Abstract
The impact of depressed neonatal cerebral oxidative phosphorylation for diagnosing the severity of perinatal asphyxia was estimated by correlating the concentrations of phosphocreatine (PCr) and ATP as determined by magnetic resonance spectroscopy with the degree of hypoxic-ischemic encephalopathy(HIE) in 23 asphyxiated term neonates. Ten healthy age-matched neonates served as controls. In patients, the mean concentrations ±SD of PCr and ATP were 0.99 ± 0.46 mmol/L (1.6 ± 0.2 mmol/L) and 0.99 ± 0.35 mmol/L (1.7 ± 0.2 mmol/L), respectively (normal values in parentheses). [PCr] and [ATP] correlated significantly with the severity of HIE (r = 0.85 and 0.9, respectively, p < 0.001), indicating that the neonatal encephalopathy is the clinical manifestation of a marred brain energy metabolism. Neurodevelopmental outcome was evaluated in 21 children at 3, 9, and 18 mo. Seven infants had multiple impairments, five were moderately handicapped, five had only mild symptoms, and four were normal. There was a significant correlation between the cerebral concentrations of PCr or ATP at birth and outcome (r = 0.8, p < 0.001) and between the degree of neonatal neurologic depression and outcome (r= 0.7). More important, the outcome of neonates with moderate HIE could better be predicted with information from quantitative 31P magnetic resonance spectroscopy than from neurologic examinations. In general, the accuracy of outcome predictability could significantly be increased by adding results from31 P magnetic resonance spectroscopy to the neonatal neurologic score, but not vice versa. No correlation with outcome was found for other perinatal risk factors, including Apgar score.
Similar content being viewed by others
Main
Perinatal asphyxia is a major cause of neonatal death, brain injury, and future neuromotor and intellectual impairment, where up to 20-30% of survivors suffer from mental retardation, cerebral palsy, and seizure disorders in later childhood(1–4). Early prognostication of the neurodevelopmental outcome of affected neonates is, thus, of great interest.
Clinical and biochemical parameters, such as depressed fetal heart rate, meconium-stained amniotic fluid, low Apgar scores, low scalp and cord pH, and high base deficit are used as early health indicators to identify and characterize neonates with acute perinatal asphyxia. The Apgar score has repeatedly been questioned as a predictor of adverse neurodevelopmental outcome(5–7), but remains widely accepted as readily accessible measure of asphyxia and neurologic depression during the first minutes of life(8). Affected term infants subsequently present with a characteristic yet nonspecific syndrome of disturbed neurologic functions during the neonatal period, termed hypoxic-ischemic encephalopathy (HIE)(9–12). In the past, signs of HIE have been found as reliable predictors for outcome in term neonates with birth asphyxia(13–15). Whereas infants with a favorable outcome can readily be differentiated from those with a poor prognosis for developing neurologic sequelae, for neonates with moderately severe HIE the prognosis is less certain. The exact mechanism of brain damage is still debated, and the cerebral metabolic alterations after perinatal asphyxia are not fully understood(16–20). It is not clear, why after virtually identical asphyxic insults, as judged by clinical and biochemical indicators, some neonates recover completely, whereas others deteriorate to finally develop severe cerebral palsy or even die.
From recent experimental studies with 31P MRS on asphyxiated neonatal animals we learned that impaired energy metabolism is the leading initial cause of marred brain function during the asphyxic insult. The brain tends to recover rapidly yet only transiently during the first 24 h after resuscitation, whereafter the cerebral energy status again deteriorates to a variable degree, depending on the severity of energy depletion of the brain during the initial illness(21–23). Whereas the primary energy failure is a direct consequence of hypoxia during labor and birth, the delayed secondary impairment of the cerebral oxidative phosphorylation during the neonatal period is triggered by biochemical and electrophysiologic mechanisms(24, 25). Estimating the ratio of PCr/Pi with 31P MRS in asphyxiated neonates, a direct relationship was found between the extent of this secondary energy failure and the neurodevelopmental outcome of the infants at 1 y(26, 27). In an earlier issue of this journal, we described a method for quantifying energy metabolites from well defined areas of the brain in neonates and infants using image-guided, volume-selective31 P MRS(28). Because such examinations are not readily available in sick neonates, a better understanding of the relationship between the depressed cerebral energy metabolism in postasphyxic neonates, and not only their clinical-neurologic characteristics, e.g. the degree of HIE, but also their future neurodevelopment, is warranted to identify preventable and potentially treatable factors, especially in the light of newer therapeutic modalities(29).
