Abstract
Background:
Gut immaturity is linked with postnatal intestinal disorders. However, biomarkers to assess the intestinal developmental stage around birth are lacking. The aim of this study was to gain more insight on intestinal fatty acid–binding protein (I-FABP) as an indicator of gut maturity.
Methods:
Antenatal I-FABP distribution and release was investigated in extremely premature, moderately premature, and term lambs, and these findings were verified in human urinary samples. Ileal I-FABP distribution was confirmed in autopsy material within 24 h postnatally.
Results:
Median (range) serum I-FABP levels were lower in extremely premature lambs compared with moderately premature lambs (156 (50.0–427) vs. 385 (100–1,387) pg/ml; P = 0.02). Contrarily, median early postnatal urine I-FABP levels in human infants were higher in extremely premature compared with moderately premature and term neonates (1,219 (203–15,044) vs. 256 (50–1,453) and 328 (96–1,749) pg/ml; P = 0.008 and P = 0.04, respectively). I-FABP expression was most prominent in nonvacuolated enterocytes and increased with rising gestational age (GA) in ovine and human tissue samples. The epithelial distribution pattern changed from a phenotype displaying I-FABP-positive enterocytes merely in the crypts early in gestation into a phenotype with I-FABP expressing cells exclusively present in the villus tips at term in ovine and human tissue.
Conclusion:
In this ovine and human study, increasing GA is accompanied by an increase in I-FABP tissue content. Cord I-FABP levels correlate with gestation in ovine fetuses, identifying I-FABP as a marker for gut maturation. Raised postnatal urine I-FABP levels in preterm human infants may indicate intestinal injury and/or inflammation in utero.
Similar content being viewed by others
Main
Immaturity of the gut plays a pivotal role in the development of necrotizing enterocolitis (NEC), gut-derived sepsis, and feeding problems (1). The underlying mechanisms remain poorly understood, but increased intestinal permeability and inadequate intestinal immune responses in preterm neonates are associated with gastrointestinal disorders (2,3,4). In order to define the maturational stage of the gut, markers of gut maturity are required.
A good candidate may be intestinal fatty acid-binding protein (I-FABP), which is a sensitive and specific enterocyte marker (5,6,7). It is released into the circulation as soon as the enterocyte’s cell membrane integrity is compromised, and it can be detected in urine (5,8), making it a suitable marker for intestinal pathologies such as NEC and coeliac disease (9,10). Moreover, I-FABP reflects enterocyte turnover and is exclusively present in mature enterocytes of the small and large intestine (11,12). During early fetal life, the intestinal epithelial lining consists of vacuolated, immature enterocytes, as shown in animal models and in the human gut (13,14,15). These immature cells gradually disappear with increasing gestational age (GA) and are completely replaced by mature enterocytes shortly after birth (14,16). More insight on I-FABP distribution and its release into the circulation as an indicator of gut maturity can aid in the management of gut-associated problems in premature neonates. We hypothesized that I-FABP distribution and release is gestation dependent. To test this hypothesis, I-FABP distribution and release were evaluated during gestation in utero in fetal lambs, since the developmental biology of sheep is closest to the human development for most major organs including the gut (17). In addition, the postnatal distribution and release of I-FABP were tested in preterm neonates.
Results
Ovine I-FABP Serum and Tissue Levels Increase With GA
Serum I-FABP levels were elevated (385 (range: 100–1,387) pg/ml) in moderately premature lambs (n = 15) when compared with extremely premature lambs (n = 11; 156 (50–427) pg/ml; P = 0.02; Figure 1 ). Median I-FABP levels tended to be elevated (255 (100–1,872) pg/ml) in the term group (n = 12) when compared with extremely premature lambs (P = 0.06). Accordingly, relative high amounts of I-FABP were detected in ileal homogenates of term animals when compared with extremely premature and moderately premature lambs ( Figure 2 ).
Ovine umbilical cord serum I-FABP levels determined by ELISA. I-FABP levels were significantly higher in the 130–135 d gestational age group compared with the 120–125 d group; *P = 0.02. ELISA, enzyme-linked immunosorbent assay; I-FABP, intestinal fatty acid–binding protein.
