Key Points
-
Most current knowledge of ex vivo cell and gene therapies has been obtained with haematopoietic cells, either lymphocytes or stem and progenitor cells. As the field moves rapidly towards developing applications for other somatic stem and progenitor cell types, such as keratinocyte, limbal, neural, cardiac and mesenchymal progenitors, the lessons learned from haematopoietic cell gene therapy will instruct these emerging studies.
-
Several studies have demonstrated the therapeutic potential of adoptive immunotherapy based on ex vivo expanded T cells, with or without genetic engineering, to harness the power of immune effector and regulatory cells against malignancies, infections and autoimmune diseases. Although the efficacy of these approaches still needs to be improved, they have generally shown an excellent safety record.
-
The first comprehensive analysis of two seminal clinical studies of haematopoietic stem cell (HSC) gene therapy for severe combined immune deficiencies (SCIDs) shows effective long-term immune system reconstitution with gene-corrected cells. Most treated patients are alive with a clear therapeutic benefit in these otherwise fatal diseases.
-
However, the occurrence of vector-related leukaemia in a fraction of treated patients calls for developing and testing improved vectors to achieve better safety. The incidence of adverse events also seems to be influenced by the underlying disease condition and transgene function.
-
Initial results of the first HSC gene therapy trials using late-generation lentiviral vectors for the treatment of adrenoleukodystrophy and β-thalassaemia show clear therapeutic benefits and support predictions from preclinical studies that lentiviral vectors provide a more efficient and safer gene shuttle into HSCs than do earlier vector types.
-
HSC gene therapy may compare favourably to allogenic HCT and, in selected conditions, become a first-line treatment. It can be applied to every patient without the limitations that can arise owing to the lack of compatible donor, and it reduces the morbidity of the transplant procedure.
-
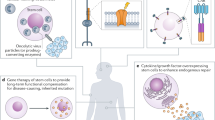
In some applications, haematopoietic gene therapy may enable new mechanisms of therapy, such as when cells are engineered to increase the therapeutic gene dosage, target a therapeutic protein to a disease site or become resistant to a pathogen.
-
The main disadvantages of ex vivo gene therapy are the possibility that the ex vivo culture required for gene transfer may decrease the reconstitution potential of the infused cells, as well as the risk of malignancy triggered by vector insertion.
-
The recent development of powerful new technologies for highly efficient gene targeting and site-specific gene editing brings the possibility of somatic gene disruption, gene correction rather than gene replacement, and targeted rather than random integration within the reach of gene therapy. Although several challenges must be addressed to fully exploit the potential of these technologies in gene and cell therapy, they offer us the potential to overcome the main hurdles that have prevented further progress of the field.
-
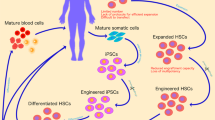
Full exploitation of these new technologies will also require sources of stem cells that can be more conveniently isolated and selected in vitro than is currently experienced with most somatic stem cell types. The fast-growing field of cell reprogramming to pluripotency should help.
Abstract
Cell-based therapies are fast-growing forms of personalized medicine that make use of the steady advances in stem cell manipulation and gene transfer technologies. In this Review, I highlight the latest developments and the crucial challenges for this field, with an emphasis on haematopoietic stem cell gene therapy, which is taken as a representative example given its advanced clinical translation. New technologies for gene correction and targeted integration promise to overcome some of the main hurdles that have long prevented progress in this field. As these approaches marry with our growing capacity for genetic reprogramming of mammalian cells, they may fulfil the promise of safe and effective therapies for currently untreatable diseases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Kay, M. A. State-of-the-art gene-based therapies: the road ahead. Nature Rev. Genet. (in the press).
Mingozzi, F. & High, K. A. Therapeutic in vivo gene transfer for genetic disease using AAV: progress and challenges. Nature Rev. Genet. (in the press).
Copelan, E. A. Hematopoietic stem-cell transplantation. N. Engl. J. Med. 354, 1813–1826 (2006).
Morgan, R. A., Dudley, M. E. & Rosenberg, S. A. Adoptive cell therapy: genetic modification to redirect effector cell specificity. Cancer J. 16, 336–341 (2010).
Brenner, M. K. & Heslop, H. E. Adoptive T cell therapy of cancer. Curr. Opin. Immunol. 22, 251–257 (2010).
Schmitt, T. M., Ragnarsson, G. B. & Greenberg, P. D. T cell receptor gene therapy for cancer. Hum. Gene Ther. 20, 1240–1248 (2009).
June, C. H., Blazar, B. R. & Riley, J. L. Engineering lymphocyte subsets: tools, trials and tribulations. Nature Rev. Immunol. 9, 704–716 (2009).
Pellegrini, G., Rama, P., Mavilio, F. & De Luca, M. Epithelial stem cells in corneal regeneration and epidermal gene therapy. J. Pathol. 217, 217–228 (2009).
Rama, P. et al. Limbal stem-cell therapy and long-term corneal regeneration. N. Engl. J. Med. 363, 147–155 (2010).
Lindvall, O. & Kokaia, Z. Stem cells in human neurodegenerative disorders — time for clinical translation? J. Clin. Invest. 120, 29–40 (2010).
Conti, L. & Cattaneo, E. Neural stem cell systems: physiological players or in vitro entities? Nature Rev. Neurosci. 11, 176–187 (2010).
