Abstract
Interleukin 33 (IL-33) is a recently discovered cytokine member of the IL-1 superfamily that is widely expressed in fixed tissue cells, including endothelial and epithelial cells. IL-33 induces helper T cells, mast cells, eosinophils, and basophils to produce type-2 cytokines through binding to the ST2/IL-1 receptor accessory protein complex. Recent studies have shown IL-33 to be upregulated in intestinal parasite infection and in epithelial cells and myofibroblasts in ulcerative colitis (UC). The findings point to a role for IL-33 in directing the TH2-type immune responses in these types of mucosal inflammation. As the IL-33/ST2 receptor axis can be manipulated by various blocking antibodies, this could be a potential therapeutic target in the future treatment of UC.
Similar content being viewed by others
Introduction
The important beneficial effect of antitumor necrosis factor-α (TNF-α) treatment on the clinical course of ulcerative colitis (UC) and Crohn's disease (CD) has taught gastroenterologist the importance of modulating of specific immunological pathways therapeutically in these diseases.1 Interleukin-33 (IL-33) is a newly described proinflammatory TH2 polarizing cytokine2 that could accomplish the requirements for being a new target in future treatment of immune-mediated diseases. IL-33 is quite dissimilar to other known immune mediators in that it is mainly produced by non-immunocompetent cells in the mucosa, but affects a wide array of immune cells.3, 4 In intestinal inflammation, IL-33 is mainly involved in TH2-type responses including immune reactions toward intestinal parasite infections and the inflammatory response found in UC, whereas IL-33 seems not to be involved in the TH1/TH17-type response in CD. The present review focuses on the regulation of IL-33 expression, its roles as a cytokine, and how the characteristics of IL-33 signaling might impact intestinal inflammation, with emphasis on its role in UC.
Search Strategy and Selection Criteria
A search of English-language publications was performed in the PubMed database until April 2011. The following search terms were applied: IL-33 or ST2 alone or combined with one of the following terms: Colitis, Crohn's disease or inflammatory bowel disease, intestinal or ulcerative colitis. English-language reviews, letters, editorials, and articles were considered. No publication date restrictions were applied. Subsequently, articles were selected on the basis of their relevance to the text, and additional articles were identified by scanning their reference lists.
IL-33: Inductor of a TH2 Response
IL-33 was first discovered in 2003 as the nuclear factor from high endothelial venules and was in 2005 described as a 30 kD protein belonging to the IL-1 cytokine family.2, 5 The IL-1 family is a conserved family of genes with 11 members, including IL-1α, IL-1β, IL-18, and IL-33.6 It was identified as a ligand for the ST2 receptor (also known as IL-1 receptor like 1 (IL-1RL1)), which prior to the identification of IL-33 was without known ligands.7 In human and mice, the IL-33 protein is primarily expressed in endothelial cells of all organs and in epithelial cells of the intestine, airways, and epidermis, and additionally on the mRNA level in a number of other fixed tissue cells, such as fibroblast-like synovium cells, fibroblasts, adipocytes, and smooth muscle cells, in various organs.8, 9, 10, 11, 12, 13, 14, 15 Although some reports indicate its expression in primary monocytes and macrophages (although this is debated and might not be the case in humans2) and mast cells, IL-33 is in general not a cytokine expressed in leukocytes.16, 17, 18 Non-dermal and non-mucosal expression of IL-33 has additionally been reported, e.g., in the human liver during inflammation and fibrosis, and in human and mice joints during arthritis.14, 19, 20, 21, 22, 23, 24
