Abstract
There is a continuous need for iterative cycles of antibiotic discovery and development to deal with the selection of resistant pathogens that emerge as therapeutic application of an antibiotic becomes widespread. A short golden age of antibiotic discovery from nature followed by a subsequent golden half century of medicinal chemistry optimization of existing molecular scaffolds emphasizes the need for new antibiotic molecular frameworks. We bring a molecule-centered perspective to the questions of where will new scaffolds come from, when will chemogenetic approaches yield useful new antibiotics and what existing bacterial targets merit contemporary re-examination.
Similar content being viewed by others
A personal pathway to antibiotics research
For one of us (CTW), a career-long interest in antibiotics1 was spurred by discussions on the mechanism of action of D-fluoroalanine2, 3 during a seminar visit, as a second year assistant professor, at Merck in 1974. This visit led to examination of the mechanism of action of mono-, di- and trifluoroalanines as mechanism-based inactivators for the bacterial pyridoxal phosphate-dependent alanine racemase, the first step in assembly of the muramyl pentapeptide of the bacterial peptidoglycan layer.4, 5, 6, 7 In turn, that led to analysis of other muramyl peptide biosynthetic enzymes, including MurA8, 9, 10, 11 (the target of fosfomycin) and MurB,12, 13, 14, 15, 16, 17, 18 which together build the lactyl ether moiety of UDP muramic acid. We progressed on to the enzyme MurF,19 the D-Ala-D-Ala ligase that adds this D-D-dipeptide to UDP-muramyl tripeptide, to yield UDP-muramyl pentatopeptide as the last step in the cytoplasmic phase of peptidoglycan assembly.20, 21
A second phase of interest was initiated when CTW was the CEO of the Dana Farber Cancer Institute in the early 1990s at a time when vancomycin was being used as the antibiotic of last resort for treatment of life-threatening Gram-positive bacterial infections of patients undergoing cycles of chemotherapy. The molecular mechanism of resistance of pathogenic vancomycin-resistant enterococci (VRE) turned out to be replacement of the D-Ala-D-Ala termini of muramyl pentapeptide intermediates with D-Ala-D-Lactate, which had 1000-fold lower affinity to vancomycin.22 We established the the VanA enzyme in VRE was not the classic D-Ala-D-Ala ligase but a D-Ala-D-Lac ligase22, 23, 24, 25, 26 and thus determined the molecular basis of drug resistance in VRE.27, 28, 29
The rise of VRE through the 1990s focused our attention on how natural product antibiotic scaffolds such as those of vancomycin and the related teicoplanin were assembled,29, 30 in part to decipher the chemical logic and molecular machinery and, in part, with the hope that one might learn to reprogram natural antibiotic assembly lines to engineer improved molecular variants.
We have subsequently deciphered many of the rules for nonribosomal peptide (NRP) synthetase assembly lines, including post-translational priming of carrier protein domains by phosphopantetheinylation, and the nature of the chain initiation, elongation and termination steps.30, 31, 32, 33, 34, 35 These efforts have allowed us and many other groups to undertake full reconstitution of NRP synthetase assembly lines, especially in siderophore biosynthesis.36 From our extensive work on characterization of natural product biosynthesis catalytic machinery and molecular logic, we have had a continued interest in new natural products and the underlying chemistry of molecular scaffold assembly.37
Antibiotics as a special class of therapeutics
One could argue that antibiotics represent a special class of therapeutic agents whose misuse affects not just the individual patient but the broader community. This is due to the almost inevitable selection for antibiotic-resistant bacteria that arise in clinically significant waves at some point after widespread introduction and use of a new antibiotic (both in veterinary and human populations). As Table 1 (modified from a review by Palumbi)38 shows, resistance is inevitable.39, 40, 41, 42, 43, 44, 45 It is not a question of if but rather a question of when. Much effort in recent years has gone into definition of the resistome,46, 47 the collection of antibiotic-resistant genomes harbored in both bacterial pathogens and in environmental bacterial populations. The origins of vancomycin resistance, for example, derive from transfer of vanHAX genes from intrinsically resistant soil microbes such as lactobacilli and leuconostoc strains to enterococci where they often reside on transposable elements.46, 48, 49 The depth of the resistome resevoir was powerfully demonstrated in the findings of D’Costa et al.50 in 2006 showing that collections of soil actinomycetes had, on average, resistance genes to 7 antibiotics while some isolates were resistant to 15 drugs.
Because of the mobilization of resistome genes into opportunistic and professional bacterial pathogens, there is always a need for the next generation of antibiotics. There are parallels to antiviral and anticancer therapeutics where the rapid proliferation and the large number of viruses and tumor cells in a patient can mirror the rapid growth and titer of bacterial pathogens. Mutations rates of 10−6 per cell divison are problematic in all the three therapeutic arenas. We shall return later to a distinction in therapeutic regimens: in antiviral and anticancer drug regimens, combination therapy is the norm while for bacterial infections monotherapy has been the default historical prescribing pattern.
Gram-positive and Gram-negative pathogens present overlapping but distinct target profiles. While Gram-positive pathogens such as VRE and methicillin-resistant Staphylococcus aureus (MRSA) have rightly drawn attention over the past two decades, the Gram-negatives, underlined, in the list of ESKAPE pathogens (Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumanii, Pseudomonas aeruginosa and Enterobacter species), are in many cases more of a pressing treatment challenge.51 The approvals of synercid and daptomycin were largely in response to VRE and MRSA challenges52, 53 but there has not been a new antibiotic scaffold for Gram-negative pathogens in decades. As a consequence polymyxins (for example, colistin) have become front-line therapy in recent years,54, 55 even though they were eschewed as too toxic when discovered 40 years ago. Multidrug-resistant tuberculosis pose their own crises for therapy around the world but, finally, promising new molecules (for example, benzothiazinone BTZ04356, 57, 58, 59, 60, 61 in late preclinical GLP/Tox funded by the European Commission, sponsored by New Medicines for Tuberculosis, and in development by Alere in Germany; nitroimidazole PA-82462, 63 in Phase II sponsored by the TB Alliance; ethylenediamine SQ10964 in Phase II sponsored by Sequella Inc and OOO Infectex; and Sutezolid65 (also known as PNU-100480) a thiooxazolidinone in Phase II under Pfizer) are progressing through late stage clinical trials or have recently been approved by the Food and Drug Administration (FDA; bedaquiline,45 a diarylquinoline inhibitor of ATP-synthase developed by J&J).66, 67
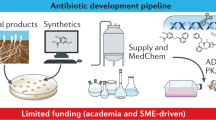
This essay is not encyclopedic and doubtless has important omissions about promising molecules in both discovery and development phases. Rather, the choices reflect the particular perspective of the authors about emerging science that seems intriguing and worthy of follow up. In consideration of the underexploited targets noted below, there is a chemocentric set of prejudices: that the availability of promising chemical matter, from Nature or from initial screening campaigns is an important precondition for finding hits, developing them into leads and conducting lead optimization for compounds to be selected as development candidates. Figure 1 is a variant of a typical drug discovery/development flow chart adapted for antibiotics;68 the low success rate emphasizes the importance of starting with molecular frameworks that can stand up to the rigors of development. The focus of the remarks in this chapter are all on discovery, not development.
Antibiotic drug discovery and development flow chart adapted from literature versions.68
A pressing need for new antibiotic scaffolds
Over the past century of antibiotic discovery and development, two parallel and independent lines of discovery have been fruitful. One route has been the identification of antimicrobial chemical weaponry in Nature as small-molecule natural products were observed to have clinically useful antibacterial activity. Among these scaffolds were the penicillins and cephalosporins, the macrolides such as erythromycin, the glycopeptides exemplified by vancomycin and teicoplanin, the tetracylines and the aminoglycosides. A separate track is represented by the discovery that aromatic sulfa scaffolds originally from the chemical dyes industry frameworks had antibiotic activity.69 The resultant sulfa drugs have been in continuous use in one incarnation or another for 80 years. The second example of man-made ‘magic bullets’ as widely used antibiotics were the fluoroquinolones, first introduced clinically in the 1960s. A third distinct synthetically derived scaffold is represented by the first-generation oxazolidinone linezolid approved in the US in 2000.
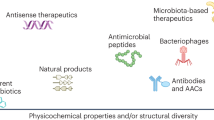
The ‘golden age’ of discovery of natural antibiotics of clinical significance was actually a short two decades (Figure 2), between 1940 and 1960. One could argue that the ensuing 50 years has been a ‘golden age’ of antibiotic medicinal chemistry where chemical tailoring of the periphery of major antibiotic classes, while leaving the core intact, has been successful in dealing with successive waves of resistant bacterial pathogens. As illustrated in Figure 3, successive generations of cephalosporins, fluoroquinolones, macrolides and tetracyclines have been developed and commercialized with significant usage. In the tetracycline arena, new synthetic methodologies have enabled synthesis of pentacyclines,70 which may become a fourth generation of this antibiotic class. Analogously, while the informal designation of generations of an antibiotic class are somewhat in the eye of the beholder, one could argue that molecules such as prulifloxacin71 represent a fifth generation of fluoroquinolones. It is unlikely that medicinal chemistry modifications of these four antibiotic classes can go indefinitely. That prediction argues for a pressing need for new antibiotic scaffolds, either from natural products or from the many strands of modern synthetic chemistries. In the short term, it is understandable that antibiotic development groups and companies choose to reduce risk by working on known scaffolds and known targets, but in the longer term, new molecules and new targets will need to be identified72 as bacterial pathogens become multidrug resistant as exemplified by some of the ESKAPE pathogens.51
Synthetic tailoring of antibiotic core structures leading to successive generations of antibiotic classes has been the mainstay of antibiotic drug development for the past 50 years. New antibiotic core scaffolds are desperately needed. Core scaffolds are shown in black and peripheral chemical derivatizations are shown in white. The quinolone/fluoroquinolone scaffolds are of synthetic origin, while all other scaffolds are natural products or their semisynthetic derivatives.
A 2011 survey of 21 antibiotics launched since 200073 revealed that the two lines of discovery and development, natural products vs synthetic chemicals, are still operant with two new natural product classes, represented by daptomycin as a stem loop lipopeptide and retapamulin as a member of the terpenoid pleuromutilins. Of the nine antibiotics of synthetic origin launched in the past 12 years, other than the oxazolidinone linezolid, the other eight are fluoroquinolones, stressing the need for scaffold diversification away from such over-reliance on the F-quinolone framework. In that same 2011 survey of five antibiotic candidates in phase III trials, the one synthetic molecule was a second-generation oxazolidinone torezolid phosphate.74, 75, 76 Another second-generation oxazolidinone, radezolid, is progressing through late stage trials.77, 78, 79, 80
Where will new scaffolds come from
The two historical lines of discovery, synthetic chemical efforts vs isolation of new natural product scaffolds are both still in play. Two contemporary lines of chemical efforts are high throughput screening of chemical libraries and target structure-guided efforts.
