Abstract
Glutaryl-CoA dehydrogenase deficiency is a neurometabolic disorder with a specific age- and region-dependent neuropathology. Between 6 and 18 mo of age, unspecific illnesses trigger acute encephalopathic crises resulting in acute striatal and cortical necrosis. We hypothesized that acute brain damage in glutaryl-CoA dehydrogenase deficiency is caused by the main pathologic metabolites 3-hydroxyglutaric and glutaric acids through an excitotoxic sequence. Therefore, we investigated the effect of 3-hydroxyglutaric acid and glutaric acid on primary neuronal cultures from chick embryo telencephalons and mixed neuronal and glial cell cultures from neonatal rat hippocampi. Exposure to glutaric acid and 3-hydroxyglutaric acid decreased cell viability in a concentration- and time-dependent fashion. This neurotoxic effect could be totally prevented by preincubation with an N-methyl-d-aspartate receptor subunit 2B (NR2B)-specific antagonist, NR2B antibodies, and an unspecific N-methyl-d-aspartate receptor blocker and was partially blocked with an NR2A-specific antagonist but not with NR2A antibodies or α-amino-3-hydroxy-5-methyl-4-isoxazole propionate receptor and metabotropic glutamate receptor antagonists. Furthermore, metabolite toxicity increased in parallel with the increasing expression of the NR2B subunit on cultured neurons from second to sixth day in vitro. We conclude from these results that 3-hydroxyglutaric acid and glutaric acid act as false neurotransmitters, in particular through NR1/2B, and that the extent of induced neurotoxicity is dependent on the temporal and spatial expression of NR1/2B in the CNS during maturation. Beyond favorable implications for treatment and long-term prognosis, glutaryl-CoA dehydrogenase deficiency is the first neurologic disease in which specific neuropathology could be experimentally linked to ontogenetic expression of a particular neurotransmitter receptor subtype.
Similar content being viewed by others
Main
GDD (synonym, glutaric aciduria type I; McKusick 231670 (ref.1) is an autosomal recessive neurometabolic disease first described in 1975 (1a), resulting in a distinct encephalopathy (2). The deficiency of the mitochondrial enzyme glutaryl-CoA dehydrogenase (EC 1.3.99.7) in the catabolic pathway of lysine, hydroxylysine, and tryptophan causes an accumulation of GA, 3-OH-GA, and glutaconic acids in body fluids as well as in brain tissue of affected patients (3, 4). Typically, between 6 and 18 mo of age, unspecific illnesses trigger encephalitis-like encephalopathic crises, leading to an irreversible destruction of certain brain areas (striatum, frontotemporal cortex) and consequently to a severe dystonic-dyskinetic disorder (2, 5). The risk of severe brain damage declines with age: no acute encephalopathic crises have been reported in children with GDD who had survived the first 5–6 y unharmed. The mechanism of the age-specific destruction of specific cerebral structures in GDD has been the subject of intense debates and different hypotheses (6, 7). Substantial evidence points to an excitotoxic sequence. Both GA and 3-OH-GA exhibit structural similarities to the excitotoxic amino acid glutamate. Post mortem examination of the basal ganglia and cortex in patients with GDD has revealed postsynaptic vacuolation similar to that of glutamate-mediated damage (3). A previous study using corticostriatal and hippocampal slice cultures in vitro, however, failed to reveal pathogenetic effects of GA, 3-OH-GA, or glutaconic acid at concentrations encountered in GDD but only reported neurotoxicity of 3-OH-GA at high concentrations (>1.5 mM), which was interpreted as a nonspecific effect by the authors (8). In contrast to this, preliminary experimental data from our group pointed to the ability of both 3-OH-GA and GA to act as neurotoxins (9).
Excitotoxicity is transmitted primarily through inotropic glutamate receptors, of which NMDA receptors are of particular importance. NMDA receptors consist of a Na+, K+, and Ca2+ ion channel formed by assembly of the obligatory NR1 subunit and any one of four modulatory NR2 subunits (NR2A–D) (10, 11). The two major NR2 subunits, NR2A and NR2B, reveal different physiologic and pharmacologic characteristics (12, 13). Studies in rats have shown that NR2B is the prevailing subunit in the rat brain during prenatal and early postnatal development and is highly expressed in forebrain areas (striatum, cortex), whereas NR2A is predominantly present in the adult brain and ubiquitously expressed (14, 15). Stimulated NR1/2B mediates excitatory postsynaptic potentials of longer duration than those of NR1/2A (16–20). Consequently, the NR2B-dominated immature brain is more susceptible to excitotoxicity than the NR2A-dominated adult brain (21, 22).
This paper contains the results of in vitro investigations on the effects of GA and 3-OH-GA on primary neuronal cultures from chick embryo telencephalons and on mixed neuronal and glial cultures from neonatal rat hippocampi to test our hypothesis that the age- and region-specific brain damage observed in GDD is caused by excitotoxic neuronal damage.
METHODS
Cell cultures.
Primary neuronal cultures from 7-d-old chick embryo telencephalons were prepared as previously described by Pettmann et al. (23). Briefly, cerebral hemispheres were dissociated through nylon meshes. The suspension was seeded onto poly-l-lysine (Sigma Chemical Co., Deisenhofen, Germany)-coated culture flasks (Nunc, Hamburg, Germany) with a density of 4 × 104 cells/cm2. Cell cultures were maintained in Dulbecco's modified Eagle medium supplemented with 20% fetal bovine serum at 37°C and 5% CO2 in a humidified atmosphere (DMEM and FBS; LifeTechnologies, Eggenstein, Germany). Every 2 d the medium was changed, and the cells were used for experiments between 2 and 6 DIV. It has been previously shown by our group that susceptibility to glutamatergic neuronal damage increased from 2 to 6 DIV in this culture (24).
