Abstract
Objective:
To compare the neurodevelopmental outcomes at 18 to 21 months corrected age (CA) of infants born at <29 weeks that received room air, an intermediate oxygen concentration or 100% oxygen at the initiation of resuscitation.
Study design:
In this retrospective cohort study, we compared neonatal and neurodevelopmental outcomes at 18 to 21 months CA among inborn infants born before 29 weeks’ gestation that received room air, intermediate oxygen concentration or 100% oxygen at the initiation of resuscitation.
Results:
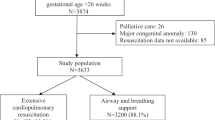
Of 1509 infants, 445 received room air, 483 received intermediate oxygen concentrations and 581 received 100% oxygen. Compared to infants that received room air, the primary outcome of death or neurodevelopmental impairment (NDI) was not different in intermediate oxygen (adjusted odds ratio (aOR) 1.01; 95% confidence interval (CI) 0.77, 1.34) or 100% oxygen (aOR 1.03; 95% CI 0.78, 1.35). Compared to room air, there was no difference in odds of death or severe NDI in intermediate oxygen (aOR 1.14; 95% CI 0.82, 1.58) or 100% oxygen group (aOR 1.22; 95% CI 0.90, 1.67). The odds of severe NDI among survivors were significantly higher in infants that received 100% oxygen as compared to room air (aOR 1.57, 95% CI 1.05, 2.35).
Conclusions:
We observed no significant difference in the primary composite outcomes of death or NDI and death or severe NDI at 18 to 21 months CA between infants that received room air, intermediate oxygen concentration or 100% oxygen at the initiation of resuscitation. However, use of 100% oxygen was associated with increased odds of severe NDI among survivors as compared to room air.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Barazzone C, Horowitz S, Donati YR, Rodriguez I, Piguet PF . Oxygen toxicity in mouse lung: pathways to cell death. Am J Respir Cell Mol Biol 1998; 19: 573–581.
Saugstad OD, Sejersted Y, Solberg R, Wollen EJ, Bjørås M . Oxygenation of the newborn: a molecular approach. Neonatology 2012; 101: 315–325.
Kapadia VS, Chalak LF, Sparks JE, Allen JR, Savani RC, Wyckoff MH . Resuscitation of preterm neonates with limited versus high oxygen strategy. Pediatrics 2013; 132: e1488–e1496.
Tataranno ML, Oei JL, Perrone S, Wright IM, Smyth JP, Lui K et al. Resuscitating preterm infants with 100% oxygen is associated with higher oxidative stress than room air. Acta Paediatr 2015; 104: 759–765.
Tan A, Schulze A, O'Donnell CP, Davis PG . Air versus oxygen for resuscitation of infants at birth. Cochrane Database Syst Rev 2005; (2): CD002273.
Rabi Y, Rabi D, Yee W . Room air resuscitation of the depressed newborn: a systematic review and meta-analysis. Resuscitation 2007; 72: 353–363.
Chen Y, Whitney PL, Frank L . Comparative responses of premature versus full-term newborn rats to prolonged hyperoxia. Pediatr Res 1994; 35: 233–237.
O’Donovan DJ, Fernandes CJ . Free radicals and diseases in premature infants. Antioxid Redox Signal 2004; 6: 169–176.
Perlman JM, Wyllie J, Kattwinkel J, Atkins DL, Chameides L, Goldsmith JP et al. Neonatal resuscitation: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Pediatrics 2010; 126: e1319–e1344.
Brown JV, Moe-Byrne T, Harden M, McGuire W . Lower versus higher oxygen concentration for delivery room stabilisation of preterm neonates: systematicreview. PLoS ONE 2012; 7: e52033.
Saugstad OD, Aune D, Aguar M, Kapadia V, Finer N, Vento M . Systematic review and meta-analysis of optimal initial fraction of oxygen levels in the delivery room at ≤32 weeks. Acta Paediatr 2014; 103: 744–751.
Oei JL, Vento M, Rabi Y, Wright I, Finer N, Rich W et al. Higher or lower oxygen for delivery room resuscitation of preterm infants below 28 completed weeks gestation: a meta-analysis. Arch Dis Child Fetal Neonatal Ed 2017; 102: F24–F30.
Saugstad OD, Ramji S, Irani SF, El-Meneza S, Hernandez EA, Vento M et al. Resuscitation of newborn infants with 21% or 100% oxygen: follow-up at 18 to 24 months. Pediatrics 2003; 112: 296–300.
