Abstract
We recently demonstrated that recombinant hGH exacerbates renal functional and structural injury in chronic puromycin aminonucleoside (PAN) nephropathy, an experimental model of glomerular disease. Therefore, we examined whether recombinant human (rh) IGF-I is a safer alternative for the treatment of growth failure in rats with chronic PAN nephropathy. The glomerulopathy was induced by seven serial injections of PAN over 12 wk. Experimental animals(n = 6) received rhIGF-I, 400 μg/d, whereas control rats(n = 6) received the vehicle. rhIGF-I improved weight gain by 14%(p < 0.05), without altering hematocrit or blood pressure in rats with renal disease. Urinary protein excretion was unaltered by rhIGF-I treatment in rats with chronic PAN nephropathy. After 12 wk, the inulin clearance was higher in rhIGF-I-treated rats, 0.48 ± 0.08versus 0.24 ± 0.06 mL/min/100 g of body weight in untreated PAN nephropathy animals, p < 0.05. The improvement in GFR was not associated with enhanced glomerular hypertrophy or increased segmental glomerulosclerosis, tubulointerstitial injury, or renal cortical malondialdehyde content. In rats with PAN nephropathy, administration of rhIGF-I increased IGF-I and GH receptor gene expression, without altering the steady state level of IGF-I receptor mRNA. In normal rats with intact kidneys, rhIGF-I administration (n = 4) did not alter weight gain, blood pressure, proteinuria, GFR, glomerular planar area, renal cortical malondialdehyde content, or glomerular or tubulointerstitial damage, compared with untreated animals (n = 4). rhIGF-I treatment reduced the steady state renal IGF-I mRNA level but did not modify gene expression of the IGF-I or GH receptors. We conclude that: 1) administration of rhIGF-I improves growth and GFR in rats with chronic PAN nephropathy and 2) unlike rhGH, long-term use of rhIGF-I does not worsen renal functional and structural injury in this disease model.
Similar content being viewed by others
Main
Growth retardation is an important complication of CRF in children. It is caused by many factors including insufficient caloric intake, metabolic acidosis and renal osteodystrophy(1). Plasma concentrations of GH are elevated and IGF-I concentrations are within the normal range in pediatric patients with CRF; however, uremic toxins or end-organ responsiveness may interfere with the growth-promoting action of these peptide hormones(1, 2).
Administration of rhGH for 3 wk to rats with 5/6 nephrectomy enhances somatic growth compared with untreated uremic counterparts(3). rhGH treatment for 3-5 y to prepubertal children with CRF improves growth velocity without undue acceleration of bone maturation(4–6).
There has been recent concern that rhGH, if administered over extended periods of time, may aggravate kidney disease and hasten the progression to end-stage renal failure. The severity of injury after renal ablation is attenuated in a mutant strain of dwarf rats that are selectively deficient in GH(7). Although rhGH administration for 8 wk to rats with 5/6 nephrectomy does not cause deterioration in renal function, glomerular hypertrophy and glomerulosclerosis are increased(8). We have demonstrated that rhGH treatment reduced GFR by 50% and increased glomerular hypertrophy, glomerulosclerosis, and tubulointerstitial fibrosis in rats with chronic PAN nephropathy. These changes were accompanied by increased lipid peroxidation of the renal parenchyma(9).
Although the growth-promoting effects of rhGH are mediated via increased production of IGF-I(10), there is evidence that GH and IGF-I have markedly different effects on the kidney. Transgenic mice carrying the bovine GH gene fused to the metallothionein-I promoter develop increased proteinuria and glomerulosclerosis(11, 12). In contrast, transgenic mice that overexpress the IGF-I gene manifest elevated circulating IGF-I concentrations and parallel increases in body and renal growth; however, they do not develop proteinuria or glomerulosclerosis(11).
Therefore, we conducted the following studies; 1) to assess the effect of rhIGF-I on chronic PAN nephropathy, an experimental glomerulopathy characterized by heavy proteinuria and renal insufficiency and 2) to compare the results of rhIGF-I versus rhGH treatment in this model of FSGS.
METHODS
Animals. Male Sprague-Dawley rats were purchased from Taconic Farms (Germantown, NY) and housed in an animal facility that was maintained at 25°C with a 12 h light-dark cycle. They were provided free access to water and standard rodent laboratory chow, containing 22% protein (Purina Mills, St. Louis, MO). Because the pattern of weight gain was similar in the two groups of rats with chronic PAN nephropathy, pair feeding was not used in these studies. The rats weighed 105-140 g at the initiation of the experimental protocols.
Disease model. Chronic PAN nephropathy was induced over 12 wk using the method described by Grond et al.(13). Briefly, rats were given seven s.c. injections of PAN, 2 mg/100 g of BW/dose, on d 1, 8, 15, 29, 43, 57, and 71. The toxin was dissolved, 10 mg/mL, in 0.9% NaCl.
