Abstract
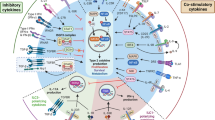
Patients with asthma, a major public health problem, are at high risk for serious disease from influenza virus infection, but the pathogenic mechanisms by which influenza A causes airway disease and asthma are not fully known. We show here in a mouse model that influenza infection acutely induced airway hyper-reactivity (AHR), a cardinal feature of asthma, independently of T helper type 2 (TH2) cells and adaptive immunity. Instead, influenza infection induced AHR through a previously unknown pathway that required the interleukin 13 (IL-13)–IL-33 axis and cells of the non-T cell, non-B cell innate lymphoid type called 'natural helper cells'. Infection with influenza A virus, which activates the NLRP3 inflammasome, resulted in much more production of IL-33 by alveolar macrophages, which in turn activated natural helper cells producing substantial IL-13.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Robinson, D.S. et al. Predominant TH2-like bronchoalveolar T-lymphocyte population in atopic asthma. N. Engl. J. Med. 326, 298–304 (1992).
Johnston, R.A. et al. Allergic airway responses in obese mice. Am. J. Respir. Crit. Care Med. 176, 650–658 (2007).
Pichavant, M. et al. Ozone exposure in a mouse model induces airway hyperreactivity that requires the presence of natural killer T cells and IL-17. J. Exp. Med. 205, 385–393 (2008).
Kim, E.Y. et al. Persistent activation of an innate immune response translates respiratory viral infection into chronic lung disease. Nat. Med. 14, 633–640 (2008).
Wright, R.J. Stress and atopic disorders. J. Allergy Clin. Immunol. 116, 1301–1306 (2005).
Oboki, K., Ohno, T., Saito, H. & Nakae, S. TH17 and allergy. Allergol. Int. 57, 121–134 (2008).
Anderson, G.P. Endotyping asthma: new insights into key pathogenic mechanisms in a complex, heterogeneous disease. Lancet 372, 1107–1119 (2008).
Kim, H.Y., DeKruyff, R.H. & Umetsu, D.T. The many paths to asthma: phenotype shaped by innate and adaptive immunity. Nat. Immunol. 11, 577–584 (2010).
Jain, S. et al. Hospitalized patients with 2009 H1N1 influenza in the United States, April-June 2009. N. Engl. J. Med. 361, 1935–1944 (2009).
Hansen, G., Berry, G., DeKruyff, R.H. & Umetsu, D.T. Allergen-specific TH1 cells fail to counterbalance TH2 cell-induced airway hyperreactivity but cause severe airway inflammation. J. Clin. Invest. 103, 175–183 (1999).
Akbari, O. et al. Essential role of NKT cells producing IL-4 and IL-13 in the development of allergen-induced airway hyperreactivity. Nat. Med. 9, 582–588 (2003).
Kanneganti, T.D. et al. Critical role for Cryopyrin/Nalp3 in activation of caspase-1 in response to viral infection and double-stranded RNA. J. Biol. Chem. 281, 36560–36568 (2006).
Thomas, P.G. et al. The intracellular sensor NLRP3 mediates key innate and healing responses to influenza A virus via the regulation of caspase-1. Immunity 30, 566–575 (2009).
Allen, I.C. et al. The NLRP3 inflammasome mediates in vivo innate immunity to influenza A virus through recognition of viral RNA. Immunity 30, 556–565 (2009).
Ichinohe, T., Pang, I.K. & Iwasaki, A. Influenza virus activates inflammasomes via its intracellular M2 ion channel. Nat. Immunol. 11, 404–410 (2010).
Moro, K. et al. Innate production of TH2 cytokines by adipose tissue-associated c-Kit+Sca-1+ lymphoid cells. Nature 463, 540–544 (2010).
Neill, D.R. et al. Nuocytes represent a new innate effector leukocyte that mediates type-2 immunity. Nature 464, 1367–1370 (2010).
Saenz, S.A. et al. IL-25 elicits a multipotent progenitor cell population that promotes TH2 cytokine responses. Nature 464, 1371–1376 (2010).
Buonocore, S. et al. Innate lymphoid cells drive interleukin-23-dependent innate intestinal pathology. Nature 464, 1371–1375 (2010).
Hammad, H. et al. House dust mite allergen induces asthma via Toll-like receptor 4 triggering of airway structural cells. Nat. Med. 15, 410–416 (2009).
Schmitz, J. et al. IL-33, an interleukin-1-like cytokine that signals via the IL-1 receptor-related protein ST2 and induces T helper type 2-associated cytokines. Immunity 23, 479–490 (2005).
Wood, I.S., Wang, B. & Trayhurn, P. IL-33, a recently identified interleukin-1 gene family member, is expressed in human adipocytes. Biochem. Biophys. Res. Commun. 384, 105–109 (2009).
Moussion, C., Ortega, N. & Girard, J.P. The IL-1-like cytokine IL-33 is constitutively expressed in the nucleus of endothelial cells and epithelial cells in vivo: a novel 'alarmin'? PLoS ONE 3, e3331 (2008).
Prefontaine, D. et al. Increased IL-33 expression by epithelial cells in bronchial asthma. J. Allergy Clin. Immunol. 125, 752–754 (2010).