IL-33 function as a proinflammatory cytokine by binding to the heterodimeric receptor complex consisting of the ST2 receptor and the widely expressed IL-1R accessory protein.25, 26 The ST2 receptor is expressed on human and mice basophilic and eosinophilic granulocytes, mast cells, monocytes, dendritic cells, mice natural killer cells, NKT cells, and human and mice TH2 lymphocytes, indicating that IL-33 has a broad range of effects on the immune system and on the inflammatory reaction.2, 27, 28, 29, 30, 31, 32, 33 Studies based on mouse mast cell lines, mouse embryonic fibroblasts and HEK293 cells has shown that binding of IL-33 to the ST2/IL-1RAP receptor heterodimer allows myeloid differentiation primary response protein 88 (MYD88) to associate with the intracellular part of the IL-1RAP, thereby recruiting IL-1R-associated kinase 1 (IRAK1) and IRAK4 to the receptor complex (Figure 1).2 The IRAKs subsequently induces activation of mitogen-activated protein kinases (MAPK), extracellular signal-regulated kinase 1 (ERK1), ERK2, p38, and JUN N-terminal kinase 1 (JNK1) through TNF receptor-associated factor 6 (TRAF6) and nuclear factor κB pathway.2, 34, 35
Interleukin-33 (IL-33) signaling pathways. IL-33 binds to the heterodimer receptor complex consisting of ST2 and IL-1 receptor accessory protein (IL-1RAP). The binding leads to recruitment of myeloid differentiation primary response protein 88 (MYD88) and tumor necrosis factor receptor-associated factor 6 (TRAF6).35 This leads to nuclear factor κB (NF-κB) activation and activation of the mitogen-activated protein kinases (MAPK) p38, signal-regulated kinase (ERK), and JUN N-terminal kinase (JNK), which are strong inducers of proinflammatory cytokines and chemokines known to be involved in inflammation in ulcerative colitis.80, 81
The mere fact that the ST2 receptor is expressed on TH2 lymphocytes and not on TH1 lymphocytes suggest that IL-33 acts as an Th2 polarizing cytokine.2, 36 Stimulation of TH2 cells with IL-33 induces IL-5 and IL-13 (both typical Th2 cytokines37) independently of a IL-4 stimulation, and IL-33 acts as a chemoattractant for TH2 cells.2, 38, 39 Further, IL-33 induces eosinophilia and activation of eosinophils to express the CXC-chemokine ligand 8 (CXCL8, also known as IL-8) and superoxide production,32, 40, 41 and it activates mast cells to secrete IL-1, IL-6, IL-13, TNF-α, and the CC-chemokine ligand 2 and 3 (CCL2 and CCL3).31, 34, 42, 43, 44, 45 In basophils, IL-33 induces secretion of IL-4, IL-13, and CXCL8 and also induces basophil cell expansion.29, 46, 47 Altogether, IL-33 promotes the activation of granulocytes and T cells to express cytokines which are typical of Th2-type responses. IL-33 is indirectly involved in attracting neutrophilic granulocytes, which do not express the ST2 receptor, through induction of the CXCL8 chemokine.41, 46, 48, 49
The response to IL-33 is most likely dependent on co-stimulation factors and immune cell differentiation since both mice and human TH2 cells, natural killer and natural killer T cells are capable of producing both interferon-γ and other TH1-type cytokines in response to different co-stimulatory regimens with IL-33.32, 33
The Bioactive Form of IL-33
Despite the increasing evidence of IL-33 being involved in inflammatory signaling, the actual way of inducing IL-33 upregulation, and especially IL-33 release from the cells, remains a controversial topic. IL-33, as most other IL-1 family cytokines, lacks signal peptides and is consequently not secreted through the classical secretory pathway engaged by several other cytokines. IL-33 is expressed as a pro-form with a N-terminal pro-domain. IL-33 was first described to be a caspase 1 substrate similar to IL-1α, IL-1β, and IL-18. For those latter cytokines activation of the multiprotein complex, the inflammasome leads to caspase 1 activation, which subsequently cleaves and matures the cytokines by removing the pro-domain.2, 50, 51, 52 However, others have shown that IL-33 may normally not be cleaved by caspase 1.17, 53, 54, 55
Much experimental work on activation of immune cells by IL-33 has been performed with the use of human recombinant mature IL-33,29, 31, 56 but it is still uncertain if this is the bioactive form.57 Indeed, there is evidence of IL-33 not being a natural substrate for caspase 1,17, 55 and that IL-33 is secreted in its pro-form.17 Further, the pro-form of IL-33 is able to activate target cells via the ST2 receptor.17, 54, 55 In fact, two groups have independently reported that IL-33 cleavage by caspase 1 (and other caspases) might attenuate the biological activity of IL-33 in vivo and in vitro.54, 55 On the other hand, in situ processing and maturing of pro-IL-33 by THP-1 cells have been reported.17 The ability of pro-IL-33 to activate cells could thus be caused by local processing of pro-IL-33 to mature IL-33, which could then bind to the ST2 receptor. The available evidence thus indicates that both pro-IL-33 and matured IL-33 could be the active form of the cytokine.
