Key Points
-
Atypical parkinsonism is a common presentation in patients with frontotemporal dementia (FTD)
-
Richardson syndrome in FTD is most commonly associated with mutations in the MAPT gene
-
A corticobasal syndrome is most frequently observed in patients who have mutations in the gene that encodes progranulin
-
C9orf72 gene expansions are the most common cause of hereditary motor neuron disease with FTD, and might present in combination with symmetrical parkinsonism
-
Mutations in the VCP, TARDBP and TREM2 genes are rare causes of parkinsonism and motor neuron disease in FTD
-
Stereotypies are common in patients with FTD, and should aid diagnosis
Abstract
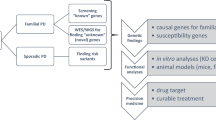
Frontotemporal dementia (FTD) refers to a group of clinically and genetically heterogeneous neurodegenerative disorders that are a common cause of adult-onset behavioural and cognitive impairment. FTD often presents in combination with various hyperkinetic or hypokinetic movement disorders, and evidence suggests that various genetic mutations underlie these different presentations. Here, we review the known syndromatic–genetic correlations in FTD. Although no direct genotype–phenotype correlations have been identified, mutations in multiple genes have been associated with various presentations. Mutations in the genes that encode microtubule-associated protein tau (MAPT) and progranulin (PGRN) can manifest as symmetrical parkinsonism, including the phenotypes of Richardson syndrome and corticobasal syndrome (CBS). Expansions in the C9orf72 gene are most frequently associated with familial FTD, typically combined with motor neuron disease, but other manifestations, such as symmetrical parkinsonism, CBS and multiple system atrophy-like presentations, have been described in patients with these mutations. Less common gene mutations, such as those in TARDBP, CHMP2B, VCP, FUS and TREM2, can also present as atypical parkinsonism. The most common hyperkinetic movement disorders in FTD are motor and vocal stereotypies, which have been observed in up to 78% of patients with autopsy-proven FTD. Other hyperkinetic movements, such as chorea, orofacial dyskinesias, myoclonus and dystonia, are also observed in some patients with FTD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Mercy, L., Hodges, J. R., Dawson, K., Barker, R. A. & Brayne, C. Incidence of early-onset dementias in Cambridgeshire, United Kingdom. Neurology 71, 1496–1499 (2008).
Perry, D. C. & Miller, B. L. Frontotemporal dementia. Semin. Neurol. 33, 336–341 (2013).
Seltman, R. E. & Matthews, B. R. Frontotemporal lobar degeneration: epidemiology, pathology, diagnosis and management. CNS Drugs 26, 841–870 (2012).
Teichmann, M. et al. Deciphering logopenic primary progressive aphasia: a clinical, imaging and biomarker investigation. Brain 136, 3474–3488 (2013).
Fujioka, S. & Wszolek, Z. K. Clinical aspects of familial forms of frontotemporal dementia associated with parkinsonism. J. Mol. Neurosci. 45, 359–365 (2011).
Siuda, J., Fujioka, S. & Wszolek, Z. K. Parkinsonian syndrome in familial frontotemporal dementia. Parkinsonism Relat. Disord. 20, 957–964 (2014).
Neary, D. et al. Frontotemporal lobar degeneration: a consensus on clinical diagnostic criteria. Neurology 51, 1546–1554 (1998).
Rascovsky, K. et al. Sensitivity of revised diagnostic criteria for the behavioural variant of frontotemporal dementia. Brain 134, 2456–2477 (2011).
The Lund and Manchester groups. Clinical and neuropathological criteria for frontotemporal dementia. J. Neurol. Neurosurg. Psychiatry 57, 416–418 (1994).
Diehl-Schmid, J. et al. Extrapyramidal signs, primitive reflexes and incontinence in fronto-temporal dementia. Eur. J. Neurol. 14, 860–864 (2007).
Padovani, A., Agosti, C., Premi, E., Bellelli, G. & Borroni, B. Extrapyramidal symptoms in frontotemporal dementia: prevalence and clinical correlations. Neurosci. Lett. 422, 39–42 (2007).
