Abstract
The granuloma that forms in response to Mycobacterium tuberculosis must be carefully balanced in terms of immune responses to provide sufficient immune cell activation to inhibit the growth of the bacilli, yet modulate the inflammation to prevent pathology. There are likely many scenarios by which this balance can be reached, given the complexity of the immune responses induced by M. tuberculosis. In this review, we focus on the key role of the macrophage in balancing inflammation in the granuloma.
Similar content being viewed by others
Introduction
Tuberculosis remains a serious health threat worldwide. There were 9.4 million new cases of tuberculosis and 1.7 million deaths in 2009.1 Although this disease can be cured by drug treatment, the regimens involve several drugs and at least 6 months of therapy; obstacles to treatment include timely diagnosis, access to health care, compliance, side effects, and drug interactions. A vaccine, BCG (Bacillus Calmette-Guerin), which is an attenuated Mycobacterium bovis strain, has been used for nearly a century, but efficacy against adult disease is questionable. In fact, most of the deaths from tuberculosis occur in countries where BCG vaccination of infants is routine.1 Clearly, better diagnostic, preventive, and therapeutic strategies are necessary to gain control of this disease.
Tuberculosis is caused by Mycobacterium tuberculosis (Mtb). This bacterium has a complex cell wall, composed of long-chain fatty acids, glycolipids, peptidoglycan, and proteins, and a slow doubling time (18–24 h). It is primarily a respiratory pathogen, and usually transmitted by the cough of a person with active disease. Primary tuberculosis can occur within the first year or so after exposure, and is the result of an uncontrolled initial infection. This could be because of an extremely virulent bacillus, large or repeated exposures, an immune response that is insufficient to control bacterial replication, or the induction of excessive pathology. The majority (90%) of infected humans effectively contain, but do not eliminate, the bacteria and are defined as having “latent” infection. This is a clinical term, meaning a person is infected (as evidenced by T-cell reactivity to mycobacterial antigens) but is asymptomatic and not contagious. However, a latently infected human has a 10% lifetime risk of reactivating the infection and presenting with active tuberculosis. Thus, the estimated 2 billion latently infected humans are an enormous reservoir of potential disease.
The factors that lead to containment of infection or progression to disease are not well understood and are multifactorial. Typically, tuberculosis presents as pulmonary disease, but with systemic manifestations, including anorexia and wasting. The old name for tuberculosis was “consumption,” as this disease appears to consume the patient. The wasting is partly because of production of inflammatory cytokines, such as tumor necrosis factor (TNF), known to cause cachexia.2, 3 Thus, the disease is driven by host and mycobacterial factors. A new complication in the setting of human immunodeficiency virus/Mtb co-infection also points to inflammation as an important contributor to tuberculosis: antiretroviral therapy that restores CD4 T-cell responses can occasionally have the paradoxical effect of unmasking or reactivating tuberculosis.4, 5, 6 This immune reconstitution inflammatory syndrome also supports that modulation of inflammation may be an essential component of management of tuberculosis.
We hypothesize that the balance of pro- and anti-inflammatory immune responses at the site of infection (the granuloma) is crucial to control of infection. Although there are numerous inflammatory mediators in tuberculosis, a key cell in the granuloma is the macrophage. Here, we focus on the macrophage as a major player in the balance of inflammation in the granuloma, necessary for inhibiting bacterial replication and for control of pathology.
Initiation of Infection
Transmission occurs when droplet nuclei of Mtb expectorated via cough from someone with active tuberculosis are inhaled. The battle between pro- and anti-inflammatory signals begins in the airways with the initial contact of bacillus with host cells. Ingestion of intracellular bacteria by airway antigen-presenting cells (macrophages and dendritic cells) initiates the first important immune responses. Mtb induces proinflammatory cytokines interleukin (IL)-12, IL-1β, and TNF (reviewed in ref. 7). IL-12 plays a critical role in initiating a T helper 1 (TH1) T-cell response.8 TNF induces cytokine and chemokine production by macrophages, activates macrophages for killing, and modulates macrophage apoptosis.9, 10, 11, 12, 13 The anti-inflammatory cytokines such as IL-10 and TGF-β can also be produced by Mtb-infected macrophages, which downregulate proinflammatory cytokines and T-cell proliferation and activation, balancing the response between bacterial eradication and host survival.7, 14
The alveolar macrophages, which line the airways, have been described as deficient in their interaction with Mtb;15 however, most humans who encounter Mtb do not become infected (as determined by immunologic reactivity), suggesting that in fact, the cells in the airways are quite robust in deterring productive infection with this bacillus. Alveolar macrophages have been considered to be anti-inflammatory in nature,15 which contributes to suppressing inflammation in the airways. How these cells, or other cells in the airways, are so successful at warding off infection, then, remains to be determined.
Granuloma Formation
After the encounter of bacillus and macrophage in the airways, the infected macrophage may facilitate the spread of disease first by cellular necrosis to disseminate extracellular bacteria and by migration to distal sites in the lungs. Once in the parenchyma, the bacilli set off a slow inflammatory process by infected macrophages. These infected macrophages recruit uninfected macrophages to ultimately form a granuloma.16, 17, 18
Dendritic cells in lungs or airways are also infected by Mtb, and migrate to thoracic lymph nodes, where a T-cell response is primed.19 This process is quite slow; studies in various animal models suggests that priming of T cells does not occur until 12–21 days postinfection.20, 21, 22, 23 Pulmonary inflammation due to interaction of bacillus with macrophages and other cells results in recruitment of monocytes, neutrophils, and primed T cells and B cells to lungs, culminating in formation of a granuloma. A granuloma is an organized and structured collection of immune cells that forms in response to chronic antigenic stimulation, in the context of macrophage-mediated factors. The granuloma is the classic pathologic feature of tuberculosis, and functions both as a niche in which the bacillus can grow or persist and an immunologic microenvironment in which cells with antimycobacterial functions interact to control and prevent dissemination of the infection.
