Abstract
Objective:
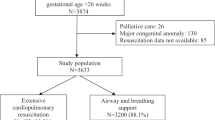
To evaluate risk factors and impact of delivery room cardiopulmonary resuscitation (DR-CPR) on very low birth weight (VLBW) preterm infants.
Study Design:
A national, population-based, observational study evaluating risk factors and short-term neonatal outcomes associated with DR-CPR among VLBW, extremely preterm infants (EPIs, 24 to 27 weeks’ gestation) and very preterm infants (VPI, 28 to 31 weeks’ gestation) born in 1995 to 2010.
Results:
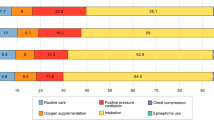
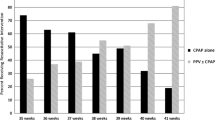
Among 17 564 VLBW infants, 636 (3.6%) required DR-CPR. In the group of 6478 EPI, 412 (6.4%) received DR-CPR compared with 224 of 11 086 infants (2.0%) in the VPI group. EPI who underwent DR-CPR had higher odds ratios (ORs (95% confidence interval)) for mortality compared to EPI not requiring DR-CPR (OR 3.32 (2.58, 4.29)), grades 3 to 4 intraventricular hemorrhage (IVH) (OR 1.59 (1.20, 2.10)) and periventricular leukomalacia (OR 1.81 (1.17, 2.82)). DR-CPR among VPI was associated with higher ORs for mortality (OR 4.99 (3.59, 6.94)), early sepsis (OR 2.07 (1.05, 4.09)), grades 3 to 4 IVH (OR 3.74 (2.55, 5.50)) and grades 3 to 4 retinopathy of prematurity (ROP) (OR 2.53 (1.18, 5.41)) compared to VPI not requiring DR-CPR. Only 11% of infants in the EPI DR-CPR group had favorable outcomes compared with 44% in the VPI DR-CPR group. Significantly higher ORs for mortality, IVH and ROP were found in the VPI compared to the EPI group.
Conclusion:
Preterm VLBW infants requiring DR-CPR were at increased risk of adverse outcomes compared to those not requiring CPR. This effect was more pronounced in the VPI group.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Lantos JD, Miles SH, Silverstein MD, Stocking CB . Survival after cardiopulmonary resuscitation in babies of very low birth weight. Is CPR futile therapy? N Engl J Med 1988; 318: 91–95.
Wyckoff MH, Salhab WA, Heyne RJ, Kendrick DE, Stoll BJ, Laptook AR . Outcome of extremely low birth weight infants who received delivery room cardiopulmonary resuscitation. J Pediatr 2012; 160: 239–244.
Finer NN, Horbar JD, Carpenter JH . Cardiopulmonary resuscitation in the very low birth weight infant: the Vermont Oxford Network experience. Pediatrics 1999; 104: 428–434.
Finer NN, Tarin T, Vaucher YE, Barrington K, Bejar R . Intact survival in extremely low birth weight infants after delivery room resuscitation. Pediatrics 1999; 104: e40.
Soraisham AS, Lodha AK, Singhal N, Aziz K, Yang J, Lee SK et al. Neonatal outcomes following extensive cardiopulmonary resuscitation in the delivery room for infants born at less than 33 weeks gestational age. Resuscitation 2014; 85: 238–243.
Handley SC, Sun Y, Wyckoff MH, Lee HC . Outcomes of extremely preterm infants after delivery room cardiopulmonary resuscitation in a population-based cohort. J Perinatol 2015; 35: 379–383.
Riskin A, Riskin-Mashiah S, Lusky A, Reichman B . Israel Neonatal Network. The relationship between delivery mode and mortality in very low birthweight singleton vertex-presenting infants. BJOG 2004; 111: 365–371.
Vermont-Oxford Trials Network. Vermont-Oxford Trials Network Database Project Manual of Operations, Release 2.0. Vermont-Oxford Trials Network: Burlington, VT, USA, 1993..
