Abstract
In men, follicle-stimulating hormone (FSH) acts on the seminiferous tubules and enhances spermatogenesis. Recently, a candidate locus (rs2414095) for FSH levels was identified by a genome-wide association study (GWAS) in Chinese men. The rs2414095 single-nucleotide polymorphism (SNP) is found on the third intron of the cytochrome P450, family 19, subfamily A, peptide 1 (CYP19A1) gene encoding an aromatase. In the present study, we performed a replication study in 1687 Japanese men (901 from cohort 1 and 786 from cohort 2) to assess whether this SNP is associated with circulating FSH levels. Furthermore, we investigated whether the rs2414095 SNP is correlated with semen quality traits in 2015 Japanese men (1224 from cohort 1 and 791 from cohort 2). The rs2414095 SNP was significantly associated with circulating FSH levels (βSTD=0.15, P=9.7 × 10-5), sperm concentration (βSTD=0.073, P=0.032) and total sperm number (TSN) (βSTD=0.074, P=0.027) in a combined analysis of the two Japanese male cohorts. We successfully replicated, in Japanese men, the results of the previous GWAS for the rs2414095 SNP in Chinese men, and found that the rs2414095 SNP was related with sperm production.
Similar content being viewed by others

Introduction
The gonadotropin-releasing hormone secreted by the hypothalamus stimulates the production of luteinizing hormone (LH) and follicle-stimulating hormone (FSH) by the pituitary gland. LH acts on Leydig cells in the testes and induces testosterone secretion.1, 2 The main action of testosterone is the development of sexual characteristics and genitalia. Sex hormone-binding globulin (SHBG) binds to 50%−60% of the testosterone in circulation, and decreases the concentration of biologically active testosterone in circulation.3 Inhibin B is a peptide hormone, the synthesis and secretion of which is promoted by FSH. Secreted inhibin B in the circulation directly acts on adenohypophysis by a feedback mechanism, and specifically inhibits FSH secretion.4 In men, FSH stimulates Sertoli cells and increases sperm production.5, 6 Therefore, low levels of FSH decrease spermatogenesis.
It has been suggested that sex hormone levels are heritable.7, 8 However, little is known about the genetic determinants of sex hormone levels. Recently, a genome-wide association study (GWAS) in 3495 healthy Chinese men revealed that the rs2414095 single-nucleotide polymorphism (SNP) in cytochrome P450, family 19, subfamily A, polypeptide 1 (CYP19A1) at 15q21.2 was significantly associated with estradiol levels (P=6.5 × 10−31) and FSH levels (P=1.6 × 10−16).9 Here, we conducted a replication study to assess whether the rs2414095 SNP is associated with circulating FSH levels or other hormone levels (including testosterone, SHBG, LH, inhibin B and calculated free testosterone) in Japanese men. Furthermore, we conducted an association analysis for semen quality traits (including sperm concentration, semen volume, sperm motility, total sperm number (TSN) and/or total motile sperm number) to establish whether this SNP influences spermatogenesis.
Materials and methods
This study was approved by the ethics committees of the University of Tokushima and St Marianna Medical University. All participants provided written informed consent.
Two Japanese cohort samples
Two Japanese cohorts, 1224 young men from the general Japanese population (cohort 1: aged 20.8±1.7 years; mean±s.d.) and 791 Japanese men of proven fertility (cohort 2: aged 31.2±4.8 years; mean±s.d.), were included in this study. Among these subjects, the hormone levels of 901 men from cohort 1 and of 786 men from cohort 2 were measured and used for the replication study for FSH levels, and samples from all subjects were used for the association analysis for semen quality. Some of the subjects in this study have been described in previous reports.10, 11, 12, 13, 14, 15, 16, 17, 18, 19 Briefly, cohort 1 subjects consisted of male university students from four study centers based in the urology departments of university hospitals in four Japanese cities (Kawasaki, Kanazawa, Nagasaki and Sapporo). Cohort 2 subjects consisted of the partners of pregnant women who attended obstetric clinics in four Japanese cities (Sapporo, Kanazawa, Osaka and Fukuoka).