In the present study we asked the following questions. 1) Are 5-min Apgar score, cord pH, and base deficit relevant measures of the oxygenation state of the neonatal brain and, hence, asphyxia? 2) Is neonatal encephalopathy the clinical manifestation of a depressed cerebral energy metabolism? 3) Does the degree of depression of the cerebral oxidative metabolism in asphyxiated neonates predict neurodevelopmental handicap at 3, 9, and 18 mo of age, and how does this association compare with the relationship between low neonatal neurologic scores or other perinatal risk factors and outcome?
METHODS
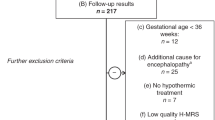
Study cohorts. Twenty-three term neonates at risk with a median gestational age of 40 wk (range, 36.9-41.9) were enrolled in this prospective study. The enrollment criteria have been described previously(30). In summary, neonates had to fulfil at least one item out of two of the following three groups of criteria: 1) signs of intrauterine asphyxia, e.g. pathologic cardiotocogram (<80 beats/min, limited beat-to-beat variability, late deceleration), meconium stained amniotic fluid; 2) signs of perinatal asphyxia,e.g. 5-min Apgar score ≤5, cord pH ≤ 7.1, base deficit ≥10 mmol/L; and 3) signs of postpartum encephalopathy starting within the first 48 h, e.g. decreased muscle tone, pathologic spontaneous movements, lethargy, coma, or seizures. All children were born in outside hospitals. Neonates with severe diseases (septicemia, meningitis, or hyaline membrane disease) or presenting with congential malformations were excluded from the study. Table 1 summarizes the relevant clinical data of the study cohort.
In addition, 10 age-matched healthy term newborns (range of gestational age 36.3-42.1 wk) with a normal clinical and neurologic examination, hospitalized for nonneurologic reasons, served as the control group. The study was approved by the local ethics committee of the University Children's Hospital Zurich, and a written informed consent was obtained from the parents before the examinations.
Neonatal neurologic evaluation. All 23 neonates were evaluated neurologically for signs of HIE by experienced neonatologists on several occasions during the 1st wk of life, timed as close as possible to the magnetic resonance examination. Where necessary, the neurologic assessment had to be delayed for at most 18 h until the child was weaned from the respirator. The patients were classified into three categories, which represent their best neurologic achievement: NNS 3 means only mild disability, e.g. mild muscular hypotonia, normal or weak suck reflex, hyperalertness, jittery, and absence of seizures (generalized sympathetic); NNS 2 signifies moderately encephalopathy, e.g. decreased level of consciousness, somnolence, decreased muscular tone, weak or absent suck reflex, brady-cardia, frequent seizures (generalized parasympathetic); whereas NNS 1 indicates severe HIE,e.g. stuporous or comatose, flaccid, absence of primitive reactions,± seizures (both autonomic systems depressed). The 10 neonates forming the control group were selected on the basis of a normal neurologic examination and were, thus, given a NNS of 4.
Brain MRS. 31P MRS examinations were carried out in all 23 asphyxiated neonates as well as in the 10 healthy neonates on a 2.35 Tesla 40-cm small bore magnet system (MEDSPEC 24/40, Bruker-Spectrospin, Fällanden, Switzerland). The examinations occurred between postnatal d 1 and 6 in all but three patients (Table 2). Complying with the caring physician's decision, unstable newborns were kept in a special thermoregulated incubator, which fitted into the magnet; others were wrapped in isolation blankets. If necessary, the patients were mechanically ventilated during the whole examination. Extensive monitoring was routinely set up for measuring body temperature, blood pressure, transcutaneous Pco2 and Po2, ECG and heart rate, and oxygen saturation with a pulse oximetry during the entire magnetic resonance examination(31). In ventilated infants end-expiratory Pco2 was continuously measured. T1-weighted (TR/TE 500/22 ms) and T2-weighted (TR/TE 3000/120 ms) spin echo sequences were carried out in at least two orthogonal planes. They were used for selecting and localizing volumes for MRS. Immediately subsequent to the imaging sequences, fully relaxed 31P spectra were collected with a repetition time of 12 s (64 average, 13-min scan time), using a pediatric Helmholtz-type volume coil to transmit and receive. Image-guided localization was achieved with the ISIS pulse sequence, applying standard 180 ° sinc and 90 ° block pulses to select 4.5 cm3 volumes comprising 45% of the parietal, 15% of the frontal, and 10% of the occipital lobes, and 20% of the basal ganglia(32). Absolute metabolite concentrations were determined by calibrating the in vivo brain spectra with a full-size head-shaped phantom filled with 0.9 L of a 75 mmol/L KH2PO4 solution(33). The calibration measurements were carried out immediately after the in vivo examination, leaving all measurement parameters unchanged and adjusting the coil load to match that of the in vivo examination. The brain and phantom data were finally processed by fitting the free induction decay signals iteratively in the time domain using all prior knowledge available.