Ovine ileal tissue I-FABP content determined by western blot. Relative band intensities (corrected for actin) measured by Odyssey are depicted in the graph. *P = 0.04. I-FABP, intestinal fatty acid–binding protein.
I-FABP Distribution Pattern in the Ovine Ileal Epithelium Is GA Dependent
I-FABP expression was most prominent in nonvacuolated enterocytes. In extremely premature lambs, positive cells were only found in the primitive crypts and basis of the villi ( Figure 3a ). In the moderately premature group, the crypts and lower parts of the villi were positive for I-FABP ( Figure 3b ). In the term animals, I-FABP expression was exclusively present in the villus tips ( Figure 3c ).
Immunohistochemical staining of I-FABP in ovine ileum. (a) 120–125 d. (b) 130–135 d. (c) 140–145 d. (d) Negative control. I-FABP expression gradually disappears from the crypts with advancing gestational age, changing into a phenotype characterized by I-FABP expression in the villus tips (magnification ×200; scale bar = 100 μm). I-FABP, intestinal fatty acid–binding protein.
I-FABP Distribution Pattern in Human Intestine Resembles the Ovine Situation
The postnatal distribution of I-FABP in extremely preterm, moderately preterm, and term born infants was studied in neonates who died within 24h after birth. Patient characteristics are summarized in Table 1 . As in ovine tissue, the same patterns of enterocyte vacuolization were seen dependent on GA. Moreover, I-FABP was predominantly present in nonvacuolated enterocytes. I-FABP expressing cell numbers increased with rising GA, comparable with the I-FABP distribution pattern in ovine fetuses ( Figure 4 ).
Immunohistochemical staining of I-FABP in human ileum. (a) <28 wk. (b) 28–37 wk. (c) 37–42 wk. (d) Negative control. Paralleling ovine intestinal development, I-FABP expression gradually disappears from the crypts with advancing gestational age, changing into a phenotype characterized by I-FABP expression in the villus tips (magnification ×200; scale bar = 100 μm). I-FABP, intestinal fatty acid–binding protein.
Epithelial Proliferation and Apoptosis Are Not Dependent on GA in Human and Ovine Intestine
As epithelial I-FABP distribution was dependent on GA, the relationship with proliferation and apoptosis was investigated. To determine whether increased I-FABP levels were related with increased epithelial proliferation rates, the proliferative marker Ki-67 was stained. Ki-67 positive cells were primarily located in the crypts of the ileum and to a lesser extent in the villi in all animals ( Figure 5 ). No differences were found between the GA groups. Similar to the ovine data, proliferation was not different throughout gestation on human tissue sections as measured by Ki67 (data not shown).
Immunohistochemical staining of Ki-67. (a) 120–125 d. (b) 130–135 d. (c) 140–145 d. (d) Negative control. No differences were found between the different gestational age groups (magnification ×200; scale bar = 100 μm).
To evaluate whether increased I-FABP levels correlated with decreased epithelial apoptosis rates, immunohistochemical staining for caspase-3 was performed, revealing sparse apoptotic activity in ileal tissue. No differences in caspase-3 presence were seen in GA groups ( Figure 6 ).
Immunohistochemical staining of caspase-3. (a) 120–125 d. (b) 130–135 d. (c) 140–145 d. (d) Negative control. Caspase-3-positive cells are indicated by arrowheads. No differences in caspase-3 expression were found between age groups (magnification ×200; scale bar = 100 μm).
Human Urinary I-FABP Levels Are Elevated in the Extremely Premature Neonates Shortly After Birth
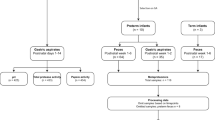
Thirty-four neonates were included in the current study; 16 in the group with GA <28 wk (extremely premature), 18 in the group with GA 28–37 wk (moderately premature), and 12 in the group with GA 37–42 wk (term). Patient characteristics are outlined in Table 2 , and clinical parameters are summarized in Table 3 . Expectedly, GA at birth weight were significantly different between the groups. Moreover, there was a significant difference between the groups in Apgar scores, histopathologically confirmed chorioamnionitis, postnatal use of antibiotics and nonsteroidal anti-inflammatory drugs, and timing of first enteral feeding.
