Abstract
Idiopathic intracranial hypertension (IIH) is a rare disorder that typically affects obese women of childbearing age, but can also occur in paediatric populations. Patients usually present with diffuse, daily headache and visual disturbances, but either symptom can occur in isolation. Patients with IIH often have papilloedema; however, IIH without papilloedema is fairly common in patients with chronic daily headache. The pathogenesis of IIH is unknown; the high incidence of comorbid bilateral transverse sinus stenosis (BTSS) in patients with IIH suggests that the two conditions are linked, although no direct causal relationship has been established. Cerebrospinal fluid (CSF) pressure monitoring or lumbar puncture—which provides immediate symptomatic relief—are important in making a diagnosis of IIH. Current treatments for IIH include weight reduction, medical treatment, CSF diversion surgery, optic nerve sheath fenestration and, potentially, endovascular stenting (in patients with BTSS). Prevention of visual loss (which can be substantial) is the main goal of treatment. Residual headache and IIH recurrence are not uncommon after treatment, and regular follow-up is, therefore, warranted even in patients who achieve remission. This Review provides an update of current knowledge of the aetiology, pathophysiology and treatment of IIH.
Key Points
-
Idiopathic intracranial hypertension (IIH) is a rare headache disorder that predominantly affects obese women of childbearing age
-
Diagnosis of IIH requires exclusion of metabolic, endocrine and drug-related aetiologies; magnetic resonance venography is crucial to identify venous thrombosis and bilateral transverse sinus stenosis
-
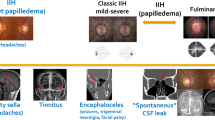
The most common symptoms of IIH are headache, papilloedema and pulsatile tinnitus; however, patients might not present with all three symptoms
-
In patients with suspected IIH, symptomatic relief resulting from a decrease in CSF pressure (achieved by lumbar puncture) confirms the diagnosis
-
Current treatment options for IIH include lumbar puncture, diversion surgery, optic nerve sheath fenestration, and weight reduction (in obese individuals)
-
Visual loss is likely in patients with IIH who are male, of African ancestry, or have systemic hypertension, anaemia or obesity—close follow-up is recommended for these patient populations
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Durcan, F. J., Corbett, J. J. & Wall, M. The incidence of pseudotumor cerebri. Population studies in Iowa and Louisiana. Arch. Neurol. 45, 875–877 (1988).
Gjerris, F., Soelberg Sorensen, P., Vorstrup, S. & Paulson, O. B. Intracranial pressure, conductance to cerebrospinal fluid outflow, and cerebral blood flow in patients with benign intracranial hypertension (pseudotumor cerebri). Ann. Neurol. 17, 158–162 (1985).
Soelberg Sorensen, P., Gjerris, F. & Svenstrup, B. Endocrine studies in patients with pseudotumor cerebri. Estrogen levels in blood and cerebrospinal fluid. Arch. Neurol. 43, 902–906 (1986).
King, J. O., Mitchell, P. J., Thomson, K. R. & Tress, B. M. Cerebral venography and manometry in idiopathic intracranial hypertension. Neurology 45, 2224–2228 (1995).
Karahalios, D. G., Rekate, H. L., Khayata, M. H. & Apostolides, P. J. Elevated intracranial venous pressure as a universal mechanism in pseudotumor cerebri of varying etiologies. Neurology 46, 198–202 (1996).
Bono, F. et al. Bilateral transverse sinus stenosis predicts IIH without papilledema in patients with migraine. Neurology 67, 419–423 (2006).
Bono, F. et al. Bilateral transverse sinus stenosis and idiopathic intracranial hypertension without papilledema in chronic tension-type headache. J. Neurol. 255, 807–812 (2008).
Radhakrishnan, K., Thacker, A. K., Bohlaga, N. H., Maloo, J. C. & Gerryo, S. E. Epidemiology of idiopathic intracranial hypertension: a prospective and case–control study. J. Neurol. Sci. 116, 18–28 (1993).
Digre, K. B. et al. A comparison of idiopathic intracranial hypertension with and without papilledema. Headache 49, 185–193 (2009).
Rowe, F. J. Assessment of visual function in idiopathic intracranial hypertension. Br. J. Neurosurg. 25, 45–54 (2011).
