Abstract
Background
Previous studies have reported that high-dose supplementation of n-3 polyunsaturated fatty acids (PUFAs) may reduce the risk of metabolic diseases, but there is limited evidence of an effect on body fat. We examined the associations of erythrocyte n-3 PUFAs with body fat and fat distribution in a general population consuming a normal diet.
Methods
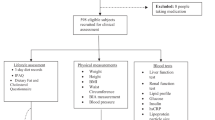
This community-based cross-sectional study included 3075 Chinese (68% women, 40–75 years) recruited between 2008 and 2013. We collected general information and measured anthropometric indices; erythrocyte n-3 PUFAs (including α-C18:3, C20:5, C22:5 and C22:6) by gas-chromatography, and fat mass (FM) and %FM at the total body (TB), android (A) and gynoid (G) regions by dual-energy X-ray absorptiometry (DXA).
Results
Both minimally and maximally adjusted models showed dose-dependent inverse associations of total and individual levels of erythrocyte n-3 PUFAs (except C20:5 n-3[EPA]) with adiposity indices. In the full model, the mean differences between quartiles 4 and 1 of total n-3 PUFAs were −1.60% (BMI), −4.06% (TB FM), −5.38% (A FM), −2.05% (G FM), −2.05% (TB %FM), −3.39% (A %FM) and −2.50% (% A/G); the ORs (95% CI) of %FM-derived obesity (≥25% for men, ≥35% for women) for the highest (vs. lowest) quartile were 0.70 (0.57, 0.86) for total n-3 PUFAs and 0.71 (0.58, 0.87), 0.96(0.78, 1.18), 0.82(0.67, 1.00), 0.66 (0.54, 0.81) for α-C18:3/C20:5/C22:5/C22:6 n-3, respectively. The favourable associations were more pronounced for the DXA-derived FM indices, measurements at the android region and for C22:6 n-3. No significant associations between C20:5 n-3 and the adiposity indices were observed.
Conclusions
Higher levels of circulating n-3 PUFAs were dose-dependently associated with better profiles of body fat and fat distribution, particularly in the abdominal regions in this population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Hotamisligil GS. Inflammation and metabolic disorders. Nature. 2006;444:860–67.
Hill JH, Solt C, Foster MT. Obesity associated disease risk: the role of inherent differences and location of adipose depots. Horm Mol Biol Clin Investig. 2018;33:1868–91.
Piche ME, Poirier P, Lemieux I, Despres JP. Overview of epidemiology and contribution of obesity and body fat distribution to cardiovascular disease: an update. Prog Cardiovasc Dis. 2018;61:103–13.
Sethi JK, Vidal-Puig AJ. Thematic review series: adipocyte biology. Adipose tissue function and plasticity orchestrate nutritional adaptation. J Lipid Res. 2007;48:1253–62.
Lorente-Cebrian S, Costa AG, Navas-Carretero S, Zabala M, Martinez JA, Moreno-Aliaga MJ. Role of omega-3 fatty acids in obesity, metabolic syndrome, and cardiovascular diseases: a review of the evidence. J Physiol Biochem. 2013;69:633–51.
Abete I, Goyenechea E, Zulet MA, Martinez JA. Obesity and metabolic syndrome: potential benefit from specific nutritional components. Nutr Metab Cardiovasc Dis. 2011;21(Suppl 2):1–15.
Buckley JD, Howe PR. Anti-obesity effects of long-chain omega-3 polyunsaturated fatty acids. Obes Rev. 2009;10:648–59.
Buckley JD, Howe PR. Long-chain omega-3 polyunsaturated fatty acids may be beneficial for reducing obesity-a review. Nutrients. 2010;2:1212–30.
Albracht-Schulte K, Kalupahana NS, Ramalingam L, Wang S, Rahman SM, Robert-McComb J, et al. Omega-3 fatty acids in obesity and metabolic syndrome: a mechanistic update. J Nutr Biochem. 2018;58:1–16.
