Abstract
Intestinal epithelial (Caco-2) cells secrete the chemokine, IL-8, after stimulation with IL-1β, but not after lipopolysaccharide. Butyrate is a short chain fatty acid derived from the metabolism of intestinal contents by gut bacteria. Butyrate concentrations reflect, therefore, the bacterial microenvironment established within the intestine. We hypothesized that butyrate may alter the secretion of IL-8 by intestinal epithelial cells in response to stimulation by IL-1β or lipopolysaccharide. Caco-2 cells were incubated in varying concentrations of sodium butyrate (0-20 mM) for 24 h before stimulation with lipopolysaccharide or IL-1β. IL-8 secretion was measured over 24 h by ELISA. IL-8 mRNA accumulation was detected by Northern blots. Lipopolysaccharide induced the secretion of IL-8 only after Caco-2 cells cells had been cultured with sodium butyrate. Furthermore, butyrate significantly enhanced IL-8 secretion by cells stimulated with IL-1β. Butyrate also increased IL-8 mRNA accumulation in stimulated Caco-2 cells. Intestinal epithelial cells can, therefore, be primed by butyrate to become activated by lipopolysaccharide and proinflammatory cytokines. This may represent a mechanism by which intestinal epithelial cells can regulate intestinal inflammation in response to changes in the intestinal milieu.
Similar content being viewed by others
Main
The intestinal epithelium is continuously exposed at the epithelial cell's apical surface to luminal factors, including nutrients and bacterial products. The epithelial cell is also in contact at its basolateral surface with cytokines secreted by cells in the intestinal mucosa. Although the primary role of the epithelium is the absorption of nutrients, it also acts as a protective barrier for the host against infectious agents, toxins, and antigens within the intestinal lumen(1, 2). Mucosal immune responses play a central role in epithelial defensive mechanisms that are mediated, in part, by secretory IgA. In addition, intestinal epithelial cells secrete IL-1, IL-6, tumor necrosis factor-α, IL-10(2), and chemotactic cytokines (chemokines), including IL-8(3–6).
IL-8 is an α-chemokine with a molecular weight of 8-10 kD. IL-8 possesses potent neutrophil chemoattractant and activating properties(7, 8). It is secreted by granulocytes, endothelial cells, fibroblasts, T cells, keratinocytes, monocytes/macrophages(7), and by intestinal epithelial cells(3–6). IL-8 is increased in the mucosa of patients with both active ulcerative colitis and active Crohn's disease(5, 9).
Intestinal epithelial cells may, by secreting chemokines, participate in the attraction of leukocytes into the intestinal mucosa(2–6). The question arises, therefore, whether the intestinal milieu regulates this epithelial participation. The short chain fatty acids, acetate, propionate, and butyrate, are the products of bacterial fermentation of carbohydrate(10–12). We hypothesized, therefore, that factors in the lumen, such as short chain fatty acids, may alter the production of IL-8 by epithelial cells. Thus, butyrate may not only be an energy source for colonocytes(13), stimulating epithelial cell proliferation in vivo(14), but it may also carry information on the bacterial ecosystem to the intestinal epithelium. The concentration of butyrate varies from 5 mM(15) to 24 mM(16) in the normal large intestine.
We examined whether sodium butyrate altered the secretion of IL-8 by epithelial cells stimulated with proinflammatory molecules. Lipopolysaccharide, a component of the outer membrane of Gram-negative bacteria, by itself does not stimulate IL-8 secretion by Caco-2 cells(3). However, it does stimulate IL-1β production from macrophages(17). We, therefore, also examined whether IL-1β could act in synergy with butyrate to alter IL-8 secretion by intestinal epithelial cells. Our studies demonstrate that changes in butyrate concentrations are directly associated with changes in chemokine secretion by epithelial cell line cells stimulated with lipopolysaccharide or IL-1β.
METHODS
Culture of Caco-2 cell or H-4 cell monolayers. Caco-2 cells constitute a cell line derived from human colon carcinoma which differentiates spontaneously in culture(18–20). The H-4 cell line is a nonmalignant human small intestinal epithelial cell clone derived from human fetal small intestine(21). Caco-2 cells (American Type Culture Collection, Rockville, MD, passages 20-40) and H-4 cells (passages 20-36) were plated into 12-well plates (Falcon, Becton Dickinson, Franklin Lakes, NJ) at an initial density of 5 × 104 cells/cm2. Both Caco-2 cells and H-4 cells were grown in DMEM(GIBCO-Life Technologies, Inc., Grand Island, NY) containing FCS (Hyclone Laboratories, Logan, UT), 2 mM glutamine (GIBCO), 100,000 U/L penicillin, and 100 mg/L streptomycin (GIBCO), 0.1 mM minimal essential medium nonessential amino acid solution (GIBCO), and 10 mM HEPES buffer solution (GIBCO) in a humid atmosphere at 37°C and 5% CO2.