IL-33 can be expressed in the nuclei of cells.11, 16, 57 This expression pattern is also observed for other cytokines, e.g., pro-IL-1α and high-mobility group box 1.58, 59 High-mobility group box 1 and pro-IL-1α have been shown to be released during necrosis of cells, and in part they mediate the inflammatory response seen in necrosis by acting as “alarmins” that both recruit and activate immune cells.60, 61 In contrary, during apoptosis, these mediators are proteolysed and inactivated by caspases, thereby avoiding inflammation.62 Similar to high-mobility group box 1 and IL-1α, IL-33 is released by necrosis and cleaved and inactivated by caspases during apoptosis, and IL-33 has accordingly by some researchers been classified as an alarmin.9, 54, 55, 57 It is, however, evident that IL-33 is produced and released from non-necrotic cells,17 and therefore that IL-33 acts as a more classic cytokine, apart from the putative role as an alarmin.57
IL-33 in Intestinal Inflammation
The intestine is an immune organ, which upon infection or dysregulation of the immune system can mount inflammatory responses. These T-cell-mediated responses have broadly been divided into TH1, TH2, and TH17-type responses depending on the type of T helper cells and cytokine profiles involved.63, 64 Helminth infection responses are prototypes of TH2 responses,65 and a similar response is thought to play a key role in the immune reaction of UC, whereas inflammation in CD is characterized by a TH1/TH17-type response.64, 66 As IL-33 produces a TH2-type response in a number of immune cells, it has been of interest to investigate if this cytokine is involved in typical TH2-type intestinal immune reactions.
IL-33 in UC
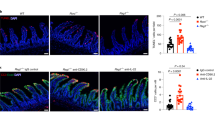
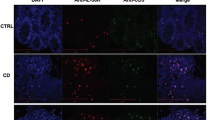
IL-33 was recently found to be significantly upregulated, both on the mRNA and protein level in colonic epithelial cells from patients with active UC, as compared to patients with quiescent disease and control subjects.4 IL-33 was expressed primarily in the cytoplasm of the colonic epithelial cells. Endothelial cells normally express IL-33, but do not so in active UC. This finding can be explained by a previous report of a decreased endothelial IL-33 expression in endothelial cells exposed to proinflammatory cytokines.67 The finding of upregulated IL-33 in active UC has later been confirmed by Pastorelli et al.,22 who also found an increased expression of IL-33 in epithelial cells in active UC, and in lamina propria inflammatory cells, with the intestinal IL-33 being in its pro-form, whereas circulating IL-33 was found elevated in its matured form. The explanation for the lack of expression of matured IL-33 in the mucosa and epithelium could be that colonic epithelial cells express very low levels of cleaved active caspase 1 in active UC.4 Infliximab treatment reduced circulating IL-33 levels in patients with UC, but it was not reported if the disease activity correlated with circulating IL-33 levels.22 Flow cytometry of lamina propria mononuclear cells from patients with UC revealed that macrophages (CD11b+) and apparently B cells (CD19+) had an expression of IL-33. A parallel report confirmed an increased mucosal IL-33 expression in epithelial cells in UC.68 This group, however, found IL-33 abundantly expressed in control specimens as well, including epithelial cells. Additionally two recent reports have described IL-33 to be increased primarily in ulceration-associated myofibroblasts in active UC.3, 69
Altogether, these results point to an increased expression of IL-33 in the mucosa of patients with active UC. Both epithelial cells and myofibroblasts seem to be contributors to the IL-33 production in active UC: Epithelial cells could be the primary source of IL-33 in mild-to-moderate UC without macroscopic lesions of the mucosa, whereas myofibroblasts become activated to produce IL-33 by mucosal wounding and mucosal exposure to luminal antigens in severe UC. In the latter case, IL-33 could be regarded as an alarmin in severely active UC.
The ST2 receptor has been reported to be upregulated in active UC on CD11b+ macrophages and CD4+ lymphocytes.22, 68 Interestingly, the ST2 receptor is expressed in colonic epithelial cells in control specimens, whereas this expression is significantly decreased in active UC, both on the mRNA and the protein level.22 Both studies also found an increase in the IL-33, binding soluble form of the ST2 receptor, the decoy sST2 receptor in active UC sera as compared with controls.22, 68
What actually activates IL-33 expression and secretion is much less investigated than the effects of IL-33 stimulation on target cells. However, in immortalized human fibroblasts, IL-33 could be induced by the Toll-like receptor 3 agonist poly (I:C), and the expression could be enhanced by transforming growth factor-β co-stimulation.69 Isolated colonic myofibroblasts and fibroblasts responded with an increased IL-33 expression to a combination of TNF-α and IL-1β stimulation,3, 69 whereas similar cytokine exposure of the colonic epithelial Caco2 cell line did not affect the IL-33 expression.3, 4 However, IL-33 has been found to be induced by TNF-α treatment of the HT29 colonic epithelial cancer cell line, suggesting cell-line-specific differences.22 Both IL-1β and TNF-α can together with stimulation of Toll-like receptors 2, 3, 9 and mechanical strain upregulate IL-33 in a number of cell types, but their effect on intestinal epithelial cells have not yet been investigated, apart from the role of TNF-α in HT29 cells.2, 8, 14, 21, 70, 71 A proposed integrated model of the IL-33/ST2 signaling in UC is presented in Figure 2.
