Abstract
Erythropoietin (Epo) is a normal constituent of human milk, but the origin and fate of this cytokine in milk are not known. Regarding its origin, we hypothesized that cells of the mammary gland secrete Epo into milk actively and, therefore, that concentrations in milk do not correlate with concentrations in serum. Regarding its fate, we hypothesized that Epo concentrations in milk change with time postpartum and that Epo in milk is protected from digestion in the neonatal gastrointestinal tract. To address these issues, we measured Epo concentrations in 103 milk samples (ELISA), 55 of which were paired with serum. Mammary duct epithelial cells were evaluated as a source of Epo by breast tissue immunohistochemistry and by cell culture. Circulating and milk Epo were compared by Western analysis to detect size differences, possibly reflecting differences in processing. Epo stability in simulated conditions of digestion was evaluated. We observed that milk Epo concentrations increase as a function of duration of breast-feeding and have a negative correlation with serum Epo or milk protein concentration. Mammary duct epithelial cells from breast biopsies of lactating women had marked immunoreactivity to Epo, but such activity was minimal to absent in nonlactating breast tissue. Further evidence that mammary duct epithelia produce Epo was obtained by observing Epo mRNA and protein expression in cultured human mammary epithelial cells. The molecular size of Epo in milk and serum is identical. Recombinant Epo added to human milk or commercial infant formulas was relatively stable in conditions that simulate gastric and small intestinal conditions of newborn infants; however, recombinant Epo added to D5W was not protected from digestion. We conclude that Epo concentrations in milk increase as a function of the duration of breast feeding, that Epo is actively secreted into human milk by mammary duct epithelia, and that the Epo within milk is largely protected from digestion.
Similar content being viewed by others
Main
Significant Epo concentrations have been measured in human milk (1), but the origin and fate of Epo in milk are not known. Specifically, it is not known whether Epo is secreted actively or passively into milk, whether any Epo-producing cells exist in breast tissue, whether maternal serum Epo concentrations correlate with milk Epo concentrations, or whether milk Epo is processed differently from circulating Epo, resulting in a difference in glycosylation. In addition, it is not known whether Epo concentrates in a particular partition (fore, mid, or hind milk) or phase (aqueous versus lipid) of milk. No information is available regarding the stability of rEpo added to commercially available infant formulas or whether routine storage conditions (freeze/thaw) or pasteurization procedures (heating) degrade Epo.
A physiologic role for enteral Epo is likely, as Epo-R are present on mucosal cells of the fetal and neonatal GI tract (2, 3), and specific binding of rEpo to Epo-R in rat gastric mucosal cells has been established (4). Intestinal cells are exposed to intraluminal Epo during fetal life because it is present in amniotic fluid (5, 6), which is continually swallowed by the fetus. Intraluminal exposure to Epo continues postnatally as it is present in colostrum and breast milk. Possible roles for enteral Epo include systemic absorption with subsequent erythropoietic effects or, alternatively, local effects in bowel. In vitro studies of rat intestinal epithelial cells (IEC-6) show that the enteral Epo-R are functional, because stimulation of these cells with rEpo increases the rate of cell migration and attenuates apoptotic death after exposure to toxic cytokines (3). Animal and human studies regarding the absorption of Epo after enteral dosing are controversial (7–11). More studies are needed to clarify this issue.
The present study was designed to test the hypotheses that 1) Epo concentrations in milk change with time postpartum, 2) Epo is secreted actively into human milk, and 3) rEpo added to milk or commercial infant formulas is resistant to digestion in the neonatal GI tract.
Comparison of Simultaneous Serum and Milk Epo Concentrations
Milk and serum samples.
One hundred three milk samples were obtained from 44 postpartum women after informed consent was obtained. Fifty-five milk samples had a simultaneous paired serum sample. The duration of time postpartum was recorded for each sample, as was the gestational age of the infant at delivery. Ten samples were evaluated for Epo concentration in fore, mid, and hind milk. These fractions were defined as the first, middle, and last 5 min of pumping. The phase of milk (whole milk, aqueous phase, and lipid phase) in which Epo resided was investigated in 10 samples. The present study was approved by the University of Florida Institutional Review Board.
Epo ELISA.