Ling, H. et al. Does corticobasal degeneration exist? A clinicopathological re-evaluation. Brain 133, 2045–2057 (2010).
Stamelou, M., Quinn, N. P. & Bhatia, K. P. 'Atypical' atypical parkinsonism: new genetic conditions presenting with features of progressive supranuclear palsy, corticobasal degeneration, or multiple system atrophy — a diagnostic guide. Mov. Disord. 28, 1184–1199 (2013).
Respondek, G. et al. The phenotypic spectrum of progressive supranuclear palsy: a retrospective multicenter study of 100 definite cases. Mov. Disord. 29, 1758–1766 (2014).
Armstrong, M. J. et al. Criteria for the diagnosis of corticobasal degeneration. Neurology 80, 496–503 (2013).
Mathew, R., Bak, T. H. & Hodges, J. R. Diagnostic criteria for corticobasal syndrome: a comparative study. J. Neurol. Neurosurg. Psychiatry 83, 405–410 (2012).
Dickson, D. W., Ahmed, Z., Algom, A. A., Tsuboi, Y. & Josephs, K. A. Neuropathology of variants of progressive supranuclear palsy. Curr. Opin. Neurol. 23, 394–400 (2010).
Williams, D. R. et al. Characteristics of two distinct clinical phenotypes in pathologically proven progressive supranuclear palsy: Richardson's syndrome and PSP-parkinsonism. Brain 128, 1247–1258 (2005).
Foster, N. L. et al. Frontotemporal dementia and parkinsonism linked to chromosome 17: a consensus conference. Ann. Neurol. 41, 706–715 (1997).
Hutton, M. et al. Association of missense and 5′-splice-site mutations in tau with the inherited dementia FTDP-17. Nature 393, 702–705 (1998).
Baker, M. et al. Mutations in progranulin cause tau-negative frontotemporal dementia linked to chromosome 17. Nature 442, 916–919 (2006).
Ludolph, A. C. et al. Tauopathies with parkinsonism: clinical spectrum, neuropathologic basis, biological markers, and treatment options. Eur. J. Neurol. 16, 297–309 (2009).
Yu, C. E. et al. The spectrum of mutations in progranulin: a collaborative study screening 545 cases of neurodegeneration. Arch. Neurol. 67, 161–170 (2010).
van Swieten, J. C. & Heutink, P. Mutations in progranulin (GRN) within the spectrum of clinical and pathological phenotypes of frontotemporal dementia. Lancet Neurol. 7, 965–974 (2008).
Boeve, B. F. & Hutton, M. Refining frontotemporal dementia with parkinsonism linked to chromosome 17: introducing FTDP-17 (MAPT) and FTDP-17 (PGRN). Arch. Neurol. 65, 460–464 (2008).
Rohrer, J. D. et al. The heritability and genetics of frontotemporal lobar degeneration. Neurology 73, 1451–1456 (2009).
Arima, K. et al. Two brothers with frontotemporal dementia and parkinsonism with an N279K mutation of the tau gene. Neurology 54, 1787–1795 (2000).
Yasuda, M. et al. A mutation in the microtubule- associated protein tau in pallido–nigro–luysian degeneration. Neurology 53, 864–868 (1999).
Pickering-Brown, S. M. et al. Inherited frontotemporal dementia in nine British families associated with intronic mutations in the tau gene. Brain 125, 732–751 (2002).
Bermingham, N., Cowie, T. F., Paine, M., Storey, E. & McLean, C. Frontotemporal dementia and parkinsonism linked to chromosome 17 in a young Australian patient with the G389R Tau mutation. Neuropathol. Appl. Neurobiol. 34, 366–370 (2008).
Rossi, G. et al. The G389R mutation in the MAPT gene presenting as sporadic corticobasal syndrome. Mov. Disord. 23, 892–895 (2008).
Tacik, P. et al. A novel tau mutation in exon 12, p. Q336H, causes hereditary pick disease. J. Neuropathol. Exp. Neurol. 74, 1042–1052 (2015).
Tacik, P. et al. A novel tau mutation, p. K317N, causes globular glial tauopathy. Acta Neuropathol. 130, 199–214 (2015).