Mixed neuronal and glial cultures from neonatal rat hippocampi (P1–2) were prepared as described by Sengpiel et al. (25). Briefly, the isolated hippocampi were dissected, treated with 0.1% papain (Sigma) in Leibovitz's L-15 medium (LifeTechnologies), and gently triturated. Recovered supernatants were transferred to 4 mL of 1% trypsin inhibitor in minimal essential medium (MEM; LifeTechnologies) containing 1% BSA, centrifuged (40 ×g, 20°C, 10 min), and then seeded onto poly-l-lysine-coated culture dishes (Nunc) at a density of 2 × 105 cells/cm2. The cells were cultivated in MEM supplemented with amphotericin, 10% NU-serum, 20 U/mL penicillin, and 20 μg/mL streptomycin for 2 d (LifeTechnologies). Thereafter, cultures remained unchanged in serum-free neurobasal medium supplemented with B-27 (LifeTechnologies) in a humidified atmosphere of 95% air and 5% CO2 at 37°C until the cells were used for experiments at 10 DIV. It has been previously described by our group that mixed neuronal and glial cultures are susceptible to glutamatergic neuronal damage between 10 and 14 DIV (26). Animal care followed official governmental guidelines and were approved by the government ethics committee.
Drug treatment.
GA (Sigma) and 3-OH-GA (Prof. Buckel, Institute of Microbiology, Philipps University of Marburg, Germany) were dissolved in the respective culture media, and the antagonists, 10 μM ifenprodil (Sigma), 10 μM MK-801, 50 μM CNQX, 50 μM L-AP3 (Tocris, Bristol, UK), 100 μM l-NAME, and 10 μM CGS-19755 (RBI, Natick, MA) were dissolved in PBS. Primary neuronal cultures from chick embryo telencephalons were incubated for 1–24 h with different concentrations (0.1–5 mM) of 3-OH-GA and GA at 6 DIV. Antagonists and antibodies were added to sister cultures 1 h before 1 mM GA or 3-OH-GA at 6 DIV. Furthermore, ifenprodil was added to sister cultures 1 h before 3-OH-GA and GA at different DIV (2, 4, 5, and 6).
Mixed neuronal and glial cultures from neonatal rat hippocampi were incubated for 1–24 h with different concentrations (0.5–5 mM) of 3-OH-GA and GA at 10 DIV. Antagonists were added to sister cultures 1 h before 1 mM GA or 3-OH-GA.
Trypan-blue exclusion method.
Cell viability was determined by trypan blue (0.4% in PBS) exclusion method 24 h after the beginning of the incubation period with GA or 3-OH-GA. The uptake of trypan blue indicates membrane leakage, an end point of neuronal degeneration. Cells were washed once with PBS and then were exposed to trypan blue for 5 min. The number of stained (nonviable) and unstained (viable) cells were counted under a microscope, and the level of cell viability was expressed as the percent ratio of unstained versus total number of cells. Only darkly stained neurons were considered damaged. A total number of 500–600 neurons were counted in eight randomly chosen subfields per group (n = 8). Cell counts were performed without knowledge of the respective treatment.
LDH release.
Cell viability was also determined by LDH release (27). After exposure to 0.1–5 mM GA or 3-OH-GA for 24 h, the intracellular and extracellular LDH activity was determined by an LDH assay kit (Sigma) on the basis of the optimized method as recommended by the German Society for Clinical Chemistry (n = 6 culture flasks per group). LDH release was calculated as the percent ratio of the changes in extinction per minute at a wavelength of 340 nm. of the extracellular versus the intracellular LDH activity. Controls were taken as 100%.
Nuclear staining of apoptotic cells with Hoechst 33258.
After fixation of cultured chick embryonic neurons with methanol and an incubation (15 min, 37°C) with 10 μg/mL DNA-binding fluorescent dye Hoechst 33258 (Sigma), nuclear morphology was observed under an Axiovert fluorescence microscope (Zeiss, Oberkochen, Germany) using a 40× fluorescence objective. Viable control cells showed a normal-size nucleus with a normal chromatin. In contrast, condensed chromatin at the nuclear periphery or nuclear fragmentation with reduction of nuclear size was found in apoptotic cells (28). Normal nuclei, nuclei exhibiting chromatin condensation, or nuclear fragmentation was counted in eight randomly chosen subfields per group (n = 8). Apoptosis was expressed as the percent ratio of apoptotic versus total number of cells. Cell counts were performed without knowledge of the respective treatments.
Immunocytochemistry of NR2B.
Cultured chick embryonic neurons (n = 3 culture flasks per group) were fixed with methanol and then incubated for 30 min with PBS containing 1% BSA. Thereafter, primary antibodies (anti-rat NR2B, rabbit IgG fraction; Molecular Probes, Eugene, OR), diluted 1:200, were added overnight at 4°C. After washing with PBS, neurons were incubated with the secondary antibody (Oregon Green 488 goat anti-rabbit IgG; Molecular Probes), diluted 1:100, for 30 min at room temperature. After removing and washing with PBS, the neurons were observed under an Axiovert fluorescence microscope (Zeiss) using a 40× fluorescence objective. Negative controls were performed by omitting the primary antibody.