Median urinary I-FABP levels at 0–3 days postpartum were significantly higher in extremely premature neonates compared with moderately premature neonates and term neonates (1,219 (203–15,044) pg/ml, 256 (50–1,453) pg/ml (P = 0.008), 328 (96–1,749) pg/ml (P = 0.04); Figure 7a ). This difference was still present at 4–7 d postpartum between extremely premature neonates (631 (191–3,670) pg/ml) and moderately premature neonates (282 (67–1,863) pg/ml, P = 0.004) but not between extremely premature neonates and term neonates (302 (66–3,261); P = 0.16; Figure 7b ). From 0–3 d to 4–7 d postpartum, I-FABP levels decreased significantly (P = 0.04), with median 24%. However, this difference was obviously caused by a decrease of urinary I-FABP levels in the extremely premature group (median decrease: 64%; P = 0.04), while in the moderately premature and term groups, urinary I-FABP levels did not decrease significantly (P = 0.79 and P = 0.45, respectively).
Urinary I-FABP determined by ELISA in extremely premature, moderately premature, and term neonates. (a) I-FABP levels in the first 3 d of life. *P = 0.008; **P = 0.04. (b) Urinary I-FABP 4–7 d postpartum. *P = 0.004. ELISA, enzyme-linked immunosorbent assay; I-FABP, intestinal-fatty acid-binding protein.
Discussion
This study shows that the intestinal distribution pattern of I-FABP is GA dependent in both sheep and humans. In the ovine gut, I-FABP levels increase during gestation, which is also reflected by I-FABP levels in umbilical cord serum upon delivery. The epithelial distribution pattern changes from a phenotype displaying I-FABP positive enterocytes merely in the crypts at 120–125 d of gestation to a phenotype with I-FABP expressing cells restricted to the villus tips in term lambs. In human intestine, similar changes of epithelial maturation during gestation were seen. However, the human urinary I-FABP levels during the first 3 d after birth were inconsistent with ovine data and human in utero data.
The differences may be explained by the following aspects. First, the fetal gut contains immature vacuolated enterocytes, which decrease in number through gestation, as observed in the current study and by others (15,18). After birth, vacuolated enterocytes rapidly mature, resulting in high enterocyte turnover rates and I-FABP release. As the extremely premature gut contains more immature enterocytes, turnover rates can be higher compared with the less premature intestine. This seems however unlikely as the current data do not show differences between GA groups in mucosal proliferation rates in the first days after birth. Second, the stimuli of bacterial colonization after birth may lead to an inflammatory response, leading to damage of immature enterocytes due to inadequate immune response and barrier function associated with prematurity (19). Elevated I-FABP levels may even underestimate the amount of enterocyte damage. Early intestinal damage affects primarily the villus tips. In extreme preterm infants, such mucosal injury may not lead to a significant increase in serum and urinary I-FABP levels since the protein is primarily expressed by epithelial cells lining the crypts and lower half of the villi. Reference values in clinical practice should therefore be adapted according to GA. In this context, the number of days after birth should be taken into account. Third, in the ovine model lambs are born prematurely because of human intervention. In humans however, preterm labor is frequently caused by chorioamnionitis (20). Incidence of chorioamnionitis was indeed increased in extremely premature neonates in this cohort. Previous studies have shown that chorioamnionitis can cause intestinal damage in utero (21,22,23). It is therefore likely that premature born neonates have already suffered intestinal damage in utero, reflected by high urinary I-FABP levels directly after birth. Other confounding factors such as indomethacin use may also increase I-FABP levels in premature neonates after birth. Finally, differences in renal function might contribute to antenatal and postnatal I-FABP levels. However, due to its small molecular size (14 kDa), plasma and urinary I-FABP levels are hardly affected by renal function. In a recent study, we have shown that differences in urinary I-FABP levels are not affected when corrected for creatinine even in severely ill neonates (24).
