Abstract
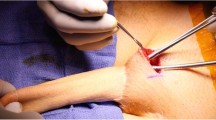
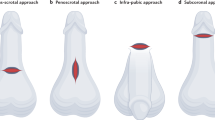
The aim of this study was to describe the technical aspects and short-term outcomes of inflatable penile prosthesis (IPP) implantation after neophallus reconstruction at a single institution. Nine men with previously constructed radial forearm neophalli underwent IPP implantation. The etiologies of their penile anomaly were bladder exstrophy complex in five, disorder of sexual differentiation in two and genital obliteration secondary to ballistic trauma in two. Median follow-up was 9.6 months (range 1.5–139.7). The records for these patients were retrospectively reviewed and outcomes recorded. Mean age was 23.6 (range 18–31) years, and mean time interval from neophalloplasty to IPP implantation was 22.1 months (range 3–48). In all cases, 3-piece IPPs were employed, with eight of patients having one cylinder implanted in the native corporal body and extending into the neophallus. Mean surgical time was 222 min (range 142–409). Median length of implanted device was 22 cm. No intraoperative complications were observed. At the most recent follow-up, six patients (66.7%) had functional devices, with acceptable surgical outcomes. Three patients (33.3%) sustained device infections, and three (33.3%) sustained cylinder erosion. In three patients in whom neo-tunica albuginea were fashioned by ensheathing the cylinder with allograft human dermal tissue matrix, no erosions occurred. One patient underwent two revisions, the first for the associated erosion and infection and the second for genital pain, and was left with a semi-rigid prosthesis. IPP implantation affords the best opportunity for functionality for patients with a radial forearm free flap neophallus. Caution must be taken to ensure viability of the neophallus intraoperatively, and protocols to minimize the risk of infection should be followed. Fashioning neo-tunica albuginea using graft material may reduce risk of erosion.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bluebond-Langner R, Redett RJ . Phalloplasty in complete aphallia and ambiguous genitalia. Semin Plast Surg 2011; 25: 196–205.
Bettocchi C, Ralph DJ, Pryor JP . Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int 2005; 95: 120–124.
Hoebeke P, de Cuypere G, Ceulemans P, Monstrey S . Obtaining rigidity in total phalloplasty: experience with 35 patients. J Urol 2003; 169: 221–223.
Hoebeke PB, Decaestecker K, Beysend M, Opdenakker Y, Lumen N, Monstrey SM . Erectile implants in female-to-male transsexuals: our experience in 129 patients. Eur Urol 2010; 57: 334–341.
Lumen N, Monstrey S, Selvaggi G, Ceulemans P, De Cuypere G, Van Laecke E et al. Phalloplasty: a valuable treatment for males with penile insufficiency. Urology 2008; 71: 272–276.
Garaffa G, Raheem AA, Christopher NA, Ralph DJ . Total phallic reconstruction after penile amputation for carcinoma. BJU Int 2009; 104: 852–856.
Massanyi EZ, Gupta A, Goel S, Gearhart JP, Burnett AL, Bivalacqua TJ et al. Radial Forearm Free Flap Phalloplasty for Penile Inadequacy in Exstrophy Patients. J Urol 2012; 190 (4 Suppl): 1577–1582.
Jordan GH, Alter GJ, Gilbert DA, Horton CE, Devine CJ . Penile prosthesis implantation in total phalloplasty. J Urol 1994; 152: 410–414.
Ballaro A, Pryor JP, Ralph DJ . Prosthesis implantation after radial free flap phalloplasty in patient with bladder exstrophy. Int J Imp Res 1999; 11: 341–342.
Levine LA, Zachary LS, Gottlieb LJ . Prosthesis placement after total phallic reconstruction. J Urol 1993; 149: 593–598.
Hage JJ . Dynaflex prosthesis in total phalloplasty. Plast Reconstr Surg 1997; 99: 479–485.
Katz DJ, Stember DS, Nelson CJ, Mulhall JP . Perioperative prevention of penile prosthesis infection: practice patterns among surgeons of SMSNA and ISSM. J Sex Med 2012; 9: 1705–1712.
Fisch M, Wammack R, Ahlers J, Sennerich T, Müller SC, Hohenfellner R . Osseous fixation of a penile prosthesis after transsexual phalloplasty: a case report. J Urol 1993; 149: 122–125.
Perovic SV, Djinovic R, Bumbasirevic M, Djordjevic M, Vukovic P . Total phalloplasty using a musculocutaneous latissimus dorsi flap. BJU Int 2007; 100: 899–905.
Serefoglu EC, Mandava SH, Gokce A, Chouhan JD, Wilson SK, Hellstrom WJ . Long-Term Revision Rate due to infection in hydrophilic-coated inflatable penile prostheses: 11-year follow-up. J Sex Med 2012; 9: 2182–2186.
Wilson SK, Zumbe J, Henry GD, Salem EA, Delk JR, Cleves MA . Infection reduction using antibiotic-coated inflatable penile prosthesis. Urol 2007; 70: 337–340.
Silver RI, Yang A, Ben-Chaim J, Jeffs RD, Gearhart JP . Penile length in adulthood after exstrophy reconstruction. J Urol 1997; 157: 999–1003.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Segal, R., Massanyi, E., Gupta, A. et al. Inflatable penile prosthesis technique and outcomes after radial forearm free flap neophalloplasty. Int J Impot Res 27, 49–53 (2015). https://doi.org/10.1038/ijir.2014.30
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2014.30
This article is cited by
-
Current management of classic bladder exstrophy in the modern era
African Journal of Urology (2023)
-
Erectile device insertion following phalloplasty in transgender and non-binary individuals assigned female at birth: a narrative review
International Journal of Impotence Research (2023)
-
Vascularized composite allotransplantation of the penis: current status and future perspectives
International Journal of Impotence Research (2022)
-
Inflatable penile prosthesis implantation after gender affirming phalloplasty with radial forearm free flap
International Journal of Impotence Research (2020)
-
Male Genital Reconstruction in the Exstrophy-Epispadias Complex
Current Sexual Health Reports (2020)