Protein gel electrophoresis and Western blotting.
Cells were rinsed with PBS and lysed in Tris-buffered saline containing SDS, glycerin, and protease inhibitors. Samples (n = 3 culture flasks per group) were supplemented with 2-mercaptoethanol and denatured at 95°C for 5 min. SDS-PAGE was performed according to the technique of Laemmli (29) using 7.5% gels with 30 μg of protein per lane, which was transferred to a nitrocellulose membrane (Protran BA 83; Schleicher & Schüll, Dassel, Germany). Afterward, membranes were stained with Ponceau S. Nonspecific binding was blocked with blocking buffer containing 5% milk powder, 2% BSA, and 0.02% Tween 20 in PBS at room temperature for 3 h. Subsequently, membranes were incubated with polyclonal rabbit anti-rat NR2A or NR2B antibodies (Molecular Probes), or monoclonal anti-rat NR1 antibodies (Calbiochem, San Diego, CA), diluted 1:200 in blocking buffer, overnight at 4°C. Membranes were washed in washing buffer (0.05% Tween 20 in PBS) and incubated with horseradish peroxidase-conjugated anti-rabbit (polyclonal primary antibodies) or anti-mouse (monoclonal primary antibody) IgG (Promega, Madison, WI), diluted 1:2500 in blocking buffer, at room temperature for 1 h. After several rinses in washing buffer, immunoreactive proteins were visualized using an enhanced chemiluminescence detection system (SuperSignal; Pierce, Rockford, IL). Negative controls were performed by omitting the primary antibody.
Statistical analysis.
Data are expressed as mean ± SD for n = 8 (trypan blue exclusion method and staining with Hoechst 33258), n = 6 (LDH release), or n = 3 (Western blotting and immunocytochemistry). All experiments were performed in triplicate. Significant differences in cell viability after incubation with 3-OH-GA and GA, as well as antagonists and antibodies, were determined by one-way ANOVA followed by Scheffé's test. The difference between the effect of 3-OH-GA and GA from 2 to 6 DIV was determined by two-way ANOVA. The difference between NMDA receptor antagonists in inhibiting neuronal damage was determined by t test. A p < 0.05 was considered to indicate significance.
RESULTS
3-OH-GA and GA induce concentration- and time-dependent neuronaldamage.
Incubation with 0.1–5 mM GA and 3-OH-GA at 6 DIV decreased cell viability in chick embryonic neuronal cultures, depending on metabolite concentration (Fig. 1A, data of the 24-h group) and length of incubation period (Fig. 1B). Trypan blue exclusion method (performed 24 h after the beginning of the incubation period) revealed a significant decrease in cell viability after incubating 1 and 24 h at concentrations of ≥0.5 mM GA or ≥0.75 mM 3-OH-GA and ≥0.1 mM GA and ≥0.5 mM 3-OH-GA, respectively. Maximum decrease of cell viability was found at a concentration of 5 mM for both metabolites, but there was only a little additional reduction in cell viability when concentrations of GA or 3-OH-GA were raised to >1 mM, at incubation times of either 1 or 24 h. A direct comparison of GA or 3-OH-GA in sister cultures (24-h incubation) showed that 3-OH-GA induced a more pronounced decrease in cell viability at concentrations of ≥1 mM than GA (p < 0.001, 3-OH-GA versus GA, t test). Two-way ANOVA revealed a difference between the two metabolites, suggesting that 3-OH-GA is a slightly stronger neurotoxin than GA (p < 0.001; 3-OH-GA versus GA). By LDH release (6 DIV), it was shown that GA- and 3-OH-GA-induced efflux of LDH increased in a concentration-dependent manner at concentrations of ≥0.5 mM GA or 3-OH-GA, respectively, after an incubation period of 24 h (Fig. 1C).
Neurotoxic effect of 3-OH-GA and GA, as well as of different glutamate receptor antagonists and antibodies, on primary cultures from chick embryo telencephalons at 6 DIV. Data are shown as mean ± SD. A, concentration-dependent decrease in cell viability at 6 DIV (n = 8) as determined by trypan blue exclusion method after an incubation period of 24 h with 0.1–5 mM 3-OH-GA or GA. *p < 0.001 vs control. B, time-dependent decrease in cell viability at 6 DIV (n = 8) after incubation with 1 mM 3-OH-GA or GA for 1, 4, or 24 h. Cell viability was determined by trypan blue exclusion method 24 h after the beginning of the incubation. *p < 0.001. C, concentration-dependent increase in LDH release at 6 DIV (n = 6) after incubation with 0.1–5 mM 3-OH-GA or GA for 24 h. *p < 0.001 vs control. Preincubation of ifenprodil (IFP, 10 μM) prevented increase in LDH release. #p < 0.001. D, apoptotic cell damage at 6 DIV (n = 8) after an incubation with 0.1–5 mM 3-OH-GA or GA for 24 h as determined by staining with DNA fluorochrome Hoechst 33258. *p < 0.05 vs control. E, protective effect of NMDA receptor antagonists and NR2B antibodies (n = 8). Neurons were preincubated with antagonists and antibodies 1 h before the incubation with 3-OH-GA or GA. Cell viability was determined by trypan blue exclusion method 24 h after beginning of incubation with 1 mM 3-OH-GA or GA. *p < 0.001 vs 3-OH-GA or GA. CGS, CGS-19755. F, effect of other antagonists and NR2A antibodies (n = 8). No protection against neuronal damage was found. p > 0.05 vs 3-OH-GA or GA.