Saugstad OD, Vento M, Ramji S, Howard D, Soll RF . Neurodevelopmental outcome of infants resuscitated with air or 100% oxygen: a systematic review and meta-analysis. Neonatology 2012; 102: 98–103.
Kapadia V, Ofman G, Savani R, Heyne R, Wyckoff M Delivery Room Resuscitation Using 2011 Neonatal Resuscitation Program Oxygen Guidelines and Neurodevelopmental Outcomes in Preterm neonates. Proceedings of the Pediatric Academic Societies Meeting, April 2015, San Diego, CA, USA. E-PAS 2015; 3585: 7..
Boronat N, Aguar M, Rook D, Iriondo M, Brugada M, Cernada M et al. Survival and neurodevelopmental outcomes of preterms resuscitated with different oxygen fractions. Pediatrics 2016; 138, pii: e20161405.
Canadian Neonatal Network. Abstractor’s manual v2.1.2:2014. Available at: http://www.canadianneonatalnetwork.org/portal/CNNHome/Publications.aspx. Accessed on January 2016.
Canadian Neonatal Follow-Up Network. 18 month corrected age assessment manual. September 2012, version 5. Available at: http://www.cnfun.ca/Resources.aspx. Accessed on January 2016.
Papile LA, Munsick-Bruno G, Schaefer A . Relationship of cerebral intraventricular hemorrhage and early childhood neurologic handicaps. J Pediatr 1983; 103 (2): 273–277.
Walsh MC, Kliegman RM . Necrotizing enterocolitis: treatment based on staging criteria. Pediatr Clin North Am 1986; 33: 179–201.
Shennan AT, Dunn MS, Ohlsson A, Lennox K, Hoskins EM . Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics 1988; 82: 527–532.
International Committee for the Classification of Retinopathy of Prematurity. The international classification of retinopathy of prematurity revisited. Arch Ophthalmol 2005; 123: 991–999.
Synnes A, Luu TM, Moddemann D, Church P, Lee D, Vincer M et al. Determinants of developmental outcomes in a very preterm Canadian cohort. Arch Dis Child Fetal Neonatal Ed 2017; 102: F235–F243.
Bayley N Manual for the Bayley Scales of Infant and Toddler Development, 3rd edn. The Psychological Corporation: San Antonio, TX, USA, 2006.
Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B . Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol 1997; 39: 214–223.
Wang CL, Anderson C, Leone TA, Rich W, Govindaswami B, Finer NN . Resuscitation of preterm neonates by using room air or 100% oxygen. Pediatrics 2008; 121: 1083–1089.
Escrig R, Arruza L, Izquierdo I, Villar G, Sáenz P, Gimeno A et al. Achievement of targeted saturation values in extremely low gestational age neonates resuscitated with low or high oxygen concentrations: a prospective, randomized trial. Pediatrics 2008; 121: 875–881.
Vento M, Moro M, Escrig R, Arruza L, Villar G, Izquierdo I et al. Preterm resuscitation with low oxygen causes less oxidative stress, inflammation, and chronic lung disease. Pediatrics 2009; 124: e439–e449.
Rabi Y, Singhal N, Nettel-Aguirre A . Room-air versus oxygen administration for resuscitation of preterm infants: the ROAR study. Pediatrics 2011; 128: e374–e381.
Hartnett ME, Penn JS . Mechanisms and management of retinopathy of prematurity. N Engl J Med 2012; 367: 2515–2526.
Shoji H, Ikeda N, Hosozawa M, Ohkawa N, Matsunaga N, Suganuma H et al. Oxidative stress early in infancy and neurodevelopmental outcome in very low-birth weight infants. Pediatr Int 2014; 56: 709–713.
Rabi Y, Lodha A, Soraisham A, Singhal N, Barrington K, Shah PS . Outcomes of preterm infants following the introduction of room air resuscitation. Resuscitation 2015; 96: 252–259.
Oei JL, Saugstad OD, Lui K, Wright IM, Smyth JP, Craven P et al. Targeted oxygen in the resuscitation of preterm infants, a randomized clinical trial. Pediatrics 2017; 139, pii: e20161452..