Rats with chronic PAN nephropathy and a cohort of normal rats with intact kidney function were randomly assigned to an experimental group that received rhIGF-I and a control group given sham injections. The following four groups of rats were studied;
-
Group IA (n = 6): PAN nephropathy + vehicle
-
Group IB (n = 6): PAN nephropathy + rhIGF-I
-
Group IIA (n = 4): Normal rats + vehicle
-
Group IIB (n = 4): Normal rats + rhIGF-I.
rhIGF-I, dissolved 5 mg/mL in 126 mM NaCl, 10 mM citrate buffer, was diluted with 0.9% NaCl to a final concentration of 2 mg/mL. Experimental rats received 0.1 mL (200 μg/dose) of rhIGF-I solution as a s.c. injection twice daily, 5 d/wk for 12 wk. rhIGF-I treatment commenced on the day of the first PAN injection. Control animals were given 0.1 mL of vehicle.
Rats were weighed biweekly and blood pressure was measured each month in the awake conscious state using a tail cuff plethysmograph (Narco BioSystems, Houston, TX). Every 2 wk, animals were placed in individual metabolic cages(Nalge, Rochester, NY) for collection of 24-h urine samples to determine urinary protein and creatinine concentrations. Rats were given free access to water but not food while they were in the metabolic cages. Each month, a fasting blood sample was obtained by retro-orbital plexus puncture at the completion of the urine collection for measurement of hematocrit, serum Na+, creatinine, cholesterol, triglyceride, and albumin concentrations.
Inulin clearance. At the end of the 12-wk study, 12 h after the final rhIGF-I injection, rats were anesthetized with Inactin (Promonta, Byk Golden, Konstanz, Germany; 100 mg/kg of BW) and placed on a heated animal operating table. Body temperature was monitored with a YSI telethermometer and maintained at 36.5-37.5°C throughout the study. A tracheostomy was performed, and the left external jugular vein was cannulated for infusion of[3H]inulin. A suprapubic cystotomy was performed for the collection of urine into tared test tubes. After preparation of the animal, 0.2 mL of a solution containing 12.5 mCi [3H]inulin/mL was injected as a priming dose, followed by infusion of the same solution at a rate of 0.12 mL/h. After a 30-min equilibration period, three timed 30-min urine collections were made, and midpoint blood specimens were obtained. Serum and urinary[3H]inulin activities were determined with a liquid scintillation counter (LKB Rackbeta). Inulin and creatinine clearances were calculated from the standard equation and data are expressed as mL/min/100 g of BW.
Histopathology examination. At the completion of the clearance studies, rats were anesthetized by injection of pentobarbital, 50 mg/kg of BW, and killed by exsanguination. Kidneys were immersion-fixed in a 10% formalin solution and stained with hematoxylin-eosin and periodic acid-Schiff reagents. Segmental sclerosis was defined as localized collapse of capillary lumina and replacement with eosinophilic hyalinized material, occasionally accompanied by adhesions to Bowman's capsule. The number of segmentally sclerosed glomeruli was expressed as a percentage of the number of glomeruli which exceeded 250 in each sample. The tubules and interstitium were examined for dilatation, intratubular casts and tubular atrophy, interstitial infiltration with mononuclear cells, and fibrosis. Tubulointerstitial changes were graded on a scale from 0 to 3+ as follows: 0, normal kidney; 1+, mild, affecting <25% of the renal parenchyma; 2+, moderate, 25-50% involvement; and 3+, severe,>50% of the kidney manifested abnormalities.
The glomerular planar area was determined using a computerized digitizing pad (Micro-plan II, Laboratory Computer Systems, Inc., Monsanto Corp., Natick, NY) and surveying 40-50 glomeruli in each kidney specimen. Glomeruli throughout the cortex that were not globally sclerosed and that had clear delineation of the hilar region were included in this analysis.
