Abstract
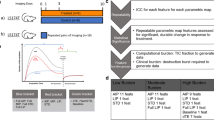
Techniques for noninvasive imaging of specific disease-related molecular changes are being developed to enhance diagnosis and therapeutic decision making in the clinical setting, and to facilitate research efforts. Molecular imaging with contrast-enhanced ultrasonography relies on the detection of the acoustic signal produced by microbubble or nanoparticle agents that are targeted to sites of disease. This Review describes the basis for ultrasound molecular imaging, the unique features of contrast agent behavior or detector performance in relation to clinical or research needs, and the progress that has been made to date in imaging key events in cardiovascular medicine, such as atherosclerosis, postischemic inflammation, angiogenesis, transplant rejection and thrombus formation.
Key Points
-
Targeted microbubble contrast agents are intravascular tracers and are, therefore, best suited to detection of disease states where molecular changes occur within the vascular space
-
Advantages of contrast-enhanced ultrasonography for molecular imaging include speed of imaging (10 min), ability to perform repetitive injections to image multiple targets, and sensitivity
-
Disadvantages of contrast-enhanced ultrasonography are that the contrast agent cannot access pathologic targets outside the vascular space and has a relatively short lifespan, which limits their ability to track cell migration or survival
-
Imaging of inflammation in ischemia, infarction, transplant rejection, and atherosclerosis has been achieved by targeting microbubbles to immune cells (including monocytes and neutrophils) or to endothelial cell adhesion molecules
-
Imaging of endothelial markers of angiogenesis or components of the immune response associated with angiogenesis can provide information on endogenous or growth-factor-stimulated vascular remodeling before flow changes occur
-
Thrombus targeting is possible by targeting ultrasound contrast agents to activated platelets or fibrin, although problems with ligand specificity have limited rapid progress of this strategy
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
DeJong, N. et al. Optical imaging of contrast agent microbubbles in an ultrasound field with a 100-MHz camera. Ultrasound Med. Biol. 26, 487–492 (2000).
Dayton, P. A., Morgan, K. E., Klibanov, A. L., Brandenburger, G. H. & Ferrara, K. W. Optical and acoustical observations of the effects of ultrasound on contrast agents. IEEE Trans. Ultrason. Ferroelectr. Freq. Control 46, 220–232 (1999).
Kaufmann, B., Wei, K. & Lindner, J. R. Contrast Echocardiography. Curr. Prob. Cardiol. 32, 45–96 (2007).
Epstein, P. S. & Plesset, M. S. On the stability of gas bubbles in liquid-gas solutions. J. Chem. Phys. 18, 1505–1509 (1950).
Sarkar, K., Shi, W. T., Chatterjee, D. & Forsberg, F. Characterization of ultrsaound contrast microbubbles using in vitro experiments and viscous and viscoelastic interface models for encapsulation. J. Acoust. Soc. Am. 118, 539–550 (2005).
Lindner, J. R. et al. Noninvasive imaging of inflammation by ultrasound detection of phagocytosed microbubbles. Circulation 102, 531–538 (2000).
Dayton, P. A. et al. Optical and acoustical dynamics of microbubble contrast agents inside neutrophils. Biophys. J. 80, 1547–1556 (2000).
Dayton, P. A. et al. Ultrasonic analysis of peptide- and antibody-targeted microbubble contrast agents for molecular imaging of αvβ3-expressing cells. Mol. Imag. 3, 125–134 (2004).
Lankford, M. et al. Effect of microbubble attachment to cells on ultrasound signal enhancement: implications for targeted imaging. Invest. Radiol. 41, 721–728 (2006).
Lindner, J. R. et al. Microbubble persistence in the microcirculation during ischemia-reperfusion and inflammation: integrin- and complement-mediated adherence to activated leukocytes. Circulation 101, 668–675 (2000).
Lindner, J. R. et al. Noninvasive ultrasound imaging of inflammation using microbubbles targeted to activated leukocytes. Circulation 102, 2745–2750 (2000).
Christiansen, J. P. et al. Non-invasive imaging of myocardial reperfusion injury using leukocyte-targeted contrast echocardiography. Circulation 105, 1764–1767 (2002).
Kondo, I. et al. Leukocyte-targeted myocardial contrast echocardiography can assess the degree of acute allograft rejection in a rat cardiac transplantation model. Circulation 109, 1056–1061 (2004).
Behm, C. Z. et al. Molecular imaging of VCAM-1 and inflammatory cell recruitment during arteriogenesis and vasculogenesis. Circulation 117, 2902–2911 (2008).
Lindner, J. R., Song, J., Jayaweera, A. R., Sklenar, J. & Kaul, S. Microvascular rheology of Definity microbubbles after intra-arterial and intravenous administration. J. Am. Soc. Echocardiogr. 15, 396–403 (2002).
Anderson, D. R., Tsutsui, J. M., Xie, F., Radio, S. J. & Porter, T. R. The role of complement in the adherence of microbubbles to dysfunctional arterial endothelium and atherosclerotic plaque. Cardiovasc. Res. 73, 597–606 (2007).
Lindner, J. R. et al. Ultrasound assessment of inflammation and renal tissue injury with microbubbles targeted to P-selectin. Circulation 104, 2107–2112 (2001).
Bevilacqua, M. & Nelson, R. M. Selectins. J. Clin. Invest. 91, 379–387 (1993).
Chukwuemeka, A. O., Brown, A., Venn, G. E. & Chambers, D. J. Changes in P-selectin expression on cardiac microvessels in blood-perfused rat hearts subjected to ischemia reperfusion. Ann. Thorac. Surg. 79, 204–211 (2005).