A comprehensive screening effort against genetically validated essential targets, on the part of many companies, most notably detailed by a GSK group in 2007,81 effectively failed to find new chemical matter worthy of development. This has properly dampened enthusiasm for continued screening campaigns. On the other hand, the development of focused libraries, more suited for specific target classes, could hold more promise. A Pfizer group repurposed a library built for eukaryotic kinase projects and identified hits and optimized leads against the bacterial form of the ATP-dependent biotin carboxylase, which generates malonyl CoA from acetyl CoA at the start of fatty acid biosynthesis.82
Chemical libraries that mimic the scaffold complexity of natural products in three dimensional architectures, regiochemical constraints, multiple stereogenic centers and high density of functional groups have not been available over the first two decades of combichem efforts. Such libraries, even relatively small and focused around particular scaffolds, may be requisite for screening efforts to increase in success rates against bacterial targets.83, 84, 85, 86
A recent report of a structure-guided antibiotic discovery effort comes from an Astra Zeneca team on thymidylate kinase inhibition. Reasoning that this kinase lies at the intersection of both salvage and de novo formation of dTMP, essential for DNA synthesis, Keating et al.87, 88 designed scaffolds to bind to the dTMP subsite rather than the ATP subsite, using the X-ray structure of the enzyme as guide. TK-666 (Figure 4a) represents a thymine-sugar mimic with fragment coupling to two additional rings. The molecule is rapidly bacteriocidal against Gram-positives such as S. aureus, with MIC of 0.25 μg ml−1 and a Ki against pure S. aureus dTMP kinase of 0.33 nM. Inhibition of thymidylate kinase from a variety of pathogenic microbes is being pursued by several groups using modified thymidine scaffolds and mimetics.89, 90, 91, 92, 93
(a) Structure of TK-666, a potent synthetic inhibitor of bacterial thymidylate kinase developed by researchers at AstraZeneca. (b) Structure of platensimycin, a potent inhibitor of bacterial β-ketoacyl-ACP synthase type I/II (FabF/B) isolated from Streptomyces platensis by a group at Merck. (c) Structure of kibdelomycin, an inhibitor of DNA gyrase subunit A isolated from Kibdelosporangium sp. MA7385 by a group at Merck. (d) Structure of abyssomycin C, an isoprenoid inhibitor of p-aminobenzoate biosynthesis in the folate biosynthetic pathway. (e) Structure of tetarimycin A, an anti-MRSA tetracyclic molecule discovered through heterologous expression of a gene cluster found in environmental DNA.
The parallel search for new scaffolds in Nature bears fruit when new assays are developed, new cultivation methods established94, 95, 96 and new niches explored.97, 98 As will be noted in a subsequent section, the platensin and platensimycin scaffolds (Figure 4b) were discovered99, 100 in antisense screens that made FabF the rate-limiting step in S. aureus lipid biosynthesis and made bacterial growth sensitive to inhibition of this step. The initial enthusiasm over these potent Fab enzyme inhibitors has been partially muted by the observation that some bacteria can scavenge host lipids during infection.101 With a collection of 245 S. aureus strains similarly manipulated to lower the bacterial cell levels of encoded enzymes, a Merck group102 reported the isolation of kibdelomycin (Figure 4c) as a DNA gyrase subunit A inhibitor, the first new natural product scaffold against gyrase in the past several decades. This antisense approach is discussed further in a subsequent section.
Exploration of new niches has traditionally yielded new molecular frameworks. In this vein, isolation of microbes from the abyss in the Sea of Japan led to the novel isoprenoid abyssomycins, which inhibit para-aminobenzoate biosynthesis in the folate biosynthetic pathway103 (Figure 4d). The genome sequences of several thousand bacteria reveal up to two dozen silent clusters for natural product biosynthesis, typically polyketide (PK), NRP and hybrid PK-NRP frameworks.104, 105, 106, 107, 108, 109, 110 Fungi similarly harbor multiple biosynthetic gene clusters that are cryptic under normal laboratory culture conditons.111 A variety of approaches have been used to turn on silent biosynthetic gene clusters to evaluate the novelty and activity of the resultant small molecules.111, 112, 113
Progress also continues in examination of the genomes of uncultivated microbes through induced expression of environmental DNA gene clusters.96, 98, 114 One recent example is the isolation of tetarimycin A (Figure 4e), a tetracyclic molecule active against MRSA. This was accomplished by insertion of e-DNA containing the PK gene cluster along with a regulatory protein promoter, into the generic host Streptomyces albus under the control of a constitutive erythromycin-resistance promoter.115
Challenges of a target-poor therapeutic arena
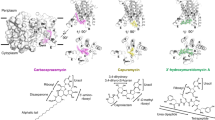
Historically, the treatment of human bacterial infections by antibiotics has been a target-poor therapeutic arena. Despite thousands of molecules shown to have antibiotic properties, there are essentially five major clinically validated antibacterial targets/pathways.1 As schematized in Figure 5, these include bacterial peptidoglycan/cell wall biosynthesis, targeted by both the β-lactams and the vancomcyin-type glycopeptides. A second set of targets is encompassed by bacterial protein synthesis, with most antibiotics targeting the ribosome. Daniel Wilson has provided an elegant, structurally oriented compendium of the A–Z of molecules targeting the small and large ribosomal subunits and the interface between them.116 A third target area is the blockade of DNA replication and transcription to RNA, most notably the targeting of DNA gyrase and RNA polymerase. The fourth is the folate biosynthetic pathway, which provides the one carbon unit required for the deoxythymidylate building block for DNA synthesis. The sulfa drugs and the folate analogs, used in combination, block two sequential steps in that biosynthetic pathway.117 The fifth and perhaps the most recent target of widespread clinical utility has been daptomycin disruption of bacterial membrane integrity.118, 119
The five major clinically validated antibacterial targets/pathways. (a) Inhibition of cell wall biosynthesis. (b) Inhibition of protein synthesis. (c) Inhibition of DNA or RNA synthesis. (d) Inhibition of folate biosynthesis. (e) Disruption of membrane integrity. Modified from the cover of Walsh.1
When will chemogenetic approaches pay off?
Over the decades since the 1960s, the antibiotics research community has sought to broaden the number of clinically validated targets, using many rational as well as screening approaches. A particularly concerted effort went on with the advent of genome sequences of the most common bacterial pathogens and the determination of essential genes. Their protein products were intensively examined in a first wave of screens in the chemogenetics era. The hallmark paper from the GSK group in 200781 noted above, summarizing more than 100 screens, starkly described the failure of that first wave. Among the resultant questions were the utility of in vitro screening of a target vs whole-cell assays and also the utility of chemical library collections in pharmaceutical companies for screening prokaryotic rather than the eukaryotic targets, for which many of those libraries were biased.
Smart screens: leads for combination therapies?
Among the smart screens to be employed in recent years are a series of publications102, 120, 121, 122, 123 from the Merck groups on a 245 siRNA collection to lower the levels of essential gene expressions in MRSA, one at a time. These siRNAs may thereby render that particular step in a pathway sufficiently rate determining to give a growth impairment signal when inhibited by a small molecule. Screening of such strains with these and related gene knock-down collections in other pathogens has turned up new scaffolds from both natural and synthetic sources. This approach led to discovery of the platensin and platensimycin (Figure 4b) novel terpenoid architectural frameworks that target fatty acid biosynthesis,96, 99 although their clinical utility has been questioned.101 This approach also turned up kibdelomycin (Figure 4c) as the first new natural product scaffold for gyrase inhibition in 60 years.102 The coumarin antibiotics (which are not used in human bacterial infections) target the ATPase domain in the GyrB subunit of DNA gyrase.1 Although structurally related to the coumarin antibiotics, kibdelomycin shows no cross resistance indicating that it targets a distinct subsite of DNA gyrase, possibly within the GyrA subunit or the catalytic active site of GyrB.102 The kibdelomycin scaffold is forbiddingly complex for structure-activity relationship (SAR) work, but there is the eribulin anticancer drug precedent86, 124 to show that a complex (32 step) synthesis can be commercially viable.
The Merck 245 siRNA collection targeting MRSA screens may also be useful in finding rational choices for new combination therapies.122, 123 Interactome analysis in such collections challenged with different subsets of β-lactam antibiotics turned up molecules that resensitize MRSA to carbapenems. A 256-fold gain in sensitivity to imipenem was seen in the presence of a small-molecule inhibitor of glucosamine synthase.121 For example, L-norvaline-N3-(4-methoxyfumaroyl)-L-2,3-diaminopropanoic acid (Nva-FMDP) is a mimetic of the natural product dapdiamide, which captures the active site Cys thiolate of the glutaminase domain of glucosamine synthase.125, 126 Deprivation of glucosamine units required for peptidoglycan assembly generates a defective cell wall that shows synergistic suceptibility to imipenem. A distinct but parallel approach to resensitize MRSA to β-lactam antibiotics is conferred by tunicamycin, which blocks wall teichoic acid biosynthesis.127 A third example involved a screen for inhibitors of lipid II flippase, with a synthetic library.122 Again, a molecule was detected that was read out as a regain of sensitivity to carbapenems.
Inter alia, these results, with both natural product and synthetic chemical libraries, bring into high relief the whole issue of default monotherapy for treatment of bacterial infections vs combinations of antibiotics. These sensitization-screening approaches may offer good algorithms for choice of the combinations and might be extended; for example, to molecules that could combine with colistin for treating MDR Gram-negative pathogens. Although consecutive deployment of antibiotics one at a time to treat persistent bacterial infections has been a long held approach, there are multiple examples reflecting combination therapy with antibiotics that may presage a future where combinations are applied simultaneously, with real-time knowledge of the pathogen genotypes as a guide. Those combinations include β-lactams and β-lactamase inhibitors such as augmentin (amoxicillin and clavulanate), sulfa drugs plus trimethoprim to block two consecutive steps in folate biosynthesis and the standard drug cocktails used in front-line tuberculosis therapy which include rifampin, isoniazid, pyrazinamide and ethambutol.1
Second-generation combinations of β-lactam and β-lactamase inhibitor are progressing through clinical trials. The lactamase inhibitors are not clavulanate or the penicillin sulfones used in the first- and second-generation combinations but rather bicyclic diazabycyclooctanes (Figure 6) in which the warhead is not the traditional four membered β-lactam but instead a five member γ-lactam bearing an O-sulfate substituent on the nitrogen128 in the clinical candidates avibactam and MK-7655. Studies on avibactam with purified lactamase show that γ-lactam is opened by the active site Ser-OH to yield a variant of the typical O-acyl-lactamase covalent intermediate.129 Over time, the lactam ring can reform and induce deacylation and regain lactamase activity, but the residence time suffices for either ceftaroline or ceftazidime, cephalosporins administered in combination with avibactam to reach their penicillin-binding proteins and function as killing antibiotics. Merck’s MK-7655 is being clinically evaluated in combination with the carbapenem imipenem.128
Should some underexplored targets be revisited?
