Abstract
In the general population, it is unknown whether stress-related perinatal factors influence lymphocyte subset counts in neonates. The aim of this study was to assess the associations of perinatal factors related to stress and hypoxia (mode of delivery, Apgar scores, and umbilical cord blood pH) with absolute lymphocyte subset counts (T, B, NK, helper T, cytotoxic T, naïve, memory T) in cord blood of 571 neonates. This study was embedded in a population-based prospective cohort study from fetal life onwards. All models were adjusted for gestational age, birth weight, gender, maternal fever, and each of the other perinatal stress-relating factors. Our results showed that increasing stress-related mode of delivery was positively associated with NK and memory T-lymphocyte subset counts (all p < 0.01). Effects of Apgar scores on lymphocyte subsets were explained by umbilical cord blood pH. Lower umbilical cord blood pH was associated with higher B, NK, and memory T-lymphocyte counts (all p < 0.05). Effects of mode of delivery and umbilical cord blood pH on other lymphocyte subsets were not observed. We conclude that, in the general population, lymphocyte subset counts in neonates increase with increasing stress- and hypoxia-related perinatal factors.
Similar content being viewed by others
Main
The immunologic status of the neonate is frequently established by assessing absolute numbers of various lymphocyte subsets in cord blood (1–4). However, such data at birth must be interpreted with care since the lymphocyte subset counts might be influenced by growth, stress, and hypoxia related events that occur in late prenatal and early postnatal life. It has been suggested that the distribution of lymphocyte subsets is related to gestational age at birth and birth weight (5–8). It is not well known whether other perinatal factors associated with fetal well-being, stress and hypoxia, including mode of delivery, Apgar scores, or umbilical cord blood pH, influence the various lymphocyte subset counts at birth.
So far, studies on mode of delivery and lymphocyte subsets remain inconclusive. This might be due to small study populations, the variability of lymphocyte subsets studied, or not taking other possible influencing factors into account (5,6,9–16). Results of the majority of these studies suggested a tendency toward increased lymphocyte subset counts in neonates born by vaginal delivery compared with neonates born by caesarean delivery (9–11,13–16). The endocrine-metabolic variations during a stressful delivery, particularly hypoxia and the increase of catecholamines and cortisol, were considered as the main cause of these effects (17–19). Additionally to this stress concept, adverse Apgar scores and umbilical cord blood pH, both results of perinatal hypoxia, are thought to influence lymphocyte subset counts at birth (9,20–22).
We examined in 571 neonates participating in a population-based prospective cohort study, the associations of perinatal factors related to stress and hypoxia, including mode of delivery, Apgar scores, and umbilical cord blood pH with absolute numbers of lymphocytes (T, B, and NK) and T-lymphocyte subsets (helper, cytotoxic, naïve, and memory T) in cord blood of neonates.
METHODS
Design.
This study was embedded in the Generation R Study, a population-based prospective cohort study from fetal life until young adulthood. The Generation R Study was designed to identify early environmental and genetic determinants of growth, development, and health and has been described previously in detail (23,24). More detailed assessments of fetal and postnatal growth and development were conducted in a subgroup of 1232 Dutch pregnant women and their children, referred to as the Generation R Focus Study (23,24). Of all approached pregnant women and their partners, 79% participated in the Generation R Focus Study. Their children were born between February 2003 and August 2005. The Medical Ethics Committee of the Erasmus Medical Center, Rotterdam, has approved the study. Written informed consent was obtained from all participants.
Mode of delivery, Apgar scores, and umbilical cord blood pH.
Information about mode of delivery, 1- and 5-min Apgar scores (assigning a score of 0–2 to heart rate, respiratory effort, muscle tone, reflex irritability, and color), and umbilical cord blood pH were obtained from standardized delivery registrations of midwives and obstetricians (23–26). Heparinized cord blood samples were taken from an immediate clamped, isolated piece of the umbilical cord. Cord blood gases were analyzed on routine automatic gas check machines for pH, Po2, and Pco2, whereas base excess was computed. The delay between cord blood sampling and determination was less than 60 min. The blood gas analyzers were calibrated and standardized with reference gases and pH solutions.
Immunophenotyping of lymphocyte subsets.
