Abstract
Objective:
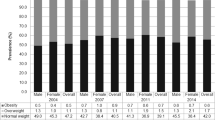
Previous data indicate a rapidly increasing prevalence of obesity and overweight among English children and an emerging socioeconomic gradient in prevalence. The main aim of this study was to update the prevalence trends among school-age children and assess the changing socioeconomic gradient.
Design:
A series of nationally representative household-based health surveys conducted between 1997 and 2007 in England.
Subjects:
15 271 white children (7880 boys) aged 5 to 10 years with measured height and weight.
Measurements:
Height and weight were directly measured by trained fieldworkers. Overweight (including obesity) and obesity prevalence were calculated using the international body mass index cut-offs. Socioeconomic position (SEP) score was a composite score based on income and social class. Multiple linear regression assessed the prevalence odds with time point (1997/8, 2000/1, 2002/3, 2004/5, 2006/7) as the main exposure. Linear interaction terms of time by SEP were also tested for.
Results:
There are signs that the overweight and obesity trend has levelled off from 2002/3 to 2006/7. The odds ratio (OR) for overweight in 2006/7 compared with 2002/3 was 0.99 (95% CI 0.88–1.11) and for obesity OR=1.06 (0.86–1.29). The socioeconomic gradient has increased in recent years, particularly in 2006/7. Compared to 1997/8, the 2006/7 age and sex-adjusted OR for overweight was 1.88 (1.52 to 2.33) in low-SEP, 1.25 (1.04 to 1.50) in middle-SEP, and 1.13 (0.86 to 1.48) in high-SEP children.
Conclusion:
Childhood obesity and overweight prevalence among school-age children in England has stabilized in recent years, but children from lower socio-economic strata have not benefited from this trend. There is an urgent need to reduce socio-economic disparities in childhood overweight and obesity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Lobstein T . Obesity in children and young people: a crisis in public health. Obes Rev 2004; 5 (s1): 4–85.
Popkin BM, Conde W, Hou N, Monteiro C . Is there a lag globally in overweight trends for children compared with adults? Obesity 2006; 14: 1846–1853.
Von Mutius E, Schwartz J, Neas LM, Dockery D, Weiss ST . Relation of body mass index to asthma and atopy in children: the National Health and Nutrition Examination Study III. Thorax 2001; 56: 835–838.
Fagot-Campagna A, Pettitt DJ, Engelgau MM, Burrows NR, Geiss LS, Valdez R et al. Type 2 diabetes among North American children and adolescents: an epidemiologic review and a public health perspective. J Pediatr 2000; 136: 664–672.
Kvaavik E, Tell GS, Klepp KI . Predictors and tracking of body mass index from adolescence into adulthood. Follow-up of 18 to 20 years in the Oslo Youth Study. Arch Pediatr Adolesc Med 2003; 157: 1212–1218.
Guo SS, Chumlea W . Tracking of body mass index in children in relation to overweight in adulthood. Am J Clin Nutr 2000; 70 (Suppl): 145S–148S.
Gunnell D, Frankel S, Nanchahal K, Peters TJ, Davey Smith G . Childhood obesity and adult cardiovascular mortality: a 57-year follow-up study based on the Boyd Orr cohort. Am J Clin Nutr 1998; 67: 1111–1118.
Must A, Jacques PF, Dallal GE, Bajema CJ, Dietz WH . Long-term morbidity and mortality of overweight adolescents - a follow-up of the Harvard growth study of 1922–1935. N Engl J Med 1992; 327: 1350–1355.
Engeland A, Bjorge T, Sogaard AJ, Tverdal A . Body mass index in adolescence in relation to total mortality: 32-year follow-up of 227 000 Norwegian boys and girls. Am J Epidemiol 2003; 157: 517–523.
Wang Y, Zhang Q . Are American children and adolescents of low socioeconomic status at increased risk of obesity? Changes in the association between overweight and family income between 1971 and 2002. Am J Clin Nutr 2006; 84: 707–716.
Shrewsbury V, Wardle J . Socioeconomic status and adiposity in childhood: a systematic review of cross-sectional studies 1990–2005. Obesity 2008; 16: 275–284.
Liberatos P, Link BG, Kelsey JL . The measurement of social class in epidemiology. Epidemiol Rev 1988; 10: 87–121.
Krieger N, Williams DR, Moss NE . Measuring social class in US public health research: concepts, methodologies, and guidelines. Annu Rev Public Health 1997; 18: 341–378.
Braveman PA, Cubbin C, Egerter S, Chideya S, Marchi KS, Metzler M et al. Socioeconomic status in health research: one size does not fit all. JAMA 2005; 294: 2879–2888.
Wardle J, Waller J, Jarvis MJ . Sex differences in the association of socioeconomic status with obesity. Am J Public Health 2002; 92: 1299–1304.
Stamatakis E, Primatesta P, Chinn S, Rona R, Falascheti E . Overweight and obesity trends from 1974–2003 in English children: what is the role of socioeconomic factors? Arch Disease Child 2005; 90: 999–1004.
Prescott-Clarke P, Primatesta P (eds) Health Survey for England 1995. HMSO: London, 1997.