Epo concentrations in milk and serum (100-μL aliquots) were determined by specific ELISA (R&D System, Minneapolis, MN, U.S.A.). A standard curve was established using duplicate measurements of the standard solutions provided with the ELISA, and separate curves were generated using milk samples “spiked” with rEpo to assess the ELISA function in milk. The curve generated using spiked samples (25, 50, 75, and 100 mU/mL added) paralleled the standard curve; however, a significant but consistent quenching of Epo was noted to the extent that approximately 65 to 70% of added rEpo was detected. This quenching effect was observed in all milk samples regardless of whether they were fresh, frozen and thawed, or heated. (We postulate that this is likely a result of the high fatty acid content in milk, resulting in decreased binding of Epo to antibody.) Values are reported as the measured concentration.
Protein analysis.
Milk protein concentrations were determined by Bio-Rad DC Protein Assay kit (Bio-Rad, Hercules, CA, U.S.A.).
Immunoprecipitation and Western analysis.
Milk and serum samples known to have high (>70 mU/mL) Epo concentrations were chosen for analysis. Immunoprecipitation was done using polyclonal goat anti-Epo primary antibody (Santa Cruz Biotechnology, Santa Cruz, CA, U.S.A.) conjugated to protein A-agarose (Santa Cruz). Beads were washed four times with RIPA buffer (Santa Cruz) and the pellet resuspended in 40 μL of 200 mM Tris-Tricine sample buffer (Bio-Rad Cat #161-0739 200 mM Tris-HCl, pH 6.8, 40% glycerol, 2% SDS, 0.04 Coomassie Blue). Proteins were separated on a 16.5% Tris-Tricine gel. After transfer to an Immune-Blot® PVDF membrane (Bio-Rad), the membrane was incubated in 15 mL of blocking buffer (3% BSA and 0.05% Tween 20 in 50 mM Tris-HCl, pH 7.4, 260 mM NaCl, 0.1% Triton X-100) at 4°C overnight. It was then probed with a monoclonal mouse anti-human Epo antibody (Genzyme, Cambridge, MA, U.S.A.) for 2 h, washed, and secondary antibody (goat, anti-mouse diluted 1:2000; Southern Biotechnology Associates, Inc., Birmingham, AL, U.S.A.) applied. The Alkaline Phosphatase Substrate Kit (Vector Laboratories) was used to detect the protein on the filter.
Potential Sources of Epo in Milk
Immunohistochemistry.
Specimens of lactating breast tissue were compared with age-matched nonlactating tissue samples. Samples were obtained from needle biopsies or surgical specimens from women evaluated for breast masses or during breast reduction surgery. Table 1 shows the relevant clinical information from these individuals. Only areas of tissues that were histologically normal in appearance (as determined by a surgical pathologist) were evaluated. Five-micrometer sections were deparaffinized in two xylene washes and then rehydrated through a graded series of alcohols, finishing with water. Staining was done using the Ventana automated slide-staining system (Ventana Medical Systems, Tucson, AZ, U.S.A.) with diaminobenzidine as the chromogen. A monoclonal mouse anti-human Epo antibody (Genzyme) was used at 1:100 dilution for 32 min to detect Epo immunoreactivity. A polyclonal antibody to the Epo-R (Santa Cruz) diluted 1:100 was used to detect Epo-R immunoreactivity. PBS containing 0.1% Triton X-100 was used as antibody diluent. Sections were counterstained for 4 min with hematoxylin and bluing (Ventana). Absence of the primary antibody was used as a negative control for each antibody, and, in addition, for Epo-R staining, preincubation with an excess of specific blocking peptide was used (Santa Cruz). All negative controls showed absence of staining. Human fetal liver and placenta were used as positive controls for both antibodies.
Cell culture.
HMEC were obtained from Clonetics (Bio Whittaker, Inc., San Diego, CA, U.S.A.). This cell culture was established from normal human breast tissue and was not transformed. Cells were grown in mammary epithelial cell growth medium containing 10 ng/mL human recombinant epidermal growth factor, 5 μg/mL insulin, 0.5 μg/mL hydrocortisone, 50 μg/mL gentamicin, 50 ng/mL amphotericin-B, and 13 mg/mL bovine pituitary extract (Clonetics). Cells were grown to approximately 70% confluence in 100-mm dishes. Triplicate cultures were changed to quiescent media (no pituitary extract added) and then exposed to the following conditions that we predicted might result in Epo production:1) control, 2) IGF-1 (10 ng/mL) for 16 h, 3) hypoxia (24 h at 8% oxygen). To evaluate Epo and Epo-R protein expression in these cells, they were grown in the above conditions in chamber slides (Lab-Tek) and then immunostained using antibodies to Epo and Epo-R as described previously (2).