Dandy, W. Intracranial pressure without brain tumor: diagnosis and treatment. Ann. Surg. 106, 492–513 (1937).
Smith, J. L. Whence pseudotumor cerebri? J. Clin. Neuroophthalmol. 5, 55–56 (1985).
The International Classification of Headache Disorders: 2nd edition. Cephalalgia 24 (Suppl. 1), 9–160 (2004).
Yabe, I., Moriwaka, F., Notoya, A., Ohtaki, M. & Tashiro, K. Incidence of idiopathic intracranial hypertension in Hokkaido, the northernmost island of Japan. J. Neurol. 247, 474–475 (2000).
Friesner, D., Rosenman, R., Lobb, B. M. & Tanne, E. Idiopathic intracranial hypertension in the USA: the role of obesity in establishing prevalence and healthcare costs. Obes. Rev. 12, e372–e380 (2011).
Raoof, N., Sharrack, B., Pepper, I. M. & Hickman, S. J. The incidence and prevalence of idiopathic intracranial hypertension in Sheffield, UK. Eur. J. Neurol. 18, 1266–1268 (2011).
Galvin, J. A. & Van Stavern, G. P. Clinical characterization of idiopathic intracranial hypertension at the Detroit Medical Center. J. Neurol. Sci. 223, 157–160 (2004).
Mezaal, M. & Saadah, M. Idiopathic intracranial hypertension in Dubai: nature and prognosis. Acta Neurol. Scand. 112, 298–302 (2005).
Radhakrishnan, K., Ahlskog, J. E., Cross, S. A., Kurland, L. T. & O'Fallon, W. M. Idiopathic intracranial hypertension (pseudotumor cerebri). Descriptive epidemiology in Rochester, Minn, 1976 to 1990. Arch. Neurol. 50, 78–80 (1993).
Kim, T. W., Choung, H. K., Khwarg, S. I., Hwang, J.-M. & Yang, H. J. Obesity may not be a risk factor for idiopathic intracranial hypertension in Asians. Eur. J. Neurol. 15, 876–879 (2008).
Liu, I.-H., Wang, A.-G. & Yen, M.-Y. Idiopathic intracranial hypertension: clinical features in Chinese patients. Jpn J. Ophthalmol. 55, 138–142 (2011).
Bruce, B. B., Preechawat, P., Newman, N. J., Lynn, M. J. & Biousse, V. Racial differences in idiopathic intracranial hypertension. Neurology 70, 861–867 (2008).
Glueck, C. J. et al. Idiopathic intracranial hypertension, polycystic-ovary syndrome, and thrombophilia. J. Lab. Clin. Med. 145, 72–82 (2005).
Kesler, A., Hadayer, A., Goldhammer, Y., Almog, Y. & Korczyn, A. D. Idiopathic intracranial hypertension: risk of recurrences. Neurology 63, 1737–1739 (2004).
Szewka, A. J., Bruce, B. B., Newman, N. J. & Biousse, V. Idiopathic intracranial hypertension: relation between obesity and visual outcomes. J. Neuroophthalmol. http://dx.doi.org/10.1097/WNO.0b013e31823f852d.
Bruce, B. B. et al. Atypical idiopathic intracranial hypertension: normal BMI and older patients. Neurology 74, 1827–1832 (2010).
Bruce, B. B. et al. Idiopathic intracranial hypertension in men. Neurology 72, 304–309 (2009).
Lee, A. G. et al. Sleep apnea and intracranial hypertension in men. Ophthalmology 109, 482–485 (2002).
Hung., H. L., Kao, L. Y. & Huang, C. C. Ophthalmic features of idiopathic intracranial hypertension. Eye (Lond.) 17, 793–795 (2003).
WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 363, 157–163 (2004).
Zheng, W. et al. Association between body-mass index and risk of death in more than 1 million Asians. N. Engl. J. Med. 364, 719–729 (2011).
Babikian, P., Corbett, J. & Bell, W. Idiopathic intracranial hypertension in children: the Iowa experience. J. Child. Neurol. 9, 144–149 (1994).
Kesler, A. & Fattal-Valevski, A. Idiopathic intracranial hypertension in the pediatric population. J. Child. Neurol. 17, 745–748 (2002).