Acknowledgements
We would like to acknowledge the staff of the Canadian Neonatal Network and Canadian neonatal Follow-up Network coordinating center for their tireless and diligent work and Natasha Musrap, PhD, (Maternal Infant Care Research Centre, Mount Sinai Hospital) for editorial assistance. The Maternal-Infant Care Research Centre is supported by the Ontario Ministry of Health and Long-Term Care. Organizational support to the Canadian Neonatal Network is provided by the Canadian Institutes of Health Research-funded Team in Maternal-Infant Care. We thank the data abstractors of the CNN, staff of the CNN and CNFUN coordinating centers for providing organizational support, and all CNN and CNFUN site investigators. Administrative and statistical support for the study was provided by the Canadian Neonatal Network Coordinating Centre at the Maternal-Infant Research Centre, Mount Sinai Hospital, Toronto, Ontario. The Maternal-Infant Research Centre is supported by funding from the Canadian Institutes of Health Research (CIHR) (CTP87518) and the Ministry of Health and Long-Term Care, Ontario, Canada.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Members of the investigators of the Canadian Neonatal Network and Canadian Neonatal Follow up Network
A Synnes5, PS Shah6, A Harrison7, T Pillay7, Z Cieslak8, T Sorokan9, R Sherlock9, J Ting10, W Yee11, R Sauve11, K Aziz12, Z Kalapesi13, J Bodani13, K Sankaran14, S Daspal14, M Seshia15 and D Moddemann15, R Alvaro16, S Shivananda17, S el Helou17, O DaSilva18, D Lee18, C Nwaesei19, KS Lee20, L Ly20, E Kelly21, M Dunn22, P Church22, N Rouvinez-Bouali23, Brigitte Lemyre23, T Daboval23, K Dow24, E Pelausa25, K Barrington26, F Lefebvre26, C Drolet27, S Belanger27, P Riley28, M Claveau28, D Faucher29, V Bertelle30, E Masse30, C Demers30, R Canning31, B Bulleid32, H Makary32, C Ojah33, L Monterrosa33, A Deshpandey34, P Murphy34, J Afifi35, M Vincer35, A Kajetanowicz36, SK Lee37
5Children’s & Women’s Health Centre of British Columbia, Vancouver, BC, Canada; 6Mount Sinai Hospital, Toronto, Ontario; 7Victoria General Hospital, Victoria, BC, Canada; 8Royal Columbian Hospital, New Westminster, BC, Canada; 9Surrey Memorial Hospital, Surrey, BC, Canada; 10Children’s & Women’s Health Centre of British Columbia, Vancouver, BC, Canada; 11Foothills Medical Centre, Calgary, AB, Canada; 12Royal Alexandra Hospital, A. Reichert, Glenrose Rehabilitation Hospital, Edmonton, AB, Canada; 13Regina General Hospital, Regina, SK, Canada; 14Royal University Hospital, Saskatoon, SK, Canada; 15Winnipeg Health Sciences Centre, Winnipeg, MB, Canada; 16St. Boniface General Hospital, Winnipeg, MB, Canada; 17Hamilton Health Sciences Centre, Hamilton, ON, Canada; 18London Health Sciences Centre, London, ON, Canada; 19Windsor Regional Hospital, Windsor, ON, Canada; 20Hospital for Sick Children, Toronto, ON, Canada; 21Mount Sinai Hospital, Toronto, ON, Canada; 22Sunnybrook Health Sciences Centre, Toronto, ON, Canada; 23Children’s Hospital of Eastern Ontario and Ottawa General Hospital, Ottawa, ON, Canada; 24Kingston General Hospital, Kingston, ON, Canada; 25Jewish General Hospital, Montreal, QC, Canada; 26Hopital Sainte-Justine, Montreal, QC, Canada; 27Centre Hospitalier Universitaire de Quebec, Sainte-Foy, QC, Canada; 28Montreal Children’s Hospital, Montreal, QC, Canada; 29Royal Victoria Hospital, Montreal, QC, Canada; 30Centre Hospitalier Universitaire de Sherbrooke, Sherbrooke, QC, Canada; 31Moncton Hospital, Moncton, NB, Canada; 32Dr Everett Chalmers Hospital, Fredericton, NB, Canada; 33Saint John Regional Hospital, Saint John, NB, Canada; 34Janeway Children’s Health and Rehabilitation Centre, St. John’s, NL, Canada; 35IWK Health Centre, Halifax, NS, Canada; 36Cape Breton Regional Hospital, Sydney, NS, Canada; 37Mount Sinai Hospital, Toronto, ON, Canada.
Rights and permissions
About this article
Cite this article
Soraisham, A., Rabi, Y., Shah, P. et al. Neurodevelopmental outcomes of preterm infants resuscitated with different oxygen concentration at birth. J Perinatol 37, 1141–1147 (2017). https://doi.org/10.1038/jp.2017.83
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.83
This article is cited by
-
Oxygen therapy of the newborn from molecular understanding to clinical practice
Pediatric Research (2019)