Assessment of outcome. Twenty-one infants could be followed with neurologic and developmental testing for up to 18 mo of age. Two infants died during the neonatal period for reasons probably related to birth asphyxia.
Neurodevelopmental assessment was carried out at the age of 3, 9, and 18 mo by pediatricians who had not been involved in the neonatal care of the infants. It consisted of Griffiths developmental testing and a standardized neurologic examination(34, 35). The entire testing was videotaped in the presence of at least one parent and lasted 1.5-2 h. Subsequently the videotape was analyzed together with a specialist in developmental neurology (R.H.L.). The five subscores of the Griffiths test were divided in a motor developmental quotient (DQ locomotion), a mental DQ(personal and social behavior, hearing and speech, hand-eye coordination, and task performance), and a total DQ. The individual DQs were then compared with those of a control group of age-matched healthy term children and were, after normalization, expressed as SDS. This was achieved by dividing the difference between the individual DQ and the mean DQ of the control group by the SD of the control group. It allows a direct comparison of each individual's deviation from a normative population on SD measures.
In the neurologic examination spontaneous motility, posture, involuntary movements, muscle tone, tendon reflexes, primitive reflexes, and quality of movements were assessed in a standardized manner. The results were expressed in type and distribution, and the severity of the neurologic impairment was graded as LNS, with grade 1 being severely, grade 2 moderately, and grade 3 slightly abnormal, whereas grade 4 indicated normal and age-appropriate.
The latest neurodevelopmental tests were obtained in 18 children at 18 mo, but in two infants only at 9 mo and in one at 3 mo of age, because the parents refused further control examinations in these three infants(Table 3). No arbitrary classification was done for the severity of developmental impairment, but rather the individual total DQ values were correlated with the clinical and spectroscopic parameters assessed at birth.
Statistics. The relationship between the three clinical-biochemical parameters (5-min Apgar score, cord pH, base deficit) and the NNS as well as between the Apgar score and the seven neonatal cerebral MRS parameters (PCr/Pi, [PCr], [ATP], [Pi], [Ptot], pHi) were analyzed by calculating the Spearman correlation coefficients(r) using the SYSTAT statistical package. In addition, probabilities for significance of the various correlations and differences between the groups of NNS 1 to 4 in relation to the phosphorus metabolite concentrations(Fig. 2) were calculated, using the Wilcoxon rank test.
To compare the predictive value of the various parameters obtained during the 1st wk of life with later outcome, 1) the clinical health indicators (5-min Apgar score, cord pH, base deficit); 2) the cerebral 31P metabolites (PCr/Pi, [PCr], [ATP], [Pi],[Ptot]) plus the intracellular pHi; and 3) the NNS were correlated with the SDS of the latest available total DQ and the LNS by calculating the Spearman correlation coefficients (r). Because the outcome is estimated on a continuous scale and reliable normative values for the various MRS parameters are not yet available, correlations were calculated rather than sensitivity, specificity, or predictive values, which would require arbitrary cutoff points.
Analysis of covariance was used to test for a possible increase in accuracy of outcome predictability when combining data from 31P MRS and neonatal neurology.
RESULTS
Signs of depression at birth. Clinical and biochemical findings from 23 patients immediately after birth and relevant information during labor and delivery are presented in Table 1. Eighteen neonates had a pathologic cardiotogram during labor, with late decelerations, 15 had meconium-stained amniotic fluid, and 16 were born either by instrumental delivery or cesarean section. The mean 5-min Apgar score, cord pH, and base deficit in the cord blood were 5.7 (range, 1-9), 6.97 (range, 6.55-7.28), and 16.2 mmol/L (range, 6.0-30.0 mmol/L), respectively. Nineteen out of the 23 newborns needed artificial ventilation for various lengths of time. Two infants (MNa and SAn) died during the 1st mo of life.
Neonatal neurologic findings. The results of the neurologic examinations of all 23 asphyxiated and the 10 healthy neonates, expressed as the individual NNS, are presented in Table 1. Nineteen infants were examined during the 1st wk of life, whereas four could be evaluated only between the ages of 8 and 14 d (median = 4 d, range 2-14 d). Eight neonates were found to be mildly affected, i.e. NNS = 3. Eight showed moderate signs of HIE, i.e. NNS = 2, presenting with hypotonia, stupor, and poor suck; five of them experienced early neonatal seizures. Finally, seven neonates were comatose, suffering from severe HIE with seizures, i.e. NNS = 1.
