Abstract
Objective:
A meta-analysis of randomized controlled trials (RCTs) was conducted to evaluate whether tranexamic acid (TXA) could significantly reduce blood loss during and after cesarean section (CS) when compared with no TXA.
Study design:
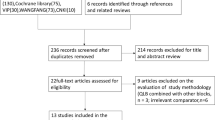
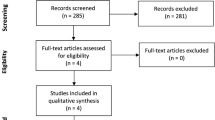
MEDLINE (PubMed), EMBASE, Cochrane Central Register of Controlled Trials and Web of Science were searched to identify RCTs that compared intravenous TXA with no TXA before CS for blood loss. The related data were extracted by two independent authors. The fixed or random-effect methods were used to combine data.
Result:
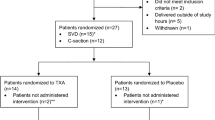
Eleven RCTs were included in this analysis with a total of 1276 women in TXA group and 1255 in no TXA (control) group. Total blood loss during and after CS was significantly less in TXA group than in control group (mean difference (MD) −141.61 ml, 95% confidence interval (CI) −207.09 to −76.14, P<0.01). There was a significant reduction in intraoperative and postpartum blood loss in TXA group as compared with control group (MD −143.36 ml, 95% CI −220.38 to −66.35, P<0.01; and MD −38.20 ml, 95% CI −59.27 to −17.12, P<0.01, respectively). Declines in hemoglobin and hematocrit values after CS were both significantly less in TXA group than in control group. The difference of postpartum hemorrhage rate was statistically significant between groups (risk ratio (RR) 0.57, 95% CI 0.37 to 0.89, P=0.01). The need for blood transfusion was significantly less in TXA group than control group (RR 0.23, 95% CI 0.10 to 0.57, P<0.01).
Conclusion:
Our results demonstrate that TXA offers an advantage over no TXA in reducing blood loss during and after CS.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout










Similar content being viewed by others
References
Betran AP, Merialdi M, Lauer JA, Bing-Shun W, Thomas J, Van Look P et al. Rates of caesarean section: analysis of global, regional and national estimates. Paediatr Perinat Epidemiol 2007; 21 (2): 98–113.
Menacker F, Hamilton BE . Recent trends in cesarean delivery in the United States. NCHS Data Brief 2010; 35: 1–8.
Mi J, Liu F . Rate of caesarean section is alarming in China. Lancet 2014; 383 (9927): 1463–1464.
World Health Organization. The World Health Report, 2005: Make Every Mother and Child Count. World Health Organization: Geneva, 2005.
Ekeroma AJ, Ansari A, Stirrat GM . Blood transfusion in obstetrics and gynaecology. Br J Obstet Gynaecol 1997; 104 (3): 278–284.
AbouZahr C . Global burden of maternal death and disability. Br Med Bull 2003; 67: 1–11.
Hoylaerts M, Lijnen HR, Collen D . Studies on the mechanism of the antifibrinolytic action of tranexamic acid. Biochim Biophys Acta 1981; 673 (1): 75–85.
Dunn CJ, Goa KL . Tranexamic acid: a review of its use in surgery and other indications. Drugs 1999; 57 (6): 1005–1032.
Gai MY, Wu LF, Su QF, Tatsumoto K . Clinical observation of blood loss reduced by tranexamic acid during and after caesarian section: a multi-center, randomized trial. Eur J Obstet Gynecol Reprod Biol 2004; 112 (2): 154–157.
Gohel M, Patel P, Gupta A, Desai P . Efficacy of tranexamic acid in decreasing blood loss during and after cesarean section: a randomized case controlled prospective study. J Obstet Gynecol India 2007; 57 (3): 227–230.
Sekhavat L, Tabatabaii A, Dalili M, Farajkhoda T, Tafti AD . Efficacy of tranexamic acid in reducing blood loss after cesarean section. J Matern Fetal Neonatal Med 2009; 22 (1): 72–75.
Movafegh A, Eslamian L, Dorabadi A . Effect of intravenous tranexamic acid administration on blood loss during and after cesarean delivery. Int J Gynaecol Obstet 2011; 115 (3): 224–226.
Gungorduk K, Yildirim G, Asicioglu O, Gungorduk OC, Sudolmus S, Ark C . Efficacy of intravenous tranexamic acid in reducing blood loss after elective cesarean section: a prospective, randomized, double-blind, placebo-controlled study. Am J Perinatol 2011; 28 (3): 233–240.
