Abstract
The transmembrane glycoprotein CD98 regulates integrin signaling that in turn controls cell proliferation and survival. CD98 expression is upregulated in various carcinomas, including colorectal cancer. Recently, by generating gain- and loss-of-function mouse models featuring genetic manipulation of CD98 expression specifically in intestinal epithelial cells (IECs), we have explored the crucial role of CD98 in the regulation of intestinal homeostasis and inflammation-associated tumorigenesis. In the present study, we investigated the contribution of CD98 to intestinal tumorigenesis in ApcMin/+ mice and the underlying mechanism of action. Mice featuring IEC-specific CD98 overexpression (Tg animals) were crossed with ApcMin/+ mice, and the characteristics of intestinal adenoma formation were assessed. Compared with ApcMin/+ mice, Tg/ApcMin/+ animals exhibited increases in both intestinal tumor incidence and tumor size; these parameters correlated with enhanced proliferation and decreased apoptosis of IECs. IEC-specific CD98 overexpression resulted in increased synthesis of the oncogenic proteins c-myc and cyclin-D1 in ApcMin/+ mice, independently of the Wnt-APC-β-catenin pathway, suggesting the implication of CD98 overexpression-mediated Erk activation. IEC-specific CD98 overexpression enhanced the production of proinflammatory cytokines and chemokines that are crucial for tumorigenesis. We validated our results in mice exhibiting IEC-specific CD98 downregulation (CD98flox/+VillinCre animals). IEC-specific CD98 downregulation efficiently attenuated tumor incidence and growth in ApcMin/+ mice. The reduction of intestinal tumorigenesis upon IEC-specific CD98 downregulation was caused by the attenuation of IEC proliferation and cytokine/chemokine production. In conclusion, we show that CD98 exerts an oncogenic activity in terms of intestinal tumorigenesis, via an ability to regulate tumor growth and survival.
Similar content being viewed by others
Main
The transmembrane glycoprotein CD98 associates with integrin β1 subunits, thereby regulating integrin signaling that in turn controls cell proliferation, survival, migration, and epithelial adhesion/polarity.1, 2, 3 Expression of the transmembrane glycoprotein CD98, encoded by SLC3A2, is increased in various carcinomas.4, 5, 6, 7 Recently, we generated both gain- and loss-of-function mouse models featuring genetic manipulation of CD98 expression specifically in intestinal epithelial cells (IECs), and explored the roles of CD98 in intestinal homeostasis, inflammation, and colitis-associated tumorigenesis.8
The adenomatous polyposis coli (APC) gene is critical for initiation of colorectal cancer (CRC), one of the most common malignancies worldwide.9 APC is mutated in >95% of familial adenomatous polyposis patients, and in 80% of those with sporadic CRC.10 The ApcMin/+ mouse, which contains a germline mutation in APC, serves as an animal model of human familial adenomatous polyposis.11 ApcMin/+ mice spontaneously develop numerous adenomas in the small intestine.12 APC is involved in the action of the Wnt-β-catenin signaling pathway and, importantly, regulates proliferation of intestinal crypt epithelia. In the absence of Wnt signaling, APC permits phosphorylation of β-catenin, leading to ubiquitination and degradation of the latter protein.13 In the early stages of intestinal tumorigenesis, mutational inactivation of APC both stabilizes and facilitates nuclear accumulation of β-catenin.14 In the nucleus, β-catenin forms a complex with T-cell factor (TCF); this complex in turn activates oncogenes including c-myc15 and cyclin D1.16, 17
In the present study, we used two genetically manipulated mouse strains8 that exhibit either IEC-specific CD98 overexpression or downregulation. We investigated the role shown by CD98, and its mechanism(s) of action, in intestinal tumorigenesis in ApcMin/+ mice.
MATERIALS AND METHODS
Mice
CD98 transgenic (Tg) and CD98f/+VillinCre (CD98f/+VC) mice were previously generated.8 Founder C57BL/6J male mice heterozygous for the ApcMin allele (ApcMin/+) were purchased from the Jackson Laboratory. Tg mice were congenically rebred to C57Bl/6 (Jackson Laboratories) for eight generations. Tg females were mated with ApcMin/+ males to generate wild-type (WT), Tg, ApcMin/+, and Tg/ApcMin/+ mice. CD98f/+VC females were mated with ApcMin/+ males to generate CD98f/+, CD98f/+VC, CD98f/+/ApcMin/+, and CD98f/+VC/ApcMin/+ mice. Mice were maintained in standard cages and were allowed standard chow and tap water ad libitum. All animal procedures were in accordance with the Emory University Institutional Animal Care and Use Committee.