mRNA isolation and RNase protection assay. Total RNA was isolated from renal tissue using the Trizol reagent (Life Technologies, Inc., Bethesda, MD), and the amount was quantitated spectrophotometrically at OD 260/280. The RNA was then applied to a denaturing 0.8% agarose gel, and the integrity of the RNA was assessed by ethidium bromide staining of the 28S and 18S ribosomal RNA bands. The rat IGF-I probe (from C. Roberts, Jr., and D. LeRoith of NIDDK of the National Institutes of Health) was a 376-bpHin dIII/EcoRI fragment in riboprobe vector pGEM-3(Promega, Madison, WI). The GH receptor probe (from W. Baumbauch of American Cyanamid, Princeton, NJ) was a 544-bp HindIII/BgIII fragment cloned between the HindIII and BamhI sites of pGEM-3. These two plasmids were linearized with HindIII. The rat IGF-I receptor probe (from C. Roberts, Jr., and D. LeRoith) was a 265-bpEco RI-RsaI fragment. The probe was subcloned into pGEM-3 that had been digested with EcoRI and SmaI and was linearized with EcoRI. For all three probes, the antisense RNA was synthesized with T7 polymerase using the Promega in vitro transcription kit and [α-32P]GTP (NEN DuPont, Boston, MA). The abundance of the mRNA for IGF-I, IGF-I receptor, and GH receptor was determined using an RNase protection assay and related to the total RNA(14). Sample loading was comparable in all groups, and this was confirmed by visual inspection of the 18S RNA band in ethidium bromide-stained gels.
Analytic methods. Serum Na+, glucose, creatinine, cholesterol, triglyceride, and urinary creatinine determinations were made using an automated analyzer (Beckman, Fullertown, CA). Serum albumin levels were assayed with the bromcresol green binding reagent (Sigma), and absorbance was monitored at 628 nm. Urinary protein concentration was measured using the Coomassie Blue binding reagent (Bio-Rad, Richmond, CA).
Serum IGF-I concentrations were determined with a RIA (Nichols Institute Diagnostics, San Juan Capistrano, CA) after acid-ethanol extraction of the samples. The intraassay variability was 6.7%. The recovery of IGF-I from the samples was consistently greater than 90% and was comparable in nephrotic and normal sera, 93 ± 2 and 94 ± 1%, respectively.
Portions of the renal cortex were homogenized in 1.15% KCl solution (1:9 wt/vol) for assay of malondialdehyde content as described by Ohkawa et al.(15). A reaction mixture containing 0.2 mL of sample, 0.2 mL of 8.1% SDS, 1.5 mL of 20% acetic acid adjusted to pH 3.5 with NaOH, and 1.5 mL of 0.8% aqueous solution of thiobarbituric acid was brought up to 4 mL with distilled water. The mixture was heated for 60 min at 95°C and then cooled with tap water, after which 1 mL of water and 5 mL of a mixture of n-butanol and pyridine (15:1, vol/vol) were added. The sample was shaken vigorously and centrifuged at 4 000 rpm for 10 min, and the organic layer was removed. Absorbance was measured at 532 nm, using 1,1,3,3-tetramethoxypropane as a standard. The renal cortical lipid peroxide level was expressed as nanomoles/mg of protein.
The water content of the kidney, expressed as milliliters/100 g of dry weight, was determined by drying tissue specimens at 80°C for 72 h.
Statistical analysis. The differences between groups were analyzed using a t test, Wilcoxon test, and analysis of variance where appropriate. The differences between experimental groups were considered statistically significant if p < 0.05.
RESULTS
The rats in the four experimental groups had similar BW, blood pressure, urinary protein excretion, and serum creatinine, albumin, and cholesterol concentrations at the start of the study (Table 1).
Administration of rhIGF-I enhanced weight gain in rats with PAN nephropathy(group IB); the increment was 14% compared with untreated animals with PAN nephropathy (group IA) at 12 wk, p < 0.05 (Table 1). After 4 wk of IGF-I treatment, rats in group IB had a significantly lower serum glucose concentration compared with the untreated rats with PAN nephropathy, p < 0.01 (Table 1). However, hypoglycemia (serum glucose concentration <3.9 mmol/L) was not detected at 8-12 wk of therapy in rhIGF-I-treated rats with chronic PAN. There were no other adverse metabolic side effects of rhIGF-I treatment. In fact, serum cholesterol and triglyceride concentrations were lower in rhIGF-I-treated(group IB) versus untreated rats with chronic PAN nephropathy (group IA) (Table 2).
The serum IGF-I concentration was measured at the completion of 12 wk of treatment in specimens that were obtained 12 h after the last dose. The serum IGF-I concentration was lower in rats with PAN nephropathy compared with normal animals, 103 ± 39 versus 539 ± 19 ng/mL,p < 0.001. Administration of rhIGF-I raised the circulating peptide level nearly 4-fold in animals with glomerular disease; however, the change was not statistically significant (Table 3).
Blood pressure was comparable in both groups of rats with PAN nephropathy until 12 wk when rhIGF-I-treated animals (group IB) had lower blood pressure levels than untreated rats with glomerular disease (group IA), 135 ± 3versus 154 ± 8 mm Hg, p < 0.05(Table 1).
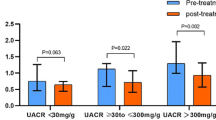
Urinary protein excretion (mg/24 h) was virtually identical throughout the study in rats in group IA and group IB (Fig. 1).
