Abstract
Current guidance around the prevention of cardiovascular events is based on long-term risk, typically calculated over 10 years. A growing body of evidence, however, suggests that vascular risk fluctuates greatly over much shorter time periods. We suggest a new paradigm for cardiovascular risk management that is based on targeting interventions during periods of enhanced risk. During such high-risk time windows, prophylactic therapy could have a disproportionately large absolute benefit, altering the risk–benefit balance and cost-effectiveness of available treatments. Major surgery is an example of an exposure known to lead to a transient increase in vascular risk. Emerging evidence supports the usefulness of short-term preventative interventions in the perioperative period. Influenza infection is another exposure known to increase the risk of vascular events, and cardiovascular mortality and morbidity are likely to be major features associated with pandemic influenza. Important questions remain, however, before preventative interventions can be offered as a routine part of influenza management.
Similar content being viewed by others
Considering risk fluctuation is vital
Atherosclerosis is a fairly benign chronic condition; its devastating effects on morbidity and mortality result largely from acute arterial events, such as myocardial infarction (MI) and stroke. Interventions to reduce the risk of such vascular events are currently guided by estimations of long-term cardiovascular risk. For example, both US national guidelines1 and the guidance by the UK's National Institute for Health and Clinical Excellence2 recommend the use of statins by people whose absolute risk of a cardiovascular event exceeds 20% over the next 10 years. Emerging evidence, however, indicates that the risk of vascular events is not homogeneous over time, but rises and falls within short time periods in response to a range of common physiological and environmental exposures.
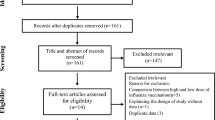
An example of one of these factors is infection. The risk of MI is increased up to fourfold (Figure 1) and that of stroke more than twofold in the period following naturally occurring infections.3 Such an effect on cardiovascular risk may be particularly marked in the setting of influenza infection.4,5 In an influenza pandemic, during which a substantial proportion of the adult population may be infected, even a short-lived effect could lead to a high number of vascular events. The high risk of vascular events following major surgery is also well established. In the first 30 days following major elective noncardiac surgery, the absolute risk of nonfatal MI, cardiac arrest or cardiovascular mortality is 6%,6 a higher absolute risk during a single month than many people experience over 5 years. A link between short-term systemic inflammation and endothelial dysfunction was observed after therapy for severe periodontal disease, an intervention known to lead to a marked inflammatory response,7 and may also underlie the increased cardiovascular risk associated with other infections or surgery.
Data from Smeeth et al. N. Engl. J. Med. 351, 2611–2618 (2004).3
Environmental exposures can also increase short-term cardiovascular risk, and while their effects may seem small, the large number of individuals affected could translate into a substantial public health impact. Evidence exists that short-term fluctuations in air pollution affect the risk of MI. The most consistent finding relates to small particulate matter, with estimates for the increased risk of MI ranging from 5% to 17% per 10 mg/m3 increase in particulate matter of <2.5 µm diameter.8 Unusually high or low ambient temperatures are also associated with an increased risk of MI.9 A relative risk of MI of 1.02 per degree temperature may sound small, but because the whole population is exposed, this risk translates into a 2% increase in the total number of MIs for each degree change.
Other factors that affect physiology may also lead to short-term increases in cardiovascular risk. Acute exertion has long been recognized as a trigger for MI10 and even an apparently benign activity such as watching a soccer match is associated with a doubling in the risk of cardiovascular events.11
It is time to take notice of these acute fluctuations. The fluctuation of cardiovascular risk across short time periods has not been taken into account by the current general guidelines for reduction of cardiovascular risk.
Prevention at high-risk times
We suggest a new paradigm for cardiovascular risk management that is based on identifying specific periods of enhanced risk and targeting interventions during these periods. During such high risk periods, the absolute benefits of interventions are far higher than in periods of lesser risk, which provides an opportunity to prevent large numbers of vascular events. This opportunity is currently being largely ignored. The absolute risk of an event over a 30-day period is <0.2% in individuals with a 10-year risk of cardiovascular disease of 20% (currently the recommended threshold for statin treatment). By contrast, the observed 30-day event rate for people older than 50 years of age who undergo elective surgery is 6%. Administration of statins to people at increased risk of vascular disease was shown to reduce the long-term risk of a first or recurrent vascular event by around 20% in primary and secondary prevention studies, respectively.12,13 Therefore, among the group of people who are at the recommended threshold for preventative statin treatment, around 3,000 people would need to be treated (Box 1) with statins for 1 month to prevent one event. Assuming the same relative reduction in risk with statin treatment, the number needed to be treated for 1 month postoperatively could be as low as 84. Therefore, targeting statin treatment to high-risk periods would be highly cost-effective.