Preparation of total RNA.
Total RNA was extracted from the cultured HMEC by using the RNeasy elution kit, a method of RNA extraction based on the selective binding of RNA to a silica membrane (Qiagen, Chatsworth, CA, U.S.A.) (12, 13). Manufacturer directions were followed. Purity and concentration of extracted RNA were determined by measuring UV absorbance at 260 and 280 nm. Total RNA was treated with RNase-free DNase I (GIBCO, Gaithersburg, MD, U.S.A.) before further experimentation.
Reverse transcription of RNA and semiquantitative PCR.
Reverse transcription of RNA and amplification of cDNA were performed as previously described (3). Primer pairs used to identify Epo were 5′-CCCTGTTGGTCAACTCTTCC and 5′-GTGTACAGCTTCAGCTTTCC (234-bp fragment). Epo-R primers were 5′-GGCAGTGTGGACATAGTGGC and 5′-AGCAGGATGGA TTGGGCAGA (497-bp fragment), and β-actin primers were 5′-TGACGGGGTCACCCACACTG TGCCCATCTA and 5′-CTAGA-GCATTTGCGGTGGACGATGGAGGG (661-bp fragment). RNA was tested for DNA contamination by running a PCR sample using RNA that had not been reverse transcribed. All negative controls were negative. Fetal liver was positive control. Semiquantitative PCR was performed relating synthesis of Epo cDNA to 18S RNA as an internal standard (Ambion, Inc., Austin, TX, U.S.A.). Initial experiments were done to determine the optimal 18S primer/Competimer concentration (1:9). After completion of the PCR (35 cycles), 15 μL of the reaction was separated by electrophoresis through a 2% agarose gel in 0.5X Tris-borate-EDTA buffer, and size was standardized with 100-bp DNA markers (GIBCO). The PCR products were photographed, digitized, and stored as TIFF files. Scion Image software (Scion Corp, Fredrick, MD, U.S.A.) was used to determine band intensities. Ratios of band intensities were calculated and normalized for molecular weight by using Microsoft Excel (Microsoft, U.S.A.). The normalized ratios were plotted on a log-log scale versus copy number, and a best fit curve and the equation for the line (y = mx + b) were determined using Sigma Chemical Co. Plot (SPSS Inc., Chicago, IL, U.S.A.).
Epo secretion by HMEC.
Spent medium from HMEC cells was removed and concentrated 10-fold using Cenricon centrifugal filter devices YM-10 (Millipore Corp., Tempe, AZ, U.S.A.). Epo concentration was then determined by specific ELISA.
Immunoprecipitation and Western analysis.
Confluent HMEC cells were lysed in 1 mL of lysis buffer consisting of 50 mM Tris-HCl, pH 8.0, 1.0% Triton X-100, 1 μM pepstatin, 1 μM leupeptin, 1 μM antipain and 2 μM phenylmethylsulfonyl fluoride and 0.02% sodium azide. For the identification of Epo, goat anti-human Epo antibody (Santa Cruz) was used for immunoprecipitation and rabbit anti-human Epo antibody (Sigma Chemical Co.) for Western analysis (12% Tris-glycine gel). Goat anti-human Epo-R antibody (R&D Systems) was used for Epo-R detection by Western analysis of Epo-R (10% Tris-glycine).