Kramer MS, Platt RW, Wen SW, Joseph KS, Allen A, Abrahamowicz M et al. A new and improved population-based Canadian reference for birth weight for gestational age. Pediatrics 2001; 108: E35.
Bancalari E, Abdenour GE, Feller R, Gannon J . Bronchopulmonary dysplasia: clinical presentation. J Pediatr 1979; 95: 819–823.
An international classification of retinopathy of prematurity. The Committee for the Classification of Retinopathy of Prematurity. Arch Ophthalmol 1984; 102: 1130–1134.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 1978; 92: 529–534.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg 1978; 187: 1–7.
John CP, Brian J . Decision-making in neonatal intensive care. Neoreviews 2009; 10: e270–e279.
Whitelaw A . Core concepts: intraventricular hemorrhage. Neoreviews 2011; 12: e94–e101.
Volpe JJ . Neurobiology of periventricular leukomalacia in the premature infant. Pediatr Res 2001; 50: 553–562.
Davis DJ . How aggressive should delivery room cardiopulmonary resuscitation be for extremely low birth weight neonates? Pediatrics 1993; 92: 447–450.
Grisaru-Granovsky S, Reichman B, Lerner-Geva L, Boyko V, Hammerman C, Samueloff A et al. Mortality and morbidity in preterm small-for-gestational-age infants: a population based study. Am J Obstet Gynecol 2012; 206: 150.e1-7.
Acknowledgements
The Israel National VLBW infant database is partially funded by the Israel Center for Disease Control and the Israel Ministry of Health.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Appendices
Coordinating center
The Israel Neonatal Network, participating centers in the Israel National Very Low Birth Weight Infant database
The Women and Children’s Health Research Unit, Gertner Institute, Tel Hashomer.
Neonatology departments
Assaf Harofeh Medical Center, Rishon Le Zion; Barzilay Medical Center, Ashkelon; Bikur Holim Hospital, Jerusalem; Bnei Zion Medical Center, Haifa; Carmel Medical Center, Haifa; English (Scottish) Hospital, Nazareth; French Hospital, Nazareth; Hadassah University Hospital Ein Kerem, Jerusalem; Hadassah University Hospital Har Hazofim, Jerusalem; Haemek Medical Center, Afula; Hillel Yafe Medical Center, Hadera; Italian Hospital, Nazareth; Kaplan Hospital, Rehovot; Laniado Hospital, Netanya; Maayanei Hayeshua Hospital, Bnei Brak; Meir Medical Center, Kfar Saba; Misgav Ladach Hospital, Jerusalem; Naharia Hospital, Naharia; Poria Hospital, Tiberias; Rambam Medical Center, Haifa; Rivka Ziv Hospital, Safed; Schneider Children’s Medical Center of Israel, Petach Tikva; Rabin Medical Center (Beilinson Campus), Petach Tikva; Shaare Zedek Hospital, Jerusalem; Sheba Medical Center, Tel Hashomer; Soroka Medical Center, Beer Sheba; Sourasky Medical Center, Tel Aviv; Wolfson Medical Center, Holon; Yoseftal Hospital, Eilat.
Rights and permissions
About this article
Cite this article
Arnon, S., Dolfin, T., Reichman, B. et al. Delivery room resuscitation and adverse outcomes among very low birth weight preterm infants. J Perinatol 37, 1010–1016 (2017). https://doi.org/10.1038/jp.2017.99
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.99
This article is cited by
-
Delivery room resuscitation intensity and associated neonatal outcomes of 24+0–31+6 weeks’ preterm infants in China: a retrospective cross-sectional study
World Journal of Pediatrics (2024)
-
Neuroprotection care bundle implementation is associated with improved long-term neurodevelopmental outcomes in extremely premature infants
Journal of Perinatology (2022)
-
Impact of neonatal resuscitation changes on outcomes of very-low-birth-weight infants
Scientific Reports (2021)
-
A clinical scoring system to predict the need for extensive resuscitation at birth in very low birth weight infants
BMC Pediatrics (2019)