Prophylactic interventions to prevent cardiovascular disease could be particularly important in those people whose 10-year risk of cardiovascular disease is well below the widely used 20% threshold—and who thus will not be taking a statin or other preventative therapies—but who will experience transient periods of much higher risk. During these high-risk periods, the relative risk reductions achieved by prophylactic therapy will translate into a large absolute benefit, which provides an opportunity to prevent major events. The concept of providing prophylactic pharmacological interventions during high-risk periods is already well established for preventing venous thromboembolism during hospital admission.14 Such an approach, however, has not been widely considered or evaluated for arterial thromboembolic disease.
Possible short-term therapies
Possible therapies for use over short periods of increased risk are likely to be those shown to be safe and efficacious in long-term settings. The two most widely used long-term prophylactic drug therapies for cardiovascular disease are statins and aspirin. Growing evidence shows that statins exert rapid effects: endothelial function and arterial flow improve within 24 h of initiation of statin administration,15 and the levels of inflammatory markers such as C-reactive protein are reduced within 3 days.16 The beneficial effects of statin therapy among people at increased risk of vascular disease are clear; the life-table plot for the occurrence of cardiovascular events of the group of patients receiving statins separates almost immediately from that of patients receiving placebo.12 Although the number of events that occurred in the first few weeks of these trials were small, which limits the power to analyze this time frame, substantial benefits of statin administration on vascular end points are evident in the first year of treatment.13 Furthermore, early initiation of statin therapy in acute coronary syndrome reduces the risk of death and nonfatal vascular events.17 These findings suggest that the benefits of statins would be exhibited during short-term high-risk periods.
The evidence for short-term cardiovascular effects of aspirin and other antiplatelet agents is strong. Although the risk–benefit ratio of aspirin therapy in primary prevention of cardiovascular disease seems likely to be unfavorable in people at low to moderate vascular risk,18 during high-risk windows its beneficial effects may well outweigh the documented risks of hemorrhage. The benefits of aspirin or clopidogrel or both during acute vascular events are established, and stopping antiplatelet therapy is associated with a rapid increase in risk of recurrent MI and death.19 Prasugrel20 and ticagrelor,21 novel antiplatelet agents with a more rapid onset than clopidogrel, may be of particular value as acute short-term therapies.
Antihypertensive drugs, such as calcium-channel blockers, rapidly reduce blood pressure. In randomized trials, their full effect on blood-pressure reduction is achieved within the first year of treatment.22 Whether protective effects are seen more rapidly is unclear. Anticoagulation agents are other potential therapies for acute periods of high cardiovascular risk. Among these, the relatively slow onset and the need for dose adjustment and monitoring make warfarin problematic as an acute therapy compared with newer agents. Both rivaroxaban23 (a factor Xa inhibitor) and dabigatran24 (a thrombin inhibitor), however, do not have these problems, which makes them good candidates for study as prophylactic agents during short-term high-risk periods.
The beneficial effects of β-blocker use following MI suggest that these agents may have a useful role also in other high-risk periods. Considerable interest has been raised about their role in the postoperative period, particularly in preventing MI, as discussed in the next section of this article.
Measures that are not based on drug treatment may also have a role in reducing short-term cardiovascular risk. Ischemic preconditioning involves deliberately exposing tissues to brief, repeated periods of vascular occlusion to render them resistant to the adverse effects of severe ischemia.25 Inducing episodes of myocardial ischemia is not a practical intervention for widespread use. However, in a study of remote conditioning, arm ischemia induced in three 5 min cycles by means of an inflatable cuff protected the myocardium perioperatively.26 Such remote ischemic preconditioning could be a simple and cheap method of providing vascular protection during short-term periods of increased risk. Preconditioning would be expected to reduce the severity of an ischemic event rather than prevent occurrence altogether, which suggests that this approach might be most useful as adjunctive therapy.