The inulin clearance after 12 wk of chronic PAN nephropathy was significantly higher in rhIGF-I rats (group IB), 0.48 ± 0.08versus 0.24 ± 0.06 mL/min/100 g BW in untreated animals in group IA, p < 0.05 (Fig. 2). The difference in inulin clearance persisted if the GFR was expressed per g kidney weight, 0.14 ± 0.03 (group IA) versus 0.33 ± 0.05 (group IB),p < 0.05. This contrasts sharply with the 50% reduction in GFR observed in rats with chronic PAN nephropathy that received rhGH(9).
Total kidney weight was not increased by rhIGF-I treatment in rats with chronic PAN nephropathy, 5.91 ± 0.45 g (group IB) compared with 5.84± 0.40 g (group IA). In fact, if kidney weight was expressed as a percentage of BW, administration of rhIGF-I lowered this ratio from 1.71± 0.10 (group IA) to 1.46 ± 0.11% (group IB). Water content was also similar in untreated rats with chronic PAN nephropathy compared with those given rhIGF-I, 439 ± 7 versus 429 ± 11 mL/100 g dry weight, respectively. Renal histopathology studies indicated that glomerular planar area was enlarged by 38% in rats with chronic PAN nephropathy (group IA) compared with normal animals (group IIA). Glomerular hypertrophy was not enhanced by treatment with rhIGF-I (group IB)(Fig. 3). Moreover, administration of rhIGF-I to rats with chronic PAN nephropathy did not alter renal parenchymal injury. The percentage of segmentally sclerosed glomeruli was 28.9 ± 4.7% in group IB,versus 32.8 ± 9.6% in group IA; the tubulointerstitial injury score paralleled glomerular damage i.e., 1.25 ± 0.11 in group IB versus 1.42 ± 0.15 in group IA (Table 4).
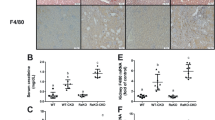
In animals with chronic PAN nephropathy, renal steady state concentrations of IGF-I and IGF-I receptor mRNA were comparable to those detected in normal rats. GH receptor mRNA level was reduced by 50% in rats with glomerular disease (p < 0.001). Administration of rhIGF-I increased gene expression of IGF-I by 203% (p < 0.01) and GH receptor by 136%(p < 0.01), without influencing IGF-I receptor mRNA abundance(Fig. 4). A representative autoradiogram of the RNase protection assay for IGF-I, IGF-I receptor and GH receptor in the four experimental groups is illustrated in Figure 5.
Steady state renal mRNA levels of IGF-I, IGF-I receptor and GH receptor. Open bar, normal rats + vehicle (n = 4);bar with diagonal lines, normal rats + rhIGF-I (n = 4);bar with horizontal lines, PAN nephropathy + vehicle (n = 6); bar with cross-hatch pattern, PAN nephropathy + IGF-I(n = 6). *p < 0.01 vs normals rats + vehicle;**p < 0.01 vs normals rats + vehicle and PAN rats + vehicle.
Renal cortical and hepatic malondialdehyde content were significantly greater than normal in animals with chronic PAN nephropathy (group IA), 2.51± 0.07 and 0.98 ± 0.17 nmol/mg protein, respectively. Unlike rhGH which increased renal malondialdehyde content in chronic PAN nephropathy(9), lipid peroxidation in the kidney and liver was not altered by rhIGF-I treatment in rats with glomerular disease, 2.36 ± 0.21 and 0.71 ± 0.07 nmol/mg protein, respectively(Fig. 6).
Renal and hepatic malondialdehyde content (nmol/mg protein) in normal and PAN nephropathy rats. Open bar, normal rats + vehicle; bar with diagonal lines, normal rats + rhIGF-I; bar with horizontal lines, PAN nephropathy + vehicle; bar with cross-hatch pattern, PAN nephropathy + IGF-I. *p < 0.01vs normal rats + vehicle; **p < 0.01 vs normal rats + rhIGF-I.
Administration of rhIGF-I to intact rats with normal kidney function (group IIB) doubled the circulating level of the peptide (Table 3). The treatment had no discernible effect on somatic growth, blood pressure, hematocrit, or serum glucose concentration compared with normal rats receiving no therapy (group IIA) (Table 1). rhIGF-I did not alter the serum albumin, cholesterol, triglycerides, or creatinine concentration in normal rats (Table 2). In addition, there was no increase in urinary protein excretion in group IIB animals(Fig. 1).
