Abstract
Deleterious responses to pathogens during infancy may contribute to infection and associated asthma. Chlamydia respiratory infections in early life are common causes of pneumonia and lead to reduced lung function and asthma. We investigated the role of interleukin-13 (IL-13) in promoting early-life Chlamydia respiratory infection, infection-induced airway hyperresponsiveness (AHR), and severe allergic airway disease (AAD). Infected infant Il13−/− mice had reduced infection, inflammation, and mucus-secreting cell hyperplasia. Surprisingly, infection of wild-type (WT) mice did not increase IL-13 production but reduced IL-13Rα2 decoy receptor levels compared with sham-inoculated controls. Infection of WT but not Il13−/− mice induced persistent AHR. Infection and associated pathology were restored in infected Il13−/− mice by reconstitution with IL-13. Stat6−/− mice were also largely protected. Neutralization of IL-13 during infection prevented subsequent infection-induced severe AAD. Thus, early-life Chlamydia respiratory infection reduces IL-13Rα2 production, which may enhance the effects of constitutive IL-13 and promote more severe infection, persistent AHR, and AAD.
Similar content being viewed by others
Introduction
Respiratory infections in early life with the intracellular bacterium Chlamydia are common and up to 50% of young adults have anti-Chlamydia pneumoniae antibodies, indicating the prevalence of these infections in the community.1, 2 These infections are often asymptomatic but are a significant cause of community-acquired pneumonia especially in infants,3 and infection in childhood promotes long-term reductions in lung function.4 In adults, Chlamydia infections typically induce potent and protective T helper cell type 1 (Th1), interleukin (IL)-12, and interferon-γ-dominated responses and antibody responses.5, 6 These responses effectively clear the bacteria, but the strong inflammatory responses can damage the airways and parenchyma, leading to pathology and the development of pneumonia. In early life, the factors induced by infection and that are involved in clearance are less well understood although Th1 responses are known to be important.7, 8
There is a substantial body of evidence that links Chlamydia lung infections in early life with the development of wheezing and asthma.6, 9 This bacterium has been detected in the bronchoalveolar lavage (BAL) fluid of up to 46% of pediatric patients with asthma.10, 11 However, the mechanisms of how these Th1-inducing infections are associated with Th2-mediated asthma remain unknown. The age of infection may be critical as the Th2 bias of early life12 may promote susceptibility to intracellular infections.
Asthma is a chronic inflammatory condition of the airways that is commonest in children and is underpinned by aberrant Th2-mediated inflammatory responses to environmental antigens. The hallmark features of allergic asthma are induced by effector functions of the Th2 cytokines IL-4, IL-5, and IL-13.13 The aberrant inflammatory responses that underpin the development of asthma indicate that altered immune programming in early life that is induced by specific infections (e.g. Chlamydia, respiratory syncytial virus and rhinovirus) may have a critical role in the induction and progression of disease.6, 12, 14 However, the mechanisms involved remain poorly understood.
IL-13 is a key regulator of asthma pathogenesis and can induce many of the features of disease. This cytokine signals through the IL-4Rα/IL-13Rα1 receptor and signal transducer and activator of transcription 6 (STAT6) to promote inflammation, mucus-secreting cell (MSC) metaplasia/hyperplasia, and airway hyperresponsiveness (AHR).15, 16, 17 AHR is a heightened contractile response to non-specific stimuli and leads to excessive broncho-constriction, wheezing, and breathing difficulties. IL-13-mediated responses are modulated by the activity of its decoy receptor (IL-13Rα2),18 which inhibits IL-13-induced AHR and MSC metaplasia.19, 20, 21, 22 IL-13 also promotes the expression of genes associated with an alternatively activated macrophage (AAM) phenotype, including arginase-1 (Arg-1), chitinase-3-like protein 3 (Chi3l3/Ym-1), and found in inflammatory zone 1 (FIZZ-1).23, 24, 25
Studies in our laboratory have shown that early-life Chlamydia respiratory infections in mice, with the natural mouse pathogen Chlamydia muridarum, reduces lung function in the long term by promoting the development of AHR that persists into adulthood.26, 27 Infection also increased the severity of allergic airway disease (AAD) in later life.26, 27 These observations have been confirmed by others.28 Infection in early life also leads to increased production of IL-13 during AAD in adult mice.27 We have also shown in adult mice that C. muridarum respiratory infection leads to enhanced IL-13 production and that this cytokine increases susceptibility to Chlamydia respiratory and genital tract infections.29 Furthermore, infection of bone marrow–derived dendritic cells (BMDC) induces DCs and T cells to produce increased IL-13 in vitro, and adoptive transfer of Chlamydia-infected BMDC induced AHR and increased IL-13 production in vivo.30 Nevertheless, the role of IL-13 in Chlamydia respiratory infection in early life and the development of persistent AHR and enhanced AAD in later life is unknown.
In this study, we demonstrate for the first time that an early-life Chlamydia respiratory infection suppresses the levels of IL-13Rα2, which enhances the effects of constitutively produced IL-13. This promotes a more severe infection, which drives the development of persistent AHR, and increases the severity of AAD in later life.
Results
The absence of IL-13 reduces Chlamydia respiratory infection in early life and associated histopathology, mucus hypersecretion and inflammation
To investigate the influence of IL-13 on the course of Chlamydia respiratory infection in infancy, 3-week-old wild-type (WT) and Il13−/− mice were infected intranasally (IN) with C. muridarum and Chlamydia load in whole lungs was assessed 5, 10, 15, and 20 days post infection (dpi; Figure 1a). In WT mice, there was a significant increase in Chlamydia load at 5 dpi, infection peaked at 10 dpi, then there was a significant decrease at 15 dpi, before clearance of the infection at 20 dpi. In Il13−/− mice, infection was detectable by 5 dpi but there was no change in load between 5 and 10 dpi, and there was a significant reduction between 10 and 15 dpi. Infection was cleared in Il13−/− mice by 20 dpi. Importantly, Il13−/− had significantly reduced Chlamydia load at 5, 10, and 15 dpi compared with infected WT controls.