The data in this study have important implications. As intestinal and circulatory I-FABP levels increase with GA, I-FABP reflects gut maturation, which is underlined by the histological change of phenotype. This makes I-FABP a potentially suitable marker for intestinal maturation, at least in the sterile and healthy intestine. Markers for intestinal maturation are currently lacking and may be of great value for guiding feeding strategies. It is shown that standardized feeding protocols result in earlier successful enteral feeding without increased rates of major morbidities (25,26). A clinical study is needed to investigate whether implementation of I-FABP measurements in such a protocol is beneficial, for instance, with slower feeding advancements in patients with low perinatal I-FABP levels reflecting gut immaturity. However, it should be noted that urinary I-FABP levels within the first 3 d after birth are not suitable for this purpose, since these levels do not reflect the in utero situation, possibly due to confounding factors such as bacterial colonization, chorioamnionitis, and indomethacin use. It may therefore be more adequate to measure perinatal I-FABP levels in cord blood, which is acquired routinely in most in-hospital deliveries. In the current study, this was impossible due to its retrospective design; however, the ovine cord blood data underline this hypothesis. In the future, it should be investigated whether human cord blood I-FABP levels correlate with the development of gastrointestinal morbidity, such as NEC and feeding intolerance.
In this study, neonates with intestinal disease were excluded to avoid confounding effects on I-FABP levels. It is appealing to investigate whether (extremely) premature neonates with high I-FABP levels shortly after birth are at increased risk for developing intestinal disorders or whether these high levels normalize without an increased risk. I-FABP as a screening tool for NEC has been investigated before (27). Urinary I-FABP levels in the first 90 h after birth were measured in 55 preterm neonates. In this group, nine infants developed NEC, all of them having elevated I-FABP values. Sixteen other neonates also had high I-FABP values but did not develop NEC. Interestingly, all 16 patients had significantly more feeding problems compared with the infants with normal I-FABP values. Future studies could address the effectiveness of preventive strategies in premature neonates with high I-FABP levels.
In conclusion, I-FABP distribution is maturation dependent both in ovine and human gut. Increasing GA parallels an increase in I-FABP tissue content and circulating I-FABP levels in sheep, making I-FABP a promising marker of gut maturation. However, this study shows that extremely preterm neonates suffer from more intestinal damage early in life than late preterm infants, indicating that the effect of maturation is confounded by postnatal factors. Urinary I-FABP levels in the first days after birth are therefore not suitable to assess gut maturation. Future research should evaluate whether I-FABP levels in human cord blood accurately measure gut maturation.
Methods
Animals
This study was approved by the Animal Ethics Committee of the University of Maastricht, The Netherlands. Time-mated pregnant ewes and fetuses were humanely killed by i.v. pentobarbital (150–200 mg/kg) injection, and lambs were delivered by cesarean section either extremely preterm (120–125 dGA, comparable to <28 wk GA in humans), preterm (130–135 d GA, comparable to 28–37 wk GA in humans), or term (140–145 d GA, comparable to 37–42 wk GA in humans). Samples of the small intestine were collected and both snap frozen and fixated in formalin. Cord blood was immediately sampled from the umbilical artery, cooled on ice, centrifuged at 3,500 rotations per minute for 15 min, and serum samples were stored at −80 °C until batch analysis.
Patients
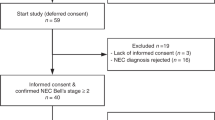
Neonates admitted to the neonatal intensive care unit at the Maastricht University Medical Centre between July 2007 and July 2008 were eligible for inclusion, if not admitted after the third postnatal day. Neonates with asphyxia or those developing gastrointestinal events such as NEC or feeding problems were excluded retrospectively at neonatal intensive care unit discharge. Infants were divided into an extremely premature group (<28 wk of gestation), a moderately premature group (28–37 wk), and a term group (37–42 wk). Eligibility and inclusion numbers are outlined in Table 4 . It was anticipated that only 25 extremely premature infants would be admitted to the neonatal intensive care unit during the study period, therefore the first 25 consecutive infants of all three groups were approached for consent. None of the approached parents refused consent; however, some infants were excluded retrospectively based on the exclusion criteria mentioned above. Written informed consent was obtained from both parents. The study was conducted with the approval from the local medical ethical committee, and the principles of good clinical practice were followed during this study.
