Abstract
Objectives:
Bronchopulmonary dysplasia (BPD) and the associated complication of pulmonary hypertension (PH) leads to increased mortality and a longer length of stay among survivors. Placental histopathology may give early clues of subsequent events. The objective was to evaluate the relationship of maternal vascular underperfusion (MVU) changes on placental histopathology with subsequent development of BPD-associated PH in a cohort of extremely premature infants.
Study Design:
In a cohort of preterm infants ‘⩽28 weeks’ gestational age (GA) and with ‘severe’ BPD, this retrospective study evaluated specific placental histopathological changes and assessed the relationship with subsequent development of PH. ‘Severe’ BPD was defined as the need for ⩾30% oxygen and/or positive pressure ventilation at 36 weeks postmenstrual age. Placental and echocardiographic assessments were done by investigators masked to the grouping and clinical outcomes.
Results:
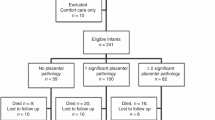
Fifty six infants with severe BPD formed the cohort; PH was noted in 22 (39.3%) infants. The GA of the infants with and without PH was comparable (25.8±1.6 vs 25.8±1.3 weeks, P=0.9). On placental histopathological examination, 13 (23%) had features of MVU. On univariate logistic regression, the presence of changes consistent with MVU increased the relative risk of subsequent BPD-associated PH by 2.75 (95% confidence interval 1.56 to 4.85, P=0.004). The significance persisted after adjustment for GA. Stratification by the presence or absence of fetal growth restriction, yielded nonsignificant associations (P=0.17).
Conclusion:
Based on the results of the present study, specific placental histopathological changes may give early clues to the subsequent development of BPD-associated PH.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Mourani PM, Mullen M, Abman SH . Pulmonary hypertension in bronchopulmonary dysplasia. Prog Pediatr Cardiol 2009; 27: 43–48.
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook AR, Walsh MC et al. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics 2010; 126: 443–456.
Chow SSW, Le Marsney R, Haslam R, Lui K . Report of the Australia and New Zealand Neonatal Network 2014. 2016.
An HS, Bae EJ, Kim GB, Kwon BS, Beak JS, Kim EK et al. Pulmonary hypertension in preterm infants with bronchopulmonary dysplasia. Korean Circ J 2010; 40: 131–136.
Bhat R, Salas AA, Foster C, Carlo WA, Ambalavanan N . Prospective analysis of pulmonary hypertension in extremely low birth weight infants. Pediatrics 2012; 129: e682–e689.
Fouron JC, Le Guennec JC, Villemant D, Perreault G, Davignon A . Value of echocardiography in assessing the outcome of bronchopulmonary dysplasia of the newborn. Pediatrics 1980; 65: 529–535.
Revanna GK, Kunjunju A, Sehgal A . Bronchopulmonary dysplasia associated pulmonary hypertension: making the best use of bedside echocardiography. J Pediatr 2017; 185: 33–41.
Kim GB . Pulmonary hypertension in infants with bronchopulmonary dysplasia. Korean J Pediatr 2010; 53: 688–693.
Bose C, Van Marter LJ, Laughon M, O’Shea TM, Allred EN, Karna P et al. Fetal growth restriction and chronic lung disease among infants born before the 28th week of gestation. Pediatrics 2009; 124: e450–e458.
Check J, Gotteiner N, Liu X, Su E, Porta N, Steinhorn R et al. Fetal growth restriction and pulmonary hypertension in premature infants with bronchopulmonary dysplasia. J Perinatol 2013; 33: 553e7.
Ozkan H, Cetinkaya M, Koksal N . Increased incidence of bronchopulmonary dysplasia in preterm infants exposed to preeclampsia. J Matern Fetal Neonatal Med 2012; 25: 2681e5.
Mourani PM, Abman SH . Pulmonary vascular disease in bronchopulmonary dysplasia: pulmonary hypertension and beyond. Curr Opin Pediatr 2013; 25: 329–337.
Rozance PJ, Seedorf GJ, Brown A, Roe G, O’Meara MC, Gien J et al. Intrauterine growth restriction decreases pulmonary alveolar and vessel growth and causes pulmonary artery endothelial cell dysfunction in vitro in fetal sheep. AJP Lung Cell Mol Physiol 2011; 301: L860–L871.
Barker DJ, Gluckman PD, Godfrey KM, Harding JE, Owens JA, Robinson JS . Fetal nutrition and cardiovascular disease in adult life. Lancet 1993; 341: 938–941.
Mestan KK, Check J, Minturn L, Yallapragada S, Farrow KN, Liu X et al. Placental pathologic changes of maternal vascular under perfusion in bronchopulmonary dysplasia and pulmonary hypertension. Placenta 2014; 35: 570–574.
Jobe AH, Bancalari E . Bronchopulmonary dysplasia. Am J Respir Crit Care Med 2001; 163: 1723–1729.
Lau EM, Manes A, Celermajer DS, Galiè N . Early detection of pulmonary vascular disease in pulmonary arterial hypertension: time to move forward. Eur Heart J 2011; 32: 2489–2498.
Nagiub M, Lee S, Guglani L . Echocardiographic assessment of pulmonary hypertension in infants with bronchopulmonary dysplasia: Systematic review of literature and a proposed algorithm for assessment. Echocardiography 2015; 32: 819–833.