Furthermore, by nuclear staining with the DNA fluorochrome Hoechst 33258, we observed that both GA and 3-OH-GA caused necrosis rather than apoptosis in chick embryo neuronal cultures. Apoptosis was significant on a low level at concentrations of ≥0.5 mM GA, whereas 3-OH-GA induced apoptosis only at 5 mM after an incubation period of 24 h (Fig. 1D).
Preincubation with MK-801, ifenprodil, and NR2B antibodies totallyprevents 3-OH-GA- and GA-induced neuronal damage.
To determine whether 3-OH-GA- and GA-induced neuronal damage was mediated through glutamate receptors, we preincubated primary neuronal cultures from chick embryo telencephalons with different antagonists and antibodies 1 h before the application of 1 mM 3-OH-GA or GA at 6 DIV. Cell viability was measured 24 h after the beginning of the incubation period. Both 3-OH-GA- and GA-induced neuronal damage could be completely blocked by 10 μM MK-801 (nonspecific NMDA receptor antagonist), 10 μM [ifenprodil (NR2B-specific antagonist (12, 13)], and NR2B antibodies (1:200), whereas it was only partially blocked by 10 μM CGS-19755 [3-fold more selective for NR2A than for NR2B (13); Fig. 1E]. Neuronal damage was not prevented by NR2A antibodies (1:200), 50 μM CNQX (α-amino-3-hydroxy-5-methyl-4-isoxazole propionate receptor antagonist), 50 μM L-AP3 (metabotropic glutamate receptor antagonist), or 100 μM l-NAME (nitric oxide synthase inhibitor) (Fig. 1F). CGS-19755 blocked only 3-OH-GA- but not GA-induced neuronal damage and was less potent in inhibiting 3-OH-GA- and GA-induced neuronal damage than MK-801 and ifenprodil (p < 0.001, MK-801 or ifenprodil versus CGS-19755, t test). Ifenprodil, MK-801, and CGS-19755 inhibited 3-OH-GA- and GA-induced cell damage in a concentration-dependent manner. 3-OH-GA- and GA-induced increases in LDH release were prevented by preincubation with ifenprodil (Fig. 1C).
Similar results were found in mixed neuronal and glial cultures from neonatal rat hippocampi. Trypan blue exclusion method revealed a decrease in cell viability at concentrations of ≥1 mM GA after an incubation period of 24 h, reaching a maximum at 5 mM GA or 3-OH-GA (Fig. 2A). A time-dependent decrease in cell viability was found for 3-OH-GA but not for GA (Fig. 2B).
Effect of 3-OH-GA and GA on mixed neuronal and glial cultures from neonatal rat hippocampi at 10 DIV. Cell viability was determined by trypan blue exclusion method 24 h after the beginning of the incubation with 3-OH-GA or GA. Data are shown as mean ± SD. A, concentration-dependent decrease in cell viability at 10 DIV (n = 8) after an incubation period of 24 h with 0.5–5 mM 3-OH-GA or GA. **p < 0.01, ***p < 0.001 vs control. B, cell viability of cultured neurons after an incubation with 1 mM 3-OH-GA or GA for 1, 4, or 24 h. **p < 0.01, ***p < 0.0001. No time-dependent effect was found for GA. C, effect of different glutamate receptor antagonists on neuronal damage induced by 3-OH-GA or GA (n = 8). *p < 0.05, ***p < 0.001 vs 3-OH-GA or GA. IFP, ifenprodil.
The results were confirmed by mixed neuronal and glial cell cultures from neonatal rat hippocampi (Fig. 2C). Preincubation with 10 μM ifenprodil and 10 μM MK-801 prevented neuronal damage induced by 3-OH-GA or GA, whereas 50 μM CNQX and 50 μM L-AP3 did not.
Expression of NR1/2B and susceptibility to 3-OH-GA- and GA-inducedneuronal damage.
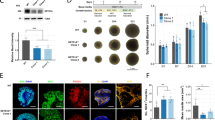
We investigated the expression of the NMDA receptor subunits NR1, NR2A, and NR2B on cultured chick embryonic neurons from 2 to 6 DIV. NR2A scarcely increased during the period in culture, whereas the expression of NR1 and NR2B increased markedly from 2 to 6 DIV (Fig. 3A). Immunocytochemistry revealed a time-dependent pattern of NR2B expression on cultured neurons. At 2 DIV NR2B was diffusely expressed on the soma, whereas its expression increased at the axonal pole of the neurons in particular at 6 DIV (Fig. 3B). Exposure of cultured chick embryo neurons to 1 mM GA or 3-OH-GA at different DIV showed a marked increase of susceptibility to 3-OH-GA- and GA-induced neuronal damage from 2 to 6 DIV (Fig. 3, C and D ). 3-OH-GA and GA differed from each other concerning neurotoxicity (Fig. 3, C and D ). At all DIV, we found that preincubation with ifenprodil protected cultured neurons against neuronal damage induced by 3-OH-GA, as well as GA (Fig. 3, C and D ).