Spectroscopic results. Figure 1 shows three representative 31P spectra of patient ABe, who sustained severe perinatal asphyxia with a 5-min Apgar score of 1, a cord pH of 6.65, and a base deficit of 30 mmol/L. The first spectrum taken at 24 h postpartum was highly abnormal, with [PCr] of 0.09 (1.6 ± 0.2), [ATP] of 0.35 (1.7± 0.2), and of [Pi] of 1.55 (0.7 ± 0.1) mmol/L (normal values from the control group in parentheses). PCr/Pi, which is a measure of the cellular energy reserve (phosphorylation potential), was 0.06(2.5 ± 0.6). The intracellular pHi was alkaline (7.54), and the child survived with a low neonatal neuroscore of 1. Upon reexamination at the age of 7 d, the energy metabolism recovered somewhat with [PCr] of 0.40, [ATP] of 0.75, and [Pi] of 1.18 mmol/L, and PCr/Pi of 0.34. On d 35 after birth, the 31P brain spectrum had a qualitatively normal appearance, yet the energy metabolites were still significantly below normal(0.92, 0.92, 0.56, and 1.65, respectively). At that time, the infant exhibited a generalized increased muscle tone, suffered from seizure disorders, and had to be fed by nasogastric tube, because it was unable to swallow.
Three consecutive brain 31P spectra of infant ABe. The top spectrum (24 h after birth) indicates severe energy failure:[Pi] = 1.55 (0.7 ± 0.1), [PCr] = 0.09 (1.6 ± 0.2), and[ATP] = 0.35 (1.7 ± 0.2) mmol/L; PCr/Pi = 0.06 (2.5 ± 0.6) (normal values from control group in parentheses). Some recovery of the cerebral energy metabolism after 1 wk (middle spectrum). The bottom spectrum(1 mo postpartum) looks qualitatively normal, yet the respective brain metabolite concentrations were still severely pathologic (0.56, 0.92, 0.92 mmol/L, and PCr/Pi = 1.65).
Table 2 lists the individual values as well as the group means and standard deviations of the cerebral phosphorous metabolites PCr/Pi, [PCr], [ATP], [Pi], [Ptot], and pHi of all 23 neonates at risk grouped according to the achieved NNS (1 to 3). When more than one spectrum per patient was obtained, always the first spectrum beyond 24 h of life was taken for analysis. In addition, the MRS parameters of the 10 healthy neonates with a normal NNS of 4 are shown for comparison. Neonates with a NNS = 1 had mean concentrations of PCr and ATP of 0.58 and 0.76 mmol/L, respectively, and a mean ratio of PCr/Pi of 0.81. The respective mean values of neonates with NNS = 2 were 1.14 and 1.12 mmol/L, and the mean ratio was 2.07. Those infants with NNS = 3 had [PCr] and [ATP] of 1.36 and 1.27 mmol/L, respectively, and a PCr/Pi of 2.66. In addition, the respective values from a group of 10 age-matched healthy neonates with NNS = 4 were 1.65 and 1.72 mmol/L, and the ratio was 2.51. When compared with the normal controls, the mean concentrations of PCr, ATP, and Pi of all asphyxiated neonates differed significantly (p < 0.001), whereas the respective ratios of PCr/Pi did not reach the level of significance. Four of the 23 asphyxiated neonates exhibited a [PCr] within the normal range of 1.65 ± 0.24 mmol/L, but all [ATP] were below the age-matched physiologic range of 1.72 ± 0.22 mmol/L. Interestingly, Ptot was not equal among the four groups, but decreased instead with increasing severity of HIE. Furthermore, the mean values of [Pi] and pHi did not differ significantly between the asphyxiated newborns and healthy controls; however, the pHi values of the former group were spread over a larger range (7.00-7.28).
Neurodevelopmental outcome. Twenty-one of the 23 asphyxiated infants studied during the neonatal period could be enrolled into this follow-up study. Fourteen were examined at 3 mo (median age 3.3; range, 2-5 mo), 17 infants at 9 mo (median, 8.8; range, 7.5-10.5 mo), and 18 children at 18 mo (median, 18.5; range, 15-22 mo).
The results of the latest available neurologic examination are presented in Table 3. Seven children were severely tetraspastic with various additional impairments, such as seizures, ataxia, or hemisyndromes (LNS 1); four were moderately disabled, with hemiparesis, or generalized pathologic muscle tone (LNS 2); six showed only mild neurologic symptoms, such as discrete spastic, hypotonic, or ataxic movement disorders(LNS 3); and four children were considered to be neurologically normal (LNS 4). The individual values of the developmental testing and severity and type of neurologic impairment are also listed in Table 3. At the age of 3 mo, 10 of the 14 infants performed within the normal range (total DQ > 0.75), two infants were moderately retarded (total DQ 0.6-0.75), and two children were severely retarded (total DQ ≤ 0.5). The corresponding values at 9 mo were as follows: 11 of the 17 infants were about normal (total DQ > 0.75), two were moderately retarded (total DQ 0.5-0.75), and four were severely retarded (total DQ < 0.5). At 18 mo similar results were obtained: 12 of the 18 children were normally developed, two were moderately retarded, and four were severely retarded. It ought to be emphasized that the majority of the normally developed children performed in the lower range of the normal distribution. This finding is clearly expressed by the SDS of total DQ: with the exception of three children, the SDS of the latest total DQ was negative (mean SDS of DQ -2.55) (Table 3). There was a strong positive correlation between performance in developmental testing and degree of neurologic impairment.
