Abstract
Objective:
Sex is an important determinant of neonatal outcomes and may have a significant role in the physiologic response to maternal chorioamnionitis. Our goal was to determine cerebral blood flow (CBF) parameters by sex and subsequent neurodevelopment in healthy term infants exposed to chorioamnionitis.
Study Design:
CBF by Doppler ultrasound in anterior and middle cerebral (ACA, MCA) and basilar arteries were analyzed for time-averaged maximum velocity (TAMX) and corrected resistive index in 52 term control and chorioamnionitis-exposed infants between 24 and 72 h after birth. Placental pathology confirmed histologic evidence of chorioamnionitis (HC). Bayley Scales of Infant Development-III were administered at 12 months.
Result:
HC male infants had significantly greater TAMX in the MCA and lower mean MCA and ACA resistance than HC females. Abnormal CBF correlated negatively with neurodevelopmental outcome.
Conclusion:
CBF is altered in term infants with histologically confirmed chorioamnionitis compared with control infants with sex-specific differences.
Similar content being viewed by others
Introduction
Chorioamnionitis is a common complication of labor and delivery and results in increased fetal and neonatal morbidity and mortality at any gestational age.1, 2 Bacterial products cause the release of cytokines and activation of macrophages and neutrophils in the decidua and umbilical vessels. These pro-inflammatory mediators damage the brain parenchyma and vasculature without active fetal infection.3, 4, 5 Elevated pro-inflammatory cytokines also alter the permeability of the fetal blood–brain barrier and important mediators of fetal blood flow, nitric oxide and endothelin-1, rendering the neonate susceptible to further brain injury from relatively minor episodes of hypoxia-ischemia (HI).6, 7, 8, 9
In the fetus exposed to chorioamnionitis, white and gray matter brain injury may result from a combination of changes in cerebral blood flow (CBF) and as a direct result of inflammation,10 with long-term consequences of periventricular leukomalacia, cerebral palsy and cognitive deficits.2, 11, 12, 13 A meta-analysis of preterm and term infants showed increased risks of 80 to 140% for cerebral palsy if exposed to histological or clinical chorioamnionitis (CC).13 Even in well-appearing term infants, chorioamnionitis carries an attributable risk of 11% for spastic cerebral palsy (95% confidence interval=4 to 20%).1, 2, 11, 14 However, the majority of term and late preterm infants exposed to chorioamnionitis are treated as normal newborns and receive no special observation or developmental follow-up.
Male sex confers significant disadvantages in infant mortality and morbidity, including increased risk for neurological and psychological impairments such as autism, and deficits of speech, language, academic achievements and social functioning.15, 16, 17 Different inflammatory pathways are known to be activated in males and females, however, few investigations have focused on the mechanism of chorioamnionitis-induced brain inflammation in term infants by sex. One recent report in neonatal rats showed different regulation of CBF by nitric oxide synthase in male rats after HI.18 Our goal in this pilot project was to determine differences in CBF in the first few days of life in term infants when exposed to chorioamnionitis versus control infants by sex. We hypothesized that the male infant exposed to chorioamnionitis would demonstrate significant changes in CBF and demonstrate a greater susceptibility to inflammatory brain injury, which would correlate with neurodevelopmental outcomes at 1 year of life. This is the first report that sex may have an influence on blood flow regulation in the inflamed fetal brain.
Methods
Subjects
This prospective pilot study was approved by the Institutional Review Board of the Medical University of South Carolina (MUSC). Parental consent was obtained before enrollment of infants born ⩾37 weeks of gestation to mothers with and without chorioamnionitis at MUSC from October 2006 to October 2007. To ensure availability of a single ultrasonographer and pathologist, enrollment took place Monday to Friday during regular working hours.
CC was defined by MUSC obstetricians according to standard criteria19 of maternal fever >100.4 °F with two of the following: uterine tenderness, maternal leukocytosis >12 000 cell per mm, fetal tachycardia >160 b.p.m., purulent or foul smelling vaginal discharge or maternal tachycardia >100 b.p.m. All mothers with chorioamnionitis were treated with broad spectrum antibiotics before delivery. Control participants had no evidence of chorioamnionitis and were not treated with antibiotics. Exclusion criteria were major genetic or congenital abnormality, multiple gestation, use of corticosteroids during pregnancy or participation in a therapeutic trial.