Balancing benefits and harms
Before short-term interventions to prevent arterial vascular events during high-risk periods can be advocated, we need clearer evidence on their effectiveness. The overarching question that needs to be addressed is to establish the overall risk or cost versus the benefit of these approaches. Currently, decisions about who should receive statin therapy are largely driven by cost-effectiveness, whereas for aspirin the main deciding factor is the balance between clinical risk and benefit. During transient periods of high vascular risk, both cost-effectiveness and the risk–benefit balance change radically. The low numbers needed to treat to prevent events during such high-risk periods mean that statin therapy may become highly cost-effective. The bleeding hazards associated with aspirin therapy may be outweighed by its raised potential for benefit during these periods.
Evidence to date
Evidence for the risks of aspirin when used for primary prevention emphasizes the need to be able to identify those people who will benefit the most from intervention during periods of short-term enhanced risk. One study has demonstrated the feasibility of identifying high-risk periods and initiating transient treatment with aspirin and β-blockers.27 However, while this approach was shown to be feasible, its effectiveness has not yet been clearly demonstrated. The largest body of research into the effectiveness of prophylactic therapy in periods of high cardiovascular risk comes from studies in the perioperative period, but even in this setting the findings are inconclusive. A systematic review that included two small trials and several large observational studies of perioperative statin therapy concluded that the data are insufficient to reliably guide therapy.28 A subsequent trial among patients undergoing noncardiovascular surgery did not find a significant beneficial effect of perioperative statin therapy.29 However, among patients undergoing vascular surgery, a marked protective effect of fluvastatin given perioperatively against cardiovascular death or MI was observed (hazard ratio 0.47, 95% CI 0.24–0.94).30 For perioperative β-blockers, the largest trial to date found a reduction in the primary cardiovascular end point (a composite of cardiovascular death, nonfatal MI, and nonfatal cardiac arrest), but a higher risk of stroke and total deaths among patients who received β-blockers perioperatively than among patients who did not receive this treatment.31 An updated meta-analysis concluded that the “evidence does not support the use of β-blocker therapy for the prevention of perioperative clinical outcomes in patients having noncardiac surgery”.32
Future perspectives
The inconclusive research results obtained to date highlight the importance of large randomized trials to guide therapy. An example currently applicable would be offering people with influenza-like illness randomization to short-term vascular prophylactic therapies or placebo or no prophylactic treatment. A discussion of the rationale for use of these approaches in the prevention of cardiovascular risk is needed (Box 2). Key research questions on these potential therapeutic strategies include which patients warrant treatment and how can they be identified, which interventions to use, drug dosage, length of treatment, and safety.
References
Grundy, S. M. et al. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III Guidelines. J. Am. Coll. Cardiol. 44, 720–732 (2004).
National Institute for Health and Clinical Excellence. Statins for the prevention of cardiovascular events. National Institute for Health and Clinical Excellence [online], (2006).
Smeeth, L. et al. Risk of myocardial infarction and stroke after acute infection or vaccination. N. Engl. J. Med. 351, 2611–2618 (2004).
Warren-Gash, C., Smeeth, L. & Hayward, A. C. Influenza as a trigger for acute myocardial infarction or death from cardiovascular disease: a systematic review. Lancet Infect. Dis. 9, 601–610 (2009).
Madjid, M. & Casscells, S. W. Of birds and men: cardiologists' role in influenza pandemics. Lancet 364, 1309 (2004).
Devereaux, P. J. et al. Perioperative cardiac events in patients undergoing noncardiac surgery: a review of the magnitude of the problem, the pathophysiology of the events and methods to estimate and communicate risk. CMAJ 173, 627–634 (2005).
Tonetti, M. S. et al. Treatment of periodontitis and endothelial function. N. Engl. J. Med. 356, 911–920 (2007).
Bhaskaran, K. et al. Effects of air pollution on the incidence of myocardial infarction. Heart 95, 1746–1759 (2009).
Bhaskaran, K. et al. Effects of ambient temperature on the incidence of myocardial infarction. Heart 95, 1760–1769 (2009).
Mittleman, M. A. et al. Triggering of acute myocardial infarction by heavy physical exertion. Protection against triggering by regular exertion. Determinants of Myocardial Infarction Onset Study Investigators. N. Engl. J. Med. 329, 1677–1683 (1993).