There was no rhIGF-I-induced elevation in inulin clearance in the rats in group IIB, 0.69 ± 0.07, compared with 0.69 ± 0.05 mL/min/100 g of BW in group IIA (Fig. 2). Therapy with rhIGF-I did not promote kidney enlargement in normal rats, 3.49 ± 0.14 g in group IIA and 3.46 ± 0.32 g in group IIB. Thus, kidney weight/BW ratio was unaffected by the administration of rhIGF-I, 0.78 ± 0.01 (group IIA)versus 0.76 ± 0.05% (group IIB). Kidney water content was lower in normal rats than in animals with chronic PAN nephropathy and was unaffected by rhIGF-I treatment, 299 ± 11 (group IIA) and 301 ± 1 mL/100 g of dry weight (group IIB). There was no enlargement of glomerular planar area (Fig. 3) or increase in glomerulosclerosis or tubulointerstitial damage among the normal animals given rhIGF-I compared with untreated rats (Table 4). In normal rats, administration of rhIGF-I resulted in a modest reduction in renal IGF-I mRNA levels without altering IGF-I receptor or GH receptor gene expression (Fig. 4). Finally, rhIGF-I treatment did not increase lipid peroxidation of renal or hepatic tissue in normals rats (Fig. 5).
DISCUSSION
This study demonstrates that administration of rhIGF-I to rats with chronic PAN nephropathy increased somatic growth by 14% without exacerbating renal functional and structural damage. In fact, the GFR was 2-fold higher in animals given rhIGF-I for 12 wk without concomitant increases in kidney size, glomerular planar area, glomerulosclerosis, tubulointerstitial fibrosis, or renal parenchymal lipid peroxidation. These results differ from our previous work in which rhGH treatment had no anabolic effect in rats with PAN nephropathy and aggravated the glomerulopathy(9). The present study was performed as a direct follow-up of these earlier experiments which documented the nephrotoxicity of rhGH in chronic PAN nephropathy. In normal rats, rhIGF-I treatment did not alter body growth or renal structure and function.
The rhIGF-I dose, 400 μg/d, was equal to 1-4 mg/kg/d of the peptide during the course of the study. The rationale for using this large amount was to facilitate detection of adverse effects of rhIGF-I within the time frame of the experimental protocol and to diminish the confounding effect of antibody production to rhIGF-I. This dose range has been shown to be pharmacologically active in short-term studies of normal rats(16). The rhIGF-I treatment regimen raised the circulating peptide concentration in normal and chronic PAN nephropathy rats. Reduced plasma IGF-I concentrations in animals with glomerular disease reflects massive proteinuria with losses of IGF binding proteins in the urine. Low serum IGF-I levels have been documented in acute PAN nephropathy(17) and in children with active nephrosis(18). This change may be a consequence of urinary excretion of IGF binding proteins because the RIA measures free IGF-I and peptide separated from binding proteins by acid chromatography(18). Alternatively, the low serum IGF-I concentrations may reflect reduced hepatic gene expression in PAN nephropathy(17).
Rats with normal renal function and severe glomerular disease tolerated the administration of rhIGF-I without overt metabolic sequelae. The modest reduction in the serum glucose concentration in rhIGF-I-treated rats with chronic PAN nephropathy after 4 wk may reflect occupancy of the insulin receptor by rhIGF-I(19). However, this side effect was not observed after 8-12 wk of glomerular disease. In addition, the hyperlipidemia associated with the nephrotic syndrome was attenuated by rhIGF-I therapy.
rhIGF-I, but not rhGH, promoted body growth in rats with chronic PAN nephropathy. This is consistent with studies that document an anabolic effect of rhIGF-I in rats with CRF for 1-2 wk(20, 21). Administration of rhIGF-I may induce larger increases in the concentration of this growth factor in the circulation and locally at the growth plate than can be achieved via rhGH treatment, in the face of ongoing urinary losses of IGF-I binding proteins. Higher concentrations of IGF-I may be necessary to overcome the inhibitory effect of elevated IGF-I binding proteins and to promote growth(22). The lack of effect of rhIGF-I on somatic and renal growth in normal rats contrasts with the report of Mehls et al.(16) who demonstrated that doses of rhIGF-I between 1-4 mg/kg/d enhanced BW gain. The highest dose also promoted renal enlargement.
In acute PAN nephropathy lasting 12 d, growth failure has been associated with reduced hepatic IGF-I and GH receptor gene expression(17); renal mRNA levels of IGF-I protein and receptor and GH receptor were not measured. We have demonstrated that chronic PAN nephropathy does not change renal IGF-I and IGF-I receptor mRNA levels; however, GH receptor gene expression was reduced compared with normal animals. This later abnormality may contribute to the impaired growth observed in these animals. A reduced abundance of hepatic IGF-I and GH receptor mRNA has also been observed in rats with reduced renal mass(14, 23). rhIGF-I treatment of rats with PAN nephropathy increased renal IGF-I and GH receptor gene expression. In contrast, administration of rhIGF-I to normal rats yielded a modest reduction in renal IGF-I mRNA levels. In rats with 5/6 nephrectomy, short-term GH treatment has no effect on IGF-I or GH receptor mRNA levels(14, 23). The disparate effects of rhIGF-I treatment on renal IGF-I and GH receptor gene expression in rats with chronic PAN nephropathy, 5/6 nephrectomy, and normal animals may be a consequence of urinary losses of IGF-I and differences in nutritional status that alter the intra-renal tissue concentration of free IGF-I. Additional studies are needed to determine whether the differences in IGF-I mRNA abundance after rhIGF-I treatment of normal and nephrotic rats are associated with changes in kidney immunoreactive levels of the growth factor.