Study design
The umbilical cord and placenta were evaluated by a single, blinded pathologist for histological chorioamnionitis (HC) with fetal inflammatory response, using histologic criteria for intensity (grade) and disease progression (stage) defined by the Perinatal Section of the Society for Pediatric Pathology.20 As neurologic impairment is associated with fetal chorioamnionitis and chorionic plate thrombi, the placenta was also studied for vascular lesions.21 Participants were characterized as CC (histological criteria not met) or HC cohorts.
A single, blinded, certified school psychologist performed the Bayley Scales of Infant Development III at 1 year of age (11 to 14 months).
Cranial ultrasound with Doppler blood flow
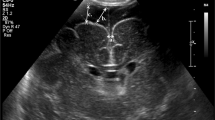
Between 24 and 72 h after birth, a cranial Doppler ultrasound was performed with spectral tracings of the middle (MCA), anterior (ACA) and basilar (BA) cerebral arteries by a single, blinded pediatric radiology technician. All scans were performed using the anterior fontanelle and temporal fossa windows with an 8 mHz transducer (Acuson Sequoia, Siemens, Mountain View, CA, USA). Analyses of the spectral wave were performed by a single, blinded pediatric radiologist for the time-averaged maximum velocity (TAMX) over a 1-min interval and the corrected resistive index(CRI) for infant heart rate.
Statistical analysis
Primary outcomes were differences in TAMX and CRI in the MCA, ACA and BA, between chorioamnionitis exposed infants and controls by sex. Bayley III scores were secondary outcomes. TAMX standard deviation of ±5 ml min−1 was estimated based on previous reports.22
Differences in maternal and infant demographic characteristics among the HC, CC and control groups were assessed using χ2 or Fisher’s exact test for categorical variables and analysis of variance for continuous variables. Differences in hemodynamic measures between HC infants and controls were assessed using Student’s t-test. Pearson correlation coefficients were used to relate all continuous hemodynamic measures to one another. MCA, ACA and BA parameters were considered within a given participant and between participants. Significance was set at P<0.05. Statistical analyses were conducted using SPSS 15.0 (SPSS Inc., Chicago, IL, USA).
Results
Fifty-three infants were enrolled, and 52 participants (17 controls, 35 chorioamnionitis) had Doppler studies for analysis. CC mothers (n=7) had fever but negative placental pathology or unavailable pathology (n=3). HC (n=28, 13 females, 15 males) had confirmed placental inflammation, whereas control study participants mothers had no clinical signs of chorioamnionitis (n=17, 10 females, 7 males). No CC or HC infant had positive blood cultures, but all received empiric antibiotics discontinued at 48 h, except for one infant treated for 7 days based on bandemia on a complete blood count. All study participants were cared for in the level 1 nursery. Demographics analyses showed no significant differences among control, HC and CC groups, or between males and females (Table 1). HC was present in 80% of enrolled chorioamnionitis mothers.
CBF was altered in infants exposed to chorioamnionitis compared with control infants
Between the HC and control groups, there were no significant differences in TAMX or CRI in any vessel in the combined gender analysis. However, when analyzed by sex, HC females had significantly lower mean MCA TAMX (P=0.029) and a lower mean ACA TAMX (P=0.064) compared with control females (Table 2). HC males had significantly higher mean MCA TAMX and lower CRI than control males (P=0.016, P=0.054, respectively).
In the combined female/male group, although the sample size was small, CC had significantly lower CRI values in the MCA (P=0.004) and BA (P=0.041), and lower ACA CRI (P=0.058) compared with those in the control group. CBF measures in HC were not different than CC in the combined sex group or in males. However, HC females had higher mean CRI in all three vessels compared with CC females (P⩽0.03). Because of this finding and the low number of CC patients, we did not combine the HC and CC groups. Thus, the HC group included only patients with histologically confirmed chorioamnionitis (n=28, 13 females and 15 males).
Chorioamnionitis was associated with asynchronous CBF
TAMX measurements in all three vessels were strongly correlated in the control group (P<0.008). However, in the infants with funisitis (HC), TAMX measures in the MCA and BA did not correlate, suggesting an alteration of normal synchrony of CBF. ACA velocities correlated with both MCA (r=0.527, P=0.004) and the BA (r=0.605, P=0.001) individually.
Males exposed to chorioamnionitis had significantly higher CBF
Within the HC group, males had a significantly higher mean MCA TAMX (P=0.003) and lower mean CRI in the MCA and ACA than females (P=0.001, P=0.044, respectively). Control females tended to have a higher mean MCA TAMX than males (P=0.060; Table 2).