Craig R, Mindell J (eds) The Health Survey for England 2006: CVD and risk factors adults, obesity and risk factors children. Information Centre: Leeds, 2008, http://www.ic.nhs.uk/pubs/HSE06CVDandriskfactors (accessed 18th February 2009).
Cameron N . The growth of London schoolchildren 1904–1966: An analysis of secular trend and intra-county variation. Ann Hum Biol 1979; 6: 505–525.
Szreter SRS . The genesis of the Registrar-General's social classification of occupations. Br J Sociol 1984; 35: 522–546.
Stamatakis E, Hillsdon M, Mishra G, Hamer M, Marmot M . Television viewing and other screen-based entertainment in relation to multiple socioeconomic status indicators and area deprivation: The Scottish Health Survey 2003. J Epidemiol Community Health 2009; 63(9): 734–740.
Hillsdon M, Lawlor DA, Ebrahim S, Morris JN . Physical activity in older women: associations with area deprivation and with socioeconomic position over the life course: observations in the British Women's Heart and Health Study. J Epidemiol Community Health 2008; 62: 344–350.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH . Establishing a standard definition for child overweight and obesity worldwide: an international survey. BMJ 2000; 320: 1–6.
Lioret S, Touvier M, Dubuisson C, Dufour A, Calamassi-Tran G, Lafay L et al. Trends in child overweight rates and energy intake in France from 1999–2007: relationships with socioeconomic status. Obesity 2009; 17: 1092–1100.
Péneau S, Salanave B, Rolland-Cachera MF, Castetbon K, Hercberg S . The prevalence of overweight and obesity in 7–9 year old children in France is stable between 2000 and 2007. Int J Obes 2008; 32: S196.
Aeberli I, Amman RS, Knabenhans M, Zimmermann MB . The national prevalence of overweight in school-age children in Switzerland has decreased between 2002 and 2007. Int J Obes 2008; 32: S214.
Sjöberg A, Albertsson-Wikland LLK, Mårild S . Recent anthropometric trends among Swedish school children: evidence for decreasing prevalence of overweight in girls. Acta Pædiatrica 2008; 97: 118–123.
Ogden CL, Carroll MD, Flegal KM . High body mass index for age among US children and adolescents, 2003–2006. JAMA 2008; 299: 2401–2405.
International Food Information Council Foundation. Trends in Obesity-related media coverage Available online http://www.ific.org/research/obesitytrends.cfm (accessed 27th February 2009).
Department of Health. Spending Review 2004 Public Service Agreement. Department of Health: London, 2007, http://www.dh.gov.uk/en//AboutusHowDHworks/Servicestandardsandcommitments/DHPublicServiiceAgreement/DH_4106188 (accessed 27th February 2009).
Hercberg S, Chat-Yung S, Chauliac M . The French National Nutrition and Health Program: 200120062010. Int J Pub Health 2008; 53: 68–77.
Prescott-Clarke P, Primatesta P (eds) Health Survey for England. The health of young people ′95–97. HMSO: London, 1998.
Adler NE, Boyce T, Chesney MA, Cohen S, Folkman S, Kahn RL, Syme SL . Socioeconomic-status and health—the challenge of the gradient. Am Psychol 1994; 49: 15–24.
Iversen AC, Kraft P . Does socio-economic status and health consciousness influence how women respond to health related messages in media? Health Educ Res 2006; 21: 601–610.
King's Fund Health Development Agency. Public attitudes to public health policy. King's Fund: London, 2004.
Turrell G, Patterson C, Oldenburg B, Gould T, Roy M-A . The socio-economic patterning of survey participation and non-response error in a multi-level study of food purchasing behaviour: area- and individual-level characteristics. Public Health Nutr 2002; 6: 181–189.
Colhoun H, Prescott-Clarke P (eds) The Health Survey for England 1994 Volume II: Survey Methodology and Documentation. The Stationery Office: London, 1996.
Sobal J, Stunkard AJ . Socioeconomic status and obesity—a review of the literature. Psychol Bull 1989; 105: 260–275.
Acknowledgements
The Health Survey for England is funded by the English Department of Health and the Health and Social Care Information Centre. This work was not supported by any specific source of funding. We thank the families and children who participated in the Health Survey for England.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stamatakis, E., Wardle, J. & Cole, T. Childhood obesity and overweight prevalence trends in England: evidence for growing socioeconomic disparities. Int J Obes 34, 41–47 (2010). https://doi.org/10.1038/ijo.2009.217
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2009.217
Keywords
This article is cited by
-
The influence of immigrant background and parental education on overweight and obesity in 8-year-old children in Norway
BMC Public Health (2023)
-
Decomposing the Intraurban Malnutrition Gap Between Poor and Non-poor Children in Colombia
Journal of Urban Health (2023)
-
Update on the Obesity Epidemic: After the Sudden Rise, Is the Upward Trajectory Beginning to Flatten?
Current Obesity Reports (2023)
-
Perceptions of a family-based lifestyle intervention for children with overweight and obesity: a qualitative study on sustainability, self-regulation, and program optimization
BMC Public Health (2022)
-
Interventions in the first 1000 days to prevent childhood obesity: a systematic review and quantitative content analysis
BMC Public Health (2022)