Ng, Y. T. & Bodensteiner, J. B. Idiopathic intracranial hypertension in the pediatric population. J. Child. Neurol. 18, 440 (2003).
Cinciripini, G. S., Donahue, S. & Borchert, M. S. Idiopathic intracranial hypertension in prepubertal pediatric patients: characteristics, treatment, and outcome. Am. J. Ophthalmol. 127, 178–182 (1999).
Weisberg, L. A. & Chutorian, A. M. Pseudotumor cerebri of childhood. Am. J. Dis. Child. 131, 1243–1248 (1977).
Balcer, L. J. et al. Idiopathic intracranial hypertension: relation of age and obesity in children. Neurology 52, 870–872 (1999).
Brara, S. M., Koebnick, C., Porter, A. H. & Langer-Gould, A. Pediatric idiopathic intracranial hypertension and extreme childhood obesity. J. Pediatr. 161, 602–607 (2012).
Faz, G., Butler, I. J. & Koenig, M. K. Incidence of papilledema and obesity in children diagnosed with idiopathic “benign” intracranial hypertension: case series and review. J. Child. Neurol. 25, 1389–1392 (2010).
Wall, M. & George, D. Idiopathic intracranial hypertension. A prospective study of 50 patients. Brain 114, 155–180 (1991).
Marcelis, J. & Silberstein, S. D. Idiopathic intracranial hypertension without papilledema. Arch. Neurol. 48, 392–399 (1991).
Lim, M., Kurian, M., Penn, A., Calver, D. & Lin, J. P. Visual failure without headache in idiopathic intracranial hypertension. Arch. Dis. Child. 90, 206–210 (2005).
Corbett, J. J. et al. Visual loss in pseudotumor cerebri. Follow-up of 57 patients from five to 41 years and a profile of 14 patients with permanent severe visual loss. Arch. Neurol. 39, 461–474 (1982).
Hayreh, S. S. Optic disc edema in raised intracranial pressure. VI. Associated visual disturbances and their pathogenesis. Arch. Ophthalmol. 95, 1566–1579 (1977).
Rowe, F. J. & Sarkies, N. J. Assessment of visual function in idiopathic intracranial hypertension: a prospective study. Eye (Lond.) 12, 111–118 (1998).
Rowe, F. J. & Sarkies, N. J. Visual outcome in a prospective study of idiopathic intracranial hypertension. Arch. Ophthalmol. 117, 1571 (1999).
Bruce, B. B., Newman, N. J. & Biousse, V. Ophthalmoparesis in idiopathic intracranial hypertension. Am. J. Ophthalmol. 142, 878–880 (2006).
Lipton, H. L. & Michelson, P. E. Pseudotumor cerebri syndrome without papilledema. JAMA 220, 1591–1592 (1972).
Wang, S. J., Silberstein, S. D., Patterson, S. & Young, W. B. Idiopathic intracranial hypertension without papilledema: a case-control study in a headache center. Neurology 51, 245–249 (1998).
Torbey, M. T., Geocadin, R. G., Razumovsky, A. Y., Rigamonti, D. & Williams, M. A. Utility of CSF pressure monitoring to identify idiopathic intracranial hypertension without papilledema in patients with chronic daily headache. Cephalalgia 24, 495–502 (2004).
Donnet, A. et al. Endovascular treatment of idiopathic intracranial hypertension: clinical and radiologic outcome of 10 consecutive patients. Neurology 70, 641–647 (2008).
Ahmed, R. M. et al. Transverse sinus stenting for idiopathic intracranial hypertension: a review of 52 Patients and of model predictions. AJNR Am. J. Neuroradiol. (2011).
Friedman, D. I. & Jacobson, D. M. Diagnostic criteria for idiopathic intracranial hypertension. Neurology 59, 1492–1495 (2002).
Silver, R. I., Moonis, G., Schlosser, R. J., Bolger, W. E. & Loevner, L. A. Radiographic signs of elevated intracranial pressure in idiopathic cerebrospinal fluid leaks: a possible presentation of idiopathic intracranial hypertension. Am. J. Rhinol. 21, 257–261 (2007).
Bradley, W. G., Daroff, R. B., Fenichel, G. M. & Jankovic J. (Eds). Neurology in Clinical Practice 5th edn (Butterworth-Heinemann, Oxford, 2007).
