Abstract
Moyamoya disease (MMD) is a rare cerebrovascular disease characterized by progressive occlusion of the terminal portion of the internal carotid arteries and their branches. A genetic background was under speculation, because of the high incidence of familial occurrence. Sibling cases usually exhibit a similar clinical course. Recently, RNF213 was identified as the first MMD susceptibility gene. The c.14576G>A variant of RNF213 significantly increases the MMD risk, with an odds ratio of 190.8. Furthermore, there is a strong association between clinical phenotype and the dosage of this variant. The present study described sibling MMD cases having homozygous and heterozygous c.14576G>A variant in RNF213, as well as different clinical course and disease severity. The homozygote of c.14576G>A variant showed an early onset age and rapid disease progress, which resulted in significant neurological deficits with severe and wide distribution of vasculopathy. In contrast, the heterozygote of the variant showed a relatively late-onset age and mild clinical course without irreversible brain lesions with limited distribution of vasculopathy. This is the first report of sibling MMD cases with different doses of the RNF213 variant, showing its genetic impact on clinical phenotype even in members with similar genetic background.
Similar content being viewed by others
Main
Moyamoya disease (MMD) is a rare cerebrovascular disease characterized by progressive occlusion of terminal portions of the internal carotid arteries (ICAs) and their distal branches, which is later accompanied by compensatory recruitment of an abnormal vascular network termed the ‘moyamoya’ vessels.1 MMD is a relatively common cause of pediatric stroke,2, 3 which might lead to irreversible and devastating neurological deficits and intellectual impairments if left untreated. Genetic factors have been speculated, because of the high incidence of familial occurrence. Recently, the first MMD susceptibility gene, RNF213, was reported.4, 5 The c.14576G>A variant of RNF213 is a missense variant that switches arginine to lysine; the variant has been shown to significantly increase the risk of MMD with an odds ratio of 190.8.4 In addition, c.14576G>A homozygotes exhibit more severe and wider vasculopathy than heterozygotes.6 Here, we present sibling cases of MMD having homozygous and heterozygous c.14576G>A variant in RNF213, as well as different clinical course and disease severity.
The cases are Japanese siblings born to nonconsanguineous, healthy unaffected parents. They had a brother without MMD (Figure 1a). Case 1 (proband) is a 21-year-old male. His pregnancy and delivery were unremarkable and he exhibited normal psychomotor development. He had a first history of transient ischemic attack (TIA) associated with left-sided weakness at age 2, and was subsequently diagnosed with MMD. Bilateral encephalo-duro-arterio-synangiosis (EDAS)7 was performed 2 months after the initial TIA. However, left hemiparesis persisted after surgery. Brain computed tomography (CT) results revealed a low-density area in the territory of right middle cerebral artery (MCA), and the right cerebral hemisphere was atrophic. An older ischemic lesion was also present in the right occipital region. Cerebral angiograms demonstrated that right ICA, MCA and anterior cerebral artery (ACA) were steno-occlusive with a poor moyamoya vascular network. Left ICA, MCA and ACA were also stenotic, but an abundant moyamoya vascular network was observed. Bilateral frontal omental transplantation8 was performed at age 3. At 5 years of age, TIAs associated with visual disturbance frequently occurred, and bilateral occipital gracilis muscle transplantation9 was performed. Following surgery, the TIAs disappeared. Intellectual ability was slowly deteriorating. At age 9, his total intelligence quotient (IQ) was 68, verbal IQ was 73 and performance IQ was 68. At age 12, he suffered repetitive TIAs associated with right-sided weakness. A cerebral blood flow study with stable xenon-enhanced CT showed a diffuse decrease, especially in the left cerebral hemisphere (Figure 1b). A subcutaneous tissue graft, which included a parietal branch of the left superficial temporal artery and a relevant vein,10 was transplanted in the left parietal lobe, and TIAs subsequently decreased. At present, mild to moderate hemiparesis was observed on both sides. He can perform basic activities of daily living independently, including self-feeding using chopsticks. TIAs associated with bilateral weakness of lower extremities and dysarthria occur less than once a month. Frequent fore-headache remained. Brain magnetic resonance imaging (MRI) obtained at age 21 showed multiple infarctions with brain atrophy, with no gross interval changes since the previous surgery (Figure 1c), and cerebral angiograms demonstrated bilateral ICA and posterior cerebral artery (PCA) occlusion (Figure 1d).