There is an intra-renal GH-IGF-I axis(24). The kidney responds to GH administration with increased synthesis of IGF-I in tubular cells, primarily in the distal nephron(25). There are receptors for GH and IGF-I in the proximal and collecting tubules and binding of GH stimulates the synthesis of IGF-I(26, 27). IGF-I regulates solute and fluid transport in these nephron segments(28). The mesangial cell also has a specific membrane surface receptor for IGF-I(29). Binding of IGF-I to mesangial cells acts as a progression factor to increase proliferation(29). Local production of IGF-I in the kidney is increased when renal growth is stimulated, e.g. compensatory hypertrophy after unilateral nephrectomy(30) and early experimental diabetes mellitus(31).
Several studies have examined the in vivo effect of rhIGF-I in experimental renal disease. In rats with acute renal failure after bilateral renal artery clamping for 60-75 min, treatment with rhIGF-I for 3-7 d reduced catabolism and accelerated recovery of renal function(32, 33). Martin et al.(34) demonstrated an improved anabolic status but no amelioration of impaired kidney function in rats subjected to bilateral renal artery occlusion for 45 min. Administration of rhIGF-I to rats with reduced renal mass for 1-2 wk did not alter the GFR(20, 21). However, short-term provision of rhIGF-I to patients with CRF increased inulin and PAH clearances by 32 and 28%, respectively(35). In chronic PAN nephropathy, 12 wk of rhIGF-I treatment consistently doubled the inulin clearance without aggravating glomerulosclerosis or tubulointerstitial fibrosis. Although the improvement in GFR was most likely a direct action of rhIGF-I(19, 21), these studies do not exclude indirect effects such as inhibition of endogenous GH secretion. In the absence of serial measurements of GFR, we also cannot exclude the possibility that the beneficial effect of rhIGF-I was the consequence of the early administration of rhIGF-I rather than its long term use. It should be noted that an increased GFR despite persistently elevated proteinuria has been observed in cats with 5/6 nephrectomy fed a high protein/calorie diet(36).
The effects of rhIGF-I are in sharp contrast to the deleterious impact of rhGH on renal structure and function in chronic PAN nephropathy(9). The disparate effects of rhIGF-I and rhGH in PAN nephropathy are paralleled by studies in which mice that were transgenic for rhGH, but not IGF-I, developed proteinuria, mesangial accumulation of extracellular matrix and glomerulosclerosis(11, 12). It is conceivable that more prolonged administration of rhIGF-I or larger doses that raise the serum IGF-I concentration to the level in normal treated animals might result in sustained hyperfiltration and adverse effects on kidney structure and function in PAN nephropathy. The later concern is especially relevant in the context of nephrotic range proteinuria with urinary losses of IGF binding proteins. Because more unbound IGF-I is available for renal clearance, this may increase the intra-renal free IGF-I concentration. However, the current data suggest that the deleterious effects of GH on the kidney that we observed in rats with chronic PAN nephropathy are not mediated by increased systemic or intrarenal production of IGF-I(9).
In chronic PAN nephropathy, numerous factors contribute to the progressive kidney injury including glomerular hypertrophy(37), hyperfiltration(38), and renal lipid peroxidation(9). rhGH treatment exacerbated glomerular enlargement, enhanced renal oxidant damage and accelerated the deterioration in kidney function and structure(9). In contrast, administration of rhIGF-I increased GFR without augmenting glomerular hypertrophy or enhancing renal malondialdehyde content. Thus, our data suggest that glomerular hypertrophy in response to circulating, paracrine, and autocrine growth factors may be a more important factor in progressive renal disease than alterations in intraglomerular hemodynamics(37).
Long-term rhGH treatment for up to 5 y improves growth velocity and facilitates catch-up growth without loss of growth potential or evident renal toxicity in children with CRF(4–6). There have been no clinical studies of rhIGF-I for the treatment of short stature in children with CRF. rhIGF-I has been administered for an extended period to patients with resistance to exogenous insulin and refractory hyperglycemia(19, 39). Treatment of obese type II diabetic patients with rhIGF-I was associated with intolerable side effects such as edema, weight gain, arthralgias, myalgias and orthostatic hypotension(39). The efficacy and safety of rhIGF-I compared with rhGH in promoting growth in rats with chronic PAN nephropathy justify further investigation of rhIGF-I versus rhGH in the long-term treatment of growth failure in other experimental models of CRF, e.g. after 5/6 nephrectomy.
