Abstract
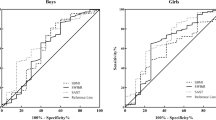
To characterize the prevalence of hypertension and prehypertension and its association with four anthropometrics among children aged 7–15 years in Tianjin, China, a school-based cross-sectional survey was conducted from May to August 2010. Multistage random cluster sampling was used to select the participants. Body mass index (BMI), waist circumference (WC), waist-to-height ratio (WHtR), and waist-to-hip ratio (WHR) were measured. Hypertension and prehypertension were identified according to the definition of United State Fourth Report. Logistic regression, linear regression and the area under receiver operating curves (AUC) was used for assessing the association. Among 1898 eligible children, the prevalence of hypertension and prehypertension was 6% and 6.6%, respectively. No statistically significant differences were found between boys and girls. Both linear and logistic regression showed that the four anthropometrics were all positively related to blood pressure value or the risk of prehypertension and hypertension. Of the four anthropometrics, BMI might be the most sensitive indicator for predicting elevated blood pressure, followed by WC and WHtR, whereas WHR had the lowest predicting capacity, with the AUCs being 0.72 (0.68,0.75), 0.69 (0.65,0.73), 0.67 (0.63,0.71), and 0.61 (0.57,0.65), respectively. A significantly increased prevalence of hypertension was observed when BMI > P90 percentiles, but for prehypertension, the risk of prehypertension began to increase when BMI was still at a median level. In conclusion, four anthropometrics all had positive relationship with elevated blood pressure. BMI and WC were superior to WHtR and WHR in predicting elevated blood pressure among children and adolescents.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Whitworth JA. 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J Hypertens. 2003;21:1983–92.
Chen L, Simonsen N, Liu L. Racial differences of pediatric hypertension in relation to birth weight and body size in the United States. PLoS One. 2015;10:e0132606.
Kelly RK, Thomson R, Smith KJ, Dwyer T, Venn A, Magnussen CG. Factors affecting tracking of blood pressure from childhood to adulthood: The Childhood Determinants of Adult Health Study. J Pediatr. 2015;167:1422–8.e2.
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J. Global burden of hypertension: analysis of worldwide data. Lancet. 2005;365:217–23.
Xi B, Liang Y, Reilly KH, Wang Q, Hu Y, Tang W. Trends in prevalence, awareness, treatment, and control of hypertension among Chinese adults 1991-2009. Int J Cardiol. 2012;158:326–9.
Wang J, Zhang L, Wang F, Liu L, Wang H. Prevalence, awareness, treatment, and control of hypertension in China: results from a national survey. Am J Hypertens. 2014;27:1355–61.
Liang YJ, Xi B, Hu YH, Wang C, Liu JT, Yan YK, et al. Trends in blood pressure and hypertension among Chinese children and adolescents: China Health and Nutrition Surveys 1991-2004. Blood Press. 2011;20:45–53.
Xi B, Liang Y, Mi J. Hypertension trends in Chinese children in the national surveys, 1993 to 2009. Int J Cardiol. 2013;165:577–9.
Xi B, Li H, Li S, Mi J. Recent prevalence of hypertension among Chinese children and adolescents based on 2010 China national blood pressure references. Int J Cardiol. 2014;174:870–1.
Dong B, Wang Z, Ma J. Urban-rural disparity in blood pressure among Chinese children: 1985-2010. Eur J Public Health. 2016;26:569–75.
Friedman GD, Selby JV, Quesenberry CP Jr, Armstrong MA, Klatsky AL. Precursors of essential hypertension: body weight, alcohol and salt use, and parental history of hypertension. Prev Med. 1988;17:387–402.
Juhola J, Oikonen M, Magnussen CG, Mikkila V, Siitonen N, Jokinen E, et al. Childhood physical, environmental, and genetic predictors of adult hypertension: the cardiovascular risk in young Finns study. Circulation. 2012;126:402–9.
Group SR, Wright JT Jr, Williamson JD, Whelton PK, Snyder JK, Sink KM, et al. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med. 2015;373:2103–16.