Measurement of clinical traits
Age, body weight and height were self-reported. Body mass index was calculated from body weight and height. Blood samples were obtained and analyzed as previously described.11, 12 Briefly, blood samples were drawn from the cubital vein of each subject usually in the mornings to reduce the effect of diurnal variations in hormone levels. Testosterone, SHBG, FSH and LH levels were determined using a time-resolved immunofluorometric assay (Delfia, Wallac, Turku, Finland), and inhibin B was measured by a specific two-sided enzyme immunometric assay (Serotec, Kidlington, UK) at the Department of Growth and Reproduction, Rigshospitalet, in Copenhagen, Denmark. Calculated free testosterone was calculated from a value of 1 × 109 mol l−1 for the association constant of SHBG to testosterone, a value of 3.6 × 104 mol l−1 for the association constant of albumin to testosterone and a fixed plasma albumin concentration of 43 g l−1 using Vermeulen’s formula.20 Semen samples were obtained and analyzed by using standardized protocols as previously described.11, 12 Briefly, semen samples were obtained by masturbation after sexual abstinence for at least 48 h and were ejaculated into clean, wide-necked, sterile and nontoxic collection containers. The samples were protected from temperature extremes and were liquefied at 37 °C before testing. The sperm concentration of each sample was assessed using a Bürker–Türk hemocytometer (Erma, Tokyo, Japan) after fixation with sodium bicarbonate–formaldehyde solution. Only sperm with tails were counted. Semen volume was measured with a graduated 5 ml syringe (Terumo, Tokyo, Japan). Sperm motility was assessed from 10 μl of well-mixed semen placed on a clean glass slide, covered and then examined microscopically at 400 × magnification at 37 °C on a microscope stage. The motility assessment was repeated twice, and the average value from two samples was calculated. The sperm were assessed using the World Health Organization motility classes A, B, C and D.21 In this study, sperm categorized as class A or B were considered motile.
Genotyping
Genomic DNA was extracted from the peripheral blood samples of subjects using a QIAamp DNA blood kit (Qiagen, Tokyo, Japan). The rs2414095 SNP was genotyped using TaqMan probes (C_15798408_20; Applied Biosystems, Tokyo, Japan) with the ABI 7900HT real-time PCR system (Applied Biosystems).
Statistical analysis
Hardy–Weinberg equilibrium was assessed in the two cohorts using Pearson’s χ2 test for genotypes.
To minimize deviation from a normal distribution, the analyses for testosterone, SHBG, FSH, LH, inhibin B and calculated free testosterone were processed using natural log-transformed variables, and sperm concentration, semen volume, TSN and total motile sperm number were processed using square-root transformed values. The associations between the rs2414095 SNP and sex hormone values were assessed using a standardized multiple linear regression test under an additive genetic model with adjustments for age and body mass index, and the associations between the rs2414095 SNP and semen quality traits were assessed using a standardized multiple linear regression test under an additive genetic model with adjustments for age, body mass index and ejaculation abstinence. Ejaculation abstinence and time from masturbation to test were additionally adjusted for in determining sperm motility and total motile sperm number.
The results from the two cohorts were combined in a meta-analysis using the meta package for R, version 3.1.2 (http://www.R-project.org/). The extent of heterogeneity among studies was quantified by the I2 statistic22 and statistically assessed by Cochran’s Q-test. If there was no heterogeneity, as determined by an I2 statistic <50% or a P-value >0.1, a fixed-effects model using the inverse variance method was used. Otherwise, the random-effects model using the DerSimonian and Laird method was used.
All statistical analyses were performed using R, version 3.1.2, and statistical significance was considered at P-values of <0.05.
Results
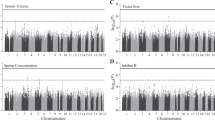
The characteristics of circulating sex hormones obtained from the two Japanese male cohorts are presented in Supplementary Table S1 as previously reported.12, 17 To investigate the associations between the rs2414095 SNP and circulating FSH levels, we genotyped the SNP in a total of 1687 men (901 from cohort 1 and 786 from cohort 2). The allele frequencies of the SNP analyzed in each cohort are shown in Table 1. The missing genotyping rate of the rs2414095 SNP was 0.1%. The genotypes of the SNP were in Hardy–Weinberg equilibrium in the two cohorts. Multiple linear regression analyses under the additive genetic model revealed that the rs2414095 SNP was significantly correlated with circulating FSH levels in both cohorts (βSTD=0.17, P=1.2 × 10-3 in cohort 1; βSTD=0.12, P=0.026 in cohort 2) (Table 1). In the meta-analysis of the two Japanese cohorts, we found that the rs2414095 SNP was significantly associated with circulating FSH levels (βSTD=0.15, P=9.7 × 10-5). The rs2414095 SNP contributed to 0.9% of variance in FSH levels.