There were no differences in TAMX or CRI between the control and HC groups in any vessel when analyzing the group as a whole. When sex was considered between the control and HC group, there were complex differences noted (Table 2, Figure 1). Among males, HC was associated with significantly higher TAMX and lower CRI in the MCA compared with controls (TAMX P=0.016, CRI P=0.054). However, the converse was found in females, as HC females had lower mean TAMX in the MCA (P=0.029) and in the ACA (P=0.064) compared with controls. BA TAMX or CRI were not significantly different for either sex.
Time-averaged maximum velocity (TAMX) by artery, sex and presence of histological chorioamnionitis (HC). ACA, anterior cerebral artery; BA, basilar artery; MCA, middle cerebral artery. *P<0.05 between control males and HC males; †P<0.05 between control females and HC females; ‡P<0.05 between HC males and HC females.
Mean Bayley outcome scores did not differ by HC or sex
Bayley examinations were performed on 59% controls (10/17) and 64% HC patients (18/28) at a mean age of 11.5±0.7 months (range: 11.0 to 13.9 months). Given that 62% of study subjects showed for the 1-year neurodevelopment assessment, statistical analyses were conducted to compare baseline characteristics of those who followed-up and those that did not at 1 year. There were no baseline characteristic differences between those two groups. Of those infants who had neurodevelopmental follow-up, a total of seven infants had at-risk scores in at least one domain (one male and one female control, three HC males). At-risk Bayley gross motor scores were present in three HC males and one female and male in the control group. At-risk scores for expressive language were found in one HC male, and for receptive language in one control female.
CBF measures correlated with Bayley Scales of Infant Development (BSID) scores in males and females in the HC group
Doppler blood flow measures correlated with Bayley scores at 12 months for HC males and females (Table 3). The ACA TAMX, which supplies the corpus callosum, correlated negatively with cognitive and motor composite scores and specific domains of personal-social skills and problem solving in males. The MCA TAMX also correlated with problem-solving skills in HC males. Conversely, ACA and BA CRIs correlated positively with language outcome scores in HC males. Taken together, these results indicate that the higher the blood flow and the lower the resistance, the lower the Bayley scores at 12 months in HC males. In HC females, blood flow changes from controls were in the opposite direction compared with HC males, and the MCA TAMX correlated positively with fine motor skills, and BA CRI correlated negatively with personal-social skills.
Discussion
In the clinical setting of chorioamnionitis, fetal inflammation is well established before uterine contractions and cord compression during delivery result in serial episodes of relative HI. Fetal sheep without inflammation were able to rapidly recover CBF by shifting blood flow to protect the brain, whereas those with inflammation were unable to fully respond when a secondary HI insult occurred.6, 23, 24
In the face of a global HI insult, the fetal animal will divert blood from cortical areas to protect deep brain structures that are more metabolically active and at greater risk of significant injury.25, 26, 27 Differential blood flow between white matter, cortical gray matter and deep gray nuclei has been shown in term asphyxiated infants within 1 to 6 days of life.28 Our chorioamnionitis infants had decreased resistance in most of the major cerebral vessels compared with controls, with HC males being more affected than HC females. Male HC infants had lower resistance and increased TAMX in the ACA and MCA compared with the BA, suggesting increased CBF in areas of inflammation. However, we also demonstrate a loss of correlation of vascular resistance between vessels in all HC infants, which were tightly correlated in our control infants. These results are consistent with independent regulation of vessels and a shift of blood flow within brain regions in the chorioamnionitis exposed infants. Cardiac dysfunction is a possible explanation for increases in CBF in the HC group, but our infants were asymptomatic, healthy term newborns without differences in heart rate between control and HC or sexes.23, 29, 30, 31
Given the higher than normal CBF because of inflammation in the male infant, it is speculated that this may be a marker for risk for brain injury because of chorioamnionitis. The ACA TAMX in HC males was significantly negatively correlated with both motor and cognitive composite scores, as well as personal-social and problem-solving skills. The ACA supplies the corpus callosum, and injury in this white matter tract is associated with negative neurodevelopmental outcome.32 The ACA also supplies the frontal lobe, which is associated with difficulties with executive function and behavior later in childhood.33 Therefore, increased CBF in the ACA in HC male infants may indicate a particular susceptibility of the male brain to inflammation, particularly in the corpus callosum and frontal lobe.