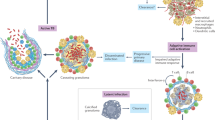
Granulomas are observed in active, latent, and reactivation tuberculosis. Thus, the mere formation of a granuloma is insufficient for control of infection—rather, the granuloma must be functioning properly. In active tuberculosis, the host often has numerous granulomas that are incapable of controlling infection; bacteria, either extracellular or within macrophages or dendritic cells, then spread throughout the lung or disseminate to other organs, initiating new granuloma formation. In latent infection, there are usually one or a few granulomas in lungs and lymph nodes, although our knowledge of the true nature of latent infection in humans is limited, and these granulomas are capable of limiting the growth and spread of Mtb. One of the major gaps in our understanding of tuberculosis is what factors define a “functioning” granuloma, i.e., the type of granuloma that eliminates or exerts long-term control over the infection. Based on the variety of immune responses shown to contribute to control or exacerbation of tuberculosis, we assume that multiple combinations of responses may constitute a functioning granuloma (Figure 1), and these likely differ among individuals and even among granulomas in a single individual.
Balance of responses in the granuloma dictate bacterial control and pathology. There are a variety of combinations that can lead to an inflammatory granuloma in active tuberculosis (TB). Three possibilities are shown: (a) Active granuloma with high bacterial numbers, many classically activated macrophages (CAMs) and alternatively activated macrophages (AAMs), T helper 1 (TH1) cells, some neutrophils, and few regulatory T cells (Tregs). (b) Active granuloma with too many Tregs, AAMs, not enough TH1 and CAMs, high neutrophils, and high bacterial load. (c) Active granuloma with fewer bacilli, but overabundance of CAMs and TH1 cells, and not enough Tregs. Two possible latent granulomas are shown, although there are likely many combinations. (d) Latent granuloma with CAMs and AAMs in balance, with relatively few T cells. (e) Latent granuloma with more Tregs to balance the higher TH17 and TH1, but a balance of AAMs and CAMs.
Although granulomas are composed of a variety of cell types, the primary cellular component of the structure is the macrophage. The macrophage is the initiating cell for granuloma formation17, 18 and the major cell type in most granulomas. Macrophages both harbor the majority of Mtb and have the effector functions to kill these bacilli. There are a variety of macrophage phenotypes in granulomas with various functions, including antimycobacterial effector mechanisms, pro- and anti-inflammatory cytokine production, and secretion of chemokines and proteins associated with tissue remodeling. Thus, this cell contributes to most aspects of inflammation and control of infection within the granuloma. This review will focus on the roles of the macrophage in promoting or controlling inflammation in tuberculosis granulomas, directly and through its interaction with other cells in the granuloma.
A Variety of Granuloma Types in Human Tuberculosis
In humans, a spectrum of granulomas is observed in active tuberculosis and even latent infection. The classic granuloma in tuberculosis is the caseous granuloma, so called because the center of this granuloma has a “cheese-like” appearance grossly. Histologically, this granuloma consists of epithelioid macrophages surrounding an acellular necrotic region, with a lymphocytic cuff, comprising both B and T cells.24 Neutrophils can also be observed within caseous granulomas. Caseous granulomas can range in size from 1 mm to >2 cm. In chronic or latent infection, this type of granuloma can become calcified, with the calcification process beginning within the caseous center. A calcified granuloma generally represents a successful immune response and is associated with fewer inflammatory cells than other granulomas. Other types of granulomas include non-necrotizing granulomas, composed primarily of macrophages with a few lymphocytes, necrotic neutrophilic granulomas, and completely fibrotic granulomas. Peripheral fibrosis can be observed in some caseous granulomas. With all of these granulomas types, it is easy to imagine several microenvironments within and among granulomas for the microbe, as well as a range of immune microenvironments.
Tuberculosis Model Systems
Tuberculosis is a human disease, but obtaining lung tissue (with granulomas) from people with tuberculosis is difficult. Thus, animal model systems are necessary for detailed studies of tuberculosis. Mice develop a chronic, progressive infection with Mtb; the granulomatous infiltration in lungs lacks the structured and organized appearance of human granulomas.25 There have been reports of mouse strains developing granulomas that more closely represent human lesions,26 and these may be useful for a focused approach to granuloma biology in a system that is rich in reagents. In Guinea pigs and rabbits, some granulomas are more human-like and studies in these species have yielded important insights on the development and structure of granulomas.25 Infection of zebrafish with Mycobacterium marinum, an aquatic mycobacterial species, recapitulates a human caseous granuloma.27 Studies in zebrafish embryos have allowed dynamic observation of granuloma formation and spread,16, 17, 18 and the use of genetic tools has enabled dissection of some of the factors important in granuloma formation and maintenance.9, 28 Non-human primates (primarily macaques) have been used as models for human tuberculosis.21, 29, 30, 31, 32, 33 A full spectrum of granuloma types identical to human granulomas can be observed in Mtb-infected macaques, and immunologic tools are available for this model. Finally, computational models of granulomas provide the unique ability to study factors involved in tuberculosis that are not possible to study in experimental systems.12, 34 Here, we draw on data from all the model systems in our discussion of granulomas in tuberculosis.
Classically and Alternatively Activated Macrophages in Tuberculosis
Monocytes migrate to the site of infection from blood, in response to inflammatory signals (cytokines and chemokines) that are often produced by macrophages as well.12 Only a fraction of macrophages in the granuloma are actually infected with Mtb, although this proportion is likely to be higher in a granuloma that is poorly functioning and not controlling the infection. It is difficult to estimate the fraction of cells infected in human granulomas, or the number of bacilli per cell because acid-fast staining for the microbe is notoriously inefficient in human and non-human primate tissues. Nonetheless, we consider the macrophage populations to consist of both infected and uninfected cells, both of which can be influenced by other factors (cells and soluble factors) in the granuloma. Mtb can have effects on macrophages from within by interacting with host receptors, such as Toll-like receptors in the phagosome.35, 36, 37, 38, 39, 40, 41, 42 It has been suggested that under some circumstances Mtb can escape the vacuole to reside in the cytoplasm,43, 44 and that mycobacterial molecules can exit the phagosome and interact with cytoplasmic receptors to induce responses.45, 46, 47, 48 Mycobacteria and microbial factors can interact with cells from the outside as well, again through Toll-like receptors or other receptors. The variety of cytokines induced by interaction of Mtb with macrophages can then act on other cells within the granuloma, including macrophages, to induce various functional and phenotypic changes in cells that then modulate the environment of the granuloma.