On d 7 after plating, the media were changed from media containing serum to media without serum (DTS). DTS medium was DMEM (GIBCO) supplemented with 5 mg/L iron-saturated human transferrin (Sigma Chemical Co., St. Louis, MO) and 5 μg/L selenous acid (Na2SeO3; Collaborative Biomedical, Bedford, MA) but contained no serum(22). Caco-2 cells grow and differentiate normally in DTS medium(22). Experimental protocols were initiated on d 14, when cells were confluent and their state of differentiation stable.
Protocol of incubation with butyrate and stimulation with IL-1β or lipopolysaccharide. IL-8 secretion by intestinal epithelial cells in media containing both sodium butyrate and lipopolysaccharide or IL-1β. Caco-2 cells or H-4 cells were incubated with varying concentrations of butyrate (0-20 mM) (Sigma Chemical Co.) in DTS media (without serum) for 48 h. No changes in the pH of the media were observed with the addition of butyrate. The epithelial cells were stimulated with 100 μg/mL lipopolysaccharide (from Escherichia coli serotype 055:85, Sigma Chemical Co.) or 1 ng/mL IL-1β (R&D Systems, Minneapolis, MN) during the last 24 h. Further experiments were performed to examine IL-8 mRNA accumulation within Caco-2 cells preincubated with 20 mM sodium butyrate for 24 h and subsequently stimulated for 2 h with 1 ng/mL IL-1β or 100 μg/mL lipopolysaccharide.
Dose response to lipopolysaccharide or IL-1β. Caco-2 cells were incubated with and without sodium butyrate (5 mM) for 48 h. After 24 h, cells were stimulated with varying concentrations of lipopolysaccharide (0-100μg/mL) or IL-1β (0-100 ng/mL) for a further 24 h.
Time course of IL-8 secretion. Caco-2 cells were incubated with and without sodium butyrate (20 mM) for 0, 12, 24, 26, and 30 h. After 24 h, cells were stimulated with IL-1β (1 ng/mL), for 2 h and for 6 h. Supernatants, Caco-2 cell proteins and Caco-2 cell RNA from the same wells were collected at the different time points described.
Sequential media exchange experiments. Cells were preincubated with sodium butyrate (0-20 mM) for 24 h, then washed twice with DTS media. Fresh DTS media without butyrate were placed into the wells followed by addition of lipopolysaccharide (100 μg/mL) or IL-1β (1 ng/mL) for a further 24 h. In these sequential media exchange experiments, butyrate and lipopolysaccharide or IL-1β were not present concurrently.
Assay of IL-8 secretion and mRNA accumulation . Measurement of IL-8 secretion. IL-8 levels were measured in cultured supernatants by ELISA (Quantikine™ R&D Systems). The culture supernatants from Caco-2 cells or H-4 cells were collected, centrifuged at 800 rpm, and stored frozen at -20°C. The amount of IL-8 was quantified within each supernatant in duplicates. The maximum variation between duplicates was 2%. Colorimetric results were read on a Titertek Multiscan II 96-well plate reader at a wavelength of 450 nm.
Measurement of total Caco-2 or H-4 cell protein. The cell protein content was measured to express IL-8 production per unit weight of cellular material. Deionized water was placed into wells containing adherent Caco-2 cells or H-4 cells to detach the cells. They were immediately sonicated with an ultrasonic cell disrupter (micro-ultrasonic cell disrupter; Kontes, Vineland, NJ). The amount of total protein was then measured with the bicinchonic acid protein assay (BCA; Pierce, Rockford, IL). Colorimetric results were read on a DU-70 spectrophotometer (Beckman Instrument Inc., Wakefield, MA) at a wavelength of 562 nm and converted into protein concentration using an albumin standard calibration curve. The protein content within each well was measured in duplicates with an experimental variation of less than 5%.
Caco-2 cell mRNA collection. Caco-2 cells were cultured in the presence or absence of butyrate for 24 h followed by lipopolysaccharide or IL-1β for 2 h. Caco-2 cells were homogenized, and the RNA was extracted, precipitated, washed, and collected according to the manufacturer's recommendations as described in the procedures for RNA isolation in the RNAzol kit (Biotecx Laboratories, Inc., Houston, TX).