Gilland, O., Tourtellotte, W. W., O'Tauma, L. & Henderson, W. G. Normal cerebrospinal fluid pressure. J. Neurosurg. 40, 587–593 (1974).
Whiteley, W., Al-Shahi, R., Warlow, C. P., Zeidler, M. & Lueck, C. J. CSF opening pressure: reference interval and the effect of body mass index. Neurology 67, 1690–1691 (2006).
Avery, R. A. et al. Reference range for cerebrospinal fluid opening pressure in children. N. Engl. J. Med. 363, 891–893 (2010).
Bono, F. et al. Obesity does not induce abnormal CSF pressure in subjects with normal cerebral MR venography. Neurology 59, 1641–1643 (2002).
Bono, F. et al. Abnormal pressure waves in headache sufferers with bilateral transverse sinus stenosis. Cephalalgia 30, 1419–1425 (2010).
Czosnyka, M. & Pickard, J. D. Monitoring and interpretation of intracranial pressure. J. Neurol. Neurosurg. Psychiatry 75, 813–821 (2004).
Agid, R., Farb, R. I., Willinsky, R. A., Mikulis, D. J. & Tomlinson, G. Idiopathic intracranial hypertension: the validity of cross-sectional neuroimaging signs. Neuroradiology 48, 521–527 (2006).
Brodsky, M. C. & Vaphiades, M. Magnetic resonance imaging in pseudotumor cerebri. Ophthalmology 105, 1686–1693 (1998).
Connolly, M. B., Farrell, K., Hill, A. & Flodmark, O. Magnetic resonance imaging in pseudotumor cerebri. Dev. Med. Child. Neurol. 34, 1091–1094 (1992).
Gass, A. et al. MRI of the optic nerve in benign intracranial hypertension. Neuroradiology 38, 769–773 (1996).
Jinkins, J. R. et al. MR of optic papilla protrusion in patients with high intracranial pressure. AJNR Am. J. Neuroradiol. 17, 665–668 (1996).
Manfre, L. et al. Idiopathic intracranial hypertension: orbital MRI. Neuroradiology 37, 459–461 (1995).
Silbergleit, R., Junck, L., Gebarski, S. S. & Hatfield, M. K. Idiopathic intracranial hypertension (pseudotumor cerebri): MR imaging. Radiology 170, 207–209 (1989).
Yuh, W. T. et al. MR imaging of pituitary morphology in idiopathic intracranial hypertension. J. Magn. Reson. Imaging 12, 808–813 (2000).
Maralani, P. J. et al. Accuracy of brain imaging in the diagnosis of idiopathic intracranial hypertension. Clin. Radiol. 67, 656–663 (2012).
Geeraerts, T. et al. Use of T2-weighted magnetic resonance imaging of the optic nerve sheath to detect raised intracranial pressure. Crit. Care 12, R114 (2008).
Leach, J. L., Fortuna, R. B., Jones, B. V. & Gaskill-Shipley, M. F. Imaging of cerebral venous thrombosis: current techniques, spectrum of findings, and diagnostic pitfalls. Radiographics 26 (Suppl. 1), S19–S41 (2006).
Farb, R. I. et al. Idiopathic intracranial hypertension: the prevalence and morphology of sinovenous stenosis. Neurology 60, 1418–1424 (2003).
Zada, G., Tirosh, A., Kaiser, U. B., Laws, E. R. & Woodmansee, W. W. Cushing's disease and idiopathic intracranial hypertension: case report and review of underlying pathophysiological mechanisms. J. Clin. Endocrinol. Metab. 95, 4850–4854 (2010).
Mowl, A. D., Grogg, J. A. & Klein, J. Secondary pseudotumour cerebri in a patient undergoing sexual reassignment therapy. Clin. Exp. Optom. 92, 449–453 (2009).
Fraser, J. A. et al. Risk factors for idiopathic intracranial hypertension in men: a case–control study. J. Neurol. Sci. 290, 86–89 (2010).
Condulis, N., Germain, G., Charest, N., Levy, S. & Carpenter, T. O. Pseudotumor cerebri: a presenting manifestation of Addison's disease. Clin. Pediatr. (Phila.) 36, 711–713 (1997).
