Abstract
Background:
Acylcarnitines are biomarkers of fatty acid metabolism, and examining their patterns in preterm newborn may reveal metabolic changes associated with particular conditions related to prematurity. Isomeric acylcarnitines in dried blood spots (DBS) and plasma have never been assessed in preterm infants.
Methods:
We studied 157 newborn divided into four groups by weeks of gestational age (GA), as follows: 22–27 wk in group 1; 28–31 wk in group 2; 32–36 wk in group 3; and 37–42 wk in group 4. Samples were collected on the third day of life. Acylcarnitines were separated and quantified using ultra-performance liquid chromatography tandem mass spectrometry.
Results:
Acylcarnitine concentrations correlated significantly with GA and birth weight in both DBS and plasma samples. Concentrations were lower in preterm newborn, except for acylcarnitines derived from branched-chain amino acids, which were higher and correlated with enteral feeding. On day 3 of life, no correlations emerged with gender, respiratory distress syndrome, bronchopulmonary dysplasia, surfactant administration, or mechanical ventilation.
Conclusion:
We established GA-based reference ranges for isomeric acylcarnitine concentrations in preterm newborn, which could be used to assess nutritional status and the putative neuroprotective role of acylcarnitines.
Similar content being viewed by others
Main
Fatty acid metabolism takes place in the mitochondria, and β-oxidation is the main process by which fatty acids are oxidized by means of a sequential removal of two-carbon units from the acyl chain. Fatty acids are activated primarily in the cytosol by fatty acyl-CoA synthase to carnitine derivatives, then they are carried by specific acylcarnitine (AC) transferases and translocases into the mitochondrial matrix where β-oxidation can begin. In successive cycles of reactions, this process generates a series of ACs that are one two-carbon unit shorter and it continues until only two or three carbons are left (forming acetyl-CoA or propionyl-CoA, respectively). AC detection is of great interest for the purpose of assessing the carnitine pool, which is essential to the diagnosis of several metabolic disorders. AC profiling is a powerful tool for the neonatal screening and diagnosis of fatty acid oxidation and organic acid disorders (1). Alongside the importance of AC in tissues such as heart and muscle, recent data indicate an involvement of these compounds in neurological protection and disorders. ACs are believed to have both energy-providing and neuroprotective roles in the brain (2,3), based on the assumption that the fatty acid oxidation pathway is active in neurons, given the localization of carnitine palmitoyltransferase enzyme 1 (CPT1) (2,4). Investigating AC profiles in preterm infants may therefore reveal metabolic changes associated with perinatal brain injury.
Mass spectrometry (MS) is commonly used to quantify ACs. Millington and co-workers pioneered tandem mass spectrometry (MS/MS) methods for assaying carnitine and ACs in urine and plasma samples (5), and in dried blood spots (DBS). The development of electrospray ionization (ESI) has enabled the sample to be added to a continuously flowing solvent stream (flow injection analysis, FIA) and offers a more robust, more sensitive alternative to fast atom bombardment (FAB) MS/MS for AC profiling (6). Each metabolic disorder is associated with primary and secondary markers and a cut-off is defined for each marker. Cut-offs for free carnitine and AC esters in DBS have been published and used in newborn screening programs (7).
AC concentrations vary with birth weight (BW), gestational age (GA), and age at the time of collection (8). As reported previously (9), premature infants have different mean values from term-born infants due to their lower birth weight and to treatments administered at the neonatal intensive care unit (NICU), so different cutoffs would need to be defined to reduce the risk of false-positive cases.
While many studies have investigated changes in preterm infants’ free carnitine levels by measuring the effects of supplementation (10,11,12), or a breast milk diet (13), little is known about the AC profile of preterm infants. Meyburg compared AC cord blood levels in preterm and full-term infants, correlating them with BW (14), and investigated AC levels longitudinally in DBS of preterm newborn during the first 4 wk of life (15). Another study was recently conducted on amino acids and AC profiles in DBS from preterm newborn (16).
FIA-ESI-MS/MS remains the first choice when screening for inborn errors of metabolism (6). The method is useful for its high throughput, but is unable to differentiate between isomers. Since numerous AC species are isomeric or isobaric with other compounds, chromatographic separation provides more detailed diagnostic information (17). The chromatographic profile of AC in preterm newborn has never been investigated to date.
