Abstract
Objective:
To evaluate the impact of statewide learning collaboratives that used national guidelines to manage jaundice on the serial prevalence of extreme hyperbilirubinemia (EHB, total bilirubin ⩾25 mg dl−1) and exchange transfusions introduced in California Perinatal Quality Care Collaborative (CPQCC) hospitals in 2007.
Study Design:
Adverse outcomes were retrieved from statewide databases on re-admissions for live births ⩾35 weeks’ gestation (2007 to 2012) in diverse CPQCC hospitals. Individual and cumulative select perinatal risk factors and frequencies were the outcomes measures.
Results:
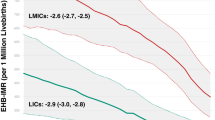
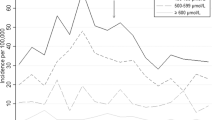
For 3 172 762 babies (2007 to 2012), 92.5% were ⩾35 weeks’ gestation. Statewide EHB and exchange rates decreased from 28.2 to 15.3 and 3.6 to 1.9 per 100 000 live births, respectively. From 2007 to 2012, the trends for TB>25 mg dl−1 rates were −0.92 per 100 000 live births per year (95% CI: −3.71 to 1.87, P=0.41 and R2=0.17).
Conclusion:
National guidelines complemented by statewide learning collaboratives can decrease or modify outcomes among all birth facilities and impact clinical practice behavior.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
American Academy of Pediatrics. Management of hyperbilirubinemia in the newborn infant ⩾35 weeks of gestation. Pediatrics 2004; 114: 297–316.
Bhutani VK, Johnson L . Synopsis report from the pilot USA Kernicterus Registry. J Perinatol 2009; 29 (Suppl 1): S4–S7.
Maisels MJ, Bhutani VK, Bogen D, Newman TB, Stark AR, Watchko JF . Hyperbilirubinemia in the newborn infant ⩾35 weeks' gestation: an update with clarifications. Pediatrics 2009; 124: 1193–1198.
US Preventive Services Task Force. Screening of infants for hyperbilirubinemia to prevent chronic bilirubin encephalopathy: US Preventive Services Task Force recommendation statement. Pediatrics 2009; 124: 1172–1177.
Bhutani VK, Johnson LH, MJ Maisels, Newman TB, Phibbs C, Stark AR et al. Kernicterus: epidemiological strategies for its prevention through systems-based approaches. J Perinatol 2004; 24: 650–662.
Newman TB, Xiong B, Gonzales VM, Escobar GJ . Prediction and prevention of extreme neonatal hyperbilirubinemia in a mature health maintenance organization. Arch Pediatr Adolesc Med 2000; 154: 1140–1147.
Geiger AM, Petitti DB, Yao JF . Rehospitalisation for neonatal jaundice: risk factors and outcomes. Paediatr Perinat Epidemiol 2001; 15: 352–358.
Maisels MJ, Kring E . Length of stay, jaundice, and hospital readmission. Pediatrics 1998; 101: 995–998.
Brooks JC, Fisher-Owens SA, Wu YW, Strauss DJ, Newman TB . Evidence suggests there was not a ‘resurgence’ of kernicterus in the 1990 s. Pediatrics 2011; 127: 672–679.
Brown AK, Kim MH, Wu PY, Bryla DA . Efficacy of phototherapy in prevention and management of neonatal hyperbilirubinemia. Pediatrics 1985; 75: 393–400.
Stark AR . Levels of neonatal care. Pediatrics 2004; 114: 1341–1347.
BiliTool. http://www.bilitool.org/.
Norman M, Aberg K, Holmsten K, Weibel V, Ekeus C . Predicting nonhemolytic neonatal hyperbilirubinemia. Pediatrics 2015; 136: 1087–1094.
Keren R, Luan X, Friedman S, Saddlemire S, Cnaan A, Bhutani VK . A comparison of alternative risk-assessment strategies for predicting significant neonatal hyperbilirubinemia in term and near-term infants. Pediatrics 2008; 121: e170–e179.
Newman TB, Liljestrand P, Escobar GJ . Combining clinical risk factors with serum bilirubin levels to predict hyperbilirubinemia in newborns. Arch Pediatr Adolesc Med 2005; 159: 113–119.
Bjerre JV, Petersen JR, Ebbesen F . Surveillance of extreme hyperbilirubinaemia in Denmark. A method to identify the newborn infants. Acta Paediatr 2008; 97: 1030–1034.
Eggert LD, Wiedmeier SE, Wilson J, Christensen RD . The effect of instituting a prehospital-discharge newborn bilirubin screening program in an 18-hospital health system. Pediatrics 2006; 117: e855–e862.
Mah MP, Clark SL, Akhigbe E, Englebright J, Frye DK, Meyers JA et al. Reduction of severe hyperbilirubinemia after institution of predischarge bilirubin screening. Pediatrics 2010; 125: e1143–e1148.
Manning D, Todd P, Maxwell M, Platt MJ . Prospective surveillance study of severe hyperbilirubinaemia in the newborn in the UK and Ireland. Arch Dis Child Fetal Neonatal Ed 2007; 92: F342–F346.
Sgro M, Campbell D, Shah V . Incidence and causes of severe neonatal hyperbilirubinemia in Canada. CMAJ 2006; 175: 587–590.
Usatin D, Liljestrand P, Kuzniewicz MW, Escobar GJ, Newman TB . Effect of neonatal jaundice and phototherapy on the frequency of first-year outpatient visits. Pediatrics 2010; 125: 729–734.
Vandborg PK, Hansen BM, Greisen G, Jepsen M, Ebbesen F . Follow-up of neonates with total serum bilirubin levels ≥25 mg/dL: a Danish population-based study. Pediatrics 2012; 130: 61–66.
Kaplan M, Hammerman C . The need for neonatal glucose-6-phosphate dehydrogenase screening: a global perspective. J Perinatol 2009; 29 (Suppl 1): S46–S52.
Nock ML, Johnson EM, Krugman RR, Di Fiore JM, Fitzgerald S, Sandhaus LM et al. Implementation and analysis of a pilot in-hospital newborn screening program for glucose-6-phosphate dehydrogenase deficiency in the United States. J Perinatol 2011; 31: 112–11.
Acknowledgements
We are thankful for the thoughtful and deliberate translation of the 2004 AAP Practice Guideline by the California-based authoring taskforce to develop a CPQCC website: ‘Severe Neonatal Hyperbilirubinemia Toolkit’ and conduct statewide initiatives. We are also indebted to the meticulous attention of CPQCC member institutions who have voluntarily retrieved, reviewed, reported and audited their respective institutional data to the CPQCC website. YK was supported in part by the NIH T32 HD007249 and the Division of Neonatal and Developmental Medicine, Department of Pediatrics, Stanford University School of Medicine, Stanford, CA, USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Bhutani, V., Meng, N., Knauer, Y. et al. Extreme hyperbilirubinemia and rescue exchange transfusion in California from 2007 to 2012. J Perinatol 36, 853–857 (2016). https://doi.org/10.1038/jp.2016.106
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.106
This article is cited by
-
Assessment, management, and incidence of neonatal jaundice in healthy neonates cared for in primary care: a prospective cohort study
Scientific Reports (2022)
-
Extreme neonatal hyperbilirubinemia and kernicterus spectrum disorder in Denmark during the years 2000–2015
Journal of Perinatology (2020)
-
High unbound bilirubin for age: a neurotoxin with major effects on the developing brain
Pediatric Research (2019)