin. Immunol. 140, 101–108 (2017).
Xue, L. et al. Prostaglandin D2 activates group 2 innate lymphoid cells through chemoattractant receptor-homologous molecule expressed on TH2 cells. J. Allergy Clin. Immunol. 133, 1184–1194 (2014).
Hirai, H. et al. Prostaglandin D2 selectively induces chemotaxis in T helper type 2 cells, eosinophils, and basophils via seven-transmembrane receptor CRTH2. J. Exp. Med. 193, 255–261 (2001).
Cahill, K. N., Bensko, J. C., Boyce, J. A. & Laidlaw, T. M. Prostaglandin D(2): a dominant mediator of aspirin-exacerbated respiratory disease. J. Allergy Clin. Immunol. 135, 245–252 (2015).
Maazi, H. et al. ICOS:ICOS-ligand interaction is required for type 2 innate lymphoid cell function, homeostasis, and induction of airway hyperreactivity. Immunity 42, 538–551 (2015).
Schwartz, C. et al. ILC2s regulate adaptive Th2 cell functions via PD-L1 checkpoint control. J. Exp. Med. 214, 2507–2521 (2017).
Halim, T. Y. et al. Group 2 innate lymphoid cells license dendritic cells to potentiate memory TH2 cell responses. Nat. Immunol. 17, 57–64 (2016).
Halim, T. Y. F. et al. Tissue-restricted adaptive type 2 immunity is orchestrated by expression of the costimulatory molecule OX40L on group 2 innate lymphoid cells. Immunity 48, 1195–1207 (2018).
Orlandi, R. R. et al. International consensus statement on allergy and rhinology: rhinosinusitis. Int. Forum Allergy Rhinol. 6, S22–S209 (2016).
Poposki, J. A. et al. Increased expression of the chemokine CCL23 in eosinophilic chronic rhinosinusitis with nasal polyps. J. Allergy Clin. Immunol. 128, 73–81 (2011).
Acknowledgements
This research was supported in part by NIH grants, R01 AI104733, R01 AI137174, R37 HL068546, U19 AI106683, and P01 AI145818, and by grants from the Janssen Research Fund and the Ernest S. Bazley Foundation. We would like to gratefully acknowledge Ms. Lydia Suh, Mr. James Norton, Mr. Roderick Carter, Ms. Caroline P.E. Price, Ms. Julia H. Huang, and Ms. Kathleen E. Harris (Northwestern University Feinberg School of Medicine) for their skillful technical assistance. We would like to gratefully acknowledge Dr. Suchitra Swaminathan and the Flow Cytometry Core Facility, supported by NCI CCSG P30 CA060553 awarded to the Robert H Lurie Comprehensive Cancer Center at Northwestern University for their technical assistance during cell sorting. Flow Cytometry Cell Sorting was performed on a BD FACSAria SORP system, purchased through the support of NIH 1S10OD011996-01.
Author information
Authors and Affiliations
Contributions
A.K. designed the study. N.O., J.A.P., A.I.K., and A.K. performed the experiments. N.O. and A.K. analyzed the data. B.K.T., K.E.H., W.W.S., A.T.P., L.C.G., K.C.W., S.S.S., D.B.C., J.R.R., P.S., K.T., T.H., R.C.K., and R.P.S. helped in sample collection and evaluation of study. A.K. and N.O. wrote the paper. All authors have read and approved the final form of the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Ogasawara, N., Poposki, J.A., Klingler, A.I. et al. Role of RANK-L as a potential inducer of ILC2-mediated type 2 inflammation in chronic rhinosinusitis with nasal polyps. Mucosal Immunol 13, 86–95 (2020). https://doi.org/10.1038/s41385-019-0215-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41385-019-0215-8
This article is cited by
-
Differential Angiogenic Induction Impacts Nasal Polyp Tissue Growth
Indian Journal of Otolaryngology and Head & Neck Surgery (2023)
-
A Critical Look at the Efficacy and Costs of Biologic Therapy for Chronic Rhinosinusitis with Nasal Polyposis
Current Allergy and Asthma Reports (2020)