We next investigated the associations between the rs2414095 SNP and other circulating hormone levels (including testosterone, SHBG, LH, inhibin B and calculated free testosterone) in the two Japanese male cohorts. We found that the rs2414095 SNP was significantly associated with circulating inhibin B levels in cohort 1 (βSTD=0.11, P=0.030), but not in cohort 2 (Table 2). In the meta-analysis of the two Japanese cohorts, the rs2414095 SNP was significantly associated with circulating inhibin B levels (βSTD=0.076, P=0.042).
We hypothesized that the SNP associated with FSH levels might influence sperm production, because FSH contributes to spermatogenesis.5, 6 To verify this, we performed an association study between the rs2414095 SNP and semen quality traits. The characteristics of semen parameters obtained from the two Japanese cohorts are presented in Supplementary Table S2 as previously reported.11, 12, 15, 18 The SNP was genotyped in a total of 2015 men (1224 from cohort 1 and 791 from cohort 2). The effect allele frequencies of this SNP was 0.29 in cohort 1 and 0.30 in cohort 2, and the genotypes of the SNP were in Hardy–Weinberg equilibrium in the two cohorts. Multiple linear regression analyses under the additive genetic model revealed that the rs2414095 SNP was significantly associated with sperm concentration (βSTD=0.11, P=0.016), TSN (βSTD=0.11, P=0.012) and total motile sperm number (βSTD=0.098, P=0.024) in cohort 1 (Table 3). However, this SNP did not display associations with semen parameters in cohort 2. In the meta-analysis of the two Japanese cohorts, we found that the rs2414095 SNP was significantly associated with sperm concentration (βSTD=0.073, P=0.032) and TSN (βSTD=0.074, P=0.027).
Discussion
A recent GWAS reported that the rs2414095 SNP was significantly associated with FSH levels in Chinese men.9 In this replication study, the rs2414095 SNP was found to significantly associate with FSH levels in a combined analysis of two cohorts in Japanese men. Therefore, we successfully validated the results of the association of the rs2414095 SNP from the previous GWAS.
The rs2414095 SNP is located on the third intron of the CYP19A1 gene that encodes aromatase. This enzyme is induced by FSH and LH secretion, and converts testosterone to estradiol (E2).23, 24, 25 Aromatase deficiency in men and women suppressed the concentration of estradiol, and elevated the concentrations of FSH and LH in circulation.26 The treatment of an aromatase inhibitor elevated serum FSH levels in nonobstructive azoospermia,27 in male breast cancer patients28 and in boys with delayed puberty.29 Insertion30 or missense31, 32, 33, 34, 35 mutations in the coding region of the CYP19A1 gene can cause aromatase deficiency. Mutations in the splicing site were also found in aromatase-deficient patients.35, 36, 37 Aromatase deficiency with mutations in the CYP19A1 gene resulted in markedly elevated FSH concentrations.32, 34, 38, 39, 40, 41 In this study, the A allele of the rs2414095 SNP was positively correlated with circulating FSH levels. The previous GWAS study reported that the G allele of the rs2414095 SNP was positively correlated with estradiol levels,9 indicating that the A allele of this SNP was negatively correlated with estradiol levels. Although the relationship between the rs24154095 SNP and aromatase expression and activity is unknown, it is suggested that the positive correlation between the A allele of this SNP and circulating FSH levels might depend on a positive feedback mechanism through decrease in the circulating estradiol levels. The rs2414095 SNP was also related with circulating inhibin B levels. Because the synthesis and secretion of inhibin B is promoted by FSH,4, 5, 6 it is suggested that the relationship between the rs2414095 SNP and inhibin B levels is an indirect connection through FSH levels. However, further studies are needed to elucidate the molecular mechanisms through which the rs24154095 SNP affects the respective circulating levels of FSH, E2 and inhibin B.