An integrated model of interleukin-33 (IL-33) signaling in ulcerative colitis (UC). IL-33 is produced by epithelial cells and mucosal myofibroblasts where the mucosa is wounded. IL-33 results in the activation of a number of leukocytes, which respond by producing proinflammatory cytokines, IL-4, IL-5, IL-6, IL-13, and tumor necrosis factor-α (TNF-α) and the chemokines chemokine (C-C motif) ligand 2 and 3 (CCL2 and CCL3) and CXC-chemokine ligand 8 (CXCL8). IL-33 might be produced by colonic epithelial cells in response to TNF-α. It is suggested that stimulation of Toll-like receptors 2, 3, and 9 (TLR2, TLR3, and TLR9) by bacterial products could also contribute to IL-33 in epithelial cells, as this has been found in other cell types. However, this has not been shown for colonic epithelial cells yet. Myofibroblasts might be stimulated to produce IL-33 by TNF-α, IL-1β, and transforming growth factor-β (TGF-β). It is suggested that myofibroblasts near wounds could also release IL-33 as an alarmin in response to cellular stress induced by the mucosal break.
IL-33 in Other Forms of Intestinal Inflammation
The first study associating IL-33 with inflammatory bowel disease actually indicated that it was upregulated on the mRNA level in endothelial cells from CD patients, although this study did not include UC specimens.11 Subsequent studies did, however, show little or no change of the mucosal IL-33 expression in both active and quiescent CD, and IL-33 is not considered to play any key role in this disease.3, 22, 68, 69
IL-33 might also play a potential role in intestinal parasite infection. Infection of mice with Trichuris muris, which were resistant to the parasite, lead to an increased expression of IL33 mRNA compared with animals susceptible to the infection, and treatment with recombinant IL-33 rendered the susceptible animals resistant to infection.72 This resistance to infection was accompanied by induction of a TH2-type cytokine profile, and repression of TH1 and TH17-type cytokines. Likewise, IL-33 has been shown to be upregulated in the dextran sulfate sodium and senescence accelerated prone mouse-mice colitis models, which are experimental TH2-type and TH1/TH2-type inflammation response acute colitis models, respectively, whereas IL-33 is actually downregulated in the severe combined immunodeficiency transfer mouse model of chronic colitis, which has a TH1-type cytokine response (own observations plus22, 73).
IL-33 as a Therapeutic Target
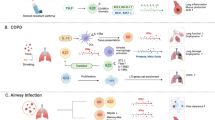
The IL-33/ST2 receptor axis has recently been the therapeutic target in models of chronic inflammation in the airways and joints. This includes an murine model of asthma, where an anti-IL-33 antibody was administered intraperitoneally and reduced inflammation and mucus secretion as well as eosinophilic counts, immunoglobulin E secretion, and IL-4 -5 and 13 concentrations of bronchial lavage.74 Another approach was to treat mice with experimental arthritis with anti-ST2 antibodies.14 This treatment resulted in the decrease of arthritis severity and a concomitant decrease in interferon-γ and IL-17 production. A similar inflammation dampening effect of anti-ST2 antibodies has been observed in an animal model of chronic airway inflammation.75
As UC is recognized as a chronic inflammatory condition with a TH2-type cytokine profile,66, 76, 77, 78, 79 and also is characterised by an increased expression of the TH2 polarizing IL-33, it is tempting to speculate that IL-33 might play a pivotal role in orchestrating the inflammation seen in UC. Given the exciting results with anti-IL-33 and anti-ST2 treatments in other chronic inflammatory conditions, it is conceivable that a similar treatment would additionally be beneficial for the treatment of UC.
Conclusions
Although IL-33 was identified only few years ago, it is now evident that this widely expressed cytokine plays a key role in different TH2-type inflammatory conditions by activating a number of immune cells. Accordingly, the current evidence suggests that IL-33 might primarily be involved in TH2-type intestinal inflammation induced by parasite infection or UC. IL-33 is upregulated in active stages of UC by an increased expression in both epithelial cells and subepithelial myofibroblasts of the colon. The significance of this upregulation remains to be established, as does the identification of signaling pathways responsible for the upregulated IL-33 expression. Thus, functional studies blocking IL-33/ST2 receptor signaling in experimental models of colitis are highly warranted. Therapeutic attempts to modify this pathway have, however, been successful in animal models of other types of chronic inflammation than colitis, and targeting the ST2/IL-33 pathway might as well be found to have an analogous relevance in the future management of UC.