Expression and distribution of NMDA receptor subunits NR1, NR2A, and NR2B and susceptibility to neuronal damage induced by 3-OH-GA or GA from 2 to 6 DIV in cultured chick embryo neurons. A, expression of NMDA receptor subunits NR1 (top), NR2B (middle), and NR2A (bottom) from 2 to 6 DIV. Western blots from a pool of n = 3 culture flasks show increasing expression of subunits NR1 and NR2B and a stable expression of subunit NR2A from 2 to 6 DIV. All lanes were loaded with equal amounts of protein. B, distribution of subunit NR2B in cultured chick embryonic neurons at 2 (left), 4 (middle), and 6 DIV (right). Pictures were taken under a fluorescence microscope (λ = 490 nm), using a 40× fluorescence objective (scale bar, 10 μm). Arrowheads indicate increasing expression of subunit NR2B at the axonal pole from 2 to 6 DIV. C, D, Susceptibility of cultured chick embryonic neurons to 1 mM 3-OH-GA (C) or GA (D) from 2 to 6 DIV as determined by trypan blue exclusion method (n = 8). Preincubation with ifenprodil (IFP) prevented neuronal damage induced by 3-OH-GA or GA. *p < 0.001 ifenprodil vs 3-OH-GA or GA. n.s. not significant, control vs ifenprodil.
DISCUSSION
The major findings of the present study are the induction of neuronal damage by 3-OH-GA and GA through NR1/2B in primary neuronal cultures from chick embryo telencephalons and mixed neuronal and glial cultures from neonatal rat hippocampi, and the dependency of neurotoxicity on metabolite concentration, length of incubation period, and expression of NR1/2B. Concentrations of 3-OH-GA and GA that we found to induce neuronal damage in our cell culture systems in vitro are similar to those found in body fluids of patients with GDD, in whom 3-OH-GA and GA concentrations in plasma and cerebrospinal fluid are usually between 5 and 400 μM (2, 5, 30) but may rise considerably higher (up to 1–2 mM) during acute encephalopathic crises (3, 31). Both in vitro systems were used for the investigation of excitotoxic neuronal damage in previous studies. Although 3-OH-GA as well as GA was neurotoxic in both systems, primary neuronal cultures from chick embryo telencephalons (23) were more susceptible to 3-OH-GA and GA than mixed neuronal and glial cultures from neonatal rat hippocampi (25). This difference could be determined by differences in species, neuronal populations, age of neurons, and expression of NMDA receptors, as well as glial influence. Previously, in organotypic brain slice cultures, only a neurotoxic effect of 3-OH-GA at high concentrations (>1.5 mM), but not one of GA, could be demonstrated, suggesting a lesser sensitivity to 3-OH-GA and GA in this system than in our in vitro systems (8). Previous studies suggested that 3-OH-GA and GA mediated neurotoxicity through the inhibition of brain glutamate decarboxylase with subsequently impaired γ-aminobutyric acid production, a reduction of glutamate uptake into synaptosomes, or an unspecific neurotoxic mechanism (6, 8, 32). For the first time, our results demonstrate a specific inhibition of 3-OH-GA- and GA-induced neuronal damage after preincubation with MK-801, ifenprodil, and NR2B antibodies, but not after preincubation with CNQX, L-AP3, l-NAME, or NR2A antibodies. This finding is consistent with the hypothesis that 3-OH-GA and GA act as false neurotransmitters—instead of the excitotoxic amino acid glutamate—specifically through NR1/2B, and is in line with the previous observation that histologic abnormalities found in basal ganglia and the cortex of patients with GDD post mortem resemble glutamate-mediated damage (3). In previous studies, it has been shown that the expression of different NR2 subunits is age- and region-dependent (14, 15, 19). The NR2B-dominated immature brain is more susceptible to NMDA-induced neurotoxicity than the NR2A-dominated mature brain is (21, 22). Therefore, our findings of an increase in 3-OH-GA- and GA-induced neurotoxicity, together with an increasing expression of NR1/2B on neurons during the culture period, are in line with the assumption of maturation-dependent neurotoxicity of 3-OH-GA and GA. Properties of NMDA receptors are also modulated by the NR1 subunit (33, 34). We demonstrated that the expression of subunit NR1 increased from 2 to 6 DIV, suggesting that functional NMDA receptors were expressed. Although not known to date, it can be supposed that the region-specific expression of different NR1 splice variants also modulates the susceptibility of certain brain areas to 3-OH-GA and GA.
Why the striatum is the primary structure involved in acute encephalopathic crises remains to be clarified. One possible explanation is a high expression of NR1/2B during a vulnerable period of time, leading to an enhanced susceptibility to excitotoxic neuronal damage (14, 15, 19, 33, 35). Furthermore, it has to be considered that the striatum has a high blood supply and metabolic rate, indicating a high demand for ATP (36, 37). Therefore, the striatum is supposed to be at particular risk for limitations of function in energy metabolism as it was previously described for the administration of 3-nitropropionic acid and methylmalonic acid (38, 39). Acute encephalopathic crises typically precipitate from a catabolic state in GDD and can be prevented by sufficient glucose and carnitine supply (5). The addition of both a high expression of NR1/2B and the particular risk of energy depletion may lead to an amplification of neuronal damage through primary and secondary excitotoxic mechanisms in the striatum (40). Although the striatum is the primary site of acute neuronal damage, other brain areas (e.g. the frontotemporal cortex) are also involved in the neurodegeneration in GDD (2, 3, 5). This observation implies that neurotoxicity induced by 3-OH-GA and GA is not restricted to a certain population of neurons but is modulated by different factors, i.e. expression of NMDA receptors and energy demand and supply, as well as region-specific input of inhibitory neurotransmitters.