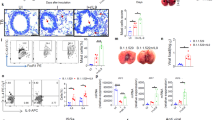
The absence of IL-13 reduces Chlamydia respiratory infection in early life and infection-induced histopathology. Infant (3-week-old) wild-type (WT) and Il13−/− BALB/c mice were infected with C. muridarum or sham-inoculated and killed 5, 10, 15 and 20 dpi (days post infection). (a) Chlamydia load in lung homogenates quantified by quantitative PCR. (b) Histopathological score of lung tissue sections. (c) Number of mucus-secreting cells (MSCs) per 100 μm basement membrane (BM). Results are presented as means±s.e.m. (sham groups n⩾4, infected groups n⩾8). * and+ represents P<0.05 between different time points in infected groups (a) or compared with sham-inoculated WT and Il13−/− mice, respectively (b, c). #P<0.05 compared with infected WT control. ifu, inclusion-forming units.
As Chlamydia load was decreased in Il13−/− mice, we next assessed the role of IL-13 in infection-induced histopathology. As we have previously described pulmonary inflammation is the major determinant of histopathological score.26 Infection of WT mice resulted in increases in histopathology and MSC numbers 10, 15 and 20 dpi (Figure 1b,c) compared with sham-inoculated WT controls. There was also a significant increase in histopathology in infected Il13−/− mice 5 dpi but not at 10, 15, or 20 dpi compared with sham-inoculated Il13−/− controls. Infected Il13−/− mice had significantly reduced histopathology compared with infected WT (C. muridarum WT) controls at 10, 15, and 20 dpi. Infection of Il13−/− did not induce the development of MSCs at any time point. There were no major differences between these or any other parameters between sham-inoculated WT and Il13−/− controls.
Given that infected Il13−/− mice had a marked reduction in pulmonary inflammation assessed by histopathology, we next examined whether there were any differences in the influx of specific types of inflammatory cells into the lung at the known peaks of infection and inflammation26 (Figure 2a–g). Infection of WT mice increased the numbers of macrophages, neutrophils, dendritic cells, and T cells in lung homogenates 10 and 15 dpi compared with sham-inoculated WT controls. Infection of Il13−/− mice resulted in increased numbers of macrophages, neutrophils, dendritic cells, and T cells at 10 but not 15 dpi compared with sham-inoculated Il13−/− controls. Infected Il13−/− mice had reduced numbers of all inflammatory cells (except CD4+ T cells) 10 and 15 dpi compared with infected WT controls.
The absence of interleukin-13 (IL-13) reduces Chlamydia respiratory infection-induced pulmonary inflammation. Infant (3-week-old) wild-type (WT) and Il13−/− BALB/c mice were infected with C. muridarum or sham-inoculated and killed at 10 and 15 dpi (days post infection). Numbers of inflammatory cells in lung homogenates were assessed by flow cytometry. (a) CD11c+ macrophages. (b) CD11b+ macrophages. (c) Neutrophils. (d) Plasmacytoid dendritic cells (pDCs). (e) Myeloid dendritic cells (mDCs). (f) CD4+ T cells. (g) CD8+ T cells. Results are presented as means±s.e.m. (n⩾6). *and + represent P⩽0.05 compared with sham-inoculated WT and Il13−/− controls, respectively. #P⩽0.05 compared with infected WT controls.
Chlamydia respiratory infection in early life does not increase IL-13 levels
As infected Il13−/− mice had significantly reduced Chlamydia load, histopathology, and inflammation following C. muridarum infection, the effect of infection on IL-13 levels in WT mice were assessed (Figure 3a,b). Surprisingly, IL-13 mRNA expression and protein levels in whole-lung homogenates did not increase at any time point throughout the course of infection compared with sham-inoculated WT controls. Infection also did not induce an early IL-13 response in the lung, with no increases in IL-13 mRNA or protein levels observed at 1 or 3 dpi (Figure 3c,d).
Chlamydia respiratory infection in early life does not increase interleukin-13 (IL-13) levels. Infant (3-week-old) wild-type (WT) BALB/c mice were infected with C. muridarum or sham-inoculated and killed 1, 3, 5, 10, 15, and 20 dpi (days post infection). Total RNA and protein were extracted from lung homogenates and mRNA expression and protein production were assessed by real time PCR and enzyme-linked immunosorbent assay, respectively. (a) IL-13 mRNA expression in lung homogenates 5, 10, 15, and 20 dpi. (b) IL-13 protein per mg of lung protein 5, 10, 15, and 20 dpi. (c) Early IL-13 mRNA expression in lung homogenates at 1 and 3 dpi. (d) Early IL-13 protein production per mg of lung tissue. Results are presented as means±s.e.m. (n⩾6). *P⩽0.05 compared with sham-inoculated control.
To investigate whether Chlamydia-specific IL-13-producing cells were present at the peak of infection and inflammation, lung, mediastinal lymph node, and spleen cells were re-stimulated with the Chlamydia major outer membrane protein (MOMP) and culture supernatants were assayed for IL-13. No MOMP-specific IL-13 was detected in any of the culture supernatants (data not shown).
Chlamydia respiratory infection in early life reduces IL-13 decoy receptor production
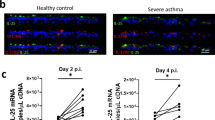
As infection had no effect on IL-13 mRNA or protein levels, the effect of infection on IL-13 receptor levels was assessed. There were no changes in IL-4Rα or IL-13Rα1 mRNA expression in lung homogenates at any time point (5, 10, 15, or 20 dpi) compared with sham-inoculated (Sham WT) controls (Figure 4a,b). By contrast and interestingly, soluble IL-13Rα2 mRNA expression level was decreased at 15 dpi, but not at 5, 10, or 20 dpi (Figure 4c). Importantly, the levels of IL-13Rα2 protein in lung homogenates were also significantly decreased at 15 dpi (but not at 5, 10, or 20 dpi, Figure 4d). There was also a concomitant suppression of soluble IL-13Rα2 protein levels in BAL supernatants and serum at 15 dpi (Figure 4e,f). Furthermore, there was less IL-13 bound to soluble IL-13Rα2 in BAL supernatants at this time point (Figure 4g), although there was no change in these levels in lung homogenates (Figure 4h).
