Abstract
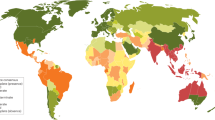
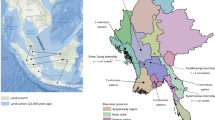
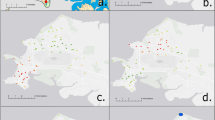
Burkholderia pseudomallei, a highly pathogenic bacterium that causes melioidosis, is commonly found in soil in Southeast Asia and Northern Australia1,2. Melioidosis can be difficult to diagnose due to its diverse clinical manifestations and the inadequacy of conventional bacterial identification methods3. The bacterium is intrinsically resistant to a wide range of antimicrobials, and treatment with ineffective antimicrobials may result in case fatality rates (CFRs) exceeding 70%4,5. The importation of infected animals has, in the past, spread melioidosis to non-endemic areas6,7. The global distribution of B. pseudomallei and the burden of melioidosis, however, remain poorly understood. Here, we map documented human and animal cases and the presence of environmental B. pseudomallei and combine this in a formal modelling framework8–10 to estimate the global burden of melioidosis. We estimate there to be 165,000 (95% credible interval 68,000–412,000) human melioidosis cases per year worldwide, from which 89,000 (36,000–227,000) people die. Our estimates suggest that melioidosis is severely underreported in the 45 countries in which it is known to be endemic and that melioidosis is probably endemic in a further 34 countries that have never reported the disease. The large numbers of estimated cases and fatalities emphasize that the disease warrants renewed attention from public health officials and policy makers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Wiersinga, W. J., Currie, B. J. & Peacock, S. J. Melioidosis. N. Engl. J. Med. 367, 1035–1044 (2012).
Aldhous, P. Tropical medicine: melioidosis? Never heard of it… Nature 434, 692–693 (2005).
Hoffmaster, A. R. et al. Melioidosis diagnostic workshop, 2013. Emerg. Infect. Dis. 21(2) (2015).
White, N. J. et al. Halving of mortality of severe melioidosis by ceftazidime. Lancet 2, 697–701 (1989).
Lipsitz, R. et al. Workshop on treatment of and postexposure prophylaxis for Burkholderia pseudomallei and B. mallei infection, 2010. Emerg. Infect. Dis. 18, e2 (2012).
Galimand, M. & Dodin, A. Repartition de Pseudomonas pseudomallei en France et dans le monde la melioidose. Bull. Soc. Vet. Prat de France 66, 651–657 (1982).
Mollaret, H. L'affaire du jardin des plantes. Med. Maladies Infect. 18(Suppl. 4), 643–654 (1988).
Bhatt, S. et al. The global distribution and burden of dengue. Nature 496, 504–507 (2013).
Gilbert, M. et al. Predicting the risk of avian influenza A H7N9 infection in live-poultry markets across Asia. Nature Commun. 5, 4116 (2014).
Pigott, D. M. et al. Mapping the zoonotic niche of Ebola virus disease in Africa. eLife 3, e04395 (2014).
Currie, B. J., Dance, D. A. & Cheng, A. C. The global distribution of Burkholderia pseudomallei and melioidosis: an update. Trans. R. Soc. Trop. Med. Hyg. 102(Suppl. 1), S1–S4 (2008).
Limmathurotsakul, D. et al. Increasing incidence of human melioidosis in northeast Thailand. Am. J. Trop. Med. Hyg. 82, 1113–1117 (2010).
Liu, X. et al. Association of melioidosis incidence with rainfall and humidity, Singapore, 2003–2012. Emerg. Infect. Dis. 21, 159–162 (2015).
Limmathurotsakul, D. et al. Activities of daily living associated with acquisition of melioidosis in northeast Thailand: a matched case-control study. PLoS Negl. Trop. Dis. 7, e2072 (2013).
Chen, P. S. et al. Airborne transmission of melioidosis to humans from environmental aerosols contaminated with B. pseudomallei. PLoS Negl. Trop. Dis. 9, e0003834 (2015).
Cheng, A. C., Jacups, S. P., Gal, D., Mayo, M. & Currie, B. J. Extreme weather events and environmental contamination are associated with case-clusters of melioidosis in the Northern Territory of Australia. Int. J. Epidemiol. 35, 323–329 (2006).
Limmathurotsakul, D. et al. Melioidosis caused by Burkholderia pseudomallei in drinking water, Thailand, 2012. Emerg. Infect. Dis. 20, 265–268 (2014).
Currie, B. J. et al. Melioidosis epidemiology and risk factors from a prospective whole-population study in northern Australia. Trop. Med. Int. Health 9, 1167–1174 (2004).