Venous cord blood was sampled in heparinized tubes by midwives and obstetricians immediately after delivery and transported at room temperature to the Immunology laboratory of the Erasmus Medical Center within 24 h. Umbilical cord blood samples not received within 24 h (weekend days) were excluded, since flow cytometric analyses of those samples showed no reliable results in the pilot phase of the study. Flow-cytometric immunophenotyping was performed to determine absolute numbers of lymphocytes (T, B, and NK) and T-lymphocyte subsets (helper, cytotoxic, naïve, and memory T). For this, the MAb CD3, CD19, CD16.CD56, CD4, CD8, CD45RA, and CD45RO were conjugated with the labels FITC (FITC, Becton Dickinson, Erebodegem, Belgium), peridin chlorophyll protein (PerCP, Becton Dickinson, Erebodegem, Belgium), peridin chlorophyll protein-cychrome 5.5 (PerCP-Cy5.5, Becton Dickinson, Erebodegem, Belgium), allophycocyanin (APC, Becton Dickinson, Erebodegem, Belgium), phycoerythrin (PE, Becton Dickinson, Erebodegem, Belgium; Dako, Glosstrup, Denmark), phycoerythrin-cyanin dye (PE-cy7, Becton Dickinson, Erebodegem, Belgium), allophycocyanin-cyanin dye (APC-cy7, Becton Dickinson, Erebodegem, Belgium), and rhodamine (RD1, Beckman Coulter, Mijdrecht, The Netherlands) (Table 1). Absolute numbers of T, B, and NK lymphocytes were determined with the lysed whole blood technique (50 μL of whole blood per sample) using the routine standardized single platform method with BD TruCOUNT Tubes of Becton Dickinson (BD). With this, lymphocytes were gated on the basis of CD45 and FSC to prevent contamination of unlysed erythrocytes (27–29). The samples were measured on a Beckman Coulter flow cytometer (BD) and analyzed with BD CellQuest software as indicated by the manufacturer. Subsets of the T lymphocytes were determined using 6-color staining and detected on a BD LSR II flow cytometer (Becton Dickinson, San Jose, CA). This flow cytometer is routinely used in the diagnostic laboratory and every day reference calibration beads are used. The subsets of T lymphocytes were analyzed with BD FacsDIVA. Therefore, erythrocytes of 1 mL whole blood were lysed using 50 mL ammonium chloride. After centrifugation, leukocytes were washed twice and suspended in 900 μL PBS/1% BSA/0.1% NaAz. Of this cell suspension (5–10 × 106/mL), 50 μL was incubated for 10 min at room temperature with combinations of the optimally titrated labeled MAb. After incubation, the cells were washed and subsequently identified by flow cytometry. Using a BD LSR II flow cytometer that had been calibrated with rainbow beads, 10,000 lymphocytes were measured. The relative count of helper T lymphocytes, cytotoxic T lymphocytes, naïve T lymphocytes, and memory T lymphocytes was expressed as the percentage within the total T lymphocyte population and calculated by the average of 2–4 independent incubations for each subset. The absolute counts of the T lymphocyte subsets were subsequently calculated from the absolute T lymphocyte counts as obtained by the lysed whole blood technique. The absolute counts of the total T lymphocytes determined with the single platform method were compared with the recalculated counts of the total T lymphocytes (% of lymphocytes within the leukocyte count, determined by a cell counter). There was no significant difference between the two methods (30).
Covariates.
Information about date of birth, birth weight, and gender was obtained from midwives and hospital registries. Gestational age was established by the first fetal ultrasound examination after enrolment (31). Information about maternal fever (>38°C), indicating a possible systemic underlying infection, was asked for in the questionnaire send to mothers >30 wk of gestation (“did you had a fever (>38°C) in the last two months?”) (24).
Statistical analysis.