Halder S, Samanta B, Sardar R, Chattopadhyay S . Tranexamic acid used before caesarean section reduces blood loss based on pre- and postoperative haemoglobin level: a case-control study. J Indian Med Assoc 2013; 111 (3): 184–186.
Goswami U, Sarangi S, Gupta S, Babbar S . Comparative evaluation of two doses of tranexamic acid used prophylactically in anemic parturients for lower segment cesarean section: a double-blind randomized case control prospective trial. Saudi J Anaesth 2013; 7 (4): 427–431.
Shahid A, Khan A . Tranexamic acid in decreasing blood loss during and after caesarean section. J Coll Physicians Surg Pak 2013; 23 (7): 459–462.
Abdel-Aleem H, Alhusaini TK, Abdel-Aleem MA, Menoufy M, Gulmezoglu AM . Effectiveness of tranexamic acid on blood loss in patients undergoing elective cesarean section: randomized clinical trial. J Matern Fetal Neonatal Med 2013; 26 (17): 1705–1709.
Senturk MB, Cakmak Y, Yildiz G, Yildiz P . Tranexamic acid for cesarean section: a double-blind, placebo-controlled, randomized clinical trial. Arch Gynecol Obstet 2013; 287 (4): 641–645.
Xu J, Gao W, Ju Y . Tranexamic acid for the prevention of postpartum hemorrhage after cesarean section: a double-blind randomization trial. Arch Gynecol Obstet 2013; 287 (3): 463–468.
Moher D, Liberati A, Tetzlaff J, Altman DG . Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 2009; 151 (4): 264–269.
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 1996; 17 (1): 1–12.
Hozo SP, Djulbegovic B, Hozo I . Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 2005; 5: 13.
Higgins JP, Thompson SG, Deeks JJ, Altman DG . Measuring inconsistency in meta-analyses. BMJ 2003; 327 (7414): 557–560.
Hong S, Wang H, Yang S, Yang K . External stent versus no stent for pancreaticojejunostomy: a meta-analysis of randomized controlled trials. J Gastrointest Surg 2013; 17 (8): 1516–1525.
Sterne JA, Egger M . Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol 2001; 54 (10): 1046–1055.
Egger M, Davey SG, Schneider M, Minder C . Bias in meta-analysis detected by a simple, graphical test. BMJ 1997; 315 (7109): 629–634.
Shakur H, Elbourne D, Gulmezoglu M, Alfirevic Z, Ronsmans C, Allen E et al. The WOMAN Trial (World Maternal Antifibrinolytic Trial): tranexamic acid for the treatment of postpartum haemorrhage: an international randomised, double blind placebo controlled trial. Trials 2010; 11: 40.
As AK, Hagen P, Webb JB . Tranexamic acid in the management of postpartum haemorrhage. Br J Obstet Gynaecol 1996; 103 (12): 1250–1251.
Yang H, Zheng S, Shi C . Clinical study on the efficacy of tranexamic acid in reducing postpartum blood lose: a randomized, comparative, multicenter trial. Zhonghua Fu Chan Ke Za Zhi 2001; 36 (10): 590–592.
Ronsmans C, Graham WJ . Maternal mortality: who, when, where, and why. Lancet 2006; 368 (9542): 1189–1200.
Ducloy-Bouthors AS, Jude B, Duhamel A, Broisin F, Huissoud C, Keita-Meyer H et al. High-dose tranexamic acid reduces blood loss in postpartum haemorrhage. Crit Care 2011; 15 (2): R117.
Stafford I, Dildy GA, Clark SL, Belfort MA . Visually estimated and calculated blood loss in vaginal and cesarean delivery. Am J Obstet Gynecol 2008; 199 (5): 511–519.
Bekassy Z, Astedt B . Treatment with the fibrinolytic inhibitor tranexamic acid—risk for thrombosis? Acta Obstet Gynecol Scand 1990; 69 (4): 353–354.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, HY., Hong, SK., Duan, Y. et al. Tranexamic acid and blood loss during and after cesarean section: a meta-analysis. J Perinatol 35, 818–825 (2015). https://doi.org/10.1038/jp.2015.93
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2015.93
This article is cited by
-
Tranexamic acid for treatment and prophylaxis of bleeding and hyperfibrinolysis
Wiener klinische Wochenschrift (2017)