Tumor Assessment
Mice were sacrificed at 16 weeks of age by CO2 asphyxiation. The entire small intestine and colon were dissected longitudinally. Intestinal tissues were examined under a dissecting microscope in a blinded fashion for the presence of adenomas. Intestinal adenomas were counted and grouped by size as follows: <1, 1–2, 2–3, and >3 mm.
Histology
Tissue sections were fixed in 10% formalin and embedded in paraffin. Sections of 5 μm were stained with H&E. Photomicrographs were taken using a Nikon Eclipse TS100 microscope.
Immunohistochemistry
Paraffin-embedded colonic sections of 5 μm were deparaffinized and antigen unmasking was performed by microwave treatment. Colonic sections were blocked in PBS with 10% normal goat serum for 30 min at 37°C, and then incubated with anti-Ki67 (Novocastra), anti-β-catenin (BD Biosciences) overnight at 4°C. After washes with PBS, tissues were treated with biotinylated secondary antibody (Vectastain Elite ABC kit, Vector Laboratories) for 1 h at room temperature. Sections were washed with PBS, incubated in the ABC reagent for 1 h at room temperature, washed again, and incubated with a peroxidase solution (Aminoethyl Carbazole Substrate Kit, Zymed). Sections were then counterstained with hematoxylin, dehydrated, and mounted in ProLong Gold (Invitrogen). Images were acquired using a Zeiss Axioskop 2 plus microscope equipped with an AxioCam MRc5 CCD camera (Zeiss).
TUNEL (Terminal Deoxynucleotidyl Transferase-Mediated Deoxyuridine Triphosphate Nick-End Labeling) Assay
Tissue sections were deparaffinized, and apoptotic cells were detected by immunofluorescent TUNEL using the In Situ Cell Death Detection Kit (Roche Applied Science). Nuclei were stained with 4′,6-diamidino-2-phenylindole (Invitrogen). Sections were mounted and photographed as described above.
Intestinal Epithelial Cell Isolation
Isolation of epithelial cells from jejunum or colon was performed as previously described.18, 19
Treatment of Caco2-BBE Cells with Lithium Chloride
The human intestinal epithelial Caco2-BBE cells were cultured as described previously.19, 20 Cells were serum starved overnight, and then treated with the canonical Wnt activator LiCl at 10 or 100 mM for 24 h. Untreated cells were used as controls. Cells were then washed, and the effect of LiCl-mediated Wnt pathway activation on levels of human CD98 or β-catenin (used as a positive control) was analyzed by western blot.
Western Blot
Cell lysates were resolved on polyacrylamide gels and transferred to nitrocellulose membranes (Bio-Rad). Membranes were probed with relevant primary antibodies followed by incubation with appropriate HRP-conjugated secondary antibodies (Amersham Biosciences). Blots were detected using the Enhanced Chemiluminescence Detection kit (Amersham Biosciences).
Quantitative Real-Time PCR (qRT-PCR)
Total RNA extracted using TRIzol (Invitrogen) was reverse transcribed using the first strand cDNA synthesis kit (Fermentas). qRT-PCR was performed using SYBR Green qPCR Master Mix (Fermentas) on a Mastercycler Realplex4 (Eppendorf). 36B4 was used as housekeeping gene. Fold-induction was calculated using the Ct method: ΔΔCt=(CtTarget gene−Cthousekeeping gene)treatment−(CtTarget gene−Cthousekeeping gene)non−treatment, and the final data were derived from 2−Ct. Primers used are as follows:
KC forward: 5′-TTGTGCGAAAAGAAGTGCAG-3′,
KC reverse: 5′-TACAAACACAGCCTCCCACA-3′;
IL-1β forward: 5′-TCGCTCAGGGTCACAAGAAA-3′,
IL-1β reverse: 5′-CATCAGAGGCAAGGAGGAAAAC-3′;
IL-6 forward: 5′-ACAAGTCGGAGGCTTAATTACACAT-3′,
IL-6 reverse: 5′- TTGCCATTGCACAACTCTTTT C-3′;
TNF-α forward: 5′-AGGCTGCCCCGACTACGT-3′,
TNF-α reverse: 5′-GACTTTCTCCTGGTATGAGATAGCA AA-3′;
Mouse CD98 forward: 5′-GAGGACAGGCTTTTGATTGC-3′,
Mouse CD98 reverse: 5′-ATTCAGTACGCTCCCCAGTG-3′;
CD98 forward: 5′-GCCGGTTCTGCAGGCACCAT-3′,
CD98 reverse: 5′-TCGGCTGCTTCTCGGGCTCT-3′;
Cyclin D1 forward: 5′-CAGACGTTCAGAACCAGATTC-3′,
Cyclin D1 reverse: 5′-CCCTCCAATAGCAGCGAAAAC-3′;
36B4 forward: 5′-TCCAGGCTTTGGGCATCA-3′,
36B4 reverse: 5′-CTTTATCAGCTGCACATCACTCAGA-3′.