Chien, K. R., Domian, I. J. & Parker, K. K. Cardiogenesis and the complex biology of regenerative cardiovascular medicine. Science 322, 1494–1497 (2008).
Singer, N. G. & Caplan, A. I. Mesenchymal stem cells: mechanisms of inflammation. Annu. Rev. Pathol. 6, 457–478 (2011).
Bianco, P., Robey, P. G. & Simmons, P. J. Mesenchymal stem cells: revisiting history, concepts, and assays. Cell Stem Cell 2, 313–319 (2008).
Aiuti, A. et al. Gene therapy for immunodeficiency due to adenosine deaminase deficiency. N. Engl. J. Med. 360, 447–458 (2009). A comprehensive account of the long-term outcome of SCID gene therapy in terms of immune system reconstitution, overall benefit and safety from a seminal study of HSC gene therapy using a γ-retroviral vector.
Hacein-Bey-Abina, S. et al. Efficacy of gene therapy for X-linked severe combined immunodeficiency. N. Engl. J. Med. 363, 355–364 (2010). A comprehensive account of the long-term outcome of SCID gene therapy in terms of immune system reconstitution and risk/benefit ratio, also in comparison with HCT, from a seminal study of HSC gene therapy using a γ-retroviral vector.
Fischer, A., Hacein-Bey-Abina, S. & Cavazzana-Calvo, M. 20 years of gene therapy for SCID. Nature Immunol. 11, 457–460 (2010).
Hacein-Bey-Abina, S. et al. Insertional oncogenesis in 4 patients after retrovirus-mediated gene therapy of SCID-X1. J. Clin. Invest. 118, 3132–3142 (2008). A detailed investigation of the mechanism of leukaemogenesis driven by vector insertional mutagenesis in an SCID HSC gene therapy clinical trial. See also the following study.
Howe, S. J. et al. Insertional mutagenesis combined with acquired somatic mutations causes leukemogenesis following gene therapy of SCID-X1 patients. J. Clin. Invest. 118, 3143–3150 (2008).
Boztug, K. et al. Stem-cell gene therapy for the Wiskott-Aldrich syndrome. N. Engl. J. Med. 363, 1918–1927 (2010). The remarkable therapeutic benefit achieved by γ-retroviral HSC gene therapy in this trial is accompanied by an alarming pattern of vector integration sites, with a high frequency of common vector integration sites near oncogenes that are different for the myeloid and lymphoid lineage of reconstituted haematopoiesis.
Ott, M. G. et al. Correction of X-linked chronic granulomatous disease by gene therapy, augmented by insertional activation of MDS1-EVI1, PRDM16 or SETBP1. Nature Med. 12, 401–409 (2006).
Stein, S. et al. Genomic instability and myelodysplasia with monosomy 7 consequent to EVI1 activation after gene therapy for chronic granulomatous disease. Nature Med. 16, 198–204 (2010). References 21 and 22 demonstrate the two facets of insertional mutagenesis. In vivo expansion of multiple myeloid clones carrying vector integration in a common set of oncogenes provides a transient therapeutic benefit, but subsequently progresses to overt myelodysplasia.
Cartier, N. et al. Hematopoietic stem cell gene therapy with a lentiviral vector in X-linked adrenoleukodystrophy. Science 326, 818–823 (2009). The first study of HSC gene therapy by lentiviral vectors, showing clear therapeutic benefit together with evidence of transduction of bona fide HSCs and a highly polyclonal pattern of vector integration sites. The potential for treating a central nervous system disorder by HSC gene therapy is also shown.
Cavazzana-Calvo, M. et al. Transfusion independence and HMGA2 activation after gene therapy of human β-thalassaemia. Nature 467, 318–322 (2010). Another seminal study of HSC gene therapy by lentiviral vectors, with the only treated patient so far showing a therapeutic benefit, albeit in the setting of oligoclonal repopulation. Molecular analysis of the dominant clone suggests a potential contribution of insertional mutagenesis, mediated by a novel mechanism in which vector insertion leads to premature termination of a transcript and removal of regulatory microRNA binding sites.
Ivics, Z. & Izsvak, Z. The expanding universe of transposon technologies for gene and cell engineering. Mob. DNA 1, 25 (2010).
Urnov, F. D., Rebar, E. J., Holmes, M. C., Zhang, H. S. & Gregory, P. D. Genome editing with engineered zinc finger nucleases. Nature Rev. Genet. 11, 636–646 (2010).
Notarangelo, L. D. Primary immunodeficiencies. J. Allergy Clin. Immunol. 125, S182–S194 (2010).
Gennery, A. R. et al. Transplantation of hematopoietic stem cells and long-term survival for primary immunodeficiencies in Europe: entering a new century, do we do better? J. Allergy Clin. Immunol. 126, 602–610 (2010).
Szabolcs, P., Cavazzana-Calvo, M., Fischer, A. & Veys, P. Bone marrow transplantation for primary immunodeficiency diseases. Pediatr. Clin. North Am. 57, 207–237 (2010).
Wynn, R. F. et al. Improved metabolic correction in patients with lysosomal storage disease treated with hematopoietic stem cell transplant compared with enzyme replacement therapy. J. Pediatr. 154, 609–611 (2009).