RNA transfer blot analysis of Caco-2 cell mRNA. Purified total RNA (30 μg) from each well was separated by electrophoresis in a 2% agarose gel containing 1.8% formaldehyde (Mallinckrodt, Paris, KY) and 20% 3-[N-Morpholino]propane sulfonic acid (Sigma Chemical Co.) and transferred to Gene-Screen Plus™ membranes (Dupont NEN, Boston, MA) by capillary action. The membranes were then baked, prehybridized, hybridized with labeled IL-8 cDNA (a gift from Dr. Joost Oppenheim, Laboratory of Molecular Immunoregulation, NCI-FCRPC, Fredrick, MD). Blots were washed in 0.5× SSC and 0.5% SDS (Bio-Rad Laboratories, Hercules, CA) at 65°C. Washed blots were analyzed by autoradiography between intensifying screens at-70°C as previously described(23).
Polarity of IL-8 secretion by Caco-2 cells. Caco-2 cells were grown on 12-mm cell culture inserts with a 0.45-μm pore size (Falcon). The change from normal media to serum-free (DTS) media was made on d 19. Confluency of Caco-2 cell monolayers in the culture inserts was confirmed by measuring transepithelial electrical resistance using a Millicell-ERS system(Millipore Corporation, Bedford, MA) on d 21. Sodium butyrate (0, 2.5, and 5 mM) was then added into both the upper and lower compartments of the inserts for 24 h, and lipopolysaccharide (100 μg/mL) was added into the upper compartments for a further 24 h. Culture supernatants were then collected, and IL-8 was measured (as described above).
Statistics. Statistical significance of the differential effects of sodium butyrate on IL-8 secretion was assessed by regression analysis. Each point entered into the data represented a separate well. Statistical differences between controls and the lowest butyrate concentrations (2.5 mM) were also examined using the t test. p values of less than 0.05 were considered statistically significant.
RESULTS
Butyrate induces Caco-2 cells to secrete IL-8 in response to lipopolysaccharide. Caco-2 cells did not secrete IL-8 when stimulated with lipopolysaccharide (100 μg/mL). This confirmed previous reports showing a lack of response of Caco-2 cells to lipopolysaccharide(3). However, when Caco-2 cells were incubated with sodium butyrate, lipopolysaccharide stimulated IL-8 secretion (Fig. 1). Furthermore, the IL-8 production increased with increasing concentrations of sodium butyrate (p < 0.001;Fig. 2). There was no plateau to this effect even at 100 mM (data not shown). There was a small, but nevertheless statistically significant, increase in IL-8 secretion (p < 0.001) by unstimulated cells incubated with sodium butyrate alone (Figs. 1 and 2). To ensure that there was no direct extracellular interaction between lipopolysaccharide and sodium butyrate, sequential media exchange experiments were performed removing butyrate completely from the culture medium before adding lipopolysaccharide. Sodium butyrate induced lipopolysaccharide responsiveness even after it had been removed before lipopolysaccharide stimulation (data not shown).
Sodium butyrate induces the secretion of IL-8 in Caco-2 cells stimulated with lipopolysaccharide (LPS). Only cells treated with sodium butyrate (5 mM) for 24 h responded to lipopolysaccharide. Concentrations greater than 1 μg/mL lipopolysaccharide stimulated IL-8 secretion. The bars represent standard deviations of three different wells for each point.
The effect of sodium butyrate on lipopolysaccharide(LPS)- or IL-1β-stimulated secretion of IL-8 by Caco-2 cells. Lipopolysaccharide at 100 μg/mL alone did not induce IL-8 secretion by Caco-2 cells, but in the presence of sodium butyrate added 24 h previously, lipopolysaccharide induced IL-8 production (p < 0.001). The magnitude of IL-8 secretion was dependent on the concentration of sodium butyrate (p < 0.001). Sodium butyrate alone induced Caco-2 cells secretion of IL-8 but to a limited extent. Sodium butyrate also enhanced the secretion of IL-8 by Caco-2 cells stimulated with IL-1β (1 ng/mL). The bars represent standard deviations of three different wells for each point. The results are representative of five experiments.
The effects of sodium butyrate were compared with equimolar concentrations of sodium bicarbonate, another weak base, to exclude the possibility that the effects of sodium butyrate may have been due to any alteration in the charge of lipopolysaccharide in the media, or of proteins at the cell membrane. Unlike sodium butyrate, sodium bicarbonate did not induce IL-8 production by Caco-2 cells stimulated with lipopolysaccharide (data not shown). Furthermore, alterations in the concentration of glutamine (a recognized epithelial nutrient) had no effect on IL-8 secretion. Thus, the effect of sodium butyrate on lipopolysaccharide induction of IL-8 secretion by Caco-2 cells was due to the butyrate moiety itself.