NMDA receptors are known to play an important role in the regulation of neurite outgrowth, pathfinding, modulation of cell migration, and synaptic plasticity in the developing CNS (41–44). Only recently it was demonstrated that NR2B is enriched in axonal processes of the neonatal rat brain, which implies a particular importance of NR2B for the above-mentioned developmental processes (43). Our observation of a time-dependent change in NR2B expression from a diffuse to a more axon-stressed pattern on cultured chick embryonic neurons is consistent with this assumption. The period from the third trimester of pregnancy to the age of 15 mo comprises the critical period for formation of synapses in prefrontal cortex. Interestingly, neuroradiologic and pathologic investigations of brains from GDD patients revealed distinct signs of a delayed maturation (2, 5, 45, 46), starting already prenatally in the third trimester of pregnancy. Although it is not known to date, it can be supposed that delayed neuronal maturation in GDD patients may also be induced by 3-OH-GA and GA through NMDA receptors (47).
Our findings of specific, NR1/2B-mediated neurotoxicity of GA and 3-OH-GA give strong support to the hypothesis that the severe age- and region-specific neuronal damage observed in GDD is related to a high expression of NR1/2B in the forebrain (striatum, cortex) during a specific vulnerable period of brain development (33, 35, 48). Although it is not proven that our results can be transferred to humans, we suppose that they give new insights in the kinetic processes in GDD (Fig. 4). These findings imply that specific inhibition of NR1/2B may be implemented into the therapeutic regimen to prevent acute encephalopathies (4).
Dynamic three-state model of GDD. High expression of NR1/2B and toxic concentrations of 3-OH-GA or GA are a conditio sine qua non for the induction of acute encephalopathic crises in GDD (immature, acute). Subtoxic concentrations of 3-OH-GA or GA do not cause excitotoxic damage but a down-regulation of NR1/2B in vitro (47), which is supposed to induce a delay in neuronal maturation (41, 43, 49, 50) (immature, chronic). A number of exogenous and endogenous factors are supposed to precipitate acute encephalopathic crises (51). After 5–6 y of life, no acute encephalopathic crises occur in the NR2A-dominated mature brain (mature, chronic). Only those children who are diagnosed early and who are treated adequately have a realistic chance to survive unharmed.
Abbreviations
- DIV:
-
days in vitro
- GA:
-
glutaric acid
- 3-OH-GA:
-
3-hydroxyglutaric acid
- GDD:
-
glutaryl-CoA dehydrogenase (EC 1.3.99.7) deficiency
- LDH:
-
lactate dehydrogenase
- [f]l-NAME:
-
Nω-nitro-l-arginine methyl ester
- NMDA:
-
N-methyl-d-aspartate
- NR1:
-
NMDA receptor subunit 1
- NR2A:
-
NMDA receptor subunit 2A
- NR2B:
-
NMDA receptor subunit 2B
References
Online Mendelian Inheritance in Man OMIM (Tm). Johns Hopkins University, Baltimore. MIM Number: 231670: Updated 8/13/98 World Wide Web URL: http://www.ncbi.nlm.nih.gov/omim
Goodman SI, Kohlhoff JG 1975 Glutaric aciduria: inherited deficiency of glutaryl CoA dehydrogenase activity. Biochem Med 13: 138–140.
Hoffmann GF, Trefz FK, Barth P, Böhles JH, Biggemann B, Bremer HJ, Christensen E, Frosch M, Hanefeld F, Hunneman DH, Jacobi H, Kurlemann G, Lawrenz-Wolf B, Rating D, Roe CR, Schutgens RBH, Ullrich K, Weisser J, Wendel U, Lehnert W 1991 Glutaryl-CoA deficiency: a distinct encephalopathy. Pediatrics 88: 1194–1203.
Goodman SI, Norenberg MD, Shikes RH, Breslich DJ, Moe PG 1977 Glutaric aciduria: biochemical and morphological considerations. J Pediatr 90: 746–750.
Baric I, Zschocke J, Christensen E, Duran M, Goodman SI, Leonard JV, Müller E, Morton DH, Superti-Furga A, Hoffmann GF 1998 Diagnosis and management of glutaric aciduria type I. J Inherit Metab Dis 21: 326–340.
Hoffmann GF, Athanassopoulos S, Burlina AB, Duran M, deKlerck JBC, Lehnert W, Leonard JV, Monavari AA, Müller E, Muntau AC, Naughten ER, Plecko-Starting B, Superti-Furga A, Zschocke J, Christensen E 1996 Clinical course, early diagnosis, treatment, and prevention of disease in glutaryl-CoA dehydrogenase deficiency. Neuropediatrics 27: 115–123.
Stokke O, Goodman SI, Moe PG 1976 Inhibition of brain glutamate decarboxylase by glutarate, glutaconate, and beta-hydroxyglutarate: explanation of the symptoms in glutaric aciduria?. Clin Chim Acta 66: 411–415.
Heyes MP 1987 Hypothesis: a role for quinolinic acid in the neuropathology of glutaric aciduria type I. Can J Neurol Sci 14: 441–443.