Differences of maternal and neonatal characteristics between neonates with and without umbilical cord blood samples were assessed by the independent sample t test for continuous normal distributed variables, nonparametric Mann-Whitney test for continuous non-normal distributed variables and the χ2 test for categorical variables. Data on all lymphocyte subsets were log-transformed to obtain normally distributed variables. Associations of mode of delivery, continuously measured Apgar scores, and umbilical cord blood pH with absolute numbers of lymphocyte subsets were analyzed using multiple linear regression models. Additionally, regression models were adjusted for the potential confounder's gestational age, birth weight, gender, and maternal fever. Finally, regression models were additionally adjusted for each of the stress-related perinatal factors to determine the independent effect of mode of delivery, Apgar scores, and umbilical cord blood pH. Measures of associations are presented as log-transformed mean differences and regression coefficients, which can be interpreted as percentages after multiplying by 100 (32), or as geometric mean differences with their 95% confidence interval. The statistical analyses were performed using the Statistical Package of Social Sciences version 11.0 for Windows (SPSS Inc., Chicago, IL).
RESULTS
In total, 1232 women were enrolled in the Generation R Focus Study. Mothers with weekend deliveries (n = 202), twin pregnancies (n = 24), and pregnancies leading to perinatal death (n = 2) were excluded from the present analysis. Of the remaining 1004 singleton live births, cord blood was collected in 889 (88.5%) infants. Immunophenotyping of lymphocytes in cord blood was not possible in 318 infants, mainly due to nonheparinized cord blood samples. Of the remaining 571 infants, 10.0% (n = 57) were siblings since mothers were allowed to participate with second or more pregnancies in the Generation R Focus study. These infants were included in the present study, since there were no differences in results after excluding them from the analyses.
Analyses of missing immunophenotyped cord blood samples (n = 433) showed that neonates without immunophenotyped cord blood samples more often were born by caesarean delivery (20.3% and 12.2%, p < 0.05), had a lower median gestational age (40.1 and 40.4 wk, p < 0.01), and lower mean birth weight (3454 and 3562 g, p < 0.01) than neonates with immunophenotyped cord blood samples.
Characteristics of the mothers and their neonates are presented in Table 2. Of the mothers, 72.6% had a vaginal, 15.2% a vacuum or forceps assisted, and 12.2% a cesarean delivery. Median Apgar scores of 1 and 5 min after birth of the neonates were 9 (range, 2–10) and 10 (range, 5–10), respectively. Mean umbilical cord blood pH was 7.26. The medians of the lymphocyte subset counts are demonstrated in Table 2.
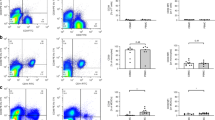
Neonates born by a forceps- or vacuum-assisted delivery had 45% higher NK lymphocyte counts (p < 0.001) than neonates born by a vaginal delivery (Table 3). No differences were found for T and B lymphocyte counts. Within the T-lymphocyte population, cytotoxic and memory T-lymphocyte counts were increased. Neonates born by a caesarean delivery had 9% lower T (p = 0.04) and 40% lower NK lymphocyte counts (p < 0.001) than neonates born by a vaginal delivery. B lymphocyte counts did not differ. Within the T-lymphocyte population, helper and naïve T lymphocyte counts were decreased in neonates born by a caesarean delivery.
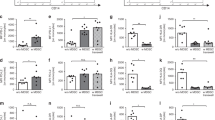
Per point increase in 1-min Apgar score, neonates had 8% lower B lymphocyte (p = 0.001) and 12% lower NK lymphocyte counts (p < 0.001). No significant changes in T lymphocytes and T lymphocyte subset counts were found for 1-min Apgar score. Apgar scores at 5 min after birth revealed 5%, 11%, and 15% lower T, B, and NK lymphocyte counts, respectively, per point increase (all p < 0.01). Cytotoxic T-lymphocyte counts were decreased with 7% (p = 0.006). No effect of the 5-min Apgar score was seen on the other T lymphocyte subset counts.
Per 0.1-point increase in umbilical cord blood pH, 5%, 22% and 30% lower T, B, and NK lymphocytes were found, respectively (all p < 0.05). Umbilical cord blood pH was not associated with the absolute numbers of T-lymphocyte subsets.
The adjusted effect estimates of the various modes of delivery on T and B lymphocyte counts improved (p < 0.05), but on cytotoxic and naïve T, lymphocyte counts declined (p > 0.05) (Fig. 1). The associations of modes of delivery with the other absolute numbers of lymphocyte subsets did not materially change, nor did the associations of 1- and 5-min Apgar scores and umbilical cord blood pH with absolute numbers of T, B, and NK lymphocytes and T-lymphocyte subsets (Figs. 2 and 3).