Relationship of signs of depression at birth with the neonatal neurologic depression, and with the neonatal cerebral energy metabolism(Table 4). No significant correlation could be found between the 5-min Apgar score, the cord pH, and the base deficit and either the NNS, or any of the cerebral 31P MRS parameters (PCr/Pi,[PCr], [ATP], [Pi], [Ptot], and pHi). Interestingly, the clinical-biochemical parameters did not even correlate well among themselves.
Relationship of the neonatal cerebral energy metabolism with the neonatal neurologic depression (Fig. 2). When the patients were classified according to the severity of their HIE (NNS 1-3), differences in absolute concentrations of [PCr] and [ATP] among the three groups of asphyxiated neonates and the group of healthy controls (NNS = 4) were found to be highly significant (p < 0.001), with Spearman correlation coefficients of r = 0.85 and 0.89, respectively. The concentration ratio of PCr/Pi just reached the level of significance(p < 0.01), with a lower correlation coefficient of r = 0.62.
Relationship of neonatal risk factors with outcome(Table 5 and Fig. 3). In general, the results of the latest available neurologic examinations (LNS) and the developmental tests(SDS of DQ) were taken as a measure of the neurodevelopmental outcome(Table 3).
Relationship between the individual NNS, the ratio of PCr/Pi, the molar concentrations of PCr, and ATP obtained during the neonatal period and the neurodevelopmental outcome (SDS of latest available DQ). Spearman correlation coefficients are listed in Table 5.
Correlation of depression at birth with outcome. The 5-min Apgar score, the umbilical cord pH, or the base deficit showed no significant relation to outcome.
Correlation of neonatal depression with outcome. There was a significant correlation of the NNS with outcome (p < 0.01). The correlation coefficient (r) for NNS with LNS was 0.61, and for NNS with SDS of DQ it was 0.69. The NNS predicted the neurologic and the developmental outcome accurately in 12 (57%) and 11 (52%) infants, respectively. Four children (19%) had a higher LNS and SDS of DQ than predicted by the NNS. However, five (24%) children were neurologically more handicapped, and at least two children (10%) were developmentally more delayed than predicted.
A highly significant correlation (p < 0.001) was found between the molar concentrations of PCr and ATP measured in the brains of asphyxiated neonates and their later neurodevelopmental outcome (r = 0.79 and 0.78 for the LNS, and 0.79 and 0.77 for the SDS of DQ, respectively). The correlation between the peak area ratio of PCr/Pi and either outcome parameter was lower, r being 0.57 and 0.66 for LNS and SDS of DQ, respectively, yet still significant (p < 0.01). This indicates that, with the exception of [Pi] and pHi, higher phosphorus metabolite concentrations or higher concentration ratios soon after birth were related to a better outcome, and vice versa.
The combination of neonatal neurologic score and cerebral metabolite concentrations as predictor for outcome. Although the NNS and the cerebral phosphorous metabolites are interrelated variables, the analysis of covariance yielded a significant gain in accuracy of outcome predictability (p< 0.005), when the NNS was taken as primary prognosticator and either [PCr] or [ATP] were added sequentially. On the other hand, if [PCr] or [ATP] were used as predictors for outcome, adding the information from the NNS did not increase the accuracy of outcome predictability.
DISCUSSION
After successful resuscitation, the asphyxiated neonates usually recover rapidly from the hypoxic energy breakdown that takes place during labor and birth (Fig. 1). However, this clinical and metabolic recovery usually lasts only for a period of about 12-24 h and is followed by a secondary, more gradual and prolonged, depression of the cerebral oxidative phosphorylation(22, 23, 26, 36). The extent of energy depletion in the brain during the initial hypoxic-ischemic event is not only directly related to the severity and duration of this delayed metabolic impairment(21), but also to the extent of the subsequent metabolic recovery(Fig. 1). In general, only one MRS examination per patient could be obtained, and thus, the most predictive metabolic trough level during the “secondary energy failure” may have been missed. Moreover, the postnatal age at examination differed among our patients by several days, depending also on the condition of the child. Three neonates could be evaluated only during the 2nd wk of life, yet they were not excluded from the analysis, because their MRS results did not deviate by more than 2 SD from the group mean.