Biffi, A. et al. Gene therapy of metachromatic leukodystrophy reverses neurological damage and deficits in mice. J. Clin. Invest. 116, 3070–3082 (2006). This study shows the unique benefit that HSC gene therapy can achieve in comparison with HCT through overexpression of the therapeutic protein in the haematopoietic progeny, which leads to its increased bioavailability and widespread cross-correction in the central nervous system.
Visigalli, I. et al. Gene therapy augments the efficacy of hematopoietic cell transplantation and fully corrects mucopolysaccharidosis type I phenotype in the mouse model. Blood 116, 5130–5139 (2010).
Krivit, W., Sung, J. H., Shapiro, E. G. & Lockman, L. A. Microglia: the effector cell for reconstitution of the central nervous system following bone marrow transplantation for lysosomal and peroxisomal storage diseases. Cell Transplant. 4, 385–392 (1995).
Priller, J. et al. Targeting gene-modified hematopoietic cells to the central nervous system: use of green fluorescent protein uncovers microglial engraftment. Nature Med. 7, 1356–1361 (2001).
Biffi, A. et al. Correction of metachromatic leukodystrophy in the mouse model by transplantation of genetically modified hematopoietic stem cells. J. Clin. Invest. 113, 1118–1129 (2004).
Ajami, B., Bennett, J. L., Krieger, C., Tetzlaff, W. & Rossi, F. M. Local self-renewal can sustain CNS microglia maintenance and function throughout adult life. Nature Neurosci. 10, 1538–1543 (2007).
Mildner, A. et al. Microglia in the adult brain arise from Ly-6ChiCCR2+ monocytes only under defined host conditions. Nature Neurosci. 10, 1544–1553 (2007).
Soulas, C. et al. Genetically modified CD34+ hematopoietic stem cells contribute to turnover of brain perivascular macrophages in long-term repopulated primates. Am. J. Pathol. 174, 1808–1817 (2009).
Ginhoux, F. et al. Fate mapping analysis reveals that adult microglia derive from primitive macrophages. Science 330, 841–845 (2010).
Sorrentino, B. P. Gene therapy to protect haematopoietic cells from cytotoxic cancer drugs. Nature Rev. Cancer 2, 431–441 (2002).
Rossi, J. J., June, C. H. & Kohn, D. B. Genetic therapies against HIV. Nature Biotech. 25, 1444–1454 (2007).
Shi, Q. & Montgomery, R. R. Platelets as delivery systems for disease treatments. Adv. Drug Deliv. Rev. 62, 1196–1203 (2010).
De Palma, M. et al. Tumor-targeted interferon-α delivery by Tie2-expressing monocytes inhibits tumor growth and metastasis. Cancer Cell 14, 299–311 (2008).
Ciceri, F. et al. Infusion of suicide-gene-engineered donor lymphocytes after family haploidentical haemopoietic stem-cell transplantation for leukaemia (the TK007 trial): a non-randomised phase I-II study. Lancet Oncol. 10, 489–500 (2009).
Pule, M. A. et al. Virus-specific T cells engineered to coexpress tumor-specific receptors: persistence and antitumor activity in individuals with neuroblastoma. Nature Med. 14, 1264–1270 (2008).
Roncarolo, M. G. & Battaglia, M. Regulatory T-cell immunotherapy for tolerance to self antigens and alloantigens in humans. Nature Rev. Immunol. 7, 585–598 (2007).
Vesely, M. D., Kershaw, M. H., Schreiber, R. D. & Smyth, M. J. Natural innate and adaptive immunity to cancer. Annu. Rev. Immunol. 5 Jan 2011 (doi:10.1146/annurev-immunol-031210-101324).
Boon, T., Coulie, P. G., Van den Eynde, B. J. & van der Bruggen, P. Human T cell responses against melanoma. Annu. Rev. Immunol. 24, 175–208 (2006).
Berger, C. et al. Adoptive transfer of effector CD8+ T cells derived from central memory cells establishes persistent T cell memory in primates. J. Clin. Invest. 118, 294–305 (2008).
Kaneko, S. et al. IL-7 and IL-15 allow the generation of suicide gene-modified alloreactive self-renewing central memory human T lymphocytes. Blood 113, 1006–1015 (2009).
Bendle, G. M. et al. Lethal graft-versus-host disease in mouse models of T cell receptor gene therapy. Nature Med. 16, 565–570 (2010).
van Loenen, M. M. et al. Mixed T cell receptor dimers harbor potentially harmful neoreactivity. Proc. Natl Acad. Sci. USA 107, 10972–10977 (2010).
Okamoto, S. et al. Improved expression and reactivity of transduced tumor-specific TCRs in human lymphocytes by specific silencing of endogenous TCR. Cancer Res. 69, 9003–9011 (2009).
Ha, S. P. et al. Transplantation of mouse HSCs genetically modified to express a CD4-restricted TCR results in long-term immunity that destroys tumors and initiates spontaneous autoimmunity. J. Clin. Invest. 120, 4273–4288 (2010).
Luo, X. M. et al. Engineering human hematopoietic stem/progenitor cells to produce a broadly neutralizing anti-HIV antibody after in vitro maturation to human B lymphocytes. Blood 113, 1422–1431 (2009).
Kitchen, S. G. et al. Engineering antigen-specific T cells from genetically modified human hematopoietic stem cells in immunodeficient mice. PLoS ONE 4, e8208 (2009).