Walker, A. E. & Adamkiewicz, J. J. Pseudotumor cerebri associated with prolonged corticosteroid therapy. Reports of four cases. JAMA 188, 779–784 (1964).
Martin, N. A., Linfoot, J. & Wilson, C. B. Development of pseudotumor cerebri after the removal of an adrenocorticotropic hormone-secreting pituitary adenoma: case report. Neurosurgery 8, 699–702 (1981).
Amaral, J. F., Tsiaris, W., Morgan, T. & Thompson, W. R. Reversal of benign intracranial hypertension by surgically induced weight loss. Arch. Surg. 122, 946–949 (1987).
Sinclair, A. J. et al. Exploring the pathogenesis of IIH: an inflammatory perspective. J. Neuroimmunol. 201–202, 212–220 (2008).
Sinclair, A. J. et al. Cerebrospinal fluid corticosteroid levels and cortisol metabolism in patients with idiopathic intracranial hypertension: a link between 11β-HSD1 and intracranial pressure regulation? J. Clin. Endocrinol. Metab. 95, 5348–5356 (2010).
Giuseffi, V., Wall, M., Siegel, P. Z. & Rojas, P. B. Symptoms and disease associations in idiopathic intracranial hypertension (pseudotumor cerebri): a case–control study. Neurology 41, 239–244 (1991).
Sheldon, R. S., Becker, W. J., Hanley, D. A. & Culver, R. L. Hypoparathyroidism and pseudotumor cerebri: an infrequent clinical association. Can. J. Neurol. Sci. 14, 622–625 (1987).
Chiu, A. M. et al. Minocycline treatment and pseudotumor cerebri syndrome. Am. J. Ophthalmol. 126, 116–121 (1998).
Kesler, A., Goldhammer, Y., Hadayer, A. & Pianka, P. The outcome of pseudotumor cerebri induced by tetracycline therapy. Acta Neurol. Scand. 110, 408–411 (2004).
Lochhead, J. & Elston, J. S. Doxycycline induced intracranial hypertension. BMJ 326, 641–642 (2003).
Kasarskis, E. J. & Bass, N. H. Benign intracranial hypertension induced by deficiency of vitamin A during infancy. Neurology 32, 1292–1295 (1982).
Jacobson, D. M. et al. Serum vitamin A concentration is elevated in idiopathic intracranial hypertension. Neurology 53, 1114–1118 (1999).
Fishman, R. A. Polar bear liver, vitamin A, aquaporins, and pseudotumor cerebri. Ann. Neurol. 52, 531–533 (2002).
Lueck, C. & McIlwaine, G. Interventions for idiopathic intracranial hypertension. Cochrane Database of Systematic Reviews, Issue 1. Art. No.: CD003434. http://dx.doi.org/10.1002/14651858.CD003434.pub2.
Newborg, B. Pseudotumor cerebri treated by rice reduction diet. Arch. Intern. Med. 133, 802–807 (1974).
Kupersmith, M. J. et al. Effects of weight loss on the course of idiopathic intracranial hypertension in women. Neurology 50, 1094–1098 (1998).
Johnson, L. N., Krohel, G. B., Madsen, R. W. & March, G. A. Jr. The role of weight loss and acetazolamide in the treatment of idiopathic intracranial hypertension (pseudotumor cerebri). Ophthalmology 105, 2313–2317 (1998).
Sinclair, A. J. et al. Low energy diet and intracranial pressure in women with idiopathic intracranial hypertension: prospective cohort study. BMJ 341, c2701 (2010).
Sugerman, H. J. et al. Gastric surgery for pseudotumor cerebri associated with severe obesity. Ann. Surg. 229, 634–640 (1999).
Nadkarni, T., Rekate, H. L. & Wallace, D. Resolution of pseudotumor cerebri after bariatric surgery for related obesity. Case report. J. Neurosurg. 101, 878–880 (2004).
Carrion, E., Hertzog, J. H., Medlock, M. D., Hauser, G. J. & Dalton, H. J. Use of acetazolamide to decrease cerebrospinal fluid production in chronically ventilated patients with ventriculopleural shunts. Arch. Dis. Child. 84, 68–71 (2001).