Epo Resistance to Simulations of Digestion
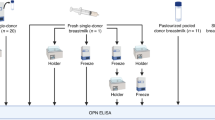
The susceptibility of milk-borne rEpo to degradation was evaluated using neonatal gastric secretions in an in vitro simulation of neonatal digestion as described by Kling et al. (1). Simulations were run for 0, 1, and 2 h, as maximal gastric acid proteolytic activity occurs at 1 h and stomach emptying is generally complete between 1 and 2 h (14, 15). Three incubation buffers were used in standard reaction mixtures:1) 0.1 M glycine at pH 3.2 (preprandial gastric conditions);2) 0.1 M maleate at pH 5.8 (postprandial gastric conditions); and 3) 0.01 M Tris 6.7 mM CaCl2 at pH 7.4 (proximal small intestinal conditions). Fifty microliters of buffer was preincubated with 50 μL of pooled and cleared neonatal gastric secretions for 15 min at 37°C. Fifty microliters of substrate spiked with rEpo was added and incubated at 37°C (final concentration of rEpo, 400 mU/mL). The substrates were 1) the aqueous fraction of preterm (n = 3) or term human milk (n = 4), 2) whole milk from mothers of preterm (n = 3) or term infants (n = 4), 3) commercially prepared infant formula (n = 8) (Enfamil, Mead Johnson Nutritionals; Similac, Ross Laboratories), or 4) 5% dextrose in water (D5W), n = 6. At the end of incubations, samples were immediately assayed for Epo by specific ELISA.
Statistical Considerations
Spearman rank correlations were used to examine linear and nonlinear associations between Epo concentrations in milk, Epo concentrations in serum, time postpartum, gestational age, and protein concentration. Variables measured repeatedly within a subject were averaged for the correlation analysis. A mixed-model ANOVA was used to compare fore, mid, and hind milk and to compare the aqueous phase, lipid phase, and a matched aliquot of whole milk. The study design called for a sample size of n = 20 to detect a Spearman rank correlation of 0.60 or smaller from 0 at 0.80 power, alpha = 0.05 using a 2-sided test. All other analyses were considered exploratory in nature. The mean ± SD was used as the summary descriptive measure. All tests were 2-sided and tested at level alpha = 0.05.
RESULTS
Forty-four women donated a total of 103 milk samples. Fourteen women donated more than one sample, and two donated more than three samples. Nine women delivered infants of less than or equal to 35 wk gestation, four were treated with terbutaline or magnesium sulfate, 15 received Pitocin, and four received antibiotics before delivery for the diagnosis of chorioamnionitis.
Epo concentrations in milk increased with time postpartum, whereas serum Epo concentrations were highest in the immediate postpartum period (Fig. 1). Time postpartum was positively correlated with Epo concentrations in milk (r = 0.72, p < 0.0001) and negatively correlated with serum Epo concentrations (r = −0.44, p = 0.008) and protein concentration (r = −0.70, p < 0.0001). A negative correlation was noted between Epo concentrations in milk and Epo concentrations in serum (r = −0.55, p = 0.0006) and protein concentration (r = −0.60, p < 0.0001). This association is nonlinear (Fig. 2). When the thirty-nine milk samples obtained within the first week of life were evaluated, we observed no correlation between gestational age (range, 24 to 41 wk of gestation) and milk Epo concentration (r = 0.27, p = 0.094).
Milk and serum Epo concentrations as a function of time postpartum. Epo concentrations are plotted on the y axis with days postpartum plotted on the x axis. The x axis is a logarithmic scale. Milk Epo concentrations, shown by open circles, are positively correlated with time postpartum (r = 0.72, p < 0.0001). Serum Epo concentrations, shown by filled triangles, are negatively correlated with time postpartum (r = −0.44, p = 0.008).
Do milk Epo concentrations correlate with serum Epo or milk protein concentrations? (A) Milk Epo concentrations (mU/mL) plotted on the y axis with serum Epo concentrations (mU/mL) shown on the x axis. A negative correlation is present between milk and serum Epo concentrations (r = −0.55, p = 0.0006). (B) Milk Epo concentrations plotted on the y axis with milk protein concentrations (mg/mL) shown on the x axis. A negative correlation is present between milk and protein concentrations (r = −0.6, p < 0.0001).
To determine whether a particular fraction or phase of milk was enriched in Epo, we measured Epo concentrations in fore, mid, and hind milk fractions and in whole milk versus aqueous and lipid phase milk. Ten samples of fore, mid, and hind milk were studied. These were obtained from women who delivered at gestational ages ranging from 27 wk to term. The time postpartum at which the milk samples were obtained ranged from 5 to 484 d. Thus, the postconceptional age at which the milk was provided ranged from 32 to 105 wk. There was no enrichment of Epo in any fraction (p = 0.17). These data are shown in Table 2. When Epo concentrations were measured in the aqueous and lipid phases of milk and compared with the concentration in a matched aliquot of whole milk, no significant differences were found (p = 0.36).