Although Bonnin used a different neuroinflammatory model, evidence from his neonatal rat stroke model shows that endothelial nitric oxide synthase and neuronal nitric oxide synthase activity are differentially regulated by phosphorylation between males and females, resulting in increased blood flow and aggravated HI injury in males. These mechanistic experimental data agree with our evidence in term human neonates exposed to chorioamnionitis presented in this manuscript.18 Male fetuses also have significantly greater release of pro-inflammatory cytokines compared with the female after ex vivo lipopolysaccaride stimulation demonstrating a sex-differential immune response in fetal life.34 Lambermont reported increased WBC response in bronchoalveolar lavage fluid and worse lung compliance in male lambs exposed to chorioamnionitis.35 This higher level of pro-inflammatory response in male fetuses is consistent with our findings of increased CBF and lower vascular resistance in males HC infants. We also found that sex differences in CBF are present in normal term infants within 72 h of birth, with control females demonstrating a higher TAMX in cerebral blood vessels than male infants, consistent with previous reports in older children and adults.36 Interestingly, different patterns of gene expression between the sexes in brain cells have been demonstrated before sex hormone maturation.37, 38 Epigenetic modification of gene expression and its role in fetal adaptation to a perinatal insult is a mechanism that could possibly explain our sex differences in chorioamnionitis infants.39 Alternatively, different intracellular post-translational modifications, as in Bonnin’s report, may also account for differential blood flow in response to an inflammatory stimulus. Taken together, these data offer compelling evidence that males may mount a more robust immune response, which may result in increased blood flow and propensity to brain injury in males.
For the pediatrician, neonatologist and care-provider, the neurodevelopmental risk of an infant exposed to chorioamnionitis would seem to be clinically paramount. None of our patients were known to suffer an adverse event at the time of delivery or in the neonatal period, and BSID III scores were within the ‘normal’ range. Nevertheless, particularly in male infants with confirmed chorioamnionitis, lower scores (80 to 90) were associated with the highest TAMX. Julkunen also found that increased CBF by Doppler was a better predictor of adverse neurological outcomes at 1 year of age in asphyxiated infants as compared with other markers.40 Elevated CBF in HC males may either directly contribute to lower scores in males or indirectly serve as a marker of fetal brain inflammation. Although correlations did exist between blood flow parameters and BSID scores for long-term outcomes, these data are speculative and not as strong as the primary outcome of sex-specific CBF data. Further investigation of CBF as a bedside measure will help define its usefulness in infants with inflammatory insult.
In summary, this is the first study to demonstrate changes in CBF soon after birth in infants with histologically confirmed chorioamnionitis compared with control infants with sex-specific differences. As most chorioamnionitis infants are discharged at 48 h and receive no special follow-up, these results are provocative. Limitations of this pilot study are small numbers, a single Doppler ultrasound and 62% neurodevelopmental follow-up at 1 year. Given the small number of infants in the CC group, these study subjects were not included and the major conclusions compared only the control infants to the histologic chorioamnionitis group. In addition, this is an exploratory pilot study, and results are not adjusted for multiple comparisons. Future studies with larger sample sizes are needed to verify our findings. Nevertheless, our results provide proof of concept that differences in CBF may be present and may indicate subtle neuroinflammation associated with the fetal response to chorioamnionitis. The observed changes in CBF suggest both a mechanism and a biomarker for subtle pathology and unexplained neurologic deficits in this population, and in particular, highlight the disadvantage the male infant may encounter in utero secondary to inflammatory exposure. Previous research has focused on the preterm infant, but our results demonstrate the importance of the inflammatory process in well-appearing term infants exposed to chorioamnionitis, and should prompt us to address important clinical questions of whether these infants also need closer evaluation and follow-up through school age.
References
Grether JK, Nelson KB . Maternal infection and cerebral palsy in infants of normal birth weight. JAMA 1997; 278 (3): 207–211.
Wu YW, Colford JM Jr. . Chorioamnionitis as a risk factor for cerebral palsy: a meta-analysis. JAMA 2000; 284 (11): 1417–1424.
Patrick LA, Gaudet LM, Farley AE, Rossiter JP, Tomalty LL, Smith GN . Development of a guinea pig model of chorioamnionitis and fetal brain injury. Am J Obstet Gynecol 2004; 191 (4): 1205–1211.
Dammann O, O'Shea TM . Cytokines and perinatal brain damage. Clin Perinatol 2008; 35 (4): 643–663 v.
Malaeb S, Dammann O . Fetal inflammatory response and brain injury in the preterm newborn. J Child Neurol 2009; 24 (9): 1119–1126.
Garnier Y, Coumans A, Berger R, Jensen A, Hasaart TH . Endotoxemia severely affects circulation during normoxia and asphyxia in immature fetal sheep. J Soc Gynecol Investig 2001; 8 (3): 134–142.