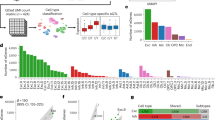
(a) Family pedigree showing the genotype of c.14576G>A variant. G/A: heterozygous c.14576G>A variant; A/A: homozygous c.14576G>A variant. (b) Stable xenon-enhanced CT of case 1 at age 12 shows decreased cerebral blood flow, especially in the left cerebral hemisphere. (c) Brain MRI (fluid-attenuated inversion recovery image (left and middle images) of case 1 at age 21, showing high-intensity lesions in bilateral occipital, right MCA territory including the watershed region, and the left semiovale. The right temporo-parietal lesion accompanies brain atrophy in the T1-weighted image (right image). (d) Cerebral angiograms of case 1 at age 21. Bilateral ICAs and PCAs are occluded. From right to left: R-CCA: A-P view; L-ICA: A-P view and lateral view; L-VA: A-P view. (e) Stable xenon-enhanced CT of case 2 at age 17 shows decreased cerebral vasoreactivity in the right frontotemporal area, comparing pre- and post-intravenous acetazolamide administration. CVR was 9.4% for the right and 23.3% for the left frontotemporal area, respectively. (f) Fluid-attenuated inversion recovery (left) and T1-weighted (right) images of brain MRI in case 2 at age 17 showing no abnormalities. (g) Cerebral angiograms of case 2 at age 17 reveal a stenotic right proximal portion of the MCA (M1), and retrograde filling from the right ACA to the MCA territory was observed. The left proximal portion of the ACA (A1) was also stenotic, and partial retrofilling from the left MCA to the left ACA territory via leptomeningeal anastomosis was observed. From right to left: R-ICA: A-P view and lateral view; L-ICA: A-P view and lateral view; R-VA: A-P view. (h) Electropherogram of the c.14576G>A variant (arrow) in RNF213. Case 1 expresses the homozygous c.14576G>A variant, and case 2 expresses the heterozygous variant. A, anterior; CCA, common carotid artery; L, left; P, posterior; R, right; VA, vertebral artery.
Case 2 was an 18-year-old female, who was the younger sister of the proband. Her pregnancy and delivery were unremarkable, and she exhibited normal psychomotor development. Her initial attack occurred as TIA associated with weakness and numbness of the left hand at age 17. On her admission to the neurosurgical clinic, no abnormal neurological findings were observed. Cerebral vasoreactivity to intravenous acetazolamide administration, evaluated by stable xenon-enhanced CT,11 was decreased in the right hemisphere (Figure 1e), although brain MRI showed normal findings (Figure 1f). Cerebral angiograms revealed that the right proximal portion of the MCA (M1) and left proximal portion of the ACA (A1) were stenotic (Figure 1g). Case 2 was diagnosed with MMD, and right superficial temporal artery–MCA anastomosis12 was performed 2 months after diagnosis. Then, the TIAs completely disappeared.
Both parents were examined by brain MRI/MR angiography (MRA) during their 20s or 30s, and the unaffected sibling, who was 20 years old at the time of the study, underwent a brain MRI/MRA at the age of 2. Results were normal for all of them.
Following written informed consent, genomic DNA from the affected siblings and unaffected family members was obtained from either peripheral blood leukocytes or saliva. The mutation analysis of RNF213 (GenBank accession number, NM_020914.4) was performed by high-resolution melting analysis and direct sequencing. The homozygous c.14576G>A variant in RNF213 was identified in case 1, and the heterozygous variant was identified in case 2 and all other unaffected family members (father, mother and unaffected sibling). No other mutation was identified in the entire RNF213 gene (Figure 1h).