Urine samples were collected by placement of a dental cotton roll (Henry Schein, Almere, The Netherlands) in the diaper of the neonate starting at the first day after birth. Once the roll was filled with urine, it was placed in a sterile 5 ml syringe (Becton Dickinson, Oxford, UK), the urine was pressed into Micronic tubes (Micronic B.V., Lelystad, the Netherlands), and stored at −20°C until analysis. Two samples were collected from each patient; one on days 0–3 after birth and one on days 4–7. Enteral feeding was initiated before the first urine sample was taken.
Human Tissue Collection
In the pathology department database of the Maastricht and Utrecht University Medical Centres, neonates who died within 24h after birth between January 2005 and December 2012 were identified. Of those patients in which intestinal tissue had been collected at postmortem examination, paraffin-embedded sections of ileal tissue were used for immunohistochemistry. Comparisons were made between extremely premature (<28 wk of gestation), moderately premature (28–37 wk), and term (37–42 wk) neonates.
Antibodies
The following antibodies were used for immunohistochemistry: rabbit antihuman cleaved caspase-3 (Asp175; Cell Signaling, Danvers, MA), rabbit antihuman I-FABP (in-house developed), and mouse antihuman Ki-67 (Clone MIB-1; Dako, Glostrup, Denmark). Goat antirabbit IgG labeled with horseradish peroxidase (Jackson ImmunoResearch, West Grove, PA) and biotin-conjugated swine antirabbit IgG (Dako), and goat antimouse IgG (Dako) were used as secondary antibodies.
For western blot, the following antibodies were used: rabbit antihuman I-FABP (in-house developed) and mouse antihuman β-actin clone ac15 (Sigma, St Louis, MO). The secondary antibodies used for western blot were IRDye 800cw goat antirabbit (LI-COR Biosciences, Lincoln, NE) and IRDye 800cw goat antimouse (LI-COR Biosciences).
Immunohistochemistry
Ovine intestinal samples were immediately immersed in 4% formaldehyde fixative (Unifix; Klinipath, Duiven, The Netherlands) and incubated for 24 h. Tissue samples were embedded in paraffin, and 4 μm sections were cut. Sections were first deparaffinized in xylene and then rehydrated in graded ethanol to distilled water. Endogenous peroxidase activity was blocked with 0.5% H2O2. Antigen retrieval was performed in citrate buffer at 90 °C for 30 min (Ki-67, I-FABP). Unspecific binding sites were blocked using normal goat serum (Ki-67) for 30 min at room temperature. Slides were incubated with the primary antibody for 60 min at room temperature (I-FABP, caspase-3) or overnight (Ki-67) at 4 °C, and then incubated with the appropriate secondary antibody for 1 h at room temperature. The tissue sections were prepared with AB-complex (Ki-67, caspase-3). For I-FABP, positive staining was visualized with 3-amino-9-ethylcarbazole. Counterstaining of the nuclei was performed using hematoxylin. For Ki-67 and caspase-3, the staining was visualized with Nickel-sulfate 3,3-diaminobenzidine, counterstaining with Nuclear Fast Red.
Enzyme-Linked Immunosorbent Assay
Urinary and serum I-FABP was measured using an in-house enzyme-linked immunosorbent assay that selectively detects human and ovine I-FABP (standard: 10–800 pg/ml, lower detection level: 50 pg/ml). I-FABP concentrations are given in pg/ml. Human urine samples were batch analyzed after inclusion of the complete cohort.