Absolute numbers of lymphocyte and T-lymphocyte subsets in neonates born by various modes of deliveries. All models were adjusted for gestational age, birth weight, gender, and maternal fever. □ = forceps or vacuum assisted delivery, ▪ = vaginal delivery, and  = caesarean section delivery. Values are geometric means (95% confidence intervals); reference category is vaginal delivered neonates. *p < 0.05, **p < 0.01.
= caesarean section delivery. Values are geometric means (95% confidence intervals); reference category is vaginal delivered neonates. *p < 0.05, **p < 0.01.
(A) Absolute numbers of lymphocyte subsets in neonates with 1-min Apgar scores at birth. All models were adjusted for gestational age, birth weight, gender, and maternal fever. The estimated back-transformed regression lines reflect the number of lymphocyte subsets per point increase in 1-min Apgar score. (B) Absolute numbers of lymphocyte subsets in neonates with 5-min Apgar scores at birth. All models were adjusted for gestational age, birth weight, gender, and maternal fever. The estimated back-transformed regression lines reflect the number of lymphocyte subsets per point increase in 5-min Apgar score. Both panels (line, no symbol) T lymphocytes; • B lymphocytes; ○ NK lymphocytes; ▪ Helper T lymphocytes; □, cytotoxic T lymphocytes; ▴, naïve T lymphocytes; ▵, memory T lymphocytes. *p < 0.05, **p < 0.01.
Absolute numbers of lymphocyte subsets in neonates with various umbilical cord blood pHs at birth. All models were adjusted for gestational age, birth weight, gender, and maternal fever. The estimated back-transformed regression lines reflect the number of lymphocyte subsets per 0.1 point increase in umbilical cord blood pH. (Line, no symbol), T lymphocytes; •, B lymphocytes; ○, NK lymphocytes; ▪, Helper T lymphocytes; □, cytotoxic T lymphocytes; ▴, naïve T lymphocytes; ▵, memory T lymphocytes. *p < 0.05, **p < 0.01.
An independent effect for mode of delivery on NK lymphocyte and memory T-lymphocyte counts (p < 0.01) was found, but not for the other lymphocyte subset counts (Table 4). The effect of Apgar scores on all lymphocyte subset counts declined (p > 0.05). Umbilical cord blood pH showed an independent association with B, NK, and memory T-lymphocyte counts (p < 0.05), but not with the other T lymphocyte subset counts.
DISCUSSION
This study showed that independent of the other perinatal stress-relating factors, increasing mode of delivery associated stress showed increasing NK and memory T-lymphocyte counts and lower umbilical cord blood pH showed higher NK, B, and memory T lymphocytes. We did not observe independent effects of 1- and 5-min Apgar scores on lymphocyte subsets.
Previous studies on mode of delivery did not assess the effects on all lymphocyte and T-lymphocyte subset counts (5,9–13,15,16,33). These studies showed inconclusive results, probably due to the small study populations (12–126 subjects). One large study of umbilical cord blood samples (more than 8000 cord blood units), banked for future umbilical cord blood transplantation, showed decreased percentages of helper T, cytotoxic T and B lymphocytes, and increased percentages of NK lymphocytes in cord blood of neonates born by a caesarean delivery compared with vaginally delivered neonates (6). Differences between vaginal and forceps or vacuum deliveries, the exact amount of change in absolute numbers of lymphocyte subsets, and the specific maternal and neonatal characteristics were not presented. Our study showed effects of mode of delivery mainly on NK lymphocytes. The precise functional role of these lymphocytes during labor remains to be studied. Forceps- and vacuum-assisted delivered neonates showed the highest lymphocyte subset counts and caesarean-delivered neonates the lowest lymphocyte subset counts. This phenomenon suggests a continuous trend of increasing recruitment of lymphocyte subsets into neonatal blood with increasing mode of delivery-associated stress. Underlying biologic mechanisms might be that neonates born by vaginal deliveries have higher levels of catecholamines and cortisol compared with neonates born by caesarean deliveries (16–19,33–35). Vaginal delivered neonates with higher umbilical cord blood cortisol levels have higher lymphocyte counts (16,19). It is has been suggested that infants born by a caesarean delivery have less recruitment of lymphocyte subsets due to maternal anesthetics, which crosses the placenta and inhibit release of catecholamines and cortisol (33,36,37). A limitation in our study is that we could not make a distinction between a primary caesarean delivery, usually planned due to previously known maternal indication, and a secondary caesarean delivery because of acute fetal or maternal distress.
