Abstract
Objectives
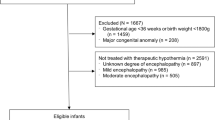
To determine the prevalence of hypothermia on admission and at 24 h of life in very low birth weight infants (VLBWI) and associated morbidity and mortality.
Study design
Hospital records of VLBWI admitted to a neonatal unit were reviewed for information on patient's body temperature, clinical characteristics and mortality. Comparisons between normothermic and hypothermic VLBWI were performed.
Results
Mean gestational age and birth weight of enrolled infants were 29 ± 3 weeks and 1140 ± 253 g, respectively. Prevalence of admission hypothermia was 46.1%, with 38% developing hypothermia within 24-h following admission. VLBWI with hypothermia were more likely to have been born vaginally [aOR 2.85 (1.37–5.91)], have a birth weight < 1000 g [aOR 2.28 (1.25–4.16)], required resuscitation at birth [aOR 2.20 (1.23–3.94)], develop metabolic acidosis [aOR 3.04 (1.35–6.84)] and die within the first week of life [aOR 4.79 (1.43–16.02)].
Conclusions
Prevalence of hypothermia in VLBWI is high and is associated with poor outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others

References
World Health Organization. Thermal protection of the newborn: a practical guide. Geneva: Maternal and Newborn Health/Safe Motherhood Unit, Division of Reproductive Health; 1997.
Bissinger R, Annibale D. Thermoregulation in very low-birth-weight infants during the golden hour results and implications. Adv Neonatal Care. 2010;10:230–8.
Aylott M. The neonatal energy triangle part 2: thermoregulatory and respiratory adaptation. Journal of Paediatric nursing. 2016;18:38–43.
Laptook AR, Salhab W, Bhaskar B. Admission temperature of low birth weight infants: predictors and associated morbidities. Pediatrics. 2007;119:e643–9.
Gandy GM, Adamsons K, Cunningham N, Silverman WA, James LS. Thermal environment and acid-base homeostasis in human infants during the first few hours of life. J Clin Investig. 1964;43:751–8.
Adamsons K, Gandy GM, James LS. The influence of thermal factors upon oxygen consumption of the newborn human infant. J Paediatr. 1965;66:495–508.
Linder N, Haskin O, Levit O, Klinger G, Prince T, Naor N, et al. Risk factors for intraventricular hemorrhage in very low birth weight premature infants: a retrospective case-control study. Pediatrics. 2003;111:e590–5.
Miller SS, Lee HC, Gould JB. Hypothermia in very low birth weight infants: distribution, risk factors and outcomes. J Perinatol. 2011;31 Suppl 1:S49–56.
Wilson E, Norman M, Wilson E, Norman M, Wilson E, Maier RF, et al. Admission hypothermia in very preterm infants and neonatal mortality and morbidity. J Pediatr. 2016;175:61–67.e4.
Chang H-Y, Sung Y-H, Wang S-M, Lung H-L, Chang J-H, Hsu C-H, et al. Short- and long-term outcomes in very low birth weight infants with admission hypothermia. PLoS ONE. 2015;10:e0131976.
Boo NY, Guat-Sim Cheah I. Admission hypothermia among VLBW infants in Malaysian NICUs. J Trop Pediatr. 2013;59:447–52.
Ogunlesi TA, Ogunfowora OB, Adekanmbi FA, Fetuga BM, Olanrewaju DM. Point-of-admission hypothermia among high-risk Nigerian newborns. BMC Pediatr. 2008;8:40.
Sodemann M, Nielsen J, Veirum J, Jakobsen MS, Biai S, Aaby P. Hypothermia of newborns is associated with excess mortality in the first 2 months of life in Guinea-Bissau, West Africa. Trop Med Int Heal. 2008;13:980–6.
Manji KP, Kisenge R. Neonatal hypothermia on admission to a special care unit in Dar-es-Salaam, Tanzania: a cause for concern. Cent Afr J Med. 2003;49:23–7.
Ogunlesi TA, Ogunfowora OB, Adekanmbi FA, Fetuga BM, Olanrewaju DM. Point-of-admission hypothermia among high- risk Nigerian newborns. BMC Pediatr. 2008;8:1–5.
Ludington-Hoe SM, Nguyen N, Swinth JY, Satyshur RD. Kangaroo care compared to incubators in maintaining body warmth in preterm infants. Biol Res Nurs. 2000;2:60–73.
Caldas JP, de S, Millen F, de C, Camargo JF, de, Castro PAC, et al. Effectiveness of a measure program to prevent admission hypothermia in very low-birth weight preterm infants. J Pediatr. 2017;94:368–73.
Acknowledgements
We acknowledge the work done by the clinical staff at the Chris Hani Baragwanath Academic Hospital neonatal unit, and the records department for assistance in retrieval of the medical records.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical statement
Ethical approval for the study was received from the University of Witwatersrand Human Research Ethics Committee prior to undertaking the study (Protocol reference number M170540).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ng’eny, J.C., Velaphi, S. Hypothermia among neonates admitted to the neonatal unit at a tertiary hospital in South Africa. J Perinatol 40, 433–438 (2020). https://doi.org/10.1038/s41372-019-0539-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0539-y
This article is cited by
-
Outcomes of neonatal hypothermia among very low birth weight infants: a Meta-analysis
Maternal Health, Neonatology and Perinatology (2021)