Butyrate enhances IL-1β stimulation of IL-8 secretion by Caco-2 cells. The cells of the intestinal epithelium are directly exposed not only to bacterial products from the lumen but also to proinflammatory cytokines from immune cells in the lamina propria that are activated during inflammation. The effect of sodium butyrate on IL-1β stimulation of IL-8 secretion by Caco-2 epithelial cell line cells was, therefore, examined. In contrast to the effects of lipopolysaccharide, IL-1β stimulated IL-8 production by Caco-2 cells in the absence of sodium butyrate as has been previously shown by others(3). However, sodium butyrate markedly enhanced IL-8 secretion by Caco-2 cells when stimulated by IL-1β (p < 0.001; Fig. 2).
The dose-response curve of IL-8 secretion by Caco-2 cells after stimulation with varying concentrations of IL-1β showed a peak IL-8 production at a concentration of 1 ng/mL IL-1β (Fig. 3). This concentration of IL-1β also induced a maximal response in cells incubated with 5 mM sodium butyrate. However, butyrate increased the response of IL-8 secretion to IL-1β at this and every other concentration of IL-1β tested (Fig. 2). Sodium bicarbonate had no effect on IL-8 production by Caco-2 cells stimulated with IL-1β, again demonstrating that butyrate's effects were not due to its being a weak base. In addition, in sequential media exchange experiments, sodium butyrate enhanced the responsiveness of cells to IL-1β stimulation, even though it was not present concurrently with IL-1β in the medium (data not shown). Butyrate did not, therefore, interact with IL-1β in the media, but acted instead by upregulating IL-8 synthesis within the cell.
Sodium butyrate enhances the secretion of IL-8 by Caco-2 cells. IL-8 secretion increased with increasing doses of IL-1β(0-100 ng/mL) for 24 h with a peak IL-8 secretion at 1 ng/mL IL-1β. At every concentration of IL-1β, 5 mM sodium butyrate enhanced the secretion of IL-8 by Caco-2 cells. The bars represent standard deviations of three different wells for each point. The results are representative of two experiments.
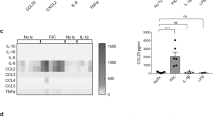
Similar effects on the secretion of another chemokine, such as GRO-α, by Caco-2 epithelial cells were observed when cells were stimulated with IL-1β and sodium butyrate. IL-1β stimulated GRO-α secretion by Caco-2 cells in the absence of sodium butyrate. This secretion was further enhanced when cells were preincubated with sodium butyrate and then stimulated with IL-1β (Table 1).
Butyrate enhances Caco-2 cell accumulation of IL-8 mRNA. Treatment with lipopolysaccharide alone did not induce IL-8 mRNA except when cells had been treated with sodium butyrate (Fig. 4). IL-1β stimulation induced IL-8 mRNA in the absence of sodium butyrate. However, the amount of IL-8 mRNA was increased by incubation with sodium butyrate (Fig. 4). This effect was dose-dependent (data not shown). In unstimulated cells, IL-8 mRNA was discernible in cells incubated with 20 mM sodium butyrate (Fig. 4), but could not be detected by Northern blot analysis at concentrations below this.
Sodium butyrate (20 mM) enhanced IL-8 mRNA accumulation in Caco-2 cells in response to stimulation with lipopolysaccharide(LPS) (100 μg/mL) or IL-1β (1 ng/mL). Caco-2 cell RNA (30μg) was electrophoresed in each lane and probed with an IL-8 cDNA. The upper panel shows hybridization of IL-8 cDNA to RNA. The membrane was reprobed with glyceraldehyde-3-phosphate dehydrogenase (GAPDH) cDNA (lower panel) showing equivalent loading of total RNA. Sodium butyrate enhanced IL-8 accumulation in Caco-2 cells in response to stimulation with lipopolysaccharide or IL-1β. The results are representative of five experiments.
IL-8 mRNA accumulation in Caco-2 cells was detected 2 h after stimulation with 1 ng/mL IL-1β (Fig. 5). IL-8 mRNA was greater when the Caco-2 cells had been incubated with 20 mM sodium butyrate for 24 h (Fig. 5). IL-8 mRNA was no longer detectable 6 h after IL-1β stimulation whether or not cells had been incubated in butyrate. The increase in IL-8 mRNA, induced by butyrate, was associated with greater secretion of IL-8 in Caco-2 cells (p < 0.05). Unlike mRNA, IL-8 secretion continued to rise even at 6 h after incubation with IL-1β whether or not cells received butyrate.