Flott-Rahmel B, Falter C, Schluff R, Fingerhut R, Christensen E, Jakobs C, Musshoff U, Fauter JD, Deufel T, Ludolph A, Ullrich K 1997 Nerve cell lesions caused by 3OH-glutaric acid: a possible mechanism for neurodegeneration in glutaric acidaemia I?. J Inherit Metab Dis 20: 387–390.
Kölker S, Ahlemeyer B, Krieglstein J, Hoffmann GF 1999 3-Hydroxyglutaric and glutaric acids are neurotoxic through NMDA receptors in vitro. J Inherit Metab Dis 22: 259–262.
Choi DW 1988 Glutamate neurotoxicity and diseases of the nervous system. Neuron 1: 623–634.
Scatton B 1993 The NMDA receptor complex. Fundam Clin Pharmacol 7: 389–400.
Williams K 1993 Ifenprodil discriminates subtypes of the N-methyl- d -aspartate receptor: selectivity and mechanisms at recombinant heteromeric receptors. Mol Pharmacol 44: 851–859.
Priestley T, Ochu E, Kemp JA 1994 Subtypes of NMDA receptor in neurones cultured from rat brain. Neuroreport 5: 1763–1765.
Portera-Cailliau C, Price DL, Martin LJ 1996 N-methyl- d- aspartate receptor proteins NR2A and NR2B are differentially distributed in the developing rat central nervous system as revealed by subunit-specific antibodies. J Neurochem 66: 692–700.
Wenzel A, Fritschy JM, Mohler H, Benke D 1997 NMDA receptor heterogeneity during postnatal development of the rat brain: differential expression of the NR2A, NR2B, and NR2C subunit proteins. J Neurochem 68: 469–478.
Tsumoto T, Hagihara K, Sato H, Hata Y 1987 NMDA receptors in the visual cortex of young kittens are more effective than those of adult cats. Nature 327: 513–514.
Carmignoto G, Vicini S 1992 Activity-dependent decrease in NMDA receptor responses during development of the visual cortex. Science 258: 1007–1011.
Hestrin S 1992 Developmental regulation of NMDA receptor-mediated synaptic currents at a central synapse. Nature 357: 686–689.
Monyer H, Burnashev N, Laurie DJ, Sakmann B, Seeburg PH 1994 Developmental and regional expression in the rat brain and functional properties of four NMDA receptors. Neuron 12: 529–540.
Ramoa AS, McCormick DA 1994 Enhanced activation of NMDA receptor responses at the immature retinogeniculate synapse. J Neurosci 14: 2098–2105.
McDonald JW, Silverstein FS, Johnston MV 1988 Neurotoxicity of N-methyl- d -aspartate is markedly enhanced in developing rat central nervous system. Brain Res 459: 200–203.
McDonald JW, Behrens MI, Chung C, Bhattacharyya T, Choi DW 1997 Susceptibility to apoptosis is enhanced in immature cortical neurons. Brain Res 759: 228–232.
Pettmann B, Louis JC, Sensenbrenner MCL 1979 Morphological and biochemical maturation of neurones cultured in the absence of glial cells. Nature 281: 378–380.
Prehn J 1992 Protektive Effekte von Pharmaka gegen exzitotoxische neuronale Schädigung in vitro und und ischämische neuronale Schädigung in vivo. Dissertation, Philipps University of Marburg, Germany
Sengpiel B, Preis E, Krieglstein J, Prehn JHM 1998 NMDA-induced superoxide production and neurotoxicity in cultured rat hippocampal neurons: role of mitochondria. Eur J Neurosci 10: 1903–1910.
Lippert K 1993 Neuroprotektive Arzneistoffeffekte gegen eine exzitotoxische Schädigung. Untersuchung an dissoziiert kultivierten Neuronen des selektiv vulnerablen Hippocampus. Dissertation, Philipps University of Marburg, Germany
Koh JY, Choi DW 1987 Quantitative determination of glutamate-mediated cortical neuronal injury in cell culture by lactate dehydrogenase efflux assay. J Neurosci Methods 20: 83–90.
Leist M, Nicotera P 1997 Breakthroughs and views: the shape of cell death. Biochem Biophys Res Commun 236: 1–9.
Laemmli UK 1970 Cleavage of structural proteins during the assembly of the head of bacteriophage T4. Nature 227: 680–685.
Merinero B, Pérez-Cerdà C, Font LM, Garcia MJ, Aparicio M, Lorenzo G 1995 Variable clinical and biochemical presentation of seven Spanish cases with glutaryl-CoA dehydrogenase deficiency. Neuropediatrics 26: 238–242.
Land JM, Goulder P, Johnson A, Hockaday J 1992 Glutaric aciduria type I: an atypical presentation together with some observations upon treatment and the possible cause of cerebral damage. Neuropediatrics 23: 322–326.
Bennett JP, Logan WJ, Snyder SH 1973 Amino acids as central nervous transmitters: the influence of ions, amino acid analogues, and ontogeny on transport systems for l -glutamic and l -aspartic acids and glycine into central nervous synaptosomes of the rat. J Neurochem 21: 1533–1550.
Standaert DG, Testa CM, Young AB, Penney JB Jr 1994 Organization of N-methyl- d -aspartate receptor gene expression in the basal ganglia of the rat. J Comp Neurol 343: 1–16.
Laurie DJ, Seeburg PH 1994 Regional and developmental heterogeneity in splicing of the rat brain NMDAR1 mRNA. J Neurosci 14: 3180–3194.