Both low Apgar scores and low umbilical cord blood pH can be seen as measures of hypoxia and stress of the neonate, implying that the labor-associated stress hypothesis could also be applied to these parameters. The effects of Apgar scores and umbilical cord blood pH were mainly found on the major lymphocyte subset counts, and to a lesser extent on T-lymphocyte subset counts. The latter might be explained because all T lymphocyte subsets contributed to an increase of the total T lymphocytes. Studies on Apgar scores and effects on lymphocyte subset counts are very limited and showed that low 1-min and 5-min Apgar scores increase immunoglobulin secreting cell counts and proliferative responses of mononuclear cells in vitro (21,22). We found larger effect estimates of 5-min Apgar scores on lymphocyte subset counts than 1-min Apgar scores. Apgar scores 5 min after birth probably better reflect the condition of neonates. This is in line with a previous study, which observed associations of 5-min Apgar scores and mortality rates (38). Apgar scores at 1 and 5 min after birth are subjective scoring systems for the condition of the neonate. Our fully adjusted regression models confirms this subjectivity of the Apgar scores since the independent effect of these scores declined severely and the effects of umbilical cord blood pH, an objective method for hypoxia, remained on most of the major lymphocyte subsets. A previous study found an inverse association between the number of leukocytes and umbilical cord blood pH (9). In this study, the effects of cord blood pH on the various leukocyte subtypes were not explored. One study assessed the relation between umbilical cord blood pH and distribution of major lymphocyte subsets and found decreasing percentages of T lymphocytes and increasing percentages of NK lymphocytes with decreasing umbilical cord blood pH (20). Differences with our study might be explained due to their different study population of only vaginal delivered infants with mothers frequently receiving labor-inducing medication, spasmolytics, neuroplegic, and epidural analgesia (7 of 70 mothers received no medication). Unfortunately, data on perinatal medication were not available in our study. Another difference with our study might be that they used percentages of lymphocytes (T + B + NK = 100%) instead of absolute values of lymphocyte subsets. A low percentage of T lymphocytes automatically provides a high percentage of B or NK lymphocytes. Umbilical cord blood pH therefore might lead to an opposite effect on those lymphocytes. The use of percentages instead of absolute counts of the major lymphocyte subsets in our cohort confirms this hypothesis. An increase of 0.1-point in umbilical cord blood pH showed an increase of percentual T lymphocytes [regression coefficient (95% confidence interval): 5 (3–6)], a decrease of percentual B lymphocytes [−1 (−2, −0.6)] and a decrease of NK lymphocytes]−3 (−4, −2)]. For absolute counts of lymphocyte subsets, an increase of umbilical cord blood pH led to a decrease of all the major lymphocyte subsets (Table 3). Therefore, it is preferable to use absolute counts, instead of percentages of lymphocyte subsets, to reflect actual changes of lymphocyte subsets due to various factors.
Some methodologic issues should be considered. In our study, excluding participants with missing data would lead to selection biased results if the associations of stress-related perinatal factors with absolute numbers of lymphocyte subsets differ between participants with and without complete data. Of all participating singleton live births, information about mode of delivery was missing in only 5.3%. Of neonates with information of mode of delivery, neonates with missing data on lymphocyte subsets more often had a caesarean delivery than neonates with data on lymphocyte subsets. Therefore, it is likely that because of this selective group of missing outcomes the observed effects of mode of delivery with absolute numbers of lymphocyte subsets may be underestimated. However, caesarean delivery may be performed primary or secondary. Since the associations of primary and secondary caesarean deliveries with lymphocyte subsets counts are expected to be in the opposite direction, our effect estimates may be somewhat biased toward null. Our results are probably demonstrating the difference between primary caesarean delivery and vaginal delivery. We expect to have relatively more missing lymphocyte subset counts among neonates born after a secondary caesarean delivery due to logistical constraints in the acute setting.