In recent years, the complexity of macrophage populations has gained appreciation.49, 50 For ease of discussion, macrophages differentiated in response to cytokine signals have been termed either classically activated macrophages (CAMs) or alternatively activated macrophages (AAMs).49, 50, 51, 52 CAMs arise in response to TH1 T-cell signals (interferon-γ and TNF). These macrophages produce proinflammatory cytokines (TNF and IL-12) and chemokines and are capable of killing bacilli; in mice, a marker for CAM is inducible nitric oxide synthase (iNOS). iNOS uses arginine as a substrate for production of nitric oxide that can kill Mtb. In mice, iNOS is essential for control of Mtb infection.53, 54, 55 iNOS expression in human tuberculous lung macrophages has been reported,56, 57 and we have detected iNOS expression in macrophages in macaque granulomas (J.T. Mattila and J.L. Flynn, personal communication).
AAMs are anti-inflammatory in nature, and were initially described as arising in response to TH2 cytokines IL-13 and IL-4.50, 51 These macrophages can produce IL-10, TGF-β, and IL-6. In a TH2 environment, induction of the AAM phenotype is STAT-6 (signal transducer and activation of transcription 6) dependent.51 There are a set of genes and proteins used to characterize AAMs, with the primary marker being arginase.51 Arginase also uses arginine as a substrate and directly competes with iNOS for arginine, making the relative expression of these genes in a macrophage an important balancing feature for whether the macrophage will be pro- or anti-inflammatory, and directly affects the ability of a macrophage to kill Mtb (Figure 1).
There are several recent studies of AAMs in tuberculosis. Unlike parasitic and worm diseases, or asthma, where AAMs have been predominantly studied, tuberculosis induces a TH1-mediated immune response. It is difficult to measure IL-4 or IL-13 in tuberculous granulomas, and interruption of these genes in mice has little effect on Mtb infections, although there are a few reports that these cytokines can interfere with adequate control of tuberculosis.58, 59, 60 The generation of AAMs in tuberculous (TH1) granulomas appears to have a different mechanism. Mtb induces arginase (Arg1) gene expression in a MyD88-dependent but STAT-6-independent fashion in murine macrophages.36 This Arg1 induction by mycobacteria was mediated by Toll-like receptor-induced IL-6, IL-10, and granulocyte colony-stimulating factor production by macrophages.61 However, only a subset of AAM markers were induced by these cytokines, suggesting perhaps an intermediate AAM phenotype compared with a TH2 environment. Other studies using a mouse that overexpressed IL-10 from macrophages supported that IL-10 can strongly induce arginase expression in the lungs of Mtb-infected mice.61 The latter study also suggested that IL-10 enhanced the sensitivity of macrophages to IL-4, exacerbating induction of AAMs even in the presence of very low IL-4 levels, as might occur in a granuloma. These mice had higher numbers of Mtb in the lungs, which was correlated with increased AAMs. Mice lacking arginase specifically in macrophages controlled Mtb infection better than wild-type mice, and Arg1−/− macrophages had enhanced iNOS expression and increased killing of Mtb in vitro. Thus, although Mtb appears to have a different mechanism for induction of arginase than a TH2-mediated disease, arginase and AAM appear to inhibit control of Mtb infection.
Some studies have suggested that alveolar macrophages are inherently alternatively activated, and may allow Mtb bacilli to gain a foothold immediately upon entering the airway, as they are impaired in their ability to kill bacilli.15 Gordon and Martinez51 have suggested that true AAMs require a signal of “activation” to attain the qualities of AAMs, and hence although alveolar macrophages before infection are not classically activated, they may not be true AAMs, either. There is clearly a spectrum of activation for macrophages, and incompletely activated cells may possess some but not all qualities of AAMs or CAMs, depending on the local cytokine environment.
Bacterial Killing vs. Pathology: Balance of Responses in the Granuloma
The battle for control of Mtb infection occurs in granulomas, and the mechanisms that contribute to bacterial killing can also contribute to pathology. Excessive pathology also results in disease exacerbation. With a focus on macrophages, one can consider the balance of CAMs and AAMs to be crucial to the successful granuloma (Figure 1). Whereas CAMs are required for killing bacilli, the production of proinflammatory mediators and the continued recruitment and stimulation of T cells can lead to tissue damage and poor resolution of granulomas. Conversely, mouse data suggest that a granuloma with a substantial representation of AAMs would impair killing of bacteria, even while dampening inflammation and T-cell proliferation. The balance of CAMs and AAMs in a granuloma may be necessary to control infection and tissue damage. It also may be that CAMs and AAMs are spatially located differently in the human granuloma and play both roles—microbial killing and T-cell recruitment and activation where bacteria are more plentiful and downregulation of the T-cell environment where necessary to prevent tissue damage. Changes to location or numbers of macrophage types could affect the balance of the granuloma and lead to increased pathology or decreased bacterial killing (Figure 1). Location differences would not be apparent from the murine studies, as these granulomas have little of the organized structure of human granulomas.
What Factors Might Contribute to the Balance of AAM and CAM?
Macrophages can differentiate in response to many factors, including cytokines, direct cell-to-cell contact with T cells, antibodies from B cells, and microbial factors (interacting through pattern recognition receptors). These factors in aggregate likely affect the balance of inflammation in a single granuloma. Because the factors that control inflammation are dynamic, each granuloma in a host could act independently in terms of inflammation and bacterial numbers; data from the macaque model supports this (P.L. Lin and J.L. Flynn, unpublished data).