The aim of our study was thus to assess AC profiles in neonates born at term and with different degrees of immaturity with a view to shedding light on metabolism in preterm infants. For the first time, AC measurements were obtained using an ultra-performance liquid chromatography (UPLC) MS/MS method capable of discriminating between isomeric ACs, as previously described by our group (17), to assess the contribution of ACs deriving from branched-chain amino acid (BCAA) catabolism.
Results
The Shapiro–Wilk test showed that the distributions of AC concentrations in DBS and plasma were not normal. Data were expressed as µmol/l and means with SDs, medians, and percentiles were calculated. Boxplots of the free carnitine and the main ACs identified in DBS and plasma are shown in Figures 1 and 2 , respectively. The sample of newborn was divided into four groups by GA: group 1 (G1) included those with a GA of 22–27 wk; group 2 (G2) those with a GA of 28–31 wk; group 3 (G3) those with a GA of 32–36 wk; and group 4 (G4) those with a GA of 37–42 wk.
Box and whisker plots of characteristic short-, medium-, and long-chain acylcarnitines (ACs) in dried blood spots (DBS): (a) free carnitine, (b) C2, (c) 2-methylbutyril, (d) C6, (e) C8, (f) C10, (g) C12, (h) C14, and (i) C16. The values are stratified by gestational age (GA) group, from G1 to G4. The box shows the medians (solid bar), interquartile ranges (IQRs) (box), and 90th and 10th percentiles (whiskers).
Box and whisker plots of characteristic short-, medium-, and long-chain acylcarnitines (ACs) in plasma: (a) free carnitine, (b) C2, (c) 2-methylbutyril, (d) C6, (e) C8, (f) C10, (g) C12, (h) C14, and (i) C16. The values are stratified by gestational age (GA) group, from G1 to G4. The box shows the medians (solid bar), interquartile ranges (IQRs) (box), and 90th and 10th percentiles (whiskers).
Acylcarnitine Profiles in DBS
The AC concentrations in DBS are shown in Tables 1 and 2 ; P values were calculated with the Kruskal–Wallis test.
When the data were divided by GA group, most of the analytes differed significantly (with the exception of C3, C4, C16:1OH, C16OH, and C18:1). The Mann–Whitney test results showed significant differences when the premature newborn groups G1, G2, and G3 were compared with the term-born group G4. The results of comparisons between the preterm groups were only statistically significant for G1 vs. G2. (Supplementary Table S1 online).
All AC concentrations correlated directly with GA, except for the ACs derived from BCAAs, which were inversely correlated. The amounts of medium-chain (C6, C8, C10), the related unsaturated fatty acids and long-chain (C14, C16, C18) ACs appeared to be 20–50% lower in the extremely preterm neonates (G1) than in G4. Concentrations of 2-methyl-butyrylcarnitine were higher in the preterm groups (0.179 ± 0.057 µmol/l in G1, 0.124 ± 0.041 µmol/l in G2, and 0.092 ± 0.026 µmol/l in G3) than in G4 (0.069 ± 0.018 µmol/l). Only minor differences were seen for isobutyryl carnitine (isoC4) and C5:1.
Acylcarnitine Profiles in Plasma
Plasma AC concentrations are summarized in Tables 3 and 4 .
The AC profiles of plasma samples differed slightly from those found in DBS, especially as regards the long-chain ACs. The levels of C14 and C16 were lower in plasma than in DBS. The differences related to the contribution of long-chain ACs of the erythrocyte membranes (8).
Analyses by GA group indicated that free, isoC4, C5:1, C5, and C18:1 did not differ significantly, while—as in DBS—the other ACs showed significant differences when each preterm group was compared with G4. No differences emerged between the preterm groups, apart from 2-methylbutyrylcarnitine, which was significantly higher in the premature (0.246 ± 0.101, 0.149 ± 0.057, and 0.090 ± 0.03 µmol/l in G1, G2 and G3 respectively) than in the term-born (0.049 ± 0.019 µmol/l in G4); and it correlated inversely with GA, confirming the findings in DBS (Supplementary Table S1 online).
Correlation of Acylcarnitines With Clinical Data
Differences in analyte concentrations were assessed by gender, birth weight, feeding method, calorie intake, total parenteral nutrition, and use of antenatal steroids. For patients admitted to the NICU, some variables—i.e., respiratory distress syndrome (RDS), bronchopulmonary dysplasia (BPD), sepsis, exogenous surfactant administration, mechanical ventilation and transfusions—correlated with AC concentrations.
