Abstract
The role of oxidative stress in the pathogenesis of liver disease in Wilson disease (WD), a genetic disorder characterized by excess hepatic deposition of copper that generates free radicals, remains unclear. This study investigates oxidative stress on the liver and hepatic antioxidant responses in WD using liver specimens from affected patients showing mild liver damage (group I, n = 3), moderate or greater liver damage (group II, n = 5), and fulminant hepatic failure (group III, n = 5) and from asymptomatic carriers (n = 2). Decreased ratios of reduced glutathione (GSH) to oxidized glutathione (GSSG) and increased thiobarbituric acid reactive substance (TBARS), a lipid peroxidation product, were found in every affected patient, especially in group II and III patients. Activities and protein expressions of Mn-dependent superoxide dismutase (Mn-SOD), CuZn-dependent superoxide dismutase (CuZn-SOD), and catalase were decreased in all patients, especially in group III patients. Glutathione peroxidase (GPx) activity was decreased only in group III patients. Asymptomatic carriers without any clinical manifestations showed normal TBARS level and GSH/GSSG ratio with increases in both GSH and GSSG levels. Their CuZn-SOD, Mn-SOD, and catalase activities were increased. These results suggest that excessive copper-derived oxidants contribute to development and progression of liver disease in WD.
Similar content being viewed by others
Main
WD is an autosomal recessive disorder. The gene responsible for it is ATP7B, which encodes a copper transporting P-type ATPase (1). In this disorder, copper transport from hepatocytes to bile flow and incorporation of copper into ceruloplasmin are impaired. Consequently, excess copper accumulates in various organs, particularly the liver and brain, resulting in various clinical manifestations (2,3).
Many previous reports have described hepatic presentations in WD precisely (2–6). However, the mechanisms of copper hepatotoxicity remain unclear. It has been proposed that free radical generation by excess copper and the subsequent oxidative changes in hepatocyte organellar lipids and thiol-containing proteins account for the development and progression of liver disease (7–9). Several experiments using HepG2 cells have shown that proteins involved in antioxidant defenses in this cell line are altered dramatically by chronic copper exposure (10,11). However, in humans, the magnitude of copper-derived oxidative stress and the state of antioxidant defense system in the liver have not been elucidated sufficiently (12–15). Recently, oxidative stress and antioxidant defense systems in various liver diseases have been studied extensively, especially those in nonalcoholic fatty liver. The deep associations of oxidative stress with inflammation, fibrosis, and apoptosis of hepatic tissues have been shown (16–19).
The present study evaluated the magnitude of oxidative stress in the livers of patients with WD with various liver manifestations and those of carriers without any clinical manifestations. Enzymes acting against oxidative stress, including Mn-SOD, CuZn-SOD, GPx, and catalase, were also examined (20–22).
This report presents a description of the considerable differences in the magnitude of hepatic oxidative stress load and hepatic antioxidant responses in patients with WD, according to the severity of liver damage. The critical role of oxidative stress in the development and progression of liver disease in WD is discussed.
SUBJECTS AND METHODS
Subjects.
This study enrolled 13 patients (five males and eight females) with WD aged 3–14 y; they all had presented with liver dysfunction, but none with neuropsychological manifestations. The diagnosis of WD was made using clinical presentations, serum ceruloplasmin level, liver histology, and copper contents of the liver at 2–7 mo after they were found to have liver dysfunction (Tables 1 and 2). In addition, analyses of the ATP7B gene, a gene that is responsible for WD, were performed for nine of the patients.
Patients were classified into three groups, I, II, and III, according to their respective clinical manifestations, liver functions, and liver histologic results (Tables 1 and 2). As a histologic estimation of liver injury, the stage and grade scores, which respectively reflect the fibrosis and inflammatory activity of the liver, were determined according to the well-established METAVIR scoring system of stages F0–F4 and of grades A0–A3 (23).
Liver dysfunctions of three patients in group I (I-1, I-2, and I-3), who were the youngest, were mild, and their liver histology showed little fibrosis and mild infiltrations of inflammatory cells in portal areas, compatible with the findings of early-stage liver disease (stage F1; grade A1). In addition, periportal glycogen-filled swollen nuclei and microvesicular steatosis, which are characteristic histologic findings of WD, were observed (2–4). Immediately after confirmation of the diagnosis, they received trientine, a chelating agent, with a dose of 40–50 mg/kg/d.