Chaunu, M. P. et al. Juvenile frontotemporal dementia with parkinsonism associated with tau mutation G389R. J. Alzheimers Dis. 37, 769–776 (2013).
Lossos, A. et al. Frontotemporal dementia and parkinsonism with the P301S tau gene mutation in a Jewish family. J. Neurol. 250, 733–740 (2003).
Sperfeld, A. D. et al. FTDP-17: an early phenotype with parkinsonism and epileptic seizures caused by a novel mutation. Ann. Neurol. 46, 708–715 (1999).
Werber, E., Klein, C., Grünfeld, J. & Rabey, J. M. Phenotypic presentation of frontotemporal dementia with parkinsonism-chromosome 17 type P301S in a patient of Jewish–Algerian origin. Mov. Disord. 18, 595–598 (2003).
Boeve, B. F. et al. Longitudinal characterization of two siblings with frontotemporal dementia and parkinsonism linked to chromosome 17 associated with the S305N tau mutation. Brain 128, 752–772 (2005).
Skoglund, L. et al. The tau S305S mutation causes frontotemporal dementia with parkinsonism. Eur. J. Neurol. 15, 156–161 (2008).
Lynch, T. et al. Clinical characteristics of a family with chromosome 17-linked disinhibition−dementia−parkinsonism−amyotrophy complex. Neurology 44, 1878–1884 (1994).
Rohrer, J. D. et al. Novel L284R MAPT mutation in a family with an autosomal dominant progressive supranuclear palsy syndrome. Neurodegener. Dis. 8, 149–152 (2011).
Ogaki, K. et al. Analyses of the MAPT, PGRN, and C9orf72 mutations in Japanese patients with FTLD, PSP, and CBS. Parkinsonism Relat. Disord. 19, 15–20 (2013).
Spina, S. et al. The tauopathy associated with mutation +3 in intron 10 of tau: characterization of the MSTD family. Brain 131, 72–89 (2008).
Baba, Y. et al. Clinical and genetic features of families with frontotemporal dementia and parkinsonism linked to chromosome 17 with a P301S tau mutation. J. Neural Transm. (Vienna) 114, 947–950 (2007).
Kouri, N. et al. Novel mutation in MAPT exon 13 (p.N410H) causes corticobasal degeneration. Acta Neuropathol. 127, 271–282 (2014).
Kelly, B. J. et al. Prominent phenotypic variability associated with mutations in progranulin. Neurobiol. Aging 30, 739–751 (2009).
Le Ber, I. et al. Phenotype variability in progranulin mutation carriers: a clinical, neuropsychological, imaging and genetic study. Brain 131, 732–746 (2008).
Davion, S. et al. Clinicopathologic correlation in PGRN mutations. Neurology 69, 1113–1121 (2007).
Masellis, M. et al. Novel splicing mutation in the progranulin gene causing familial corticobasal syndrome. Brain 129, 3115–3123 (2006).
Josephs, K. A. et al. Neuropathologic features of frontotemporal lobar degeneration with ubiquitin-positive inclusions with progranulin gene (PGRN) mutations. J. Neuropathol. Exp. Neurol. 66, 142–151 (2007).
Spina, S. et al. Corticobasal syndrome associated with the A9D progranulin mutation. J. Neuropathol. Exp. Neurol. 66, 892–900 (2007).
Benussi, L. et al. A novel deletion in progranulin gene is associated with FTDP-17 and CBS. Neurobiol. Aging 29, 427–435 (2008).
Benussi, L. et al. Progranulin Leu271LeufsX10 is one of the most common FTLD and CBS associated mutations worldwide. Neurobiol. Dis. 33, 379–385 (2009).
Rusina, R. et al. FTLD-TDP with motor neuron disease, visuospatial impairment and a progressive supranuclear palsy-like syndrome: broadening the clinical phenotype of TDP-43 proteinopathies. A report of three cases. BMC Neurol. 11, 50 (2011).
Renton, A. E. et al. A hexanucleotide repeat expansion in C9ORF72 is the cause of chromosome 9p21-linked ALS-FTD. Neuron 72, 257–268 (2011).