Garnier Y, Coumans AB, Jensen A, Hasaart TH, Berger R . Infection-related perinatal brain injury: the pathogenic role of impaired fetal cardiovascular control. J Soc Gynecol Investig 2003; 10 (8): 450–459.
Coumans AB, Garnier Y, Supcun S, Jensen A, Berger R, Hasaart TH . Nitric oxide and fetal organ blood flow during normoxia and hypoxemia in endotoxin-treated fetal sheep. Obstet Gynecol 2005; 105 (1): 145–155.
Adamson SL, Whiteley KJ, Langille BL . Endothelin-1 constricts fetoplacental microcirculation and decreases fetal O2 consumption in sheep. Am J Physiol 1996; 270 (1 Pt 2): H16–H23.
Eklind S, Mallard C, Leverin AL, Gilland E, Blomgren K, Mattsby-Baltzer I et al. . Bacterial endotoxin sensitizes the immature brain to hypoxic—ischaemic injury. Eur J Neurosci 2001; 13 (6): 1101–1106.
Wu YW, Escobar GJ, Grether JK, Croen LA, Greene JD, Newman TB . Chorioamnionitis and cerebral palsy in term and near-term infants. JAMA 2003; 290 (20): 2677–2684.
Boksa P . Effects of prenatal infection on brain development and behavior: a review of findings from animal models. Brain Behav Immun 2010; 24 (6): 881–897.
Shatrov JG, Birch SC, Lam LT, Quinlivan JA, McIntyre S, Mendz GL . Chorioamnionitis and cerebral palsy: a meta-analysis. Obstet Gynecol 2010; 116 (2 Pt 1): 387–392.
De Felice C, Del Vecchio A, Criscuolo M, Lozupone A, Parrini S, Latini G . Early postnatal changes in the perfusion index in term newborns with subclinical chorioamnionitis. Arch Dis Child Fetal Neonatal Ed 2005; 90 (5): F411–F414.
Johnson EO, Breslau N . Increased risk of learning disabilities in low birth weight boys at age 11 years. Biol Psychiatry 2000; 47 (6): 490–500.
Hindmarsh GJ, O'Callaghan MJ, Mohay HA, Rogers YM . Gender differences in cognitive abilities at 2 years in ELBW infants. Extremely low birth weight. Early Hum Dev 2000; 60 (2): 115–122.
Stevenson DK, Verter J, Fanaroff AA, Oh W, Ehrenkranz RA, Shankaran S et al. Sex differences in outcomes of very low birthweight infants: the newborn male disadvantage. Arch Dis Child Fetal Neonatal Ed 2000; 83 (3): F182–F185.
Bonnin P, Leger PL, Villapol S, Deroide N, Gressens P, Pocard M et al. Dual action of NO synthases on blood flow and infarct volume consecutive to neonatal focal cerebral ischemia. Exp Neurol 2012; 236 (1): 50–57.
Newton ER . Chorioamnionitis and intraamniotic infection. Clin Obstet Gynecol 1993; 36 (4): 795–808.
Redline RW, Faye-Petersen O, Heller D, Qureshi F, Savell V, Vogler C . Amniotic infection syndrome: nosology and reproducibility of placental reaction patterns. Pediatr Dev Pathol 2003; 6 (5): 435–448.
Redline RW, Wilson-Costello D, Borawski E, Fanaroff AA, Hack M . Placental lesions associated with neurologic impairment and cerebral palsy in very low-birth-weight infants. Arch Pathol Lab Med 1998; 122 (12): 1091–1098.
Kehrer M, Goelz R, Krageloh-Mann I, Schoning M . Measurement of volume of cerebral blood flow in healthy preterm and term neonates with ultrasound. Lancet 2002; 360 (9347): 1749–1750.
Saito M, Matsuda T, Okuyama K, Kobayashi Y, Kitanishi R, Hanita T et al. Effect of intrauterine inflammation on fetal cerebral hemodynamics and white-matter injury in chronically instrumented fetal sheep. Am J Obstet Gynecol 2009; 200 (6): 663 e1–11.
Fu J, Olofsson P . Restrained cerebral hyperperfusion in response to superimposed acute hypoxemia in growth-restricted human fetuses with established brain-sparing blood flow. Early Hum Dev 2006; 82 (3): 211–216.
Ashwal S, Dale PS, Longo LD . Regional cerebral blood flow: studies in the fetal lamb during hypoxia, hypercapnia, acidosis, and hypotension. Pediatr Res 1984; 18 (12): 1309–1316.