Statistical Analysis
Values are expressed as mean±s.e.m. Statistical analysis was performed using unpaired two-tailed Student's t-test by the InStat v3.06 (GraphPad) software. P<0.05 was considered significant.
RESULTS
CD98 Expression is Increased in Intestinal Adenomas of ApcMin/+ Mice
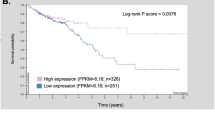
CD98 expression is upregulated in numerous cancers.4, 5, 6, 7 In the present report, we investigated whether CD98 expression was increased in intestinal adenomas developed in the well-established ApcMin/+ mouse model of intestinal tumorigenesis. Figure 1 shows that the levels of CD98 mRNA and protein expression increased in intestinal adenomas of ApcMin/+ mice compared with those in normal intestinal tissue of ApcMin/+ animals or intestinal epithelia of WT mice. No significant difference was found when CD98 expression levels in IECs derived from WT mice and non-tumor regions of ApcMin/+ animals were compared (Figure 1). This suggests that CD98 overexpression is specifically associated with intestinal tumorigenesis in ApcMin/+ mice.
CD98 expression is increased in intestinal adenomas of ApcMin/+ mice. Adenomas were isolated using a dissecting microscope. Total RNA (a and b) and protein (c and d) were isolated from small intestinal (a and c) or colonic (b and d) epithelia of wild-type mice (WT) and ApcMin/+ animals, from either normal epithelia or adenomas. CD98 mRNA and protein expression levels were assessed by qRT-PCR (a and b) and western blotting (c and d), respectively. Data are mean±s.e.m. *P<0.05 vs WT.
As CD98 expression was upregulated in ApcMin/+ tumors, we tested the possibility that CD98 might function as a downstream target of Wnt/β-catenin pathway. For that, intestinal epithelial Caco2-BBE cells were treated with LiCl, which has been used as an activator of canonical Wnt signaling by acting through glycogen synthase kinase-3 beta inhibition.21, 22 As expected, LiCl treatment induced a stabilization and accumulation of β-catenin in Caco2-BBE cells at both 10 and 100 mM, indicating activation of Wnt pathway (Supplementary Figure S1). However, expression levels of human (h) CD98 in Caco2-BBE cells remained unchanged upon LiCl treatment, even at 100 mM (Supplementary Figure S1). These data indicate that CD98 is not a direct downstream target of Wnt/β-catenin pathway.
IEC-Specific CD98 overexpression Increases Formation of Intestinal Adenomas in ApcMin/+ Mice
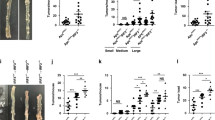
To explore the role of IEC-specific CD98 overexpression in ApcMin/+ mice, Tg animals were crossed with ApcMin/+ mice. Western blotting confirmed that hCD98 was expressed at high levels in small intestinal and colonic lysates from Tg/ApcMin/+ mice, whereas their control ApcMin/+ littermates did not express hCD98 (Figure 2a). In an effort to analyze the total expression levels of human (h) CD98 and endogenous murine (m) CD98 in ApcMin/+ and Tg/ApcMin/+ mice, we performed western blot analysis using an antibody that recognizes both hCD98 and mCD98. Our data showed a marked increase in total CD98 protein expression, including hCD98 and mCD98, in intestinal lysates from Tg/ApcMin/+ mice compared with ApcMin/+ mice (Figure 2b, upper panel). Analysis of total CD98 mRNA expression levels in intestinal lysates by qRT-PCR using specific primers recognizing both hCD98 and mCD98 transcripts showed a 21-fold increase in Tg/ApcMin/+ (21.15±5.56-fold) compared with ApcMin/+ mice (1-fold; Figure 2b, bottom panel). The extent of intestinal adenoma formation was determined at 16–18 weeks of age. As expected, all ApcMin/+ and Tg/ApcMin/+ mice developed tumors predominantly in the distal small intestine. The numbers of adenomas per animal in the small intestines of Tg/ApcMin/+ mice was 128±45, which was markedly greater than 54±21 adenomas in the ApcMin/+ group (Figure 2c). We also noted that the number of colonic adenomas was elevated in Tg/ApcMin/+ (3.1±0.4) vs ApcMin/+ (1.2±0.2) animals (Figure 2d). Analysis of total adenomas size (mm) developed in each mouse showed an increase in Tg/ApcMin/+ (200.5±54.1) compared with ApcMin/+ (75.1±23.5) group (Figure 2e). Examination of tumor size distribution revealed more tumors of larger size in Tg/ApcMin/+ mice compared with ApcMin/+ animals (Figure 2f). Histologically, the adenomas were consistently larger in small intestinal and colonic sections from Tg/ApcMin/+ mice compared with ApcMin/+ animals (Figure 2g). These findings indicated that CD98 expression in IECs regulates tumor development and progression in ApcMin/+ mice.