Kosinski CM, Standaert DG, Counihan TJ, Scherzer CR, Kerner JA, Daggett LP, Velcelebi G, Penney JB, Young AB, Landwehrmeyer GB 1998 Expression of N-methyl- d -aspartate receptor subunit mRNAs in the human brain: striatum and globus pallidus. J Comp Neurol 390: 63–74.
Hawkins RA, Mans AM, Davis DW, Hibbard LS, Lu DM 1983 Glucose availability to individual cerebral structures is correlated to glucose metabolism. J Neurochem 40: 1013–1018.
Cunningham VJ, Hargreaves RJ, Pelling D, Moorhouse SR 1986 Regional blood-brain transfer in the rat: a novel double-membrane kinetic analysis. J Cereb Blood Flow Metab 6: 305–315.
Wajner M, Coelho JC 1997 Neurological dysfunction in methylmalonic acidaemia is probably related to the inhibitory effect of methylmalonate on brain energy production. J Inherit Metab Dis 20: 761–768.
Ludolph AC, He F, Spencer PS, Hammerstad J, Sabri M 1991 3-Nitropropionic acid: exogenous animal neurotoxin and possible human striatal toxin. Can J Neurol Sci 18: 492–498.
Ludolph AC, Riepe M, Ullrich K 1993 Excitotoxicity, energy metabolism and neurodegeneration. J Inherit Metab Dis 16: 716–723.
Komuro H, Rakic P 1993 Modulation of neuronal migration by NMDA receptors. Science 260: 95–97.
Bliss TVP, Collingridge GL 1993 A synaptic model of memory: long-term potentiation in the hippocampus. Nature 361: 31–39.
Herkert M, Röttger S, Becker CM 1998 The NMDA receptor subunit NR2B of neonatal rat brain: complex formation and enrichment in axonal growth cones. Eur J Neurosci 10: 1553–1562.
Sprengel R, Suchanek B, Amico C, Brusa R, Burnashev N, Rozov A, Hvalby O, Jensen V, Paulsen O, Andersen P, Kim JJ, Thompson RF, Sun W, Webster LC, Grant SGN, Eilers J, Konnerth A, Li J, McNamara JO, Seeburg PH 1998 Importance of the intracellular domain of NR2 subunits for NMDA receptor function in vivo. Cell 92: 279–289.
Amir N, Elpeleg O, Shalev RS, Christensen E 1987 Glutaric aciduria type I: clinical heterogeneity and neuroradiologic features. Neurology 37: 1654–1657.
Brismar J, Ozand PT 1995 CT and MR of the brain in glutaric acidemia type I: a review of 59 published cases and a report of 5 new patients. Am J Neuroradiol 16: 675–683.
Kölker S, Ahlemeyer B, Krieglstein J, Hoffmann GF 1999 Hypothesis: delay in neuronal maturation in GA-I is a consequence of NMDA receptor downregulation by 3-OH-glutaric and glutaric acids. J Inherit Metab Dis 22: 137abstr
Stocca G, Vicini S 1998 Increased contribution to NR2A subunit to synaptic NMDA receptors in developing rat cortical neurons. J Physiol Lond 507: 13–24.
Resink A, Villa M, Benke D, Hidaka H, Möhler H, Balázs R 1996 Characterization of agonist-induced down-regulation of NMDA receptors in cerebellar granule cell cultures. J Neurochem 66: 369–377.
Tatum WO, Coker SB, Ghobrial M, Abd-Allah S 1989 The open opercular sign: diagnosis and significance. Ann Neurol 25: 196–199.
Kölker S, Ahlemeyer B, Krieglstein J, Hoffmann GF 1999 Trigger factors of acute encephalopathy in GA-I: fever and TNF-α. J Inherit Metab Dis 22: 115abstr
Acknowledgements
3-Hydroxyglutaric acid was generously custom synthesized by Prof. W. Buckel (Institute of Microbiology, Philipps University of Marburg, Germany).
Author information
Authors and Affiliations
Additional information
Supported by the Deutsche Forschungsgemeinschaft KO 2010/1–1.
Rights and permissions
About this article
Cite this article
Kölker, S., Ahlemeyer, B., Krieglstein, J. et al. Maturation-Dependent Neurotoxicity of 3-Hydroxyglutaric and Glutaric Acids In Vitro : A New Pathophysiologic Approach to Glutaryl-CoA Dehydrogenase Deficiency. Pediatr Res 47, 495–503 (2000). https://doi.org/10.1203/00006450-200004000-00014
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200004000-00014
This article is cited by
-
Sensitive neurotoxicity assessment of bisphenol A using double immunocytochemistry of DCX and MAP2
Archives of Pharmacal Research (2018)
-
A cross-sectional controlled developmental study of neuropsychological functions in patients with glutaric aciduria type I
Orphanet Journal of Rare Diseases (2015)
-
Age and Brain Structural Related Effects of Glutaric and 3-Hydroxyglutaric Acids on Glutamate Binding to Plasma Membranes During Rat Brain Development
Cellular and Molecular Neurobiology (2007)
-
Biochemistry and bioenergetics of glutaryl‐CoA dehydrogenase deficiency
Journal of Inherited Metabolic Disease (2007)
-
Infant mice with glutaric acidaemia type I have increased vulnerability to 3‐nitropropionic acid toxicity
Journal of Inherited Metabolic Disease (2006)