In the introduction we addressed several questions, which will be answered sequentially:
First, being aware of the small number of patients (n = 23), no significant correlation could be found between the perinatal risk factors(5-min Apgar score, cord pH, and base deficit) and either the degree of depression of the neonatal cerebral energy metabolism or the severity of encephalopathy, expressed by the NNS (Table 4). The 5-min Apgar scores were >5 in 12 neonates; however, nine of them were ventilated, which might have lead to falsely high scores. Presuming a successful resuscitation, our observation leads to the conclusion that a newborn with a complicated birth, e.g. low Apgar score, is not necessarily placed at a heightened risk of significant encephalopathy. A low Apgar score should, therefore, be seen as an index of the momentary cardiorespiratory status of the infant, not necessarily related to brain oxygenation and, hence, asphyxia, and unrelated to the neurologic status. This would be in agreement with the statement that “low Apgar scores are probably results of what has already happened rather than causes of what follows”(12).
Second, an important finding was the significant and high correlation between the absolute concentrations of cerebral energy metabolites and the degree of neonatal encephalopathy (Fig. 2), indicating that the degree of cerebral energetic breakdown was the leading cause of a corresponding failure in neurologic performance. This is remarkable, because the 31P MRS data were processed fully automatically without manual phase or baseline corrections, to eliminate unnecessary bias. However, when the neonates were classified according to their best neurologic achievement, the ratio of PCr/Pi just reached the level of significance (p< 0.01), but could not differentiate between patients with NNS 2 or 3 and healthy neonates (Fig. 2). Thus, quantitative 31P MRS is preferably used for assessing cerebral metabolic breakdown in asphyxiated neonates.
Third, regarding outcome, our results are in agreement with earlier reports that the extent of depression of the cerebral oxidative phosphorylation in asphyxiated newborns is related to the severity of unfavorable neurodevelopmental outcome(26, 27). Note fromTable 5 and Fig. 3 that absolute concentrations of phosphorus metabolites (PCr and ATP) tended to predict outcome more accurately than did the ratio of PCr/Pi. The lack of correlation between the intracellular pHi and outcome can be explained by the rapid fluctuation from acidotic to alkalotic values and is well in agreement with other studies(36).
The severity of HIE indicated by the NNS was not only the bestclinical indicator that an infant had suffered from perinatal asphyxia, but also the only clinical parameter for predicting outcome, which corroborates earlier reports(6, 15). However, the relationship between the NNS and either the neurologic or the neurodevelopmental outcome was weaker compared with that between the neonatal cerebral metabolite concentrations (PCr, ATP) and the LNS or the SDS of DQ(Table 5). Especially the outcome of moderately affected neonates (NNS 2) was unpredictable (Fig. 3). Of the eight children with a SDS of DQ ≤ -2, four had an NNS of 2 (moderate HIE) and four had an NNS of 1 (severe encephalopathy), whereas all eight neonates had[PCr] and [ATP] <1 mmol/L. Moreover, the median concentration of PCr in the brains of all infants with NNS 2 was 0.98 mmol/L (range, 0.75 to 1.26 mmol/L), which is significantly lower than the normal value of 1.65 (± 0.24) mmol/L. This is an important finding and leads to the conclusion, that the outcome of neonates with moderate encephalopathy (NNS 2, corresponding to Sarnat grade 2) could more accurately be predicted with quantitative31 P MRS than with clinical neurologic judgment. This might be of special importance for ventilated neonates or those on sedative or antiepileptic drug treatment.
The 5-min Apgar scores, the umbilical cord pH, and the base deficit did not correlate at all with outcome (Table 5), which is in agreement with recent investigations(37, 38). Epidemiologic studies have shown that cerebral palsy is at most only equivocally related to the Apgar score at birth(1). The present data illustrate that it would be false to conclude from this lack of correlation that subsequent neurologic sequelae, e.g. cerebral palsy, would be unrelated to neonatal brain oxygenation. Quite the contrary seems to be the case. If, however, a severe HIE, signified by NNS 1, and a depression of the cerebral energy metabolism could be observed as a consequence of a perinatal asphyxia, indicated by signs of depression at birth, then these consequences were of important prognostic value. Out of the 11 neonates with 5-min Apgar scores ≤5, six had an NNS of 1 and very low cerebral concentrations of PCr and ATP (0.09-1.11 mmol/L and 0.29-1.16 mmol/L, respectively). Two infants (MNa and SAn) died probably as a consequence of asphyxia. Three were severely handicapped (-7.9 to -7 SDS of DQ, and LNS 1), whereas one child was only mildly disabled (-1 SDS of DQ, LNS 3). Signs of depression at birth, such as low Apgar scores, cord pH, and high base deficits, do represent risk factors for encephalopathy and, thus, characterize neonates at risk for unfavorable outcome, yet they are per se of no prognostic value for these events to really take place.