IEC-specific CD98 overexpression increases intestinal tumorigenesis in ApcMin/+ mice. Mice were sacrificed at 16 weeks of age, and tumor numbers and sizes were determined using a dissecting microscopy. (a) Human (h) CD98 expression in small intestinal or colonic lysates of ApcMin/+ and Tg/ApcMin/+ mice as determined by western blotting. (b) Total human and mouse CD98 expression in intestinal lysates of ApcMin/+ and Tg/ApcMin/+ mice analyzed by western blotting and qRT-PCR. The numbers of adenomas/mouse in the small intestine (c) and colon (d), as well as total adenomas size (mm) developed in each mouse (e) are shown. All data are mean±s.e.m. N=12 mice/group. (*P<0.05; **P<0.005) vs ApcMin/+. (f) The size distribution of intestinal adenomas. (g) The histology of representative tumors from the small intestine and colon.
IEC-Specific CD98 Overexpression Increases Cell Proliferation and Reduces Apoptosis in ApcMin/+ Mice
We recently showed that IEC-specific CD98 overexpression affects integrin signaling, leading to changes in cell proliferation and survival.8 As both cell proliferation and survival contribute to tumor growth, we investigated these properties in Tg/ApcMin/+ mice in comparison with ApcMin/+ animals to understand the mechanism underlying the effect of IEC-specific CD98 overexpression on tumor development. Immunohistological staining for Ki67 revealed a significant increase in the number of Ki67-positive epithelia in Tg/ApcMin/+ mice compared with ApcMin/+ animals, in both tumor and non-tumor regions (Figure 3a). Consistent with this result, we found a significant increase in cyclin D1 mRNA and protein levels in intestinal lysates from Tg/ApcMin/+ mice compared with ApcMin/+ animals (Figure 3b and c). Furthermore, expression levels of cyclin D1 were increased in Tg/ApcMin/+ compared with ApcMin/+ mice in both adenomas and normal epithelia (Figure 3d). In addition, Tg/ApcMin/+ mice exhibited decreased apoptosis of the intestinal epithelium, as revealed by lower TUNEL-positive cell numbers (Figure 4a), and increased phospho-Akt with reduced cleaved caspase 3 levels (Figure 4b). Thus, IEC-specific CD98 overexpression enhances tumor development in ApcMin/+ mice by promoting proliferation and decreasing apoptosis of IECs.
IEC-specific CD98 overexpression increases cell proliferation in ApcMin/+ mice. (a) Immunolabeling for Ki67 in jejunal sections of ApcMin/+ and Tg/ApcMin/+ mice. Cyclin D1 mRNA and protein levels in total intestinal mucosal lysates were analyzed by qRT-PCR (b) and western blot (c), respectively. *P<0.05 vs ApcMin/+. Cyclin D1 expression levels in normal epithelia and adenomas from ApcMin/+ and Tg/ApcMin/+ mice analyzed by western blot (d).
IEC-specific CD98 Overexpression Enhances Intestinal Tumorigenesis in ApcMin/+ Mice by Activating the MEK/ERK Signaling Pathway
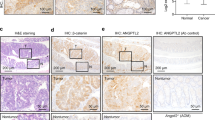
Transcription of c-myc is induced by activation of β-catenin, which is mediated by APC inactivation. As c-myc is known to be essential for tumorigenesis in ApcMin/+ mice, we tested the effect of IEC-specific CD98 expression on c-myc expression levels in this model. Immunoblotting revealed an increase in the level of c-myc expression in intestinal lysates from Tg/ApcMin/+ mice compared with ApcMin/+ animals (Figure 5a). Immunohistochemical staining for β-catenin yielded strong nuclear and cytoplasmic signals in intestinal tissues of ApcMin/+ and Tg/ApcMin/+ mice; the staining levels were similar (Figure 5b). Similar β-catenin expression levels in intestinal lysates from Tg/ApcMin/+ and ApcMin/+ mice were also observed by immunoblotting (Figure 5c). These results indicate that IEC-specific CD98 overexpression did not affect either the expression level or localization of β-catenin.
