Abstract
All clinicians face the challenge of practicing evidence-based medicine and are confronted with data from a variety of studies, ranging from prospective randomized and registry studies to retrospective analyses. Unfortunately, the data frequently provide conflicting recommendations. How then should one interpret the information so that study findings can be applied directly in patient care? To evaluate the relevance of the abundance of studies published and how they apply to an individual patient, physicians must understand subtle nuances of study design and their effect on the interpretation of the results. In this Review, we examine the strengths and weaknesses of different study designs with the aim of providing the reader with a greater understanding how best to apply study results in the clinical setting.
Key Points
-
The practice of 'evidence-based medicine' is challenging, as the results of randomized and observational studies can seem conflicting
-
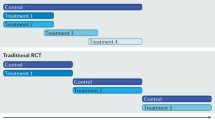
Randomization distributes both known and unknown confounders between treatment groups such that at baseline the groups will differ only by chance, while observational studies can be adjusted only for known confounders
-
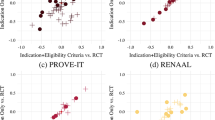
Strict inclusion and exclusion criteria mean that the results of randomized studies might not be as applicable to general populations as are findings from observational studies, including both clinical registries and retrospective reviews
-
In the clinical application of the results of any study to the treatment of an individual patient, the clinician must be cognizant of statistical power and the subtle implications of combined end points and surrogate outcomes
-
Peer review has a critical role in assuring the legitimacy of data presented and of conclusions stated in a manuscript, but cannot assure the validity of conclusions drawn by the reader or substitute for an informed analysis
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Pereira AC et al. (2006) Clinical judgment and treatment options in stable multivessel coronary artery disease: results from the one-year follow-up of the MASSII (Medicine, Angioplasty, or Surgery Study II). J Am Coll Cardiol 48: 948–953
King SB 3rd et al. for the Emory Angioplasty versus Surgery Trial Investigators (1997) Angioplasty or surgery for multivessel coronary artery disease: comparison of eligible registry and randomized patients in the EAST trial and influence of treatment selection on outcomes. Am J Cardiol 79: 1453–1459
Mercado N et al. (2005) One-year outcomes of coronary artery bypass graft surgery versus percutaneous coronary intervention with multiple stenting for multisystem disease: a meta-analysis of individual patient data from randomized clinical trials. J Thorac Cardiovasc Surg 130: 512–519
Jones RH et al. (1996) Long-term survival benefits of coronary artery bypass grafting and percutaneous transluminal angioplasty in patients with coronary artery disease. J Thorac Cardiovasc Surg 111: 1013–1025
Hannan EL et al. (2005) Long-term outcomes of coronary-artery bypass grafting versus stent implantation. N Engl J Med 352: 2174–2183
Steg PG et al. for the GRACE Investigators (2007) External validity of clinical trials in acute myocardial infarction. Arch Intern Med 167: 68–73
Detre KM et al. (1999) Coronary revascularization in diabetic patients: a comparison of the randomized and observational components of the Bypass Angioplasty Revascularization Investigation (BARI). Circulation 99: 633–640
Mack MJ et al. (2004) Comparison of coronary bypass surgery with and without cardiopulmonary bypass in patients with multivessel disease. J Thorac Cardiovasc Surg 127: 167–173
van Dijk D et al. for the Octopus Study Group (2007) Cognitive and cardiac outcomes 5 years after off-pump vs on-pump coronary artery bypass graft surgery. JAMA 297: 701–708
Berger PB et al. for the BARI investigators (2001) Survival following coronary angioplasty versus coronary artery bypass surgery in anatomic subsets in which coronary artery bypass surgery improves survival compared with medical therapy: results from the Bypass Angioplasty Revascularization Investigation (BARI). JACC 38: 1440–1449
Granger CB et al. for the COMMA Investigators (2003) Pexelizumab, an anti-C5 complement antibody, as adjunctive therapy to primary percutaneous coronary intervention in acute myocardial infarction: the COMplement inhibition in Myocardial infarction treated with Angioplasty (COMMA) trial. Circulation 108: 1184–1190
Armstrong PW et al. for the APEX AMI Investigators (2007) Pexelizumab for acute ST-elevation myocardial infarction in patients undergoing primary percutaneous coronary intervention: a randomized controlled trial. JAMA 297: 43–51
Hammermeister K et al. (2000) Outcomes 15 years after valve replacement with a mechanical versus a bioprosthetic valve: final report of the Veterans Affairs randomized trial. J Am Coll Cardiol 36: 1152–1158
Fleming TR and DeMets DL (1996) Surrogate end points in clinical trials: are we being misled? Ann Intern Med 125: 605–613
Connolly SJ (2006) Use and misuse of surrogate outcomes in arrhythmia trials. Circulation 113: 764–766
Cleland JG et al. (2006) Longer-term effects of cardiac resynchronization therapy on mortality in heart failure [the CArdiac REsynchronization-Heart Failure (CARE-HF) trial extension phase]. Eur Heart J 27: 1928–1932
Bigger JT Jr (1985) Patients with malignant or potentially malignant ventricular arrhythmias: opportunities and limitations of drug therapy in prevention of sudden death. J Am Coll Cardiol 5 (Suppl 6): 23B–26B
CAST investigators (1989) The cardiac arrhythmia suppression trial. N Engl J Med 321: 1754–1756
Kastrati A et al. (2007) Analysis of 14 trials comparing sirolimus-eluting stents with bare-metal stents. N Engl J Med. 356: 1030–1039
Montori VM et al. (2005) How should clinicians interpret results reflecting the effect of an intervention on composite endpoints: should I dump this lump? ACP J Club 143: A8
Freemantle N et al. (2003) Composite outcomes in randomized trials: greater precision but with greater uncertainty? JAMA 289: 2554–2559
Stone GW et al. for the TAXUS-IV Investigators (2004) One-year clinical results with the slow-release, polymer-based, paclitaxel-eluting TAXUS stent: the TAXUS-IV trial. Circulation 109: 1942–1947
The ISIS-2 Investigators for the ISIS-2 (Second International Study of Infarct Survival) Collaborative Group (1988) Randomized trial of intravenous streptokinase, oral aspirin, both, or neither among 17,187 cases of suspected acute myocardial infarction: ISIS-2. Lancet 2: 349–360
Benos DJ et al. (2003) How to review a paper. Advan Physiol Edu 27: 47–52
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Brown, M., Gersh, B., Holmes, D. et al. From randomized trials to registry studies: translating data into clinical information. Nat Rev Cardiol 5, 613–620 (2008). https://doi.org/10.1038/ncpcardio1307
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncpcardio1307
This article is cited by
-
The role of early-phase trials and real-world evidence in drug development
Nature Cardiovascular Research (2024)
-
Revascularization in stable coronary disease: evidence and uncertainties
Nature Reviews Cardiology (2018)
-
Akademische Gefäßchirurgie in Deutschland – eine (selbst-)kritische Bestandsaufnahme
Gefässchirurgie (2015)
-
Determining the prevalence and predictors of sleep disordered breathing in patients with chronic heart failure: rationale and design of the SCHLA-HF registry
BMC Cardiovascular Disorders (2014)