Combining the results from NNS and 31P MRS significantly increased the accuracy of outcome predictability, but only when the NNS was taken as the original predictor and the MRS results were sequentially added. However, no further improvement in accuracy of outcome predictability could be found by sequentially adding the information from the neonatal neurologic scores, when the MRS results were assigned as primary predictors.
Abbreviations
- HIE:
-
hypoxic-ischemic encephalopathy
- DQ:
-
(neuro)developmental quotient
- LNS:
-
late neurologic score
- MRS:
-
magnetic resonance spectroscopy
- NNS:
-
neonatal neurologic score
- PCr:
-
phosphocreatine
- Pi:
-
inorganic phosphate
- Ptot:
-
total MRS-“visible” phosphorus-31 metabolites
- pHi:
-
intracellular pH
- SDS:
-
SD score
References
Nelson KB 1988 What proportion of cerebral palsy is related to birth asphyxia?. (editor's column) J Pediatr 112: 572–574.
Robertson CMT, Finer NN, Grace MGA 1989 School performance of survivors of neonatal encephalopathy associated with birth asphyxia at term. J Pediatr 114: 753–760.
Hull J, Dodd K 1991 What is birth asphyxia?. Br J Obstet Gynaecol 98: 953–955.
Bax M, Nelson KB 1993 Birth asphyxia: a statement. Dev Med Child Neurol 35: 1015–1024.
Sykes GS, Johnson P, Ashworth F, Molloy PM, Gu W, Stirrat GM, Turnbull AC 1982 Do Apgar scores indicate asphyxia?. Lancet 2: 494–496.
Finer NL, Robertson CM, Peters KL, Coward JH 1983 Factors affecting outcome in hypoxic-ischemic encephalopathy in term infants. Am J Dis Child 137: 21–25.
Marlow N 1992 Do we need an Apgar score?. Arch Dis Child 67: 765–769.
Nelson KB, Leviton MD 1991 How much of neonatal encephalopathy is due to birth asphyxia?. Am J Dis Child 145: 1325–1331.
Sarnat HB, Sarnat MS 1976 Neonatal encephalopathy following foetal distress. A clinical and electroencephalographic study. Arch Neurol 33: 696–705.
Low JA, Galbraith RS, Muir DW, Killen HL, Pater EA, Karchmar EJ 1985 The relationship between perinatal hypoxia and newborn encephalopathy. Am J Obstet Gynaecol 152: 256–260.
Robertson C, Finer N 1985 Term infants with hypoxic-ischemic encephalopathy: outcome at 3.5 years. Dev Med Child Neurol 27: 473–484.
Nelson KB, Stanley Emery E 1993 Birth asphyxia and the neonatal brain: what do we know and when do we know it?. Clin Perinatol 20: 327–344.
Levene MI, Grindulis H, Sands C, Moore JR 1986 Comparison of two methods of predicting outcome in perinatal asphyxia. Lancet 1: 67–68.
Amiel-Tison C, Ellison P 1986 Birth asphyxia in the fullterm newborn: Early assessment and outcome. Dev Med Child Neurol 28: 671–682.
Nelson KB, Ellenberg JH 1987 The asymptomatic newborn and risk of cerebral palsy. Am J Dis Child 141: 1333–1335.
Fenichel GM 1983 Hypoxic-ischemic encephalopathy in the newborn. Arch Neurol 40: 261–266.
Blair E 1993 A research definition for “birth asphyxia”?. Dev Med Child Neurol 35: 449–455.
Levene MI 1993 Management of the asphyxiated full term infant. Arch Dis Child 68: 612–616.
Williams CE, Mallard C, Tan W, Gluckman PD 1993 Pathophysiology of perinatal asphyxia. Clin Perinatol 20: 305–326.
Volpe JJ 1995 Hypoxic-ischemic encephalopathy: clinical aspects. In: Neurology of the Newborn, 3rd Ed. WB Saunders, Philadelphia, pp 314–372.
Lorek A, Takei V, Cady EB, Wyatt JS, Penrice J, Edwards AD, Peebles D, Wylezinska M, Owen-Reece H, Kirkbride V, Cooper CE, Aldridge RF, Roth SC, Brown G, Delpy DT, Reynolds EOR 1994 Delayed(“secondary”) cerebral energy failure after acute hypoxia-ischemia in the newborn piglet: continuous 48-hour studies by phosphorus magnetic resonance spectroscopy. Pediatr Res 36: 699–706.
Rumpel H, Buchli R, Martin E 1995 Brain energy metabolism and edema formation in asphyxiated neonatal rats: a combined MRI-MRS study. Biol Neonate 67: 311
Rumpel H, Nedelcu H, Ekatodramis D, Buchli R, Martin E 1995 Temporal evolution of hypoxic-ischemic brain edema in the neonatal rat by magnetic resonance (MR). Pediatr Res 38: 452
Siesjo BK, Smith ML 1991 The biochemical basis of ischemic brain lesions. Drug Res 41: 288–292.