Khan, B. K. et al. Atypical, slowly progressive behavioural variant frontotemporal dementia associated with C9ORF72 hexanucleotide expansion. J. Neurol. Neurosurg. Psychiatry 83, 358–364 (2012).
Van Langenhove, T. et al. Distinct clinical characteristics of C9orf72 expansion carriers compared with GRN, MAPT, and nonmutation carriers in a Flanders–Belgian FTLD cohort. JAMA Neurol. 70, 365–373 (2013).
Boeve, B. F. et al. Characterization of frontotemporal dementia and/or amyotrophic lateral sclerosis associated with the GGGGCC repeat expansion in C9ORF72. Brain 135, 765–783 (2012).
O'Dowd, S. et al. C9ORF72 expansion in amyotrophic lateral sclerosis/frontotemporal dementia also causes parkinsonism. Mov. Disord. 27, 1072–1074 (2012).
Goldman, J. S. et al. Multiple system atrophy and amyotrophic lateral sclerosis in a family with hexanucleotide repeat expansions in C9orf72. JAMA Neurol. 71, 771–774 (2014).
Cooper-Knock, J. et al. C9ORF72 expansions, parkinsonism, and Parkinson disease: a clinicopathologic study. Neurology 81, 808–811 (2013).
Lindquist, S. G. et al. Corticobasal and ataxia syndromes widen the spectrum of C9ORF72 hexanucleotide expansion disease. Clin. Genet. 83, 279–283 (2013).
Snowden, J. S. et al. Distinct clinical and pathological characteristics of frontotemporal dementia associated with C9ORF72 mutations. Brain 135, 693–708 (2012).
Daoud, H. et al. Investigation of C9orf72 repeat expansions in Parkinson's disease. Neurobiol. Aging 34, 1710.e7–1710.e9 (2013).
Harms, M. B. et al. Parkinson disease is not associated with C9ORF72 repeat expansions. Neurobiol. Aging 34, 1519.e1–1519.e2 (2013).
Xi, Z. et al. Investigation of c9orf72 in 4 neurodegenerative disorders. Arch. Neurol. 69, 1583–1590 (2012).
Lesage, S. et al. C9orf72 repeat expansions are a rare genetic cause of parkinsonism. Brain 136, 385–391 (2013).
Majounie, E. et al. Frequency of the C9orf72 hexanucleotide repeat expansion in patients with amyotrophic lateral sclerosis and frontotemporal dementia: a cross-sectional study. Lancet Neurol. 11, 323–330 (2012).
Nuytemans, K. et al. C9ORF72 intermediate repeat copies are a significant risk factor for Parkinson disease. Ann. Hum. Genet. 77, 351–363 (2013).
Akimoto, C. et al. No GGGGCC-hexanucleotide repeat expansion in C9ORF72 in parkinsonism patients in Sweden. Amyotroph. Lateral Scler. Frontotemporal Degener. 14, 26–29 (2013).
Cooper-Knock, J., Shaw, P. J. & Kirby, J. The widening spectrum of C9ORF72-related disease; genotype/phenotype correlations and potential modifiers of clinical phenotype. Acta Neuropathol. 127, 333–345 (2014).
Dombroski, B. A. et al. C9orf72 hexanucleotide repeat expansion and Guam amyotrophic lateral sclerosis-parkinsonism-dementia complex. JAMA Neurol. 70, 742–745 (2013).
Floris, G. et al. Frontotemporal dementia with psychosis, parkinsonism, visuo-spatial dysfunction, upper motor neuron involvement associated to expansion of C9ORF72: a peculiar phenotype? J. Neurol. 259, 1749–1751 (2012).
Snowden, J. S. et al. Psychosis, C9ORF72 and dementia with Lewy bodies. J. Neurol. Neurosurg. Psychiatry 83, 1031–1032 (2012).
Robinson, A., Davidson, Y., Snowden, J. S. & Mann, D. M. C9ORF72 in dementia with Lewy bodies. J. Neurol. Neurosurg. Psychiatry 85, 1435–1436 (2014).
Morgan, S. et al. Differentiation of frontotemporal dementia from dementia with Lewy bodies using FP-CIT SPECT. J. Neurol. Neurosurg. Psychiatry 83, 1063–1070 (2012).