Gender, birth weight, and AC profile. No differences in AC levels were found between males and females.
In DBS, significant positive correlations emerged between AC levels and BW, with the exception of free, C5OH, isoC4, C5:1, 2-methyl-butyryl and C5, which were inversely correlated. In plasma, ACs correlated significantly with BW as in DBS, except for free, isoC4 and C5:1, which were not correlated. A negative correlation with BW and GA was also found in plasma for C14OH, C16:1OH, C16OH, C18:2, C18:1, C18, C18:2OH, C18:1OH, C18OH, and C20 (Supplementary Table S2 online).
Mode of delivery and AC profile. The Kruskal–Wallis test revealed significant differences emerged for some ACs in relation to whether the mode of delivery was vaginal (VD) or cesarean section (CS). The differences were not confirmed, however, when the comparison was drawn by GA group using the Mann–Whitney test (no such comparison could be drawn for G1 because they were all cases of CS). The results obtained with the Kruskal–Wallis test referred to all the newborn and were biased by the large number of vaginally delivered term-born infants.
Respiratory diseases and AC profile. No associations were found between RDS or BPD and AC concentrations, not even when intra-group differences were considered. Similarly, no significant differences emerged in the AC profiles of newborn who were or were not administered exogenous surfactants, or who required mechanical ventilation in the first 3 d of life.
Nutrition and AC profile. No correlations came to light between ACs and fat intake, intravenous fluids or calorie intake.
C5:1, 2-methyl-butyryl, C5, C4DC, and C6DC correlated inversely with the amounts of enteral feeding administered on the first, second, and third days of life (Spearman −0.28 < R < −0.59, P < 0.01) (Supplementary Table S2 online).
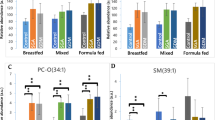
To assess AC levels by type of feeding, term-born neonates were grouped as: breastfed (BF, n = 27; 53%), mixed fed (MF, n = 21; 41%), and formula fed (FF, n = 3; 6%). The BF and MF infants had lower free carnitine levels than the FF (21.94 ± 8.04; 22.17 ± 7.96 and 30.56 ± 7.96 µmol/l, P < 0.01). C5:1 and C5 were similarly reduced: C5:1 was 0.028 ± 0.003 in BF, 0.028 ± 0.002 in MF, and 0.010 ± 0.002 µmol/l in FF (P < 0.001); and C5 was 0.072 ± 0.017, 0.076 ± 0.017, and 0.047 ± 0.010 µmol/l in BF, MF and FF respectively (P < 0.05, only for MF vs. FF). A higher level of isoC4 was also seen in FF (0.375 ± 0.203 µmol/l, P < 0.01) by comparison with BF (0.192 ± 0.066 µmol/l) and MF (0.208 ± 0.078 µmol/l).
Treatments and AC profile. There were no significant differences in AC profile between the newborn who did and those who did not receive blood transfusions, nor were there any changes in the AC concentrations under antenatal steroids. The newborn of mothers treated with antenatal corticosteroid therapy did show significant differences in several acylcarnitines, however, in DBS and plasma, when the whole sample of newborn was considered. When the whole sample was stratified by GA, the newborn’s distribution was too heterogeneous, since G1 consisted entirely of cases treated with antenatal steroids while G4 had none. No changes were seen under antenatal steroids in G2. In G3, C4, C12:1, and C12 were lower in both DBS and plasma: in DBS, C4 was 0.12 ± 0.10 and 0.21 ± 0.09 µmol/l (P < 0.001), C12:1 was 0.08 ± 0.02 vs. 0.10 ± 0.04 µmol/l (P = 0.003), and C12 was 0.09 ± 0.02 vs. 0.12 ± 0.03 µmol/l (P = 0.050) in the treated vs. untreated newborn, respectively; in plasma, C4 was 0.19 ± 0.13 vs. 0.33 ± 0.16 µmol/l (P = 0.008), C12:1 was 0.03 ± 0.01 vs. 0.05 ± 0.03 µmol/l (P = 0.028), and C12 was 0.03 ± 0.01 vs. 0.05 ± 0.03 µmol/l (P = 0.095) in the treated and untreated cases, respectively.
