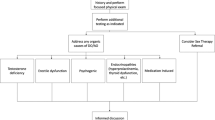
Key Points
-
Management decisions based purely on pure anatomical and/or neurological findings should be supplemented by greater attention to the quality of life of each patient with SCI, in a culturally sensitive way
-
The exact nature of neurogenic dysfunctions of the bladder, bladder neck and sphincter, and their coordinated function are specific in each individual patient
-
Diagnosis should be made after taking into account all available clinical data, including data from specific tests
-
Bladder management should form a part of the comprehensive management of a patient with SCI
-
Treatment should be conservative, and surgical techniques should be reserved for patients with a high risk of a loss of renal function, urinary incontinence and infection, despite proper use of conservative approaches
Abstract
The management of patients with neurogenic bladder has changed substantially over the past decades. Obtaining balanced lower urinary tract function has become possible in most patients, although, urological complications remain among the most serious complications these patients are likely to have and, even today, these can have a negative effect on quality of life. To this extent, patients with spinal cord injury (SCI) are likely to develop neurogenic bladder, and data are available on most aspects of neurogenic bladder in these patients. Data on physiology and pathophysiology form the basis of our understanding of patients' symptoms, and also provide a basis for the management of these patients. The use of conservative, and/or more invasive treatment measures, their complications and measures to prevent these complications, are all important clinical aspects that merit discussion. Considerable progress has been made in the urological management of patients with SCI over the past decades, but opportunities remain to make diagnosis more accurate and therapy more successful.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Girard, R. & Tricot, A. in La Paraplégie (ed. Maury. M) 622–627 (French) (Flammarion, 1981).
Lidal, I. B. et al. Mortality after spinal cord injury in Norway. J. Rehabil. Med. 39, 145–151 (2007).
Hackler, R. H. A. 25-year prospective mortality study in the spinal cord injured patient: comparison with the long-term living paraplegic. J. Urol. 117, 486–488 (1977).
Wyndaele, J. J. et al. in Incontinence (eds Abrams, P., Cardozo, L., Khoury, S. & Wein, A.) 793–960 (ICUD, 2009).
Weld, K. J. & Dmochowski, R. R. Effect of bladder management on urological complications in spinal cord injured patients. J. Urol. 163, 768–772 (2000).
Ruffion, A. et al. Renal failure and neurogenic bladder. Prog. Urol. 17, 424–430 (French) (2007).
Changlai, S. P., Bih, L. & Lin, D. B. Tc-99m MAG3 renal studies: renogram and effective renal plasma flow in spinal cord injury patients. Urol. Int. 63, 224–227 (1999).
Pagliacci, M. C. et al. Hospital care of postacute spinal cord lesion patients in Italy: analysis of readmissions into the GISEM study. Am. J. Phys. Med. Rehabil. 87, 619–626 (2008).
Kuzeyli, K., Cakir, E., Baykal, S. & Karaarslan, G. Diabetes insipidus secondary to penetrating spinal cord trauma: case report and literature review. Spine 26, E510–E511 (2001).
de Groat, W. C., Griffiths, D. & Yoshimura, N. Neural control of the lower urinary tract. Compr. Physiol. 5, 327–396 (2015).
Wyndaele, M. et al. Exploring associations between lower urinary tract symptoms (LUTS) and gastrointestinal (GI) problems in women: a study in women with urological and GI problems versus a control population. BJU Int. 115, 958–967 (2015).
Persyn, S. et al. Mechanisms of pelvic organ cross-talk: impact of urethral ligation on the inhibitory rectovesical reflex. J. Urol. 192, 1574–1579 (2014).
Minagawa, T. et al. Mechanisms of pelvic organ cross-talk: 2. Impact of colorectal distention on afferent nerve activity of the rat bladder. J. Urol. 190, 1123–1130 (2013).
Linsenmeyer, T. A. & Stone, J. M. in Rehabilitation Medicine: Principles and Practice (ed. DeLisa, J. A.) 1073–1106 (Lippincott-Raven, 1998).
Wyndaele, M. & Wyndaele, J. J. Incidence, prevalence and epidemiology of spinal cord injury: what learns a worldwide literature survey? Spinal Cord 44, 523–529 (2006).
