Abstract
Objective:
Assess association of NICU size, and occupancy rate and resource utilization at admission with neonatal outcome.
Study Design:
Retrospective cohort study of 9978 infants born at 23–32 weeks gestation and admitted to 23 tertiary-level Canadian NICUs during 2010–2012. Adjusted odds ratios (AOR) were estimated for a composite outcome of mortality/any major morbidity with respect to NICU size, occupancy rate and intensity of resource utilization at admission.
Results:
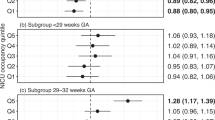
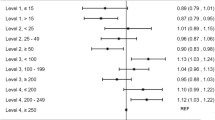
A total of 2889 (29%) infants developed the composite outcome, the odds of which were higher for 16–29, 30–36 and >36-bed NICUs compared with <16-bed NICUs (AOR (95% CI): 1.47 (1.25–1.73); 1.49 (1.25–1.78); 1.55 (1.29–1.87), respectively) and for NICUs with higher resource utilization at admission (AOR: 1.30 (1.08–1.56), Q4 vs Q1) but not different according to NICU occupancy.
Conclusion:
Larger NICUs and more intense resource utilization at admission are associated with higher odds of a composite adverse outcome in very preterm infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Swyer PR . The regional organisation of special care for the neonate. Pediatr Clin North Am 1970; 17: 761–776.
Yu VY, Dunn PM . Development of regionalized perinatal care. Semin Neonatol 2004; 9: 89–97.
Ohlsson A, Fohlin L . Reproductive medical care in Sweden and the Province of Ontario, Canada. A comparative study. Acta Paediatr Scand Suppl 1983; 306: 1–15.
Sinclair JC . The neonatal intensive care unit: organization of care of the low-birthweight infant. Birth Defects Orig Artic Ser 1988; 24: 11–21.
Investigators of the Vermont-Oxford Trials Network Database Project. The Vermont-Oxford Trials Network: very low birth weight outcomes for 1990. Pediatrics 1993; 91: 540–545.
Draper ES, Zeitlin J, Fenton AC, Weber T, Gerrits J, Martens G et al. Investigating the variations in survival rates for very preterm infants in 10 European regions: the MOSAIC birth cohort. Arch Dis Child Fetal Neonatal Ed 2009; 94: F158–F163.
Isayama T, Lee SK, Mori R, Kusuda S, Fujimura M, Ye XY et al. Comparison of mortality and morbidity of very low birth weight infants between Canada and Japan. Pediatrics 2012; 130: e957–e965.
Kusuda S, Fujimura M, Sakuma I, Aotani H, Kabe K, Itani Y et al. Morbidity and mortality of infants with very low birth weight in Japan: center variation. Pediatrics 2006; 118: e1130–e1138.
Lee SK, McMillan DD, Ohlsson A, Pendray M, Synnes A, Whyte R et al. Variations in practice and outcomes in the Canadian NICU network: 1996-1997. Pediatrics 2000; 106: 1070–1079.
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook AR, Walsh MC et al. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics 2010; 126: 443–456.
Synnes AR, Chien LY, Peliowski A, Baboolal R, Lee SK . Variations in intraventricular hemorrhage incidence rates among Canadian neonatal intensive care units. J Pediatr 2001; 138: 525–531.
Synnes AR, Macnab YC, Qiu Z, Ohlsson A, Gustafson P, Dean CB et al. Neonatal intensive care unit characteristics affect the incidence of severe intraventricular hemorrhage. Med Care 2006; 44: 754–759.
Bartels DB, Wypij D, Wenzlaff P, Dammann O, Poets CF . Hospital volume and neonatal mortality among very low birth weight infants. Pediatrics 2006; 117: 2206–2214.
Lorch SA, Baiocchi M, Ahlberg CE, Small DS . The differential impact of delivery hospital on the outcomes of premature infants. Pediatrics 2012; 130: 270–278.