Discussion
This study provides a GA-based quantification of AC levels in preterm newborn and shows that premature are metabolically dissimilar from term-born infants, with significant differences across GA groups. The UPLC-MS/MS method used in this study enabled isomeric ACs to be detected for the first time in DBS and plasma samples from premature neonates.
Acylcarnitine profiles did not correlate with gender, RDS, BPD, or the use of surfactants or mechanical ventilation. Preterm infants showed no signs of carnitine deficiency, but significantly lower amounts of ACs derived from fatty acid metabolism, whereas the BCAA-derived ACs were significantly higher and correlated with enteral feeding.
Free Carnitine Status
Carnitine, or β-hydroxy-γ-trimethylaminobutyric acid, carries long-chain fatty acids across the mitochondrial membrane where they undergo β-oxidation. While it is not considered an essential nutrient in adults, it may be conditionally essential in the newborn. In the immediate postnatal period, the metabolism needs to undergo postnatal adaptation because neonates have to be able to switch their energy production from glucose to fatty acid metabolism. Endogenous carnitine synthesis is limited in the neonate due to low levels of γ-butyrobetaine hydroxylase, the enzyme that catalyzes the final step in carnitine synthesis, from γ-butyrobetaine to carnitine (18). In addition, due to a decreased tissue storage and the placental transfer of carnitine occurring during the third trimester, preterm newborn are particularly at risk of carnitine deficiency (19,20,21). Previous investigations have shown that neonates receiving parenteral nutrition devoid of carnitine are unable to synthesize sufficient carnitine to maintain normal plasma concentrations (19,20,22,23), and Bonner suggested parenteral carnitine supplementation to increase the reserves in preterm newborns (22). Many authors have studied free carnitine levels in preterm infants using various methods and obtained different results. Seliger, Meyburg, Giannacopoulou, and Shenai found higher free carnitine levels in preterm than in full-term infants (12,15,24,25), whereas newborn screening data (26) and a study on Japanese preterm infants (27) identified GA-related carnitine deficiencies.
In our sample, the free carnitine levels in the preterm groups were the same as in the full-term group (they were only found significantly higher in G4 than in G2, in DBS). On intra-group comparisons, free carnitine did not change on the first or second days of life in enterally fed newborn, while a small increase was apparent on the third day. The preterm infants enrolled in this study were not given L-carnitine supplementation, and any exogenous intake consisted only of the amount contained in the formula used (0.12–0.15 mg/l of carnitine according to the product label). This is comparable with the carnitine content of expressed human milk, which is estimated to be 0.105 mg/l (28). The main nutrients given to our infants were amino acids and glucose, and enteral feeding with preterm formula contributed up to 10% of their total feeding. Under these nutritional conditions, the preterm infants reached carnitine levels comparable with those of term-born infants as a consequence of the administration of lysine and methionine—the precursors of carnitine. This suggests that newborn infants are able to synthesize carnitine in the same way, whether they are born prematurely or at term. It has already been demonstrated (29) that human infants are capable of converting exogenous trimethyllysine into carnitine and carnitine esters at a low rate. In this study, the total contribution of carnitine from blood transfusions (the use of which was similar in the various groups) was negligible, as confirmed by the lack of correlation between transfusions and AC concentrations in our statistical results.
Fatty Acid–Derived Acylcarnitines
Unlike Meyburg and Mandour (15,16), we found lower concentrations of almost all ACs in preterm than in term-born infants, except for the isomeric form deriving from BCAA catabolism. This finding could relate to low lipid levels at birth, and particularly to limited amounts of lipids in preterm newborn, as suggested by previous studies (19,20). The amount of palmitoylcarnitine in our groups G1, G2, and G3 was respectively 60, 37, and 30% lower than in G4. Similar observations have been reported by Zytkovicz (9), and more recently by Ryckman (30). It was demonstrated that hepatic fatty acid oxidation was the same in preterm and term-born pigs (31), but available data on preterm infants are still limited. We might speculate that the production of palmitoylcarnitine from palmitoyl-CoA and carnitine induced by CPT enzyme activity occurs at the same rate in all infants, whatever their GA at birth, but a proper experimental design should lead to a better understanding of this issue.