Chlamydia respiratory infection in early life reduces interleukin-13 (IL-13) decoy receptor production. Infant (3-week-old) wild-type (WT) BALB/c mice were infected with C. muridarum or sham inoculated. Total RNA and protein were extracted from lung homogenates and IL-4Rα and IL-13Rα1 mRNA expression assessed by quantitative PCR, and IL-13Rα2 was assessed by enzyme-linked immunosorbent assay (ELISA). Receptor levels in bronchoalveolar lavage (BAL) and serum were determined by ELISA. (a) IL-4Rα mRNA in lung homogenates. (b) IL-13Rα1 mRNA in lung homogenates. (c) sIL-13 Rα2 mRNA in lung homogenates. (d) IL-13Rα2 protein in lung homogenates. (e) IL-13Rα2 protein in BAL 15 dpi (days post infection). (f) IL-13Rα2 protein in serum at 15 dpi. (g) IL-13-bound IL-13Rα2 in BAL at 15 dpi. (h) IL-13-bound IL-13Rα2 in lung homogenates. Results are presented as means±s.e.m. (n⩾6). *P⩽0.05 compared with sham-inoculated control.
IL-13 promotes the expression of AAM genes in the lung during Chlamydia respiratory infection
IL-13 drives the development of AAMs, which contribute to the Th2 cytokine milieu and impair immune responses to intracellular pathogens.24, 25, 31 Thus, we investigated the impact of Chlamydia respiratory infection on the expression of genes associated with an AAM phenotype in the lung. Infection of infant WT mice had increased expression of inducible nitric oxide synthase (iNOS), Arg-1, Ym-1, and FIZZ-1 mRNA in lung homogenates during infection compared with sham-inoculated WT controls (Figure 5a–d). Because these factors were most highly upregulated at 10 dpi in WT mice, their expression was assessed at this time point in Il13−/− mice. Infection of Il13−/− mice also increased iNOS, Arg-1, Ym-1 and FIZZ-1, compared with sham-inoculated Il13−/− controls (Figure 5e–h). However, infected Il13−/− mice had significantly reduced iNOS, Arg-1, and FIZZ-1 (but not Ym-1) mRNA expression compared with infected WT controls. Analysis of BAL macrophages at 10 dpi also showed that infection of WT and Il13−/− mice increased iNOS and Arg-1 but not Ym-1 mRNA expression. Expression of iNOS and Ym-1 but not Arg-1 were significantly reduced in Il13−/− macrophages (Figure 5i–k). There was no significant change in FIZZ-1 expression in any group (Figure 5l).
Interleukin-13 (IL-13) promotes the expression of alternatively activated macrophage genes in the lung following Chlamydia respiratory infection in early life. Infant (3-week-old) wild-type (WT) and Il13−/− BALB/c mice were infected with C. muridarum or sham-inoculated. Total RNA was extracted from lung homogenates or bronchoalveolar lavage (BAL) macrophages and mRNA expression assessed by quantitative PCR. (a) iNOS, (b) Arg-1, (c) Ym-1, and (d) FIZZ-1 in lung homogenates of WT mice at 5, 10, 15, and 20 dpi (days post infection). (e) iNOS, (f) Arg-1, (g) Ym-1, and (h) FIZZ-1 in lung homogenates of WT and Il13−/− mice at 10 dpi. (i) iNOS, (j) Arg-1, (k) Ym-1, and (l) FIZZ-1 in BAL macrophages of WT and Il13−/− mice at 10 dpi. Results are presented as means±s.e.m. (n⩾6 for lung homogenates, n=2 replicates of four pooled samples for BAL macrophages). *and +represent P⩽0.05 compared with sham-inoculated WT and Il13−/− controls, respectively. #P⩽0.05 compared with infected WT control.
Early-life Chlamydia respiratory infection-induced persistent AHR is IL-13-dependent
We have previously shown that early-life Chlamydia respiratory infection in mice induces the development of AHR that persists into later life.26, 27 To determine the role of IL-13 in promoting infection-induced AHR, infant WT and Il13−/− mice were infected and AHR was assessed at 61 dpi. As shown previously,27 infection of WT mice induced AHR by significantly increasing transpulmonary (Figure 6a) resistance and decreasing dynamic compliance (Figure 6b) compared with sham-inoculated WT controls. By contrast, infection of Il13−/− mice did not induce AHR, with no change in resistance or compliance, compared with sham-inoculated WT or Il13−/− controls.
Early-life Chlamydia respiratory infection–induced persistent airway hyperresponsiveness is interleukin-13 (IL-13)-dependent. Infant (3-week-old) wild-type (WT) and Il13−/− BALB/c mice were infected with C. muridarum or sham inoculated and lung function was assessed at 61 days post infection. (a) Transpulmonary resistance. (b) Dynamic compliance. Results are presented as means±s.e.m. (n⩾8). *P⩽0.05 compared with sham-inoculated WT control. #P⩽0.05 compared with infected WT control.
Administration of recombinant IL-13 to Il13−/− mice during Chlamydia respiratory infection in early life increases infection, and infection-induced histopathology, mucus hypersecretion, and persistent AHR
Given that IL-13 was not increased during infection in WT mice but that Il13−/− mice had reduced infection and infection-induced pathology, we next administered IL-13 during infection of infant Il13−/− mice to determine whether the phenotype could be rescued (Figure 7a–f). Administration of rIL-13 to sham-inoculated WT or Il13−/− mice did not induce inflammation or increases in MSCs or expression of AAM genes at 10 dpi or AHR at 61 dpi, indicating that only constitutive levels of IL-13 were reconstituted. However, administration of rIL-13 to infected Il13−/− mice increased infection, histopathology, mucus hypersecretion, AAM gene expression, and AHR compared with infected WT controls that were treated with sterile phosphate-buffered saline.