IEC-specific CD98 overexpression does not modulate either expression level or protein localization of β-catenin in ApcMin/+ mice. Expression levels of c-myc (a); β-catenin (c); and phospho-Erk and Erk (d), in intestinal lysates, were analyzed by western blotting. Immunohistochemical staining of β-catenin in sections of the small intestine from ApcMin/+ and Tg/ApcMin/+ animals (b).
It is known that the MEK-ERK pathway phosphorylates c-myc, thereby stabilizing c-myc by preventing it from ubiquitination and proteasomal degradation.23, 24, 25 It has recently been shown that ERK activation increases the level of c-myc protein and drives intestinal tumorigenesis in ApcMin/+ mice.26 We recently showed that IEC-specific CD98 overexpression increases activation of MEK-ERK signaling pathway.8 Therefore, we examined the levels of phospho-ERK in ApcMin/+ and Tg/ApcMin/+ mice. Figure 5d shows that, compared with ApcMin/+ mice, intestinal lysates of Tg/ApcMin/+ animals exhibited a marked increase in phospho-ERK level. Together, these data suggested that IEC-specific CD98 overexpression promotes tumorigenesis in the ApcMin/+ mouse model by activating the MEK-ERK signaling pathway, independently of the Wnt-APC-β-catenin pathway. However, we can not exclude the possibility that changes in phospho-ERK levels only reflect the changes in cycling cells in Tg/ApcMin/+ animals, and the cause-consequence relationships between tumorigenesis and ERK activation could not be definitely concluded and needs further studies.
IEC-Specific CD98 Overexpression Enhances Intestinal Tumorigenesis in ApcMin/+ Mice by Increasing Expression of Proinflammatory Cytokines and Chemokines
We further investigated the role shown by CD98 in intestinal tumorigenesis by analyzing the expression levels of proinflammatory cytokines and chemokines that can promote tumor development.27 Significant increases in the levels of mRNA encoding proinflammatory cytokines (TNF-α, IL-1β, and IL-6) and keratinocyte-derived chemokine (KC) were found in Tg/ApcMin/+ mice compared with ApcMin/+ animals (Figure 6). Overall, the results showed that IEC-specific CD98 overexpression enhances intestinal tumorigenesis in ApcMin/+ mice by increasing the expression levels of positive regulators of tumorigenesis.
IEC-specific CD98 overexpression increases expression of proinflammatory cytokines and chemokines in ApcMin/+ mice. The levels of mRNAs, in small intestinal extracts, encoding cytokines and chemokines, were analyzed by qRT-PCR. Data are mean±s.e.m. (n=8 mice/group). *P<0.05; **P<0.005 vs ApcMin/+ animals.
IEC-Specific CD98 Downregulation Decreases Intestinal Tumorigenesis in ApcMin/+ Mice by Reducing Cell Proliferation and Expression Levels of Cytokines and Chemokines
To confirm the role shown by CD98 in intestinal tumorigenesis in ApcMin/+ mice, we crossed such animals with CD98f/+VC mice having IEC-specific CD98 downregulation, which we recently generated.8 Compared with CD98f/+/ApcMin/+ mice, CD98f/+VC/ApcMin/+ animals developed a significantly decreased number of intestinal adenomas, as determined at 16–18 weeks of age (Figure 7a). Interestingly, only 42% of CD98f/+VC/ApcMin/+ mice (5/12 animals) developed tumors in the colon compared with 83% of CD98f/+/ApcMin/+ mice (10/12 animals; Figure 7b). Analysis of total adenomas size (mm) developed in each mouse showed a significant decrease in CD98f/+VC/ApcMin/+ (34.2±8.2) compared with CD98f/+/ApcMin/+ (63.1±10.6) group (Figure 7c), with more smaller tumors observed (Figure 7d).