The time course of IL-8 mRNA accumulation and IL-8 secretion by Caco-2 cells after stimulation with IL-1β. The secretion of IL-8 (upper panel) and accumulation of IL-8 mRNA (lower panel) were examined in the same cells. Sodium butyrate (20 mM) was given 24 h (-24 h) before stimulation with IL-1β (1 ng/mL) at time 0. Higher IL-8 mRNA production resulted in greater secretion of IL-8 protein in Caco-2 cells. IL-8 protein secretion continued after IL-8 mRNA production in Caco-2 cells. Each lane contained equal amounts of RNA.
Butyrate induces nonmalignant human intestinal epithelial cells(H-4 Cells) to secrete IL-8 in response to IL-1 β stimulation. Caco-2 cells are derived from intestinal cancer cells and thus, may have an aberrant gene expression which could possibly affect the regulation, synthesis, and secretion of IL-8. H-4 cells are nonmalignant human small intestinal epithelial cells cloned from normal human fetal small intestine(32). As in Caco-2 cells, butyrate enhanced the secretion of IL-8 by H-4 cells after stimulation with IL-1β(Fig. 6). Thus, the effects of butyrate on IL-8 secretion were not limited to epithelial cells that had undergone malignant transformation.
Sodium butyrate enhances IL-8 secretion by the nonmalignant human small intestinal epithelial cell line (H-4 cells) in response to IL-1β stimulation. Sodium butyrate induced IL-8 secretion by H-4 cells in response to 1 ng/mL IL-1β stimulation in a dose-dependent manner (p < 0.05, IL-1β vs 5 mM butyrate + IL-1β). The bars represent standard deviations of three different wells for each point. Results were representative of five experiments.
Butyrate induces bipolar IL-8 secretion by Caco-2 cells after stimulation with lipopolysaccharide . In vivo, the intestinal epithelium is a polarized cell monolayer which is constantly exposed to bacterial products, such as lipopolysaccharide, at its apical surface. To examine the effect of sodium butyrate on the polarity of IL-8 secretion by Caco-2 cells after lipopolysaccharide stimulation, Caco-2 cells were cultured in cell culture inserts suspended in media with or without butyrate in both compartments. Lipopolysaccharide (100 μg/mL) was then added into the apical compartment of the wells. Lipopolysaccharide alone had no effect on IL-8 secretion. In the presence of 2.5 mM sodium butyrate, IL-8 secretion was secreted from both apical and basal poles in response to lipopolysaccharide stimulation (Fig. 7). This secretion was further increased with 5 mM sodium butyrate (Fig. 7).
The effect of sodium butyrate on the polarity of IL-8 secretion by Caco-2 cells stimulated by lipopolysaccharide (LPS). Sodium butyrate induced Caco-2 cells to secrete IL-8 from both its apical and basolateral poles in response to apical lipopolysaccharide (100 μg/mL) stimulation. The bars represent standard deviations of three different wells for each point. Results were representative of four experiments.
DISCUSSION
The epithelium serves as a line of defense against an array of substances in the intestine, including resident and pathogenic microorganisms(1). There is now evidence that the intestinal epithelium is able to secrete a wide array of cytokines, including chemokines, which alter responses in the mucosal immune system(2–6). However, the evidence that the production of such molecules is regulated by events in the lumen of the intestine is sparse. It is known that invasive bacteria may induce the release of IL-8(4, 6, 24), but the possibility that epithelial cells respond to variations in the normal environment of the intestinal lumen is less well documented. Normal resident bacteria alter the fucosylated glycoconjugates on the epithelial cell surface(25). These alterations were due to a bacterial metabolite, as yet not identified. Our present data now demonstrate that a normal metabolic product of intestinal bacteria, sodium butyrate, significantly increases the secretion of IL-8 by intestinal epithelial cells. This effect of butyrate on IL-8 secretion is particularly marked when epithelial cells are also stimulated by the proinflammatory cytokine, IL-1β, or by the bacterial product, lipopolysaccharide. Thus, bacterial signals in the form of butyrate are translated into chemokine secretion by epithelial cells.