Administration of recombinant interleukin-13 (IL-13) to Il13−/− mice during Chlamydia infection in early life increases infection, and infection-induced histopathology, mucus hypersecretion and persistent airway hyperresponsiveness. Infant (3-week-old) wild-type (WT) and Il13−/− BALB/c mice were infected with C. muridarum or sham inoculated and treated with 10 ng rIL-13 in 30 μl sterile phosphate-buffered saline (PBS). (a) Chlamydia load at 10 dpi (days post infection). (b) Histopathological score at 10 dpi. (c) Number of mucus-secreting cells (MSCs) per 100 μm basement membrane (BM) at 10 dpi. (d) inducible nitric oxide synthase (iNOS), Arg-1, Ym-1, and FIZZ-1 mRNA expression in lung homogenates at 10 dpi. (e) Transpulmonary resistance at 61 dpi. (f) Dynamic compliance at 61 dpi. Results are presented as means±s.e.m. (n⩾4 for sham controls and n⩾8 for infected groups). * and +represents P⩽0.05 compared with sham-inoculated WT and Il13−/− controls, respectively. ifu, inclusion-forming units.
IL-13-mediated effects during Chlamydia respiratory infection in early life are both STAT6-dependent and -independent
IL-13 mediates its effects largely by signaling through STAT6.16, 17 To investigate the involvement of STAT6 in IL-13-mediated effects during Chlamydia respiratory infection, Stat6−/− mice were infected, and infection, histopathology, MSCs, AAM gene expression, and AHR were assessed. In Stat6−/− mice infection was detectable by 5 dpi but there was no difference in Chlamydia load between 5, 10, and 15 dpi (Figure 8a). Infected Stat6−/− mice had significantly lower Chlamydia load at 10 dpi, but not at 5 or 15 dpi, compared with infected WT controls.
Interleukin-13 (IL-13)-mediated effects during Chlamydia respiratory infection in early life are both STAT6-dependent and -independent. Infant (3-week-old) wild-type (WT) and Stat-6−/− BALB/c mice were infected with C. muridarum or sham-inoculated. (a) Chlamydia load. (b) Histopathological score. (c) Number of mucus-secreting cells (MSCs) per 100μm basement membrane (BM). (d) iNOS, Arg-1, Ym-1, and FIZZ-1 mRNA expression in lung homogenates 10 dpi (days post infection). (e) Transpulmonary resistance 61 dpi. (f) Dynamic compliance 61 dpi. Results are presented as means±s.e.m. (n⩾4 for sham controls and n⩾8 for the infected groups). WT data (Figure 8a–c) is recapitulated from Figure 1. * and + represents P⩽0.05 compared with sham-inoculated WT and Stat-6−/− controls, respectively. #P⩽0.05 compared with infected WT control. ifu, inclusion-forming units.
Infected Stat6−/− mice had increased histopathological score at 5 and 15 dpi, but not at 10 dpi, compared with sham-inoculated Stat6−/− controls (Figure 8b). In stark contrast to Il13−/− mice, Stat6−/− mice were not protected against infection-induced increases in MSCs, as infected Stat6−/− mice had significantly elevated numbers of these cells 10 and 15 dpi compared with sham-inoculated Stat6−/− controls (Figure 8c). Furthermore, infected Stat6−/− mice did not have reduced histopathology or MSC numbers compared with infected WT controls. There was no change in these or other parameters between sham-inoculated WT and Stat6−/− controls.
Infected Stat6−/− mice had increased Arg-1 and FIZZ-1 but not iNOS or Ym-1 at 10 dpi compared with sham-inoculated Stat6−/− controls (Figure 8d). Similar to Il13−/− mice, infected Stat6−/− mice had decreased iNOS, Arg-1, and FIZZ-1 but not Ym-1 at 10 dpi compared with infected WT controls.
Similar to Il13−/− mice and in contrast to WT mice, infected Stat6−/− mice did not develop infection-induced AHR in later life. Infection did not change resistance or compliance compared with sham-inoculated WT or Stat6−/− controls (Figure 8e,f).
Inhibition of IL-13 during Chlamydia respiratory infection in early life prevents infection-induced increases in the severity of AAD in later life
We have previously shown that an early life but not adult Chlamydia respiratory infection increases the severity of AAD in later life, characterized by increased mucus hypersecretion and AHR.26, 27 In order to assess the effect of IL-13 during infection on subsequent AAD in later life, we administered neutralizing monoclonal antibodies against IL-13 only during the infection on 0, 7, and 14 dpi (Figure 9a). We then sensitized mice to ovalbumin (Ova) 45 dpi and challenged with Ova on days 57-60 dpi and assessed the hallmark features of AAD 24 h after the final Ova challenge. Inhibition of IL-13 during infection suppressed the development of more severe AAD by reducing the number of MSCs around the airways and by suppressing transpulmonary resistance compared with isotype-treated infected controls with AAD (Figure 9b,c).
Inhibition of interleukin-13 (IL-13) during Chlamydia respiratory infection in early life prevents infection-induced increases in the severity of allergic airway disease (AAD) in later life. Infant (3-week-old) wild-type (WT) BALB/c mice were infected with C. muridarum and (a) treated with anti-IL-13 or isotype control intraperitoneally (IP) every 7 days from day 0–14. Forty-five days after infection (dpi), mice were subjected to ovalbumin (Ova)-induced AAD and AAD was assessed at 61 dpi. (b) Numbers of mucus-secreting cells (MSCs) per 100 μM basement membrane (BM). (c) Transpulmonary resistance. Results are presented as means±s.e.m. (n⩾8). *P⩽0.05 compared with isotype-treated control. IN, intranasally.
Discussion
In this study, we show that Chlamydia respiratory infection in early life suppresses IL-13Rα2 levels, which enables constitutive IL-13 to promote infection and infection-induced AHR, and increases in the severity of AAD in later life.
This study used infection with the natural mouse respiratory pathogen C. muridarum, which develops a productive infection and induces similar immunological and pathological features in mice that are observed in Chlamydia respiratory infection in humans, including cytokine secretion, inflammatory cell infiltration, mucus hypersecretion, and altered lung function, as we have previously described.6, 27 Inoculation with 100 inclusion-forming units of C. muridarum is representative of a community-acquired infection, where a small number of bacteria may be transmitted via aerosols following a cough or sneeze.