IEC-specific CD98 downregulation attenuates intestinal tumorigenesis in ApcMin/+ mice via a decrease in IEC proliferation and reduced expression of cytokines and chemokines. CD98f/+/ApcMin/+ and CD98f/+VC/ApcMin/+ mice were sacrificed at 16 weeks of age, and tumor numbers and sizes were determined by microscopic dissection. The numbers of adenomas/mouse in the small intestine (a) and colon (b), as well as total adenomas size (mm) developed in each mouse (c) are shown. Data are mean±s.e.m. N=12 mice/group. *P<0.05 vs CD98f/+/ApcMin/+ mice. The size distributions of intestinal adenomas (N=12 mice/group) are also indicated (d). Ki67-specific immunolabeling of jejunal sections (e). The expression levels of cyclin D1 and c-myc in intestinal lysates were analyzed by western blotting (f). Cyclin D1 expression levels in normal epithelia (non-tumor region) from CD98f/+/ApcMin/+ and CD98f/+VC/ApcMin/+ mice were analyzed by western blot (g). The mRNA expression levels of cytokines and chemokines in small intestinal extracts were analyzed by qRT-PCR (h). Data are mean±s.e.m. (8 mice/group). *P<0.05; **P<0.005 vs CD98f/+/ApcMin/+ mice.
As expected, compared with CD98f/+/ApcMin/+ mice, CD98f/+VC/ApcMin/+ animals exhibited attenuated intestinal epithelial proliferation as shown by decreases in the numbers of Ki67-positive epithelia in both tumor and non-tumor regions (Figure 7e), and reduction of expression of both cyclin D1 and c-myc in intestinal lysates (Figure 7f). In addition, analysis of cyclin D1 expression levels in normal epithelia (non-tumor regions) showed a decrease in CD98f/+VC/ApcMin/+ compared with CD98f/+/ApcMin/+ mice (Figure 7g), suggesting that CD98 expression in IECs controls cyclin D1 expression, which consequently affects tumorigenesis in ApcMin/+ mice. Immunohistochemical staining for β-catenin did not reveal any difference in cytoplasmic or nuclear accumulation of β-catenin between CD98f/+/ApcMin/+ and CD98f/+VC/ApcMin/+ mice (data not shown), further confirming that intestinal CD98 modulates tumorigenesis in ApcMin/+ mice independently of the action of the Wnt-APC-β-catenin pathway. In addition, the levels of mRNA encoding the cytokines/chemokines TNF-α, IL-1β IL-6, and KC were significantly decreased in CD98f/+VC/ApcMin/+ compared with CD98f/+/ApcMin/+ mice (Figure 7h). Overall, the results showed that IEC-specific CD98 downregulation suppresses intestinal tumorigenesis in ApcMin/+ mice by inhibiting expression of positive regulators of tumorigenesis.
DISCUSSION
It is widely recognized that overt inflammation can promote neoplasia.28, 29 Recently, we generated gain- and loss-of-function mouse models featuring genetic manipulation of CD98 expression specifically in IECs, and showed that CD98 has a critical role in the regulation of intestinal homeostasis, inflammation, and inflammation-associated tumorigenesis. In the present study, we show that IEC-specific CD98 expression critically regulates intestinal tumorigenesis in the ApcMin/+ mouse model.
We recently assessed the role shown by intestinal CD98 in inflammation-induced tumorigenesis using a mouse model of colitis-associated cancer.8 We found that IEC-specific CD98 overexpression promoted colitis-associated tumorigenesis by stimulating cell proliferation and production of proinflammatory mediators.8 In the present study, we show that CD98 expression is upregulated in the intestinal adenomas of ApcMin/+ mice, which spontaneously develop colon cancer because of the presence of a germ-line mutation in the tumor suppressor APC gene. In addition, CD98 overexpression in IECs increased both tumor incidence and size in ApcMin/+ mice. It is worthy to note that Tg mice did not develop spontaneously intestinal adenomas. We further show that the effect of CD98 overexpression on intestinal tumorigenesis in ApcMin/+ mice could be explained by the fact that CD98 regulates cell proliferation and survival. Indeed, it has been shown that CD98 controls integrin signaling, which regulates cell proliferation, survival, migration, and epithelial adhesion/polarity,1, 2, 3 and has crucial roles in intestinal homeostasis and tumorigenesis in mice.8 In the present work, we observed that IEC-specific CD98 overexpression increased cell proliferation and reduced apoptosis in ApcMin/+ mice, with both of these effects contributed to intestinal tumorigenesis. We speculate that CD98 overexpression affects integrin signaling, which is accompanied by enhanced cell proliferation and survival; these are important aspects of the tumorigenic activity associated with IEC-specific CD98 overexpression in ApcMin/+ mice.