Lou HC, Tweed WA, Davies JM . Preferential blood flow increase to the brain stem in moderate neonatal hypoxia: reversal by naloxone. Eur J Pediatr 1985; 144 (3): 225–227.
Yan EB, Baburamani AA, Walker AM, Walker DW . Changes in cerebral blood flow, cerebral metabolites, and breathing movements in the sheep fetus following asphyxia produced by occlusion of the umbilical cord. Am J Physiol Regul Integr Comp Physiol 2009; 297 (1): R60–R69.
Wintermark P, Hansen A, Gregas MC, Soul J, Labrecque M, Robertson RL et al. Brain perfusion in asphyxiated newborns treated with therapeutic hypothermia. AJNR American journal of neuroradiology 2011; 32 (11): 2023–2029.
Seehase M, Gantert M, Ladenburger A, Garnier Y, Kunzmann S, Thomas W et al. Myocardial response in preterm fetal sheep exposed to systemic endotoxinaemia. Pediatr Res 2011; 70 (3): 242–246.
Abdulkadir AA, Kimimasa T, Bell MJ, Macpherson TA, Keller BB, Yanowitz TD . Placental inflammation and fetal hemodynamics in a rat model of chorioamnionitis. Pediatr Res 2010; 68 (6): 513–518.
Feng SY, Samarasinghe T, Phillips DJ, Alexiou T, Hollis JH, Yu VY et al. Acute and chronic effects of endotoxin on cerebral circulation in lambs. Am J Physiol Regul Integr Comp Physiol 2010; 298 (3): R760–R766.
Andrews JS, Ben-Shachar M, Yeatman JD, Flom LL, Luna B, Feldman HM . Reading performance correlates with white-matter properties in preterm and term children. Dev Med Child Neurol 2010; 52 (6): e94–100.
Cai W, Leung HC . Rule-guided executive control of response inhibition: functional topography of the inferior frontal cortex. PLoS One 2011; 6 (6): e20840.
Kim-Fine S, Regnault TR, Lee JS, Gimbel SA, Greenspoon JA, Fairbairn J et al. Male gender promotes an increased inflammatory response to lipopolysaccharide in umbilical vein blood. J Matern Fetal Neonatal Med 2012; 25 (11): 2470–2474.
Lambermont VA, Been JV, Kunzmann S, Vanterpool SF, Newnham JP, Kallapur SG et al. Sex differences in lung gas volumes after lipopolysaccharide-induced chorioamnionitis in fetal sheep. Gender medicine 2012; 9 (4): 278–286.
Tontisirin N, Muangman SL, Suz P, Pihoker C, Fisk D, Moore A et al. Early childhood gender differences in anterior and posterior cerebral blood flow velocity and autoregulation. Pediatrics 2007; 119 (3): e610–e615.
Dewing P, Shi T, Horvath S, Vilain E . Sexually dimorphic gene expression in mouse brain precedes gonadal differentiation. Brain Res Mol Brain Res 2003; 118 (1-2): 82–90.
Arnold AP, Burgoyne PS . Are XX and XY brain cells intrinsically different? Trends Endocrinol Metab 2004; 15 (1): 6–11.
Joss-Moore LA, Metcalfe DB, Albertine KH, McKnight RA, Lane RH . Epigenetics and fetal adaptation to perinatal events: diversity through fidelity. J Anim Sci 2010; 88 (13 Suppl): E216–E222.
Julkunen MK, Uotila J, Eriksson K, Janas M, Luukkaala T, Tammela O . Obstetric parameters and Doppler findings in cerebral circulation as predictors of 1 year neurodevelopmental outcome in asphyxiated infants. J Perinatol 2012; 32 (8): 631–638.
Acknowledgements
This study was funded by SCOR grant from NICHD through the Women’s Research Center at MUSC, project #P50DA016511; Clinical Translational Research Center Grant UL1 RR029882.
We acknowledge Charlene Fessler, B.S. and R.D.M.S for performing all ultrasound studies; the Clinical and Translational Research Center; Renee Martin, M.D., for statistical advice; Thomas Hulsey, PhD, and Myla Ebeling, RA, for their initial advice on study structure; and most importantly, our study patients and their parents.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Koch, F., Wagner, C., Jenkins, D. et al. Sex differences in cerebral blood flow following chorioamnionitis in healthy term infants. J Perinatol 34, 197–202 (2014). https://doi.org/10.1038/jp.2013.179
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2013.179