Johnston MV 1993 Cellular alterations associated with perinatal asphyxia. Clin Invest Med 16: 122–132.
Azzopardi D, Wyatt JS, Cady EB, Delpy DT, Baudin J, Stewart AL, Hope PL, Hamilton PA, Reynolds EOR 1989 Prognosis of newborn infants with hypoxic ischemic brain injury assessed by phosphorus magnetic resonance spectroscopy. Pediatr Res 25: 445–451.
Roth SC, Edwards AD, Cady EB, Delpy DT, Wyatt JS, Azzopardi D, Baudin J, Townsend J, Stewart AL, Reynolds EOR 1992 Relation between cerebral oxidative metabolism following birth asphyxia, and neurodevelopmental outcome and brain growth at one year. Dev Med Child Neurol 34: 285–295.
Buchli R, Martin E, Boesiger P, Rumpel H 1994 Developmental changes of phosphorus metabolite concentrations in the human brain: a 31P magnetic resonance spectroscopy study in vivo. Pediatr Res 35: 431–435.
Volpe JJ 1992 Brain injury in the premature infant-current concepts of pathogenesis and prevention. Biol Neonate 62: 231–242.
Baenziger O, Martin E, Steinlin M, Good M, Largo R, Burger R, Fanconi S, Duc G, Buchli R, Rumpel H 1993 Early pattern recognition in severe perinatal asphyxia: a prospective MRI study. Neuroradiology 35: 437–442.
Boesch Ch, Martin E 1988 Combined application of MR imaging and spectroscopy in neonates and children: installation and operation of a 2.35-T system in a clinical setting. Radiology 168: 481–488.
Buchli R, Martin E, Boesiger P 1994 Assessment of absolute metabolite concentrations in human tissue by 31P MRS in vivo; Part I. Cerebrum, cerebellum, cerebral grey and white matter. Magn Reson Med 32: 447–452.
Buchli R, Martin E, Boesiger P 1994 Comparison of calibration strategies for the in vivo determination of absolute metabolite concentrations in the human brain by 31P MRS. NMR Biomed 7: 225–230.
Griffiths R 1970 The Abilities of Young Children. Association for Research in Infant and Child Development, High Wycombe, UK
Largo RH, Pfister D, Molinari L, Kundu S, Lipp A, Duc G 1989 Significance of prenatal, perinatal and postnatal factors in the development of AGA preterm infants at five to seven years. Dev Med Child Neurol 31: 440–456.
Hope PL, Costello AM del, C Cady EB, Delpy DT, Tofts PS, Chu A, Hamilton PA, Reynolds EOR, Wilkie DR 1984 Cerebral energy metabolism studied with phosphorus NMR spectroscopy in normal and birth-asphyxiated infants. Lancet 2: 366–370.
Ruth VH, Raivio KO 1988 Perinatal brain damage: predictive value of metabolic acidosis and the Apgar score. BMJ 297: 24–27.
Yudkin PL, Johnson A, Clover LM, Murphy KW 1994 Clustering of perinatal markers of birth asphyxia and outcome at age five years. Br J Obstet Gynaecol 101: 774–781.
Acknowledgements
The authors thank Brigit Graf and Sara Djahanschahi for fruitful cooperation; Prof. A. Fanconi, Chairman, Department Pediatrics, for his continuous support; Prof. Hans C. Lou, Glostrup Denmark, for critically reviewing the manuscript; Dr. Luciano Molinari for help with the statistical analysis; and Heidi Rutz and Rosina Zoppi for monitoring of the infants and preparing the manuscript.
Author information
Authors and Affiliations
Additional information
Supported by Swiss National Science Foundation (SNF-Nr. 31-28630.90 and 32-37811.93), Committee for the Promotion of Applied Scientific Research(KWF-Nr. 2094.2), and Prof. Max Cloëtta Foundation (Zurich).
Rights and permissions
About this article
Cite this article
Martin, E., Buchli, R., Ritter, S. et al. Diagnostic and Prognostic Value of Cerebral31P Magnetic Resonance Spectroscopy in Neonates with Perinatal Asphyxia. Pediatr Res 40, 749–758 (1996). https://doi.org/10.1203/00006450-199611000-00015
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199611000-00015
This article is cited by
-
Na+/H+ Exchangers and Intracellular pH in Perinatal Brain Injury
Translational Stroke Research (2014)
-
Systemic hypothermia to decrease morbidity of hypoxic-ischemic brain injury
Journal of Perinatology (2007)
-
Mild hypothermia via selective head cooling as neuroprotective therapy in term neonates with perinatal asphyxia: an experience from a single neonatal intensive care unit
Journal of Perinatology (2006)