In the absence of IL-13, less severe infection and infection-induced histopathology was observed, which were associated with decreases in the numbers of a range of inflammatory cells infiltrating the lung. Interestingly, early-life infection did not increase the expression of IL-13 or IL-4Rα/IL-13Rα1 but significantly decreased IL-13Rα2 levels, removing an important regulatory mechanism that controls IL-13 signaling. Infection of WT mice resulted in the development of an AAM phenotype, which was reduced in Il13−/− mice. Early-life infection of WT mice induced the development of AHR that persisted into adulthood and was ablated in Il13−/− mice. Administration of IL-13 to Il13−/− mice during infection restored the phenotype observed in WT mice. The IL-13-mediated effects were both STAT6-dependent and -independent. Stat6−/− mice were protected against infection, infection-induced expression of AAM genes, and persistent AHR. However, Stat6−/− mice still had substantial histopathology and, surprisingly, were not protected against infection-induced increases in MSCs. Finally, neutralization of IL-13 during early-life infection prevented the development of AHR and more severe AAD in later life.
We have previously shown that IL-13 promotes susceptibility to Chlamydia respiratory and genital tract infections in adult BALB/c mice.29 In that study, IL-13 was rapidly produced following infection in WT mice, and Il13−/− mice had less severe infection and fewer inflammatory cells in the BAL than infected WT controls.29 Furthermore, depletion of CD4+ T cells in Il13−/− mice did not affect infection, suggesting a role for IL-13 from innate cells rather than CD4+ Th2 cells.29 The absence of IL-13 increased macrophage uptake of Chlamydia in vitro and in vivo, and depletion of IL-13 during infection of lung epithelial cells in vitro decreased the percentage of infected cells.29 Similar to an adult infection, the absence of IL-13 during an early-life Chlamydia infection resulted in less severe infection, pulmonary inflammation, and mucus hypersecretion.
In contrast to an adult infection, Chlamydia respiratory infection in early life did not affect the expression of IL-13 but, instead, suppressed the levels of IL-13Rα2, which allowed constitutive IL-13 to induce greater effects. IL-13Rα2 is a high affinity IL-13 receptor, which preferentially binds IL-13 to prevent signaling through the IL-4Rα/IL-13Rα1 receptor complex and activation of STAT6, which would normally lead to inflammation and MSC hyperplasia.19, 20, 21, 22, 32 We showed that the total levels of IL-13Rα2 were decreased in lung homogenates of Chlamydia-infected mice, which is representative of membrane-bound and intracellular IL-13Rα2 in the lung and is likely to be important in humans. We also demonstrated that Chlamydia respiratory infection decreased the amount of soluble IL-13Rα2 in both the BAL and serum. Soluble IL-13Rα2 has not been detected in plasma, serum, or BAL of human asthmatics and healthy controls.33, 34 Nevertheless, and most importantly, Chen et al.,34 recognize that soluble IL-13Rα2 is likely to be an important regulator of IL-13 activity in lung tissues of humans. They suggest that cell surface IL-13Rα2 may be enzymatically cleaved from the cell surface to generate the soluble form. Intriguingly, the enzymatic activity of house-dust mite allergens is capable of releasing cell surface–bound murine IL-13Rα2, but this has not yet been shown for the human receptor. This may also potentially occur during bacterial (e.g. Chlamydia) infection. Moreover, membrane-bound IL-13Rα2 in the human lungs (or cells such as macrophages and fibroblasts33) may be cleaved by matrix metalloproteinases (MMPs)/MMP-8 causing the release of membrane-bound IL-13Rα2, which may act as a soluble form of IL-13Rα2. Therefore, the presence and activity of soluble IL-13Rα2 in the human lung is still likely to be important during infection and infection-associated asthma.
IL-13 is known to drive the formation of AAMs through STAT6-dependent signaling pathways, which can have deleterious effects on the clearance of intracellular pathogens and promote Th2-mediated immune responses.23, 24, 25 AAMs express high levels of Arg-1 and low levels of iNOS, which suppresses effective immunity against intracellular pathogens31 and prevents bacterial growth by increasing the production of nitric oxide, respectively.35, 36 Several other genes, including Ym-1 and FIZZ-1, have been associated with the AAM phenotype.23, 24, 25 In this study, we show for the first time that Chlamydia respiratory infection induces the expression of iNOS, Arg-1, Ym-1, and FIZZ-1 in the lung, which were suppressed (excluding Ym-1) in Il13−/− mice. Surprisingly, iNOS expression was decreased in Il13−/− mice. This may be explained by the reduction in Chlamydia load and consequently the lower number of macrophages infiltrating the lungs at 10 dpi. Chlamydia is known to be able to infect immune cells5 and the development of an AAM phenotype may be a result of the infection of macrophages, which occurs to a greater extent in the presence of IL-13.29
We have previously shown that an early life, but not adult, Chlamydia respiratory infection induces the development of persistent AHR, even in the absence of allergen challenge,26, 27 which has been confirmed by others.28 Here, we identify the mechanisms that may be involved. We discovered that constitutive IL-13, which is present during the early-life infection, drives the development of AHR. This is also the first study to demonstrate that an early-life infection can suppress IL-13Rα2 production, leading to the removal of an important immunomodulatory mechanism that controls IL-13 signaling.
STAT6 is downstream of IL-13 and has been shown to facilitate IL-13-induced effects, including inflammation, MSC metaplasia, AAM gene expression, and AHR.16, 17 No study to date has shown a role for STAT6 in Chlamydia infection or infection-induced pathology. Chlamydia load, infection-induced AAM gene expression, and AHR were significantly suppressed in the absence of STAT6. However, somewhat surprisingly, Stat6−/− mice were not protected against infection-induced inflammation and MSC metaplasia, suggesting that these effects were induced by an IL-13-mediated STAT6-independent pathway.