Johnson, J. O. et al. Exome sequencing reveals VCP mutations as a cause of familial ALS. Neuron 68, 857–864 (2010).
Spina, S. et al. Phenotypic variability in three families with valosin-containing protein mutation. Eur. J. Neurol. 20, 251–258 (2013).
Majounie, E. et al. Mutational analysis of the VCP gene in Parkinson's disease. Neurobiol. Aging 33, 209.e1–209.e2 (2012).
Gydesen, S. et al. Chromosome 3 linked frontotemporal dementia (FTD-3). Neurology 59, 1585–1594 (2002).
Deng, H., Gao, K. & Jankovic, J. The role of FUS gene variants in neurodegenerative diseases. Nat. Rev. Neurol. 10, 337–348 (2014).
Isaacs, A. M., Johannsen, P., Holm, I. & Nielsen, J. E. & FReJA consortium. Frontotemporal dementia caused by CHMP2B mutations. Curr. Alzheimer Res. 8, 246–251 (2011).
Yan, J. et al. Frameshift and novel mutations in FUS in familial amyotrophic lateral sclerosis and ALS/dementia. Neurology 75, 807–814 (2010).
Seelaar, H. et al. Frequency of ubiquitin and FUS-positive, TDP-43-negative frontotemporal lobar degeneration. J. Neurol. 257, 747–753 (2010).
Josephs, K. A. et al. Caudate atrophy on MRI is a characteristic feature of FTLD-FUS. Eur. J. Neurol. 17, 969–975 (2010).
Mosca, L. et al. Wide phenotypic spectrum of the TARDBP gene: homozygosity of A382T mutation in a patient presenting with amyotrophic lateral sclerosis, Parkinson's disease, and frontotemporal lobar degeneration, and in neurologically healthy subject. Neurobiol. Aging 33, 1846.e1–1846.e4 (2012).
Quadri, M. et al. Broadening the phenotype of TARDBP mutations: the TARDBP Ala382Thr mutation and Parkinson's disease in Sardinia. Neurogenetics 12, 203–209 (2011).
Rayaprolu, S. et al. TARDBP mutations in Parkinson's disease. Parkinsonism Relat. Disord. 19, 312–315 (2013).
Fujita, Y., Ikeda, M., Yanagisawa, T., Senoo, Y. & Okamoto, K. Different clinical and neuropathologic phenotypes of familial ALS with A315E TARDBP mutation. Neurology 77, 1427–1431 (2011).
Borghero, G. et al. A patient carrying a homozygous p.A382T TARDBP missense mutation shows a syndrome including ALS, extrapyramidal symptoms, and FTD. Neurobiol. Aging 32, 2327.e1–2327.e5 (2011).
Espay, A. J. et al. Rapidly progressive atypical parkinsonism associated with frontotemporal lobar degeneration and motor neuron disease. J. Neurol. Neurosurg. Psychiatry 82, 751–753 (2011).
Kabashi, E. et al. No TARDBP mutations in a French Canadian population of patients with Parkinson disease. Arch. Neurol. 66, 281–282 (2009).
Ticozzi, N. et al. Mutational analysis of TARDBP in neurodegenerative diseases. Neurobiol. Aging 32, 2096–2099 (2011).
Takahashi, K., Rochford, C. D. & Neumann, H. Clearance of apoptotic neurons without inflammation by microglial triggering receptor expressed on myeloid cells-2. J. Exp. Med. 201, 647–657 (2005).
Bianchin, M. M. et al. Nasu–Hakola disease (polycystic lipomembranous osteodysplasia with sclerosing leukoencephalopathy — PLOSL): a dementia associated with bone cystic lesions. From clinical to genetic and molecular aspects. Cell. Mol. Neurobiol. 24, 1–24 (2004).
Giraldo, M. et al. Variants in triggering receptor expressed on myeloid cells 2 are associated with both behavioral variant frontotemporal lobar degeneration and Alzheimer's disease. Neurobiol. Aging 34, 2077.e11–2077.e18 (2013).
Guerreiro, R. et al. TREM2 variants in Alzheimer's disease. N. Engl. J. Med. 368, 117–127 (2013).