T cells
T-cell responses are primary players in the inflammatory balance in the granuloma.62, 63 This includes cytotoxic T cells (which can kill infected cells), TH1 T cells that produce combinations of IL-2, interferon-γ, and TNF,64 TH17 cells producing IL-17, and regulatory T cells (Tregs) that can produce IL-10 or TGF-β and inhibit proliferation and cytokine production by other cells. It is not clear what controls the balance of T cells within a granuloma, and how dynamic the changes are over the course of infection. There is a strong TH1 response in most people infected with Mtb, regardless of whether they develop active disease or latent infection. Recent intriguing data demonstrated that the immunodominant T-cell epitopes are conserved in Mtb strains,65 leading to speculation that it is to the advantage of the bacillus to induce strong T-cell responses. Mtb heat-shock protein 70 can interact with the CD40 receptor on dendritic cells, leading to increased IL-12 production and TH1 responses,66 again supporting that Mtb has evolved mechanisms for driving strong T-cell responses.67 Robust T-cell responses are linked to cavitary disease,68, 69, 70 a form of tuberculosis in which a granuloma is in direct contact with an airway, allowing bacteria to be more easily transmitted to a new host. Thus, regulation of TH1 responses may be necessary for optimal control of the infection and pathology.
TH17 responses in mice precede a strong TH1 response in the lungs, and increased TH17 cells can lead to enhanced recruitment of TH1 cells.71, 72, 73 This appears to be important in vaccine-induced control of Mtb in mice,73 but the long-term role for TH17 cells in inducing or recruiting TH1 cells, and the effect this may have on the inflammatory balance in the granuloma in humans is not known. IL-17 also contributes to neutrophil recruitment in other systems, and neutrophils can increase the inflammatory nature of a granuloma. Excessive neutrophils have been implicated in active tuberculosis in humans.74 The data for the importance of TH17 cells in human tuberculosis are scarce so far (reviewed in ref. 75); BCG immunization does induce both TH1 and TH17 cells,76 but whether these are necessary for protection or contribute to pathology is not clear.
CD4+Foxp3+ Treg cells are important contributors to dampening inflammation. These cells are present in the granuloma of humans, non-human primates, and mice.77, 78, 79 The loss of Foxp3+ Tregs in mice leads to higher bacterial loads.79 However, modulation of the Treg population in certain mice leads to increased mortality because of enhanced inflammation in the lungs.80 Tregs are good candidates for balancing immune responses through their interactions with T cells and necessary for preventing autoimmune diseases. Although Tregs are often only considered in their capacity to downregulate effector T-cell responses, and therefore exacerbate the infection, in chronic or persistent infections, these cells may be crucial players in preventing pathology. In macaques, Tregs rapidly left the blood and appeared in the airways following Mtb infection.78 Surprisingly, those monkeys with high levels of Tregs in blood before infection (presumably resulting in higher levels in lungs postinfection) were more likely to develop latent, rather than active tuberculosis. Thus, these cells may modulate the granuloma environment, and downregulate inflammation, which somehow contributes to the success of the granuloma in containing the infection (Figure 1).
The importance of regulating the T-cell response to control granulomatous inflammation is also demonstrated by the phenotype of programmed death-1 (PD-1) knockout mice. PD-1 is an exhaustion marker for T cells and engagement of PD-1 inhibits T-cell responses. In PD-1-deficient mice, the effector CD4 T-cell response was substantially enhanced, but the mice succumbed quickly because of increased pathology and higher bacterial load.81, 82 The mechanisms by which this occurs in the PD-1 knockout mice are not clear, and may be because of enhanced necrosis in the lungs due to strong T-cell responses, providing the right environment for robust growth of the bacilli. These data support that increased CD4 TH1 cells do not necessarily enhance control of infection, and that the lack of regulation of T cells by several different mechanisms exacerbates pathology.
B cells
B cells are a major cellular component of granulomas in humans, non-human primates, and mice infected with Mtb83, 84, 85, 86 (J.L. Flynn, J. Chan and J. Phuah, unpublished data). In Mtb-infected mice, B cells constitute 5–7% of total leukocytes present in lungs.84 They form discrete aggregates suggestive of tertiary lymphoid tissues with features of germinal center B cells,87, 88 which are in close proximity to macrophages84 (Figure 1). Emerging evidence in mice indicates that B cells are required for optimal immunity against Mtb, modulating susceptibility, cytokine production, histopathology, neutrophilic infiltration, as well as T-cell responses.89 How B cells regulate the immune response to Mtb is just beginning to be addressed. B cells can produce antibodies, cytokines, and present antigens,89 which potentially regulate other immune cells in the granuloma in a direct or indirect fashion. In particular, the macrophage is subject to regulation by B cells.
There are B-cell subsets with distinct immunologic function,90, 91, 92 including signature cytokine profiles, much like in the T-cell TH1/TH2 paradigm.90, 92 The functional relevance of the different cytokine profiles is underscored by the ability of distinct effector B-cell subsets to bias the development of T cells along the TH1 or TH2 lineage.90, 92 In infectious diseases model, AAM macrophages are conducive to persistence of certain pathogens.93 Recently, B1 cells, a subset of B lymphocytes, have been shown to promote the polarization of macrophages to a unique phenotype, including upregulation of IL-10 production, downregulation of TNF, IL-1β, and CCL3 (chemokine (C-C motif) ligand 3), as well as expression of typical AAM markers such as Ym1 and Fizz1.94 The key factor mediating polarization is IL-10.95 It is possible that by regulating macrophage functions, B cells can affect immune responses to the tubercle bacillus.
By virtue of their ability to produce antibodies, B cells are requisite to formation of immune complexes with potent immunoregulatory roles. For example, ligation of Fcγ receptors (FcγRs) on macrophages by immune complexes can have remarkable immunological effects. Ligation of FcγRs by antibody-coated Leishmania results in increased IL-10 and decreased IL-12 production by macrophages,96 enhancing leishmanial growth in macrophages. As a result, the phenomenon has been termed “antibody-dependent enhancement (ADE) of microbial infection.”96 ADE was originally observed in viral pathogens, most notably the Dengue virus,97, 98, 99, 100, 101 and can be dependent on the nature of the immune complex.102 Whether ADE is applicable to in vivo Mtb infection, where immune complexes are known to exist,103, 104 remains to be determined. Plasma cells, B cells that produce large quantities of antibodies, are found in macaque granulomas (J. Phuah and J.L. Flynn, unpublished data). Mice infected with monoclonal antibody-coated Mtb displayed improved outcome.105 The FcγRIIB-deficient knockout strain has increased control of Mtb infection, concomitant with an enhanced Th1 T-cell response.106 Furthermore, although immune complex engagement of activating FcγR has been reported to a major mechanism underlying IL-10-enhancing ADE, immune complex-treated Mtb-infected FcγRIIB knockout macrophages produce enhanced IL-12p40.106 Thus, through antibody production, B cells can modulate host immune responses by different mechanisms, one of which could be regulation of macrophage via FcgR engagement with immune complexes.