Several reports on sibling MMD cases have revealed a tendency towards similar onset age and similar clinical courses.13, 14 These similarities could be due to similar genetic and environmental backgrounds that the siblings share. The present cases, however, were rather atypical. Case 1, a homozygote of c.14576G>A variant, exhibited an early-onset age and rapid disease progress, which resulted in significant neurological deficits. Cerebral angiograms revealed severe and wide distribution of vasculopathy. In contrast, case 2, the heterozygote of the variant, exhibited a relatively late-onset age and mild clinical course without irreversible brain lesions. Vasculopathy of case 2 appeared milder and exhibited more limited distribution than case 1 (Table 1). The differences in clinical phenotypes between the siblings could be explained by different genetic backgrounds: one had two copies of the c.14576G>A variant and the other had only one copy. Present cases give us another evidence that clinical phenotypes of MMD are associated with a dose effect of the heterozygous and homozygous c.14576G>A variants of RNF213. This variant might have a much larger impact on MMD phenotype than common variants of other common diseases.
Why there are both heterozygote of this variant with and without MMD is a difficult question, as it is unclear how much risk one would own with this variant. To solve this, we calculated the life-time incidence rate of MMD if one Japanese has the heterozygous c.14576G>A variant. It was reported that heterozygotes were identified in 153/204 (75%) of patients with MMD, and in 5/283 (1.8%) of normal Japanese controls.6 Annual incidence is estimated at 0.35–0.94 per 100 000 person-years in Japan.15, 16 Appling the Bayes' theorem with these data, the life-time incidence rate of MMD having heterozygous was calculated to be 1.44–3.77%. It is suggested that the incidence rate of MMD is relatively low if one had the heterozygous variant, whereas incidence rate for homozygotes are extremely high (>78%).6 This also reflects the effect of this variant with the dose effect.
In conclusion, a family with sibling MMD cases having different doses of the RNF213 variant is first described, clearly showing impact of the variant on clinical phenotype even in members with similar genetic background.
Accession codes
References
Suzuki, J. & Takaku, A. Cerebrovascular ‘moyamoya’ disease. Disease showing abnormal net-like vessels in base of brain. Arch. Neurol. 20, 288–299 (1969).
Bigi, S., Fischer, U., Wehrli, E., Mattle, H. P., Boltshauser, E., Burki, S. et al. Acute ischemic stroke in children versus young adults. Ann. Neurol 70, 245–254 (2011).
Mackay, M. T., Wiznitzer, M., Benedict, S. L., Lee, K. J., Deveber, G. A. & Ganesan, V. Arterial ischemic stroke risk factors: the International Pediatric Stroke Study. Ann. Neurol. 69, 130–140 (2011).
Kamada, F., Aoki, Y., Narisawa, A., Abe, Y., Komatsuzaki, S., Kikuchi, A. et al. A genome-wide association study identifies RNF213 as the first Moyamoya disease gene. J. Hum. Genet. 56, 34–40 (2011).
Liu, W., Morito, D., Takashima, S., Mineharu, Y., Kobayashi, H., Hitomi, T. et al. Identification of RNF213 as a susceptibility gene for moyamoya disease and its possible role in vascular development. PLoS ONE 6, e22542 (2011).
Miyatake, S., Miyake, N., Touho, H., Nishimura-Tadaki, A., Kondo, Y., Okada, I. et al. Homozygous c.14576G>A variant of RNF213 predicts early-onset and severe form of moyamoya disease. Neurology 78, 803–810 (2012).
Matsushima, Y., Fukai, N., Tanaka, K., Tsuruoka, S., Inaba, Y., Aoyagi, M. et al. A new surgical treatment of moyamoya disease in children: a preliminary report. Surg. Neurol. 15, 313–320 (1981).