References
Nielsen, O.H., Seidelin, J.B., Munck, L.K. & Rogler, G. Use of biological molecules in treatment of inflammatory bowel disease. J. Intern. Med.; 269, e-pub ahead of print 17 Jan 2011.
Schmitz, J. et al. IL-33, an interleukin-1-like cytokine that signals via the IL-1 receptor-related protein ST2 and induces T helper type 2-associated cytokines. Immunity 23, 479–490 (2005).
Kobori, A. et al. Interleukin-33 expression is specifically enhanced in inflamed mucosa of ulcerative colitis. J. Gastroenterol. 45, 999–1007 (2010).
Seidelin, J.B., Bjerrum, J.T., Coskun, M., Widjaya, B., Vainer, B. & Nielsen, O.H. IL-33 is upregulated in colonocytes of ulcerative colitis. Immunol. Lett. 128, 80–85 (2010).
Baekkevold, E.S. et al. Molecular characterization of NF-HEV, a nuclear factor preferentially expressed in human high endothelial venules. Am. J. Pathol. 163, 69–79 (2003).
Sims, J.E. & Smith, D.E. The IL-1 family: regulators of immunity. Nat. Rev. Immunol. 10, 89–102 (2010).
Tominaga, S. A putative protein of a growth specific cDNA from BALB/c-3T3 cells is highly similar to the extracellular portion of mouse interleukin 1 receptor. FEBS Lett. 258, 301–304 (1989).
Sanada, S., Hakuno, D., Higgins, L.J., Schreiter, E.R., McKenzie, A.N. & Lee, R.T. IL-33 and ST2 comprise a critical biomechanically induced and cardioprotective signaling system. J. Clin. Invest. 117, 1538–1549 (2007).
Moussion, C., Ortega, N. & Girard, J.P. The IL-1-like cytokine IL-33 is constitutively expressed in the nucleus of endothelial cells and epithelial cells in vivo: a novel ‘alarmin’? PLoS One 3, e3331 (2008).
Miller, A.M. et al. IL-33 reduces the development of atherosclerosis. J. Exp. Med. 205, 339–346 (2008).
Carriere, V. et al. IL-33, the IL-1-like cytokine ligand for ST2 receptor, is a chromatin-associated nuclear factor in vivo. Proc. Natl. Acad. Sci. USA 104, 282–287 (2007).
Prefontaine, D. et al. Increased expression of IL-33 in severe asthma: evidence of expression by airway smooth muscle cells. J. Immunol. 183, 5094–5103 (2009).
Wood, I.S., Wang, B. & Trayhurn, P. IL-33, a recently identified interleukin-1 gene family member, is expressed in human adipocytes. Biochem. Biophys. Res. Commun. 384, 105–109 (2009).
Palmer, G. et al. Inhibition of interleukin-33 signaling attenuates the severity of experimental arthritis. Arthritis Rheum. 60, 738–749 (2009).
Verri, W.A. Jr et al. IL-33 mediates antigen-induced cutaneous and articular hypernociception in mice. Proc. Natl. Acad. Sci. USA 105, 2723–2728 (2008).
Nile, C.J., Barksby, E., Jitprasertwong, P., Preshaw, P.M. & Taylor, J.J. Expression and regulation of interleukin-33 in human monocytes. Immunology 130, 172–180 (2010).
Talabot-Ayer, D., Lamacchia, C., Gabay, C. & Palmer, G. Interleukin-33 is biologically active independently of caspase-1 cleavage. J. Biol. Chem. 284, 19420–19426 (2009).
Hsu, C.L., Neilsen, C.V. & Bryce, P.J. IL-33 is produced by mast cells and regulates IgE-dependent inflammation. PLoS One 5, e11944 (2010).
Prefontaine, D. et al. Increased IL-33 expression by epithelial cells in bronchial asthma. J. Allergy Clin. Immunol. 125, 752–754 (2010).
Roth, G.A. et al. Up-regulation of interleukin 33 and soluble ST2 serum levels in liver failure. J. Surg. Res. 163, e79–e83 (2010).
Marvie, P. et al. Interleukin-33 overexpression is associated with liver fibrosis in mice and humans. J. Cell Mol. Med. 14, 1726–1739 (2010).
Pastorelli, L. et al. Epithelial-derived IL-33 and its receptor ST2 are dysregulated in ulcerative colitis and in experimental Th1/Th2 driven enteritis. Proc. Natl. Acad. Sci. USA 107, 8017–8022 (2010).
Kaieda, S. et al. Synovial fibroblasts promote the expression and granule accumulation of tryptase via interleukin-33 and its receptor ST-2 (IL1RL1). J. Biol. Chem. 285, 21478–21486 (2010).