Through antibody production and modulation of macrophages, modulation of T cells,89, 91 as well as direct cytokine production, B cells have the ability to contribute to the inflammatory balance in the granuloma (Figure 1). Although neglected to date, the role of B cells in regulating the immune response during Mtb infection warrants further investigation.
Conclusions
Mtb orchestrates a complex set of immune responses in humans, with the most common outcome being lifetime control of the infection. However, when the balance of immune responses is disturbed, primary tuberculosis or reactivation of latent infection can occur. Here we explored the macrophage as a key mediator of inflammatory control in the granuloma, as it is the cell that interacts most frequently with the bacillus and the other key cells within the granuloma. Thus, it acts as the central control cell for events within the granuloma, dictating the outcome of infection. Strategies for modulating the macrophages may be useful in preventing disease, but must be approached carefully, as we do not understand the balance of cells and mediators necessary to kill bacilli, yet prevent lung pathology. These are important areas for further study.
References
Global Tuberculosis Control WHO Report 2010. ( World Health Organization, Geneva, 2010 ).
van Lettow, M., van der Meer, J.W., West, C.E., van Crevel, R. & Semba, R.D. Interleukin-6 and human immunodeficiency virus load, but not plasma leptin concentration, predict anorexia and wasting in adults with pulmonary tuberculosis in Malawi. J. Clin. Endocrinol. Metab. 90, 4771–4776 (2005).
Santucci, N. et al. A clinical correlate of the dysregulated immunoendocrine response in human tuberculosis. Neuroimmunomodulation 17, 184–187 (2010).
Lawn, S.D., Myer, L., Edwards, D., Bekker, L.G. & Wood, R. Short-term and long-term risk of tuberculosis associated with CD4 cell recovery during antiretroviral therapy in South Africa. AIDS 23, 1717–1725 (2009).
Lawn, S.D., Wilkinson, R.J., Lipman, M.C. & Wood, R. Immune reconstitution and “unmasking” of tuberculosis during antiretroviral therapy. Am. J. Respir. Crit. Care Med. 177, 680–685 (2008).
Meintjes, G. et al. Tuberculosis-associated immune reconstitution inflammatory syndrome: case definitions for use in resource-limited settings. Lancet Infect. Dis. 8, 516–523 (2008).
van Crevel, R., Ottenhoff, T.H. & van der Meer, J.W. Innate immunity to Mycobacterium tuberculosis. Clin. Microbiol. Rev. 15, 294–309 (2002).
Cooper, A.M., Solache, A. & Khader, S.A. Interleukin-12 and tuberculosis: an old story revisited. Curr. Opin. Immunol. 19, 441–447 (2007).
Clay, H., Volkman, H.E. & Ramakrishnan, L. Tumor necrosis factor signaling mediates resistance to mycobacteria by inhibiting bacterial growth and macrophage death. Immunity 29, 283–294 (2008).
Algood, H.M., Lin, P.L. & Flynn, J.L. Tumor necrosis factor and chemokine interactions in the formation and maintenance of granulomas in tuberculosis. Clin. Infect. Dis. 41 (Suppl 3), S189–S193 (2005).
Algood, H.M. et al. TNF influences chemokine expression of macrophages in vitro and that of CD11b+ cells in vivo during Mycobacterium tuberculosis infection. J. Immunol. 172, 6846–6857 (2004).
Ray, J.C., Flynn, J.L. & Kirschner, D.E. Synergy between individual TNF-dependent functions determines granuloma performance for controlling Mycobacterium tuberculosis infection. J. Immunol. 182, 3706–3717 (2009).
Lee, J., Remold, H.G., Ieong, M.H. & Kornfeld, H. Macrophage apoptosis in response to high intracellular burden of Mycobacterium tuberculosis is mediated by a novel caspase-independent pathway. J. Immunol. 176, 4267–4274 (2006).
Marino, S., Myers, A., Flynn, J.L. & Kirschner, D.E. TNF and IL-10 are major factors in modulation of the phagocytic cell environment in lung and lymph node in tuberculosis: a next-generation two-compartmental model. J. Theor. Biol. 265, 586–598 (2010).
Day, J., Friedman, A. & Schlesinger, L.S. Modeling the immune rheostat of macrophages in the lung in response to infection. Proc. Natl. Acad. Sci. USA 106, 11246–11251 (2009).
Davis, J.M. et al. Real-time visualization of mycobacterium-macrophage interactions leading to initiation of granuloma formation in zebrafish embryos. Immunity 17, 693–702 (2002).
Clay, H. et al. Dichotomous role of the macrophage in early Mycobacterium marinum infection of the zebrafish. Cell Host Microbe 2, 29–39 (2007).
Davis, J.M. & Ramakrishnan, L. The role of the granuloma in expansion and dissemination of early tuberculous infection. Cell 136, 37–49 (2009).
Wolf, A.J. et al. Mycobacterium tuberculosis infects dendritic cells with high frequency and impairs their function in vivo. J. Immunol. 179, 2509–2519 (2007).
Chackerian, A.A., Alt, J.M., Perera, T.V., Dascher, C.C. & Behar, S.M. Dissemination of Mycobacterium tuberculosis is influenced by host factors and precedes the initiation of T-cell immunity. Infect. Immun. 70, 4501–4509 (2002).
Lin, P.L. et al. Early events in Mycobacterium tuberculosis infection in cynomolgus macaques. Infect. Immun. 74, 3790–3803 (2006).
Wolf, A.J. et al. Initiation of the adaptive immune response to Mycobacterium tuberculosis depends on antigen production in the local lymph node, not the lungs. J. Exp. Med. 205, 105–115 (2008).