Karasawa, J., Kikuchi, H., Kawamura, J. & Sakai, T. Intracranial transplantation of the omentum for cerebrovascular moyamoya disease: a two-year follow-up study. Surg. Neurol. 14, 444–449 (1980).
Touho, H., Karasawa, J. & Ohnishi, H. Cerebral revascularization using gracilis muscle transplantation for childhood moyamoya disease. Surg. Neurol. 43, 191–197 (1995).
Touho, H. Subcutaneous tissue graft including a scalp artery and a relevant vein for the treatment of cerebral ischemia in childhood moyamoya disease. Surg. Neurol. 68, 639–645 (2007).
Touho, H., Karasawa, J., Nakagawara, J., Tazawa, T., Yamada, K., Kuriyama, Y. et al. Mapping of local cerebral blood flow with stable xenon-enhanced CT and the curve-fitting method of analysis. Radiology 168, 207–212 (1988).
Karasawa, J., Kikuchi, H., Furuse, S., Kawamura, J. & Sakaki, T. Treatment of moyamoya disease with STA-MCA anastomosis. J. Neurosurg. 49, 679–688 (1978).
Hamada, J. I., Yoshioka, S., Nakahara, T., Marubayashi, T. & Ushio, Y. Clinical features of moyamoya disease in sibling relations under 15 years of age. Acta. Neurochir. 140, 455–458 (1998).
Yamauchi, T., Houkin, K., Tada, M. & Abe, H. Familial occurrence of moyamoya disease. Clin. Neurol. Neurosurg. 99, S162–S167 (1997).
Wakai, K., Tamakoshi, A., Ikezaki, K., Fukui, M., Kawamura, T., Aoki, R. et al. Epidemiological features of moyamoya disease in Japan: findings from a nationwide survey. Clin. Neurol. Neurosurg. 99, S1–S5 (1997).
Baba, T., Houkin, K. & Kuroda, S. Novel epidemiological features of moyamoya disease. J. Neurol. Neurosurg. Psychiatry 79, 900–904 (2008).
Acknowledgements
We thank all the participants for their cooperation in this study. We also thank Ms Y Yamashita, Dr K Nishiyama, Ms K Takabe, Mr T Miyama and Ms E Koike from the Department of Human Genetics, Yokohama City University, Graduate School of Medicine, for their technical assistance. This study was supported by a grant from the Ministry of Health, Labor and Welfare, the Japan Science and Technology Agency (NM, HS and NMiyake), a Grant-in-Aid for Scientific Research on Innovative Areas (Foundation of Synapse and Neurocircuit Pathology) from the Ministry of Education, Culture, Sports, Science, and Technology of Japan (NM), a Grant-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (NM), a grant from the Takeda Science Foundation(NM), and a Grant-in-Aid for Young Scientists from the Japan Society for the Promotion of Science (HS and NMiyake), a Grant-in-Aid for Japan Foundation for Neuroscience and Mental Health (SM).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Miyatake, S., Touho, H., Miyake, N. et al. Sibling cases of moyamoya disease having homozygous and heterozygous c.14576G>A variant in RNF213 showed varying clinical course and severity. J Hum Genet 57, 804–806 (2012). https://doi.org/10.1038/jhg.2012.105
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhg.2012.105
Keywords
This article is cited by
-
Risk Factors for Preoperative Cerebral Infarction in Infants with Moyamoya Disease
Translational Stroke Research (2023)
-
The Genetic Basis of Moyamoya Disease
Translational Stroke Research (2022)
-
Rare RNF213 variants and the risk of intracranial artery stenosis/occlusion disease in Chinese population: a case-control study
BMC Medical Genetics (2019)
-
Individual risk alleles of susceptibility to schizophrenia are associated with poor clinical and social outcomes
Journal of Human Genetics (2016)
-
A new horizon of moyamoya disease and associated health risks explored through RNF213
Environmental Health and Preventive Medicine (2016)