Western Blot
Western blot was used for the analysis of I-FABP protein content of ovine ileal samples. First, snap-frozen tissues were homogenized in radioimmunoprecipitation assay buffer containing protease inhibitors (1 mmol/l phenylmethylsulfonyl fluoride, 0.1 U/ml aprotinin, and 1 µg/ml leupeptin). Determination of the protein concentration in the final supernatants was performed using the bicinchoninic acid protein assay. Equal amounts of total protein (20 or 40 µg where applicable) were heated at 100 °C for 10 min in sodium dodecyl sulfate buffer containing β-mercaptoethanol. Proteins were separated by running the samples through a 15% sodium dodecyl sulfate–polyacrylamide gel and transferred to a nitrocellulose membrane. After a blocking step, the membranes were incubated with the primary antibody overnight. Incubation with the secondary antibody was performed for 1 h. Membranes were reprobed with mouse antihuman β-actin to ensure equal loading. Protein bands were visualized using an Odyssey Infrared Imaging System (LI-COR Biosciences).
Statistical Analysis
Normality was tested using Kolmogorov–Smirnov test. Between-groups comparisons for continuous data were performed by Mann–Whitney U-test and Kruskal–Wallis with post hoc Dunn’s multiple comparison test, where appropriate. All data are expressed as median and range. A two-sided P value <0.05 was considered statistically significant. Statistical analysis was performed using Prism 5.0 for Windows (Graphpad software, San Diego, CA).
Statement Of Financial Support
No financial assistance was received to support this study.
Disclosure
No disclosures reported.
References
Neu J . Gastrointestinal development and meeting the nutritional needs of premature infants. Am J Clin Nutr 2007;85:629S–34S.
Rouwet EV, Heineman E, Buurman WA, ter Riet G, Ramsay G, Blanco CE . Intestinal permeability and carrier-mediated monosaccharide absorption in preterm neonates during the early postnatal period. Pediatr Res 2002;51:64–70.
Neu J, Chen M, Beierle E . Intestinal innate immunity: how does it relate to the pathogenesis of necrotizing enterocolitis. Semin Pediatr Surg 2005;14:137–44.
Lin PW, Nasr TR, Stoll BJ . Necrotizing enterocolitis: recent scientific advances in pathophysiology and prevention. Semin Perinatol 2008;32:70–82.
Kanda T, Fujii H, Tani T, et al. Intestinal fatty acid-binding protein is a useful diagnostic marker for mesenteric infarction in humans. Gastroenterology 1996;110:339–43.
Thuijls G, Derikx JP, van Wijck K, et al. Non-invasive markers for early diagnosis and determination of the severity of necrotizing enterocolitis. Ann Surg 2010;251:1174–80.
Derikx JP, Evennett NJ, Degraeuwe PL, et al. Urine based detection of intestinal mucosal cell damage in neonates with suspected necrotising enterocolitis. Gut 2007;56:1473–5.
van de Poll MC, Derikx JP, Buurman WA, et al. Liver manipulation causes hepatocyte injury and precedes systemic inflammation in patients undergoing liver resection. World J Surg 2007;31:2033–8.
Ng EW, Poon TC, Lam HS, et al. Gut-associated biomarkers L-FABP, I-FABP, and TFF3 and LIT score for diagnosis of surgical necrotizing enterocolitis in preterm infants. Ann Surg 2013;258:1111–8.
Adriaanse MP, Tack GJ, Passos VL, et al. Serum I-FABP as marker for enterocyte damage in coeliac disease and its relation to villous atrophy and circulating autoantibodies. Aliment Pharmacol Ther 2013;37:482–90.
Derikx JP, Blijlevens NM, Donnelly JP, et al. Loss of enterocyte mass is accompanied by diminished turnover of enterocytes after myeloablative therapy in haematopoietic stem-cell transplant recipients. Ann Oncol 2009;20:337–42.
Veerkamp JH, Paulussen RJ, Peeters RA, Maatman RG, van Moerkerk HT, van Kuppevelt TH . Detection, tissue distribution and (sub)cellular localization of fatty acid-binding protein types. Mol Cell Biochem 1990;98:11–8.