On the other hand, liver histology of five patients in group II (II-1, II-2, II-3, II-4, and II-5) showed fibrosis stretching to neighboring portal areas (stage F2–F3), and infiltrations of inflammatory cells spilling over into the lobule from the portal area (grade A2–A3). Those findings were compatible with those of moderate or more severe liver damage. Furthermore, mild or more severe steatosis was observed. Their liver dysfunctions were moderate or more severe, supporting the histologic findings. After the diagnosis, they were also administered with chelating agents (20–30 mg/kg/d d-penicillamine or 40–50 mg/kg/d trientine).
Clinical presentations of the five patients in group III (III-1, III-2, III-3, III-4, and III-5) were compatible with those of fulminant hepatic failure (FHF) (3,5). Characteristic findings were obtained for them: profoundly prolonged prothrombin time, mild or moderate elevation of serum transaminase level, prominent hyperbilirubinemia, and hemolysis. Liver histology results indicated massive necrosis and ballooning of hepatocytes with severe or moderate fibrosis, corresponding to grade F2–F4 and stage A3. Furthermore, Mallory body formation in hepatocytes was observed in two of five patients. All patients received trientine 40–50 mg/kg/d, but their liver dysfunctions deteriorated to liver failure. They underwent liver transplantation from living related donors (mother or father) within a few months of the onset of hepatic presentation.
The copper content of liver from every affected patient was extremely high. Among the three groups, the hepatic copper contents of groups II and III were considerably higher than that of group I (Table 1). All patients, especially patients of groups I and II, had low serum ceruloplasmin level (Table 2).
Two related donors (H-1, father of III-2; H-2, father of III-3) without obesity and smoking history were also enrolled in this study. They were confirmed to be heterozygote for ATP7B mutations. Their serum ceruloplasmin levels were below the normal range but were higher than those of patients. Copper contents of their livers were overtly high, compared with those of control livers but were considerably lower than those of patients. Their liver functions and histology were entirely normal (Tables 1 and 2).
Fragments of livers were obtained from 12 nonrelated donors for liver transplantation (nine males and three females) with ages of 28–42 y and were used as controls; they were entirely healthy and had no history of smoking.
This study was approved by an institutional review board, and parents of all patients provided written informed consent before the start of this study.
Study design.
Percutaneous liver biopsy was performed for eight patients in groups I and II before the start of medication with chelating agents; the copper contents of liver as well as liver histology were examined. The remaining liver samples were preserved at −80°C until the following analyses were made. Liver samples of five patients of group III (recipients) and two carriers (donors) were those from excised livers.
Oxidative stress parameters in liver homogenates were examined. Reduced GSH and GSSG concentrations in liver homogenate were determined and the ratio of GSH to GSSG was calculated to evaluate the redox state in the liver. TBARS, a lipid peroxidation product, was also examined (24,25).
To assess hepatic antioxidant enzymatic function, CuZn-SOD, Mn-SOD, GPx, and catalase activities were examined. Furthermore, protein expressions of CuZn-SOD, Mn-SOD, and catalase in the liver were examined.
Determination of serum ceruloplasmin level.
The serum ceruloplasmin level was determined by a routine procedure using nephelometry.
Determination of copper content in the liver.
The copper content in the liver copper was determined using atomic emission spectroscopy with an ICP emission spectrometer (JY38P; Jobin Yvon Instruments, SA) and expressed as micrograms per gram of dry weight.
Quantification of GSH and GSSG.
Each liver sample was homogenized and sonicated in 10 mmol/L phosphate buffer of pH 7.80. After precipitation of proteins with perchloric acid/ethylenediamine tetraacetic acid (EDTA) and centrifugation at 8000 × g for 2 min, the resultant supernatant was adjusted to pH 5–6 and was further centrifuged at 12,000 × g for 5 min.