Hansson, E. M., Lindsay, M. E. & Chien, K. R. Regeneration next: toward heart stem cell therapeutics. Cell Stem Cell 5, 364–377 (2009).
Tedesco, F. S., Dellavalle, A., Diaz-Manera, J., Messina, G. & Cossu, G. Repairing skeletal muscle: regenerative potential of skeletal muscle stem cells. J. Clin. Invest. 120, 11–19 (2010).
Prockop, D. J. Repair of tissues by adult stem/progenitor cells (MSCs): controversies, myths, and changing paradigms. Mol. Ther. 17, 939–946 (2009).
Pluchino, S. et al. Neurosphere-derived multipotent precursors promote neuroprotection by an immunomodulatory mechanism. Nature 436, 266–271 (2005).
Lee, J. P. et al. Stem cells act through multiple mechanisms to benefit mice with neurodegenerative metabolic disease. Nature Med. 13, 439–447 (2007).
Tamaki, S. J. et al. Neuroprotection of host cells by human central nervous system stem cells in a mouse model of infantile neuronal ceroid lipofuscinosis. Cell Stem Cell 5, 310–319 (2009).
Jaderstad, J. et al. Communication via gap junctions underlies early functional and beneficial interactions between grafted neural stem cells and the host. Proc. Natl Acad. Sci. USA 107, 5184–5189 (2010).
Le Blanc, K. et al. Mesenchymal stem cells for treatment of steroid-resistant, severe, acute graft-versus-host disease: a phase II study. Lancet 371, 1579–1586 (2008).
Alaiti, M. A., Ishikawa, M. & Costa, M. A. Bone marrow and circulating stem/progenitor cells for regenerative cardiovascular therapy. Transl. Res. 156, 112–129 (2010).
Dorrell, C., Gan, O. I., Pereira, D. S., Hawley, R. G. & Dick, J. E. Expansion of human cord blood CD34+CD38− cells in ex vivo culture during retroviral transduction without a corresponding increase in SCID repopulating cell (SRC) frequency: dissociation of SRC phenotype and function. Blood 95, 102–110 (2000).
Mazurier, F., Gan, O. I., McKenzie, J. L., Doedens, M. & Dick, J. E. Lentivector-mediated clonal tracking reveals intrinsic heterogeneity in the human hematopoietic stem cell compartment and culture-induced stem cell impairment. Blood 103, 545–552 (2004).
Sauce, D. et al. Retrovirus-mediated gene transfer in primary T lymphocytes impairs their anti-Epstein-Barr virus potential through both culture-dependent and selection process-dependent mechanisms. Blood 99, 1165–1173 (2002).
Marktel, S. et al. Immunologic potential of donor lymphocytes expressing a suicide gene for early immune reconstitution after hematopoietic T-cell-depleted stem cell transplantation. Blood 101, 1290–1298 (2003).
Gattinoni, L. et al. Acquisition of full effector function in vitro paradoxically impairs the in vivo antitumor efficacy of adoptively transferred CD8+ T cells. J. Clin. Invest. 115, 1616–1626 (2005).
North, T. E. et al. Prostaglandin E2 regulates vertebrate haematopoietic stem cell homeostasis. Nature 447, 1007–1011 (2007).
Zhang, C. C., Kaba, M., Iizuka, S., Huynh, H. & Lodish, H. F. Angiopoietin-like 5 and IGFBP2 stimulate ex vivo expansion of human cord blood hematopoietic stem cells as assayed by NOD/SCID transplantation. Blood 111, 3415–3423 (2008).
Himburg, H. A. et al. Pleiotrophin regulates the expansion and regeneration of hematopoietic stem cells. Nature Med. 16, 475–482 (2010).
Boitano, A. E. et al. Aryl hydrocarbon receptor antagonists promote the expansion of human hematopoietic stem cells. Science 329, 1345–1348 (2010).
Davidson, B. L. & McCray, P. B. Jr. Current prospects for RNA interference-based therapies. Nature Rev. Genet. (in the press).
Kazuki, Y. et al. Refined human artificial chromosome vectors for gene therapy and animal transgenesis. Gene Ther. 18 Nov 2010 (doi:10.1038/gt.2010.147).
Bushman, F. et al. Genome-wide analysis of retroviral DNA integration. Nature Rev. Microbiol. 3, 848–858 (2005).
Ivics, Z., Hackett, P. B., Plasterk, R. H. & Izsvak, Z. Molecular reconstruction of Sleeping Beauty, a Tc1-like transposon from fish, and its transposition in human cells. Cell 91, 501–510 (1997). The original study reporting the rescue of a transposon and its application to human gene transfer. See also the two following studies.
Izsvak, Z., Chuah, M. K., Vandendriessche, T. & Ivics, Z. Efficient stable gene transfer into human cells by the Sleeping Beauty transposon vectors. Methods 49, 287–297 (2009).
Mates, L. et al. Molecular evolution of a novel hyperactive Sleeping Beauty transposase enables robust stable gene transfer in vertebrates. Nature Genet. 41, 753–761 (2009).
Calos, M. P. The phiC31 integrase system for gene therapy. Curr. Gene Ther. 6, 633–645 (2006).
Su, K., Wang, D., Ye, J., Kim, Y. C. & Chow, S. A. Site-specific integration of retroviral DNA in human cells using fusion proteins consisting of human immunodeficiency virus type 1 integrase and the designed polydactyl zinc-finger protein E2C. Methods 47, 269–276 (2009).