In the normal human large intestine, butyrate concentrations vary from 5 mM(15) to 24 mM(16); and in ileostomy effluents, the concentration of butyrate ranges between 0.1 and 16 mM(26). If butyrate is a normal constituent of the intestine, the question arises as to why in vivo intestinal epithelial cells are not continuously releasing IL-8. Such secretion would cause a continued state of inflammation in the normal intestine. The answer may lie in the observation that butyrate had little effect on IL-8 secretion by epithelial cells in the absence of a second signal, such as IL-1β or lipopolysaccharide. IL-1β is not secreted in appreciable quantities in the healthy intestine. Lipopolysaccharide concentrations reaching the apical membrane in health would also be low because of the mucous barrier. By contrast, in inflammatory conditions where butyrate concentrations are elevated, such as Crohn's disease(15) or necrotizing enterocolitis(27), there is appreciable IL-1β secretion, loss of the mucosal barrier, and large numbers of Gram-negative bacteria. Our data indicate that a small amount of IL-8 is, however, secreted by Caco-2 cells given high concentrations of butyrate without IL-1β or lipopolysaccharide. In healthy mice, high concentrations of butyrate instilled into the rectum do, in fact, cause inflammatory changes in the colon(28). The effects of butyrate in vivo are, therefore, consistent with its actions in vitro.
Caco-2 cells, although derived from colonic cancer cells, were chosen because they are a well established model for the human intestinal epithelium(18–20). We have used, in addition, a nonmalignant cell line (H-4 cells) derived from human fetal intestine(21) to confirm that our results could be reproduced in intestinal epithelial cells that have not undergone malignant transformation (Fig. 6).
The up-regulatory effects of sodium butyrate on chemokine secretion by intestinal epithelial cells indicate that the effects of butyrate are more complex than has been hitherto thought. Sodium butyrate is a normal metabolite of luminal bacteria. Butyrate not only functions as an energy source(13), but modulates the intestinal epithelial cell's response to inflammatory mediators, resulting in chemokine secretion. The cells examined in our models were both healthy and viable. The lack of response in cells without butyrate was not due to any nutritional deprivation, because Caco-2 cells express brush border enzymes(22) and proliferate normally in the absence of butyrate. Addition of serum to the cells in parallel studies did not alter the effects of butyrate. Furthermore, variations in glutamine concentration (another epithelial cell nutrient) did not alter IL-8 secretion patterns.
Future experiments will be needed to show whether butyrate's effects on IL-8 production are through diverse mechanisms (for example by increasing the expression of the receptors for lipopolysaccharide, including CD14 and the IL-1β receptor) or through a single mechanism (for example by binding a specific nuclear protein to the IL-8 promoter). A single mechanism would appear more likely because, at high concentrations, sodium butyrate alone induces small amounts of IL-8 secretion. One attractive hypothesis is that sodium butyrate, by its known action on c-fos induction in Caco-2 cells(29), results in increased heterodimerization of the c-fos and c-jun nuclear proteins, which could then bind to the AP-1 site of the IL-8 promoter(30) resulting, in turn, in the enhancement of IL-8 transcription. In stimulated cells, this nuclear factor may act in association with NFκB, induced by both lipopolysaccharide(31) and IL-1β(32), in increasing IL-8 synthesis(33).
Lipopolysaccharide induced IL-8 secretion from both basolateral and apical poles of Caco-2 cells (Fig. 7). Apical stimulation can, therefore, induce basolateral secretion of IL-8. This is important if intestinal epithelial cells are to act as a system signaling events in the lumen to the mucosal immune system. IL-8 was also secreted apically. It is more difficult to ascribe a function to IL-8 secreted apically than to that secreted basolaterally, but our data are consistent with other observations. First, IL-8 levels in the lumen are elevated during intestinal inflammation in vivo(34). Second, IL-8 secretion by polarized intestinal epithelial cell lines is greater in the direction of the proinflammatory stimulus(35).
In summary, we have shown that butyrate, a normal bacterial metabolite, has a marked effect on the ability of intestinal epithelial cells to secrete IL-8. Because intestinal epithelial cells may participate in the attraction of leukocytes into the intestinal mucosa, we believe that we have identified a mechanism by which bacteria potentially modulate inflammatory responses within the intestine.
