Abstract
Objective:
To evaluate the hemodynamic changes occurring after rescue surfactant dosing in relation to the clinical respiratory response in preterm infants with respiratory distress syndrome.
Study Design:
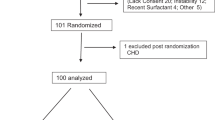
We studied 20 infants who received surfactant (poractant alfa) after failing continuous positive airway pressure (CPAP) beyond 2 h of life. Consecutive echocardiograms were performed before the surfactant dose, 10 min after and 1 h after the surfactant dose. Superior vena cava flow, right ventricular output, atrial and patent ductus arteriosus diameter and direction of shunting were measured. A surfactant responder (SR) was defined as an infant whose inspired fraction of oxygen was reduced to air (0.21) by 3 h after surfactant administration. A surfactant non-responder (SNR) was defined as an infant who remained on more than 0.21 at 3 h postsurfactant administration. Concurrent physiological parameters (heart rate, transcutaneous CO2, mean arterial blood pressure, mean airway pressure) were also recorded. Subject characteristics were compared relative to noted hemodynamic effects.
Results:
Of the 20 infants enrolled in the study, 12 were SR. These infants received surfactant earlier and had increased measures of systemic blood flow after receipt of surfactant compared with baseline. SNR did not have changes in systemic blood flow from baseline after surfactant dosing. There was no change in ductal shunting or atrial shunting between the two groups.
Conclusions:
A good clinical response to rescue surfactant is seen in infants who received surfactant earlier and is associated with increase in systemic blood flow. Timing of rescue surfactant administration needs to be further evaluated in larger prospective studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Soll F . Prophylactic natural surfactant extract for preventing morbidity and mortality in preterm infants. Cochrane Database Syst Rev 2000; CD000511.
Finer NN, Carlo WA, Walsh MC, Rich W, Gantz MG, Laptook AR et al. Early CPAP versus surfactant in extremely preterm infants. N Engl J Med 2010; 362: 1970–1979.
Sandri F, Plavka R, Simeoni U . CURPAP Advisory Board. The CURPAP study: an international randomized controlled trial to evaluate the efficacy of combining prophylactic surfactant and early nasal continuous positive airway pressure in very preterm infants. Neonatology 2008; 94 (1): 60–62.
Dunn MS, Kaempf J, de Klerk A, de Klerk R, Reilly M, Howard D et al. Randomized trial comparing 3 approaches to the initial respiratory management of preterm neonates. Pediatrics 2011; 128: 1069–1076.
Shangle CE, Haas RH, Vaida F, Rich WD, Finer NN . Effects of endotracheal intubation and surfactant on a 3-channel neonatal electroencephalogram. J Pediatr 2012; 161 (2): 252–257.
McPherson C, Gal P, Ransom JL, Carlos RQ, Dimaguila MA, Smith M et al. Indomethacin pharmacodynamics are altered by surfactant: a possible challenge to current indomethacin dosing guidelines created before surfactant availability. Pediatr Cardiol 2010; 31 (4): 505–510.
Raju TN, Langenberg P . Pulmonary hemorrhage and exogenous surfactant therapy: a metaanalysis. J Pediatr 1993; 123: 603–610.
Saliba E, Nashashibi M, Vaillant MC, Nasr C, Laugier J . Instillation rate effects of Exosurf on cerebral and cardiovascular haemodynamics in preterm neonates. Arch Dis Child Fetal Neonatal Ed 1994; 71: F174–F178.
Rabe H, Jorch G . Cerebral hemodynamics in perinatal pharmacology. Dev Pharmacol Ther 1991; 17: 128–132.
Cowan F, Whitelaw A, Wertheim D, Silverman M . Cerebral blood flow velocity changes after rapid administration of surfactant. Arch Dis Child 1991; 66: 1105–1109.
Roll C, Knief J, Horsch S, Hanssler L . Effect of surfactant administration on cerebral haemodynamics and oxygenation in premature infants—a near infrared spectroscopy study. Neuropediatrics 2000; 31: 16–23.
Seppanen M, Kaapa P, Kero P . Acute effects of synthetic surfactant replacement on pulmonary blood flow in neonatal respiratory distress syndrome. Am J Perinatol 1994; 11: 382–385.
Hamdan AH, Shaw NJ . Changes in pulmonary artery pressure in infants with respiratory distress syndrome following treatment with Exosurf. Arch Dis Child Fetal Neonatal Ed 1995; 72: F176–F179.
Bloom MC, Roques-Gineste M, Fries F, Lelong-Tissier MC . Pulmonary haemodynamics after surfactant replacement in severe neonatal respiratory distress syndrome. Arch Dis Child Fetal Neonatal Ed 1995; 73: F95–F98.
Chu J, Clements JA, Cotton EK, Klaus MH, Sweet AY, Tooley WH et al. Neonatal pulmonary ischemia. I. Clinical and physiological studies. Pediatrics 1967; 40: 709–782.
Sehgal A, Mak W, Dunn M, Kelly E, Whyte H, McCrindle B et al. Haemodynamic changes after delivery room surfactant administration to very low birth weight infants. Arch Dis Child Fetal Neonatal Ed 2010; 95 (5): F345–F351.
Kluckow M, Evans N . Superior vena cava flow in newborn infants: a novel marker of systemic blood flow. Arch Dis Child Fetal Neonatal Ed 2000; 82: F182–F187.
Hunt RW, Evans N, Rieger I, Kluckow M . Low superior vena cava flow and neurodevelopment at 3 years in very preterm infants. J Pediatr 2004; 145: 588–592.
Kluckow M, Evans N . Low superior vena cava flow and intraventricular haemorrhage in preterm infants. Arch Dis Child Fetal Neonatal Ed 2000; 82 (3): F188–F194.
Evans N, Kluckow M, Currie A . Range of echocardiographic findings in term neonates with high oxygen requirements. Arch Dis Child Fetal Neonatal Ed 1998; 78: F105–F111.
Wiswell TE . Expanded uses of surfactant therapy. Clin Perinatol 2001; 3: 695–711.
Kluckow M, Gill A, Jefferey M Evans N Ductal Echocardiographic Targeting and Early Closure Trial (DETECT): A Pilot Randomised Control Trial E-PAS;1675.5 2012.
Evans N, Gournay V, Cabanas F, Kluckow M, Leone T, Groves A et al. Point-of-care ultrasound in the neonatal intensive care unit: international perspectives. Semin Fetal Neonatal Med 2011; 16 (1): 61–68.
Acknowledgements
The authors did not receive any financial support for the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Katheria, A., Leone, T. Changes in hemodynamics after rescue surfactant administration. J Perinatol 33, 525–528 (2013). https://doi.org/10.1038/jp.2012.166
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2012.166
Keywords
This article is cited by
-
A novel delivery system for supraglottic atomization allows increased lung deposition rates of pulmonary surfactant in newborn piglets
Pediatric Research (2020)
-
Timing of umbilical cord clamping among infants born at 22 through 27 weeks’ gestation
Journal of Perinatology (2016)