Peptidoglycan biosynthesis
In peptidoglycan assembly, the nascent disaccharyl pentapeptide units are incorporated into existing cell wall by two kinds of enzymes, the PG transpeptidases (TPases), long the targets of clinically useful β-lactam and glycopeptides antibiotics, and the PG transglycosylases (TGases; Figure 7a). The transpeptidases are robust targets, in part, because their active sites are accessible from the periplasmic face in Gram-negative membranes and from the outside environment in Gram-positives. Bifunctional versions of the TPases and TGases are common killing targets in many bacteria, where inhibition of the TPase leaves mechanically weakened cell wall layers.1
(a) Inhibition of PG transglycosylases (TGases) by moenomycin and inhibition of PG transpeptidases (TPases) by β-lactams. (b) X-ray crystal structure of a moenomycin analog containing a 10-carbon neryl chain bound to the TGase domain of PBP1A from Aquifex aeolicus.134 The α-amino-β-hydroxy-cyclopentenol ring of the moenomycin analog was highly distorted and is therefore omitted from the structure. Image was generated from PDB entry 3D3H134 using PyMOL (The PyMOL Molecular Graphics System, Version 1.4, Schrödinger, LLC).
Although β-lactam antibiotics have been in use for 70 years, by contrast, no TGase inhibitors, which would have the same outcome in accumulation of uncrosslinked peptidoglycan units, are in human clinical use. Nature has turned up one TGase-targeting scaffold in the glycolipid moenomycins, metabolites from streptomycetes. Moenomycins are structurally complex natural products with five sugars and an isoprenoid C25 lipid tail connected by a glycerol phosphate linker.130 They are used in veterinary medicine but have poor pharmacokinetic properties, which curtail their use in humans.130 Nonetheless, recent advances of note are the determination of the X-ray structure of the PG transglycosylase, now from three different research groups131, 132, 133, 134, 135, 136 working with three distinct organisms (E. coli, S. aureus, A. aeolius), some with moenomycin bound131, 134, 135, 136 (Figure 7b). This structural information along with advances in chemical synthesis,137 biosynthesis138 and assay development139 should enable structure-driven optimization/simplification of the moenomycin scaffold (by synthesis and/or by pathway engineering) to get to a minimal structural core with potential amelioration of physical and pharmacodynamic properties that would move a moenomycin framework from veterinary to human indications.
Lipid II
Lipid II, at a few thousand molecules per bacterial cell, is the C55 isoprenoid carrier that receives the muramyl pentapeptide at the end of the cytoplasmic phase of peptidoglycan biosynthesis. While still on the inner face of the cytoplasmic membrane, the muramyl-pentapeptidyl-lipid II is a substrate for glycosylation by MurG. Then the disaccharyl-pentapeptidyl-lipid II is translocated by membrane flippases140 to the outer face of the cytoplasmic membrane. On the outward membrane face, it can be a substrate for the TPases and TGases that add these peptidoglycan-building blocks to existing PG strands. When the disaccharyl-pentapeptidyl-lipid II (Figure 8) is exposed at the outer surface of the membrane, the lipid II moiety is targeted at different subregions of its scaffold by two kinds of antibiotics.141 The vancomycin family glycopeptide antibiotics interact with the D-Ala-D-Ala terminus29, 142 while the antibiotics, such as the food preservative nisin, instead bind to the pyrophosphate subregion143 of Lipid II. A third class of natural molecules, the defensin family of peptides/small proteins, also bind to lipid II; the interaction of plectasin with lipid II has been characterized by NMR,144 and this structure may serve as starting point for peptidomimetics that may span multiple subregions of lipid II. These antimicrobial peptides by themselves have presented challenges for development,145 but we shall return to the peptidomimetic approach in a subsequent section on LptD in the lipopolysaccharide (LPS) export pathway.
One recent advance of note is the work of Boger’s group to generate the aglycone form of an amidine derivative of vancomycin146, 147 (Figure 9). The synthetic design took inspiration from the fact that VRE lower the affinity of vancmycin family glycopeptides for the uncrosslinked PG termini by substitution of D-Ala-D-Ala for D-Ala-D-lactate.22 The loss of one H-bond and the electronic repulsion of the D-Ala-D-Lac lone pair on the oxygen of the ester can be compensated in the amidine derivative. Not only did the amidine regain activity against VRE but also maintained acceptable activity against the wild-type D-Ala-D-Ala PG terminus. Addition of the glucosyl-1,2-vancosamine disaccharide moiety to the amidine aglycone, by chemical or enzymatic means, might result in a useful third-generation glycopeptide antibiotic (where the recently approved telavancin148 would be considered a second-generation molecule).
Diagram of the vancomycin-D-Ala-D-Lactate (a) and Boger’s synthetic amidine vancomycin aglycone-D-Ala-D-Lactate (b) hydrogen bonding networks. Boger’s amidine vancomycin aglycone increases the binding affinity for the uncrosslinked D-Ala-D-Lactate moiety found in modified lipid II of the peptidoglycan (normal lipid II contains a terminal D-Ala-D-Ala) by restoring a key hydrogen bond and compensating for electrostatic repulsion created by this increasingly common resistance conferring lipid II structural modification.
More natural lipopeptides and variants
With the success of the lipodepsipeptide daptomycin (Figure 10a) in treatment of bacterial infections in humans over the past decade,118, 119 there has been renewed interest in natural and semisynthetic versions of other lipopeptides as antibiotics. We take up acyldepsipeptides (ADEPS) below in the context of ATP-utilizing bacterial enzymes but note here the inhibition of signal peptidases (SPs) by arylomycins,149, 150 actinocarbasins,151 krisynomycin,151 the polyketide macrolactone antibiotic TA152 (also known as myxovirescin) and globomycin153, 154 (Figures 10b and c). Each of these natural products has a constrained conformation due to macrocyclization that is imposed during biosynthesis. The arylomycins and actinocarbasins have a dihydroxybiphenyl moiety that arises from coupling of two tyrosine side chains in the precursor peptide, presumably through a radical coupling mediated by an iron-enzyme that can make high valent oxo-iron intermediates.155 This C-C coupling is reminiscent of the coupling of residues 5 and 7 in vancomycin. The natural fatty acyl chain in the N-terminal tail of the actinocarbasins can be replaced semisynthetically with typical med chem biphenyl chains.151, 156 Gram-negative bacteria have two signal peptidases.157 Type I signal peptidase (SPI) is a serine protease with a catalytic mechanism distinct from eukaryotic serine proteases for trimming the signal sequence from secreted proteins, outer membrane proteins and periplasmic proteins. Type II signal peptidase (SPII) are completely absent in eukaryotes, making this an ideal antibiotic target, and function as an aspartyl protease that trims the precursor forms of lipoproteins found in the outer membranes of Gram-negative bacteria. While arylomycins target SPI, antibiotic TA and globomycin target SPII and are bacteriocidal at low concentrations.152 One feature of potential interest is that arylomycins synergize with aminoglycosides150 while actinocarbasins and krisynomycin do so with β-lactams.151 These natural products may therefore serve as starting points for further semisynthetic modifications of the frameworks through synthesis156, 158, 159, 160, 161 and pathway engineering,155, 162, 163, 164, 165, 166 with an eye towards combination therapy.
(a) Structure of daptomycin, a lipodepsipeptide antibiotic produced by Streptomyces roseosporus, discovered by Eli Lilly and Co. in the late 1980s, acquired and developed by Cubist Pharmaceuticals in 1997 and FDA approved in 2003. (b) Structures of the arylomycin, actinocarbasin and krisynomycin macrocyclic antibiotics that target type I bacterial signal peptidases. (c) Structures of antibiotic TA (also known as myxovirescin) and globomycin macrolactone antibiotics that target type II bacterial signal peptidases.
LPS: is the time ripe for a renewed assault on those enzymes?
One of the holy grails of antibiotic discovery efforts in Gram-negative pathogens has been the search for a broadly active inhibitor of lps biosynthesis and/or export. For decades, investigators have focused on the rate-determining step in lps biogenesis, the second committed step catalyzed by the zinc-dependent deacetylase LpxC (Figure 11a).167 The central metabolite UDP-GlcNAc undergoes long chain acylation at the 3′-OH of the GlcNAc by LpxA and then LpxC mediates deacetylation of the acetyl moiety on the 2′-amino group. A series of acylations, glycosylations and phosphoryl transfers then ensue on the way to the lipid A core of lps.168 A prototype alkynyl hydroxamate CHIR-090 has been characterized for mechanism and structure with LpxC,169 but narrow spectrum and pathogen mutation to resistance have been problematic for its development. Recent structure–function analysis has led to a diacetylenic congener LPC-009,170 which overcome the loss of affinity in point mutations that negate CHIR-090 binding (Figure 11b). Perhaps there is finally momentum towards a clinical candidate, at which point toxicology and pharmacology in human hosts will become crucial gating parameters.
(a) LpxC inhibitors block the first committed step of lipid A biosynthesis, a pathway specific to Gram-negative bacteria. (b) Structure-guided efforts inspired by the prototype alkynyl hydroxamate LpxC inhibitor CHIR-090 revealed the next generation diacetylenic inhibitor LPC-009, which overcomes point mutations (G214 to S214 in Rhzobium leguminosarum) associated with CHIR-090 resistance in Gram-negative pathogens. Images were created using PyMOL from PDB entries 2JT2169 (LpxC-CHIR-090 complex) and 3P3C170 (LpxC-LPC-009 complex). For both the cases, the structure was solved for WT LpxC from Aquifex aeolicus complexed to the inhibitor and a point mutation of G198 to S198 was inserted computationally into the PyMOL structure to demonstrate in this figure how this mutation leads to steric repulsion in the LpxC-CHIR-090 complex.
There has also been dramatic progress in recent years in delineation of the roles and structures of the periplasmic and outer membrane proteins LptA-E that function as chaperones for lps molecules to get across the periplasmic space.171, 172, 173, 174, 175, 176, 177, 178, 179, 180, 181, 182 The Lpt protein machinery also effects insertion of the translocated lps molecules and localization in the outer leaflet of the outer membrane in most Gram-negatives. In that context, the outer membrane β-barrel protein LptD has been known to be inhibited by an 18 residue antimicrobial peptide (AMP) protegrin I from porcine leukocytes.183 John Robinson and coworkers used this as a starting point for building a peptidomimetic scaffold (Figure 12).183, 184, 185 The natural bridging disulfide was removed, the rest of protegrin β-sheet was used as template and the framework cyclized with a diproline insert to give a potent inhibitor of lps trafficking in pseudomonas.183 Challenges remain to optimize broad spectrum Gram-negative activity. If the peptide framework is not sufficiently stable to protease breakdown, there is the traditionally difficult challenge to go from a peptide-based to a nonpeptidic scaffold to improve in vivo lifetimes while preserving activity. Although LptD is in the outer membrane and perhaps thereby particularly accessible to external agents, the other components of the Lpt assembly pathway also seem reasonable targets, and structural information is accruing on their bridge functions, architecture and roles in moving Lps through the periplasm.171, 172, 173, 174, 175, 176, 177, 178, 179, 180, 181, 182
Protegrin I is a naturally occurring disulfide-stabilized beta-turn antimicrobial peptide that targets LptD and served as inspiration for the rational design of template-stabilized beta-turn peptidomimetic scaffolds, such as POL7001, progressing towards clinically useful antimicrobial peptides targeting LptD.