Murray, L. J. et al. Thrombopoietin, flt3, and kit ligands together suppress apoptosis of human mobilized CD34+ cells and recruit primitive CD34+ Thy-1+ cells into rapid division. Exp. Hematol. 27, 1019–1028 (1999).
Naldini, L. et al. In vivo gene delivery and stable transduction of nondividing cells by a lentiviral vector. Science 272, 263–267 (1996). The original study reporting the generation of hybrid lentiviral vectors for integrative gene transfer into non-dividing cells.
Wang, G. P. et al. Analysis of lentiviral vector integration in HIV+ study subjects receiving autologous infusions of gene modified CD4+ T cells. Mol. Ther. 17, 844–850 (2009). A report from the first clinical trial of HIV-based vectors in T cells. Lymphocytes from HIV-infected people were engineered for viral resistance and followed up in vivo by integration site analysis.
Unutmaz, D., KewalRamani, V. N., Marmon, S. & Littman, D. R. Cytokine signals are sufficient for HIV-1 infection of resting human T lymphocytes. J. Exp. Med. 189, 1735–1746 (1999).
Ailles, L. et al. Molecular evidence of lentiviral vector-mediated gene transfer into human self-renewing, multi-potent, long-term NOD/SCID repopulating hematopoietic cells. Mol. Ther. 6, 615–626 (2002).
Zielske, S. P. & Gerson, S. L. Cytokines, including stem cell factor alone, enhance lentiviral transduction in nondividing human LTCIC and NOD/SCID repopulating cells. Mol. Ther. 7, 325–333 (2003).
Cavalieri, S. et al. Human T lymphocytes transduced by lentiviral vectors in the absence of TCR activation maintain an intact immune competence. Blood 102, 497–505 (2003).
Santoni de Sio, F. R., Cascio, P., Zingale, A., Gasparini, M. & Naldini, L. Proteasome activity restricts lentiviral gene transfer into hematopoietic stem cells and is down-regulated by cytokines that enhance transduction. Blood 107, 4257–4265 (2006).
Biasco, L. et al. Integration profile of retroviral vector in gene therapy treated patients is cell-specific according to gene expression and chromatin conformation of target cell. EMBO Mol. Med. 3, 89–101 (2011).
Baum, C. Insertional mutagenesis in gene therapy and stem cell biology. Curr. Opin. Hematol. 14, 337–342 (2007).
Kool, J. & Berns, A. High-throughput insertional mutagenesis screens in mice to identify oncogenic networks. Nature Rev. Cancer 9, 389–399 (2009).
Modlich, U. et al. Leukemias following retroviral transfer of multidrug resistance 1 (MDR1) are driven by combinatorial insertional mutagenesis. Blood 105, 4235–4246 (2005).
Montini, E. et al. Hematopoietic stem cell gene transfer in a tumor-prone mouse model uncovers low genotoxicity of lentiviral vector integration. Nature Biotech. 24, 687–696 (2006).
Modlich, U. et al. Cell-culture assays reveal the importance of retroviral vector design for insertional genotoxicity. Blood 108, 2545–2553 (2006). This study describes the use of an in vitro cell immortalization assay to compare the genotoxic potential of different vector types and designs.
Modlich, U. et al. Leukemia induction after a single retroviral vector insertion in Evi1 or Prdm16. Leukemia 22, 1519–1528 (2008).
Montini, E. et al. The genotoxic potential of retroviral vectors is strongly modulated by vector design and integration site selection in a mouse model of HSC gene therapy. J. Clin. Invest. 119, 964–975 (2009). References 95 and 98 describe the use of HSC from tumour-prone mice to quantitatively study the genotoxic potential of different vector types and designs in a sensitized in vivo transplantation model. The studies validate the use of SIN LTRs and highlight the improved biosafety that is achieved by lentiviral vectors.
Modlich, U. et al. Insertional transformation of hematopoietic cells by self-inactivating lentiviral and gammaretroviral vectors. Mol. Ther. 17, 1919–1928 (2009).
Zychlinski, D. et al. Physiological promoters reduce the genotoxic risk of integrating gene vectors. Mol. Ther. 16, 718–725 (2008). This study demonstrates the safety advantage of using moderate cellular promoters instead of strong viral promoters within SIN vectors by the in vitro immortalization assay described in reference 96.
Wu, X., Li, Y., Crise, B. & Burgess, S. M. Transcription start regions in the human genome are favored targets for MLV integration. Science 300, 1749–1751 (2003). A seminal study describing the genomic integration biases of murine leukaemia virus (MLV).
De Palma, M. et al. Promoter trapping reveals significant differences in integration site selection between MLV and HIV vectors in primary hematopoietic cells. Blood 105, 2307–2315 (2005).
Mitchell, R. S. et al. Retroviral DNA integration: ASLV, HIV, and MLV show distinct target site preferences. PLoS Biol. 2, e234 (2004). One of the first studies to comparatively assess the integration biases of different retroviruses.
Bonini, C. et al. Safety of retroviral gene marking with a truncated NGF receptor. Nature Med. 9, 367–369 (2003).
Recchia, A. et al. Retroviral vector integration deregulates gene expression but has no consequence on the biology and function of transplanted T cells. Proc. Natl Acad. Sci. USA 103, 1457–1462 (2006).