The amount of total glutathione (GSH + GSSG) in the supernatant was determined according to the method described by Summer and Eisenburg (13) and Tietze (26). In brief, the supernatant was dissolved in phosphate-EDTA buffer, pH 7.5 and was then added to a solution containing 5,5′-dithibis[2-nitrobenzoic] acid (DTNB) and glutathione reductase. GSH-dependent DTNB reduction initiated by an addition of triphosphopyridine nucleotide was monitored with spectrophotometer at 412 nm (Shimazu UV-160); the final volume (1 mL) of this reaction mixture contained 0.6 μmol DTNB, 1 U glutathione reductase, and 0.2 μmol triphosphopyridine nucleotide. It was confirmed by experiments using control liver samples that the determination of glutathione concentration using this assay was not influenced by the addition of copper.
GSSG in the supernatant was determined according to the method described by Summer and Eisenburg (13) and Sies and Summer (27). In brief, GSSG-dependent NADH reduction initiated by the addition of 0.6 U glutathione reductase to 1 mL of the mixture containing 20 mmol/L triethanolamine and 5 μmol/L NADPH was monitored with spectrometer at 340 nm (Hitachi 181).
Thiobarbituric acid–reactive substances.
The concentration of thiobarbituric acid–reactive substances in the liver, which was homogenated and sonicated as above, was determined using fluorometric assay according to the method described previously (24,28).
Enzyme activities.
Frozen liver samples were homogenized in 10 mmol/L phosphate buffer pH 7.80 containing 1 mmol/L EDTA; they were then sonicated for 1 min with icing. Total-SOD activity was measured at pH 7.8 using a commercial kit according to the method described by McCord and Fridovich (29). The CuZn-SOD activity was measured at pH 10.2 using the same kit. The Mn-SOD activity was calculated using subtraction of CuZn-SOD from the total SOD. The GPx activity was measured using a commercial kit according to the method described by Paglia and Valentine (30). Catalase activity was measured by a spectrophotometric method using H2O2 as a substrate (11).
Immunoblotting.
Frozen liver samples (100 mg) were homogenized in 1 mL lysis buffer containing 10 mmol/L Tris-HCl, 200 mmol/L NaCl, 1 mmol/L EDTA, 5% glycerol, and 5 mmol/L 2-mercaptoethanol, 1 mmol/L MgCl2, and 0.5 mmol/L phenylmethylsulfonyl fluoride, a protease inhibitor. After centrifugation at 1500 × g for 1 min, the protein concentration in the supernatant was determined using Bradford reagent (Sigma Chemical Co.) The supernatant was boiled in an equal volume of loading buffer containing 125 mmol/L Tris-HCl, pH 6.8, 4% sodium dodecylsulfate (SDS), 20% glycerol, and 10% 2-mercaptoethanol; it was then applied to 10% SDS-polyacrylamide gel electrophoresis. After electrophoresis, the separated proteins were transferred electronically to nitrocellulose membranes (Millipore Corp., Tokyo, Japan). The membranes were blocked with 10% nonfat dried milk in Tris phosphate–buffered saline. They were then reacted with sheep anti-CuZn-SOD or sheep anti–Mn-SOD antibody (The Binding Site Ltd., Birmingham, UK), or a rabbit anti–catalase antibody (Calbiochem-Bering Corp., San Diego, CA) (31). After washing the membranes, appropriate secondary anti–animal IgG antibodies conjugated with peroxidase (The Binding Site Ltd.) were mounted on the membranes for 1 h. The membranes were washed and incubated in enhanced chemiluminescence reagents (ECL, Ashermann, Buckinghamshire, UK), and exposed to chemiluminescence film according to the manufacturer's instructions. Quantification of the bands was performed using an ultrascan laser densitometer (LKB 2202; Pharmacia LKB, Uppsala, Sweden) and expressed as the ratios of the respective protein expressions to β-actin expression that was visualized with a mouse anti–β-actin antibody (Sigma Chemical Co.–Aldrich Inc, St. Louis, MO).