Winslow, G.M., Cooper, A., Reiley, W., Chatterjee, M. & Woodland, D.L. Early T-cell responses in tuberculosis immunity. Immunol. Rev. 225, 284–299 (2008).
Flynn, J.L. & Klein, E. “Pulmonary Tuberculosis in Monkeys” in A Color Atlas of Comparative Pulmonary Tuberculosis Histopathology (Leong, J., Datois, V., Dick T., eds) p83–p106, Taylor & Francis Publishers: Boca Raton, FL (2011).
Flynn, J.L., Tsenova, L., Izzo, A. & Kaplan, G. “Experimental animal models of tuberculosis” in Handbook of Tuberculosis: Immunology and Cell Biology, (Kaufmann, S.H.E., Britton W.J., eds) pp 389–417, Wiley-VCH, Weinheim, Vol. 2 (2008).
Pichugin, A.V., Yan, B.S., Sloutsky, A., Kobzik, L. & Kramnik, I. Dominant role of the sst1 locus in pathogenesis of necrotizing lung granulomas during chronic tuberculosis infection and reactivation in genetically resistant hosts. Am. J. Pathol. 174, 2190–2201 (2009).
Pozos, T.C. & Ramakrishnan, L. New models for the study of Mycobacterium-host interactions. Curr. Opin. Immunol. 16, 499–505 (2004).
Tobin, D.M. et al. The lta4h locus modulates susceptibility to mycobacterial infection in zebrafish and humans. Cell 140, 717–730 (2010).
Lin, P.L. et al. TNF neutralization results in disseminated disease during acute and latent M. tuberculosis infection with normal granuloma structure. Arthritis Rheum. 62, 340–350 (2010).
Lin, P.L. et al. Quantitative comparison of active and latent tuberculosis in the cynomolgus macaque model. Infect. Immun. 77, 4631–4642 (2009).
Mehra, S. et al. Transcriptional reprogramming in nonhuman primate (rhesus macaque) tuberculosis granulomas. PLoS One 5, e12266 (2010).
Langermans, J.A. et al. Divergent effect of bacillus Calmette-Guerin (BCG) vaccination on Mycobacterium tuberculosis infection in highly related macaque species: implications for primate models in tuberculosis vaccine research. Proc. Natl. Acad. Sci. USA 98, 11497–11502 (2001).
Chen, C.Y. et al. A critical role for CD8 T cells in a nonhuman primate model of tuberculosis. PLoS Pathog. 5, e1000392 (2009).
Fallahi-Sichani, M., El-Kebir, M., Marino, S., Kirschner, D.E. & Linderman, J.J. Multiscale computational modeling reveals a critical role for TNF-α receptor 1 dynamics in tuberculosis granuloma formation. J. Immunol. 186, 3472–3483 (2011).
Drage, M.G. et al. TLR2 and its co-receptors determine responses of macrophages and dendritic cells to lipoproteins of Mycobacterium tuberculosis. Cell. Immunol. 258, 29–37 (2009).
El Kasmi, K.C. et al. Toll-like receptor-induced arginase 1 in macrophages thwarts effective immunity against intracellular pathogens. Nat. Immunol. 9, 1399–1406 (2008).
Velez, D.R. et al. Variants in toll-like receptors 2 and 9 influence susceptibility to pulmonary tuberculosis in Caucasians, African-Americans, and West Africans. Hum. Genet. 127, 65–73 (2010).
Ito, T. et al. TLR9 activation is a key event for the maintenance of a mycobacterial antigen-elicited pulmonary granulomatous response. Eur. J. Immunol. 37, 2847–2855 (2007).
Numata, K. et al. Overexpression of suppressor of cytokine signaling-3 in T cells exacerbates acetaminophen-induced hepatotoxicity. J. Immunol. 178, 3777–3785 (2007).
Pompei, L. et al. Disparity in IL-12 release in dendritic cells and macrophages in response to Mycobacterium tuberculosis is due to use of distinct TLRs. J. Immunol. 178, 5192–5199 (2007).
Hawn, T.R. et al. A common human TLR1 polymorphism regulates the innate immune response to lipopeptides. Eur. J. Immunol. 37, 2280–2289 (2007).
Thuong, N.T. et al. A polymorphism in human TLR2 is associated with increased susceptibility to tuberculous meningitis. Genes Immun. 8, 422–428 (2007).
van der Wel, N. et al. M. tuberculosis and M. leprae translocate from the phagolysosome to the cytosol in myeloid cells. Cell 129, 1287–1298 (2007).
McDonough, K.A., Kress, Y. & Bloom, B.R. Pathogenesis of tuberculosis: interaction of Mycobacterium tuberculosis with macrophages. Infect. Immun. 61, 2763–2773 (1993).
Carlsson, F. et al. Host-detrimental role of Esx-1-mediated inflammasome activation in mycobacterial infection. PLoS Pathog. 6, e1000895 (2010).
Leber, J.H. et al. Distinct TLR- and NLR-mediated transcriptional responses to an intracellular pathogen. PLoS Pathog. 4, e6 (2008).
McElvania Tekippe, E. et al. Granuloma formation and host defense in chronic Mycobacterium tuberculosis infection requires PYCARD/ASC but not NLRP3 or caspase-1. PLoS One 5, e12320 (2010).
DiGiuseppe Champion, P.A., Champion, M.M., Manzanillo, P. & Cox, J.S. ESX-1 secreted virulence factors are recognized by multiple cytosolic AAA ATPases in pathogenic mycobacteria. Mol. Microbiol. 73, 950–962 (2009).
Gordon, S. & Taylor, P.R. Monocyte and macrophage heterogeneity. Nat. Rev. Immunol. 5, 953–964 (2005).
Martinez, F.O., Sica, A., Mantovani, A. & Locati, M. Macrophage activation and polarization. Front. Biosci. 13, 453–461 (2008).
Gordon, S. & Martinez, F.O. Alternative activation of macrophages: mechanism and functions. Immunity 32, 593–604 (2010).