Bacterial RNA polymerase: many natural products bind in adjacent subsites
Bacterial RNA polymerase has been a validated antibacterial target for decades. It is the target for rifampicin and derivatives as front-line agents in combination therapy against Mycobacterium tuberculosis. In fact, a wide range of natural product scaffolds have been examined and found to inhibit bacterial transcription by targeting RNA polymerase.186 One of the most recently approved antibiotics fidaxomicin, an 18 membered polyketide macrolactone (Figure 13a) from Dactylosporangium auranticum187 likewise blocks RNA transcription and has been approved by the FDA for the treatment of Clostridium difficile infections.188 The drug is poorly adsorbed from the gastrointestinal tract, supporting its use against C. difficile. As shown in Figure 13b, rifamycins189 and the natural product sorangicin190 bind to almost identical subsites of the enzyme while streptolydigin191 and myxopyronin192 bind in separate subsites.193 The bicyclic phosphate metabolite tagetitoxin from the phytopathogenic Pseudomonas syringae pv tagetis binds in yet a fourth subsite coordinating the Mg2+ in the active site.194 Nature clearly presents a rich variety of small molecular frameworks to target different pockets in RNAP. The specific binding subsite for fidaxomycin is not yet determined. One anticipates that other scaffolds may be found for additional or overlapping RNAP subsites and that structure-based evaluation might guide combinations directed against RNAP beyond Tb and C. difficile colitis.
(a) Structure of fidaxomycin, an 18-membered polyketide macrolactone bacterial RNAP inhibitor produced by Dactylosporangium auranticum approved by the FDA in 2011 for the treatment of C. difficile infections. (b) Surface structure of bacterial RNA polymerase from Thermus aquaticus showing the binding sites of a representative panel of natural product inhibitors (rifampin, sorangicin, streptolydigin, myxopyronin and tagetitoxin). Image was generated from PDB entries 1YNN189 (RNAP-rifampin complex; used for alignment of all structures), 1YNJ190 (RNAP-sorangicin complex), 1ZYR191 (RNAP-streptolydigin complex), 3DXJ192 (RNAP-myxopyronin complex) and 2BE5194 (RNAP-tagetitoxin complex) using PyMOL software.
ATP-dependent enzyme targets
For the past 15 years, inhibition of eukaryotic ATP-dependent protein kinases has been a mainstay of pharmaceutical and biotech research and development activity across a broad swath of human disease areas.195, 196 Although protein tyrosine kinase equivalent catalysts are almost absent in bacterial life, Ser/Thr kinases have become more prominent with knowledge of bacterial genomes. The histidine kinases that are the front end of dozens of two component signaling systems in bacteria have been investigated multiple times but, as yet, no robust, optimizable chemical scaffolds have emerged.197 Nonetheless, the ATP-dependent biotin carboxylase component of bacterial acetyl CoA carboxylase, the first committed step in fatty acid biosynthesis, has been targeted with specificity and potency by repurposed kinase libraries by a team at Pfizer.82 There is no a priori reason to think this need be an isolated success against a bacterial ATP-generating/consuming enzyme (for example, the Lps kinases that install the phosphates on lipid A)168 but does suggest investment in library design may be required.
Figure 14 introduces three additional such targets in bacteria. DNA gyrase, with type II topoisomerase activity for unwinding concatenated DNA at the end of replication, could be considered the grandfather of this ATP-targeting paradigm. In these topoisomerases, ATP hydrolysis powers the mechanical work of strand cleavage, passage and repair.1 The venerable and contemporary fluoroquinolones block the GyrA subunit and possibly the newly identified kibdelomycin family of natural products targets this same gyrase subunit,102 while the coumarin1 and cyclothialidine198 families of natural products inhibit the ATPase activity conferred by the GyrB subunit.
A second successful example of an antibiotic targeting an ATP-dependent bacterial enzyme is bedaquiline, a diarylquinoline identified in a screening campaign for molecules that could kill M. tuberculosis.199 The mechanism of action was determined by generation of resistant mutants and mapping them by whole-genome sequencing, allowing identification of the Fo subunit of the Mtb ATP synthase.200, 201 The molecule is specific for mycobacterial ATP synthase202 and has proven efficacy through phase II trials,199, 203 with a new drug application filed in July 2012 and approval granted at the start of 2013.45 Perhaps there are still more ATP-utilizing proteins within the Mtb proteome that might surface as valid therapeutic targets.204
The third potential antibacterial target, the chambered proteases of the ClpP family,205, 206 are acted on by a family of related lipopeptidolactones, known as ADEPS,207, 208 originally isolated from Streptococcus hawaiiensis in 1985 by scientists at Eli Lilly and Co.209 Semisynthetic tailoring of the scaffold has led to increased potency; for example, in ADEP2 (Figure 14).205 These bacterial chambered proteases, in mechanistic and structural analogy to eukaryotic chambered proteasomes, require ATP hydrolysis to unfold and thread protein substrates into the central cavity containing the protease sites. ADEPS are intriguing because they are actually activators, not inhibitors, of the basal protease activity of ClpP and so uncouple protease activity from ATP hydrolysis.205, 206 This occurs by allosteric activation207, 208 on the outer surface of the multisubunit proteases. Turning up unregulated protease activity is harmful to cells that contain active ClpPs. Of recent note is the connection of ADEP-mediated ClpP activity to disruption of cell division. One of the early key structural proteins to form the cell division ring is FtsZ. It is poorly folded and subject to the inappropriately activated ClpP-mediated degradation in ADEP-treated cells.210 In turn, the cell division septum does not form and/or is degraded and cell division abrogated. Although ADEPS may have liabilities in monotherapy, such as rates of mutation of the allosteric site to insensitivity, they may have value in combination regimens.
FtsZ itself is a homolog of eukyaryotic tubulin and shows GTPase activity involved in assembly of the divisome components.211 A molecule known as PC19073212 (Figure 15) has been reported to be an FtsZ inibitor by polymerization assays213 and X-ray crystallography.214 However, more recently, Shaw and coworkers215 failed to detect inhibition of GTPase activity. They also noted that many structures cited in preliminary reports as FtsZ inhibitors are either aggregators and/or nonspecific GTPase inhibitors. They pointed out zantrin Z3 (Figure 15) as a bona fide, specific albeit weak (IC50=20 μM) starting lead for future SAR work.215
Protein synthesis inhibitors
We noted previously that inhibition of protein synthesis is one of the five major clinically validated antibacterial pathways (Figure 5), with most antibiotics in this class targeting the ribosome.116 These have spurred at least one company Ribex to use structure-based approaches to design next-generation ribosome-directed antibiotics. We also noted new developments in tetracycline chemistry70 and still more structural information is being reported on this class of antibiotics.216 The clinical progression of second-generation oxazolidinones into phase II studies was also mentioned.74, 75, 76, 77, 78, 79, 80 Achaogen is working to bring forward new aminoglycoside protein synthesis inhibitors, such as plazomicin (ACHN-490), which successfully completed a phase II trial for urinary tract infections.217 Novartis has converted the natural thiopeptide GE2270A, an inhibitor of elongation factor Tu,218 to a semisynthetic version with a 105 increase in aqueous solubility and moved it into phase II trials for C. difficile infections.219 Other protein synthesis halting antibacterials currently in various stages of clinical development include members of the pleuromutilin (BC-3781, BC-7013, BC-3205) and macrolide (Cethromycin) structural classes.73
Summary thoughts
This perspective has argued that there is a continuing need for new cycles of antibiotic discovery and development. The genes found in the global resistomes are mobilizable with different frequencies to propel waves of resistant bacteria to each generation of newly introduced antibiotics. Given that the past half century has turned up few new molecular scaffolds, the fine tuning of existing frameworks by medicinal chemists may be approaching an asymptotic limit.
One small surprise has been the rise in usage/rediscovery of lipopeptides made by NRP synthetase machineries as antibiotics. Although daptomycin is the poster child of the past decade, ADEPS show unanticipated mechanisms, not working through membrane disruption. Even the polymyxins have come back into prominence, given the multidrug-resistant profiles of Gram-negative pathogens. There are certainly many more lipopeptide natural products in the biosphere, and they may be starting points for combination therapies. New approaches to interrogation of the biosynthetic capacity of the microbial world for conditional metabolites suggests new scaffolds will be found, presumably opening up additional rounds of both chemical and bioengineering optimization of those novel molecular scaffolds. Different approaches to synthetic library design may also enrich the hit rates in whole bacterial screens, especially to combat the permeability barriers and efflux pumps of the ESKAPE pathogens.
In parallel, we have opined on a select, possibly representative set of targets that we suggest are underexploited based on chemocentric past experience that promising, specific chemical matter has been identified, often in the form of natural product scaffolds. Improvements in biological assay designs and configurations almost always turn up new molecules. Smart screens have already shown that activity-guided isolation of novel natural molecular architectures is still possible. Several of these screens have assayed for resensitization and/or synergy with existing antibiotics to which pathogens have become insensitive. These augur for early guidance for combination therapies against particular pathogens.
More combination therapy seems a likely way forward, paralleling the trend of therapeutic modalities in viral infections and in cancer treatments. In that eventuality, coupling real-time diagnostics of the pathogen population in each patient to a proven or predictively effective combination of antibiotics may be a way forward, although Kishony and coworkers have noted the downside potential for resistance development in combination approaches.220
References
Walsh, C. Antibiotics: Actions, origins, and resistance, ASM Press: Washington DC, USA, (2003).
Kollonitsch, J., Barash, L., Kahan, F. M. & Kropp, H. New antibacterial agent via photofluorination of a bacterial cell wall constituent. Nature 243, 346–347 (1973).
Kollonitsch, J. & Barash, L. Organofluorine synthesis via photofluorination: 3-fluoro-D-alanine and 2-deuterio analogue, antibacterials related to the bacterial cell wall. J. Am. Chem. Soc. 98, 5591–5593 (1976).
Wang, E. & Walsh, C. Suicide substrates for the alanine racemase of Escherichia coli B. Biochemistry 17, 1313–1321 (1978).
Wang, E. A. & Walsh, C. Characteristics of β,β-difluoroalanine and β,β,β-trifluoroalanine as suicide substrates for Escherichia coli B alanine racemase. Biochemistry 20, 7539–7546 (1981).
Walsh, C. T. Suicide substrates, mechanism-based enzyme inactivators: recent developments. Ann. Rev. Biochem. 53, 493–535 (1984).
Faraci, W. S. & Walsh, C. T. Mechanism of inactivation of alanine racemase by β,β,β-trifluoroalanine. Biochemistry 28, 431–437 (1989).
Brown, E. D., Vivas, E. I., Walsh, C. T. & Kolter, R. MurA (MurZ), the enzyme that catalyzes the first committed step in peptidoglycan biosynthesis, is essential in Escherichia coli. J. Bacteriol. 177, 4194–4197 (1995).