In this study, we found that the A allele of the rs2414095 SNP was positively correlated with sperm concentration and TSN. FSH activates Sertoli cells and induces spermatogenesis in the presence of testosterone.42 Therefore, the relationship between the rs2414095 SNP and sperm production may also be indirectly affected by FSH levels. Further replication studies using larger samples with different circulating FSH levels and low sperm concentrations such as azoospermic and/or oligozoospermic patients will be needed to provide compelling evidence for this association.
In summary, we replicated the association between the rs2414095 SNP and circulating FSH levels in Japanese men. In addition, we found that the rs2414095 SNP was associated with sperm production. It is suggested that the rs2414095 SNP has an indirect influence on spermatogenesis through regulating FSH levels.
References
Belchetz, P. E., Plant, T. M., Nakai, E. J. & Knobil, E. Hypophysial responses to continuous and intermittent delivery of hypopthalamic gonadotropin-releasing hormone. Science 202, 631–633 (1978).
Smith, M. A. & Vale, W. W. Desensitization to gonadotropin-releasing hormone observed in superfused pituitary cells on Cytodex beads. Endocrinology 108, 752–759 (1981).
Kaufman, J. M. & Vermeulen, A. The decline of androgen levels in elderly men and its clinical and therapeutic implications. Endocr. Rev. 26, 833–876 (2005).
Raivio, T., Toppari, J., Perheentupa, A., McNeilly, A. S. & Dunkel, L. Treatment of prepubertal gonadotrophin-deficient boys with recombinant human follicle-stimulating hormone. Lancet 350, 263–264 (1997).
Bonn, D. Male contraceptive research steps back into spotlight. Lancet 353, 302 (1999).
Amory, J. K. Progress and prospects in male hormonal contraception. Curr. Opin. Endocrinol. Diabetes Obes. 15, 255–260 (2008).
Ring, H. Z., Lessov, C. N., Reed, T., Marcus, R., Holloway, L., Swan, G. E. et al. Heritability of plasma sex hormones and hormone binding globulin in adult male twins. J. Clin. Endocrinol. Metab. 90, 3653–3658 (2005).
Kuijper, E. A., Lambalk, C. B., Boomsma, D. I., van der Sluis, S., Blankenstein, M. A., de Geus, E. J. et al. Heritability of reproductive hormones in adult male twins. Hum. Reprod. 22, 2153–2159 (2007).
Chen, Z., Tao, S., Gao, Y., Zhang, J., Hu, Y., Mo, L. et al. Genome-wide association study of sex hormones, gonadotropins and sex hormone-binding protein in Chinese men. J. Med. Genet. 50, 794–801 (2013).
Nakahori, Y., Sato, Y., Ewis, A. A., Iwamoto, T., Shinka, T., Nozawa, S. et al. Climatic influence on the reproductive characteristics of Japanese males. J. Hum. Genet. 57, 375–378 (2012).
Iwamoto, T., Nozawa, S., Yoshiike, M., Namiki, M., Koh, E., Kanaya, J. et al. Semen quality of fertile Japanese men: a cross-sectional population-based study of 792 men. BMJ Open 3, e002223 (2013).
Iwamoto, T., Nozawa, S., Mieno, M. N., Yamakawa, K., Baba, K., Yoshiike, M. et al. Semen quality of 1559 young men from four cities in Japan: a cross-sectional population-based study. BMJ Open 3, e002222 (2013).
Sato, Y., Shinka, T., Iwamoto, T., Yamauchi, A. & Nakahori, Y. Y chromosome haplogroup D2* lineage is associated with azoospermia in Japanese males. Biol. Reprod. 88, 107 (2013a).
Sato, Y., Jinam, T., Iwamoto, T., Yamauchi, A., Imoto, I., Inoue, I. et al. Replication study and meta-analysis of human non-obstructive azoospermia in Japanese populations. Biol. Reprod. 88, 87 (2013b).
Sato, Y., Iwamoto, T., Shinka, T., Nozawa, S., Yoshiike, M., Koh, E. et al. Y chromosome gr/gr subdeletion is associated with lower semen quality in young men from the general Japanese population but not in fertile Japanese men. Biol. Reprod. 90, 116 (2014a).
Sato, Y., Shinka, T., Ewis, A. A., Yamauchi, A., Iwamoto, T. & Nakahori, Y. Overview of genetic variation in the Y chromosome of modern Japanese males. Anthropol. Sci. 122, 131–136 (2014b).