Neogi SB, Malhotra S, Zodpey S, Mohan P . Does facility based newborn care improve neonatal outcomes? A review of evidence. Indian Pediatr 2012; 49: 651–658.
Phibbs CS, Bronstein JM, Buxton E, Phibbs RH . The effects of patient volume and level of care at the hospital of birth on neonatal mortality. JAMA 1996; 276: 1054–1059.
Phibbs CS, Baker LC, Caughey AB, Danielsen B, Schmitt SK, Phibbs RH . Level and volume of neonatal intensive care and mortality in very-low-birth-weight infants. N Engl J Med 2007; 356: 2165–2175.
Chung JH, Phibbs CS, Boscardin WJ, Kominski GF, Ortega AN, Gregory KD et al. Examining the effect of hospital-level factors on mortality of very low birth weight infants using multilevel modeling. J Perinatol 2011; 31: 770–775.
Horbar JD, Badger GJ, Lewit EM, Rogowski J, Shiono PH . Hospital and patient characteristics associated with variation in 28-day mortality rates for very low birth weight infants. Vermont Oxford Network. Pediatrics 1997; 99: 149–156.
Tucker J . Patient volume, staffing, and workload in relation to risk-adjusted outcomes in a random stratified sample of UK neonatal intensive care units: a prospective evaluation. Lancet 2002; 359: 99–107.
Hamilton K, Gould C, Tarnow-Mordi W . Hospital mortality in relation to staffing levels in the first three days of neonatal care. Proceedings of the 4th Annual Congress of the Perinatal Society of Australia and New Zealand 2000; 109 (abstract).
Hamilton KE, Redshaw ME, Tarnow-Mordi W . Nurse staffing in relation to risk-adjusted mortality in neonatal care. Arch Dis Child Fetal Neonatal Ed 2007; 92: F99–F103.
Haley RW, Bregman DA . The role of understaffing and overcrowding in recurrent outbreaks of staphylococcal infection in a neonatal special-care unit. J Infect Dis 1982; 145: 875–885.
Parry GJ, Tucker JS, Tarnow-Mordi WO . Relationship between probable nosocomial bacteraemia and organisational and structural factors in UK neonatal intensive care units. Qual Saf Health Care 2005; 14: 264–269.
Canadian Neonatal Network. Abstractor's Manual v2.1.2. 2014. Available from http://www.canadianneonatalnetwork.org/portal/CNNHome/Publications.aspx Last accessed: March 18th, 2014.
Gray JE, Richardson DK, McCormick MC, Workman-Daniels K, Goldmann DA . Neonatal therapeutic intervention scoring system: a therapy-based severity-of-illness index. Pediatrics 1992; 90: 561–567.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 1978; 92: 529–534.
International Committee for the Classification of Retinopathy of Prematurity. The International Classification of Retinopathy of Prematurity revisited. Arch Ophthalmol 2005; 123: 991–999.
Shennan AT, Dunn MS, Ohlsson A, Lennox K, Hoskins EM . Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics 1988; 82: 527–532.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg 1978; 187: 1–7.
Kramer MS, Platt RW, Wen SW, Joseph KS, Allen A, Abrahamowicz M et al. A new and improved population-based Canadian reference for birth weight for gestational age. Pediatrics 2001; 108: E35.
Richardson DK, Corcoran JD, Escobar GJ, Lee SK . SNAP-II and SNAPPE-II: Simplified newborn illness severity and mortality risk scores. J Pediatr 2001; 138: 92–100.
Marlow N, Bennett C, Draper ES, Hennessy EM, Morgan AS, Costeloe KL . Perinatal outcomes for extremely preterm babies in relation to place of birth in England: the EPICure 2 study. Arch Dis Child Fetal Neonatal Ed 2014; 99: F181–F188.
Tarnow-Mordi WO, Hau C, Warden A, Shearer AJ . Hospital mortality in relation to staff workload: a 4-year study in an adult intensive-care unit. Lancet 2000; 356: 185–189.