Hu J, Chu GP, Huang FF, Zhou YK, Teng CG, Yang HB, et al. Relation of body mass index (BMI) to the prevalence of hypertension in children: a 3years’ school-based prospective study in Suzhou, China. Int J Cardiol. 2016;222:270–4.
Zhu H, Zhang X, Li MZ, Xie J, Yang XL. Prevalence of type 2 diabetes and pre-diabetes among overweight or obese children in Tianjin, China. Diabet Med. 2013;30:1457–65.
Liu Y, Kuang MH, Liu Y, Yang Q-T, Xie X-X, Rang W-Q. Prevalence of hypertension among children and adolescents in china: a meta-analysis. Chinese J Child Health Care. 2017;25:59-62.
National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics. 2004;114(2 Suppl 4th Report):555–76.
Group of China Obesity Task Force. Body mass index reference norm for screening overweight and obesity in Chinese children and adolescents. Zhonghua Liu Xing Bing Xue Za Zhi. 2004;25:97–102.
Wang Y, Mi J, Shan XY, Wang QJ, Ge KY. Is China facing an obesity epidemic and the consequences? The trends in obesity and chronic disease in China. Int J Obes. 2007;31:177–88.
Ruo ran LV, Zheng X, Ying S, Li xin T, Wei G. Study on normal waist-to-hip ratio of children and adolescents in Beijing. Chin. J Sch Health. 2012;06:750–1.
Ma GS, Ji CY, Ma J, Mi J, Sung R, Xiong F, et al. Waist circumference reference values for screening cardiovascular risk factors in Chinese children and adolescents aged 7-18 years. Zhonghua Liu Xing Bing Xue Za Zhi . 2010;31:609–15.
Schwandt P. Defining central adiposity in terms of clinical practice in children and adolescents. Int J Prev Med. 2011;2:1–2.
DeLong ER, DeLong DM, Clarke-Pearson DL. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics. 1988;44:837–45.
Zhai Y, Li WR, Shen C, Qian F, Shi XM. Prevalence and correlates of elevated blood pressure in chinese children aged 6-13 years: a Nationwide School-Based Survey. Biomed Environ Sci. 2015;28:401–9.
Larkins N, Teixeira-Pinto A, Banks E, Gunasekera H, Cass A, Kearnes J, et al. Blood pressure among Australian Aboriginal children. J Hypertens. 2017;35:1801–7.
Rosner B, Cook NR, Daniels S, Falkner B. Childhood blood pressure trends and risk factors for high blood pressure: the NHANES experience 1988-2008. Hypertension. 2013;62:247–54.
Martinovic M, Belojevic G, Evans GW, Kavaric N, Asanin B, Pantovic S, et al. Hypertension and correlates among Montenegrin school children-a cross-sectional study. Public Health. 2017;147:15–19.
Zhao Y, Wang L, Xue B, Wang Y. Associations between general and central obesity and hypertension among children: The Childhood Obesity Study in China Mega-Cities. Sci Rep. 2017;7:16895.
Dasgupta K, O’Loughlin J, Chen S, Karp I, Paradis G, Tremblay J, et al. Emergence of sex differences in prevalence of high systolic blood pressure: analysis of a longitudinal adolescent cohort. Circulation. 2006;114:2663–70.
Yang Y, Dong B, Wang S, Dong Y, Zou Z, Fu L, et al. Prevalence of high blood pressure subtypes and its associations with BMI in Chinese children: a national cross-sectional survey. BMC Public Health. 2017;17:598.
Ebrahimi H, Emamian MH, Hashemi H, Fotouhi A. Prevalence of prehypertension and hypertension and its risk factors in Iranian school children: a population-based study. J Hypertens. 2018. https://doi.org/10.1097/HJH.0000000000001789.
Okpokowuruk FS, Akpan MU, Ikpeme EE. Prevalence of hypertension and prehypertension among children and adolescents in a semi-urban area of Uyo Metropolis, Nigeria. Pan Afr Med J. 2017;28:303.
Wang J, Zhu Y, Jing J, Chen Y, Mai J, Wong SH, et al. Relationship of BMI to the incidence of hypertension: a 4 years’ cohort study among children in Guangzhou, 2007–11. BMC Public Health. 2015;15:782.