Sato, Y., Shinka, T., Nozawa, S., Yoshiike, M., Koh, E., Kanaya, J. et al. Y chromosome haplogroup D2a1 is significantly associated with high levels of luteinizing hormone in Japanese men. Andrology 3, 520–525 (2015a).
Sato, Y., Tajima, A., Tsunematsu, K., Nozawa, S., Yoshiike, M., Koh, E. et al. Lack of replication of four candidate SNPs implicated in human male fertility traits: a large-scale population-based study. Hum. Reprod. 30, 1505–1509 (2015b).
Sato, Y., Tajima, A., Tsunematsu, K., Nozawa, S., Yoshiike, M., Koh, E. et al. An association study of four candidate loci for human male fertility traits with male infertility. Hum. Reprod. 30, 1510–1514 (2015c).
Vermeulen, A., Verdonck, L. & Kaufman, J. M. A critical evaluation of simple methods for the estimation of free testosterone in serum. J. Clin. Endocrinol. Metab. 84, 3666–3672 (1999).
World Health Organization.WHO Laboratory Manual for the Examination of Human Semen and Sperm-cervical Mucus Interaction. 4th edn (Cambridge University Press, Cambridge, UK, 1999).
Higgins, J. P, Thompson, S. G., Deeks, J. J. & Altman, D. G. Measuring inconsistency in meta-analyses. BMJ 327, 557–560 (2003).
Hillier, S. G., Whitelaw, P. F. & Smyth, C. D. Follicular oestrogen synthesis: the 'two-cell, two-gonadotrophin' model revisited. Mol. Cell Endocrinol. 100, 51–54 (1994).
Smyth, C. D., Miro, F., Howles, C. M. & Hillier, S. G. Effect of luteinizing hormone on follicle-stimulating hormone-activated paracrine signaling in rat ovary. Hum. Reprod. 1, 33–39 (1995).
Thompson, E. A. Jr & Siiteri, P. K. Utilization of oxygen and reduced nicotinamide adenine dinucleotide phosphate by human placental microsomes during aromatization of androstenedione. J. Biol. Chem. 249, 5364–5372 (1974).
Morishima, A., Grumbach, M. M., Simpson, E. R., Fisher, C. & Qin, K. Aromatase deficiency in male and female siblings caused by a novel mutation and the physiological role of estrogens. J. Clin. Endocrinol. Metab. 80, 3689–3698 (1995).
Zhao, D., Pan, L., Zhang, F., Pan, F., Ma, J., Zhang, X. et al. Successful use of aromatase inhibitor letrozole in NOA with an elevated FSH level: a case report. Andrologia 46, 456–457 (2014).
Bighin, C., Lunardi, G., Del Mastro, L., Marroni, P., Taveggia, P., Levaggi, A. et al. Estrone sulphate, FSH, and testosterone levels in two male breast cancer patients treated with aromatase inhibitors. Oncologist 15, 1270–1272 (2010).
Wickman, S., Sipilä, I., Ankarberg-Lindgren, C., Norjavaara, E. & Dunkel, L. A specific aromatase inhibitor and potential increase in adult height in boys with delayed puberty: a randomised controlled trial. Lancet 357, 1743–1748 (2001).
Harada, N., Ogawa, H., Shozu, M., Yamada, K., Suhara, K., Nishida, E. et al. Biochemical and molecular genetic analyses on placental aromatase (P-450AROM) deficiency. J. Biol. Chem. 267, 4781–4785 (1992).
Ito, Y., Fisher, C. R., Conte, F. A., Grumbach, M. M. & Simpson, E. R. Molecular basis of aromatase deficiency in an adult female with sexual infantilism and polycystic ovaries. Proc. Natl Acad. Sci. USA 90, 11673–11677 (1993).
Morishima, A., Grumbach, M. M., Simpson, E. R., Fisher, C. & Qin, K. Aromatase deficiency in male and female siblings caused by a novel mutation and the physiological role of estrogens. J. Clin. Endocrinol. Metab. 80, 3689–3698 (1995).
Hauri-Hohl, A., Meyer-Böni, M., Lang-Muritano, M., Hauri-Hohl, M., Schoenle, E. J. & Biason-Lauber, A. Aromatase deficiency owing to a functional variant in the placenta promoter and a novel missense mutation in the CYP19A1 gene. Clin. Endocrinol. (Oxf) 75, 39–43 (2011).