We next sought Epo immunoreactivity in lactating breast tissue. Figure 3A shows Epo immunoreactivity in a biopsy of a lactating woman 2 d after term delivery. Mammary duct epithelial cells are strongly immunoreactive (brown staining). When nonlactating breast tissue is compared, only weak immunoreactivity is noted (Fig. 3D). We examined samples of breast tissue at several points during gestation (see Table 1) and found that Epo immunoreactivity increased as term gestation approached. Epo-R immunoreactivity was also examined in all tissue samples. Weak to moderate immunoreactivity with anti-Epo-R antibody was observed in the epithelial duct cells of all breast tissues tested and did not change significantly with gestational age or the presence or absence of lactation.
Immunohistochemistry of lactating and nonlactating breast tissue. The upper panel shows breast tissue from a lactating woman compared with nonlactating breast tissue in the bottom panel. All photos were taken at ×400 original magnification. Panels A and D show Epo immunoreactivity (brown staining) present in the mammary tubular epithelial cells. Panels B and E show Epo-R immunoreactivity. Panels C and F are negative controls.
Because the tubular epithelial cells were positive for both Epo-R and Epo immunoreactivity, we sought to determine whether the cells actually expressed Epo or whether the observed immunoreactivity was due to binding of milk-borne Epo to epithelial cell Epo-R. We cultured HMEC to determine whether they expressed Epo and Epo-R mRNA and protein. Figure 4 shows reverse transcription PCR results, demonstrating expression of both Epo and Epo-R mRNA in all conditions tested. When HMEC grown in chamber slides were immunostained using antibodies to Epo and Epo-R, immunoreactivity was noted in all conditions with no detectable differences between conditions (data not shown). Epo concentration in spent media from these cultured HMEC ranged from 0.2 to 2.9 mU/mL (n = 4). Western analysis of HMEC cells for the presence of Epo and Epo-R was also positive, showing bands specific for Epo (Fig. 5A) and Epo-R (Fig. 5B).
Reverse transcription PCR (RT-PCR) of mammary epithelial cells. This Figure shows a representative ethidium bromide-stained 2% wt/vol agarose gel showing RT-PCR cDNA fragments for Epo, Epo-R, and β-actin from nontransformed HMEC. Lanes 1 and 7 show a 100-bp ladder as a molecular-weight marker. Lanes 2–4 show RT-PCR fragments amplified from HMEC cultured in the presence of control conditions (2), IGF-1 (10 ng/mL) (3), or hypoxia for 24 h (4). Lane 5 shows fetal liver, the positive control, and lane 6 shows the negative control, RNA that was not reverse transcribed.
Western analysis of Epo and Epo-R expression by HMEC. (A) Shows Epo immunoprecipitation followed by Western analysis of HMEC lysate. Lane 1 shows recombinant Epo (∼40 kD). Lanes 2 and 3 show control HMEC cells and those grown in the presence of IGF-1. (B) Shows Western analysis of HMEC grown in control conditions (lane 1) and in the presence of IGF-1 (lane 2) and hypoxia (lane 3).
To determine whether a difference in glycosylation occurs in the processing of milk Epo compared with circulating Epo, we evaluated Epo size by Western analysis as shown in Figure 6. No size difference was noted.
Milk Epo vs serum Epo size by Western analysis. Samples were electrophoresed into a 3.5% stacking gel, resolved on a 16.5% Tris-Tricine gel, and then transferred to a PVDF membrane. Lane 1 contains the reference ladder. Lane 2 shows rEpo (∼40 kD) used as a positive antibody control. Serum Epo is compared with milk Epo from two different milk samples in lanes 3–5.
The stability of rEpo in human milk, infant formula, and glucose water was evaluated using simulated preprandial, postprandial, and small bowel conditions. Figure 7 shows the comparison of such digestions when rEpo was added to human milk, to commercially available infant formula, or to D5W. All human milk digestions were considered together, as no differences were noted between the milk from women who had delivered preterm versus term nor in aqueous phase versus whole milk. The importance of digestion condition (preprandial, postprandial, and small bowel), solution type (breast milk, infant formula, and D5W), and time (1 and 2 h) was evaluated by ANOVA, and all three factors were significant (p < 0.0001 for each).