Matsuyama, Y. et al. Increased levels of interleukin 33 in sera and synovial fluid from patients with active rheumatoid arthritis. J. Rheumatol. 37, 18–25 (2010).
Chackerian, A.A., Oldham, E.R., Murphy, E.E., Schmitz, J., Pflanz, S. & Kastelein, R.A. IL-1 receptor accessory protein and ST2 comprise the IL-33 receptor complex. J. Immunol. 179, 2551–2555 (2007).
Greenfeder, S.A., Nunes, P., Kwee, L., Labow, M., Chizzonite, R.A. & Ju, G. Molecular cloning and characterization of a second subunit of the interleukin 1 receptor complex. J. Biol. Chem. 270, 13757–13765 (1995).
Espinassous, Q. et al. IL-33 enhances lipopolysaccharide-induced inflammatory cytokine production from mouse macrophages by regulating lipopolysaccharide receptor complex. J. Immunol. 183, 1446–1455 (2009).
Rank, M.A., Kobayashi, T., Kozaki, H., Bartemes, K.R., Squillace, D.L. & Kita, H. IL-33-activated dendritic cells induce an atypical TH2-type response. J. Allergy Clin. Immunol. 123, 1047–1054 (2009).
Suzukawa, M. et al. An IL-1 cytokine member, IL-33, induces human basophil activation via its ST2 receptor. J. Immunol. 181, 5981–5989 (2008).
Moulin, D., Donze, O., Talabot-Ayer, D., Mezin, F., Palmer, G. & Gabay, C. Interleukin (IL)-33 induces the release of pro-inflammatory mediators by mast cells. Cytokine 40, 216–225 (2007).
Iikura, M. et al. IL-33 can promote survival, adhesion and cytokine production in human mast cells. Lab. Invest 87, 971–978 (2007).
Smithgall, M.D., Comeau, M.R., Yoon, B.R., Kaufman, D., Armitage, R. & Smith, D.E. IL-33 amplifies both Th1- and Th2-type responses through its activity on human basophils, allergen-reactive Th2 cells, iNKT and NK cells. Int. Immunol. 20, 1019–1030 (2008).
Bourgeois, E. et al. The pro-Th2 cytokine IL-33 directly interacts with invariant NKT and NK cells to induce IFN-gamma production. Eur. J. Immunol. 39, 1046–1055 (2009).
Pushparaj, P.N. et al. The cytokine interleukin-33 mediates anaphylactic shock. Proc. Natl. Acad. Sci. USA 106, 9773–9778 (2009).
Funakoshi-Tago, M. et al. TRAF6 is a critical signal transducer in IL-33 signaling pathway. Cell Signal 20, 1679–1686 (2008).
Chan, W.L., Pejnovic, N., Lee, C.A. & Al-Ali, N.A. Human IL-18 receptor and ST2L are stable and selective markers for the respective type 1 and type 2 circulating lymphocytes. J. Immunol. 167, 1238–1244 (2001).
Weaver, C.T., Hatton, R.D., Mangan, P.R. & Harrington, L.E. IL-17 family cytokines and the expanding diversity of effector T cell lineages. Annu. Rev. Immunol. 25, 821–852 (2007).
Kurowska-Stolarska, M. et al. IL-33 induces antigen-specific IL-5+ T cells and promotes allergic-induced airway inflammation independent of IL-4. J. Immunol. 181, 4780–4790 (2008).
Komai-Koma, M., Xu, D., Li, Y., McKenzie, A.N., McInnes, I.B. & Liew, F.Y. IL-33 is a chemoattractant for human Th2 cells. Eur. J. Immunol. 37, 2779–2786 (2007).
Kurowska-Stolarska, M. et al. IL-33 amplifies the polarization of alternatively activated macrophages that contribute to airway inflammation. J. Immunol. 183, 6469–6477 (2009).
Cherry, W.B., Yoon, J., Bartemes, K.R., Iijima, K. & Kita, H. A novel IL-1 family cytokine, IL-33, potently activates human eosinophils. J. Allergy Clin. Immunol. 121, 1484–1490 (2008).
Ho, L.H. et al. IL-33 induces IL-13 production by mouse mast cells independently of IgE-FcepsilonRI signals. J. Leukoc. Biol. 82, 1481–1490 (2007).
Allakhverdi, Z., Smith, D.E., Comeau, M.R. & Delespesse, G. Cutting edge: the ST2 ligand IL-33 potently activates and drives maturation of human mast cells. J. Immunol. 179, 2051–2054 (2007).