Wang L, Manson JE, Rautiainen S, Gaziano JM, Buring JE, Tsai MY, et al. A prospective study of erythrocyte polyunsaturated fatty acid, weight gain, and risk of becoming overweight or obese in middle-aged and older women. Eur J Nutr. 2016;55:687–97.
Harris WS, Pottala JV, Lacey SM, Vasan RS, Larson MG, Robins SJ. Clinical correlates and heritability of erythrocyte eicosapentaenoic and docosahexaenoic acid content in the Framingham Heart Study. Atherosclerosis. 2012;225:425–31.
Micallef M, Munro I, Phang M, Garg M. Plasma n-3 polyunsaturated fatty acids are negatively associated with obesity. Br J Nutr. 2009;102:1370–4.
Howe PR, Buckley JD, Murphy KJ, Pettman T, Milte C, Coates AM. Relationship between erythrocyte omega-3 content and obesity is gender dependent. Nutrients. 2014;6:1850–60.
Zhuang P, Lu Y, Shou Q, Mao L, He L, Wang J, et al. Differential anti-adipogenic effects of eicosapentaenoic and docosahexaenoic acids in obesity. Mol Nutr Food Res. 2019; https://doi.org/10.1002/mnfr.201801135.
Jakobsen MU, Dethlefsen C, Due KM, Slimani N, Chajes V, May AM, et al. Plasma phospholipid long-chain n-3 polyunsaturated fatty acids and body weight change. Obes Facts. 2011;4:312–8.
Jakobsen MU, Madsen L, Skjoth F, Berentzen TL, Halkjaer J, Tjonneland A, et al. Dietary intake and adipose tissue content of long-chain n-3 PUFAs and subsequent 5-year change in body weight and waist circumference. Am J Clin Nutr. 2017;105:1148–57.
Hastert TA, Otto MCD, Le-Scherban F, Steffen BT, Steffen LM, Tsai MY, et al. Association of plasma phospholipid polyunsaturated and trans fatty acids with body mass index: results from the multi-ethnic study of atherosclerosis. Int J Obes. 2018;42:433–40.
Bender N, Portmann M, Heg Z, Hofmann K, Zwahlen M, Egger M. Fish or n3-PUFA intake and body composition: a systematic review and meta-analysis. Obes Rev. 2014;15:657–65.
Couet C, Delarue J, Ritz P, Antoine JM, Lamisse F. Effect of dietary fish oil on body fat mass and basal fat oxidation in healthy adults. Int J Obes Relat Metab Disord. 1997;21:637–43.
Krebs JD, Browning LM, McLean NK, Rothwell JL, Mishra GD, Moore CS, et al. Additive benefits of long-chain n-3 polyunsaturated fatty acids and weight-loss in the management of cardiovascular disease risk in overweight hyperinsulinaemic women. Int J Obes. 2006;30:1535–44.
DeFina LF, Marcoux LG, Devers SM, Cleaver JP, Willis BL. Effects of omega-3 supplementation in combination with diet and exercise on weight loss and body composition. Am J Clin Nutr. 2011;93:455–62.
Hill AM, Buckley JD, Murphy KJ, Howe PR. Combining fish-oil supplements with regular aerobic exercise improves body composition and cardiovascular disease risk factors. Am J Clin Nutr. 2007;85:1267–74.
Kabir M, Skurnik G, Naour N, Pechtner V, Meugnier E, Rome S, et al. Treatment for 2 mo with n-3 polyunsaturated fatty acids reduces adiposity and some atherogenic factors but does not improve insulin sensitivity in women with type 2 diabetes: a randomized controlled study. Am J Clin Nutr. 2007;86:1670–9.
Yamaoka S, Fujimoto M, Mori M, Mori H, Yamori Y. Risk reduction of lifestyle-related diseases in young adults on soy- or fish-rich traditional japanese meals. Clin Exp Pharmacol Physiol. 2007;34:S79–81.
Jang H, Park K. Omega-3 and omega-6 polyunsaturated fatty acids and metabolic syndrome: a systematic review and meta-analysis. Clin Nutr. 2019; https://doi.org/10.1016/j.clnu.2019.03.032.