Stöhrer, M. et al. The standardization of terminology in neurogenic lower urinary tract dysfunction: with suggestions for diagnostic procedures: International Continence Society Standardization Committee. Neurourol. Urodyn. 18, 139–158 (1999).
Jeong, S. J., Cho, S. Y. & Oh, S. J. Spinal cord/brain injury and neurogenic bladder. Urol. Clin. North Am. 37, 537–546 (2010).
Wyndaele, J. J. Investigation of the afferent nerves of the lower urinary tract in patients with 'complete' and 'incomplete' spinal cord injury. Paraplegia 29, 490–494 (1991).
Kirshblum, S. C. International standards for neurological classification of spinal cord injury. J. Spinal Cord Med. 34, 535–546 (2011).
Devivo, M. J. et al. Standardization of data analysis and reporting of results from the International Spinal Cord Injury Core Data Set. Spinal Cord 49, 596–599 (2011).
Abrams, P. et al. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol. Urodyn. 21, 167–178 (2002).
Naoemova, I., De Wachter, S. & Wyndaele, J. J. Comparison of sensation-related voiding patterns between continent and incontinent women: a study with a 3-day sensation-related bladder diary (SR-BD). Neurourol. Urodyn. 27, 511–514 (2008).
Young, M. & Rovner, E. S. in Textbook of the Neurogenic Bladder 3rd edn (eds Corcos, J., Ginsberg, D. & Karsenty, G.) 351–353 (CRC Press, 2016).
Biering-Sørensen, F. et al. International lower urinary tract function basic spinal cord injury data set. Spinal Cord 46, 325–330 (2008).
Welk, B. et al. The validity and reliability of the neurogenic bladder symptom score (NBSS). J. Urol. 192, 452–457 (2014).
Hill, M. R. et al. Quality of life instruments and definitions in individuals with spinal cord injury: a systematic review. Spinal Cord 48, 438–450 (2010).
Wyndaele, M. et al. Development and psychometric evaluation of a Dutch questionnaire for the assessment of anorectal and lower urinary tract symptoms. Acta Gastroenterol. Belg. 74, 295–303 (2011).
Bacsu, C. & Lemack, G. E. in Textbook of the Neurogenic Bladder 3rd edn (eds Corcos, J., Ginsberg, D. & Karsenty, G.) 337–345 (CRC Press, 2016).
Norris, J. P. & Staskin, D. R. History, physical examination, and classification of neurogenic voiding dysfunction. Urol. Clin. North Am. 23, 337–343 (1996).
Schurch, B., Schmid, D. M. & Kaegi, K. Value of sensory examination in predicting bladder function in patients with T12-L1 fractures and spinal cord injury. Arch. Phys. Med. Rehabil. 84, 83–89 (2003).
Blaivas, J. G., Zayed, A. A. & Labib, K. B. The bulbocavernosus reflex in urology: a prospective study of 299 patients. J. Urol. 126, 197–199 (1981).
Wyndaele, J. J. Correlation between clinical neurological data and urodynamic function in spinal cord injured patients. Spinal Cord 35, 213–216 (1997).
Watanabe, T. et al. High incidence of occult neurogenic bladder dysfunction in neurologically intact patients with thoracolumbar spinal injuries. J. Urol. 159, 965–968 (1998).
Pannek, J. et al. Prostate size and PSA serum levels in male patients with spinal cord injury. Urology 62, 845–848 (2003).
Bartoletti, R. et al. Prostate growth and prevalence of prostate diseases in early onset spinal cord injuries. Eur. Urol. 56, 142–148 (2009).
Pannek, J. et al. Prostate volume in male patients with spinal cord injury: a question of nerves? BJU Int. 112, 495–500 (2013).
Wyndaele, J. J., Del Popolo, G., Kovindha, A., Pannek, J. & Wöllner, J. in ISCOS Textbook on Comprehensive Management of Spinal Cord Injuries (ed. Chhabra, H. S.) (Lippincott Williams and Wilkins, 2015)
Konety, B. R. et al. Evaluation of the effect of spinal cord injury on serum PSA levels. Urology 56, 82–86 (2000).