RESULTS
Table 3 shows that both GSH and GSSG concentrations in the two carriers were apparently higher than the respective control levels, but the GSSG/GSH ratio was at the control level. In group I, on the other hand, the GSSG concentration was high, whereas GSH concentrations were within the normal range, resulting in a GSH/GSSG ratio that was lower than those in the controls. In group II, the GSSG concentration was as high as that in group I, whereas GSH concentrations were apparently below the normal range, rendering the GSH/GSSG ratio much lower than the control level. In group III, GSSG concentration showed a level at around the upper limit of the normal range, but the GSH concentration exhibited an extremely low value, engendering an extremely low GSSH/GSH ratio.
The TBARS concentrations in the carriers were within the control range (Table 3). The TBARS concentration in group I was higher than the control level. Those of groups II and III were extremely high.
Table 4 shows activities of enzymes involved in the hepatic antioxidant defense system. CuZn-SOD, Mn-SOD, and catalase activities in carriers were substantially increased, whereas those in groups I, II, and III were decreased. The decreases in CuZn-SOD, Mn-SOD, and catalase activities in group III were especially marked. On the other hand, the GPx activity was lower only in group III. Those in the other two groups and carriers were maintained at the control level.
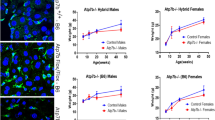
Figure 1A and B represents, respectively, immunoblotting patterns of enzymes and their relative densitometric intensity. Protein expression levels of CuZn-SOD, Mn-SOD, and catalase in carriers were slightly higher than those of the controls, whereas those in affected patients were apparently low. In particular, low CuZn-SOD, Mn-SOD, and catalase levels in group III were remarkable. These findings are consistent with the results of enzyme activity shown in Table 4.
Western blot analyses of CuZn-SOD (•), Mn-SOD (○), and catalase (▵) in the liver. (A) The Western blot pattern. (B) The relative intensity of respective enzyme bands as calculated against β-actin band. Cont, healthy controls; II-1–II-5 (n = 5), patients in group II presenting with moderate or more severe liver damage; I-1–I-3 (n = 3), patients in group I presenting with mild liver damage; III-1–III-5 (n = 5), patients in group III manifesting fulminant hepatic failure; H-1 and H-2, heterozygous carriers
DISCUSSION
Development and subsequent progression of liver disease in WD are inferred to result from copper accumulation in hepatocytes beyond the toxic level (1–6). However, the mechanisms through which the copper accumulation causes liver injury have never been studied thoroughly. Recent studies have raised the possibility that oxidative stress contributes to inflammation, fibrosis, and apoptosis of hepatic tissues (10,16–19). In particular, the contribution of oxidative stress as the secondary impact to the development of nonalcoholic hepatosteatosis has been described (16,17).
Copper generates free radicals. It is therefore likely that oxidative stress accounts for the development and progression of liver damage in WD (7,8). However, limited data are available regarding oxidative stress by copper deposition in the human liver and resultant changes in hepatic antioxidant defense system. Several studies have suggested that copper-generated free radicals cause oxidative changes in hepatocyte organellar lipids and thiol-containing proteins, engendering hepatocyte dysfunction or injury (3,9,10,13). In addition, it has been shown that a sudden onset of fulminant hepatic failure in patients with WD results from the massive apoptosis of hepatocytes attributable to extraordinarily intense oxidant stress loads (3,10).
This study showed that TBARS, a lipid peroxidation product, in liver tissues manifesting mild damage (group I) was substantially high. Those manifesting moderate or more severe liver damage (groups II and III) exhibited considerably higher values than did control livers. These results provided strong evidence that lipid peroxidation actually took place in the livers of patients with WD and greatly contributed to the development and progression of liver damage in WD. On the other hand, in asymptomatic carriers, although their hepatic copper contents were more than four times higher than those of the controls, the hepatic TBARS concentrations were almost at the control levels, indicating that the copper-derived oxidative stress might be suppressed by certain antioxidant defense systems. Increased GSH concentrations detected in their livers would participate in the maintenance of a normal TBARS level.