Giraud T, Dhainaut JF, Vaxelaire JF, Joseph T, Journois D, Bleichner G et al. Iatrogenic complications in adult intensive care units: a prospective two-center study. Crit Care Med 1993; 21: 40–51.
Donchin Y, Gopher D, Olin M, Badihi Y, Biesky M, Sprung CL et al. A look into the nature and causes of human errors in the intensive care unit. Crit Care Med 1995; 23: 294–300.
Clark K, Normile L . Nursing informatics and data collection from the electronic medical record: Study of characteristics, factors and occupancy impacting outcomes of critical care admissions from the Emergency Department. Health Informatics J 2012; 18: 309–319.
Boyle J, Zeitz K, Hoffman R, Khanna S, Beltrame J . Probability of severe adverse events as a function of hospital occupancy. IEEE J Biomed Health Inform 2014; 18: 15–20.
Volpe FM, Magalhaes AC, Rocha AR . High bed occupancy rates: Are they a risk for patients and staff? Int J Evid Based Healthc 2013; 11: 312–316.
Whitfield M, Chessex P . The need for public involvement when operating a regionalized neonatal care system at maximum capacity. Paediatr Child Health 2010; 15: 573–575.
Howell EM, Richardson D, Ginsburg P, Foot B . Deregionalization of neonatal intensive care in urban areas. Am J Public Health 2002; 92: 119–124.
Caveney AF, Silbergleit R, Frederiksen S, Meurer WJ, Hickenbottom SL, Smith RW et al. Resource utilization and outcome at a university versus a community teaching hospital in tPA treated stroke patients: a retropsective cohort study. BMC Health Serv Res 2010; 10: 44.
Acknowledgements
We thank the staff of the Canadian Neonatal Network (CNN) Coordinating Centre, Mr Junmin Yang for statistical support, and Dr Ruth Warre for editorial help during manuscript preparation. Although no funding was received specifically for this study, the CNN Coordinating Centre is based at the Maternal-Infant Care Research Centre (MiCare) at Mount Sinai Hospital, Toronto, Ontario, Canada. MiCare is supported by grant funding from the Canadian Institutes of Health Research and in-kind support from Mount Sinai Hospital, Toronto. Although no funding was received specifically for this study, the CNN Coordinating Centre is based at the Maternal-Infant Care Research Centre (MiCare) at Mount Sinai Hospital, Toronto, Ontario, Canada. MiCare is supported by grant funding from the Canadian Institutes of Health Research and in-kind support from Mount Sinai Hospital, Toronto.
Author Contributions
Dr Shah had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Shah, Mirea. Acquisition, analysis or interpretation of data: all authors. Drafting of the manuscript: Shah. Critical revision of the manuscript for important intellectual content: all authors. Statistical analysis: Mirea with assistance from Yang (additional contributor). Study supervision: Shah, Lee.