Zheng JS, Huang T, Yang J, Fu YQ, Li D. Marine N-3 polyunsaturated fatty acids are inversely associated with risk of type 2 diabetes in Asians: a systematic review and meta-analysis. PloS One. 2012;7:e44525.
Raatz SK, Conrad Z, Johnson LK, Picklo MJ, Jahns L. Relationship of the reported intakes of fat and fatty acids to body weight in US adults. Nutrients. 2017;9:438.
Lentjes M, Mulligan A, Welch AA, Bhaniani A, Luben R, Khaw KT. Contribution of cod liver oil‐related nutrients (vitamins A, D, E and eicosapentaenoic acid and docosahexaenoic acid) to daily nutrient intake and their associations with plasma concentrations in the EPIC‐Norfolk cohort. J Hum Nutr Diet. 2015;28:568–82.
Shen X, Fang AP, He JJ, Liu ZQ, Guo MH, Gao R, et al. Trends in dietary fat and fatty acid intakes and related food sources among Chinese adults: a longitudinal study from the China Health and Nutrition Survey (1997-2011). Public Health Nutr. 2017;20:2927–36.
FAO/WHO. Expert consultation on fats and fatty acids in human nutrition: fats and fatty acids in human nutrition: report of an expert consultation; 10–14 November 2008. Geneva, Food and Agriculture Organization of the United Nations, 2010.
Skeaff CM, Hodson L, McKenzie JE. Dietary-induced changes in fatty acid composition of human plasma, platelet, and erythrocyte lipids follow a similar time course. J Nutr. 2006;136:565–9.
Chen YM, Liu Y, Liu YH, Wang X, Guan K, Zhu HL. Higher serum concentrations of betaine rather than choline is associated with better profiles of DXA-derived body fat and fat distribution in Chinese adults. Int J Obes. 2015;39:465–71.
Zhang CX, Ho SC. Validity and reproducibility of a food frequency questionnaire among Chinese women in Guangdong province. Asia Pac J Clin Nutr. 2009;18:240–50.
Liu B, Woo J, Tang N, Ng K, Ip R, Yu A. Assessment of total energy expenditure in a Chinese population by a physical activity questionnaire: examination of validity. Int J Food Sci Nutr. 2001;52:269–82.
Liu YH, Xu Y, Wen YB, Guan K, Ling WH, He LP, et al. Association of weight-adjusted body fat and fat distribution with bone mineral density in middle-aged chinese adults: a cross-sectional study. PloS One. 2013;8:e63339.
Morrison WR, Smith LM. Preparation of fatty acid methyl esters and dimethylacetals from lipids with boron fluoride-methanol. J Lipid Res. 1964;5:600–8.
Lillington JM, Trafford DJ, Makin HL. A rapid and simple method for the esterification of fatty acids and steroid carboxylic acids prior to gas-liquid chromatography. Clin Chim Acta. 1981;111:91–8.
Dai XW, Zhang B, Wang P, Chen CG, Chen YM, Su YX. Erythrocyte membrane n-3 fatty acid levels and carotid atherosclerosis in Chinese men and women. Atherosclerosis. 2014;232:79–85.
Li L, Wang C, Bao Y, Peng L, Gu H, Jia W. Optimal body fat percentage cut-offs for obesity in Chinese adults. Clin Exp Pharmacol Physiol. 2012;39:393–8.
Tang QQ, Lane MD. Adipogenesis: from stem cell to adipocyte. Annu Rev Biochem. 2012;81:715–36.
Hanada H, Morikawa K, Hirota K, Nonaka M, Umehara Y. Induction of apoptosis and lipogenesis in human preadipocyte cell line by n-3 PUFAs. Cell Biol Int. 2011;35:51–9.
Kim HK, Della-Fera M, Lin J, Baile CA. Docosahexaenoic acid inhibits adipocyte differentiation and induces apoptosis in 3T3-L1 preadipocytes. J Nutr. 2006;136:2965–9.