Bouchoucha, N., Samara-Boustani, D., Pandey, A. V., Bony-Trifunovic, H., Hofer, G., Aigrain, Y. et al. Characterization of a novel CYP19A1 (aromatase) R192H mutation causing virilization of a 46,XX newborn, undervirilization of the 46,XY brother, but no virilization of the mother during pregnancies. Mol. Cell. Endocrinol. 390, 8–17 (2014).
Marino, R., Perez Garrido, N., Costanzo, M., Guercio, G., Juanes, M., Rocco, C. et al. Five new cases of 46,XX aromatase deficiency: clinical follow-up from birth to puberty, a novel mutation, and a founder effect. J. Clin. Endocrinol. Metab. 100, E301–E307 (2015).
Harada, N., Ogawa, H., Shozu, M. & Yamada, K. Genetic studies to characterize the origin of the mutation in placental aromatase deficiency. Am. J. Hum. Genet. 51, 666–672 (1992).
Herrmann, B. L., Saller, B., Janssen, O. E., Gocke, P., Bockisch, A., Sperling, H. et al. Impact of estrogen replacement therapy in a male with congenital aromatase deficiency caused by a novel mutation in the CYP19 gene. J. Clin. Endocrinol. Metab. 87, 5476–5484 (2002).
Conte, F. A., Grumbach, M. M., Ito, Y., Fisher, C. R. & Simpson, E. R. A syndrome of female pseudohermaphrodism, hypergonadotropic hypogonadism, and multicystic ovaries associated with missense mutations in the gene encoding aromatase (P450arom). J. Clin. Endocrinol. Metab. 78, 1287–1292 (1994).
Mullis, P. E., Yoshimura, N., Kuhlmann, B., Lippuner, K., Jaeger, P. & Harada, H. Aromatase deficiency in a female who is compound heterozygote for two new point mutations in the P450arom gene: impact of estrogens on hypergonadotropic hypogonadism, multicystic ovaries, and bone densitometry in childhood. J. Clin. Endocrinol. Metab. 82, 1739–1745 (1997).
Carani, C., Qin, K., Simoni, M., Faustini-Fustini, M., Serpente, S., Boyd, J. et al. Effect of testosterone and estradiol in a man with aromatase deficiency. N. Engl. J. Med. 337, 91–95 (1997).
Belgorosky, A., Pepe, C., Marino, R., Guercio, G., Saraco, N., Vaiani, E. et al. Hypothalamic-pituitary-ovarian axis during infancy, early and late prepuberty in an aromatase-deficient girl who is a compound heterocygote for two new point mutations of the CYP19 gene. J. Clin. Endocrinol. Metab. 88, 5127–5131 (2003).
Schlatt, S. & Ehmcke, J. Regulation of spermatogenesis: an evolutionary biologist's perspective. Semin. Cell Dev. Biol. 29, 2–16 (2014).
Acknowledgements
We thank all the volunteers who participated in this study. We are grateful to the late Professor Yutaka Nakahori for collecting blood samples from the participants. We also thank Professor Toyomasa Katagiri for his assistance with the AB GeneAmp PCR system 9700. This study was supported in part by the Ministry of Health and Welfare of Japan (1013201) (to TI), Grant-in-Aids for Scientific Research (C) (26462461) (to YS) and (23510242) (to ATa), Grant-in-Aids for Scientific Research (B) (15H04320) (to ATa) from the Japan Society for the Promotion of Science, the European Union (BMH4-CT96-0314) (to TI), the Takeda Science Foundation (to ATa) and a research program for the development of intelligent Tokushima artificial Exosome (iTEX) from Tokushima University.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on Journal of Human Genetics website
Supplementary information
Rights and permissions
About this article
Cite this article
Sato, Y., Tajima, A., Katsurayama, M. et al. A replication study of a candidate locus for follicle-stimulating hormone levels and association analysis for semen quality traits in Japanese men. J Hum Genet 61, 911–915 (2016). https://doi.org/10.1038/jhg.2016.82
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2016.82
This article is cited by
-
Association of TUSC1 and DPF3 gene polymorphisms with male infertility
Journal of Assisted Reproduction and Genetics (2018)