Disclosure
The funding agencies had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Site Investigators for the Canadian Neonatal Network (Collaborators):
Prakesh S Shah, MD, MSc (Director, Canadian Neonatal Network), Mount Sinai Hospital, Toronto, Ontario, Canada; Adele Harrison, MD, MBChB, Victoria General Hospital, Victoria, British Columbia, Canada; Anne Synnes, MDCM, MHSC, British Columbia Children’s Hospital, Vancouver, British Columbia, Canada; Todd Sokoran, MD, Royal Columbian Hospital, New Westminster, British Columbia, Canada and Surrey Memorial Hospital, Surrey, British Columbia, Canada; Wendy Yee, MD, Foothills Medical Centre, Calgary, Alberta, Canada; Khalid Aziz, MBBS, MA, MEd, Royal Alexandra Hospital, Edmonton, Alberta, Canada; Zarin Kalapesi, MD, Regina General Hospital, Regina, Saskatchewan, Canada; Koravangattu Sankaran, MD, MBBS, Royal University Hospital, Saskatoon, Saskatchewan, Canada; Mary Seshia, MBChB, Winnipeg Health Sciences Centre, Winnipeg, Manitoba, Canada; Ruben Alvaro, MD, St Boniface General Hospital, Winnipeg, Manitoba, Canada; Sandesh Shivananda, MBBS, MD, DM, Hamilton Health Sciences Centre, Hamilton, Ontario, Canada; Orlando Da Silva, MD, MSc, London Health Sciences Centre, London, Ontario, Canada; Chuks Nwaesei, MD, Windsor Regional Hospital, Windsor, Ontario, Canada; Kyong-Soon Lee, MD, MSc, Hospital for Sick Children, Toronto, Ontario, Canada; Michael Dunn, MD, Sunnybrook Health Sciences Centre, Toronto, Ontario, Canada; Nicole Rouvinez-Bouali, MD, Children’s Hospital of Eastern Ontario and Ottawa General Hospital, Ottawa, Ontario, Canada; Kimberly Dow, MD, Kingston General Hospital, Kingston, Ontario, Canada; Ermelinda Pelausa, MD, Jewish General Hospital, Montréal, Québec, Canada; Keith Barrington, MBChB, Hôpital Sainte-Justine, Montréal, Québec, Canada; Christine Drolet, MD, Centre Hospitalier Universitaire de Québec, Sainte Foy Québec, Canada; Patricia Riley, MD, MDCM, BSc, Montréal Children’s Hospital, Montréal, Québec, Canada and Royal Victoria Hospital, Montréal, Québec, Canada; Valerie Bertelle, MD, Centre Hospitalier Universitaire de Sherbrooke, Sherbrooke, Québec, Canada; Rody Canning, MD, Moncton Hospital, Moncton, New Brunswick, Canada; Barbara Bulleid, MD, Dr Everett Chalmers Hospital, Fredericton, New Brunswick, Canada; Cecil Ojah, MBBS, and Luis Monterrosa, MD, Saint John Regional Hospital, Saint John, New Brunswick, Canada; Akhil Deshpandey, MD, MBBS, Janeway Children’s Health and Rehabilitation Centre, St John’s, Newfoundland; Jehier Afifi, MB BCh, MSc, IWK Health Centre, Halifax, Nova Scotia, Canada; Andrzej Kajetanowicz, MD, Cape Breton Regional Hospital, Sydney, Nova Scotia, Canada; Shoo K Lee, MBBS, PhD (Chairman, Canadian Neonatal Network), Mount Sinai Hospital, Toronto, Ontario, Canada.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
Dr Prakesh Shah holds an Applied Research Chair in Reproductive and Child Health Services and Policy Research awarded by the Canadian Institutes of Health Research. The remaining authors declare no conflict of interest.
Additional information
A full list of Site Investigators for the Canadian Neonatal Network (Collaborators) is given before References.
Supplementary Information accompanies the paper on the Journal of Perinatology website
Supplementary information
Rights and permissions
About this article
Cite this article
Shah, P., Mirea, L., Ng, E. et al. Association of unit size, resource utilization and occupancy with outcomes of preterm infants. J Perinatol 35, 522–529 (2015). https://doi.org/10.1038/jp.2015.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2015.4
This article is cited by
-
Neonatal intensive care unit occupancy rate and probability of discharge of very preterm infants
Journal of Perinatology (2023)
-
Are birth outcomes in low risk birth cohorts related to hospital birth volumes? A systematic review
BMC Pregnancy and Childbirth (2021)
-
Association of nursing overtime, nurse staffing and unit occupancy with medical incidents and outcomes of very preterm infants
Journal of Perinatology (2018)
-
Volume, size, professionals' specialization and nutrition management of NICUs and their association with treatment quality in VLBW infants
Journal of Perinatology (2018)
-
A systematic review of neonatal treatment intensity scores and their potential application in low-resource setting hospitals for predicting mortality, morbidity and estimating resource use
Systematic Reviews (2017)