Kim, D. H., Tucker-Kellogg, G. W., Lees, W. J. & Walsh, C. T. Analysis of fluoromethyl group chirality establishes a common stereochemical course for the enolpyruvate transfers catalyzed by EPSP synthase and UDP-GlcNAc enolpyruvyl transferase. Biochemistry 35, 5435–5440 (1996).
Skarzynski, T., Kim, D. H., Lees, W. J., Walsh, C. T. & Duncan, K. Stereochemical course of enzymatic enolpyruvyl transfer and catalytic conformation of the active site revealed by the crystal structure of the fluorinated analogue of the reaction tetrahedral intermediate bound to the active site of the C115A mutant of MurA. Biochemistry 37, 2572–2577 (1998).
Kim, D. H. et al. Characterization of a Cys115 to Asp substitution in the Escherichia coli cell wall biosynthetic enzyme UDP-GlcNAc enolpyruvyl transferase (MurA) that confers resistance to inactivation by the antibiotic fosfomycin. Biochemistry 35, 4923–4928 (1996).
Benson, T. E., Marquardt, J. L., Marquardt, A. C., Etzkorn, F. A. & Walsh, C. T. Overexpression, purification, and mechanistic study of UDP-N-acetylpyruvylglucosamine reductase. Biochemistry 32, 2024–2030 (1993).
Benson, T. E., Walsh, C. T. & Hogle, J. M. Crystallization and preliminary X-ray crystallographic studies of UDP-N-acetylpyruvylglucosamine reductase. Protein Sci. 3, 1125–1127 (1994).
Benson, T. E., Filman, D. J., Walsh, C. T. & Hogle, J. M. An enzyme-substrate complex involved in bacterial cell wall biosynthesis. Nat. Struct. Biol. 2, 644–653 (1995).
Benson, T. E., Walsh, C. T. & Hogle, J. M. The structure of the substrate-free form of MurB, an essential enzyme for the synthesis of bacterial cell walls. Structure 4, 47–54 (1996).
Lees, W. J., Benson, T. E., Hogle, J. M. & Walsh, C. T. (E)-Enolbutyryl-UDP-N-acetylglucosamine as a mechanistic probe of UDP-N-acetylenolpyruvylglucosamine reductase (MurB). Biochemistry 35, 1342–1351 (1996).
Benson, T. E., Walsh, C. T. & Massey, V. Kinetic characterization of wild-type and S229A mutant MurB: evidence for the role of Ser 229 as a general acid. Biochemistry 36, 796–805 (1997).
Benson, T. E., Walsh, C. T. & Hogle, J. M. X-ray crystal structures of the S229A mutant and wild-type MurB in the presence of the substrate enolpyruvyl-UDP-N-acetylglucosamine at 1.8-Å resolution. Biochemistry 36, 806–811 (1997).
Duncan, K., van Heijenoort, J. & Walsh, C. T. Purification and characterization of the D-alanyl-D-alanine-adding enzyme from Escherichia coli. Biochemistry 29, 2379–2386 (1990).
Walsh, C. T. Enzymes in the D-alanine branch of bacterial cell wall peptidoglycan assembly. J. Biol. Chem. 264, 2393–2396 (1989).
Bugg, T. D. H. & Walsh, C. T. Intracellular steps of bacterial cell wall peptidoglycan biosynthesis: enzymology, antibiotics, and antibiotic resistance. Nat. Prod. Rep. 9, 199–215 (1992).
Bugg, T. D. H. et al. Molecular basis for vancomycin resistance in Enterococcus faecium BM4147: biosynthesis of a depsipeptide peptidoglycan precursor by vancomycin resistance proteins VanH and VanA. Biochemistry 30, 10408–10415 (1991).
Chang, F., Moews, P. C., Walsh, C. T. & Knox, J. R. Vancomycin resistance: structure of D-alanine:D-alanine ligase at 2.3 Å resolution. Science 266, 439–443 (1994).
Shi, Y. & Walsh, C. T. Active site mapping of Escherichia coli D-Ala-D-Ala ligase by structure-based mutagenesis. Biochemistry 34, 2768–2776 (1995).
Lessard, I. A., Healy, V. L., Park, I. S. & Walsh, C. T. Determinants for differential effects on D-Ala-D-lactate vs D-Ala-D-Ala formation by the VanA ligase from vancomycin-resistant enterococci. Biochemistry 38, 14006–14022 (1999).
Kuzin, A. P. et al. Enzymes of vancomycin resistance: the structure of D-alanine-D-lactate ligase of naturally resistant Leuconostoc mesenteroides. Structure 8, 463–470 (2000).
Walsh, C. T., Fisher, S. L., Park, I. S., Prahalad, M. & Wu, Z. Bacterial resistance to vancomycin: fve genes and one missing hydrogen bond tell the story. Chem. Biol. 3, 21–28 (1996).
Healy, V. L., Lessard, I. A., Roper, D. I., Knox, J. R. & Walsh, C. T. Vancomycin resistance in enterococci: reprogramming of the D-Ala-D-Ala ligases in bacterial peptidoglycan biosynthesis. Chem. Biol. 7, R109–R119 (2000).
Kahne, D., Leimkuhler, C., Lu, W. & Walsh, C. Glycopeptide and lipoglycopeptide antibiotics. Chem. Rev. 105, 425–448 (2005).
Hubbard, B. K. & Walsh, C. T. Vancomycin assembly: nature’s way. Angew. Chem. Int. Ed. Engl. 42, 730–765 (2003).
Walsh, C. T. et al. Tailoring enzymes that modify nonribosomal peptides during and after chain elongation on NRPS assembly lines. Curr. Opin. Chem. Biol. 5, 525–534 (2001).
Walsh, C. T. Polyketide and nonribosomal peptide antibiotics: modularity and versatility. Science 303, 1805–1810 (2004).
Fischbach, M. A. & Walsh, C. T. Assembly-line enzymology for polyketide and nonribosomal peptide antibiotics: logic, machinery, and mechanisms. Chem. Rev. 106, 3468–3496 (2006).
Walsh, C. T. The chemical versatility of natural-product assembly lines. Acc. Chem. Res. 41, 4–10 (2008).
Sattely, E. S., Fischbach, M. A. & Walsh, C. T. Total biosynthesis: in vitro reconstitution of polyketide and nonribosomal peptide pathways. Nat. Prod. Rep. 25, 757–793 (2008).
Crosa, J. H. & Walsh, C. T. Genetics and assembly line enzymology of siderophore biosynthesis in bacteria. Microbiol. Mol. Biol. Rev. 66, 223–249 (2002).
Walsh, C. T. & Fischbach, M. A. Natural products version 2.0: connecting genes to molecules. J. Am. Chem. Soc. 132, 2469–2493 (2010).
Palumbi, S. R. Humans as the world's greatest evolutionary force. Science 293, 1786–1790 (2001).
Ronald, A. R., Turck, M. & Petersdorf, R. G. A critical evaluation of nalidixic acid in urinary-tract infections. New Engl. J. Med. 275, 1081–1089 (1966).
Kresken, M. & Wiedemann, B. Development of resistance to nalidixic acid and the fluoroquinolones after the introduction of norfloxacin and ofloxacin. Antimicrob. Agents Chemother. 32, 1285–1288 (1988).
Tsiodras, S. et al. Linezolid resistance in a clinical isolate of Staphylococcus aureus. Lancet 358, 207–208 (2001).
Sabol, K. et al. Emergence of daptomycin resistance in Enterococcus faecium during daptomycin therapy. Antimicrob. Agents Chemother. 49, 1664–1665 (2005).
Gentry, D. R. et al. Genetic characterization of Vga ABC proteins conferring reduced susceptibility to pleuromutilins in Staphylococcus aureus. Antimicrob. Agents Chemother. 52, 4507–4509 (2008).
Goldstein, E. J. C. et al. Comparative suscpetibilities to fidaxomicin (OPT-80) of isolates collected as baseline, recurrence, and failure from patients in two phase III trials of fidaxomicin against Clostridium difficile infection. Antimicrob. Agents Chemother. 55, 5194–5199 (2011).
Cohen, J. Approval of novel TB drug celebrated—with restraint. Science 339, 130 (2013).
Wright, G. D. The antibiotic resistome: the nexus of chemical and genetic diversity. Nat. Rev. Microbiol. 5, 175–186 (2007).
Forsberg, K. J. et al. The shared antibiotic resistome of soil bacteria and human pathogens. Science 337, 1107–1111 (2012).
Walsh, C. T. Vancomycin resistance: decoding the molecular logic. Science 261, 308–309 (1993).
Arthur, M. & Courvalin, P. Genetics and mechanisms of glycopeptide resistance in enterococci. Antimicrob. Agents Chemother. 37, 1563–1571 (1993).
D'Costa, V. M., McGrann, K. M., Hughes, D. W. & Wright, G. D. Sampling the antibiotic resistome. Science 311, 374–377 (2006).
Boucher, H. W. et al. Bad bugs, no drugs: no ESKAPE! an update from the Infectious Diseases Society of America. Clin. Infect. Dis. 48, 1–12 (2009).
Allington, D. R. & Rivey, M. P. Quinupristin/dalfopristin: a therapeutic review. Clin. Ther. 23, 24–44 (2001).
Tally, F. P. & DeBruin, M. F. Development of daptomycin for Gram-positive infections. J. Antimicrob. Chemother. 46, 523–526 (2000).
Falagas, M. E. & Kasiakou, S. K. Colistin: the revival of polymyxins for the management of multidrug-resistant Gram-negative bacterial infections. Clin. Infect. Dis. 40, 1333–1341 (2005).
Fernández, L. et al. Characterization of the polymyxin B resistome of Pseudomonas aeruginosa. Antimicrob. Agents Chemother. 57, 110–119 (2013).
Makarov, V. et al. Benzothiazinones kill Mycobacterium tuberculosis by blocking Arabinan synthesis. Science 324, 801–804 (2009).
Trefzer, C. et al. Benzothiazinones: prodrugs that covalently modify the decaprenylphosphoryl-β-D-ribose 2′-epimerase DprE1 of Mycobacterium tuberculosis. J. Am. Chem. Soc. 132, 13663–13665 (2010).
Trefzer, C. et al. Benzothiazinones are suicide inhibitors of mycobacterial decaprenylphosphoryl-β-D-ribofuranose 2'-oxidase DprE1. J. Am. Chem. Soc. 134, 912–915 (2012).
Batt, S. M. et al. Structural basis of inhibition of Mycobacterium tuberculosis DprE1 by benzothiazinone inhibitors. Proc. Natl Acad. Sci. USA 109, 11354–11359 (2012).
Neres, J. et al. Structural basis for benzothiazinone-mediated killing of Mycobacterium tuberculosis. Sci. Transl. Med. 4, 150ra121 (2012).