Ellis, J. Silencing and variegation of gammaretrovirus and lentivirus vectors. Hum. Gene Ther. 16, 1241–1246 (2005).
May, C. et al. Therapeutic haemoglobin synthesis in β-thalassaemic mice expressing lentivirus-encoded human β-globin. Nature 406, 82–86 (2000).
Pawliuk, R. et al. Correction of sickle cell disease in transgenic mouse models by gene therapy. Science 294, 2368–2371 (2001). References 107 and 108 demonstrated the value of lentiviral vectors for efficient and stable delivery of complex globin transgene cassettes in the HSC gene therapy of haemoglobinopathies.
Brown, B. D. et al. Endogenous microRNA can be broadly exploited to regulate transgene expression according to tissue, lineage and differentiation state. Nature Biotech. 25, 1457–1467 (2007).
Gentner, B. et al. Identification of hematopoietic stem cell-specific miRNAs enables gene therapy of globoid cell leukodystrophy. Sci. Transl. Med. 2, 58ra84 (2010).
Brown, B. D., Venneri, M. A., Zingale, A., Sergi Sergi, L. & Naldini, L. Endogenous microRNA regulation suppresses transgene expression in hematopoietic lineages and enables stable gene transfer. Nature Med. 12, 585–591 (2006). References 109–111 introduced new approaches to stringently regulate transgene expression in gene transfer by exploiting endogenous microRNA regulation. By making the vector transcript susceptible to microRNA-mediated degradation, one can exploit differential microRNA expression among different tissues or cell types to post-transcriptionally suppress transgene expression in unwanted cell types.
Brown, B. D. & Naldini, L. Exploiting and antagonizing microRNA regulation for therapeutic and experimental applications. Nature Rev. Genet. 10, 578–585 (2009).
Gentner, B. et al. Stable knockdown of microRNA in vivo by lentiviral vectors. Nature Methods 6, 63–66 (2009).
Carroll, D. Progress and prospects: zinc-finger nucleases as gene therapy agents. Gene Ther. 15, 1463–1468 (2008).
Sander, J. D. et al. Selection-free zinc-finger-nuclease engineering by context-dependent assembly (CoDA). Nature Methods 8, 67–69 (2011).
Silva, G. et al. Meganucleases and other tools for targeted genome engineering: perspectives and challenges for gene therapy. Curr. Gene Ther. 11, 11–27 (2011).
Christian, M. et al. Targeting DNA double-strand breaks with TAL effector nucleases. Genetics 186, 757–761 (2010).
Miller, J. C. et al. A TALE nuclease architecture for efficient genome editing. Nature Biotech. 29, 143–148 (2011).
Porteus, M. H. & Baltimore, D. Chimeric nucleases stimulate gene targeting in human cells. Science 300, 763 (2003). The first demonstration that ZFNs enhance gene targeting in human cells.
Ciccia, A. & Elledge, S. J. The DNA damage response: making it safe to play with knives. Mol. Cell 40, 179–204 (2010).
Perez, E. E. et al. Establishment of HIV-1 resistance in CD4+ T cells by genome editing using zinc-finger nucleases. Nature Biotech. 26, 808–816 (2008). The first application of non-homologous end-joining-mediated gene disruption by ZFNs to establish resistance to HIV-1 infection in primary T lymphocytes. See also the study below for application to haematopoietic progenitors. Clinical trials based on this strategy are underway in patients infected with HIV.
Holt, N. et al. Human hematopoietic stem/progenitor cells modified by zinc-finger nucleases targeted to CCR5 control HIV-1 in vivo. Nature Biotech. 28, 839–847 (2010).
Urnov, F. D. et al. Highly efficient endogenous human gene correction using designed zinc-finger nucleases. Nature 435, 646–651 (2005). The first demonstration of gene conversion at an endogenous locus of human cells induced by ZFN-mediated gene targeting.
Lombardo, A. et al. Gene editing in human stem cells using zinc finger nucleases and integrase-defective lentiviral vector delivery. Nature Biotech. 25, 1298–1306 (2007). This study demonstrates that gene conversion and targeted integration of a transgene cassette into a ZFN target site can be achieved with high efficiency in human cells, including embryonic stem cells, by vectorization of the ZFNs and donor template.
Grizot, S. et al. Efficient targeting of a SCID gene by an engineered single-chain homing endonuclease. Nucleic Acids Res. 37, 5405–5419 (2009).
Zou, J. et al. Gene targeting of a disease-related gene in human induced pluripotent stem and embryonic stem cells. Cell Stem Cell 5, 97–110 (2009).
Hockemeyer, D. et al. Efficient targeting of expressed and silent genes in human ESCs and iPSCs using zinc-finger nucleases. Nature Biotech. 27, 851–857 (2009).
Aiuti, A. et al. Correction of ADA-SCID by stem cell gene therapy combined with nonmyeloablative conditioning. Science 296, 2410–2413 (2002). This study introduced the use of non-myeloablative conditioning to favour stable engraftment of gene-corrected cells in HSC gene therapy of SCID.
Gattinoni, L. et al. Removal of homeostatic cytokine sinks by lymphodepletion enhances the efficacy of adoptively transferred tumor-specific CD8+ T cells. J. Exp. Med. 202, 907–912 (2005).