Abbreviations
- BW:
-
body weight
- CRF:
-
chronic renal failure
- FSGS:
-
focal segmental glomerulosclerosis
- PAN:
-
puromycin aminonucleoside
- rh:
-
recombinant human
References
Broyer M 1982 Growth in children with renal insufficiency. Pediatr Clin North Am 29: 991–1003
Fine RN 1992 Stimulating growth in uremic children. Kidney Int 42: 188–197
Mehls O, Ritz E, Hunziker EB, Eggli P, Heinrich U, Zapf J 1988 Improvement of growth and food utilization by human recombinant growth hormone in uremia. Kidney Int 33: 45–52
Fine RN, Kohaut EC, Brown D, Perlman AJ 1994 Genentech Cooperative Study Group. Growth after recombinant human growth hormone treatment in children with chronic renal failure: report of a multicenter randomized double-blind placebo-controlled study. J Pediatr 124: 374–382
Fine RN, Yadin O, Moulton L, Nelson PA, Boechat MI, Lippe BM 1994 Five years experience with recombinant human growth hormone treatment of children with chronic renal failure. J Pediatr Endocrinol 7: 1–12
Tonshoff B, Mehls O, Heinrich U, Blum WF, Ranke MB, Schauer A 1990 Growth-stimulating effects of recombinant human growth hormone in children with end-stage renal disease. J Pediatr 116: 561–566
El Nahas AM, Bassett AH, Cope GH, LeCarpenter JE 1991 Role of growth hormone in the development of experimental renal scarring. Kidney Int 40: 29–34
Allen DB, Fogo A, El-Hayek R, Langhough R, Friedman AL 1992 Effects of prolonged growth hormone administration in rats with chronic renal insufficiency. Pediatr Res 31: 406–410
Trachtman H, Futterweit S, Schwob N, Maesaka J, Valderrama E 1993 Recombinant human growth hormone exacerbates chronic puromycin aminonucleoside nephropathy in rats. Kidney Int 44: 1281–1288
Schaff-Blass E, Burstein S, Rosenfield RL 1984 Advances in diagnosis and treatment of short stature with special reference to the role of growth hormone. J Pediatr 104: 801–813
Doi T, Striker LJ, Gibson CC, Agodoa LYC, Brinster RL, Striker GE 1990 Glomerular lesions in mice transgenic for growth hormone and insulinlike growth factor-I. I. Relationship between increased glomerular size and mesangial sclerosis. Am J Pathol 137: 541–552
Doi T, Striker LJ, Kimata K, Peten EP, Yamada Y, Striker GE 1991 Glomerulosclerosis in mice transgenic for growth hormone: increased mesangial extracellular matrix is correlated with kidney mRNA levels. J Exp Med 173: 1287–1290
Grond J, Weening JJ, Elema JD 1984 Glomerular sclerosis in rats: comparison of the long-term effects of Adriamycin and aminonucleoside. Lab Invest 51: 277–285
Chan W, Valerie KC, Chan JCM 1993 Expression of insulin-like growth factor-1 in uremic rats: growth hormone resistance and nutritional intake. Kidney Int 43: 790–795
Ohkawa H, Ohishi N, Yagi K 1979 Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Anal Biochem 95: 351–358
Mehls O, Irzynjec T, Ritz E, Eden S, Kovacs G, Klaus G, Floege J, Mall G 1993 Effects of rhGH and rhIGF-I on renal growth and morphology. Kidney Int 44: 1251–1258
Thabet MA, Challa A, Chan W, Liu F, Hintz RL, Chan JCM 1994 Insulin-like growth factor and growth hormone receptor in nephrotic rats. Am J Physiol 266:E102–E106
Garin EH, Grant MB, Silverstein JH 1989 Insulinlike growth factors in patients with active nephrotic syndrome. Am J Dis Child 143: 865–867
Kolaczynski JW, Caro JF 1994 Insulin-like growth factor-I therapy in diabetes: physiologic basis, clinical benefits, and risks. Ann Intern Med 120: 47–55
Martin AA, Tomas FM, Owens PC, Knowles SE, Ballard FJ, Read LC 1991 IGF-I and its variant, des-(1-3)IGF-I, enhance growth in rats with reduced renal mass. Am J Physiol 261:F626–F633
Miller SB, Hansen VA, Hammerman MR 1990 Effects of growth hormone and IGF-I on renal function in rats with normal and reduced renal mass. Am J Physiol 259:F747–F751
Powell Dr, Liu F, Baker B, Lee PDK, Belsha CW, Brewer ED, Hintz RL 1993 Characterization of insulin-like growth factor binding protein-3 in chronic renal failure serum. Pediatr Res 33: 136–143