Low GSH concentration, together with high GSSG concentration, was observed in the livers of patients with WD, suggesting the substantial alteration of a redox state in their livers. In particular, decreases in GSH concentration were prominent in patients with mild or more severe liver damage (group II) and with fulminant hepatic failure (group III). An increment of GSSG efflux from hepatocytes to bile during oxidative stress has been suggested by results of experiments using animals, but GSH production and the GSH-GSSG recycling system, including enzymes such as glutathione synthetase, glutathione reductase, and GPx in the liver, has not been fully elucidated (32,33). The GSH depletion found in our patients might be explained to result from consumption of GSH due to the intense oxidative stress and/or decreased hepatic GSH production, although those causes were not confirmed by the results of this study.
For maintenance of the cellular reducing environment, GSH is known to be important (34,35). Furthermore, recent studies have shown that GSH is involved in the intracellular processing of copper (36–38). In this context, GSH depletion should render hepatocytes more susceptible to undergoing copper-induced cytotoxicity.
Numerous enzymes are involved in the antioxidative defense system. In particular, coordinated actions of CuZn-SOD, Mn-SOD, catalase, and GPx against oxidant stress have been well established (20–22). The sequential elimination of superoxide radical and hydrogen peroxide by synergistic action of SODs, catalase, and GPx prevents the formation of hydroxyl radical, which exhibits an extremely toxic action. It has been shown that oxidative stress itself upregulates activities of such antioxidative enzymes; at advanced stages of liver disease, such enzymes are downregulated (12,39). Substantially high activities of CuZn-SOD, Mn-SOD, and catalase in the liver of carriers would be the cases representing such the enzyme upregulation. On the other hand, activities and protein expressions of CuZn-SOD, Mn-SOD, and catalase in group I patients manifesting mild liver damage were substantially decreased. These decreased enzyme activities would also accelerate oxidant-triggered liver injury. In particular, a decreased activity of Mn-SOD, which is localized in mitochondria and counteracts oxidant stress, might participate in mitochondrial damage leading to cell apoptosis. The reason for the decreases in activities and expression levels of such enzymes in patients at advanced stage (groups II and III) could be explained as a result of severe liver damage, but such an explanation could not be applied to patients at early stage (group I). There remains a possibility that enzyme activities in the latter patients are inherently low. In contrast, GPx activity remained at normal levels, even in patients showing moderate or more severe liver damage. Levels of GPx were decreased only in patients manifesting FHF, possibly reflecting the low protein synthesis caused by a profoundly damaged liver. Nevertheless, GPx apparently behaved rather independently from other antioxidant enzymes in patients with WD. The GPx catalyzes the reduction of hydrogen peroxide, organic hydroperoxide, and lipid peroxides through the conversion of GSH to GSSG and thereby plays a crucial role in the protection of cells against oxidative damage. In this context, it can be assumed that induction of GPx is upregulated under the oxidative stress and maintained until the liver is severely damaged.
Unlike WD with hepatic presentation, the liver of asymptomatic carriers showed substantially high activities of CuZn-SOD, Mn-SOD, and catalase. These results allowed us to assume that, aside from an increase in GSH production, increases of such enzymes also contribute to the attenuation of copper-derived oxidant stress.
This study described the great differences in hepatic antioxidative systems between asymptomatic carriers and patients with WD. These results suggest that an appropriate antioxidative therapy is useful in treatment of patients with WD. In particular, glutathione augmentation using GSH precursors such as N-acetyl cysteine and γ-glutamyl cysteine is expected to exert an inhibitory effect on the progression of liver disease (40).