We have previously shown that Chlamydia respiratory infection in early life increases the severity of AAD in later life, by enhancing MSC hyperplasia and AHR.27 In this study, we demonstrate that neutralization of IL-13 during early-life infection prevented infection-enhanced MSC hyperplasia and AHR during Ova-induced AAD in later life. The role of IL-13 in early life may be further assessed using studies involving administration of rIL-13. However, in our study, we did not observe any infection-induced increase in IL-13 levels in early life. Thus, rIL-13 treatment would not mirror the effects of infection. Administration of rIL-13 to Il13−/− mice during infancy and subsequent assessment of AAD in later life is not possible as IL-13 is required for the induction of AAD.13 Several other early-life infections, including rhinovirus (RV1B), influenza (H1N1), and respiratory syncytial virus have been shown to increase the severity of AAD in later life.37, 38, 39 Inhibition of IL-13 during primary respiratory syncytial virus infection has also been shown to inhibit the exacerbation of AHR in adult mice.38 However, our study is the first to identify that targeting constitutive IL-13 during an infection in early life may suppress infection and subsequent AAD. Anti-IL-13 is already in clinical trials for asthma in adults. Our study therefore indicates that anti-IL-13 therapies may have therapeutic benefit in early-life infections and in preventing infection-induced asthma in humans.
In summary, this study demonstrates that IL-13Rα2 controls constitutive IL-13 signaling in Chlamydia respiratory infection in early life to prevent the development of infection, inflammation, and histopathology as well as subsequent infection-induced AHR and increased severity of AAD. We demonstrate that an infection can decrease IL-13Rα2 levels and that constitutive IL-13 signaling through STAT6 is pivotal in promoting Chlamydia respiratory infection and its downstream consequences. Our study identifies IL-13 and STAT6 during Chlamydia respiratory infection in early life as potential novel therapeutic targets for preventing infection-induced AHR and increased asthma severity in later life.
Methods
Ethics statement. This study was performed in strict accordance with the recommendations in the Australian code of practise for the care and use of animals for scientific purposes issued by the National Health and Medical Research Council of Australia. All protocols were approved by the Animal Ethics Committee of the University of Newcastle.
C. muridarum respiratory infection. Infant (3-week-old) WT, Il13−/− or Stat6−/− BALB/c mice were infected IN with the natural mouse pathogen C. muridarum (100 inclusion-forming units, ATCC VR-123, in 30 μl sucrose phosphate glutamate buffer.27 Controls were sham inoculated with 30 μl sucrose phosphate glutamate IN. Mice were killed at 1, 3, 5, 10, 15, 20, or 61 dpi to assess infection and pathology.
Infection. Total RNA, DNA, and protein was isolated from lung homogenates using SurePrep RNA/DNA/Protein Purification kits (Fisher Bioreagents, Scorsby, Australia). Chlamydia numbers were determined by real-time quantitative PCR as previously described.27, 29, 40
Histopathology. Formalin-fixed, lung sections were stained with hematoxylin and eosin (for histopathology) and periodic acid–schiff (for MSCs). Histopathology and MSC numbers were quantified as previously described.26, 41
Flow cytometry. Single-cell suspensions of collagenase-D-digested lungs were stained for the surface markers CD3, CD4, CD8, F4/80, CD11c, CD11b, Gr-1, and PDCA (Biolegend, Karrinyup, Australia) and fixed with 4% paraformaldehyde as previously described.40, 42, 43 Cell populations (Table 1) were analyzed using a FACSCanto with FACSDiva software (BD Biosciences, North Ryde, Australia).
mRNA expression. Total RNA was isolated from lung homogenates using the SurePrep RNA/DNA/Protein Purification kit (Fisher Bioreagents) and from BAL cells using the Purelink RNA extraction kit (Invitrogen, Mount Waverly, Australia) according to the manufacturers’ instructions. Extracted RNA was treated with DNAseI (Sigma, Castle Hill, Australia) and reverse-transcribed using Bioscript (Bioline, Alexandria, Australia) and random hexamer primers (Invitrogen). Relative abundance of cDNA was determined compared with the reference gene hypoxanthine-guanine phosphoribosyltransferase by real-time PCR using an Eppindorf RealPlex 2 System (Eppindorf, North Ryde, Australia). IL-13 mRNA expression was determined as previously described.27 Custom-designed primers (IDT, Coralville, IA) were used for HPRT (hypoxanthine-guanine phosphoribosyltransferase; For: 5′-AGGCCAGACTTTGTTGGATTTGAA; Rev: 5′-CAACTTGCGCTCATCTTAGGCTTT), iNOS (For: 5′-AGCGAGGAGCAGGTGGAAGACT; Rev: 5′-TTCGGTGCAGTCTTTTCCTATGG), Arg-1 (For: 5′-GGCAGAGGTCCAGAAGAATG; Rev: 5′-CATTTGGGTGGATGCTCAC), Ym-1 (For: 5′-CCCCAGGAAGTACCCTATGCCT; Rev: 5′-AACCACTGAAGTCATCCATGTCC), FIZZ1 (For: 5′-TACTTGCAACTGCCTGTGCTTACT; Rev: 5′-TATCAAAGCTGGGTTCTCCACCTC), IL-4Rα (For: 5′-GGGCTGTCTGATTTTGCTGT; Rev: 5′-TGGAAGTGCGGATGTAGTCA), IL-13Rα1 (For: 5′ CACAGTCAGAGTAAGAGTCAAAACA; Rev: 5′-ATGGTGGTGTAGAAGGTGGA), and IL-13Rα2 (For: 5′ AGGAATGTTGGGAAGAGCCTCCA; Rev: 5′ ACT CCT GCT GGC TGG CTC TAT GT).
Enzyme-linked immunosorbent assay. Purified total protein from lung homogenates was quantified using BCA Protein Assay Kits (Pierce, Scorsby, Australia). The concentrations of IL-13, IL-13Rα2, and IL-13-bound IL-13Rα2 in lung homogenates, IL-13Rα2 and IL-13-bound IL-13Rα2 in BAL, and IL-13Rα2 in serum were determined by enzyme-linked immunosorbent assay (R&D systems, Gymea, Australia) as previously described.44 In some experiments, the lung, mediastinal lymph node or spleen cells (1 × 106)27 were isolated and restimulated with Chlamydia MOMP45 and cultured for 4 days in Gibco RPMI-1640 containing 10% fetal calf serum, 20 mmol l−1HEPES (4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid), 10 μg ml−1 penicillin/streptomycin, 2 mmol l−1 L-gluatamine, and 50 μmol/ l−1 2-mercaptoethanol. The concentration of IL-13 in culture supernatants was determined by enzyme-linked immunosorbent assay.