To assess the contribution of nutrition, the type of feeding was considered in our G4 group of term-born infants (the only group to have been fed in different ways). They were fed breast milk alone (BF), breast milk supplemented with formula (MF), or formula alone (FF). The formula contained a large amount of fatty acids derived from triglycerides, which accounted for 35–50% of the total energy supply for newborn. The AC concentrations did not change with the three types of feed. FF infants showed only a slight increase in free carnitine, C5 and C5:1 levels by comparison with the BF and MF newborn, probably due to the free carnitine in the formula and to the contribution of absorbed amino acids. This result might indicate that type of feeding has no influence on AC profile, but our FF subgroup included only three infants, so further evidence from a randomized clinical trial is needed to confirm this impression.
BCAA-Derived Acylcarnitines
BCAA-derived AC levels were significantly higher in premature infants. The effect of nutrition might explain the increase in isoC4, C5:1, and C5 isomers in preterm neonates, and the strong inverse correlation with GA and BW. IsoC4 is an intermediate of valine catabolism, while 2-methylbutyrylcarnitine and isovalerylcarnitine (C5) balance the intermediates of isoleucine and leucine BCAA catabolism, respectively. Coupled with the known BCAA catabolic pathways, these findings suggest that these ACs—which are direct products of BCAA catabolism—could accumulate with mild amino acid overfeeding, as previously reported (32). These changes may reflect an increased BCAA turnover by specific translocases (33). The effects appeared more evident for leucine and isoleucine metabolites, than for valine.
The concentrations of C3 acylcarnitine (which represents propionyl-CoA, an intermediate of isoleucine and valine catabolism) did not differ significantly between the groups, and the amounts found in plasma suggested a different trend from that of the previously mentioned BCAA metabolites.
Consistently with this hypothesis, we found higher levels of leucine/isoleucine (measured by newborn screening in DBS) in preterm infants given intravenous amino acid supplementation (126.9 ± 39.6 vs. 117.0 ± 24.9 µmol/l in those not given supplements). The mean concentration of leucine/isoleucine in the G3 group was very similar to that of the infants given no supplementation, while in G1 and G2 the values were 23 and 21% higher, respectively, than in G3. No significant differences were found in valine concentrations when intravenous amino acid supplementation was (91.8 ± 34.5 µmol/l) or was not administered (90.2 ± 21.7 µmol/l). A reduction in the β-oxidative cascade in preterm infants is therefore likely.
Consistently with our data, an increase in the levels of short- and medium-chain AC esters (C4, C5, C6, and C8) has been reported in both venous and arterial umbilical blood in very low birth weight (VLBW) newborn, but not in their mother’s blood (34), suggesting an increased transplacental transfer of short- and medium-chain AC esters towards the fetus in extreme prematurity. The data obtained will need to be confirmed by further studies focusing on establishing whether these higher levels are a consequence of NICU treatments or transplacental transfer.
Conclusions
It is well known that AC profiling is done in the biochemical screening of fatty acid oxidation and organic acid metabolic disorders. Defining cutoffs and ranges for these analytes, and ratios between them, for the purpose of newborn screening is challenging, but has recently been validated thanks to international cooperation (7). As reported by Zytkovicz and Ryckman (9,35), preterm infants represent a population that contributes significantly to the false positive rate. There are many reasons for this, including endogenous and metabolic differences due to their lower BW and immaturity, or the effects of treatments administered at the NICU. Our study showed that AC levels are lower in the preterm than in term-born infants and, in contrast with previously reported data (15,16), we found higher levels of BCAA-related metabolites in the former than the latter. This goes to show the importance of defining cutoffs: it is essential for each laboratory to establish its own concentrations and cutoffs for NICU patients and preterm infants in order to assess AC profiles accurately and avoid false negative or false positive results in the MS/MS screening of preterm infants.
Amino acids, and especially essential BCAAs, have a crucial role in premature infant nutrition. Several studies have been conducted with a view to optimizing parenteral amino acid supplementation and meeting nutritional needs without inducing any toxicity or metabolic acidosis. The results of our study suggest that BCAA-related AC levels rise with mild overfeeding, so the ACs could serve as useful biomarkers for identifying safe intake with a view to avoiding any harmful accumulation of BCAA catabolic products. In addition to the well-established roles of ACs in metabolism, recent data (34) have demonstrated their role in the brain, and identified carnitine/acylcarnitine carriers in the central and peripheral nervous system, and particularly its mitochondrial localization in the sensory neurons. Almost all nutrients affect the major brain processes, and especially neurogenesis, neural differentiation, myelination, and synaptogenesis, which all proceed at a rapid rate between 22 and 42 wk of age after conception. Nutritional strategies to optimize brain growth and development thus include assessing nutritional status at birth, providing nutrients in abundance, and immediately making good any nutritional deficits in both preterm and term-born neonates. The GA-based ranges reported here could be used to assess nutritional status and the reported neuroprotective role of ACs in future studies.