Kaufmann, B., Lewis, C., Xie, A., Mirza-Mohd, A. & Lindner, J. R. Detection of recent myocardial ischemia by molecular imaging of P-selectin with targeted contrast echocardiography. Eur. Heart J. 28, 2011–2017 (2007).
Villanueva, F. S. et al. Myocardial ischemic memory imaging with molecular echocardiography. Circulation 115, 345–352 (2007).
Weller, G. E. et al. Ultrasound imaging of acute cardiac transplant rejection with microbubbles targeted to intercellular adhesion molecule-1. Circulation 108, 218–224 (2003).
Iiyama, K. et al. Patterns of vascular cell adhesion molecule-1 and intercellular adhesion molecule-1 expression in rabbit and mouse atherosclerotic lesions and at sites predisposed to lesion formation. Circ. Res. 85, 199–207 (1999).
O'Brien, K. D., McDonald, T. O., Chait, A., Allen, M. D., Alpers, C. E. Neovascular expression of E-selectin, intercellular adhesion molecule-1, and vascular cell adhesion molecule-1 in human atherosclerosis and their relation to intimal leukocyte content. Circulation 93, 672–682 (1996).
Kaufmann, B. et al. Molecular imaging of inflammation in atherosclerosis with targeted ultrasound detection of vascular cell adhesion molecule-I. Circulation 116, 276–284 (2007).
Demos, S. M. et al. In vivo targeting of acoustically reflective liposomes for intravascular and transvascular ultrasonic enhancement. J. Am. Coll. Cardiol. 33, 867–875 (1999).
Hamilton, A. J. et al. Intravascular ultrasound molecular imaging of atheroma components in vivo. J. Am. Coll. Cardiol. 43, 453–460 (2004).
Kaufmann, B. A. et al. Molecular imaging of endothelial cell activation predicts future atherosclerotic plaque development [abstract 904-253]. J. Am. Coll. Cardiol. 51 (Suppl. A), A125 (2008).
Lee, S. et al. Contrast-enhanced ultrasound characterization of inflammation and vasa vasoral proliferation caused by mural hemorrhage and platelet deposition [abstract 1074]. Circulation 118 (Suppl. 2), S644 (2008).
Kolodgie, F. D. et al. Intraplaque hemorrhage and progression of coronary atheroma. N. Engl. J. Med. 349, 2316–2325 (2003).
Moreno, P. R., Purushothaman, K. R., Sirol, M., Levy, A. P. & Fuster, V. Neovascularization in human atherosclerosis. Circulation 113, 2245–2252 (2006).
Leong-Poi, H., Christiansen, J., Klibanov, A. L., Kaul, S. & Lindner, J. R. Non-invasive assessment of angiogenesis by ultrasound and microbubbles targeted to αv-integrins. Circulation 107, 455–460 (2003).
Ellegala, D. B. et al. Imaging tumor angiogenesis with contrast ultrasound and microbubbles targeted to αvβ3 . Circulation 108, 336–341 (2003).
Leong Poi, H. et al. Assessment of endogenous and therapeutic arteriogenesis by contrast ultrasound molecular imaging of integrin expression. Circulation 111, 3248–3254 (2005).
Unger, E. C., McCreery, T. P., Sweitzer, R. H., Shen, D. & Wu, G. In vitro studies of a new thrombus-specific ultrasound contrast agent. Am. J. Cardiol. 81, 58G–61G (1998).
Alonso, A. et al. Molecular imaging of human thrombus with novel abciximab immunobubbles and ultrasound. Stroke 38, 1508–1514 (2007).
Takeuchi, M. et al. Enhanced visualization of intravascular and left atrial appendage thrombus with the use of a thrombus-targeting ultrasonographic contrast agent (mrx-408a1): In vivo experimental echocardiographic studies. J. Am. Soc. Echocardiogr. 12, 1015–1021 (1999).
Lanza, G. M. et al. A novel site-targeted ultrasonic contrast agent with broad biomedical application. Circulation 9, 3334–3340 (1996).
Molina, C. A. et al. Microbubble administration accelerates clot lysis during continuous 2-MHz ultrasound monitoring in stroke patients treated with intravenous tissue plasminogen activator. Stroke 37, 425–429 (2006).
Xie, F. et al. Effectiveness of lipid microbubbles and ultrasound in declotting thrombosis. Ultrasound Med. Biol. 31, 979–985 (2005).
Bekeredjian, R., Grayburn, P. A. & Shohet, R. V. Use of ultrasound contrast agents for gene or drug delivery in cardiovascular medicine. J. Am. Coll. Cardiol. 45, 329–335 (2005).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
J. R. Lindner is a patent holder/applicant with the Oregon Health & Science University.
Rights and permissions
About this article
Cite this article
Lindner, J. Molecular imaging of cardiovascular disease with contrast-enhanced ultrasonography. Nat Rev Cardiol 6, 475–481 (2009). https://doi.org/10.1038/nrcardio.2009.77
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2009.77
This article is cited by
-
In vivo Biodistribution of Radiolabeled Acoustic Protein Nanostructures
Molecular Imaging and Biology (2018)
-
Feasibility of Lactadherin-Bearing Clinically Available Microbubbles as Ultrasound Contrast Agent for Angiogenesis
Molecular Imaging and Biology (2013)
-
Perspectives and opportunities for nanomedicine in the management of atherosclerosis
Nature Reviews Drug Discovery (2011)
-
Molecular Imaging of Vasa Vasorum Neovascularization via DEspR-targeted Contrast-enhanced Ultrasound Micro-imaging in Transgenic Atherosclerosis Rat Model
Molecular Imaging and Biology (2011)