Lung function. Lung function, in terms of AHR, was measured in anesthetized mice using whole-body plethysmography by determination of the peak of transpulmonary resistance and dynamic compliance in response to increasing doses of nebulized methacholine (Sigma, Castle Hill, Australia) as previously described.26, 27, 46, 47, 48, 49, 50
In vivo administration of recombinant (r)IL-13. WT and Il13−/− mice were treated with 10 ng murine rIL-13 in 30 μL sterile phosphate-buffered saline IN (R&D systems) and controls were sham treated with phosphate-buffered saline 0, 3, 6, 9, 12, and 15 dpi.29
In vivo neutralization of IL-13 and induction of AAD. Infected WT mice were treated with neutralizing anti-IL-13 monoclonal antibody or isotype control (20 μg g−1 body weight intraperitoneally, Janssen Research & Development, NJ) 0, 7, and 14 dpi as recommended by the supplier. AAD was then induced 45–61 dpi and assessed as previously described.26, 27, 46, 47, 48, 49, 50 Briefly, mice were sensitized to Ova by intraperitoneal injection (50 μg of Ova (Sigma, Castle Hill, Australia) and 1 mg of Rehydragel (Reheis, Berkeley Heights, NJ) in 200 μl of 0.9% sterile saline). Twelve days after sensitization mice were challenged IN with Ova (10 μg, 50 μl of phosphate-buffered saline, for 4 consecutive days). One day later, mice were killed by sodium pentobarbital overdose (Abbott Australasia, Kurnell, Australia) and features of AAD were characterized.
Statistics. Results are represented as the mean±s.e.m., which is representative of 2–3 independent experiments that used 2–4 mice each. Statistical significance for multiple comparisons was determined by one-way or two-way ANOVA with Bonferroni post-test, or non-parametric equivalent, where appropriate using GraphPad Prism Software version 5 (San Diego, CA).
References
Kuo, C.C., Jackson, L.A., Campbell, L.A. & Grayston, J.T. Chlamydia pneumoniae (TWAR). Clin. Microbiol. Rev. 8, 451–461 (1995).
Grayston, J.T. Chlamydia pneumoniae, strain TWAR pneumonia. Annu. Rev. Med. 43, 317–323 (1992).
Blasi, F. Atypical pathogens and respiratory tract infections. Eur. Respir. J. 24, 171–181 (2004).
Harrison, H.R, Taussig, L.M. & Fulginiti, V.A. Chlamydia trachomatis and chronic respiratory disease in childhood. Pediatr. Infect. Dis. 1, 29–33 (1982).
Beagley, K.W., Huston, W.M., Hansbro, P.M. & Timms, P. Chlamydial infection of immune cells: altered function and implications for disease. Crit. Rev. Immunol. 29, 275–305 (2009).
Hansbro, P.M., Beagley, K.W., Horvat, J.C. & Gibson, P.G. Role of atypical bacterial infection of the lung in predisposition/protection of asthma. Pharmacol. Ther. 101, 193–210 (2004).
Jupelli, M. et al. Endogenous IFN-gamma production is induced and required for protective immunity against pulmonary chlamydial infection in neonatal mice. J. Immunol. 180, 4148–4155 (2008).
Jupelli, M. et al. The contribution of interleukin-12/interferon-gamma axis in protection against neonatal pulmonary Chlamydia muridarum challenge. J. Interferon Cytokine Res. 30, 407–415 (2010).
Zaitsu, M. Does Chlamydia pneumoniae infection trigger to development of asthma in wheezy infants? J. Asthma 46, 967–968 (2009).
Webley, W.C. et al. Occurrence of Chlamydia trachomatis and Chlamydia pneumoniae in paediatric respiratory infections. Eur. Respir. J. 33, 360–367 (2009).
Webley, W.C. et al. The bronchial lavage of pediatric patients with asthma contains infectious Chlamydia. Am. J. Respir. Crit. Care Med. 171, 1083–1088 (2005).
Hansbro, P.M., Starkey, M.R., Kim, R.Y., Foster, P.S. & Horvat, J.C. Programming of the lung by early life infection. J. Dev. Orig. Health Dis. 3, 153–158 (2012).
Hansbro, P.M., Kaiko, G.E. & Foster, P.S. Cytokine/anti-cytokine therapy-novel treatments for asthma? Br. J. Pharmacol. 163, 81–95 (2011).
Hansbro, N.G., Horvat, J.C., Wark, P.A. & Hansbro, P.M. Understanding the mechanisms of viral induced asthma: new therapeutic directions. Pharmacol. Ther. 117, 313–353 (2008).
Wills-Karp, M. et al. Interleukin-13: central mediator of allergic asthma. Science 282, 2258–2261 (1998).
Yang, M. et al. Interleukin-13 mediates airways hyperreactivity through the IL-4 receptor-alpha chain and STAT-6 independently of IL-5 and eotaxin. Am. J. Respir. Cell Mol. Biol. 25, 522–530 (2001).
Kuperman, D.A. et al. Direct effects of interleukin-13 on epithelial cells cause airway hyperreactivity and mucus overproduction in asthma. Nat. Med. 8, 885–889 (2002).
Tabata, Y. & Khurana Hershey, G.K. IL-13 receptor isoforms: breaking through the complexity. Curr. Allergy. Asthma Rep. 7, 338–345 (2007).
Grunig, G. et al. Requirement for IL-13 independently of IL-4 in experimental asthma. Science 282, 2261–2263 (1998).
Taube, C. et al. The role of IL-13 in established allergic airway disease. J. Immunol. 169, 6482–6489 (2002).
Wilson, M.S. et al. IL-13Ralpha2 and IL-10 coordinately suppress airway inflammation, airway-hyperreactivity, and fibrosis in mice. J. Clin. Invest. 117, 2941–2951 (2007).
Zheng, T. et al. IL-13 receptor alpha2 selectively inhibits IL-13-induced responses in the murine lung. J. Immunol. 180, 522–529 (2008).