Trahair J, Robinson P . The development of the ovine small intestine. Anat Rec 1986;214:294–303.
Asari M, Kawaguchi N, Wakui S, Fukaya K, Kano Y . Development of the bovine ileal mucosa. Acta Anat (Basel) 1987;129:315–24.
Moxey PC, Trier JS . Specialized cell types in the human fetal small intestine. Anat Rec 1978;191:269–85.
Skrzypek T, Valverde Piedra JL, Skrzypek H, Kazimierczak W, Biernat M, Zabielski R . Gradual disappearance of vacuolated enterocytes in the small intestine of neonatal piglets. J Physiol Pharmacol 2007;58:Suppl 3:87–95.
Wolfs TG, Jellema RK, Turrisi G, Becucci E, Buonocore G, Kramer BW . Inflammation-induced immune suppression of the fetus: a potential link between chorioamnionitis and postnatal early onset sepsis. J Matern Fetal Neonatal Med 2012;25:Suppl 1:8–11.
Trahair JF, Wilson JM, Neutra MR . Identification of a marker antigen for the endocytic stage of intestinal development in rat, sheep, and human. J Pediatr Gastroenterol Nutr 1995;21:277–87.
Adkins B, Leclerc C, Marshall-Clarke S . Neonatal adaptive immunity comes of age. Nat Rev Immunol 2004;4:553–64.
Goldenberg RL, Hauth JC, Andrews WW . Intrauterine infection and preterm delivery. N Engl J Med 2000;342:1500–7.
Been JV, Lievense S, Zimmermann LJ, et al. Chorioamnionitis as a risk factor for necrotizing enterocolitis: a systematic review and meta-analysis. J Pediatr 2013;162:236–42 e2.
Wolfs TG, Buurman WA, Zoer B, et al. Endotoxin induced chorioamnionitis prevents intestinal development during gestation in fetal sheep. PLoS One 2009;4:e5837.
Wolfs TG, Kallapur SG, Knox CL, et al. Antenatal ureaplasma infection impairs development of the fetal ovine gut in an IL-1-dependent manner. Mucosal Immunol 2013;6:547–56.
Reisinger KW, Derikx JP, Thuijls G, et al. Noninvasive measurement of intestinal epithelial damage at time of refeeding can predict clinical outcome after necrotizing enterocolitis. Pediatr Res 2013;73:209–13.
Kuzma-O’Reilly B, Duenas ML, Greecher C, et al. Evaluation, development, and implementation of potentially better practices in neonatal intensive care nutrition. Pediatrics 2003;111(4 Pt 2):e461–70.
McCallie KR, Lee HC, Mayer O, Cohen RS, Hintz SR, Rhine WD . Improved outcomes with a standardized feeding protocol for very low birth weight infants. J Perinatol 2011;31:Suppl 1:S61–7.
Mannoia K, Boskovic DS, Slater L, Plank MS, Angeles DM, Gollin G . Necrotizing enterocolitis is associated with neonatal intestinal injury. J Pediatr Surg 2011;46:81–5.
Acknowledgements
We thank Jasper V. Been for thoroughly reviewing the manuscript and Nico Kloosterboer for expert technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Reisinger, K., Elst, M., Derikx, J. et al. Intestinal fatty acid–binding protein: a possible marker for gut maturation. Pediatr Res 76, 261–268 (2014). https://doi.org/10.1038/pr.2014.89
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2014.89
This article is cited by
-
Neonatal anemia relates to intestinal injury in preterm infants
Pediatric Research (2022)
-
Normative values for circulating intestinal fatty acid binding protein and calprotectin across gestational ages
BMC Pediatrics (2020)
-
Selective IL-1α exposure to the fetal gut, lung, and chorioamnion/skin causes intestinal inflammatory and developmental changes in fetal sheep
Laboratory Investigation (2016)
-
Clinical significance of FABP2 expression in newborns with necrotizing enterocolitis
World Journal of Pediatrics (2016)
-
Are EGF and TLR-4 crucial to understanding the link between milk and NEC?
Mucosal Immunology (2015)