Epo digestions in human milk, formula, and D5W. In the top panel, the percent of spiked rEpo remaining after simulated digestions (y axis is shown in human milk) (n = 14). The middle panel shows similar digestions with rEpo spiked into infant formula (n = 8). The bottom panel shows digestions carried out in D5W (n = 6). The x axis shows digestive conditions and the length of the digestion (1 vs 2 h). The top, bottom, and line through the middle of the box plot show the 75th, 25th, and 50th percentile (median), respectively. The whiskers on the bottom extend from the 10th to the 90th percentile. Mean values for each group are denoted by the filled square. ★p < 0.0001 compared with digestion in human milk.
Epo stability in milk was also evaluated by measuring Epo concentrations (spiked and endogenous) in individual samples of human milk and comparing it with rEpo spiked into glucose water under conditions of repeated freeze/thaw cycles and heating. We found Epo to be stable with an insignificant decrease after six freeze/thaw cycles. Heating rEpo in human milk to 60°C for 1 or 5 min did not appreciably decrease the Epo concentration; however, if rEpo was similarly heated in D5W, essentially all was degraded.
DISCUSSION
Our overall hypothesis was that the presence of Epo in human milk is the result of an active process. We postulated that if the patterns of Epo concentration in milk and serum differed as time postpartum progressed, this would support our hypothesis. We further postulated that if milk-borne Epo was higher than serum Epo, this would suggest that Epo is actively concentrated or secreted into milk. To address this, we determined Epo concentrations in milk as a function of time postpartum and compared milk-borne Epo concentrations to Epo measured in paired serum samples.
We found milk and serum Epo concentrations to be discordant, with milk Epo concentrations increasing whereas serum Epo concentrations decreased with time postpartum. Thus, early in the postnatal course, serum Epo concentrations were generally higher or the same as milk Epo concentrations, but, by 2 to 3 mo after birth, milk Epo concentrations were considerably higher than paired serum samples. This suggests that Epo can be actively secreted or concentrated into milk.
Western analysis of Epo in milk and serum Epo was done to determine whether any differences in their apparent size were detectable. It has been previously reported that the biologically active Epo expressed in rabbit milk has a higher specific activity than that reported for rabbit serum Epo, suggesting differences in the glycosylation pattern; however, we found no such size difference in Epo isolated from human milk compared with serum (16).
To determine whether mammary cells may be a possible source of milk Epo, we studied breast biopsy specimens of lactating and nonlactating women by using anti-Epo and anti-Epo-R antibodies. We found robust Epo immunoreactivity on mammary tubule epithelial cells from lactating breast tissue, with less reactivity noted during gestation and in nonlactating breast. Weak Epo-R immunoreactivity was present on mammary duct epithelial cells regardless of its lactational state. Unfortunately, mRNA quantitation or localization (in situ hybridization) of Epo expression in these biopsy specimens was not possible.
To further test the capacity of mammary epithelial cells to express Epo, we investigated nontransformed HMEC in vitro and found that these cells expressed both the mRNA and protein for Epo and its receptor in all conditions tested. Expression of Epo and its receptor was not appreciably changed by the culture conditions selected at the time interval investigated (17). Although we did not identify factors that regulate Epo expression by cultured mammary epithelial cells, we speculate that such regulation occurs in vivo as we observed a qualitative difference between Epo immunoreactivity as pregnancy and lactation progressed, and Epo concentrations in milk increased over time postpartum during a time in which serum Epo concentrations decreased. This suggests that the control of Epo expression is a more complex interaction. Although beyond the scope of this article, investigation into the regulation of milk Epo secretion merits further study.
To produce an effect in the neonate, orally administered Epo must resist degradation by the GI environment. Kling et al. (1) demonstrated the presence of Epo in human milk and that a proportion of this Epo remains intact after exposure to pre- and postprandial conditions as well as to conditions typically found in the small bowel. Using comparable conditions but measuring remaining Epo by ELISA rather than RIA, we showed variable resistance to degradation with Epo preservation being highest in human milk. As the Epo ELISA only tests for Epo immunoreactivity, the functionality of the remaining Epo cannot be commented on, and, therefore, the biologic effects are speculative. The conditions used for our experiments certainly overestimate the degradative conditions present during normal feeding, because it would be unlikely that when at full feeding volume, the Epo contained in milk (or formula) would be exposed to an equal volume of gastric juice as occurred in these experiments.