Gordon, S. Alternative activation of macrophages. Nat. Rev. Immunol. 3, 23–35 (2003).
Martinez, F.O., Helming, L. & Gordon, S. Alternative activation of macrophages: an immunologic functional perspective. Annu. Rev. Immunol. 27, 451–483 (2009).
Murray, P.J. & Wynn, T.A. Protective and pathogenic functions of macrophage subsets. Nat. Rev. Immunol. 11, 723–737 (2011).
Horvat, J.C. et al. Neonatal chlamydial infection induces mixed T-cell responses that drive allergic airway disease. Am. J. Respir. Crit. Care Med. 176, 556–564 (2007).
Horvat, J.C. et al. Early-life chlamydial lung infection enhances allergic airways disease through age-dependent differences in immunopathology. J. Allergy Clin. Immunol. 125, 617–625 625 e611-625 e616 (2010).
Jupelli, M. et al. Neonatal chlamydial pneumonia induces altered respiratory structure and function lasting into adult life. Lab. Invest. 91, 1530–1539 (2011).
Asquith, K.L. et al. Interleukin-13 promotes susceptibility to chlamydial infection of the respiratory and genital tracts. PLoS Pathog. 7, e1001339 (2011).
Kaiko, G.E. et al. Chlamydia muridarum infection subverts dendritic cell function to promote Th2 immunity and airways hyperreactivity. J. Immunol. 180, 2225–2232 (2008).
El Kasmi, K.C. et al. Toll-like receptor-induced arginase 1 in macrophages thwarts effective immunity against intracellular pathogens. Nat. Immunol. 9, 1399–1406 (2008).
Donaldson, D.D. et al. The murine IL-13 receptor alpha 2: molecular cloning, characterization, and comparison with murine IL-13 receptor alpha 1. J. Immunol. 161, 2317–2324 (1998).
O'Toole, M., Legault, H., Ramsey, R., Wynn, T.A. & Kasaian, M.T. A novel and sensitive ELISA reveals that the soluble form of IL-13R-alpha2 is not expressed in plasma of healthy or asthmatic subjects. Clin. Exp. Allergy 38, 594–601 (2008).
Chen, W. et al. IL-13R alpha 2 membrane and soluble isoforms differ in humans and mice. J. Immunol. 183, 7870–7876 (2009).
MacMicking, J., Xie, Q.W. & Nathan, C. Nitric oxide and macrophage function. Annu. Rev. Immunol. 15, 323–350 (1997).
Igietseme, J.U. et al. Chlamydial infection in inducible nitric oxide synthase knockout mice. Infect. Immun. 66, 1282–1286 (1998).
Schneider, D. et al. Neonatal rhinovirus infection induces mucous metaplasia and airways hyperresponsiveness. J. Immunol. 188, 2894–2904 (2012).
Lukacs, N.W. et al. Respiratory syncytial virus predisposes mice to augmented allergic airway responses via IL-13-mediated mechanisms. J. Immunol. 167, 1060–1065 (2001).
You, D. et al. Exposure of neonates to respiratory syncytial virus is critical in determining subsequent airway response in adults. Respir. Res. 7, 107 (2006).
Horvat, J.C. et al. Chlamydial respiratory infection during allergen sensitization drives neutrophilic allergic airways disease. J. Immunol. 184, 4159–4169 (2010).
Preston, J.A. et al. Inhibition of allergic airways disease by immunomodulatory therapy with whole killed Streptococcus pneumoniae. Vaccine 25, 8154–8162 (2007).
Essilfie, A.T. et al. Combined Haemophilus influenzae respiratory infection and allergic airways disease drives chronic infection and features of neutrophilic asthma. Thorax 67, 588–599 (2012).
Beckett, E.L. et al. TLR2, but not TLR4, is required for effective host defence against Chlamydia respiratory tract infection in early life. PLoS One 7, e39460 (2012).
Chen, W. et al. Matrix metalloproteinase 8 contributes to solubilization of IL-13 receptor alpha2 in vivo. J. Allergy Clin. Immunol. 122, 625–632 (2008).
Berry, L.J. et al. Transcutaneous immunization with combined cholera toxin and CpG adjuvant protects against Chlamydia muridarum genital tract infection. Infect. Immun. 72, 1019–1028 (2004).
Essilfie, A.T. et al. Haemophilus influenzae infection drives IL-17-mediated neutrophilic allergic airways disease. PLoS Pathog. 7, e1002244 (2011).
Preston, J.A. et al. Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells. Eur. Respir. J. 37, 53–64 (2011).
Thorburn, A.N. et al. Components of Streptococcus pneumoniae suppress allergic airways disease and NKT cells by inducing regulatory T cells. J. Immunol. 188, 4611–4620 (2012).
Thorburn, A.N. et al. Pneumococcal conjugate vaccine-induced regulatory T cells suppress the development of allergic airways disease. Thorax 65, 1053–1060 (2010).
Starkey, M.R. et al. Chlamydia muridarum lung infection in infants alters hematopoietic cells to promote allergic airway disease in mice. PLoS One 7, e42588 (2012).
Acknowledgements
Funding: This work was supported by grants from the National Health and Medical Research Council of Australia and the Australian Research Council.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
Rights and permissions
About this article
Cite this article
Starkey, M., Essilfie, A., Horvat, J. et al. Constitutive production of IL-13 promotes early-life Chlamydia respiratory infection and allergic airway disease. Mucosal Immunol 6, 569–579 (2013). https://doi.org/10.1038/mi.2012.99
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2012.99
This article is cited by
-
Interferon-epsilon is a novel regulator of NK cell responses in the uterus
EMBO Molecular Medicine (2024)
-
Pulmonary group 2 innate lymphoid cells: surprises and challenges
Mucosal Immunology (2019)
-
Microbiome effects on immunity, health and disease in the lung
Clinical & Translational Immunology (2017)
-
A pathogenic role for tumor necrosis factor-related apoptosis-inducing ligand in chronic obstructive pulmonary disease
Mucosal Immunology (2016)
-
Suhuang antitussive capsule at lower doses attenuates airway hyperresponsiveness, inflammation and remodeling in a murine model of chronic asthma
Scientific Reports (2016)