Tiwari, R. et al. Thiolates chemically induce redox activation of BTZ043 and related potent nitroaromatic anti-tuberculosis agents. J. Am. Chem. Soc. 135, 3539–3549 (2013).
Stover, C. K. et al. A small-molecule nitroimidazopyran drug cndidate for the treatment of tuberculosis. Nature 405, 962–966 (2000).
Ginsberg, A. M., Laurenzi, M. W., Rouse, D. J., Whitney, K. D. & Spigelman, M. K. Safety, tolerability, and pharmacokinetics of PA-824 in healthy subjects. Antimicrob. Agents Chemother. 53, 3720–3725 (2009).
Sacksteder, K. A., Protopopova, M., Barry, C. E. 3rd, Andries, K. & Nacy, C. A. Discovery and development of SQ109: a new antituberculosis drug with a novel mechanism of action. Future Microbiol. 7, 823–837 (2012).
Williams, K. N. et al. Promising antituberculosis activity of the oxazolidinone PNU-100480 relative to that of linezolid in a murine model. Antimicrob. Agents Chemother. 53, 1314–1319 (2009).
Villemagne, B. et al. Tuberculosis: the drug development pipeline at a glance. Eur. J. Med. Chem. 51, 1–16 (2012).
Lienhardt, C. et al. New drugs for the treatment of tuberculosis: needs, challenges, promise, and prospects for the future. J. Infect. Dis. 205, s241–s249 (2012).
Drug Discovery and Development. Understanding the R & D Process, Pharmaceutical Research and Manufacturers of America: Washington, DC, USA, (2007).
Amyes, S. G. B. Magic Bullets, Lost Horizons: The Rise and Fall of Antibiotics, Taylor and Francis, (2001).
Sun, C. et al. Synthesis and antibacterial activity of pentacyclines: a novel class of tetracycline analogs. J. Med. Chem. 54, 3704–3731 (2011).
Rafailidis, P. I., Polyzos, K. A., Sgouros, K. & Falagas, M. E. Prulifloxacin: a review focusing on its use beyond respiratory and urinary tract infections. Int. J. Antimicrob. Agents 37, 283–290 (2011).
Fischbach, M. A. & Walsh, C. T. Antibiotics for emerging pathogens. Science 325, 1089–1093 (2009).
Butler, M. S. & Cooper, M. A. Antibiotics in the clinical pipeline in 2011. J. Antibiot. 64, 413–425 (2011).
Bin Im, W. et al. Discovery of torezolid as a novel 5-hydroxymethyl-oxazolidinone antibacterial agent. Eur. J. Med. Chem. 46, 1027–1039 (2011).
Brown, S. D. & Traczewski, M. M. Comparative in vitro antimicrobial activities of torezolid (TR-700), the active moiety of a new oxazolidinone, torezolid phosphate (TR-701), determination of tentative disk diffusion interpretive criteria, and quality control ranges. Antimicrob. Agents Chemother. 54, 2063–2069 (2010).
Prokocimer, P. et al. Phase 2, randomized, double-blind, dose-ranging study evaluating the safety, tolerability, population pharmacokinetics, and efficacy of oral torezolid phosphate in patients with complicated skin and skin structure infections. Antimicrob. Agents Chemother. 55, 583–592 (2011).
Skripkin, E. et al. RX-01, a new family of oxazolidinones that overcome ribosome-based linezolid resistance. Antimicrob. Agents Chemother. 52, 3550–3557 (2008).
Zhou, J. et al. Design at the atomic level: design of biaryloxazolidinones as potent orally active antibiotics. Bioorg. Med. Chem. Lett. 18, 6175–6178 (2008).
Lemaire, S., Tulkens, P. M. & Van Bambeke, F. Cellular pharmacokinetics of the novel biaryloxazolidinone radezolid in phagocytic cells: studies with macrophages and polymorphonuclear neutrophils. Antimicrob. Agents Chemother. 54, 2540–2548 (2010).
Lemaire, S. et al. Cellular pharmacodynamics of the novel biaryloxazolidinone radezolid: studies with infected phagocytic and nonphagocytic cells, using Staphylococcus aureus, Staphylococcus epidermidis, Listeria monocytogenes, and Legionella pneumophila. Antimicrob. Agents Chemother. 54, 2549–2559 (2010).
Payne, D. J., Gwynn, M. N., Holmes, D. J. & Pompliano, D. L. Drugs for bad bugs: confronting the challenges of antibacterial discovery. Nat. Rev. Drug Discov. 6, 29–40 (2007).
Mochalkin, I. et al. Discovery of antibacterial biotin carboxylase inhibitors by virtual screening and fragment-based approaches. ACS Chem. Biol. 4, 473–483 (2009).
Schreiber, S. L. Target-oriented and diversity-oriented organic synthesis in drug discovery. Science 287, 1964–1969 (2000).
Galloway, W. R. J. D., Bender, A., Welch, M. & Spring, D. R. The discovery of antibacterial agents using diversity-oriented synthesis. Chem. Commun. 2446–2462 (2009).
Nielsen, T. E. & Schreiber, S. L. Towards the optimal screening collection: a synthesis strategy. Angew. Chem. Int. Ed. Engl. 47, 48–56 (2008).
Schreiber, S. L. Organic synthesis toward small-molecule probes and drugs. Proc. Natl Acad. Sci. USA 108, 6699–6702 (2011).
Martínez-Botella, G. et al. Discovery of selective and potent inhibitors of Gram-positive bacterial thymidylate kinase (TMK). J. Med. Chem. 55, 10010–10021 (2012).
Keating, T. A. et al. In vivo validation of thymidylate kinase (TMK) with a rationally designed, selective antibacterial compound. ACS Chem. Biol. 7, 1866–1872 (2012).
Yong Choi, J. et al. Structure guided development of novel thymidine mimetics targeting Pseudomonas aeruginosa thymidylate kinase: from hit to lead generation. J. Med. Chem. 55, 852–870 (2012).
Van Poecke, S., Munier-Lehmann, H., Helynck, O., Froeyen, M. & Van Calenbergh, S. Synthesis and inhibitory activity of thymidine analogues targeting Mycobacterium tuberculosis thymidine monophosphate kinase. Bioorg. Med. Chem. 19, 7603–7611 (2011).
Cui, H. et al. Synthesis and evaluation of α-thymidine analogues as novel antimalarials. J. Med. Chem. 55, 10948–10957 (2012).
Martínez-Botella, G. et al. Sulfonylpiperidine as novel, antibacterial inhibitors of Gram-positive thymidylate kinase (TMK). Bioorg. Med. Chem. Lett. 23, 169–173 (2013).
Toti, K. S. et al. Synthesis and evaluation of 5′-modified thymidines and 5-hydroxymethyl-2′-deoxyuridines as Mycobacterium tuberculosis thymidylate kinase inhibitors. Bioorg. Med. Chem. 21, 257–268 (2013).
Kaeberlein, T., Lewis, K. & Epstein, S. S. Isolating ‘uncultivable’ microorganisms in pure culture in a simulated natural environment. Science 296, 1127–1129 (2002).
D'Onofrio, A. et al. Siderophores from neighboring organisms promote the growth of uncultured bacteria. Chem. Biol. 17, 254–264 (2010).
Lewis, K., Epstein, S., D'Onofrio, A. & Ling, L. L. Uncultured microorganisms as a source of secondary metabolites. J. Antibiot. 63, 468–476 (2010).
Clardy, J., Fischbach, M. A. & Walsh, C. T. New antibiotics from bacterial natural products. Nat. Biotechnol. 24, 1541–1550 (2006).
Bode, H. B. & Müller, R. The impact of bacterial genomics on natural product research. Angew. Chem. Int. Ed. Engl. 44, 6828–6846 (2005).
Wang, J. et al. Platensimycin is a selective FabF inhibitor with potent antibiotic properties. Nature 441, 358–361 (2006).
Young, K. et al. Discovery of FabH/FabF inhibitors from natural products. Antimicrob. Agents Chemother. 50, 519–526 (2006).
Brinster, S. et al. Type II fatty acid synthesis is not a suitable antibiotic target for Gram-positive pathogens. Nature 458, 83–87 (2009).
Phillips, J. W. et al. Discovery of kibdelomycin, a potent new class of bacterial type II topoisomerase inhibitor by chemical-genetic profiling in Staphylococcus aureus. Chem. Biol. 18, 955–965 (2011).
Bister, B. et al. Abyssomycin C-A polycyclic antibiotic from a marine Verrucosispora strain as an inhibitor of the p-aminobenzoic acid/tetrahydrofolate biosynthesis pathway. Angew. Chem. Int. Ed. Engl. 43, 2574–2576 (2004).
Watve, M. G., Tickoo, R., Jog, M. M. & Bhole, B. D. How many antibiotics are produced by the genus Streptomyces? Arch. Microbiol. 176, 386–390 (2001).
Challis, G. L. Genome mining for novel natural product discovery. J. Med. Chem. 51, 2618–2628 (2008).
Challis, G. L. Mining microbial genomes for new natural products and biosynthetic pathways. Microbiology 154, 1555–1569 (2008).
McAlpine, J. B. Advances in the understanding and use of the genomic base of microbial secondary metabolite biosynthesis for the discovery of new natural products. J. Nat. Prod. 72, 566–572 (2009).
Banskota, A. H. et al. Genomic analyses lead to novel secondary metabolites. J. Antibiot. 59, 533–542 (2006).
Udwary, D. W. et al. Significant natural product biosynthetic potential of actinorhizal symbionts of the genus Frankia, as revealed by comparative genomic and proteomic analyses. Appl. Environ. Microbiol. 77, 3617–3625 (2011).
Letzel, A.-C., Pidot, S. J. & Hertweck, C. A genomic approach to the cryptic secondary metabolome of the anaerobic world. Nat. Prod. Rep. 30, 392–428 (2013).
Brakhage, A. A. & Schroeckh, V. Fungal secondary metabolites—strategies to activate silent gene clusters. Fungal Genet. Biol. 48, 15–22 (2011).
Cichewicz, R. H. Epigenome manipulation as a pathway to new natural product scaffolds and their congeners. Nat. Prod. Rep. 27, 11–22 (2010).
Chiang, Y.-M., Chang, S.-L., Oakley, B. R. & Wang, C. C. C. Recent advances in awakening silent biosynthetic gene clusters and linking orphan clusters to natural products in microorganisms. Curr. Opin. Chem. Biol. 15, 137–143 (2011).
Brady, S. F., Simmons, L., Kim, J. H. & Schmidt, E. W. Metagenomic approaches to natural products from free-living and symbiotic organisms. Nat. Prod. Rep. 26, 1488–1503 (2009).
Kallifidas, D., Kang, H.-S. & Brady, S. F. Tetarimycin A, an MRSA-active antibiotic identified through induced expression of environmental DNA gene clusters. J. Am. Chem. Soc. 134, 19552–19555 (2012).
Wilson, D. N. The A-Z of bacterial translation inhibitors. Crit. Rev. Biochem. Mol. Biol. 44, 393–433 (2009).