Torricelli, F. C. et al. PSA levels in men with spinal cord injury and under intermittent catheterization. Neurourol. Urodyn. 30, 1522–1524 (2011).
Wyndaele, J. J. A critical review of urodynamic investigations in spinal cord injury patients. Paraplegia 22, 138–144 (1984).
Brucker, B. M., Kelly, C. E. & Nitti, V. W. in Textbook of the Neurogenic Bladder 3rd edn (eds Corcos, J., Ginsberg, D. & Karsenty, G.) 373–382 (CRC Press, 2016).
Alexander, M. S. et al. International standards to document remaining autonomic function after spinal cord injury. Spinal Cord 47, 36–43 (2009).
Wyndaele, J. J. et al. The use of one-channel water cystometry in patients with a spinal cord lesion: practicalities, clinical value and limitations for the diagnosis of neurogenic bladder dysfunction. Spinal Cord 47, 526–530 (2009).
Biering-Sørensen, F., Craggs, M., Kennelly, M., Schick, E. & Wyndaele, J. J. International Urodynamic Basic Spinal Cord Injury Data Set. Spinal Cord 46, 513–516 (2008).
Wyndaele, J. J. & Vodusek, D. B. Approach to the male patient with lower urinary tract dysfunction. Handb. Clin. Neurol. 130, 143–164 (2015).
Ersoz, M. & Akyuz, M. Bladder-filling sensation in patients with spinal cord injury and the potential for sensation-dependent bladder emptying. Spinal Cord 42, 110–116 (2004).
Madersbacher, H. Combined pressure, flow, EMG and X-ray studies for the evaluation of neurologic bladder disturbance: technique. Urol. Int. 32, 176–183 (1977).
Perkash, I. & Friedland, G. W. Ultrasonographic detection of false passages arising from the posterior urethra in spinal cord injury patients. J. Urol. 137, 701–702 (1987).
Latthe, P. M., Foon, R. & Toozs-Hobson, P. Prophylactic antibiotics in urodynamics: a systematic review of effectiveness and safety. Neurourol. Urodyn. 27, 167–173 (2008).
Bellucci, C. H. et al. Acute spinal cord injury — do ambulatory patients need urodynamic investigations? J. Urol. 189, 1369–1373 (2013).
Ronzoni, G. et al. The ice-water test in the diagnosis and treatment of the neurologic bladder. Br. J. Urol. 79, 698–701 (1997).
Van Meel, T., De Wachter, S. & Wyndaele, J. J. Repeated ice water tests and electrical perception threshold determination to detect a neurologic cause of detrusor overactivity. Urology 70, 772–776 (2007).
Sidi, A. A., Dykstra, D. D. & Peng, W. Bethanechol supersensitivity test, rhabdosphincter electromyography and bulbocavernosus reflex latency in the diagnosis of neurologic detrusor areflexia. J. Urol. 140, 335–337 (1988).
De, E. J. et al. Diagnostic discordance of electromyography (EMG) versus voiding cystourethrogram (VCUG) for detrusor-external sphincter dyssynergy (DESD). Neurourol. Urodyn. 24, 616–621 (2005).
Podnar, S. & Vodušek, D. B. in Aminoff's Electrodiagnosis in Clinical Neurology 6th edn (ed. Aminoff, M. J.) 673–695 (Elsevier, 2012).
Lee, J. P. & Dang, A. T. Evaluation of methods to estimate glomerular filtration rate versus actual drug clearance in patients with chronic spinal cord injury. Spinal Cord 49, 1158–1163 (2011).
Cameron, A. P., Lai, J., Saigal, C. S. & Clemens, J. Q. & NIDDK Urological Diseases in America Project. Urological surveillance and medical complications after spinal cord injury in the United States. Urology 86, 506–510 (2015).
Willson, M. et al. Nursing interventions to reduce the risk of catheter-associated urinary tract infection: part 2: staff education, monitoring, and care techniques. J. Wound Ostomy Continence Nurs. 36, 137–154 (2009).
Hansen, R. B., Biering-Sørensen, F. & Kristensen, J. K. Bladder emptying over a period of 10–45 years after a traumatic spinal cord injury. Spinal Cord 42, 631–637 (2004).