Tonschoff B, Eden S, Weiser E, Carlsson B, Robinson ICAF, Blum WF, Mehls O 1994 Reduced hepatic growth hormone (GH) receptor gene expression and increased plasma GH binding protein in experimental uremia. Kidney Int 45: 1085–1092
Hammerman MC 1989 The growth hormone-insulin-like growth factor axis in the kidney. Am J Physiol 257:F503–F514
Rogers SA, Miller SB, Hammerman MR 1990 Growth hormone stimulates IGF-I gene expression in isolated rat renal collecting duct. Am J Physiol 259:F474–F479
Pillion DJ, Haskell JF, Meezan E 1988 Distinct receptors for insulin-like growth factor I in rat renal glomeruli and tubules. Am J Physiol 255:E504–E512
Rogers SA, Miller SB, Hammerman MR 1991 Insulin-like growth factor 1 gene expression in isolated rat collecting duct is stimulated by epidermal growth factor. J Clin Invest 87: 347–351
Quigley R, Baum M 1991 Effects of growth hormone and insulin-like growth factor I on rabbit proximal convoluted tubule transport. J Clin Invest 88: 368–374
Doi T, Striker LJ, Elliot SJ, Conti FG, Striker GE 1989 Insulinlike growth factor-1 is a progression factor in human mesangial cells. Am J Pathol 134: 395–404
Stiles AD, Sosenko RS, D'Ercole AJ, Smith BT 1985 Relation of kidney tissue somatomedin C/insulin-like growth factor I to post-nephrectomy renal growth in the rat. Endocrinology 117: 2397–2401
Flyvberg A, Thorlacius-Ussing O, Naeraa R, Ingerslev J, Orskov H 1988 Kidney tissue somatomedin C and initial renal growth in diabetic and uninephrectomized rats. Diabetologia 31: 310–314
Ding H, Kopple JD, Cohen A, Hirschberg R 1993 Recombinant human insulin-like growth factor-I accelerates recovery and reduces catabolism in rats with ischemic acute renal failure. J Clin Invest 91: 2281–2287
Miller SB, Martin DR, Kissane J, Hammerman MR 1992 Insulin-like growth factor I accelerates recovery from ischemic acute tubular necrosis in the rat. Proc Natl Acad Sci USA 89: 11876–11880
Martin AA, Gillespie CM, Moore L, Ballard FJ, Read LC 1994 Effects of insulin-like growth factor-1 peptides in rats with acute renal failure. J Endocrinol 140: 23–32
Miller SB, Moulton M, O'Shea M, Hammerman MR 1994 Effects of IGF-I on renal structure in end-stage chronic renal failure. Kidney Int 46: 201–207
Adams LG, Plozin DJ, Osborne CA, O'Brien TD, Hostetter TH 1994 Influence of dietary protein/calorie intake on renal morphology and function in cats with 5:6 nephrectomy. Lab Invest 70: 347–357
Yoshida Y, Fogo A, Ichikawa I 1989 Glomerular hemodynamic changes vs. hypertrophy in experimental glomerular sclerosis. Kidney Int 35: 654–660
Brenner BM 1985 Nephron adaptation to renal injury or ablation. Am J Physiol 249:F324–F337
Jabri N, Schalch DS, Schwartz SL, Fischer JS, Kipnes MS, Radnik BJ, Turman NJ, Marcsisin VS, Guler HP 1994 Adverse effects of recombinant insulin-like growth factor 1 in obese insulin-resistant type II diabetic patients. Diabetes 43: 369–374
Acknowledgements
The recombinant human IGF-I used in these experiments was generously provided by Genentech, Inc. (South San Francisco, CA). The authors appreciate the careful review of this manuscript by Bernard Gauthier, M.D. They also wish to thank Douglas Yoon, Ph.D., for his assistance in performing the measurements of serum IGF-I concentration and Steven Moran for preparing the renal histopathology specimens.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Trachtman, H., Maesaka, J., Futterweit, S. et al. The Effect of Recombinant Human Insulin-Like Growth Factor-I on Chronic Puromycin Aminonucleoside Nephropathy in Rats. Pediatr Res 39, 13–19 (1996). https://doi.org/10.1203/00006450-199601000-00002
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199601000-00002
This article is cited by
-
Growth hormone aggravates glomerular sclerosis in the remnant kidney of 5/6 nephrectomized uremic rats
Clinical and Experimental Nephrology (1997)