Abbreviations
- CuZn-SOD:
-
CuZn-dependent superoxide dismutase
- GSH:
-
reduced glutathione
- GSSG:
-
oxidized glutathione
- Mn-SOD:
-
Mn-dependent superoxide dismutase
- TBARS:
-
thiobarbituric acid reactive substance
- WD:
-
Wilson disease
References
Tanzi RE, Petrukhin K, Chernov I, Pellequer JL, Wasco W, Rass B, Romano DM, Parano E, Pavone L, Brzustowicz LM 1993 The Wilson disease gene is a copper transporting ATPase with homology to the Menkes disease gene. Nat Genet 5: 344–350
Scheinberg IH, Sternlieb I 1984 Wilson disease. In: Smith LH (ed) Major Problems in Internal Medicine. Saunders, Philadelphia, pp 1–179
Sokol RJ, Narkewicz MR 2001 Copper and iron disorders. In: Suchy FJ, Sokol RJ, Balistreli WF (eds) Liver Disease in Children. Lippincott Williams & Wilkins, Philadelphia, pp 595–640
Anderson PJ, Popper H 1960 Change in hepatic structure in Wilson's disease. Am J Pathol 36: 483–497
Berman DH, Leventhal RI, Gavaler JS, Cadoff EM, Van Thiel DH 1991 Clinical differentiation of fulminant Wilsonian hepatitis from other causes of hepatic failure. Gastroenterology 100: 1129–1134
Schilsky ML, Scheinberg IH, Sternlieb I 1991 Prognosis of Wilsonian chronic active hepatitis. Gastroenterology 100: 762–767
Aust SD, Morehouse LA, Thomas CE 1985 Role of metal in oxygen radical reactions. J Free Radic Biol Med 1: 3–25
Hochstein P, Kumar KS, Forman SJ 1980 Lipid peroxidation and the cytotoxicity of copper. Ann N Y Acad Sci 355: 240–248
Sokol RJ, Twedt D, McKim JM Jr, Devereaux MW, Karrer FM, Kam I, von Steigman G, Narkewicz MR, Bacon BR, Britton RS 1994 Oxidant injury to hepatic mitochondria in patients with Wilson's disease and Bedlington terriers with copper toxicosis. Gastroenterology 107: 1788–1798
Strand S, Hofman WJ, Grambihler A, Hug H, Volkmann M, Otto G, Wesch H, Mariani SM, Hack V, Stremmel W, Krammer PH, Galle PR 1998 Hepatic failure and liver cell damage in acute Wilson's disease involve CD95(APO-1/Fas) mediated apoptosis. Nat Med 4: 588–593
Jimenez I, Aracena P, Letelier ME, Navarro P, Speisky H 2002 Chronic exposure of HepG2 cells to excess copper results in depletion of glutathione and induction of metallothionein. Toxicol In Vitro 16: 167–175
Perlemuter G, Davit-Spraul A, Cosson C, Conti M, Bigorgne A, Paradis V, Corre MP, Prat L, Kuoch V, Basdevant A, Pelletier G, Oppert JM, Buffet C 2005 Increase in liver antioxidant enzyme activities in non-alcoholic fatty liver disease. Liver Int 25: 946–953
Summer KH, Eisenburg J 1985 Low content of hepatic reduced glutathione in patients with Wilson's disease. Biochem Med 34: 107–111
Ogihara H, Ogihara T, Miki M, Yasuda H, Mino M 1995 Plasma copper and antioxidant status in Wilson's disease. Pediatr Res 37: 219–226
von Herbay A, de Groot H, Hegi U, Stremmel W, Strohmeyer G, Sies H 1994 Low vitamin E content in plasma of patients with alcoholic liver disease, hemochromatosis and Wilson's disease. J Hepatol 20: 41–46
Angulo P 2002 Nonalcoholic fatty liver disease. N Engl J Med 346: 1221–1231
Matteoni CA, Younossi ZM, Gramlich T, Boparai N, Liu YC, McCullough AJ 1999 Nonalcoholic fatty liver disease: a spectrum of clinical and pathological severity. Gastroenterology 116: 1413–1419
Reid AE 2001 Nonalcoholic steatohepatitis. Gastroenterology 121: 710–723
Okuda M, Li K, Beard MR, Showalter LA, Sholle F, Lemon SM, Weinman SA 2002 Mitochondrial injury, oxidative stress, and antioxidant gene expression are induced by hepatitis C core protein. Gastroenterology 122: 366–375
Tribble DL, Aw TY, Jones DP 1987 The pathological significance of lipid peroxidation in oxidative cell injury. Hepatology 7: 377–386
Sies H 1993 Strategies of antioxidant defense. Eur J Biochem 215: 213–219
Fridovich I 1989 Superoxide dismutases. An adaptation to a paramagnetic gas. J Biol Chem 264: 7761–7764