Abbreviations
- DMEM:
-
Dulbecco's modified Eagle's medium
- DTS:
-
DMEM supplemented with human transferrin and selenous acid
- GRO:
-
growth related
REFERENCES
Sanderson IR, Walker WA 1994 Mucosal barrier. In: Ogra PL, Mestecky J, Lamm ME, Stober W, McGhee JR, Bienenstock J (eds) Handbook of Mucosal Immunology. Academic Press, New York, pp 41–48
Stadnyk AW 1994 Cytokine production by epithelial cells. FASEB J 8: 1041–1047
Eckmann L, Jung HC, Schurer-Maly C, Panja A, Morzycka-Wroblewska E, Kagnoff MF 1993 Differential cytokine expression by human intestinal epithelial cell lines: regulated expression of interleukin-8. Gastroenterology 105: 1689–1697
Eckmann L, Reed SL, Smith JR, Kagnoff MF 1995 Entamoeba histolytica trophozoites induce an inflammatory cytokine response by cultured human cells through the paracrine action of cytolytically released interleukin-1 alpha. J Clin Invest 96: 1269–1279
Izutani R, Loh E, Reinecker HC, Ohno Y, Fusunyan RD, Lichtenstein GR, Rombeau JL, MacDermott RP 1995 Increased expression of interleukin-8 mRNA in ulcerative colitis and Crohn's disease mucosa and epithelial cells. Inflam Bowel Dis 1: 37–47
Eckmann L, Kagnoff MF, Fierer J 1993 Epithelial cells secrete the chemokine interleukin-8 in response to bacterial entry. Infect Immun 61: 4569–4574
Oppenheim JJ, Zachariae COC, Mukaida N, Matsushima K 1991 Properties of the novel inflammatory supergene “intercrine” cytokine family. Annu Rev Immunol 9: 617–648
Baggiolini M, Walz A, Kunkel SL 1989 Neutrophil-activating peptide-1/interleukin-8, a novel cytokine that activates neutrophils. J Clin Invest 84: 1045–1049
Izzo RS, Witkon K, Chen AI, Hadjiyane C, Weinstein MI, Pellechia C 1993 Neutrophil-activating peptide (interleukin-8) in colonic mucosa from patients with Crohn's disease. Scand J Gastroenterol 28: 296–300
Cummings JH, MacFarlane GT 1991 The control and consequences of bacterial fermentation in the human colon. J Appl Bacteriol 70: 443–459
Cummings JH 1981 Short chain fatty acids in the human colon. Gut 22: 763–769
Royall D, Wolever BM, Jeejeebhoy KN 1990 Clinical significance of colonic fermentation. Am J Gastroenterol 85: 1307–1312
Roediger WEW 1982 Utilization of nutrients by isolated epithelial cells of the rat colon. Gastroenterology 83: 424–429
Kripke SA, Fox AD, Berman JM, Settle RG, Rombeau JL 1989 Stimulation of intestinal mucosal growth and intracolonic infusion of short chain fatty acids. J Parenter Enteral Nutr 13: 109–116
Treem WR, Ahsan N, Shoup M, Hyams J 1994 Fecal short chain fatty acids in children with inflammatory bowel disease. J Pediatr Gastroenterol Nutr 18: 159–164
Cummings JH, Pomare EW, Branch WJ, Naylor CPE, MacFarlane GT 1987 Short chain fatty acids in human large intestine, portal, hepatic and venous blood. Gut 28: 1221–1227
Issekutz A, Bhimji S 1982 Role for endotoxin in the leukocyte infiltration accompanying Escherichia coli inflammation. Infect Immun 36: 558–566
Pinto M, Robine-Leon S, Appay MD, Kedinger M, Triadou N, Dussaulx E, Lacroix B, Simon-Assmann P, Haffen K, Fogh J, Zweibaum A 1983 Enterocyte-like differentiation and polarization of the human colon carcinoma cell line Caco-2 in culture. Biol Cell 47: 323–330
Chantret I, Barbat A, Dussaulx E, Brattain MG, Zweibaum A 1988 Epithelial polarity, villin expression, and enterocytic differentiation of cultured human colon carcinoma cells: a survey of twenty cell lines. Cancer Res 48: 1936–1942
Oguchi S, Walker WA, Sanderson IR 1994 Profile of IGF-binding proteins secreted by intestinal epithelial cells change with differentiation. Am J Physiol 267:G843–G850
Sanderson IR, Ezzell RM, Kedinger M, Erlanger M, Xu ZX, Pringault E, Leon-Robine S, Louvard D, Walker WA 1996 Human fetal enterocytes in vitro: modulation of the phenotype by extracellular matrix. Proc Natl Acad Sci USA 93: 7717–7722
Oguchi S, Walker WA, Sanderson IR 1995 Differentiation and polarity alter the binding of IGF-1 to human intestinal epithelial(Caco-2) cells. J Pediatr Gastroenterol Nutr 20: 148–155