Biering-Sørensen, F., Craggs, M., Kennelly, M., Schick, E. & Wyndaele, J. J. International urinary tract imaging basic spinal cord injury data set. Spinal Cord 47, 379–383 (2009).
Drake, M. J. et al. Prospective evaluation of urological effects of aging in chronic spinal cord injury by method of bladder management. Neurourol. Urodyn. 24, 111–116 (2005).
Parker, D. et al. Nursing interventions to reduce the risk of catheter-associated urinary tract infection. Part 1: Catheter selection. J. Wound Ostomy Continence Nurs. 36, 23–34 (2009).
Kunin, M. C. & McCormack, R. C. Prevention of catheter-induced urinary-tract infections by sterile closed drainage. N. Engl. J. Med. 274, 1155–1161 (1966).
Gould, C. V., Umscheid, C. A., Agarwal, R. K., Kuntz, G. & Pegues, D. A. Guideline for prevention of catheter-associated urinary tract infections 2009. Infect. Control Hosp. Epidemiol. 31, 319–326 (2010).
Guttmann, L. & Frankel, H. The value of intermittent catheterization in the early management of traumatic paraplegia and tetraplegia. Paraplegia 4, 63–84 (1966).
Burns, A. S., Rivas, D. A. & Ditunno, J. F. The management of neurogenic bladder and sexual dysfunction after spinal cord injury. Spine 26 (Suppl.), S129–S136 (2001).
Wyndaele, J. J., Madersbacher, H. & Kovindha, A. Conservative treatment of the neuropathic bladder in spinal cord injured patients. Spinal Cord 39, 294–300 (2001).
Wyndaele, J. J. Intermittent catheterization: which is the optimal technique? Spinal Cord 40, 432–437 (2002).
Igawa, Y., Wyndaele, J. J. & Nishizawa, O. Catheterization: possible complications and their prevention and treatment. Int. J. Urol. 15, 481–485 (2008).
Clark, J. F. et al. A cost-effectiveness analysis of long-term intermittent catheterisation with hydrophilic and uncoated catheters. Spinal Cord 54, 73–77 (2016).
Brooks, M. E. & Braf, Z. F. Oxybutynin chloride (ditrophan) — clinical uses and limitations. Paraplegia 18, 64–68 (1980).
Wyndaele, J. J. et al. Neurologic urinary incontinence. Neurourol. Urodyn. 29, 159–164 (2010).
Goldman, H. B., Wyndaele, J. J., Kaplan, S. A., Wang, J. T. & Ntanios, F. Defining response and non-response to treatment in patients with overactive bladder: a systematic review. Curr. Med. Res. Opin. 30, 509–526 (2014).
Appell, R. A. Overactive bladder in special patient populations. Rev. Urol. 8 (Suppl. 8), S37–S41 (2003).
Madhuvrata, P. et al. Anticholinergic drugs for adult neurogenic detrusor overactivity: a systematic review and meta-analysis. Eur. Urol. 62, 816–830 (2012).
Wöllner, J. & Pannek, J. Initial experience with the treatment of neurogenic detrusor overactivity with a new β-3 agonist (mirabegron) in patients with spinal cord injury. Spinal Cord 54, 78–82 (2016).
Angulo, J. et al. Tadalafil enhances the inhibitory effects of tamsulosin on neurogenic contractions of human prostate and bladder neck. J. Sex. Med. 9, 2293–2306 (2012).
Abrams, P. et al. Tamsulosin: efficacy and safety in patients with neurogenic lower urinary tract dysfunction due to suprasacral spinal cord injury. J. Urol. 170, 1242–1251 (2003).
Barendrecht, M. M. et al. Is the use of parasympathomimetics for treating an underactive urinary bladder evidence-based? BJU Int. 99, 749–752 (2007).
Opisso, E. et al. Patient controlled versus automatic stimulation of pudendal nerve afferents to treat neurogenic detrusor overactivity. J. Urol. 180, 1403–1408 (2008).
Andrews, B. J. & Reynard, J. M. Transcutaneous posterior tibial nerve stimulation for treatment of detrusor hyperreflexia in spinal cord injury. J. Urol. 170, 926 (2003).