Le Ber, I. et al. Homozygous TREM2 mutation in a family with atypical frontotemporal dementia. Neurobiol. Aging 35, 2419.e23–2419.e25 (2014).
Guerreiro, R. J. et al. Using exome sequencing to reveal mutations in TREM2 presenting as a frontotemporal dementia-like syndrome without bone involvement. JAMA Neurol. 70, 78–84 (2013).
Rayaprolu, S. et al. TREM2 in neurodegeneration: evidence for association of the p.R47H variant with frontotemporal dementia and Parkinson's disease. Mol. Neurodegener. 8, 19 (2013).
Cairns, N. J. et al. α-internexin is present in the pathological inclusions of neuronal intermediate filament inclusion disease. Am. J. Pathol. 164, 2153–2161 (2004).
Cairns, N. J. et al. Clinical and neuropathologic variation in neuronal intermediate filament inclusion disease. Neurology 63, 1376–1384 (2004).
Molina-Porcel, L. et al. Clinical and pathological heterogeneity of neuronal intermediate filament inclusion disease. Arch. Neurol. 65, 272–275 (2008).
Wong, T. H. et al. PRKAR1B mutation associated with a new neurodegenerative disorder with unique pathology. Brain 137, 1361–1373 (2014).
Mendez, M. F. & Shapira, J. S. The spectrum of recurrent thoughts and behaviors in frontotemporal dementia. CNS Spectr. 13, 202–208 (2008).
Shigenobu, K. et al. The Stereotypy Rating Inventory for frontotemporal lobar degeneration. Psychiatry Res. 110, 175–187 (2002).
Mateen, F. J. & Josephs, K. A. The clinical spectrum of stereotypies in frontotemporal lobar degeneration. Mov. Disord. 24, 1237–1240 (2009).
Jankovic, J. in Principles and Practice of Movement Disorders 2nd edn Ch. 17 (eds Fahn, S., Jankovic, J. & Hallett, M.) 380–388 (Churchill Linvingstone, 2011).
Edwards, M. J., Lang, A. E. & Bhatia, K. P. Stereotypies: a critical appraisal and suggestion of a clinically useful definition. Mov. Disord. 27, 179–185 (2012).
Ames, D., Cummings, J. L., Wirshing, W. C., Quinn, B. & Mahler, M. Repetitive and compulsive behavior in frontal lobe degenerations. J. Neuropsychiatry Clin. Neurosci. 6, 100–113 (1994).
Prioni, S. et al. Stereotypic behaviors in degenerative dementias. J. Neurol. 259, 2452–2459 (2012).
Miller, B. L. et al. A study of the Lund–Manchester research criteria for frontotemporal dementia: clinical and single-photon emission CT correlations. Neurology 48, 937–942 (1997).
Bozeat, S., Gregory, C. A., Ralph, M. A. & Hodges, J. R. Which neuropsychiatric and behavioural features distinguish frontal and temporal variants of frontotemporal dementia from Alzheimer's disease? J. Neurol. Neurosurg. Psychiatry 69, 178–186 (2000).
Nyatsanza, S. et al. A study of stereotypic behaviours in Alzheimer's disease and frontal and temporal variant frontotemporal dementia. J. Neurol. Neurosurg. Psychiatry 74, 1398–1402 (2003).
Snowden, J. S. et al. Distinct behavioural profiles in frontotemporal dementia and semantic dementia. J. Neurol. Neurosurg. Psychiatry 70, 323–332 (2001).
Ikeda, M. et al. Efficacy of fluvoxamine as a treatment for behavioral symptoms in frontotemporal lobar degeneration patients. Dement. Geriatr. Cogn. Disord. 17, 117–121 (2004).
Ondo, W. G. Tetrabenazine treatment for stereotypies and tics associated with dementia. J. Neuropsychiatry Clin. Neurosci. 24, 208–214 (2012).
Jankovic, J. & Clarence-Smith, K. Tetrabenazine for the treatment of chorea and other hyperkinetic movement disorders. Expert Rev. Neurother. 11, 1509–1523 (2011).