Scholar, E. M. & Pratt, W. B. The Antimicrobial Drugs 2nd ed. Oxford University Press: New York, NY, USA, (2000).
Baltz, R. H. Daptomycin: mechanisms of action and resistance, and biosynthetic engineering. Curr. Opin. Chem. Biol. 13, 144–151 (2009).
Robbel, L. & Marahiel, M. A. Daptomycin, a bacterial lipopeptide synthesized by a nonribosomal machinery. J. Biol. Chem. 285, 27501–27508 (2010).
Donald, R. G. K. et al. A Staphylococcus aureus fitness test platform for mechanism-based profiling of antibacterial compounds. Chem. Biol. 16, 826–836 (2009).
Ho Lee, S. et al. Antagonism of chemical genetic interaction networks resensitize MRSA to β-lactam antibiotics. Chem. Biol. 18, 1379–1389 (2011).
Huber, J. et al. Chemical genetic identification of peptidoglycan inhibitors potentiating carbapenem activity against methicillin-resistant Staphylococcus aureus. Chem. Biol. 16, 837–848 (2009).
Roemer, T., Davies, J., Giaever, G. & Nislow, C. Bugs, drugs and chemical genomics. Nat. Chem. Biol. 8, 46–56 (2012).
Kim, D.-S. et al. New syntheses of E7389 C14-C35 and halichondrin C14-C38 building blocks: double-inversion approach. J. Am. Chem. Soc. 131, 15636–15641 (2009).
Hollenhorst, M. A., Ntai, I., Badet, B., Kelleher, N. L. & Walsh, C. T. A head-to-head comparison of eneamide and epoxyamide inihbitors of glucosamine-6-phosphate synthase from the dapdiamide biosynthetic pathway. Biochemistry 50, 3859–3861 (2011).
Milewski, S. et al. Mechanism of action of anticandidal dipeptides containing inhibitors of glucosamine-6-phosphate synthase. Antimicrob. Agents Chemother. 35, 36–43 (1991).
Campbell, J. et al. Synthetic lethal compound combinations reveal a fundamental connection between wall teichoic acid and peptidoglycan biosyntheses in Staphylococcus aureus. ACS Chem. Biol. 6, 106–116 (2011).
Coleman, K. Diazabicyclooctanes (DBOs): a potent new class of non-β-lactam β-lactamase inhibitors. Curr. Opin. Microbiol. 14, 550–555 (2011).
Ehmann, D. E. et al. Avibactam is a covalent, reversible, non-β-lactam β-lactamase inhibitor. Proc. Natl Acad. Sci. USA 109, 11663–11668 (2012).
Ostash, B. & Walker, S. Moenomycin family antibiotics: chemical synthesis, biosynthesis, and biological activity. Nat. Prod. Rep. 27, 1594–1617 (2010).
Lovering, A. L., de Castro, L. H., Lim, D. & Strynadka, N. C. J. Structural insight into the transglycosylation step of bacterial cell-wall biosynthesis. Science 315, 1402–1405 (2007).
Yuan, Y. et al. Crystal structure of a peptidoglycan glycosyltransferase suggests a model for processive glycan chain synthesis. Proc. Natl Acad. Sci. USA 104, 5348–5353 (2007).
Sung, M.-T. et al. Crystal structure of the membrane-bound bifunctional transglycosylase PBP1b from Escherichia coli. Proc. Natl Acad. Sci. USA 106, 8824–8829 (2009).
Yuan, Y. et al. Structural analysis of the contacts anchoring moenomycin to peptidoglycan glycosyltransferases and implications for antibiotic design. ACS Chem. Biol. 3, 429–436 (2008).
Heaslet, H., Shaw, B., Mistry, A. & Miller, A. A. Characterization of the active site of S. aureus monofunctional glycosyltransferas (Mtg) by site-directed mutation and structural analysis of the protein complexed with moenomycin. J. Struct. Biol. 167, 129–135 (2009).
Fuse, S. et al. Functional and structural analysis of a key region of the cell wall inhibitor moenomycin. ACS Chem. Biol. 5, 701–711 (2010).
Taylor, J. G., Li, X., Oberthür, M., Zhu, W. & Kahne, D. E. The total synthesis of moenomycin A. J. Am. Chem. Soc. 128, 15084–15085 (2006).
Ostash, B. et al. Complete characterization of the seventeen step moenomycin biosynthetic pathway. Biochemistry 48, 8830–8841 (2009).
Gampe, C. M., Tsukamoto, H., Doud, E. H., Walker, S. & Kahne, D. Tuning the moenomycin pharmacophore to enable discovery of bacterial cell wall synthesis inhibitors. J. Am. Chem. Soc. 135, 3776–3779 (2013).
Mohammadi, T. et al. Identification of FtsW as a transporter of lipid-linked cell wall precursors across the membrane. EMBO J. 30, 1425–1432 (2011).
Breukink, E. & de Kruijff, B. Lipid II as a target for antibiotics. Nat. Rev. Drug Discov. 5, 321–332 (2006).
Nitanai, Y. et al. Crystal structures of the complexes between vancomycin and cell-wall precursor analogs. J. Mol. Biol. 385, 1422–1432 (2009).
Hsu, S.-T. D. et al. The nisin-lipid II complex reveals a pyrophosphate cage that provides a blueprint for novel antibiotics. Nat. Struct. Mol. Biol. 11, 963–967 (2004).
Schneider, T. et al. Plectasin, a fungal defensin, targets the bacterial cell wall precursor lipid II. Science 328, 1168–1172 (2010).
Fjell, C. D., Hiss, J. A., Hancock, R. E. W. & Schneider, G. Designing antimicrobial peptides: form follows function. Nat. Rev. Drug Discov. 11, 37–51 (2012).
Xie, J., Pierce, J. G., James, R. C., Okano, A. & Boger, D. L. A redesigned vancomycin engineered for dual D-Ala-D-Ala and D-Ala-D-Lac binding exhibits potent antimicrobial activity against vancomycin-resistant bacteria. J. Am. Chem. Soc. 133, 13946–13949 (2011).
James, R. C., Pierce, J. G., Okano, A., Xie, J. & Boger, D. L. Redesign of glycopeptide antibiotics: back to the future. ACS Chem. Biol. 7, 797–804 (2012).
Ralph Corey, G., Stryjewski, M. E., Weyenberg, W., Yasothan, U. & Kirkpatrick, P. Telavancin. Nat. Rev. Drug Discov. 8, 929–930 (2009).
Liu, J. et al. Synthesis and characterization of the arylomycin lipoglycopeptide antibiotics and the crystallographic analysis of their complex with signal peptidase. J. Am. Chem. Soc. 133, 17869–17877 (2011).
Smith, P. A. & Romesberg, F. E. Mechanism of action of the arylomycin antibiotics and effects of signal peptidase I inihbition. Antimicrob. Agents Chemother. 56, 5054–5060 (2012).
Therien, A. G. et al. Broadening the spectrum of β-lactam antibiotics through inhibition of signal peptidase type I. Antimicrob. Agents Chemother. 56, 4662–4670 (2012).
Xiao, Y., Gerth, K., Müller, R. & Wall, D. Myxobacterium-produced antibiotic TA (Myxovirescin) inhibits type II signal peptidase. Antimicrob. Agents Chemother. 56, 2014–2021 (2012).
Dev, I. K., Harvey, R. J. & Ray, P. H. Inhibition of prolipoprotein signal peptidase by globomycin. J. Biol. Chem. 260, 5891–5894 (1985).
Kogen, H. et al. Crystal structure and total synthesis of globomycin: establishment of relative and absolute configurations. J. Am. Chem. Soc. 122, 10214–10215 (2000).
Liu, W.-T., Kersten, R. D., Yang, Y.-L., Moore, B. S. & Dorrestein, P. C. Imaging mass spectrometry and genome mining via short sequence tagging identified the anti-infective agent arylomycin in Streptomyces roseosporus. J. Am. Chem. Soc. 133, 18010–18013 (2011).
Roberts, T. C., Schallenberger, M. A., Liu, J., Smith, P. A. & Romesberg, F. E. Initial efforts toward the optimization of arylomycins for antibiotic activity. J. Med. Chem. 54, 4954–4963 (2011).
Paetzel, M., Karla, A., Strynadka, N. C. J. & Dalbey, R. E. Signal peptidases. Chem. Rev. 102, 4549–4579 (2002).
Content, S., Dutton, C. J. & Roberts, L. Myxovirescin analogues via macrocyclic ring-closing metathesis. Bioorg. Med. Chem. Lett. 13, 321–325 (2003).
Fürstner, A. et al. Total synthesis of Myxovirescin A1 . Chem. Eur. J. 13, 8762–8783 (2007).
Kiho, T. et al. Structure-activity relationships of globomycin analogues as antibiotics. Bioorg. Med. Chem. 12, 337–361 (2004).
Sarabia, F., Chammaa, S. & García-Ruiz, C. Solid phase synthesis of globomycin and SF-1902 A5 . J. Org. Chem. 76, 2132–2144 (2011).
Jin, X. et al. Biosynthesis of new lipopentapeptides by an engineered strain of Streptomyces sp. Biotechnol. Lett. 34, 2283–2289 (2012).
Simunovic, V. et al. Myxovirescin A biosynthesis is directed by hybrid polyketide synthases/nonribosomal peptide synthetase, 3-hydroxy-3-methylglutaryl-CoA synthases, and trans-acting acyltransferases. ChemBioChem 7, 1206–1220 (2006).
Simunovic, V. & Müller, R. 3-Hydroxy-3-methylglutaryl-CoA-like synthases direct the formation of methyl and ethyl side groups in the biosynthesis of the antibiotic Myxovirescin A. ChemBioChem 8, 497–500 (2007).
Simunovic, V. & Müller, R. Mutational analysis of the Myxovirescin biosynthetic gene cluster reveals novel insights into the functional elaboration of polyketide backbones. ChemBioChem 8, 1273–1280 (2007).
Calderone, C. T., Iwig, D. F., Dorrestein, P. C., Kelleher, N. L. & Walsh, C. T. Incorporation of nonmethyl branches by isoprenoid-like logic: multiple β-alkylation events in the biosynthesis of Myxovirescin A1. Chem. Biol. 14, 835–846 (2007).
Anderson, M. S., Robertson, A. D., Macher, I. & Raetz, C. R. H. Biosynthesis of lipid A in Escherichia coli: identification of UDP-3-O-[(R)-3-hydroxymyristoyl]-α-D-glucosamine as a precursor of UDP-N2,O3-bis[(R)-3-hydroxymyristoyl]-α-D-glucosamine. Biochemistry 27, 1908–1917 (1988).
Raetz, C. R. H. & Whitfield, C. Lipopolysaccharide endotoxins. Annu. Rev. Biochem. 71, 635–700 (2002).
Barb, A. W., Jiang, L., Raetz, C. R. H. & Zhou, P. Structure of the deacetylase LpxC bound to the antibiotic CHIR-090: time-dependent inhibition and specificity in ligand binding. Proc. Natl Acad. Sci. USA 104, 18433–18438 (2007).