Moffatt, M.F. et al. A large-scale, consortium-based genomewide association study of asthma. N. Engl. J. Med. 363, 1211–1221 (2010).
Gudbjartsson, D.F. et al. Sequence variants affecting eosinophil numbers associate with asthma and myocardial infarction. Nat. Genet. 41, 342–347 (2009).
Kondo, Y. et al. Administration of IL-33 induces airway hyperresponsiveness and goblet cell hyperplasia in the lungs in the absence of adaptive immune system. Int. Immunol. 20, 791–800 (2008).
Kurowska-Stolarska, M. et al. IL-33 amplifies the polarization of alternatively activated macrophages that contribute to airway inflammation. J. Immunol. 183, 6469–6477 (2009).
Hoshino, K. et al. The absence of interleukin 1 receptor-related T1/ST2 does not affect T helper cell type 2 development and its effector function. J. Exp. Med. 190, 1541–1548 (1999).
Mangan, N.E., Dasvarma, A., McKenzie, A.N. & Fallon, P.G. T1/ST2 expression on TH2 cells negatively regulates allergic pulmonary inflammation. Eur. J. Immunol. 37, 1302–1312 (2007).
Walzl, G. et al. Inhibition of T1/ST2 during respiratory syncytial virus infection prevents T helper cell type 2 (TH2)- but not TH1-driven immunopathology. J. Exp. Med. 193, 785–792 (2001).
Xu, D. et al. Selective expression and functions of interleukin 18 receptor on T helper (Th) type 1 but not TH2 cells. J. Exp. Med. 188, 1485–1492 (1998).
Kearley, J., Barker, J.E., Robinson, D.S. & Lloyd, C.M. Resolution of airway inflammation and hyperreactivity after in vivo transfer of CD4+CD25+ regulatory T cells is interleukin 10 dependent. J. Exp. Med. 202, 1539–1547 (2005).
Silver, M.R. et al. IL-33 synergizes with IgE-dependent and IgE-independent agents to promote mast cell and basophil activation. Inflamm. Res. 59, 207–218 (2010).
Cherry, W.B., Yoon, J., Bartemes, K.R., Iijima, K. & Kita, H. A novel IL-1 family cytokine, IL-33, potently activates human eosinophils. J. Allergy Clin. Immunol. 121, 1484–1490 (2008).
Bortoluci, K.R. & Medzhitov, R. Control of infection by pyroptosis and autophagy: role of TLR and NLR. Cell. Mol. Life Sci. 67, 1643–1651 (2010).
Luthi, A.U. et al. Suppression of interleukin-33 bioactivity through proteolysis by apoptotic caspases. Immunity 31, 84–98 (2009).
Cayrol, C. & Girard, J.P. The IL-1-like cytokine IL-33 is inactivated after maturation by caspase-1. Proc. Natl. Acad. Sci. USA 106, 9021–9026 (2009).
Zhao, W. & Hu, Z. The enigmatic processing and secretion of interleukin-33. Cell. Mol. Immunol. 7, 260–262 (2010).
Baumgarth, N., Brown, L., Jackson, D. & Kelso, A. Novel features of the respiratory tract T-cell response to influenza virus infection: lung T cells increase expression of γ interferon mRNA in vivo and maintain high levels of mRNA expression for interleukin-5 (IL-5) and IL-10. J. Virol. 68, 7575–7581 (1994).
Acknowledgements
We thank M. Grusby (Harvard School of Public Health) for CD1d-deficient mice (backcrossed to the BALB/c strain) and Z. Luo for technical support. Supported by the US National Institutes of Health (R01 AI068085, R01 HL62348 and R01 051354).
Author information
Authors and Affiliations
Contributions
Y.-J.C. designed the study, did experiments, analyzed the data and wrote the manuscript; H.Y.K. did experiments and analyzed the data; L.A.A. did experiments; N.B. provided the H3N1 virus and did experiments. A.N.J.M., D.E.S. and R.H.D. provided reagents and ST2-deficient (Il1rl1−/−) and IL-13 deficient (Il13−/−) mice; and D.T.U. designed the study and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
D.E.S. is an employee and shareholder of Amgen.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–11 (PDF 4012 kb)
Rights and permissions
About this article
Cite this article
Chang, YJ., Kim, H., Albacker, L. et al. Innate lymphoid cells mediate influenza-induced airway hyper-reactivity independently of adaptive immunity. Nat Immunol 12, 631–638 (2011). https://doi.org/10.1038/ni.2045
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.2045
This article is cited by
-
Cullin5 drives experimental asthma exacerbations by modulating alveolar macrophage antiviral immunity
Nature Communications (2024)
-
Prediction of the number of asthma patients using environmental factors based on deep learning algorithms
Respiratory Research (2023)
-
The modulation of pulmonary group 2 innate lymphoid cell function in asthma: from inflammatory mediators to environmental and metabolic factors
Experimental & Molecular Medicine (2023)
-
Solar ultraviolet B radiation promotes α-MSH secretion to attenuate the function of ILC2s via the pituitary–lung axis
Nature Communications (2023)
-
Interferons as negative regulators of ILC2s in allergic lung inflammation and respiratory viral infections
Journal of Molecular Medicine (2023)