Nielsen, T. R., Bruhn, P., Nielsen, J. E. & Hjermind, L. E. Behavioral variant of frontotemporal dementia mimicking Huntington's disease. Int. Psychogeriatr. 22, 674–677 (2010).
Kovacs, G. G. et al. TARDBP variation associated with frontotemporal dementia, supranuclear gaze palsy, and chorea. Mov. Disord. 24, 1843–1847 (2009).
Wider, C. et al. Progranulin gene mutation with an unusual clinical and neuropathologic presentation. Mov. Disord. 23, 1168–1173 (2008).
Hensman Moss, D. J. et al. C9orf72 expansions are the most common genetic cause of Huntington disease phenocopies. Neurology 82, 292–299 (2014).
Dejesus-Hernandez, M. et al. Analysis of the C9orf72 repeat in Parkinson's disease, essential tremor and restless legs syndrome. Parkinsonism Relat. Disord. 19, 198–201 (2013).
Caviness, J. N. Myoclonus and neurodegenerative disease — what's in a name? Parkinsonism Relat. Disord. 9, 185–192 (2003).
Curcio, S. A. et al. A large Calabrian kindred segregating frontotemporal dementia. J. Neurol. 249, 911–922 (2002).
Bruni, A. C. et al. Heterogeneity within a large kindred with frontotemporal dementia: a novel progranulin mutation. Neurology 69, 140–147 (2007).
Pail, M., Matej, R., Husarova, I. & Rektorova, I. Generalized myoclonus as a prominent symptom in a patient with FTLD-TDP. J. Neurol. 260, 1681–1683 (2013).
Vanek, Z. & Jankovic, J. Dystonia in corticobasal degeneration. Mov. Disord. 16, 252–257 (2001).
Stamelou, M., Alonso-Canovas, A. & Bhatia, K. P. Dystonia in corticobasal degeneration: a review of the literature on 404 pathologically proven cases. Mov. Disord. 27, 696–702 (2012).
Merner, N. D. et al. Exome sequencing identifies FUS mutations as a cause of essential tremor. Am. J. Hum. Genet. 91, 313–319 (2012).
Deng, H., Liang, H. & Jankovic, J. F-box only protein 7 gene in parkinsonian-pyramidal disease. JAMA Neurol. 70, 20–24 (2013).
Hopfner, F. et al. The impact of rare variants in FUS in essential tremor. Mov. Disord. 30, 721–724 (2015).
Ishii, K. et al. Cerebral glucose metabolism in patients with frontotemporal dementia. J. Nucl. Med. 39, 1875–1878 (1998).
Jeong, Y. et al. 18F-FDG PET findings in frontotemporal dementia: an SPM analysis of 29 patients. J. Nucl. Med. 46, 233–239 (2005).
Diehl-Schmid, J. et al. Decline of cerebral glucose metabolism in frontotemporal dementia: a longitudinal 18F-FDG-PET-study. Neurobiol. Aging 28, 42–50 (2007).
Garibotto, V. et al. Subcortical and deep cortical atrophy in frontotemporal lobar degeneration. Neurobiol. Aging 32, 875–884 (2011).
Looi, J. C. et al. Caudate nucleus volumes in frontotemporal lobar degeneration: differential atrophy in subtypes. AJNR Am. J. Neuroradiol. 29, 1537–1543 (2008).
Looi, J. C. et al. Putaminal volume in frontotemporal lobar degeneration and Alzheimer disease: differential volumes in dementia subtypes and controls. AJNR Am. J. Neuroradiol. 30, 1552–1560 (2009).
Halabi, C. et al. Patterns of striatal degeneration in frontotemporal dementia. Alzheimer Dis. Assoc. Disord. 27, 74–83 (2013).
Rinne, J. O. et al. Striatal dopamine transporter and extrapyramidal symptoms in frontotemporal dementia. Neurology 58, 1489–1493 (2002).
Sedaghat, F. et al. Evaluation of dopaminergic function in frontotemporal dementia using I-FP-CIT single photon emission computed tomography. Neurodegener. Dis. 4, 382–385 (2007).
Carecchio, M. et al. Evidence of pre-synaptic dopaminergic deficit in a patient with a novel progranulin mutation presenting with atypical parkinsonism. J. Alzheimers Dis. 38, 747–752 (2014).