Martinez, F.O., Helming, L. & Gordon, S. Alternative activation of macrophages: an immunologic functional perspective. Annu. Rev. Immunol. 27, 451–483 (2009).
MacMicking, J.D. et al. Identification of nitric oxide synthase as a protective locus against tuberculosis. Proc. Natl. Acad. Sci. USA 94, 5243–5248 (1997).
Flynn, J.L., Scanga, C.A., Tanaka, K.E. & Chan, J. Effects of aminoguanidine on latent murine tuberculosis. J. Immunol. 160, 1796–1803 (1998).
Scanga, C.A. et al. The inducible nitric oxide synthase locus confers protection against aerogenic challenge of both clinical and laboratory strains of Mycobacterium tuberculosis in mice. Infect. Immun. 69, 7711–7717 (2001).
Nathan, C. Inducible nitric oxide synthase in the tuberculous human lung. Am. J. Respir. Crit. Care Med. 166, 130–131 (2002).
Choi, H.S., Rai, P.R., Chu, H.W., Cool, C. & Chan, E.D. Analysis of nitric oxide synthase and nitrotyrosine expression in human pulmonary tuberculosis. Am. J. Respir. Crit. Care Med. 166, 178–186 (2002).
Harris, J. et al. T helper 2 cytokines inhibit autophagic control of intracellular Mycobacterium tuberculosis. Immunity 27, 505–517 (2007).
Buccheri, S. et al. IL-4 depletion enhances host resistance and passive IgA protection against tuberculosis infection in BALB/c mice. Eur. J. Immunol. 37, 729–737 (2007).
Roy, E., Brennan, J., Jolles, S. & Lowrie, D.B. Beneficial effect of anti-interleukin-4 antibody when administered in a murine model of tuberculosis infection. Tuberculosis (Edinb) 88, 197–202 (2008).
Qualls, J.E. et al. Arginine usage in mycobacteria-infected macrophages depends on autocrine-paracrine cytokine signaling. Sci. Signal 3, ra62 (2010).
Cooper, A.M. Cell-mediated immune responses in tuberculosis. Annu. Rev. Immunol. 27, 393–422 (2009).
Cooper, A.M. & Khader, S.A. The role of cytokines in the initiation, expansion, and control of cellular immunity to tuberculosis. Immunol. Rev. 226, 191–204 (2008).
Mattila, J.T., Diedrich, C.R., Lin, P.L., Phuah, J. & Flynn, J.L. Simian immunodeficiency virus-induced changes in T cell cytokine responses in cynomolgus macaques with latent Mycobacterium tuberculosis infection are associated with timing of reactivation. J. Immunol. 186, 3527–3537 (2011).
Comas, I. et al. Human T cell epitopes of Mycobacterium tuberculosis are evolutionarily hyperconserved. Nat. Genet. 42, 498–503 (2010).
Lazarevic, V., Myers, A.J., Scanga, C.A. & Flynn, J.L. CD40, but not CD40L, is required for the optimal priming of T cells and control of aerosol M. tuberculosis infection. Immunity 19, 823–835 (2003).
Flynn, J.L. & Chan, J. What's good for the host is good for the bug. Trends Microbiol. 13, 98–102 (2005).
Jones, B.E. et al. Chest radiographic findings in patients with tuberculosis with recent or remote infection. Am. J. Respir. Crit. Care Med. 156, 1270–1273 (1997).
Jones, B.E. et al. CD4 cell counts in human immunodeficiency virus-negative patients with tuberculosis. Clin. Infect. Dis. 24, 988–991 (1997).
Perlman, D.C. et al. Variation of chest radiographic patterns in pulmonary tuberculosis by degree of human immunodeficiency virus-related immunosuppression. The Terry Beirn Community Programs for Clinical Research on AIDS (CPCRA). The AIDS Clinical Trials Group (ACTG). Clin. Infect. Dis. 25, 242–246 (1997).
Lin, Y. et al. Interleukin-17 is required for T helper 1 cell immunity and host resistance to the intracellular pathogen Francisella tularensis. Immunity 31, 799–810 (2009).
Khader, S.A., Gaffen, S.L. & Kolls, J.K. Th17 cells at the crossroads of innate and adaptive immunity against infectious diseases at the mucosa. Mucosal Immunol. 2, 403–411 (2009).
Khader, S.A. et al. IL-23 and IL-17 in the establishment of protective pulmonary CD4+ T cell responses after vaccination and during Mycobacterium tuberculosis challenge. Nat. Immunol. 8, 369–377 (2007).
Berry, M.P. et al. An interferon-inducible neutrophil-driven blood transcriptional signature in human tuberculosis. Nature 466, 973–977 (2010).
Cooper, A.M. Editorial: Be careful what you ask for: is the presence of IL-17 indicative of immunity? J. Leukoc. Biol. 88, 221–223 (2010).
Burl, S. et al. Delaying bacillus Calmette-Guerin vaccination from birth to 4 1/2 months of age reduces postvaccination Th1 and IL-17 responses but leads to comparable mycobacterial responses at 9 months of age. J. Immunol. 185, 2620–2628 (2010).
Rahman, S. et al. Compartmentalization of immune responses in human tuberculosis: few CD8+ effector T cells but elevated levels of FoxP3+ regulatory t cells in the granulomatous lesions. Am. J. Pathol. 174, 2211–2224 (2009).
Green, A.M. et al. CD4(+) regulatory T cells in a cynomolgus macaque model of Mycobacterium tuberculosis infection. J. Infect. Dis. 202, 533–541 (2010).
Scott-Browne, J. et al. Expansion and function of Foxp3-expressing T regulatory cells in tuberculosis. J. Exp. Med. 204, 2159–2169 (2007).
Windish, H.P. et al. Aberrant TGF-beta signaling reduces T regulatory cells in ICAM-1-deficient mice, increasing the inflammatory response to Mycobacterium tuberculosis. J. Leukoc. Biol. 86, 713–725 (2009).
Lazar-Molnar, E. et al. Programmed death-1 (PD-1)-deficient mice, are extraordinarily sensitive to tuberculosis. Proc. Natl. Acad. Sci. USA 107, 13402–13407 (2010).