Primus, G., Kramer, G. & Pummer, K. Restoration of micturition in patients with acontractile and hypocontractile detrusor by transurethral electrical bladder stimulation. Neurourol. Urodyn. 15, 489–497 (1996).
Lombardi, G. et al. Intravesical electrostimulation versus sacral neuromodulation for incomplete spinal cord patients suffering from neurogenic non-obstructive urinary retention. Spinal Cord 51, 571–578 (2013).
Hansen, J. et al. Treatment of neurogenic detrusor overactivity in spinal cord injured patients by conditional electrical stimulation. J. Urol. 173, 2035–2039 (2005).
Læssøe, L. et al. Effects of ejaculation by penile vibratory stimulation on bladder capacity in men with spinal cord lesions. J. Urol. 169, 2216–2219 (2003).
Schurch, B. et al. Botulinum-A toxin for treating detrusor hyperreflexia in spinal cord injured patients: a new alternative to anticholinergic drugs? Preliminary results. J. Urol. 164, 692–697 (2000).
Mangera, A. et al. Contemporary management of lower urinary tract disease with botulinum toxin A: a systematic review of botox (onabotulinumtoxinA) and dysport (abobotulinumtoxinA). Eur. Urol. 60, 784–795 (2011).
US Food and Drug Administration. FDA news release. FDAhttp://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm336101.htm (2013).
Mehta, S. et al. Meta-analysis of botulinum toxin A detrusor injections in the treatment of neurogenic detrusor overactivity after spinal cord injury. Arch. Phys. Med. Rehabil. 94, 1473–1481 (2013).
Finazzi-Agrò, E. et al. The use of oxybutynin in patients treated by means of botulinum neurotoxin A for neurogenic detrusor overactivity: an observational study. Spinal Cord 51, 637–641 (2013).
Kennelly, M. et al. Long-term efficacy and safety of onabotulinumtoxinA in patients with urinary incontinence due to neurogenic detrusor overactivity: an interim analysis. Urology 81, 491–497 (2013).
Wyndaele, J. J. & Van Dromme, S. Muscular weakness as side effect of botulinum toxin injection for neurogenic detrusor overactivity. Spinal Cord 40, 599–600 (2002).
Dykstra, D. D., Sidi, A. A., Scott, A. B., Pagel, J. M. & Goldish, G. D. Effects of botulinum A toxin on detrusor-sphincter dyssynergia in spinal cord injury patients. J. Urol. 139, 919–922 (1988)
Kessler, T. M. et al. Sacral neuromodulation for neurogenic lower urinary tract dysfunction: systematic review and meta-analysis. Eur. Urol. 58, 865–874 (2010).
Sievert, K. D. et al. Early sacral neuromodulation prevents urinary incontinence after complete spinal cord injury. Ann. Neurol. 67, 74–84 (2010).
Brindley, G. S. The first 500 patients with sacral anterior root stimulator implants: general description. Paraplegia 32, 795–805 (1994).
Drake, M. J. et al. in Incontinence 5th edn (eds Abrams, P., Cardozo, L., Khoury, S. & Wein, A.) 827–1000 (ICUD, 2013).
Brillhart, B. & Stewart, A. Education as the key to rehabilitation. Nurs. Clin. North Am. 24, 675–680 (1989).
About elearnSCI.org. elearnSCI [online] http://www.elearnSCI.org (2015).
Wyndaele, J. J. et al. Clean intermittent catheterization and urinary tract infection: review and guide for future research. BJU Int. 110, E910–E917 (2012).
Wyndaele, J. J., Del Popolo, G., Kessler, T. & Pannek, J. in ISCOS Textbook on Comprehensive Management of Spinal Cord Injuries (ed. Chhabra, H. S.) (Lippincott Williams and Wilkins, 2015).
Vaidyanathan, S., Soni, B. M., Dundas, S. & Krishnan, K. R. Urethral cytology in spinal cord injury patients performing intermittent catheterization. Paraplegia 32, 493–500 (1994).
Naber, K. G. et al. EAU guidelines for the management of urinary and male genital tract infections. Urinary Tract Infection (UTI) Working Group of the Health Care Office (HCO) of the European Association of Urology (EAU). Eur. Urol. 40, 576–588 (2001).