Allakhverdi, Z. et al. CD34+ hemopoietic progenitor cells are potent effectors of allergic inflammation. J. Allergy Clin. Immunol. 123, 472–478 (2009).
Ali, S., Huber, M., Kollewe, C., Bischoff, S.C., Falk, W. & Martin, M.U. IL-1 receptor accessory protein is essential for IL-33-induced activation of T lymphocytes and mast cells. Proc. Natl. Acad. Sci. USA 104, 18660–18665 (2007).
Pecaric-Petkovic, T., Didichenko, S.A., Kaempfer, S., Spiegl, N. & Dahinden, C.A. Human basophils and eosinophils are the direct target leukocytes of the novel IL-1 family member IL-33. Blood 113, 1526–1534 (2009).
Schneider, E. et al. IL-33 activates unprimed murine basophils directly in vitro and induces their in vivo expansion indirectly by promoting hematopoietic growth factor production. J. Immunol. 183, 3591–3597 (2009).
Verri, W.A. Jr et al. IL-33 induces neutrophil migration in rheumatoid arthritis and is a target of anti-TNF therapy. Ann. Rheum. Dis. 69, 1697–1703 (2010).
ves-Filho, J.C. et al. Interleukin-33 attenuates sepsis by enhancing neutrophil influx to the site of infection. Nat. Med. 16, 708–712 (2010).
Martinon, F., Burns, K. & Tschopp, J. The inflammasome: a molecular platform triggering activation of inflammatory caspases and processing of proIL-beta. Mol. Cell 10, 417–426 (2002).
Burns, K., Martinon, F. & Tschopp, J. New insights into the mechanism of IL-1beta maturation. Curr. Opin. Immunol. 15, 26–30 (2003).
Martinon, F. & Tschopp, J. Inflammatory caspases and inflammasomes: master switches of inflammation. Cell Death Differ 14, 10–22 (2007).
Ohno, T. et al. Caspase-1, caspase-8, and calpain are dispensable for IL-33 release by macrophages. J. Immunol. 183, 7890–7897 (2009).
Cayrol, C. & Girard, J.P. The IL-1-like cytokine IL-33 is inactivated after maturation by caspase-1. Proc. Natl. Acad. Sci. USA 106, 9021–9026 (2009).
Luthi, A.U. et al. Suppression of interleukin-33 bioactivity through proteolysis by apoptotic caspases. Immunity 31, 84–98 (2009).
Suzukawa, M. et al. Interleukin-33 enhances adhesion, CD11b expression and survival in human eosinophils. Lab. Invest. 88, 1245–1253 (2008).
Haraldsen, G., Balogh, J., Pollheimer, J., Sponheim, J. & Kuchler, A.M. Interleukin-33—cytokine of dual function or novel alarmin? Trends Immunol. 30, 227–233 (2009).
Golstein, P. & Kroemer, G. Cell death by necrosis: towards a molecular definition. Trends Biochem. Sci. 32, 37–43 (2007).
Taylor, R.C., Cullen, S.P. & Martin, S.J. Apoptosis: controlled demolition at the cellular level. Nat. Rev. Mol. Cell Biol. 9, 231–241 (2008).
Raucci, A., Palumbo, R. & Bianchi, M.E. HMGB1: a signal of necrosis. Autoimmunity 40, 285–289 (2007).
Scaffidi, P., Misteli, T. & Bianchi, M.E. Release of chromatin protein HMGB1 by necrotic cells triggers inflammation. Nature 418, 191–195 (2002).
Kazama, H., Ricci, J.E., Herndon, J.M., Hoppe, G., Green, D.R. & Ferguson, T.A. Induction of immunological tolerance by apoptotic cells requires caspase-dependent oxidation of high-mobility group box-1 protein. Immunity 29, 21–32 (2008).
Korn, T., Bettelli, E., Oukka, M. & Kuchroo, V.K. IL-17 and Th17 cells. Annu. Rev. Immunol. 27, 485–517 (2009).
Brand, S. Crohn's disease: Th1, Th17 or both? The change of a paradigm: new immunological and genetic insights implicate Th17 cells in the pathogenesis of Crohn's disease. Gut 58, 1152–1167 (2009).
Maizels, R.M., Pearce, E.J., Artis, D., Yazdanbakhsh, M. & Wynn, T.A. Regulation of pathogenesis and immunity in helminth infections. J. Exp. Med. 206, 2059–2066 (2009).
Niessner, M. & Volk, B.A. Altered Th1/Th2 cytokine profiles in the intestinal mucosa of patients with inflammatory bowel disease as assessed by quantitative reversed transcribed polymerase chain reaction (RT-PCR). Clin. Exp. Immunol. 101, 428–435 (1995).