King ME, Braun H, Goldblatt A, Liberthson R, Weyman AE . Interventricular septal configuration as a predictor of right ventricular systolic hypertension in children: a cross-sectional echocardiographic study. Circulation 1983; 68: 68–75.
Musewe NN, Poppe D, Smallhorn JF . Doppler echocardiographic measurement of pulmonary artery pressure from ductal Doppler velocities in the newborn. J Am Coll Cardiol 1990; 15: 446–456.
Abraham S, Weismann CG . Left ventricular end-systolic eccentricity index for assessment of pulmonary hypertension in infants. Echocardiography 2016; 33: 910–915.
Pande A, Sarkar A, Ahmed I, Naveen Chandra G, Patil SK, Kundu CK et al. Non-invasive estimation of pulmonary vascular resistance in patients of pulmonary hypertension in congenital heart disease with unobstructed pulmonary flow. Ann Pediatr Cardiol 2014; 7: 92–97.
Redline RW, Boyd T, Campbell V, Hyde S, Kaplan C, Khong TY et al. Maternal vascular under-perfusion: nosology and reproducibility of placental reaction patterns. Pediatr Dev Pathol 2004; 7: 237–249.
Khemani E, McElhinney DB, Rhein L, Andraade O, Lacro RV, Thomas KC et al. Pulmonary artery hypertension in formerly premature infants with bronchopulmonary dysplasia: clinical features and outcomes in the surfactant era. Pediatrics 2007; 120: 1260–1269.
Kim D-H, Kim H-S, Choi CW, Kim E-K, Kim BI, Choi J-H . Risk factors for pulmonary artery hypertension in preterm infants with moderate or severe bronchopulmonary dysplasia. Neonatology 2012; 101: 40–46.
Mestan KK, Gotteiner N, Porta N, Grobman W, Su EJ, Ernst LM . Cord blood biomarkers of placental maternal vascular underperfusion predict bronchopulmonary dysplasia-associated pulmonary hypertension. J Pediatr 2017; 185: 33–46 pii: S0022-S3476(17)30033-1.
Sehgal A, Malikiwi A, Paul E, Tan K, Menahem S . Systemic arterial stiffness in infants with bronchopulmonary dysplasia: potential cause of systemic hypertension. J Perinatol 2016; 36: 564–569.
Gan CTJ, Lankhaar JW, Westerhof N, Marcus JT, Becker A, Twisk JWR et al. Noninvasively assessed pulmonary artery stiffness predicts mortality in pulmonary arterial hypertension. Chest 2007; 132: 1906–1912.
Wang Z, Chesler N . Pulmonary vascular wall stiffness: an important contributor to the increased right ventricular afterload with pulmonary hypertension. Pulm Circ 2011; 1: 212–223.
Mukherjee D . Atherogenic vascular stiffness and hypertension cause or effect? JAMA 2012; 308: 919–920.
Willard JEL, Richard A, Hillis LD Cardiac catheterization. In: Kloner RA. The Guide to Cardiology, 3rd edn. Le Jacq Communications: Greenwich, CT, 1995; 151.
Shrout PE, Fleiss JL . Intraclass correlations: uses in assessing rater reliability. Psychol Bull 1979; 86: 420–428.
Yock PG, Popp RL . Non-invasive estimation of right ventricular systolic pressure by Doppler ultrasound in patients with tricuspid regurgitation. Circulation 1984; 70: 657–662.
Abbas AE, Fortuin FD, Schiller NB, Appleton CP, Moreno CA, Lester SJ . A simple method for non-invasive estimation of pulmonary vascular resistance. J Am Coll Cardiol 2003; 41: 1021–1027.
Ajami GH, Cheriki S, Amoozgar H, Borzouee M, Soltani M . Accuracy of Doppler-derived estimation of pulmonary vascular resistance in congenital heart disease: an index of operability. Pediatr Cardiol 2011; 32: 1168–1174.
Vlahos AP, Feinstein JA, Schiller NB, Silverman NH . Extension of Doppler-derived echocardiographic measures of pulmonary vascular resistance to patients with moderate or severe pulmonary vascular disease. J Am Soc Echocardiogr 2008; 21: 711–714.
Howard LS, Grapsa J, Dawson D, Bellamy M, Chambers JB, Masani ND et al. Echocardiographic assessment of pulmonary hypertension: standard operating procedure. Eur Respir Rev 2012; 21: 239–248.
Lal CV, Ambalavanan N . Biomarkers, early diagnosis, and clinical predictors of BPD. Clin Perinatol 2015; 42: 739–754.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kunjunju, A., Gopagondanahalli, K., Chan, Y. et al. Bronchopulmonary dysplasia-associated pulmonary hypertension: clues from placental pathology. J Perinatol 37, 1310–1314 (2017). https://doi.org/10.1038/jp.2017.130
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2017.130
This article is cited by
-
Placental origins of neonatal diseases: toward a precision medicine approach
Pediatric Research (2021)
-
Allogeneic administration of human umbilical cord-derived mesenchymal stem/stromal cells for bronchopulmonary dysplasia: preliminary outcomes in four Vietnamese infants
Journal of Translational Medicine (2020)
-
Is bronchopulmonary dysplasia decided before birth?
Pediatric Research (2020)
-
Impact of multiple placental pathologies on neonatal death, bronchopulmonary dysplasia, and neurodevelopmental impairment in preterm infants
Pediatric Research (2020)