Abstract
Objective
We aimed to investigate the clinical course and outcome of newborns with ductal-dependent congenital heart disease (CHD) who suffered from perinatal asphyxia.
Study design
Clinical data of 504 patients with ductal-dependent CHD and perinatal asphyxia were retrospectively analyzed over a 10-year period (2005–2014).
Result
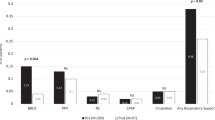
Perinatal asphyxia was diagnosed in 17 (3.4%) patients, comprising two nonoverlapping groups: Five infants with intrauterine acidosis (umbilical artery pH < 7.0), and 12 infants with persistent or deteriorating postnatal depression (Apgar score <6 at 10 min of life). Preoperative (41.7%, p < 0.001) and overall mortality (50.0%, p = 0.001) were increased in infants with asphyxia caused by persistent or deteriorating postnatal depression. Apgar scores at 10 min were independently associated with preoperative (OR 0.479, 95% CI 0.342–0.672, p < 0.001) and overall death (OR 0.655, 95% CI 0.537–0.799, p < 0.001).
Conclusions
Asphyxia caused by postnatally deteriorating depression rather than fetal acidosis is associated with high mortality.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Tagin MA, Woolcott CG, Vincer MJ, Whyte RK, Stinson DA. Hypothermia for neonatal hypoxic ischemic encephalopathy: an updated systematic review and meta-analysis. Arch Pediatr Adolesc Med. 2012;166:558–66.
Jacobs SE, Berg M, Hunt R, Tarnow-Mordi WO, Inder TE, Davis PG. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst Rev. 2013;1:CD003311.
Azzopardi DV, Strohm B, Edwards AD, Dyet L, Halliday HL, Juszczak E, et al. Moderate hypothermia to treat perinatal asphyxial encephalopathy. N Engl J Med. 2009;361:1349–58.
Hoffman JI, Kaplan S. The incidence of congenital heart disease. J Am Coll Cardiol. 2002;39:1890–900.
Akkinapally S, Hundalani SG, Kulkarni M, Fernandes CJ, Cabrera AG, Shivanna B, et al. Prostaglandin E1 for maintaining ductal patency in neonates with ductal-dependent cardiac lesions. Cochrane Database Syst Rev. 2018;2:CD011417.
Boos V, Tietze A, Berger F, Bührer C. Therapeutic hypothermia after perinatal asphyxia in infants with severe, ductal-dependent congenital heart disease. Pediatr Crit Care Med. 2019;20:457–65.
Donofrio MT, Skurow-Todd K, Berger JT, McCarter R, Fulgium A, Krishnan A, et al. Risk-stratified postnatal care of newborns with congenital heart disease determined by fetal echocardiography. J Am Soc Echocardiogr. 2015;28:1339–49.
Oosterhof T, Azakie A, Freedom RM, Williams WG, McCrindle BW. Associated factors and trends in outcomes of interrupted aortic arch. Ann Thorac Surg. 2004;78:1696–702.
Vlahos AP, Lock JE, McElhinney DB, van der Velde ME. Hypoplastic left heart syndrome with intact or highly restrictive atrial septum: outcome after neonatal transcatheter atrial septostomy. Circulation. 2004;109:2326–30.
Wolter A, Nosbüsch S, Kawecki A, Degenhardt J, Enzensberger C, Graupner O, et al. Prenatal diagnosis of functionally univentricular heart, associations and perinatal outcomes. Prenat Diagn. 2016;36:545–54.
Maeno YV, Kamenir SA, Sinclair B, van der Velde ME, Smallhorn JF, Hornberger LK. Prenatal features of ductus arteriosus constriction and restrictive foramen ovale in d-transposition of the great arteries. Circulation. 1999;99:1209–14.
Swenson AW, Dechert RE, Schumacher RE, Attar MA. The effect of late preterm birth on mortality of infants with major congenital heart defects. J Perinatol. 2012;32:51–4.
Knickmeyer RC, Gouttard S, Kang C, Evans D, Wilber K, Smith JK, et al. A structural MRI study of human brain development from birth to 2 years. J Neurosci. 2008;28:12176–82.
Levene MI, Sands C, Grindulis H, Moore JR. Comparison of two methods of predicting outcome in perinatal asphyxia. Lancet. 1986;1:67–9.
Low JA, Lindsay BG, Derrick EJ. Threshold of metabolic acidosis associated with newborn complications. Am J Obstet Gynecol. 1997;177:1391–4.
Donofrio MT, Levy RJ, Schuette JJ, Skurow-Todd K, Sten MB, Stallings C, et al. Specialized delivery room planning for fetuses with critical congenital heart disease. Am J Cardiol. 2013;111:737–47.
Chalak LF, Rollins N, Morriss MC, Brion LP, Heyne R, Sánchez PJ. Perinatal acidosis and hypoxic-ischemic encephalopathy in preterm infants of 33–35 weeks’ gestation. J Pediatr. 2012;160:388–94.
Hüseman D, Metze B, Walch E, Bührer C. Laboratory markers of perinatal acidosis are poor predictors of neurodevelopmental impairment in very low birth weight infants. Early Hum Dev. 2011;87:677–81.
Lynema S, Fifer CG, Laventhal NT. Perinatal decision making for preterm infants with congenital heart disease: determinable risk factors for mortality. Pediatr Cardiol. 2016;37:938–45.
Moonen RM, Agren P, Cogolludo AL, Perez Vizcaino F, Villamor E. Response of chicken ductus arteriosus to hypercarbic and normocarbic acidosis. Neonatology. 2010;98:47–56.
Park MK. Fetal and perinatal circulation. In: Park MK, editor. Pediatric cardiology for practitioners. Maryland Heights: Elsevier Mosby; 2007. p. 119–24.
Xanthou M, Fotopoulos S, Mouchtouri A, Lipsou N, Zika I, Sarafidou J. Inflammatory mediators in perinatal asphyxia and infection. Acta Paediatr Suppl. 2002;91:92–7.
Hong HS, Lee JY. Intracranial hemorrhage in term neonates. Childs Nerv Syst. 2018;34:1135–43.
Beca J, Gunn J, Coleman L, Hope A, Whelan LC, Gentles T, et al. Pre-operative brain injury in newborn infants with transposition of the great arteries occurs at rates similar to other complex congenital heart disease and is not related to balloon atrial septostomy. J Am Coll Cardiol. 2009;53:1807–11.
Pappas A, Shankaran S, Hansen NI, Bell EF, Stoll BJ, Laptook AR, et al. Outcome of extremely preterm infants (<1,000 g) with congenital heart defects from the National Institute of Child Health and Human Development Neonatal Research Network. Pediatr Cardiol. 2012;33:1415–26.
Hennein HA, Mendeloff EN, Cilley RE, Bove EL, Coran AG. Predictors of postoperative outcome after general surgical procedures in patients with congenital heart disease. J Pediatr Surg. 1994;29:866–70.
Lee HC, Subeh M, Gould JB. Low Apgar score and mortality in extremely preterm neonates born in the United States. Acta Paediatr. 2010;99:1785–9.
Mulkey SB, Fontenot EE, Imamura M, Yap VL. Therapeutic hypothermia in a neonate with perinatal asphyxia and transposition of the great arteries. Ther Hypothermia Temp Manag. 2011;1:205–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Boos, V., Kocjancic, L., Berger, F. et al. Delivery room asphyxia in neonates with ductal-dependent congenital heart disease: a retrospective cohort study. J Perinatol 39, 1627–1634 (2019). https://doi.org/10.1038/s41372-019-0474-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0474-y