Lee, C.-J. et al. Species-specific and inhibitor-dependent conformations of LpxC: implications for antibiotic design. Chem. Biol. 18, 38–47 (2011).
Villa, R. et al. The Escherichia coli Lpt transenvelope protein complex for lipopolysaccharide export is assembled via conserved structurally homologous domains. J. Bacteriol. 195, 1100–1108 (2013).
Okuda, S., Freinkman, E. & Kahne, D. Cytoplasmic ATP hydrolysis powers transport of lipopolysaccharide across the periplasm in E. coli. Science 338, 1214–1217 (2012).
Chng, S.-S. et al. Disulfide rearrangement triggered by translocon assembly controls lipopolysaccharide export. Science 337, 1665–1668 (2012).
Freinkman, E., Okuda, S., Ruiz, N. & Kahne, D. Regulated assembly of the transenvelope protein complex required for lipopolysaccharide export. Biochemistry 51, 4800–4806 (2012).
Chimalakonda, G. et al. Lipoprotein LptE is required for the assembly of LptD by the β-barrel assembly machine in the outer membrane of Escherichia coli. Proc. Natl Acad. Sci. USA 108, 2492–2497 (2011).
Freinkman, E., Chng, S.-S. & Kahne, D. The complex that inserts lipopolysaccharide into the bacterial outer membrane forms a two-protein plug-and-barrel. Proc. Natl Acad. Sci. USA 108, 2486–2491 (2011).
Ruiz, N., Chng, S.-S., Hiniker, A., Kahne, D. & Silhavy, T. J. Nonconsecutive disulfide bond formation in an essential integral outer membrane protein. Proc. Natl Acad. Sci. USA 107, 12245–12250 (2010).
Chng, S.-S., Ruiz, N., Chimalakonda, G., Silhavy, T. J. & Kahne, D. Characterization of the two-protein complex in Escherichia coli responsible for lipopolysaccharide assembly at the outer membrane. Proc. Natl Acad. Sci. USA 107, 5363–5368 (2010).
Gronenberg, L. S. & Kahne, D. Development of an activity assay for discovery of inhibitors of lipopolysaccharide transport. J. Am. Chem. Soc. 132, 2518–2519 (2010).
Ruiz, N., Kahne, D. & Silhavy, T. J. Transport of lipopolysaccharide across the cell envelope: the long road of discovery. Nat. Rev. Microbiol. 7, 677–683 (2009).
Chng, S.-S., Gronenberg, L. S. & Kahne, D. Proteins required for lipopolysaccharide assembly in Escherichia coli form a transenvelope complex. Biochemistry 49, 4565–4567 (2010).
Kim, S. et al. Structure and function of an essential component of the outer membrane protein assembly machine. Science 317, 961–964 (2007).
Srinivas, N. et al. Peptidomimetic antibiotics target outer-membrane biogenesis in Pseudomonas aeruginosa. Science 327, 1010–1013 (2010).
Shankaramma, S. C. et al. Macrocyclic hairpin mimetics of the cationic antimicrobial peptide protegrin I: a new family of broad-spectrum antibiotics. ChemBioChem 3, 1126–1133 (2002).
Robinson, J. A. et al. Properties and structure-activity studies of cyclic β-haripin peptidomimetics based on the cationic antimicrobial peptide protegrin I. Bioorg. Med. Chem. 13, 2055–2064 (2005).
Mariani, R. & Maffioli, S. I. Bacterial RNA polymerase inhibitors: an organized overview of their structures, derivatives, biological activity and current clinical development status. Curr. Med. Chem. 16, 430–454 (2009).
Erb, W. & Zhu, J. From natural product to marketed drug: the tiacumicin odyssey. Nat. Prod. Rep. 30, 161–174 (2013).
Venugopal, A. A. & Johnson, S. Fidaxomicin: a novel macrocyclic antibiotic approved for treatment of Clostridium difficile infection. Clin. Infect. Dis. 54, 568–574 (2012).
Campbell, E. A. et al. Structural mechanism for rifampicin inhibition of bacterial RNA polymerase. Cell 104, 901–912 (2001).
Campbell, E. A. et al. Structural, functional, and genetic analysis of sorangicin inhibition of bacterial RNA polymerase. EMBO J. 24, 674–682 (2005).
Tuske, S. et al. Inhibition of bacterial RNA polymerase by streptolydigin: stabilization of a straight-bridge-helix active-center conformation. Cell 122, 541–552 (2005).
Mukhopadhyay, J. et al. The RNA polymerase ‘switch region’ is a target for inhibitors. Cell 135, 295–307 (2008).
Ho, M. X., Hudson, B. P., Das, K., Arnold, E. & Ebright, R. H. Structures of RNA polymerase-antibiotic complexes. Curr. Opin. Struct. Biol. 19, 715–723 (2009).
Vassylyev, D. G. et al. Structural basis for transcription inhibition by tagetitoxin. Nat. Struct. Mol. Biol. 12, 1086–1093 (2005).
Cohen, P. Protein kinases—the major drug targets of the twenty-first century? Nat. Rev. Drug Discov. 1, 309–315 (2002).
Karaman, M. W. et al. A quantitative analysis of kinase inhibitor selectivity. Nat. Biotechnol. 26, 127–132 (2008).
Škedelj, V., Tomašić, T., Peterlin Mašič, L. & Zega, A. ATP-binding bite of bacterial enzymes as a target for antibacterial drug design. J. Med. Chem. 54, 915–929 (2011).
Angehrn, P. et al. A new DNA gyrase inhibitor subclass of the cyclothialidine family based on a bicyclic dilactam-lactone scaffold. Synthesis and antibacterial properties. J. Med. Chem. 54, 2207–2224 (2011).
Diacon, A. H. et al. The diarylquinolone TMC207 for multidrug-resistant tuberculosis. N. Engl. J. Med. 360, 2397–2405 (2009).
Andries, K. et al. A diarylquinoline drug active on the ATP synthase of Mycobacterium tuberculosis. Science 307, 223–227 (2005).
Koul, A. et al. Diarylquinolines target subunit C of mycobacterial ATP synthase. Nat. Chem. Biol. 3, 323–324 (2007).
Haagsma, A. C. et al. Selectivity of TMC207 towards mycobacterial ATP synthase compared with that towards the eukaryotic homologue. Antimicrob. Agents Chemother. 53, 1290–1292 (2009).
Rustomjee, R. et al. Early bactericidal activity and pharmacokinetics of the diarylquinoline TMC207 in treatment of pulmonary tuberculosis. Antimicrob. Agents Chemother. 52, 2831–2835 (2008).
Wolfe, L. M. et al. A chemical proteomics approach to profiling the ATP-binding proteome of Mycobacterium tuberculosis. Mol. Cell. Proteomics (e-pub ahead of print 5 March 2013; doi:10.1074/mcp.M112.025635) (2013).
Brötz-Oesterhelt, H. et al. Dysregulation of bacterial proteolytic machinery by a new class of antibiotics. Nat. Med. 11, 1082–1087 (2005).
Frees, D., Savijoki, K., Varmanen, P. & Ingmer, H. Clp ATPases and ClpP proteolytic complexes regulate vital biological processes in low GC, Gram-positive bacteria. Mol. Microbiol. 63, 1285–1295 (2007).
Lee, B.-G. et al. Structures of ClpP in complex with acyldepsipeptide antibiotics reveal its activation mechanism. Nat. Struct. Mol. Biol. 17, 471–479 (2010).
Shun, L. i.,D. H. et al. Acyldepsipeptide antibiotics induce the formation of a structured axial channel in ClpP: a model for the ClpX/ClpA-bound state of ClpP. Chem. Biol. 17, 959–969 (2010).
Michel, K. H. & Kastner, R. E. A54556 antibiotics and process for production thereof. US Patent 4492650 (1985).
Sass, P. et al. Antibiotic acyldepsipeptides activate ClpP peptidase to degrade the cell division protein FtsZ. Proc. Natl Acad. Sci. USA 108, 17474–17479 (2011).
Erickson, H. P., Anderson, D. E. & Osawa, M. FtsZ in bacterial cytokinesis: cytoskeleton and force generator all in one. Microbiol. Mol. Biol. Rev. 74, 504–528 (2010).
Haydon, D. J. et al. An inhibitor of FtsZ with potent and selective anti-Staphylococcal activity. Science. 321, 1673–1675 (2008).
Andreu, J. M. et al. The antibacterial cell division inhibitor PC190723 is an FtsZ polymer-stabilizing agent that induces filament assembly and condensation. J. Biol. Chem. 285, 14239–14246 (2010).
Tan, C. M. et al. Restoring methicillin-resistant Staphylococcus aureus susceptibility to β-lactam antibiotics. Sci. Transl. Med. 4, 126ra135 (2012).
Anderson, D. E. et al. Comparison of small molecule inhibitors of the bacterial cell division protein FtsZ and identification of a reliable cross-species inhibitor. ACS Chem. Biol. 7, 1918–1928 (2012).
Jenner, L. et al. Structural basis for potent inhibitory activity of the antibiotic tigecycline during protein synthesis. Proc. Natl Acad. Sci. USA 110, 3812–3816 (2013).
Becker, B. & Cooper, M. A. Aminoglycoside antibiotics in the 21st century. ACS Chem. Biol. 8, 105–115 (2013).
Parmeggiani, A. et al. Structural basis of the action of pulvomycin and GE2270 A on elongation factor Tu. Biochemistry 45, 6846–6857 (2006).
LaMarche, M. J. et al. Discovery of LFF571: an investigational agent for Clostridium difficile infection. J. Med. Chem. 55, 2376–2387 (2012).
Chait, R., Vetsigian, K. & Kishony, R. What counters antibiotic resistance in nature? Nat. Chem. Biol. 8, 2–5 (2012).
Acknowledgements
We sincerely thank Gerry Wright for thinking up this issue and all the authors who contribute articles in it. We acknowledge research efforts in our laboratory supported by NIH Grants GM 20011 and GM 49338 and the many colleagues in the Walsh group, some of whom are noted in specific references.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
CTW is on the Board of Directors of Achaogen, which has plazomicin in clinical trials.
Rights and permissions
About this article
Cite this article
Walsh, C., Wencewicz, T. Prospects for new antibiotics: a molecule-centered perspective. J Antibiot 67, 7–22 (2014). https://doi.org/10.1038/ja.2013.49
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ja.2013.49
Keywords
This article is cited by
-
Exfoliation, functionalization and antibacterial activity of transition metal dichalcogenides
Tungsten (2024)
-
Dynamics and Sensitivity of Signaling Pathways
Current Pathobiology Reports (2022)
-
A Biophysical Study of Ru(II) Polypyridyl Complex, Properties and its Interaction with DNA
Journal of Fluorescence (2022)
-
Streptomyces marianii sp. nov., a novel marine actinomycete from southern coast of India
The Journal of Antibiotics (2021)
-
Modular synthesis enables molecular ju-jitsu in the fight against antibiotic resistance
Nature (2020)