Information about 1-min Apgar scores, 5-min Apgar scores, and umbilical cord blood pH was missing in 2.6%, 1.9%, and 50.8% of the neonates, respectively. Measurements of umbilical cord blood pH in the Netherlands is not routinely performed, since approximately one-third of the deliveries in the Netherlands is performed at home and are at low risk for obstetric complications (39). In line with this, we found that neonates without umbilical cord blood pH values more often were vaginally delivered and had higher 1- and 5-min Apgar scores. Neonates without umbilical cord blood pH are more frequently from uncomplicated pregnancies with fetal distress. Thus, we expect that missing values in umbilical cord blood pH did not materially change the effect estimated but decreased the power of the study.
In our cohort study, information about maternal fever, indicating an underlying infection, was only available around the third trimester of gestation. It did not materially change the effect estimates in the associations of stress-related perinatal factors with lymphocyte subsets. However, because of the time of maternal fever in pregnancy its confounding effect is probably underestimated since an acute ongoing maternal infection during delivery might show more increasing effects on the neonatal lymphocyte subsets.
In conclusion, this population-based cohort study showed that with increasing mode of delivery-associated stress lymphocyte subset counts (NK, memory T) increase. Furthermore, lower umbilical cord blood pH is associated with an increase of lymphocyte subset counts (B, NK, memory T). Therefore, the clinical interpretation of absolute numbers of lymphocyte subsets at birth should take the effects of stress- and hypoxia-related perinatal factors into account.
References
Motley D, Meyer MP, King RA, Naus GJ 1996 Determination of lymphocyte immunophenotypic values for normal full-term cord blood. Am J Clin Pathol 105: 38–43
Rabian-Herzog C, Lesage S, Gluckman E 1992 Characterization of lymphocyte subpopulations in cord blood. Bone Marrow Transplant 9: 64–67
Raes M, Alliet P, Gillis P, Zimmermann A, Kortleven J, Magerman K, Peeters V, Rummens JL 1993 Lymphocyte subpopulations in healthy newborn infants: comparison of cord blood values with values five days after birth. J Pediatr 123: 465–467
Stern DA, Hicks MJ, Martinez FD, Holberg CJ, Wright AL, Pinnas J, Halonen M, Taussig LM 1992 Lymphocyte subpopulation number and function in infancy. Dev Immunol 2: 175–179
Kotiranta-Ainamo A, Apajasalo M, Pohjavuori M, Rautonen N, Rautonen J 1999 Mononuclear cell subpopulations in preterm and full-term neonates: independent effects of gestational age, neonatal infection, maternal pre-eclampsia, maternal betamethason therapy, and mode of delivery. Clin Exp Immunol 115: 309–314
Cairo MS, Wagner EL, Fraser J, Cohen G, van de Ven C, Carter SL, Kernan NA, Kurtzberg J 2005 Characterization of banked umbilical cord blood hematopoietic progenitor cells and lymphocyte subsets and correlation with ethnicity, birth weight, sex, and type of delivery: a Cord Blood Transplantation (COBLT) Study report. Transfusion 45: 856–866
Chandra RK 1991 Interactions between early nutrition and the immune system. Ciba Found Symp 156: 77–89; discussion 89–92.
Moore SE 1998 Nutrition, immunity and the fetal and infant origins of disease hypothesis in developing countries. Proc Nutr Soc 57: 241–247
Nikischin W, Peter M, Oldigs HD 1997 The influence of mode of delivery on hematologic values in the umbilical vein. Gynecol Obstet Invest 43: 104–107
Pittard WB III, Schleich DM, Geddes KM, Sorensen RU 1989 Newborn lymphocyte subpopulations: the influence of labor. Am J Obstet Gynecol 160: 151–154
Lim FT, van Winsen L, Willemze R, Kanhai HH, Falkenburg JH 1994 Influence of delivery on numbers of leukocytes, leukocyte subpopulations, and hematopoietic progenitor cells in human umbilical cord blood. Blood Cells 20: 547–558; discussion 558–549.