In the present study, we confirmed the presence of Epo in human milk, established that secretion of Epo into milk is likely to be an active process in the late postpartum period, and showed that HMEC express both Epo and its receptor in vivo and in vitro. The question remains, what is the function of Epo in milk?
One possible role for the increase in milk Epo with duration of lactation may be to preserve lactation. This association of Epo with reproductive function would not be unprecedented, as Epo is speculated to have a role in the regulation of the cyclic changes of the uterine endometrium (18). The cyclic changes in the endometrium are regulated primarily by 17-β-estradiol. In addition to its other effects, 17-β-estradiol increases uterine Epo protein and mRNA synthesis, which in turn promote blood vessel formation in the endometrium, an effect that can be blocked by soluble Epo-R (18). No studies have been published regarding a possible role of Epo with lactation, but the presence of the Epo-R suggests a specific role for Epo in the breast.
Other possible functions of milk Epo include effects in the neonate. These may include systemic absorption of Epo after Epo-R binding with subsequent erythropoietic activity, or, alternatively, Epo could have local effects on enterocytes. The data regarding the erythropoietic effects of Epo after enteral administration are ambiguous. An increase in erythropoiesis in nursing rat pups has been observed after maternal phlebotomy, suggesting that Epo may be transmitted through mother's milk in rodents, although in those studies, Epo concentrations in the milk or in the pups were not measured (7, 8, 19). Pilot studies from our laboratory have not demonstrated enteral absorption after enteral dosing of 1000 U·kg−1·d−1 rEpo but have demonstrated significant local trophic effects (9, 20). Two studies testing oral administration of rEpo to human infants have been published. The first, a pilot study of six premature infants treated orally with 1000 U/kg rEpo for 10 d, demonstrated no increase in hematocrit or reticulocyte count and showed only a small increase in circulating Epo concentrations 2 h after the dose but at no other time points (10). In contrast, a study of six infants who received enteric rEpo (600 U·kg−1·wk−1 given three times a week from study entry until discharge) compared with six who did not suggested that enteric Epo resulted in increased erythropoiesis. However, Epo concentrations were not measured in these infants (11). It is possible that Epo is not absorbed but influences erythropoiesis indirectly via local effects in the bowel, such as by increasing iron absorption. More studies are needed to clarify this issue.
In conclusion, we confirmed that Epo is present in human milk and established that secretion of Epo into milk is likely to be an active process in the late postpartum period and that HMEC express Epo in vivo and in vitro. Although the function of milk-borne Epo in the neonate's GI tract is not known, we have demonstrated that ingested Epo can survive conditions present in the pre- and postprandial gut.
Abbreviations
- Epo:
-
erythropoietin
- Epo-R:
-
erythropoietin receptors
- GI:
-
gastrointestinal
- HMEC:
-
human mammary epithelial cells
- rEpo:
-
recombinant erythropoietin
References
Kling PJ, Sullivan TM, Roberts RA, Philipps AF, Koldovsky O 1998 Human milk as a potential enteral source of erythropoietin. Pediatr Res 43: 216–221
Juul SE, Yachnis AT, Christensen RD 1998 Tissue distribution of erythropoietin and erythropoietin receptor in the developing human fetus. Early Hum Dev 52: 235–249
Juul SE, Joyce AE, Zhao Y, Ledbetter DJ 1999 Why is erythropoietin present in human milk? Studies of erythropoietin receptors on enterocytes of human and rat neonates. Pediatr Res 46: 263–268
Okada A, Kinoshita Y, Maekawa T, Hassan MS, Kawanami C, Asahara M, Matsushima Y, Kishi K, Nakata H, Naribayashi Y, Chiba T 1996 Erythropoietin stimulates proliferation of rat-cultured gastric mucosal cells. Digestion 57: 328–332