Methods
Patients
This study was performed at the nursery and NICU of the Women’s and Children’s Health Department at the University of Padova, Italy. The study was approved by the Padova University Hospital Ethical Committee. Written informed consent was obtained from parents prior to participation.
Over a period of 15 mo, neonates admitted to the nursery and NICU within 24 h of birth were screened for enrolment in the study. Exclusion criteria included refusal of parental consent, suspected inherited disorders of metabolism, or evidence a major congenital anomaly. We enrolled 163 newborn, but 6 were excluded because their data in the clinical database were incomplete. The 157 patients forming the study sample were divided into four groups (G1 to G4) by GA, as explained previously. The newborn’s demographic, clinical, and nutritional data were obtained from their medical records and are summarized in Table 5 .
Details of any transfusions of plasma, red blood cells (RBCs), whole blood, packed RBCs or extracorporeal membrane oxygenation (ECMO) were recorded. Based on the NICU protocol, enteral nutrition was begun on the first day of life, clinical conditions permitting. A minimum of 10 ml/kg/d was generally used initially, then the volume was increased as tolerated. Intravenous fluids were given to ensure an overall hydration of 60–70 ml/kg/d on the first day, increasing to around 20 ml/kg/d thereafter. Lipid intake was started with 0.5 g/kg/d and increased by 1 g/kg/d up to a maximum of 3 g/kg/d. Glucose administration started at a rate of 6–10 g/kg/d and was increased by 2 g/kg/d to maintain glycemia between 80–100 mg/dl. Amino acid intake was started at 1.0 g/kg/d and raised by 0.5–1 g/kg/d up to a maximum of 3.5 g/kg/d on day 3. For healthy term-born neonates, breast milk alone was given ad libitum.
Sample Collection
Plasma and DBS specimens were obtained simultaneously from each neonate on the third day of life. Whole blood was drawn by heel prick and spotted on S&S Grade 903 filter paper (Whatman, International, Maidstone, UK), during routine neonatal metabolic screening; it was dried at room temperature and stored at −20 °C until analysis. Neonatal plasma was collected (about 10 µl) using heparinized capillary tubes to harvest blood from the heel. The tubes were centrifuged for 5 min at 13,000g. Plasma aliquots were stored at −20 °C until analysis.
Sample Analysis
Acylcarnitines in DBS and plasma were measured using an UPLC-ESI-MS/MS method described elsewhere (17). Briefly, ACs from a 3.2 mm DBS and 6 µl of plasma were extracted with 100 µl of labeled internal standard methanol solution, evaporated under a nitrogen flow at 60 °C and converted into their butyl esters by adding 100 µl of freshly prepared butanol solution containing 5% v/v of acetyl chloride and heating to 60 °C for 20 min. Chromatographic separation was done using an UPLC system equipped with a BEH C18 column. A Waters Micromass Quattro Ultima (Waters, Milford, MA) tandem quadrupole MS/MS system equipped with an electrospray ion source (ESI) operating in positive mode was used for the analysis. The multiple reaction monitoring (MRM) mode was used to scan for specific mass ion intensities. Ions at m/z 85 produced by fragmentation were monitored. Concentrations of ACs were measured by integrating the peak area and fitting with calibration curves using QuanLynx software (Waters, Version 4.1)
Statistics
Statistical analysis was performed with the STATISTICA 6.0 (Stat Soft, Tulsa, OK) and SPSS for Windows (version 21, SPSS IBM, New York, NY) software packages. The Shapiro–Wilk test was used to see whether the distributions of AC esters were normal. The Kruskal–Wallis rank test and the Mann–Whitney U-test signed rank test were used to investigate significant differences between the analytes in DBS and plasma. Associations between clinical variables and AC concentrations were examined using Spearman’s rank correlation test and expressed as Spearman correlation coefficients. Significance was assumed for P < 0.05.