Sanderson IR, Ouellette AJ, Carter EA, Harmatz PR 1993 Ontogeny of Ia messenger RNA in the mouse intestinal epithelium is modulated by age of weaning and diet. Gastroenterology 105: 974–980
McCormick BA, Hofman PI, Kim Jin, Carnes DK, Miller SI, Madara JL 1995 Surface Attachment of Salmonella typhimurium to intestinal epithelia imprints the subepithelial matrix with gradients chemotactic for neutrophils. J Cell Biol 131: 1599–1608
Bry L, Falk PG, Midtvedt T, Gordon JI 1996 A model of host-microbial interactions in an open mammalian ecosystem. Science 273: 1380–1383
Nasmyth DG, Godwin PGR, Dixon MF, Williams NS, Johnston D 1989 Ileal ecology after pouch-anal anastomosis or ileostomy. Gastroenterology 96: 817–824
Dabard J, Hudault S, Saby MA, Gabilan JC, Szylit O, Raibaud P 1987 Production of butyric acid in human premature baby suffering from necrotizing enterocolitis. Proceedings of the 9th International Symposium on Gnotobiology, Versailles, pp 90–95
McCafferty DM, Zeitlin IJ 1989 Short chain fatty acid-induced colitis in mice. Int J Tissue React 11: 165–168
Souleimani A, Asselin C 1993 Regulation of c-fos expression by sodium butyrate in the human colon carcinoma cell line Caco-2. Biochem Biophys Res Commun 193: 330–336
Mukaida N, Shiroo M, Matsushima K 1989 Genomic structure of the human monocyte-derived neutrophil chemotactic factor IL-8. J Immunol 143: 1366–1371
Gromkowski SH, Mama K, Yagi J, Sen R, Rath S 1990 Double stranded RNA and bacterial lipopolysaccharide enhance sensitivity to TNF- mediated cell death. Int Immunol 2: 903–908
Beg AA, Finco TS, Nantermet PV, Baldwin AS 1993 Tumor necrosis factor and interleukin-1 lead to phosphorylation and loss of IκBa: a mechanism for NF-κB activation. Mol Cell Biol 13: 3301–3310
Mukaida N, Mahe Y, Matsushima K 1990 Cooperative Interaction of nuclear factor-κB- and cis-regulatory enhance binding protein-like factor binding elements in activating the interleukin-8 gene by proinflammatory cytokines. J Biol Chem 265: 21128–21133
Kesharvarzian A, Fusunyan RD, D'Astice M, Eiznhmer D, Sanderson IR, MacDermott RP 1995 Rectal dialysates from active ulcerative colitis patients contain increased IL-8: a possible objective measurement of colonic mucosal inflammation and disease activity. Gastroenterology 108:A848.
Lammers KM, Jansen J, Bijlsma PB, Ceska M, Tytgat GN, Laboisse CL, van Deventer SJ 1994 Polarised interleukin-8 secretion by HT 29/19A cells. Gut 35: 338–342
Acknowledgements
The authors are grateful to Dr. David Schoenfeld for statistical analyses.
Author information
Authors and Affiliations
Additional information
Supported by National Institutes of Health Grants DK47753, DK21474, DK40561, DK43351, DK08894, and DK02481, the K. C. Irving Family Research Fellowship Fund, Lahey-Hitchcock Clinic Foundation, and the Hood Foundation. I.R.S. was also supported by the Crohn's and Colitis Foundation of America.
Presented in part at the 1995 Society for Pediatric Research meeting and published in abstract form (Pediatr Res 1995;37:122A).
Rights and permissions
About this article
Cite this article
Fusunyan, R., Quinn, J., Ohno, Y. et al. Butyrate Enhances Interleukin (IL)-8 Secretion by Intestinal Epithelial Cells in Response to IL-1β and Lipopolysaccharide. Pediatr Res 43, 84–90 (1998). https://doi.org/10.1203/00006450-199801000-00013
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199801000-00013
This article is cited by
-
Influence of NFκB inhibitors on IL-1β-induced chemokine CXCL8 and -10 expression levels in intestinal epithelial cell lines: glucocorticoid ineffectiveness and paradoxical effect of PDTC
International Journal of Colorectal Disease (2010)
-
High Proportions of Proinflammatory Bacteria on the Colonic Mucosa in a Young Patient with Ulcerative Colitis as Revealed by Cloning and Sequencing of 16S rRNA Genes
Digestive Diseases and Sciences (2007)
-
Phytic Acid Modulates In Vitro IL-8 and IL-6 Release from Colonic Epithelial Cells Stimulated with LPS and IL-1β
Digestive Diseases and Sciences (2007)
-
Butyrate Switches the Pattern of Chemokine Secretion by Intestinal Epithelial Cells through Histone Acetylation
Molecular Medicine (1999)