Barber, D.L., Mayer-Barber, K.D., Feng, C.G., Sharpe, A.H. & Sher, A. CD4 T cells promote rather than control tuberculosis in the absence of PD-1-mediated inhibition. J. Immunol. 186, 1598–1607 (2011).
Gonzalez-Juarrero, M. et al. Temporal and spatial arrangement of lymphocytes within lung granulomas induced by aerosol infection with Mycobacterium tuberculosis. Infect. Immun. 69, 1722–1728 (2001).
Tsai, M.C. et al. Characterization of the tuberculous granuloma in murine and human lungs: cellular composition and relative tissue oxygen tension. Cell Microbiol. 8, 218–232 (2006).
Turner, J., Frank, A.A., Brooks, J.V., Gonzalez-Juarrero, M. & Orme, I.M. The progression of chronic tuberculosis in the mouse does not require the participation of B lymphocytes or interleukin-4. Exp. Gerontol. 36, 537–545 (2001).
Ulrichs, T. et al. Human tuberculous granulomas induce peripheral lymphoid follicle-like structures to orchestrate local host defence in the lung. J. Pathol. 204, 217–228 (2004).
Kahnert, A. et al. Mycobacterium tuberculosis triggers formation of lymphoid structure in murine lungs. J. Infect. Dis. 195, 46–54 (2007).
Maglione, P.J., Xu, J. & Chan, J. B cells moderate inflammatory progression and enhance bacterial containment upon pulmonary challenge with Mycobacterium tuberculosis. J. Immunol. 178, 7222–7234 (2007).
Maglione, P.J. & Chan, J. How B cells shape the immune response against Mycobacterium tuberculosis. Eur. J. Immunol. 39, 676–686 (2009).
Harris, D.P. et al. Reciprocal regulation of polarized cytokine production by effector B and T cells. Nat. Immunol. 1, 475–482 (2000).
Lund, F.E. & Randall, T.D. Effector and regulatory B cells: modulators of CD4(+) T cell immunity. Nat. Rev. Immunol. 10, 236–247 (2010).
Mosmann, T. Complexity or coherence? Cytokine secretion by B cells. Nat. Immunol. 1, 465–466 (2000).
Benoit, M., Desnues, B. & Mege, J.L. Macrophage polarization in bacterial infections. J. Immunol. 181, 3733–3739 (2008).
Wong, S.C. et al. Macrophage polarization to a unique phenotype driven by B cells. Eur. J. Immunol. 40, 2296–2307 (2010).
Davila, S. et al. Genetic association and expression studies indicate a role of toll-like receptor 8 in pulmonary tuberculosis. PLoS Genet. 4, e1000218 (2008).
Halstead, S.B., Mahalingam, S., Marovich, M.A., Ubol, S. & Mosser, D.M. Intrinsic antibody-dependent enhancement of microbial infection in macrophages: disease regulation by immune complexes. Lancet Infect. Dis. 10, 712–722 (2010).
Halstead, S.B., Chow, J.S. & Marchette, N.J. Immunological enhancement of dengue virus replication. Nat. New Biol. 243, 24–26 (1973).
Halstead, S.B. & O'Rourke, E.J. Dengue viruses and mononuclear phagocytes. I. Infection enhancement by non-neutralizing antibody. J. Exp. Med. 146, 201–217 (1977).
Halstead, S.B. & O'Rourke, E.J. Antibody-enhanced dengue virus infection in primate leukocytes. Nature 265, 739–741 (1977).
Kliks, S.C. & Halstead, S.B. An explanation for enhanced virus plaque formation in chick embryo cells. Nature 285, 504–505 (1980).
Kliks, S.C. & Halstead, S.B. Role of antibodies and host cells in plaque enhancement of Murray Valley encephalitis virus. J. Virol. 46, 394–404 (1983).
Mahalingam, S. & Lidbury, B.A. Suppression of lipopolysaccharide-induced antiviral transcription factor (STAT-1 and NF-kappa B) complexes by antibody-dependent enhancement of macrophage infection by Ross River virus. Proc. Natl. Acad. Sci. USA 99, 13819–13824 (2002).
Brostoff, J., Lenzini, L., Rottoli, P. & Rottoli, L. Immune complexes in the spectrum of tuberculosis. Tubercle 62, 169–173 (1981).
Sai Baba, K.S., Moudgil, K.D., Jain, R.C. & Srivastava, L.M. Complement activation in pulmonary tuberculosis. Tubercle 71, 103–107 (1990).
Teitelbaum, R. et al. A mAb recognizing a surface antigen of Mycobacterium tuberculosis enhances host survival. Proc. Natl. Acad. Sci. USA 95, 15688–15693 (1998).
Maglione, P.J., Xu, J., Casadevall, A. & Chan, J. Fc gamma receptors regulate immune activation and susceptibility during Mycobacterium tuberculosis infection. J. Immunol. 180, 3329–3338 (2008).
Acknowledgements
We acknowledge support from the NIH (J.L.F.: AI37859, HL092883; J.L.F. and J.C.: AI50732, HL71241) and the Bill and Melinda Gates Foundation (J.L.F. and P.L.L.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declared no conflict of interest.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Flynn, J., Chan, J. & Lin, P. Macrophages and control of granulomatous inflammation in tuberculosis. Mucosal Immunol 4, 271–278 (2011). https://doi.org/10.1038/mi.2011.14
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mi.2011.14
This article is cited by
-
The 1, 2-ethylenediamine SQ109 protects against tuberculosis by promoting M1 macrophage polarization through the p38 MAPK pathway
Communications Biology (2022)
-
A meta-analysis of Th1 and Th2 cytokine profiles differentiating tuberculous from malignant pleural effusion
Scientific Reports (2022)
-
Management of Sarcoidosis: When to Treat, How to Treat and for How Long?
Current Pulmonology Reports (2022)
-
Telomere length and outcome of treatment for pulmonary tuberculosis in a gold mining community
Scientific Reports (2021)
-
Different macrophage polarization between drug-susceptible and multidrug-resistant pulmonary tuberculosis
BMC Infectious Diseases (2020)