Disclosure
The authors declare no conflict of interest.
References
Carpenter KH, Wiley V . Application of tandem mass spectrometry to biochemical genetics and newborn screening. Clin Chim Acta 2002;322:1–10.
Andrews ZB, Liu ZW, Walllingford N, et al. UCP2 mediates ghrelin’s action on NPY/AgRP neurons by lowering free radicals. Nature 2008;454:846–51.
Jones LL, McDonald DA, Borum PR . Acylcarnitines: role in brain. Prog Lipid Res 2010;49:61–75.
Lee J, Wolfgang MJ . Metabolomic profiling reveals a role for CPT1c in neuronal oxidative metabolism. BMC Biochem 2012;13:23.
Millington DS, Norwood DL, Kodo N, Roe CR, Inoue F . Application of fast atom bombardment with tandem mass spectrometry and liquid chromatography/mass spectrometry to the analysis of acylcarnitines in human urine, blood, and tissue. Anal Biochem 1989;180:331–9.
Rashed M, Ozand PT, Harrison ME, Watkins PJF, Evans S . Electrospray tandem mass spectrometry in the diagnosis of organic acidemias. Rapid Commun Mass Spectrom 1994;8: 129–33.
McHugh D, Cameron CA, Abdenur JE, et al. Clinical validation of cutoff target ranges in newborn screening of metabolic disorders by tandem mass spectrometry: a worldwide collaborative project. Genet Med 2011;13:230–54.
Chace DH, Pons R, Chiriboga CA, et al. Neonatal blood carnitine concentrations: normative data by electrospray tandem mass spectometry. Pediatr Res 2003;53:823–9.
Zytkovicz TH, Fitzgerald EF, Marsden D, et al. Tandem mass spectrometric analysis for amino, organic, and fatty acid disorders in newborn dried blood spots: a two-year summary from the New England Newborn Screening Program. Clin Chem 2001;47:1945–55.
Cairns PA, Stalker DJ . Carnitine supplementation of parenterally fed neonates. Cochrane Database Syst Rev 2000;4:CD000950.
Honzík T, Chrastina R, Hansíková H, et al. Carnitine concentrations in term and preterm newborns at birth and during the first days of life. Prague Med Rep 2005;106:297–306.
Seliger G, Kantelhardt E, van der Wal C, et al. L-carnitine level in neonates - a large, retrospective analysis. Arch Perinatal Med 2007;13:17–20.
Cederblad G, Svenningsen N . Plasma carnitine and breast milk carnitine intake in premature infants. J Pediatr Gastroenterol Nutr 1986;5:616–21.
Meyburg J, Schulze A, Kohlmueller D, Linderkamp O, Mayatepek E . Postnatal changes in neonatal acylcarnitine profile. Pediatr Res 2001;49:125–9.
Meyburg J, Schulze A, Kohlmueller D, et al. Acylcarnitine profiles of preterm infants over the first four weeks of life. Pediatr Res 2002;52:720–3.
Mandour I, El Gayar D, Amin M, Farid TM, Ali AA . Amino acid and acylcarnitine profiles in premature neonates: a pilot study. Indian J Pediatr 2013;80:736–44.
Gucciardi A, Pirillo P, Di Gangi IM, Naturale M, Giordano G . A rapid UPLC-MS/MS method for simultaneous separation of 48 acylcarnitines in dried blood spots and plasma useful as a second-tier test for expanded newborn screening. Anal Bioanal Chem 2012;404:741–51.
Arenas J, Rubio JC, Martín MA, Campos Y . Biological roles of L-carnitine in perinatal metabolism. Early Hum Dev 1998;53 Suppl:S43–50.
Schmidt-Sommerfeld E, Penn D, Wolf H . Carnitine blood concentrations and fat utilization in parenterally alimented premature newborn infants. J Pediatr 1982;100:260–4.
Schiff D, Chan G, Seccombe D, Hahn P . Plasma carnitine levels during intravenous feeding of the neonate. J Pediatr 1979;95:1043–6.
Shenai JP, Borum PR . Tissue carnitine reserves of newborn infants. Pediatr Res 1984;18:679–82.
Bonner CM, DeBrie KL, Hug G, Landrigan E, Taylor BJ . Effects of parenteral L-carnitine supplementation on fat metabolism and nutrition in premature neonates. J Pediatr 1995;126:287–92.