Bedossa P, Poynard T 1996 An algorithm for the grading of activity in chronic hepatitis C. The METAVIR Cooperative Study Group. Hepatology 24: 289–293
Gutteridge JM, Halliwell B 1990 The measurement and mechanism of lipid peroxidation in biological systems. Trends Biochem Sci 129–135
Bando I, Reus MI, Andres D, Cascales M 2005 Endogenous antioxidant defense system in rat liver following mercury chloride oral intoxication. J Biochem Mol Toxicol 19: 154–161
Tietze F 1969 Enzymic method for quantitative determination of nanogram amounts of total and oxidized glutathione: applications to mammalian blood and other tissues. Anal Biochem 27: 502–522
Sies H, Summer KH 1975 Hydroperoxide-metabolizing systems in rat liver. Eur J Biochem 57: 503–512
Niehaus WG, Samuelson JR, Will ED 1969 Lipid peroxide formation in microsomes. Biochem J 113: 315–341
McCord JM, Fridovich I 1969 Superoxide dismutase. An enzymic function for erythrocuprein (hemocuprein). J Biol Chem 244: 6049–6055
Paglia DE, Valentine WN 1967 Studies on the quantitative and qualitative characterization of erythrocyte glutathione peroxidase. J Lab Clin Med 70: 158–169
Inoue I, Noji S, Awata T, Takahashi K, Nakajima T, Sonoda M, Komoda T, Katayama S 1998 Bezafibrate has an antioxidant effect: peroxisome proliferator-activated receptor alpha is associated with Cu2+, Zn2+-superoxide dismutase in the liver. Life Sci 63: 135–144
Akerboom TP, Bilzer H, Sies H 1982 The relationship of biliary glutathione disulfide efflux and intracellular glutathione disulfide content in perfused rat liver. J Biol Chem 257: 4248–4252
Gedik N, Kabasakal L, Sehirli O, Ercan F, Sirvanci S, Keyser-Uysal M, Sener G 2005 Long-term administration of aqueous garlic extract (AGE) alleviates liver fibrosis and oxidative damage induced by biliary obstruction in rats. Life Sci 76: 2593–2606
Griffith OW 1999 Biologic and pharmacologic regulation of mammalian glutathion synthesis. Free Radic Biol Med 27: 922–935
Sies H 1999 Glutathione and its role in cellular functions. Free Radic Biol Med 27: 916–921
Freedman JH, Ciriolo MR, Peisach J 1989 The role of glutathione in copper metabolism and toxicity. J Biol Chem 264: 5598–5605
Freedman JH, Peisach J 1989 Intracellular copper transport in cultured hepatome cells. Biochem Biophys Res Commun 164: 134–140
Jimenez I, Speisky H 2000 Effects of copper ions on the free radical-scavenging properties of reduced glutathione: implication of a complex formation. J Trace Elem Med Biol 14: 161–167
Sreekumar R, Rosado B, Rasmussen D, Charlton M 2003 Hepatic gene expression in historically progressive nonalcoholic hepatosteatitis. Hepatology 38: 244–251
Anderson ME, Luo JL 1998 Glutathione therapy: from prodrug and gene. Semin Liver Dis 18: 415–424
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nagasaka, H., Inoue, I., Inui, A. et al. Relationship Between Oxidative Stress and Antioxidant Systems in the Liver of Patients With Wilson Disease: Hepatic Manifestation in Wilson Disease as a Consequence of Augmented Oxidative Stress. Pediatr Res 60, 472–477 (2006). https://doi.org/10.1203/01.pdr.0000238341.12229.d3
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000238341.12229.d3
This article is cited by
-
Antioxidant Capacity Is Decreased in Wilson’s Disease and Correlates to Liver Function
Biological Trace Element Research (2023)
-
Neuropsychiatric Manifestations of Wilson Disease: Correlation with MRI and Glutamate Excitotoxicity
Molecular Neurobiology (2021)
-
Movement Disorder in Copper Toxicity Rat Model: Role of Inflammation and Apoptosis in the Corpus Striatum
Neurotoxicity Research (2020)
-
Metabolomics profiles of patients with Wilson disease reveal a distinct metabolic signature
Metabolomics (2019)
-
The adjuvant value of Herba Cistanches when used in combination with statin in murine models
Scientific Reports (2017)