Wilbert-Lampen, U. et al. Cardiovascular events during World Cup soccer. N. Engl. J. Med. 358, 475–483 (2008).
Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet 360, 7–22 (2002).
Baigent, C. et al. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 366, 1267–1278 (2005).
National Institute for Health and Clinical Excellence. Reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital. National Institute for Health and Clinical Excellence [online], (2010).
Laufs, U. et al. Rapid effects on vascular function after initiation and withdrawal of atorvastatin in healthy, normocholesterolemic men. Am. J. Cardiol. 88, 1306–1307 (2001).
Li, J. J., Fang, C. H., Qian, H. Y. & Hu, W. L. Time course of rapid C-reactive protein reduction by pravastatin in patients with stable angina. Angiology 57, 1–7 (2006).
Hulten, E., Jackson, J. L., Douglas, K., George, S. & Villines, T. C. The effect of early, intensive statin therapy on acute coronary syndrome: a meta-analysis of randomized controlled trials. Arch. Intern. Med. 166, 1814–1821 (2006).
Antithrombotic Trialists' (ATT) Collaboration. Aspirin in the primary and secondary prevention of vascular disease: collaborative meta-analysis of individual participant data from randomised trials. Lancet 373, 1849–1860 (2009).
Ho, P. M. et al. Incidence of death and acute myocardial infarction associated with stopping clopidogrel after acute coronary syndrome. JAMA 299, 532–539 (2008).
Montalescot, G. et al. Prasugrel compared with clopidogrel in patients undergoing percutaneous coronary intervention for ST-elevation myocardial infarction (TRITON-TIMI 38): double-blind, randomised controlled trial. Lancet 373, 723–731 (2009).
Wallentin, L. et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N. Engl. J. Med. 361, 1045–1057 (2009).
Law, M. R., Morris, J. K. & Wald, N. J. Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ 338, b1665 (2009).
Mega, J. L. et al. Rivaroxaban versus placebo in patients with acute coronary syndromes (ATLAS ACS-TIMI 46): a randomised, double-blind, phase II trial. Lancet 374, 29–38 (2009).
Connolly, S. J. et al. Dabigatran versus warfarin in patients with atrial fibrillation. N. Engl. J. Med. 361, 1139–1151 (2009).
Murry, C. E., Jennings, R. B. & Reimer, K. A. Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 74, 1124–1136 (1986).
Hausenloy, D. J. et al. Effect of remote ischaemic preconditioning on myocardial injury in patients undergoing coronary artery bypass graft surgery: a randomised controlled trial. Lancet 370, 575–579 (2007).
Shaw, E., Tofler, G. H., Buckley, T., Bajorek, B. & Ward, M. Therapy for triggered acute risk prevention: a study of feasibility. Heart Lung Circ. 18, 347–352 (2009).
Kapoor, A. S., Kanji, H., Buckingham, J., Devereaux, P. J. & McAlister, F. A. Strength of evidence for perioperative use of statins to reduce cardiovascular risk: systematic review of controlled studies. BMJ 333, 1149 (2006).
Dunkelgrun, M. et al. Bisoprolol and fluvastatin for the reduction of perioperative cardiac mortality and myocardial infarction in intermediate-risk patients undergoing noncardiovascular surgery: a randomized controlled trial (DECREASE-IV). Ann. Surg. 249, 921–926 (2009).
Schouten, O. et al. Fluvastatin and perioperative events in patients undergoing vascular surgery. N. Engl. J. Med. 361, 980–989 (2009).
POISE Study Group. Effects of extended-release metoprolol succinate in patients undergoing non-cardiac surgery (POISE trial): a randomised controlled trial. Lancet 371, 1839–1847 (2008).
Bangalore, S. et al. Perioperative beta blockers in patients having non-cardiac surgery: a meta-analysis. Lancet 372, 1962–1976 (2008).
Acknowledgements
Patrick Vallance contributed to discussions and Raymond Macallister provided useful comments on an earlier draft of the article. L. Smeeth is supported by a senior clinical fellowship from the Wellcome Trust (082178) and A. D. Hingorani is supported by a senior fellowship from the British Heart Foundation. The funders played no role in the preparation and content of the article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Smeeth, L., Hingorani, A. Short-term vascular risk: time to take notice?. Nat Rev Cardiol 7, 409–411 (2010). https://doi.org/10.1038/nrcardio.2010.64
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2010.64