Takahashi M, Sawaguchi S . Lipid metabolism in parenterally alimented neonates: carnitine blood concentrations and fat utilization. Indian J Pediatr 1983;50:161–8.
Giannacopoulou C, Evangeliou A, Matalliotakis I, et al. Effects of gestation age and of birth weight in the concentration of carnitine in the umbilical plasma. Clin Exp Obstet Gynecol 1998;25:42–5.
Shenai JP, Borum PR, Mohan P, Donlevy SC . Carnitine status at birth of newborn infants of varying gestation. Pediatr Res 1983;17:579–82.
Schulze A, Lindner M, Kohlmüller D, Olgemöller K, Mayatepek E, Hoffmann GF . Expanded newborn screening for inborn errors of metabolism by electrospray ionization-tandem mass spectrometry: results, outcome, and implications. Pediatrics 2003;111(6 Pt 1):1399–406.
Tokuriki S, Hayashi H, Okuno T, et al. Biotin and carnitine profiles in preterm infants in Japan. Pediatr Int 2013;55:342–5.
Penn D, Dolderer M, Schmidt-Sommerfeld E . Carnitine concentrations in the milk of different species and infant formulas. Biol Neonate 1987;52:70–9.
Vaz FM, Melegh B, Bene J, et al. Analysis of carnitine biosynthesis metabolites in urine by HPLC-electrospray tandem mass spectrometry. Clin Chem 2002;48(6 Pt 1):826–34.
Ryckman KK, Dagle JM, Shchelochkov OA, et al. Association of amino acids with common complications of prematurity. Pediatr Res 2013;73:700–5.
Campbell JA, Martin JE, Melendez K, Stout MB, Lyvers-Peffer PA . Postnatal hepatic fatty acid oxidative capacity of preterm pigs receiving TPN does not differ from that of term pigs and is not affected by supplemental arachidonic and docosahexaenoic acids. J Nutr 2010;140:752–9.
Newgard CB, An J, Bain JR, et al. A branched-chain amino acid-related metabolic signature that differentiates obese and lean humans and contributes to insulin resistance. Cell Metab 2009;9:311–26.
Roe DS, Roe CR, Brivet M, Sweetman L . Evidence for a short-chain carnitine-acylcarnitine translocase in mitochondria specifically related to the metabolism of branched-chain amino acids. Mol Genet Metab 2000;69:69–75.
Tonazzi A, Mantovani C, Colella M, Terenghi G, Indiveri C . Localization of mitochondrial carnitine/acylcarnitine translocase in sensory neurons from rat dorsal root ganglia. Neurochem Res 2013;38:2535–41.
Ryckman KK, Berberich SL, Shchelochkov OA, Cook DE, Murray JC . Clinical and environmental influences on metabolic biomarkers collected for newborn screening. Clin Biochem 2013;46:133–8.
Acknowledgements
We thank the medical, nursing, and laboratory staff who contributed to data collection and analysis at the NICU and the Women’s and Children’s Health Department, University of Padova. We also thank Paola Dalla Via and Martina Betto for their contribution to data collection and sample storage during the course of the study.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary Tables
(DOC 54 kb)
PowerPoint slides
Rights and permissions
About this article
Cite this article
Gucciardi, A., Zaramella, P., Costa, I. et al. Analysis and interpretation of acylcarnitine profiles in dried blood spot and plasma of preterm and full-term newborns. Pediatr Res 77, 36–47 (2015). https://doi.org/10.1038/pr.2014.142
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2014.142
This article is cited by
-
Associations of maternal plasma and umbilical cord plasma metabolomics profiles with birth anthropometric measures
Pediatric Research (2023)
-
Upregulating carnitine palmitoyltransferase 1 attenuates hyperoxia-induced endothelial cell dysfunction and persistent lung injury
Respiratory Research (2022)
-
Exploring the functional and metabolic effects of adding garra fish meal to a plant-based broiler chicken diet
Tropical Animal Health and Production (2022)
-
Does metabolomic profile differ with regard to birth weight?
Pediatric Research (2021)
-
Fatal pitfalls in newborn screening for mitochondrial trifunctional protein (MTP)/long-chain 3-Hydroxyacyl-CoA dehydrogenase (LCHAD) deficiency
Orphanet Journal of Rare Diseases (2018)