Accumulation of β-catenin in nuclei, via formation of the β-catenin/TCF complexes, activates various downstream targets including c-myc and cyclin D1. Herein, we show that IEC-specific CD98 overexpression increases tumorigenesis in ApcMin/+ mice in a manner independent of the action of the Wnt-APC-β-catenin pathway. It is known that activation of MEK-ERK pathway phosphorylate c-myc, thereby stabilizing c-myc by preventing ubiquitination and proteasomal degradation.23, 24, 25 It has also recently been shown that MyD88-dependent ERK activation increases the level of c-myc protein and drives intestinal tumorigenesis in ApcMin/+ mice. Therefore, our data suggest that CD98 overexpression increases synthesis of oncogenic c-myc via activation of ERK, although further studies on the role of ERK signaling pathway in CD98 effect on tumorigenesis in ApcMin/+ mice are needed to make a definite conclusion.
Another important finding of the present study is that production of proinflammatory cytokines and chemokines that critically contributes to tumor progression29 was enhanced in ApcMin/+ mice with IEC-specific CD98 overexpression (ApcMin/+/Tg). These data are consistent with our previous finding that IEC-specific CD98 overexpression enhanced colonic tumor incidence and growth by stimulating inflammation-induced production of proinflammatory cytokines/chemokines, including the critical regulators IL-6 and TNF-α. However, we can not exclude the possibility that the elevated proinflammatory cytokine/chemokine production could be a consequence of the increase in tumorigenesis in ApcMin/+/Tg mice.
Employing the IEC-specific CD98 loss-of-function mouse model that we generated recently,8 we validated the role of intestinal CD98 in modulating intestinal tumor development in ApcMin/+ mice. IEC-specific CD98 downregulation efficiently attenuated both tumor incidence and growth in such mice. The reducing effect on tumor incidence and tumor size during CAC development of IEC-specific CD98 downregulation was given by its capability to attenuate inflammation-associated cytokine/chemokine production and IEC proliferation, which is consistent with the mechanism underlying tumorigenic activity of IEC-specific CD98 overexpression.
In summary, our current findings, together with those of our previous study on the role shown by intestinal CD98 in regulation of intestinal homeostasis and inflammation-associated tumorigenesis,8 suggest that CD98 is an attractive target for the development of novel therapeutic drugs for prevention and treatment of CRC.
References
Fenczik CA, Sethi T, Ramos JW, et al. Complementation of dominant suppression implicates CD98 in integrin activation. Nature 1997;390:81–85.
Feral CC, Nishiya N, Fenczik CA, et al. CD98hc (SLC3A2) mediates integrin signaling. Proc Natl Acad Sci USA 2005;102:355–360.
Merlin D, Sitaraman S, Liu X, et al. CD98-mediated links between amino acid transport and beta 1 integrin distribution in polarized columnar epithelia. J Biol Chem 2001;276:39282–39289.
Esteban F, Ruiz-Cabello F, Concha A, et al. Relationship of 4F2 antigen with local growth and metastatic potential of squamous cell carcinoma of the larynx. Cancer 1990;66:1493–1498.
Esseghir S, Reis-Filho JS, Kennedy A, et al. Identification of transmembrane proteins as potential prognostic markers and therapeutic targets in breast cancer by a screen for signal sequence encoding transcripts. J Pathol 2006;210:420–430.
Prager GW, Poettler M, Schmidinger M, et al. CD98hc (SLC3A2), a novel marker in renal cell cancer. Eur J Clin Invest 2009;39:304–310.
Kaira K, Oriuchi N, Imai H, et al. l-Type amino acid transporter 1 and CD98 expression in primary and metastatic sites of human neoplasms. Cancer Sci 2008;99:2380–2386.
Nguyen HT, Dalmasso G, Torkvist L, et al. CD98 expression modulates intestinal homeostasis, inflammation, and colitis-associated cancer in mice. J Clin Invest 2011;121:1733–1747.
Weir HK, Thun MJ, Hankey BF, et al. Annual report to the nation on the status of cancer, 1975–2000, featuring the uses of surveillance data for cancer prevention and control. J Natl Cancer Inst 2003;95:1276–1299.
Laken SJ, Papadopoulos N, Petersen GM, et al. Analysis of masked mutations in familial adenomatous polyposis. Proc Natl Acad Sci USA 1999;96:2322–2326.
Oshima M, Oshima H, Kitagawa K, et al. Loss of Apc heterozygosity and abnormal tissue building in nascent intestinal polyps in mice carrying a truncated Apc gene. Proc Natl Acad Sci USA 1995;92:4482–4486.
Su LK, Kinzler KW, Vogelstein B, et al. Multiple intestinal neoplasia caused by a mutation in the murine homolog of the APC gene. Science 1992;256:668–670.