Samelson R, Larkey DM, Amankwah KS, McConnachie P 1992 Effect of labor on lymphocyte subsets in full-term neonates. Am J Reprod Immunol 28: 71–73
Thilaganathan B, Meher-Homji N, Nicolaides KH 1994 Labor: an immunologically beneficial process for the neonate. Am J Obstet Gynecol 171: 1271–1272
Thornton CA, Capristo CC, Power LL, Holloway JA, Popplewell EJ, Diaper ND, Warner JO 2003 The effect of labor on neonatal T-cell phenotype and function. Pediatr Res 54: 120–124
Gasparoni A, Maccario R, Chirico G, Belloni C, Mingrat G, De Amici D, Bonora MR, Rondini G 1992 Neonatal B lymphocyte subpopulations and method of delivery. Biol Neonate 61: 137–141
Chirico G, Gasparoni A, Ciardelli L, Martinotti L, Rondini G 1999 Leukocyte counts in relation to the method of delivery during the first five days of life. Biol Neonate 75: 294–299
Vogl SE, Worda C, Egarter C, Bieglmayer C, Szekeres T, Huber J, Husslein P 2006 Mode of delivery is associated with maternal and fetal endocrine stress response. BJOG 113: 441–445
Ruth V, Hallman M, Laatikainen T 1993 Corticotropin-releasing hormone and cortisol in cord plasma in relation to gestational age, labor, and fetal distress. Am J Perinatol 10: 115–118
De Amici D, Gasparoni A, Chirico G, Ceriana P, Bartoli A, Ramajoli I, Moretta A 1999 Natural killer cell activity and delivery: possible influence of cortisol and anesthetic agents. A study on newborn cord blood. Biol Neonate 76: 348–354
Dostal M, Giguere Y, Fait T, Zivny J, Sram RJ 2001 The distribution of major lymphocyte subsets in cord blood is associated with its pH. Clin Biochem 34: 119–124
Pittard WB III, Miller KM, Sorensen RU 1985 Perinatal influences on in vitro B lymphocyte differentiation in human neonates. Pediatr Res 19: 655–658
Willwerth BM, Schaub B, Tantisira KG, Gold DR, Palmer LJ, Litonjua AA, Perkins DL, Schroeter C, Gibbons FK, Gillman MW, Weiss ST, Finn PW 2006 Prenatal, perinatal, and heritable influences on cord blood immune responses. Ann Allergy Asthma Immunol 96: 445–453
Hofman A, Jaddoe VW, Mackenbach JP, Moll HA, Snijders RF, Steegers EA, Verhulst FC, Witteman JC, Buller HA 2004 Growth, development and health from early fetal life until young adulthood: the Generation R Study. Paediatr Perinat Epidemiol 18: 61–72
Jaddoe VW, Mackenbach JP, Moll HA, Steegers EA, Tiemeier H, Verhulst FC, Witteman JC, Hofman A 2006 The Generation R Study: design and cohort profile. Eur J Epidemiol 21: 475–484
Apgar V 1953 A proposal for a new method of evaluation of the newborn infant. Curr Res Anesth Analg 32: 260–267
Apgar V, Holaday DA, James LS, Weisbrot IM, Berrien C 1958 Evaluation of the newborn infant; second report. J Am Med Assoc 168: 1985–1988
de Vries E, de Bruin-Versteeg S, Comans-Bitter WM, de Groot R, Boerma GJ, Lotgering FK, van Dongen JJ 1999 Correction for erythroid cell contamination in microassay for immunophenotyping of neonatal lymphocytes. Arch Dis Child Fetal Neonatal Ed 80: F226–F229
Brando B, Gohde W Jr, Scarpati B, D'Avanzo G, European Working Group on Clinical Cell Analysis 2001 The “vanishing counting bead” phenomenon: effect on absolute CD34+ cell counting in phosphate-buffered saline-diluted leukapheresis samples. Cytometry 43: 154–160
van Lochem EG, van der Velden VH, Wind HK, te Marvelde JG, Westerdaal NA, van Dongen JJ 2004 Immunophenotypic differentiation patterns of normal hematopoiesis in human bone marrow: reference patterns for age-related changes and disease-induced shifts. Cytometry B Clin Cytom 60: 1–13
Lambert C, Cristina I, Christian G 2006 Enumeration of peripheral lymphocyte subsets using 6 vs. 4 color staining: a clinical evaluation of a new flowcytometer. Cytometry B Clin Cytom 70: 29–38