Katangwe, T. et al. Human melioidosis, Malawi, 2011. Emerg. Infect. Dis. 19, 981–984 (2013).
Centers for Disease Control and Prevention Conclusion of Select Agent Inquiry into Burkholderia pseudomallei release at Tulane National Primate Research Center (2015); http://www.cdc.gov/media/releases/2015/s0313-burkholderia-pseudomallei.html.
FAO/IIASA/ISRIC/ISSCAS/JRC. Harmonized World Soil Database (version 1.2) (FAO and IIASA, 2012).
Pumirat, P. et al. Global transcriptional profiling of Burkholderia pseudomallei under salt stress reveals differential effects on the Bsa type III secretion system. BMC Microbiol. 10, 171 (2010).
Stopnisek, N. et al. Genus-wide acid tolerance accounts for the biogeographical distribution of soil Burkholderia populations. Environ. Microbiol. 16, 1503–1512 (2013).
The World Bank World Bank open data (2013); http://data.worldbank.org/data-catalog/world-development-indicators
International Diabetes Federation Diabetes Atlas 5th edn. Country summary table: estimates for 2012 (2013); http://www.indiaenvironmentportal.org.in/files/file/diabetes%20atlas%202012.pdf
Rattanavong, S. et al. Randomized soil survey of the distribution of Burkholderia pseudomallei in rice fields in Laos. Appl. Environ. Microbiol. 77, 532–536 (2011).
GBD 2013 Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 385, 117–171 (2015).
World Health Organization Report of the first meeting of the leptospirosis burden epidemiology reference group (2010); http://whqlibdoc.who.int/publications/2010/9789241599894_eng.pdf
World Health Organization Dengue and severe dengue. http://www.who.int/mediacentre/factsheets/fs117/en/ (2015).
Newbold, T. et al. Global effects of land use on local terrestrial biodiversity. Nature 520, 45–50 (2015).
Elith, T., Leathwick, J. R. & Hastie, T. A working guide to boosted regression trees. J. Anim. Ecol. 77, 802–813 (2008).
Hijmans, R. J. Cross-validation of species distribution models: removing spatial sorting bias and calibration with a null model. Ecology 93, 679–688 (2012).
Acknowledgements
The authors thank P. Wannapinij for technical support and N. J. White and K. Schaecher for comments on the final draft. The authors also thank M. Devine for proofreading. This work was funded by the Wellcome Trust (grant no. 101103). S.I.H. is funded by a Senior Research Fellowship from the Wellcome Trust (grant no. 095066) and grants from the Bill & Melinda Gates Foundation (nos. OPP1119467, OPP1106023 and OPP1093011). S.I.H. acknowledges funding support from the RAPIDD programme of the Science & Technology Directorate, Department of Homeland Security, and the Fogarty International Center, National Institutes of Health.
Author information
Authors and Affiliations
Contributions
D.L., D.D., E.B., N.P.J.D., S.J.P. and S.I.H. conceived the research. D.L. and S.I.H. drafted the manuscript. D.L. and D.D. reviewed all the occurrence data. D.L. and N.G. carried out the modelling and analysis with advice from S.I.H. D.L., N.G., J.M. and D.P. created the maps and figures. All authors discussed the results and contributed to the revision of the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Methods, References, Table 1 and Figures 1–9. (PDF 8877 kb)
Rights and permissions
About this article
Cite this article
Limmathurotsakul, D., Golding, N., Dance, D. et al. Predicted global distribution of Burkholderia pseudomallei and burden of melioidosis. Nat Microbiol 1, 15008 (2016). https://doi.org/10.1038/nmicrobiol.2015.8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/nmicrobiol.2015.8
This article is cited by
-
Impact of template denaturation prior to whole genome amplification on gene detection in high GC-content species, Burkholderia mallei and B. pseudomallei
BMC Research Notes (2024)
-
Burkholderia pseudomallei and melioidosis
Nature Reviews Microbiology (2024)
-
Intraoperative Cardiovascular Emergency in Spinal Melioidosis Presenting as a Case of Spinal Epidural Abscess: A Rare Case Study of 2 Patients
Indian Journal of Microbiology (2024)
-
Imaging case series of melioidosis: the great masquerader
Egyptian Journal of Radiology and Nuclear Medicine (2023)
-
Burkholderia pseudomallei biofilm resists Acanthamoeba sp. grazing and produces 8-O-4′-diferulic acid, a superoxide scavenging metabolite after passage through the amoeba
Scientific Reports (2023)