Rubinfeld B, Albert I, Porfiri E, et al. Binding of GSK3beta to the APC-beta-catenin complex and regulation of complex assembly. Science 1996;272:1023–1026.
Korinek V, Barker N, Morin PJ, et al. Constitutive transcriptional activation by a beta-catenin-Tcf complex in APC−/− colon carcinoma. Science 1997;275:1784–1787.
He TC, Sparks AB, Rago C, et al. Identification of c-MYC as a target of the APC pathway. Science 1998;281:1509–1512.
Shtutman M, Zhurinsky J, Simcha I, et al. The cyclin D1 gene is a target of the beta-catenin/LEF-1 pathway. Proc Natl Acad Sci USA 1999;96:5522–5527.
Tetsu O, McCormick F . Beta-catenin regulates expression of cyclin D1 in colon carcinoma cells. Nature 1999;398:422–426.
Flint N, Cove FL, Evans GS . A low-temperature method for the isolation of small-intestinal epithelium along the crypt-villus axis. Biochem J 1991;280 (Pt 2):331–334.
Nguyen HT, Dalmasso G, Yan Y, et al. MicroRNA-7 modulates CD98 expression during intestinal epithelial cell differentiation. J Biol Chem 2010;285:1479–1489.
Nguyen HT, Dalmasso G, Yan Y, et al. Ecto-phosphorylation of CD98 regulates cell-cell interactions. PLoS One 2008;3:e3895.
Klein PS, Melton DA . A molecular mechanism for the effect of lithium on development. Proc Natl Acad Sci USA 1996;93:8455–8459.
Le Floch N, Rivat C, De Wever O, et al. The proinvasive activity of Wnt-2 is mediated through a noncanonical Wnt pathway coupled to GSK-3beta and c-Jun/AP-1 signaling. FASEB J 2005;19:144–146.
Sears R, Nuckolls F, Haura E, et al. Multiple Ras-dependent phosphorylation pathways regulate Myc protein stability. Genes Dev 2000;14:2501–2514.
Sears RC . The life cycle of C-myc: from synthesis to degradation. Cell Cycle 2004;3:1133–1137.
Vervoorts J, Luscher-Firzlaff J, Luscher B . The ins and outs of MYC regulation by posttranslational mechanisms. J Biol Chem 2006;281:34725–34729.
Lee SH, Hu LL, Gonzalez-Navajas J, et al. ERK activation drives intestinal tumorigenesis in Apc(min/+) mice. Nat Med 2010;16:665–670.
Terzic J, Grivennikov S, Karin E, et al. Inflammation and colon cancer. Gastroenterology 2010;138:2101–2114 e2105.
Karin M, Lawrence T, Nizet V . Innate immunity gone awry: linking microbial infections to chronic inflammation and cancer. Cell 2006;124:823–835.
Coussens LM, Werb Z . Inflammation and cancer. Nature 2002;420:860–867.
Acknowledgements
This work was supported by grants from the Department of Veterans Affairs and the National Institutes of Health of Diabetes and Digestive and Kidney by the Grant RO1-DK-071594 (to DM), and the Crohn's and Colitis Foundation of America (research fellowship (2008–2010) award (to GD). We are grateful to Professor Yang Vincent (Emory University) for kindly providing ApcMin/+ mice, Dr Amr Ghaleb and Nandan Mandayam (Emory University) for technical advice. We dedicate this article in the memory of Professor Shanthi V Sitarman, a brilliant scientist, dedicated physician, passionate humanitarian, and dearest friend.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Laboratory Investigation website
CD98, a regulator of integrin signaling, is shown to play a crucial role in intestinal tumorigenesis due to its role in cell proliferation and survival and its ability to modulate the production of cytokines and chemokines. CD98 may be an attractive target for the development of therapeutic agents for prevention and treatment of colorectal cancer.
Supplementary information
Rights and permissions
About this article
Cite this article
Nguyen, H., Dalmasso, G., Yan, Y. et al. Intestinal epithelial cell-specific CD98 expression regulates tumorigenesis in ApcMin/+ mice. Lab Invest 92, 1203–1212 (2012). https://doi.org/10.1038/labinvest.2012.83
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2012.83
Keywords
This article is cited by
-
Overexpression of CD98 in intestinal epithelium dysregulates miRNAs and their targeted proteins along the ileal villus-crypt axis
Scientific Reports (2018)
-
Targeting Intestinal Inflammation With CD98 siRNA/PEI–loaded Nanoparticles
Molecular Therapy (2014)