Clapp JF III, Little KD, Appleby-Wineberg SK, Widness JA 1995 The effect of regular maternal exercise on erythropoietin in cord blood and amniotic fluid. Am J Obstet Gynecol 172: 1445–1451
Richey SD, Ramin SM, Bawdon RE, Roberts SW, Dax J, Roberts J, Gilstrap LC 1995 Markers of acute and chronic asphyxia in infants with meconium-stained amniotic fluid. Am J Obstet Gynecol 172: 1212–1215
Carmichael RD, LoBue J, Gordon AS 1992 Neonatal erythropoiesis. I. Peripheral blood erythropoietic parameters: data suggest erythropoietin transfer via maternal milk. Endocr Regul 26: 83–88
Carmichael RD, LoBue J, Gordon AS 1992 Neonatal erythropoiesis. II. Bone marrow and splenic erythropoietic activity: data suggest erythropoietin transfer via maternal milk. Endocr Regul 26: 143–149
Juul SE, Ledbetter DJ, Joyce AE, Zhao Y, DeMarco V 1999 Why is erythropoietin in mothers milk? Is it enterally absorbed?. Pediatr Res 45: 156Aabstr
Britton JR, Christensen RD 1995 Enteral administration of recombinant erythropoietin to preterm infants. J Perinatol 15: 281–283
Ballin A, Bilker-Reich A, Arbel E, Davidovitz Y, Kohelet D 1999 Erythropoietin, given enterally, stimulates erythropoiesis in premature infants. Lancet 353: 1849
Juul SE, Anderson DK, Li Y, Christensen RD 1998 Erythropoietin and erythropoietin receptor in the developing human central nervous system. Pediatr Res 43: 40–49
Martin VV, Nock S, Meyer-Gauen G, Hager KP, Jensen U, Cerff R 1993 A method for isolation of cDNA-quality mRNA from immature seeds of a gymnosperm rich in polyphenolics. Plant Mol Biol 22: 555–556
Lebenthal E, Siegel M 1985 Understanding gastric emptying: implications for feeding the healthy and compromised infant. J Pediatr Gastroenterol Nutr 4: 1–3
Yahav J, Carrion V, Lee PC, Lebenthal E 1987 Meal-stimulated pepsinogen secretion in premature infants. J Pediatr 110: 949–951
Rodriguez A, Castro FO, Aguilar A, Ramos B, Del Barco DG, Lleonart R, De la Fuente J 1995 Expression of active human erythropoietin in the mammary gland of lactating transgenic mice and rabbits. Biol Res 28: 141–153
Okajima Y, Matsumura I, Nishiura T, Hashimoto K, Yoshida H, Ishikawa J, Wakao H, Yoshimura A, Kanakura Y, Tomiyama Y, Matsuzawa Y 1998 Insulin-like growth factor-I augments erythropoietin-induced proliferation through enhanced tyrosine phosphorylation of STAT5. J Biol Chem 273: 22877–22883
Yasuda Y, Masuda S, Chikuma M, Inoue K, Nagao M, Sasaki R 1998 Estrogen-dependent production of erythropoietin in uterus and its implication in uterine angiogenesis. J Biol Chem 273: 25381–25387
Carmichael RD, Gordon AS, Lobue J 1986 Effects of the hormone erythropoietin in milk on erythropoiesis in neonatal rats. Endocrinol Exp 20: 167–188
Juul SE, Zhao Y, Dame C 2000 The effects of enteral versus parenteral recombinant erythropoietin on bowel growth. Pediatr Res 47: 971Aabstr
Acknowledgements
The authors thank Dr. Raymond Hackett for his assistance in obtaining and interpreting the breast biopsy specimens and General Clinical Research Center Scatterbed nurses Pam Connolly and Ann Cothran for their assistance in obtaining milk, blood, and gastric juice specimens.
Author information
Authors and Affiliations
Additional information
Supported by CAP award RR-00082 from the National Institutes of Health and by a grant from the Children's Miracle Network.
Rights and permissions
About this article
Cite this article
Juul, S., Zhao, Y., Dame, J. et al. Origin and Fate of Erythropoietin in Human Milk. Pediatr Res 48, 660–667 (2000). https://doi.org/10.1203/00006450-200011000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200011000-00018
This article is cited by
-
Robust increases in erythropoietin production by the hypoxic fetus is a response to protect the brain and other vital organs
Pediatric Research (2018)
-
Increased yet iron-restricted erythropoiesis in postpartum mothers
Annals of Hematology (2012)
-
Erythropoietin modulates the neural control of hypoxic ventilation
Cellular and Molecular Life Sciences (2009)