Jaddoe VW, Verburg BO, de Ridder MA, Hofman A, Mackenbach JP, Moll HA, Steegers EA, Witteman JC 2007 Maternal smoking and fetal growth characteristics in different periods of pregnancy: the generation R study. Am J Epidemiol 165: 1207–1215
Cole TJ 2000 Sympercents: symmetric percentage differences on the 100 log(e) scale simplify the presentation of log transformed data. Stat Med 19: 3109–3125
Irestedt L, Lagercrantz H, Hjemdahl P, Hagnevik K, Belfrage P 1982 Fetal and maternal plasma catecholamine levels at elective cesarean section under general or epidural anesthesia versus vaginal delivery. Am J Obstet Gynecol 142: 1004–1010
Jones CM III, Greiss FC Jr 1982 The effect of labor on maternal and fetal circulating catecholamines. Am J Obstet Gynecol 144: 149–153
Jouppila R, Puolakka J, Kauppila A, Vuori J 1984 Maternal and umbilical cord plasma noradrenaline concentrations during labour with and without segmental extradural analgesia, and during caesarean section. Br J Anaesth 56: 251–255
Gasparoni A, Ciardelli L, De Amici D, Castellazzi AM, Autelli M, Bottino R, Polito E, Bartoli A, Rondini G, Chirico G 2002 Effect of general and epidural anaesthesia on thyroid hormones and immunity in neonates. Paediatr Anaesth 12: 59–64
Marx GF 1995 Evaluation of stress during labor and parturition. Am J Obstet Gynecol 172: 1948
Casey BM, McIntire DD, Leveno KJ 2001 The continuing value of the Apgar score for the assessment of newborn infants. N Engl J Med 344: 467–471
Anthony S, Buitendijk SE, Offerhaus PM, Dommelen P, Pal-de Bruin KM 2005 Maternal factors and the probability of a planned home birth. BJOG 112: 748–753
Acknowledgements
The Generation R Study is conducted by the Erasmus Medical Center, Rotterdam, in close collaboration with the School of Law and Faculty of Social Sciences of the Erasmus University Rotterdam, the Municipal Health Service Rotterdam area, the Rotterdam Homecare Foundation and the Stichting Trombosedienst & Artsenlaboratorium Rijnmond (STAR), Rotterdam. We gratefully acknowledge the contribution of general practitioners, hospitals, midwives, and pharmacies in Rotterdam. We thank Romana S. Jugooa, Jac H.S.A.M. Kuijpers-Entrup, Marja A.W. Smits-Te Nijenhuis, Ivonne J. Bronmans-Smits, and Anja X. de Jong of the Immunology Department of the Erasmus Medical Center, Rotterdam, for performing the flow-cytometric analyses.
Author information
Authors and Affiliations
Corresponding author
Additional information
The first phase of the Generation R Study was made possible by financial support from the Erasmus Medical Center, Rotterdam, the Erasmus University Rotterdam and the Netherlands Organization for Health Research and Development (Zon Mw). The present study was supported by an additional grant from Stichting W.H. Kröger, Rotterdam (Grant No. 00-048), and AGS Kinderstichting.
Rights and permissions
About this article
Cite this article
Duijts, L., Bakker-Jonges, L., Labout, J. et al. Perinatal Stress Influences Lymphocyte Subset Counts in Neonates. The Generation R Study. Pediatr Res 63, 292–298 (2008). https://doi.org/10.1203/PDR.0b013e318163a29f
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e318163a29f
This article is cited by
-
Increased mortality in infants with abnormal T-cell receptor excision circles
Pediatric Research (2024)
-
The impact of cesarean delivery on infant DNA methylation
BMC Pregnancy and Childbirth (2021)
-
The Generation R Study: Biobank update 2015
European Journal of Epidemiology (2014)
-
The Generation R Study: design and cohort update 2012
European Journal of Epidemiology (2012)
-
The Generation R Study: design and cohort update 2010
European Journal of Epidemiology (2010)