Wyndaele, J. J., De Sy, W. A. & Claessens, H. Evaluation of different methods of bladder drainage used in the early care of spinal cord injury patients. Paraplegia 23, 18–26 (1985).
Ku, J. H., Jung, T. Y., Lee, J. K., Park, W. H. & Shim, H. B. Influence of bladder management on epididymo-orchitis in patients with spinal cord injury: clean intermittent catheterization is a risk factor for epididymo-orchitis. Spinal Cord 44, 165–169 (2006).
Krebs, J., Bartel, P. & Pannek, J. Bacterial persistence in the prostate after antibiotic treatment of chronic bacterial prostatitis in men with spinal cord injury. Urology 83, 515–520 (2014).
Siroky, M. B. Pathogenesis of bacteriuria and infection in the spinal cord injured patient. Am. J. Med. 113 (Suppl. 1A), 67S–79S (2002).
Bartel, P., Krebs, J., Wöllner, J., Göcking, K. & Pannek, J. Bladder stones in patients with spinal cord injury: a long-term study. Spinal Cord 52, 295–297 (2014).
Lee, W. Y. et al. Risk of prostate and bladder cancers in patients with spinal cord injury: a population-based cohort study. Urol. Oncol. 32, 51.e1–51.e7 (2014).
Welk, B., McIntyre, A., Teasell, R., Potter, P. & Loh, E. Bladder cancer in individuals with spinal cord injuries. Spinal Cord 51, 516–521 (2013).
Ho, C. H. et al. Chronic indwelling urinary catheter increase the risk of bladder cancer, even in patients without spinal cord injury. Medicine (Baltimore) 94, e1736 (2015).
El Masri, W. S., Patil, S., Prasanna, K. V. & Chowdhury, J. R. To cystoscope or not to cystoscope patients with traumatic spinal cord injuries managed with indwelling urethral or suprapubic catheters? That is the question! Spinal Cord 52, 49–53 (2014).
Kalisvaart, J. F., Katsumi, H. K., Ronningen, L. D. & Hovey, R. M. Bladder cancer in spinal cord injury patients. Spinal Cord 48, 257–261 (2010).
Wyndaele, J. J. et al. Prostate cancer: a hazard also to be considered in the ageing male patient with spinal cord injury. Spinal Cord 36, 299–302 (1998).
Scott, P. A. Sr, Perkash, I., Mode, D., Wolfe, V. A. & Terris, M. K. Prostate cancer diagnosed in spinal cord-injured patients is more commonly advanced stage than in able-bodied patients. Urology 63, 509–512 (2004).
Brandes, S. B., Smith, J. B., Longo, W. E., Virgo, K. S. & Johnson, F. E. Renal cell carcinoma in patients with prior spinal cord injury. J. Spinal Cord Med. 24, 251–256 (2001).
Le Fort, M., Perrouin-Verbe, M. A. & Labat, J. J. in Textbook of the neurogenic bladder (eds Corcos, J., Ginsberg, D. & Karsenty, G.) 773–780 (CRC Press, 2016).
Sellers, D. J. & Chess-Williams, R. Muscarinic agonists and antagonists: effects on the urinary bladder. Handb. Exp. Pharmacol. 208, 375–400 (2012).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Wyndaele, JJ. The management of neurogenic lower urinary tract dysfunction after spinal cord injury. Nat Rev Urol 13, 705–714 (2016). https://doi.org/10.1038/nrurol.2016.206
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrurol.2016.206
This article is cited by
-
Real-time prediction of bladder urine leakage using fuzzy inference system and dual Kalman filtering in cats
Scientific Reports (2024)
-
Advanced micro-/nanotechnologies for exosome encapsulation and targeting in regenerative medicine
Clinical and Experimental Medicine (2023)
-
Functional, morphological and molecular characteristics in a novel rat model of spinal sacral nerve injury-surgical approach, pathological process and clinical relevance
Scientific Reports (2022)
-
Urological Care After Spinal Cord Injury
Current Physical Medicine and Rehabilitation Reports (2022)
-
A general framework for automatic closed-loop control of bladder voiding induced by intraspinal microstimulation in rats
Scientific Reports (2021)