Hanna, J. H., Saha, K. & Jaenisch, R. Pluripotency and cellular reprogramming: facts, hypotheses, unresolved issues. Cell 143, 508–525 (2010).
Wada, T. & Candotti, F. Somatic mosaicism in primary immune deficiencies. Curr. Opin. Allergy Clin. Immunol. 8, 510–514 (2008).
Zielske, S. P., Reese, J. S., Lingas, K. T., Donze, J. R. & Gerson, S. L. In vivo selection of MGMT(P140K) lentivirus-transduced human NOD/SCID repopulating cells without pretransplant irradiation conditioning. J. Clin. Invest. 112, 1561–1570 (2003).
Beard, B. C. et al. Efficient and stable MGMT-mediated selection of long-term repopulating stem cells in nonhuman primates. J. Clin. Invest. 120, 2345–2354 (2010).
Larochelle, A. et al. In vivo selection of hematopoietic progenitor cells and temozolomide dose intensification in rhesus macaques through lentiviral transduction with a drug resistance gene. J. Clin. Invest. 119, 1952–1963 (2009).
Nienhuis, A. W. Assays to evaluate the genotoxicity of retroviral vectors. Mol. Ther. 14, 459–460 (2006).
Will, E. et al. Importance of murine study design for testing toxicity of retroviral vectors in support of phase I trials. Mol. Ther. 15, 782–791 (2007).
Arumugam, P. I. et al. Genotoxic potential of lineage-specific lentivirus vectors carrying the β-globin locus control region. Mol. Ther. 17, 1929–1937 (2009).
McDermott, S. P., Eppert, K., Lechman, E. R., Doedens, M. & Dick, J. E. Comparison of human cord blood engraftment between immunocompromised mouse strains. Blood 116, 193–200 (2010).
Trobridge, G. D. & Kiem, H. P. Large animal models of hematopoietic stem cell gene therapy. Gene Ther. 17, 939–948 (2010).
Kiem, H. P. et al. Long-term clinical and molecular follow-up of large animals receiving retrovirally transduced stem and progenitor cells: no progression to clonal hematopoiesis or leukemia. Mol. Ther. 9, 389–395 (2004).
Enssle, J. et al. Stable marking and transgene expression without progression to monoclonality in canine long-term hematopoietic repopulating cells transduced with lentiviral vectors. Hum. Gene Ther. 21, 397–403 (2010).
Huthoff, H. & Towers, G. J. Restriction of retroviral replication by APOBEC3G/F and TRIM5α. Trends Microbiol. 16, 612–619 (2008).
Deichmann, A. et al. Vector integration is nonrandom and clustered and influences the fate of lymphopoiesis in SCID-X1 gene therapy. J. Clin. Invest. 117, 2225–2232 (2007).
Wang, G. P. et al. DNA bar coding and pyrosequencing to analyze adverse events in therapeutic gene transfer. Nucleic Acids Res. 36, e49 (2008).
Aiuti, A. et al. Multilineage hematopoietic reconstitution without clonal selection in ADA-SCID patients treated with stem cell gene therapy. J. Clin. Invest. 117, 2233–2240 (2007).
Schwarzwaelder, K. et al. Gammaretrovirus-mediated correction of SCID-X1 is associated with skewed vector integration site distribution in vivo. J. Clin. Invest. 117, 2241–2249 (2007).
Cattoglio, C. et al. High-definition mapping of retroviral integration sites defines the fate of allogeneic T cells after donor lymphocyte infusion. PLoS ONE 5, e15688 (2010).
Kustikova, O. et al. Clonal dominance of hematopoietic stem cells triggered by retroviral gene marking. Science 308, 1171–1174 (2005). This study shows that retroviral vector integrations may trigger non-malignant clonal expansion in murine mouse long-term haematopoiesis.
Calmels, B. et al. Recurrent retroviral vector integration at the Mds1/Evi1 locus in nonhuman primate hematopoietic cells. Blood 106, 2530–2533 (2005).
Kustikova, O. S. et al. Retroviral vector insertion sites associated with dominant hematopoietic clones mark “stemness” pathways. Blood 109, 1897–1907 (2007).
Xie, J. et al. Repetitive busulfan administration after hematopoietic stem cell gene therapy associated with a dominant HDAC7 clone in a nonhuman primate. Hum. Gene Ther. 21, 695–703 (2010).
Abel, U. et al. Real-time definition of non-randomness in the distribution of genomic events. PLoS ONE 2, e570 (2007).
Wang, G. P. et al. Dynamics of gene-modified progenitor cells analyzed by tracking retroviral integration sites in a human SCID-X1 gene therapy trial. Blood 115, 4356–4366 (2010).
Biffi, A. et al. Lentiviral-vector common integration sites in preclinical models and a clinical trial reflect a benign integration bias and not oncogenic selection. Blood 14 Mar 2011 (doi:10.1182/blood-2010-09-306761).
Kustikova, O. S. et al. Cell-intrinsic and vector-related properties cooperate to determine the incidence and consequences of insertional mutagenesis. Mol. Ther. 17, 1537–1547 (2009).
Mezquita, P., Beard, B. C. & Kiem, H. P. NOD/SCID repopulating cells contribute only to short-term repopulation in the baboon. Gene Ther. 15, 1460–1462 (2008).
Gabriel, R. et al. Comprehensive genomic access to vector integration in clinical gene therapy. Nature Med. 15, 1431–1436 (2009). This study reports a technological advance that allows for unbiased retrieval of vector integration sites in genome-wide studies.