Martinez-Fernandez L, Laiglesia LM, Huerta AE, Martinez JA, Moreno-Aliaga MJ. Omega-3 fatty acids and adipose tissue function in obesity and metabolic syndrome. Prostaglandins Other Lipid Mediat. 2015;121:24–41.
Flachs P, Horakova O, Brauner P, Rossmeisl M, Pecina P, Franssen-van Hal N, et al. Polyunsaturated fatty acids of marine origin upregulate mitochondrial biogenesis and induce beta-oxidation in white fat. Diabetologia. 2005;48:2365–75.
Vazquez-Vela MEF, Torres N, Tovar AR. White adipose tissue as endocrine organ and its role in obesity. Arch Med Res. 2008;39:715–28.
Itoh M, Suganami T, Satoh N, Tanimoto-Koyama K, Yuan X, Tanaka M, et al. Increased adiponectin secretion by highly purified eicosapentaenoic acid in rodent models of obesity and human obese subjects. Arterioscler Thromb Vasc Biol. 2007;27:1918–25.
Huerta AE, Navas-Carretero S, Prieto-Hontoria PL, Martinez JA, Moreno-Aliaga MJ. Effects of alpha-lipoic acid and eicosapentaenoic acid in overweight and obese women during weight loss. Obesity. 2015;23:313–21.
Mori TA, Burke V, Puddey IB, Watts GF, O ‘Neal DN, Best JD, et al. Purified eicosapentaenoic and docosahexaenoic acids have differential effects on serum lipids and lipoproteins, LDL particle size, glucose, and insulin in mildly hyperlipidemic men. Am J Clin Nutr. 2000;71:1085–94.
So J, Wu D, Lichtenstein A, Lamon-Fava S. Docosahexaenoic acid and eicosapentaenoic acid supplementation differentially modulate pro- and anti-inflammatory cytokines in subjects with chronic inflammation (OR29-02-19). Curr Dev Nutr. 2019;3(Suppl 1):489.
Cottin SC, Sanders TA, Hall WL. The differential effects of EPA and DHA on cardiovascular risk factors. Proc Nutr Soc. 2011;70:215–31.
Snijder MB, Visser M, Dekker JM, Seidell JC, Fuerst T, Tylavsky F, et al. The prediction of visceral fat by dual-energy X-ray absorptiometry in the elderly: a comparison with computed tomography and anthropometry. International journal of obesity and related metabolic disorders. Int J Obes Relat Metab Disord. 2002;26:984–93.
Mohammad A, De Lucia Rolfe E, Sleigh A, Kivisild T, Behbehani K, Wareham NJ, et al. Validity of visceral adiposity estimates from DXA against MRI in Kuwaiti men and women. Nutr Diabetes. 2017;7:e238.
Willett W. Nutritional epidemiology, 3rd ed. Oxford University Press: New York, New York; 2013.
Mocking RJT, Assies J, Lok A, Ruhe HG, Koeter MWJ, Visser I, et al. Statistical methodological issues in handling of fatty acid data: percentage or concentration. imputation and indices. Lipids. 2012;47:541–7.
Acknowledgements
We thank all the participants and the coordination staff in the GNHS cohort study gratefully.
Funding
This study was supported by National Science Foundation of China (Nos. 81773416, 81472965, 81602853); the 5010 Programme for Clinical Researches (No. 2007032) by the Sun Yat-sen University. The funders had no role in study design, the collection, analysis and interpretation of data, the writing of the report, and in the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
YMC conceived and designed the research; YHL, TYS, YYW, CFL, CWL, FFZ collected the data; YHL performed the data analysis and wrote the paper; YMC critically revised the manuscript and had primary responsibility for final content. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Li, Yh., Sun, Ty., Wu, Yy. et al. Higher erythrocyte n-3 polyunsaturated fatty acid were associated with a better profile of DXA-derived body fat and fat distribution in adults. Int J Obes 44, 1884–1892 (2020). https://doi.org/10.1038/s41366-020-0569-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-020-0569-8
This article is cited by
-
Influence of genetic variants in FADS2 and ELOVL2 genes on BMI and PUFAs homeostasis in children and adolescents with obesity
International Journal of Obesity (2021)