Pazin DC, Rosaneli CF, Olandoski M, Oliveira ERN, Baena CP, Figueredo AS, et al. Waist circumference is associated with blood pressure in children with normal body mass index: a cross-sectional analysis of 3,417 school children. Arq Bras Cardiol. 2017;109:509–15.
Dong B, Wang Z, Song Y, Wang HJ, Ma J. Understanding trends in blood pressure and their associations with body mass index in Chinese children, from 1985 to 2010: a cross-sectional observational study. BMJ Open. 2015;5:e009050.
Ma C, Wang R, Liu Y, Lu Q, Lu N, Tian Y, et al. Performance of obesity indices for screening elevated blood pressure in pediatric population: Systematic review and meta-analysis. Medicine. 2016;95:e4811.
Dong B, Wang Z, Wang HJ, Ma J. Associations between adiposity indicators and elevated blood pressure among Chinese children and adolescents. J Hum Hypertens. 2015;29:236–40.
Kryst L, Woronkowicz A, Kowal M, Pilecki MW, Sobiecki J. Abdominal obesity screening tools in the aspects of secular trend. Anthropol Anz. 2016;73:295–312.
Lu X, Shi P, Luo CY, Zhou YF, Yu HT, Guo CY, et al. Prevalence of hypertension in overweight and obese children from a large school-based population in Shanghai, China. BMC Public Health. 2013;13:24.
Liang Jj, Chen Yj, Jin Y, Yang Wh, Mai Jc, Ma J, et al. Comparison of adiposity measures in the identification of children with elevated blood pressure in Guangzhou, China. J Hum Hypertens. 2015;29:732.
Koren D, Marcus CL, Kim C, Gallagher PR, Schwab R, Bradford RM, et al. Anthropometric predictors of visceral adiposity in normal-weight and obese adolescents. Pediatr Diabetes. 2013;14:575–84.
Tu W, Eckert GJ, DiMeglio LA, Yu Z, Jung J, Pratt JH. Intensified effect of adiposity on blood pressure in overweight and obese children. Hypertension. 2011;58:818–24.
Meng L, Liang Y, Liu J, Hu Y, Yan Y, Mi J. Prevalence and risk factors of hypertension based on repeated measurements in Chinese children and adolescents. Blood Press. 2013;22:59–64.
Acknowledgements
This study was supported by Tianjin Science and Technology Development Fund for Colleges and Universities (No: 20080132), National Natural Science Foundation of China (No: 81602922), and Ministry of Education Humanities and Social Science Fund (No: 13YJCZH281).
Author contributions
HZ conceptualized and designed the study, drafted the initial manuscript, and approved the final manuscript as submitted. XZ designed the sampling method, and coordinated and supervised data collection at schools, and approved the final manuscript as submitted. YL, BL, and JX conducted the data collection, carried out the initial analyses, and approved the final manuscript as submitted. JX gave critical comments on data analysis, revised the earlier version of the manuscript, and approved the final manuscript as submitted.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Lu, Y., Luo, B., Xie, J. et al. Prevalence of hypertension and prehypertension and its association with anthropometrics among children: a cross-sectional survey in Tianjin, China. J Hum Hypertens 32, 789–798 (2018). https://doi.org/10.1038/s41371-018-0088-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-018-0088-4
This article is cited by
-
Association between body composition and blood pressure in normal-weight Chinese children and adolescents
BMC Pediatrics (2022)
-
Sleep duration and risk of high blood pressure in Thai adolescents: the Thai National Health Examination Survey V, 2014 (NHES-V)
BMC Public Health (2022)
-
Diagnostic accuracy of anthropometric indices for discriminating elevated blood pressure in pediatric population: a systematic review and a meta-analysis
BMC Pediatrics (2022)
-
Impact of updated pediatric hypertension criteria on prevalence estimates of hypertension among Chinese children
Journal of Human Hypertension (2021)
-
Prevalence of high blood pressure and high normal blood pressure among 7- to 17-year-old children and adolescents in developed regions, China from 2014 to 2017: using new national blood pressure reference for Chinese children and adolescents
Journal of Human Hypertension (2019)