Kuchler, A.M. et al. Nuclear interleukin-33 is generally expressed in resting endothelium but rapidly lost upon angiogenic or proinflammatory activation. Am. J. Pathol. 173, 1229–1242 (2008).
Beltran, C.J. et al. Characterization of the novel ST2/IL-33 system in patients with inflammatory bowel disease. Inflamm. Bowel Dis. 16, 1097–1107 (2010).
Sponheim, J. et al. Inflammatory bowel disease-associated interleukin-33 is preferentially expressed in ulceration-associated myofibroblasts. Am. J. Pathol. 177, 2804–2815 (2010).
Xu, D. et al. IL-33 exacerbates antigen-induced arthritis by activating mast cells. Proc. Natl. Acad. Sci. USA 105, 10913–10918 (2008).
Hudson, C.A., Christophi, G.P., Gruber, R.C., Wilmore, J.R., Lawrence, D.A. & Massa, P.T. Induction of IL-33 expression and activity in central nervous system glia. J. Leukoc. Biol. 84, 631–643 (2008).
Humphreys, N.E., Xu, D., Hepworth, M.R., Liew, F.Y. & Grencis, R.K. IL-33, a potent inducer of adaptive immunity to intestinal nematodes. J. Immunol. 180, 2443–2449 (2008).
Oboki, K. et al. IL-33 is a crucial amplifier of innate rather than acquired immunity. Proc. Natl. Acad. Sci. USA 107, 18581–18586 (2010).
Liu, X., Li, M., Wu, Y., Zhou, Y., Zeng, L. & Huang, T. Anti-IL-33 antibody treatment inhibits airway inflammation in a murine model of allergic asthma. Biochem. Biophys. Res. Commun. 386, 181–185 (2009).
Kearley, J., Buckland, K.F., Mathie, S.A. & Lloyd, C.M. Resolution of allergic inflammation and airway hyperreactivity is dependent upon disruption of the T1/ST2-IL-33 pathway. Am. J. Respir. Crit. Care Med. 179, 772–781 (2009).
Targan, S.R. & Karp, L.C. Defects in mucosal immunity leading to ulcerative colitis. Immunol. Rev. 206, 296–305 (2005).
Bouma, G. & Strober, W. The immunological and genetic basis of inflammatory bowel disease. Nat. Rev. Immunol. 3, 521–533 (2003).
Heller, F. et al. Interleukin-13 is the key effector Th2 cytokine in ulcerative colitis that affects epithelial tight junctions, apoptosis, and cell restitution. Gastroenterology 129, 550–564 (2005).
Fuss, I.J. et al. Disparate CD4+ lamina propria (LP) lymphokine secretion profiles in inflammatory bowel disease. Crohn's disease LP cells manifest increased secretion of IFN-gamma, whereas ulcerative colitis LP cells manifest increased secretion of IL-5. J. Immunol. 157, 1261–1270 (1996).
Coskun, M., Olsen, J., Seidelin, J.B. & Nielsen, O.H. The involvement of MAP kinases in inflammatory bowel disease. Clin. Chim. Acta. 412, 513–520 (2011).
Andresen, L., Jorgensen, V.L., Perner, A., Hansen, A., Eugen-Olsen, J. & Rask-Madsen, J. Activation of nuclear factor kappaB in colonic mucosa from patients with collagenous and ulcerative colitis. Gut 54, 503–509 (2005).
Acknowledgements
This study was supported by grants from Fonden til Lægevidenskabens Fremme (the AP Møller Foundation), the Family Erichsen Memorial Foundation, the Axel Muusfeldts Foundation, and the The Foundation of Aase and Ejnar Danielsen.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Seidelin, J., Rogler, G. & Nielsen, O. A role for interleukin-33 in TH2-polarized intestinal inflammation?. Mucosal Immunol 4, 496–502 (2011). https://doi.org/10.1038/mi.2011.22
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2011.22
This article is cited by
-
ST2 and regulatory T cells in the colorectal adenoma/carcinoma microenvironment: implications for diseases progression and prognosis
Scientific Reports (2020)
-
IL-33 deficiency protects mice from DSS-induced experimental colitis by suppressing ILC2 and Th17 cell responses
Inflammation Research (2020)
-
Cellular and clinicopathological features of the IL-33/ST2 axis in human esophageal squamous cell carcinomas
Cancer Cell International (2018)
-
Role of the IL-33-ST2 axis in sepsis
Military Medical Research (2017)
-
Exosomes miR-126a released from MDSC induced by DOX treatment promotes lung metastasis
Oncogene (2017)