Ittner, L. M. et al. Parkinsonism and impaired axonal transport in a mouse model of frontotemporal dementia. Proc. Natl Acad. Sci. USA 105, 15997–16002 (2008).
Pal, P. K. et al. Positron emission tomography in pallido–ponto–nigral degeneration (PPND) family (frontotemporal dementia with parkinsonism linked to chromosome 17 and point mutation in tau gene). Parkinsonism Relat. Disord. 7, 81–88 (2001).
Selemon, L. D. & Goldman-Rakic, P. S. Longitudinal topography and interdigitation of corticostriatal projections in the rhesus monkey. J. Neurosci. 5, 776–794 (1985).
Kobayashi, K. et al. KP1 expression of ghost Pick bodies, amyloid P-positive astrocytes and selective nigral degeneration in early onset Picks disease. Clin. Neuropathol. 18, 240–249 (1999).
Woolley, J. D. et al. Binge eating is associated with right orbitofrontal-insular-striatal atrophy in frontotemporal dementia. Neurology 69, 1424–1433 (2007).
Josephs, K. A., Whitwell, J. L. & Jack, C. R. Jr. Anatomic correlates of stereotypies in frontotemporal lobar degeneration. Neurobiol. Aging. 29, 1859–1863 (2008).
Diehl-Schmid, J., Onur, O. A., Kuhn, J., Gruppe, T. & Drzezga, A. Imaging frontotemporal lobar degeneration. Curr. Neurol. Neurosci. Rep. 14, 489 (2014).
Gómez-Tortosa, E. et al. Plasma progranulin levels in cortical dementia phenotypes with asymmetric perisylvian atrophy. Eur. J. Neurol. 20, 1319–1324 (2013).
Finch, N. et al. Plasma progranulin levels predict progranulin mutation status in frontotemporal dementia patients and asymptomatic family members. Brain 132, 583–591 (2009).
Le Ber, I. Genetics of frontotemporal lobar degeneration: an up-date and diagnosis algorithm. Rev. Neurol. (Paris) 169, 811–819 (2013).
Rostgaard, N., Waldemar, G., Nielsen, J. E. & Simonsen, A. H. Cerebrospinal fluid biomarkers in familial forms of Alzheimer's disease and frontotemporal dementia. Dement. Geriatr. Cogn. Disord. 40, 54–62 (2015).
Fekete, R. et al. Exome sequencing in familial corticobasal degeneration. Parkinsonism Relat. Disord. 19, 1049–1052 (2013).
Dani, M. Edison, P. & Brooks, D. J. Imaging biomarkers in tauopathies. Parkinsonism Relat. Disord. 22, S26–S28 (2016).
Zhang, J. Mapping neuroinflammation in frontotemporal dementia with molecular PET imaging. J. Neuroinflamm. 12, 108 (2015).
Bang, J., Spina, S. & Miller, B. L. Frontotemporal dementia. Lancet 386, 1672–1682 (2015).
Author information
Authors and Affiliations
Contributions
J.F.B.-C researched data for the article. Both authors made substantial contributions to discussion of the content, wrote the article and reviewed and/or edited the article before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Baizabal-Carvallo, J., Jankovic, J. Parkinsonism, movement disorders and genetics in frontotemporal dementia. Nat Rev Neurol 12, 175–185 (2016). https://doi.org/10.1038/nrneurol.2016.14
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2016.14
This article is cited by
-
Valosin containing protein (VCP): initiator, modifier, and potential drug target for neurodegenerative diseases
Molecular Neurodegeneration (2023)
-
Parkinsonism in complex neurogenetic disorders: lessons from hereditary dementias, adult-onset ataxias and spastic paraplegias
Neurological Sciences (2023)
-
Sirtuin-1 sensitive lysine-136 acetylation drives phase separation and pathological aggregation of TDP-43
Nature Communications (2022)
-
Brainstem atrophy is linked to extrapyramidal symptoms in frontotemporal dementia
Journal of Neurology (2022)
-
New insights into the genetic etiology of Alzheimer’s disease and related dementias
Nature Genetics (2022)