Rubin, R. C., Henderson, E. S., Ommaya, A. K., Walker, M. D. & Rall, D. P. The production of cerebrospinal fluid in man and its modification by acetazolamide. J. Neurosurg. 25, 430–436 (1966).
McCarthy, K. D. & Reed, D. J. The effect of acetazolamide and furosemide on cerebrospinal fluid production and choroid plexus carbonic anhydrase activity. J. Pharmacol. Exp. Ther. 189, 194–201 (1974).
Ball, A. K. et al. A randomised controlled trial of treatment for idiopathic intracranial hypertension. J. Neurol. 258, 874–881 (2011).
NORDIC Clinical Trials. Nordicclinicaltrials.com [online]
Liu, G. T., Glaser, J. S. & Schatz, N. J. High-dose methylprednisolone and acetazolamide for visual loss in pseudotumor cerebri. Am. J. Ophthalmol. 118, 88–96 (1994).
Soler, D., Cox, T., Bullock, P., Calver, D. M. & Robinson, R. O. Diagnosis and management of benign intracranial hypertension. Arch. Dis. Child. 78, 89–94 (1998).
Sorensen, P. S., Krogsaa, B. & Gjerris, F. Clinical course and prognosis of pseudotumor cerebri. A prospective study of 24 patients. Acta Neurol. Scand. 77, 164–172 (1988).
Ko, M. W. et al. Weight gain and recurrence in idiopathic intracranial hypertension: a case–control study. Neurology 76, 1564–1567 (2011).
Thambisetty, M., Lavin, P. J., Newman, N. J. & Biousse, V. Fulminant idiopathic intracranial hypertension. Neurology 68, 229–232 (2007).
Celebisoy, N., Gokcay, F., Sirin, H. & Akyurekli, O. Treatment of idiopathic intracranial hypertension: topiramate vs acetazolamide, an open-label study. Acta Neurol. Scand. 116, 322–327 (2007).
Panagopoulos, G. N. et al. Octreotide: a therapeutic option for idiopathic intracranial hypertension. Neurol. Neurophysiol. Neurosci. 10, 1 (2007).
Forderreuther, S. & Straube, A. Indomethacin reduces CSF pressure in intracranial hypertension. Neurology 55, 1043–1045 (2000).
London, E. & Castonguay, T. W. Diet and the role of 11β-hydroxysteroid dehydrogenase-1 on obesity. J. Nutr. Biochem. 20, 485–493 (2009).
Hermanowski-Vosatka, A. et al. 11β-HSD1 inhibition ameliorates metabolic syndrome and prevents progression of atherosclerosis in mice. J. Exp. Med. 202, 517–527 (2005).
Johnston, I. & Paterson, A. Benign intracranial hypertension. II. CSF pressure and circulation. Brain 97, 301–312 (1974).
Bateman, G. A., Stevens, S. A. & Stimpson, J. A mathematical model of idiopathic intracranial hypertension incorporating increased arterial inflow and variable venous outflow collapsibility. J. Neurosurg. 110, 446–456 (2009).
Rosenberg, M. L. et al. Cerebrospinal fluid diversion procedures in pseudotumor cerebri. Neurology 43, 1071–1072 (1993).
Sinclair, A. J. et al. Is cerebrospinal fluid shunting in idiopathic intracranial hypertension worthwhile? A 10-year review. Cephalalgia 31, 1627–1633 (2011).
Abubaker, K. et al. Idiopathic intracranial hypertension: lumboperitoneal shunts versus ventriculoperitoneal shunts—case series and literature review. Br. J. Neurosurg. 25, 94–99 (2011).
McGirt, M. J. et al. Cerebrospinal fluid shunt placement for pseudotumor cerebri-associated intractable headache: predictors of treatment response and an analysis of long-term outcomes. J. Neurosurg. 101, 627–632 (2004).
De Wecker, L. On incision of the optic nerve in cases of neuroretinitis. Int. Ophthalmol. Cong. Reps 4, 11–14 (1872).
Kelman, S. E., Heaps, R., Wolf, A. & Elman, M. J. Optic nerve decompression surgery improves visual function in patients with pseudotumor cerebri. Neurosurgery 30, 391–395 (1992).
Sergott, R. C., Savino, P. J. & Bosley, T. M. Modified optic nerve sheath decompression provides long-term visual improvement for pseudotumor cerebri. Arch. Ophthalmol. 106, 1384–1390 (1988).