Gaspar, H. B. et al. Successful reconstitution of immunity in ADA-SCID by stem cell gene therapy following cessation of PEG-ADA and use of mild preconditioning. Mol. Ther. 14, 505–513 (2006).
Kohn, D. B. & Candotti, F. Gene therapy fulfilling its promise. N. Engl. J. Med. 360, 518–521 (2009).
Kang, E. M. et al. Retrovirus gene therapy for X-linked chronic granulomatous disease can achieve stable long-term correction of oxidase activity in peripheral blood neutrophils. Blood 115, 783–791 (2010).
Jacome, A. et al. Lentiviral-mediated genetic correction of hematopoietic and mesenchymal progenitor cells from Fanconi anemia patients. Mol. Ther. 17, 1083–1092 (2009).
DiGiusto, D. L. et al. RNA-based gene therapy for HIV with lentiviral vector-modified CD34+ cells in patients undergoing transplantation for AIDS-related lymphoma. Sci. Transl. Med. 2, 36ra43 (2010).
Acknowledgements
I thank my colleagues at the Telethon San Raffaele Institute for Gene Therapy, The Division of Regenerative Medicine and Gene Therapy of the San Raffaele Institute, and all my past and current laboratory members for sharing in the excitement and challenges of making cell and gene therapy a clinical reality, as well as for critical discussion of this manuscript. The Naldini laboratory is supported by Telethon, the European Research Council, the European 7th Framework Program for Life Sciences, the Italian Association for Cancer Research, the Italian Ministries of Health and of Scientific Research, Sangamo Biosciences, the Cariplo Foundation and the Stop ALD Foundation. The author apologizes to all scientists whose research could not be properly discussed and cited in this Review owing to strict space limitations. For this reason, many primary and historical publications have not been cited, particularly in cases where topical reviews are available.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
Related links
Glossary
- Transduction
-
The transfer of genetic material into a cell mediated by a viral vector.
- Autologous
-
In transplantology, this refers to cells transplanted from an individual to that same individual (often after an ex vivo procedure has been performed).
- Storage disorder
-
A disease caused by genetic deficiency of a lysosomal or peroxysomal enzyme, leading to intracellular accumulation of undegraded substrate, cellular pathology and malfunction of multiple organs.
- Severe combined immunodeficiencies
-
A family of genetic disorders that affect T cell differentiation and B cell immunity, resulting in the absence of a functional immune system.
- Allogenic
-
In transplantology, the use of cells or tissue from any human other than self or a monozygotic twin.
- Graft versus host disease
-
A destructive attack on host tissues by immune cells that are derived from a transplant of allogenic haematopoietic cells.
- Suicide gene
-
A gene that encodes a protein that can convert a non-toxic pro-drug into a cytotoxic compound.
- Thymic selection
-
The central tolerance that occurs during early T cell development in the thymus that causes cells with strong reactivity to self-antigens to undergo apoptosis and elimination.
- Episome
-
An extrachromosomal DNA element, such as a plasmid, in a cell nucleus.
- Minichromosome
-
An extranumerary minimal chromosome that contains functional elements, such as telomeres and centromeres, and is transmitted in meiosis and mitosis.
- Retroviruses
-
RNA-containing viruses that encode an RNA-dependent DNA polymerase, reverse transcriptase. Retroviruses replicate by reverse transcription and then integrate into the host genome. They comprise simple and complex retroviruses according to the genome organization. Simple retroviruses have oncogenic potential.
- Lentiviruses
-
Retroviruses with a complex genome that usually causes delayed disease in their hosts. HIV is an example of a lentivirus.
- Transposase
-
An enzyme that carries out the site-specific DNA recombination that is required for transposition.
- Tropism
-
The spectrum of tissues and host species that a virus or viral vector can infect, owing to a restricted distribution of receptors or other essential cofactors of infection in certain tissues or species and not in others.
- Serial transplantation
-
When donor-derived cells or tissue are used for another transplant after engraftment in a primary recipient.
- Long terminal repeat
-
(LTR). A DNA sequence that is repeated at each end of an integrated retroviral DNA (provirus). A LTR contains regulatory sequences that are required to initiate transcription of the viral DNA into an RNA that is packaged into viral particles, retro-transcribed and integrated into the target cell DNA.
- Neoantigen
-
A newly encountered substance that the immune system can respond to by producing antibodies or immunoreactive T cells.
Rights and permissions
About this article
Cite this article
Naldini, L. Ex vivo gene transfer and correction for cell-based therapies. Nat Rev Genet 12, 301–315 (2011). https://doi.org/10.1038/nrg2985
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrg2985
This article is cited by
-
PEG-mediated transduction of rAAV as a platform for spatially confined and efficient gene delivery
Biomaterials Research (2022)
-
Biomimetic cell-derived nanocarriers in cancer research
Journal of Nanobiotechnology (2022)
-
Bioengineering strategies for restoring vision
Nature Biomedical Engineering (2022)
-
Lentiviral mediated RPE65 gene transfer in healthy hiPSCs-derived retinal pigment epithelial cells markedly increased RPE65 mRNA, but modestly protein level
Scientific Reports (2020)
-
Targeted gene therapy into a safe harbor site in human hematopoietic progenitor cells
Gene Therapy (2020)