Corbett, J. J., Nerad, J. A., Tse, D. T. & Anderson, R. L. Results of optic nerve sheath fenestration for pseudotumor cerebri. The lateral orbitotomy approach. Arch. Ophthalmol. 106, 1391–1397 (1988).
Goh, K. Y., Schatz, N. J. & Glaser, J. S. Optic nerve sheath fenestration for pseudotumor cerebri. J. Neuroophthalmol. 17, 86–91 (1997).
Spoor, T. C. & McHenry, J. G. Long-term effectiveness of optic nerve sheath decompression for pseudotumor cerebri. Arch. Ophthalmol. 111, 632–635 (1993).
Plotnik, J. L. & Kosmorsky, G. S. Operative complications of optic nerve sheath decompression. Ophthalmology 100, 683–690 (1993).
Mauriello, J. A. Jr, Shaderowfsky, P., Gizzi, M. & Frohman, L. Management of visual loss after optic nerve sheath decompression in patients with pseudotumor cerebri. Ophthalmology 102, 441–445 (1995).
Banta, J. T. & Farris, B. K. Pseudotumor cerebri and optic nerve sheath decompression. Ophthalmology 107, 1907–1912 (2000).
Higgins, J. N., Owler, B. K., Cousins, C. & Pickard, J. D. Venous sinus stenting for refractory benign intracranial hypertension. Lancet 359, 228–230 (2002).
Higgins, J. N. P., Cousins, C., Owler, B. K., Sarkies, N. & Pickard, J. D. Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting. J. Neurol. Neurosurg. Psychiatr. 74, 1662–1666 (2003).
Higgins, J. N., Cousins, C., Owler, B. K., Sarkies, N. & Pickard, J. D. Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting. J. Neurol. Neurosurg. Psychiatry 74, 1662–1666 (2003).
Ahmed, R., Friedman, D. I. & Halmagyi, G. M. Stenting of the transverse sinuses in idiopathic intracranial hypertension. J. Neuroophthalmol. 31, 374–380 (2011).
Albuquerque, F. C. et al. Intracranial venous sinus stenting for benign intracranial hypertension: clinical indications, technique, and preliminary results. World Neurosurg. 75, 648–652 (2011).
Bussière, M. et al. Unilateral transverse sinus stenting of patients with idiopathic intracranial hypertension. AJNR Am. J. Neuroradiol. 31, 645–650 (2010).
Fields, J. D. et al. Dural venous sinus angioplasty and stenting for the treatment of idiopathic intracranial hypertension. J. Neurointerv Surg. http://dx.doi.org/10.1136/neurintsurg-2011-010156.
Shah, V. A., Kardon, R. H., Lee, A. G., Corbett, J. J. & Wall, M. Long-term follow-up of idiopathic intracranial hypertension: the Iowa experience. Neurology 70, 634–640 (2008).
Mathew, N. T., Ravishankar, K. & Sanin, L. C. Coexistence of migraine and idiopathic intracranial hypertension without papilledema. Neurology 46, 1226–1230 (1996).
Mathews, M. K., Sergott, R. C. & Savino, P. J. Pseudotumor cerebri. Curr. Opin. Ophthalmol. 14, 364–370 (2003).
Phillips, P. H., Repka, M. X. & Lambert, S. R. Pseudotumor cerebri in children. J. AAPOS 2, 33–38 (1998).
Tibussek, D. et al. Clinical spectrum of the pseudotumor cerebri complex in children. Childs Nerv. Syst. 26, 313–321 (2010).
Soiberman, U. et al. Idiopathic intracranial hypertension in children: visual outcome and risk of recurrence. Childs Nerv. Syst. 27, 1913–1918 (2011).
Boulton, M. et al. Raised intracranial pressure increases CSF drainage through arachnoid villi and extracranial lymphatics. Am. J. Physiol. 275, R889–R896 (1998).
Johnston, M., Armstrong, D. & Koh, L. Possible role of the cavernous sinus veins in cerebrospinal fluid absorption. Cerebrospinal Fluid Res. 4, 3 (2007).
Malm, J., Kristensen, B., Markgren, P. & Ekstedt, J. CSF hydrodynamics in idiopathic intracranial hypertension: a long-term study. Neurology 42, 851–858 (1992).
Janny, P., Chazal, J., Colnet, G., Irthum, B. & Georget, A. M. Benign intracranial hypertension and disorders of CSF absorption. Surg. Neurol. 15, 168–174 (1981).
Alperin, N. et al. Evidence for altered spinal canal compliance and cerebral venous drainage in untreated idiopathic intracranial hypertension. Acta Neurochir. Suppl. 114, 201–205 (2012).
De Simone, R., Ranieri, A. & Bonavita, V. Advancement in idiopathic intracranial hypertension pathogenesis: focus on sinus venous stenosis. Neurol. Sci. 31 (Suppl. 1), S33–S39 (2010).
Higgins, J. N. & Pickard, J. D. Lateral sinus stenoses in idiopathic intracranial hypertension resolving after CSF diversion. Neurology 62, 1907–1908 (2004).
Lee, S. W., Gates, P., Morris, P., Whan, A. & Riddington, L. Idiopathic intracranial hypertension; immediate resolution of venous sinus “obstruction” after reducing cerebrospinal fluid pressure to <10 cmH2O. J. Clin. Neurosci. 16, 1690–1692 (2009).
Pickard, J. D., Czosnyka, Z., Czosnyka, M., Owler, B. & Higgins, J. N. Coupling of sagittal sinus pressure and cerebrospinal fluid pressure in idiopathic intracranial hypertension—a preliminary report. Acta Neurochir. Suppl. 102, 283–285 (2008).
Bono, F. et al. Transverse sinus stenoses persist after normalization of the CSF pressure in IIH. Neurology 65, 1090–1093 (2005).
Alper, F. et al. Importance of anatomical asymmetries of transverse sinuses: an MR venographic study. Cerebrovasc. Dis. 18, 236–239 (2004).
Kelly. L. et al. Does bilateral transverse cerebral venous sinus stenosis (TSS) really exist in patients without increased intracranial pressure (ICP)? Neurology 78 (Suppl. 1), P07.263 (2012).
Riggeal, B. et al. Does the presence of transverse sinus stenosis (TSS) influence the clinical presentation and outcome of idiopathic intracranial hypertension (IIH). Neurology 78 (Suppl. 1), P07.266 (2012).
Acknowledgements
The authors' research work is supported by grants awarded to S.-J. Wang from the Taiwan National Science Council (100-2314-B-010-019-MY2, 100-2314-B-010-018-MY3) and Taipei Veterans General Hospital (VGHUST101-G7-1-1, V101C-106, V101E7-003). The authors also acknowledge National Science Council support for the Center for Dynamic Biomarkers and Translational Medicine, National Central University, Taiwan (NSC 100-2911-I-008-001), Brain Research Center, National Yang-Ming University and a grant from the Ministry of Education, Aim for the Top University Plan.
Author information
Authors and Affiliations
Contributions
K.-P. Peng researched the data for the article. K.-P. Peng, J.-L. Fuh and S.-J. Wang contributed equally to discussions of the content. K.-P. Peng wrote the article, and K.-P. Peng, J.-L. Fuh and S.-J. Wang reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Peng, KP., Fuh, JL. & Wang, SJ. High-pressure headaches: idiopathic intracranial hypertension and its mimics. Nat Rev Neurol 8, 700–710 (2012). https://doi.org/10.1038/nrneurol.2012.223
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2012.223
This article is cited by
-
Safety and efficacy comparison between OACs plus single antiplatelet and dual antiplatelet therapy in patients with cerebral venous sinus stenosis poststenting
BMC Neurology (2022)
-
Different patterns of white matter lesions among patent foramen ovale, atherosclerotic cerebral small vessel disease and cerebral venous thrombosis
Journal of Thrombosis and Thrombolysis (2022)
-
The comparative analysis of non-thrombotic internal jugular vein stenosis and cerebral venous sinus stenosis
Journal of Thrombosis and Thrombolysis (2019)
-
Inflammatory gene expression signatures in idiopathic intracranial hypertension: possible implications in microgravity-induced ICP elevation
npj Microgravity (2018)
-
Optical coherence tomography for the diagnosis and monitoring of idiopathic intracranial hypertension
Journal of Neurology (2017)